Abstract
• Demonstrates that the relationship between loneliness and chronic diseases among older adults is mediated through depression and self-perceived health. • Identifies that the mediation pathway is stronger among younger older adults compared to their older counterparts. • Highlights the importance of addressing mental health and self-perceived health in interventions for older adults experiencing loneliness.
• Supports the development of interventions targeting loneliness to prevent chronic diseases in older adults. • Suggests gerontological practices should include mental health assessments to mitigate the negative health effects of loneliness. • Provides insights for policymakers on the need for age-specific strategies to promote healthy aging in socially isolated older adults.What this paper adds
Applications of study findings
Introduction
Loneliness and social isolation have emerged as significant public health concerns among older adults (Joshi et al., 2024). As the global population ages, understanding the complex relationship between loneliness, mental health, and physical well-being becomes increasingly crucial (Jessen et al., 2018). The negative impact of loneliness on mental health has been consistently demonstrated, with a recent longitudinal study (Lee et al., 2021) finding that loneliness was a significant predictor of depressive symptoms among adults aged 50 years and older over 12 years. Moreover, loneliness has been linked to an increased risk of chronic diseases, with a longitudinal study by Christiansen et al. (2021) revealing that loneliness was associated with a higher incidence of diabetes and hypertension among older adults in Denmark. There is a pressing need to better understand the complex pathways through which loneliness influences health outcomes in older populations, to inform targeted interventions and policies aimed at promoting healthy aging in the context of the ongoing pandemic and beyond (Ehni & Wahl, 2020). Several theoretical models offer critical insights into the complex relationships between loneliness, depression, self-perceived health, and chronic diseases. The Stress Process Model (Pearlin et al., 1981) highlights how stressors, such as loneliness, trigger both psychological and physiological responses that profoundly affect mental and physical health (Pengpid & Peltzer, 2021). Loneliness is conceptualized as a stressor that fosters depressive symptoms and negative health perceptions, which subsequently heighten vulnerability to chronic diseases (Christiansen et al., 2021). The model (Pearlin et al., 1981) emphasizes that loneliness does not function in isolation; rather, it interacts with psychosocial and physiological factors, including coping mechanisms and social support (Lochmannová & Martin, 2025), to influence health outcomes (Green, 2024). As chronic loneliness persists, it intensifies depressive symptoms, undermines self-esteem, and deteriorates overall well-being. The model further underscores the mediating role of coping strategies and social support, though it asserts that their efficacy is limited without adequate social resources. Consequently, the Stress Process Model provides a robust framework for understanding how loneliness contributes to chronic diseases via depression and self-perceived health, with age moderating these pathways (Pearlin et al., 1981). Age-related changes in social roles, health status, and psychosocial resilience may influence the strength and nature of these relationships, leading to varying health outcomes as individuals age (Green, 2022; Kim & Park, 2023).
Proposing a theoretical model, that aims to investigate the direct and indirect relationships between loneliness, depression, self-perceived health, and the number of chronic diseases among Israeli adults aged 50 and above, sheds light on the complex pathways through which loneliness may influence health outcomes in this specific population. Recent research has consistently demonstrated the negative effects of loneliness on mental health, with a particular focus on depression (Erzen & Çikrikci, 2018). A meta-analysis by Erzen and Çikrikci (2018) found a significant positive correlation between loneliness and depression across various age groups. Similarly, a longitudinal study revealed that loneliness was a full-bodied predictor of depression among older adults, highlighting the need for targeted interventions to reduce loneliness and promote mental well-being in this population (Lee et al., 2021). This suggests that the negative emotional states associated with loneliness, such as perceived isolation and lack of social support, may contribute to the development and maintenance of depression in older individuals (Hawkley & Kocherginsky, 2018).
The relationship between loneliness and self-perceived health has also gathered attention in recent years (Choi et al., 2015; Domènech-Abella et al., 2019; Ong et al., 2016). A cross-sectional study conducted by Choi et al. (2015) found that loneliness was significantly associated with poorer self-perceived health among older adults.. Moreover, a longitudinal study by Smith and Victor (2019) demonstrated that loneliness predicted a decline in self-perceived health over time, emphasizing the long-term consequences of loneliness on health perceptions (Smith & Victor, 2019). This relationship may be explained by the fact that lonely individuals tend to engage in less health-promoting behaviors, such as physical activity and social engagement, which in turn can negatively affect their subjective evaluations of their health status (Richard et al., 2017). Furthermore, studies have demonstrated that loneliness contributes to the onset of acute health events (Sedláček et al., 2024), thereby amplifying the susceptibility of older adults to the development of chronic conditions. The Biopsychosocial Model (Engel, 1977) is particularly relevant for understanding how loneliness contributes to chronic diseases through its effects on self-perceived health. This model highlights the interdependence of biological, psychological, and social factors in shaping health outcomes. Loneliness, as a biopsychosocial phenomenon, influences psychological well-being, which in turn affects physiological processes such as immune function and stress response. Loneliness acts as a stressor, intensifying depressive symptoms and negative health perceptions, thus increasing susceptibility to chronic diseases. While the model has faced critique for its lack of precise causal mechanisms and scientific rigor, particularly in establishing definitive cause-effect relationships, it remains a valuable conceptual framework (Roberts, 2023). The Biopsychosocial Model directs attention to how loneliness, depression, and self-perceived health interact, while also considering how age may moderate these relationships (Engel, 1977). As individuals age, the impact of loneliness may vary due to changes in social roles, health status, and psychosocial resilience, which influence these pathways.
Also, the impact of loneliness on the development and progression of chronic diseases has been a topic of growing interest (Christiansen et al., 2021; Lara et al., 2019; Malcolm et al., 2019). A systematic review conducted by Malcolm et al. (2019) found important evidence linking loneliness to an increased risk of cardiovascular disease and cognitive decline. Additionally, a longitudinal study conducted by Christiansen et al. (2021) revealed that loneliness was associated with a higher incidence of chronic diseases, such as diabetes and hypertension, among older adults in Denmark. This may be attributed to the chronic activation of stress response systems and inflammation in lonely individuals, which can contribute to the development and progression of various chronic conditions over time (Nersesian et al., 2018). Additionally, Life Course Theory (Elder, 1975) offers valuable insights into how the effects of loneliness, depression, and self-perceived health may evolve over time and across different life stages (Johnson et al., 2011). According to this theory, the accumulation of life experiences, including periods of loneliness, has a profound impact on long-term health outcomes. In older adults, the effects of loneliness may be exacerbated by age-related physiological and social changes. This suggests that experiences of loneliness in earlier life stages can shape health perceptions and contribute to mental and physical health decline in later life (Elder, 1998). The theory also highlights that loneliness does not operate in isolation but rather interacts with other psychosocial and physiological factors, such as depression and self-perceived health, which together influence the trajectory of health outcomes as individuals age (Elder, 1975).
While the individual relationships between loneliness, depression, self-perceived health, and chronic diseases have been explored, there is a relative lack of research examining the integrated effects of these factors (Beller & Wagner, 2018; Iecovich & Biderman, 2012; Zubala et al., 2017), particularly in the context of older Israeli adults. This gap underscores the need for a more comprehensive theoretical model that captures the complex, interwoven relationships among these variables. By incorporating these theoretical perspectives, this study aims to offer a more integrated understanding of how loneliness influences chronic disease development. Specifically, the Stress Process Model, Biopsychosocial Model, and Life Course Theory collectively provide a comprehensive framework for examining the pathways through which loneliness contributes to health outcomes, while also considering how these pathways may differ by age.
The proposed theoretical model in this study aims to address this gap by investigating the direct and indirect pathways through which loneliness influences health outcomes, with a specific focus on the mediating roles of depression and self-perceived health. In particular, the potential chain mediating effects of depression and self-perceived health in the relationship between loneliness and chronic diseases have not been fully explored (Beller & Wagner, 2018; Zubala et al., 2017), especially in the context of older Israeli adults. Given the varying social, physiological, and cognitive changes that occur in older adults, it is crucial to examine how this model operates across different age groups beyond 50 years old.
The inclusion of age as a moderating factor in the proposed model adds a novel dimension to the existing literature (Ehni & Wahl, 2020; Krendl & Perry, 2021). By examining how the relationships between loneliness, depression, self-perceived health, and chronic diseases may vary across different age groups within the older adult population, this study aims to provide more valuable insights into the age-specific vulnerabilities and potential intervention targets. Furthermore, the role of age as a moderator in these pathways merits further investigation, as the nature and strength of these relationships may vary across different stages of later life (Ehni & Wahl, 2020; Krendl & Perry, 2021).
Moreover, the focus on the Israeli context is particularly relevant, as Israel has a rapidly aging population and faces unique challenges related to social support and healthcare provision (Jacob et al., 2019; Palgi et al., 2020; Shrira et al., 2020). By conducting this research among Israeli adults aged 50 and above, the study aims to contribute to the development of culturally sensitive interventions and policies that address the specific needs of this population.
This study offers theoretical mechanisms, including psychological, behavioral, and physiological processes that interact to shape health trajectories in later life (Hawkley & Capitanio, 2015). Therefore, the present study proposes a comprehensive theoretical model to investigate the complex relationships between loneliness (behavioral aspect), depression (psychological aspect), self-perceived health (physiological aspect), and the number of chronic diseases (physiological aspect) and age (physiological aspect) among Israeli adults aged 50 and above (See Figure 1). It provides valuable insights into the mechanisms underlying the adverse health outcomes associated with loneliness. Serial mediation model: loneliness to chronic diseases through depression and self-perceived health, with age as moderator.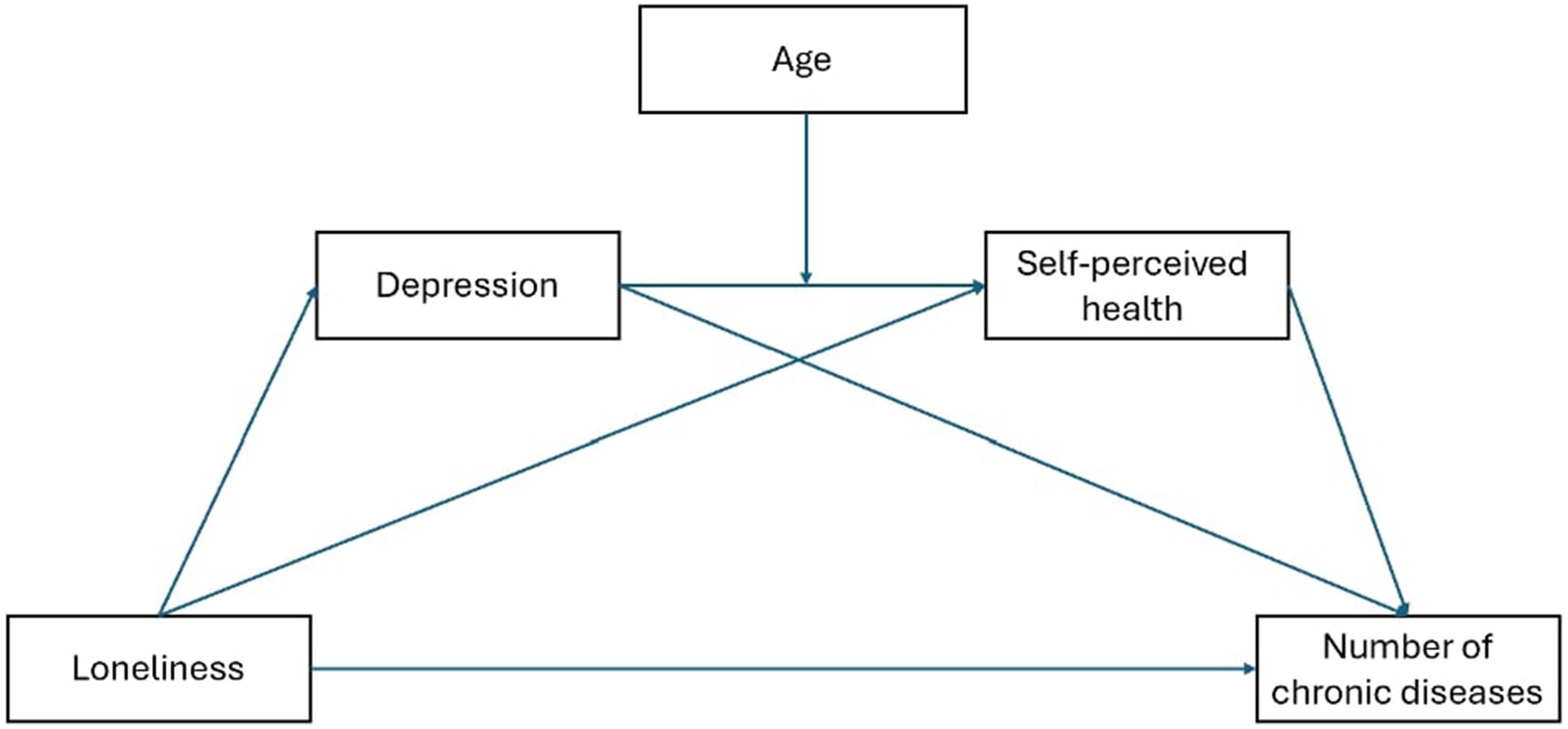
Based on the model and the study’s aim, the research hypotheses are as follows:
Methods
SHARE (Survey of Health, Ageing and Retirement in Europe) is a cross-national panel survey that collects comprehensive data on the health, socioeconomic status, and social networks of individuals aged 50 and older. While longitudinal data would provide stronger evidence for causal relationships, the cross-sectional design employed in this study is appropriate for the research aims and hypotheses. The purpose of this study was to examine the complex associations between loneliness, depression, self-perceived health, and chronic diseases among older adults in Israel at a specific point in time. Cross-sectional designs are well-suited for investigating the prevalence of health conditions and identifying associations between variables (Setia, 2016). The large, representative sample of older adults in Israel available in Wave 9 of the SHARE data allows for a comprehensive examination of the relationships between the key study variables. Cross-sectional data is appropriate for initial tests of theoretical models and can provide a foundation for future longitudinal studies to confirm the directionality and causality of the relationships (Spector, 2019).
Data
This study utilized Wave 9 of SHARE, focusing specifically on the Israeli population (Mehrbrodt et al., 2019). We extracted relevant variables, including depression (measured by the EURO-D scale), self-perceived health, number of chronic diseases, loneliness (assessed using the three-item loneliness scale), and various demographic factors such as age, years of education, number of children and grandchildren, living arrangements, relationship status, and gender. After handling missing data, the final sample consisted of 744 participants from Israel.
While additional waves of SHARE data are available, Wave 9 was selected for this study due to its recency and inclusion of relevant variables on loneliness, depression, self-perceived health, and chronic diseases. Data collection for Wave 9 was conducted from 2019 to 2021 (Börsch-Supan, 2024), providing a contemporary snapshot of the experiences of older adults in Israel. Furthermore, Wave 9 included key variables that were essential for testing the study’s hypotheses, such as the Three-Item Loneliness Scale, the EURO-D depression scale, and self-perceived health measures. The large sample size in Wave 9 (N = 744) also provided sufficient statistical power to detect the hypothesized mediation and moderation effects.
In this study, we examined missing values across all variables included in the model. The analysis revealed missing data patterns as follows: The Depression scale had 124 missing values out of 744 participants (16.7%), the loneliness measure had 59 missing values (7.9%), self-rated health had 5 missing values (0.7%), age had no missing values, and number of chronic conditions had 5 missing values (0.7%). Based on the proportion of missing values, we implemented a systematic approach to handling missing data: For variables with minimal missing values, such as self-rated health and number of chronic conditions (both with 0.7% missing), we applied mean imputation. This method is appropriate for continuous variables with negligible missing rates and is not expected to significantly impact the results (Graham, 2009).
For variables with moderate levels of missing data, specifically loneliness (7.9%) and depression (16.7%), we employed multiple imputations. This technique generates multiple complete datasets based on other variables while preserving the statistical relationships between variables (Azur et al., 2011). During the imputation process, we selected theoretically relevant predictor variables, including age and self-rated health to maintain the original data structure.
Following the imputation procedures, we repeated the analysis (PROCESS Model 91) and found that the findings remained consistent in both significance and conclusions. These results strengthen the validity of our research and indicate that the missing values did not substantially influence the main outcomes.
Instruments
Independent Variable
Loneliness variable: Loneliness was evaluated using the Three-Item Loneliness Scale (Hughes et al., 2004), a short version of the R-UCLA Loneliness Scale. It measures loneliness through three items answered on a three-point Likert scale (“frequently,” “occasionally,” “rarely or never”). The score ranges from 3 to 9, with higher scores indicating greater loneliness. An example item is “How often do you feel left out?”. The resulting score ranges from a minimum of three (“not lonely”) to a maximum of nine (“extremely lonely”). The operationalization in SHARE includes the generated Loneliness Scale variable (loneliness) within the gv_health module. This variable is a sum score derived from items mh034_, mh035_, and mh036_ in the mental health module.
Mediators
Depression mediator: Depression was measured using the EURO-D (Prince, Beekman, et al., 1999; Prince, Reischies, et al., 1999), provided in the SHARE dataset as a generated variable in the gv_health module. The scale consists of 12 items covering symptoms such as depression, pessimism, suicidality, sleep, interest, irritability, appetite, fatigue, concentration, enjoyment, and tearfulness. The EURO-D score (eurod) is generated from questions in the mental health module (mh002_–mh017_) as a composite index. The information from mh005_/mh006_, mh008_/mh009_, mh011_/mh012_, and mh014_/mh015_ is combined when generating EURO-D, reducing the original 16 items to 12 final items in gv_health module. This generated variable in the gv_health module allows for easy use in analyses and ensures consistency across different waves of the SHARE study. The scale ranges from 0 to 12, with higher scores indicating more depressive symptoms. A score of 0 represents “not depressed,” while 12 indicates “very depressed”. The EURO-D has shown good internal consistency, with a Cronbach’s alpha of 0.75. An example item is “In the last month, have you been sad or depressed?”.
Self-perceived health mediator: Self-perceived health was assessed using a single item from the US version of the self-perceived health measure. Respondents rate their present general health on a five-point Likert scale ranging from “excellent” to “poor.” This measure is based on the SF-36 questionnaire (Ware & Gandek, 1998) and has been widely used in health research. For the purposes of this study, the response scale was reversed so that higher scores indicate better self-perceived health. This recoding allows for more intuitive interpretation, where a higher score represents a better health status.
Dependent Variable (Outcome)
Number of chronic diseases: It was determined by asking participants about the presence of the number of chronic conditions (conditions such as cancer, chronic obstructive pulmonary disease, coronary heart disease, diabetes, hypertension, and stroke) from a list provided in the SHARE questionnaire. This measure indicates the overall health burden experienced by the respondent.
Background Variables
Included age, years of education, number of children, number of grandchildren, living in a nursing home, marital status, relationship status, and gender. These were collected through standard demographic questions in the SHARE survey (Mehrbrodt et al., 2019).
Statistical Analysis
Statistical analyses were conducted using IBM SPSS Statistics version 28.0. The PROCESS macro version 3.5 (Hayes, 2014) was employed for advanced analyses. Descriptive statistics were computed to summarize the sample characteristics. Pearson correlation coefficients were calculated to examine the relationships between variables. Independent sample t-tests were performed to compare group differences. To test the moderated mediation hypotheses, we utilized PROCESS models 6 and 91, which allow for the examination of sequential mediation and moderated mediation effects, respectively.
Furthermore, a reanalysis using Model 91 with a number of children and years of education as control variables confirmed a significant moderated serial mediation, where the indirect effect of loneliness on chronic illness through depression and self-perceived health is significantly moderated by age, with stronger effects observed at younger ages compared to older ages. The control variables were measured as follows: number of children (continuous variable reporting total children) and years of education (continuous variable measuring education years).
Results
The study included 744 participants, and the sample consisted of older adults with a mean age of 74.87 years (SD = 8.87), ranging from 46 to 95 years. The participants had on average 12.89 years of education (SD = 4.14), with a range of 0–25 years of formal education. Participants had an average of 3.14 children (SD = 2.02), with the number of children ranging from 0 to 13.
Regarding the key variables in our study, self-perceived health had a mean score of 3.32 (SD = 1.20), with values ranging from 1 to 5. Loneliness had a mean score of 4.35 (SD = 1.77) and ranged from 3 to 9. The depression scale showed a mean of 2.93 (SD = 2.67), with scores ranging from 0 to 12. The number of chronic diseases averaged 2.50 (SD = 2.16), ranging from 0 to 11. To situate the descriptive scores, we compared them with benchmarks from large European studies of older adults. On the Three-Item Loneliness Scale, our participants’ mean score (M = 4.35, SD = 1.77) is modestly higher than the weighted normative mean of 4.08 reported for Spanish adults aged ≥65 years in a representative national sample (Trucharte et al., 2021). Likewise, the mean EURO-D score observed here (M = 2.93, SD = 2.67) sits at the upper boundary of the 1.8–3.1 range documented across 11 European countries in the SHARE survey (Guerra et al., 2015).
Demographic Characteristics by Age Groups.
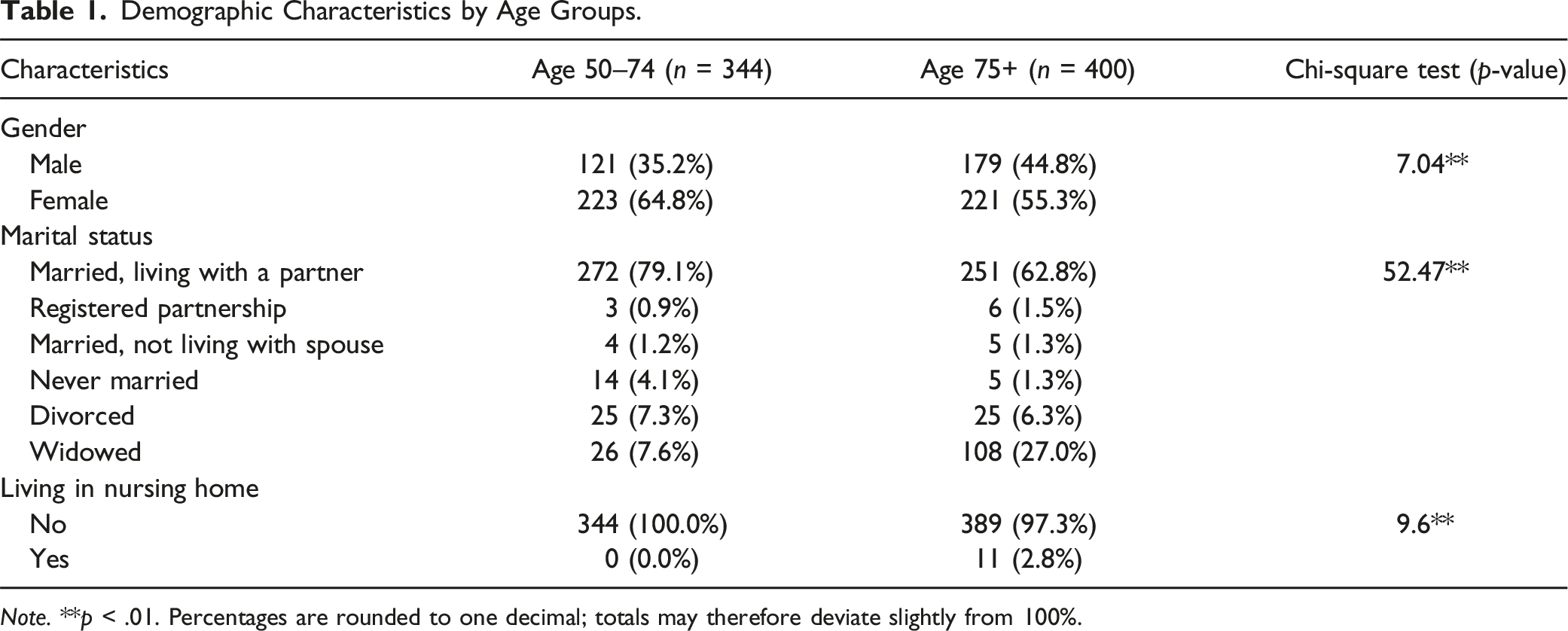
Note. **p < .01. Percentages are rounded to one decimal; totals may therefore deviate slightly from 100%.
Table 1 presents the demographic characteristics of the sample by age groups. The younger age group had a higher proportion of females (64.8%) than the older age group (55.3%).
The younger age group had a higher number of married individuals living with their partner (79.1%) than the older age group (62.8%). Widowhood was more frequent in the older age group (27.0%) than in the younger age group (7.6%). The proportion of individuals living in nursing homes was higher in the older age group (2.8%) than in the younger age group (0.0%).
Independent Samples T-Tests Comparing Age Groups on Demographic Characteristics and Health Indicators.
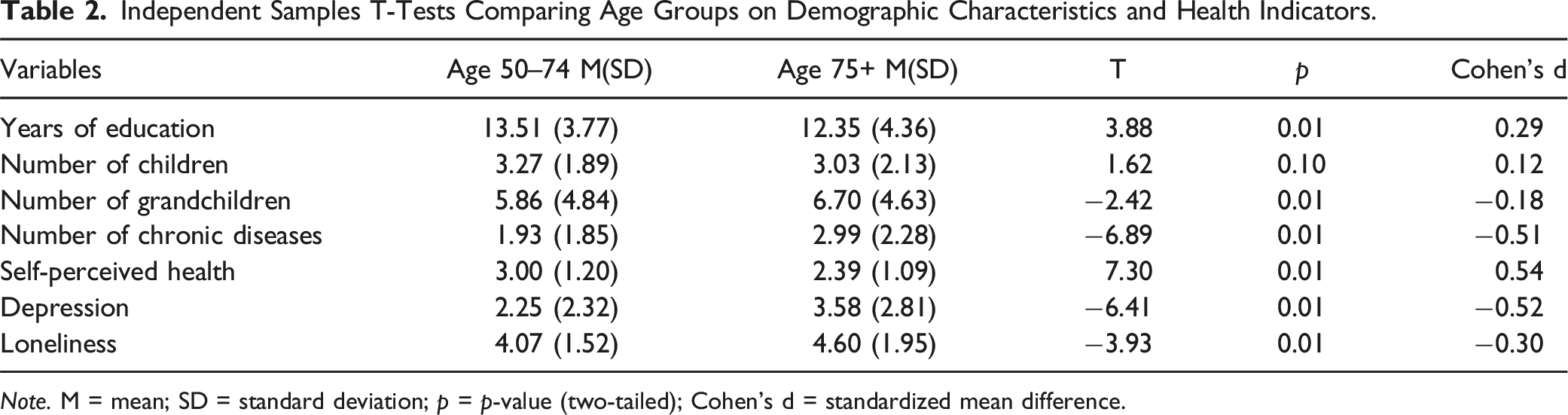
Note. M = mean; SD = standard deviation; p = p-value (two-tailed); Cohen’s d = standardized mean difference.
Table 2 presents the older age group as having significantly fewer years of education (M = 12.35, SD = 4.36) than the younger age group (M = 13.51, SD = 3.77). The older age group had significantly more grandchildren (M = 6.70, SD = 4.63) than the younger age group (M = 5.86, SD = 4.84). The older age group had significantly more chronic diseases (M = 2.99, SD = 2.28) than the younger age group (M = 1.93, SD = 1.85). Self-perceived health was significantly poorer in the older age group (M = 2.39, SD = 1.09) than in the younger age group (M = 3.00, SD = 1.20). Depression levels were higher in the older age group (M = 3.58, SD = 2.81) than in the younger age group (M = 2.25, SD = 2.32). Loneliness scores were also significantly higher in the older age group (M = 4.60, SD = 1.95) than in the younger age group (M = 4.07, SD = 1.52).
Correlations, Means, and Standard Deviations for Models' Variables.
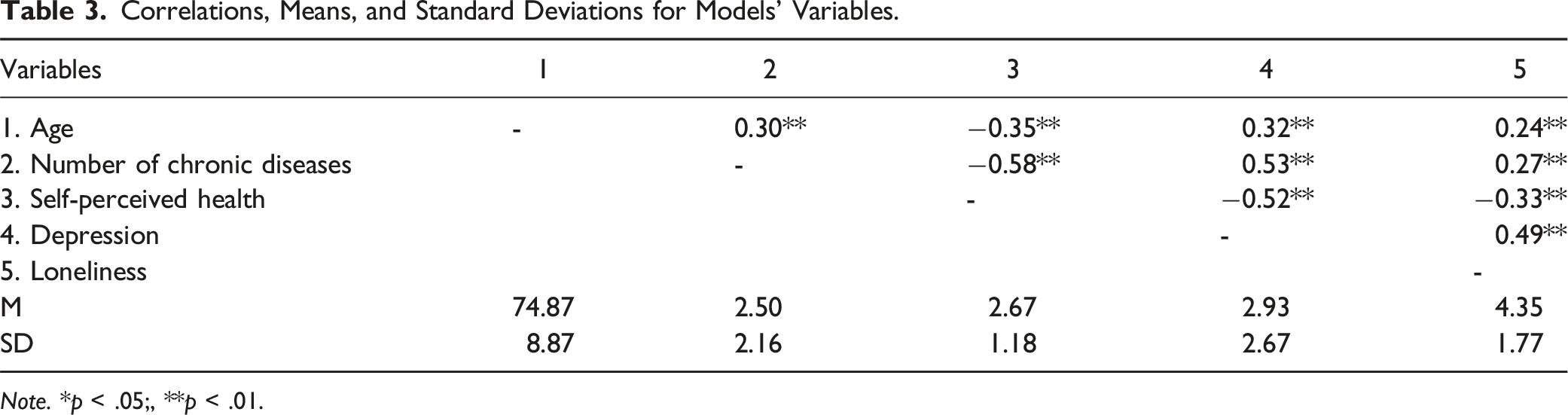
Note. *p < .05;, **p < .01.
Table 3 presents age was positively correlated with the number of chronic diseases (r = 0.30, p < .01), depression (r = 0.32, p < .01), and loneliness (r = 0.24, p < .01), and negatively correlated with self-perceived health (r = −0.35, p < .01). The number of chronic diseases was negatively correlated with self-perceived health (r = −0.58, p < .01) and positively correlated with depression (r = 0.53, p < .01) and loneliness (r = 0.27, p < .01). Self-perceived health was negatively correlated with depression (r = −0.52, p < .01) and loneliness (r = −0.33, p < .01). Finally, depression and loneliness were positively correlated (r = 0.49, p < .01).
Chain Mediating Role of Depressive Symptoms and Self-Perceived Health.
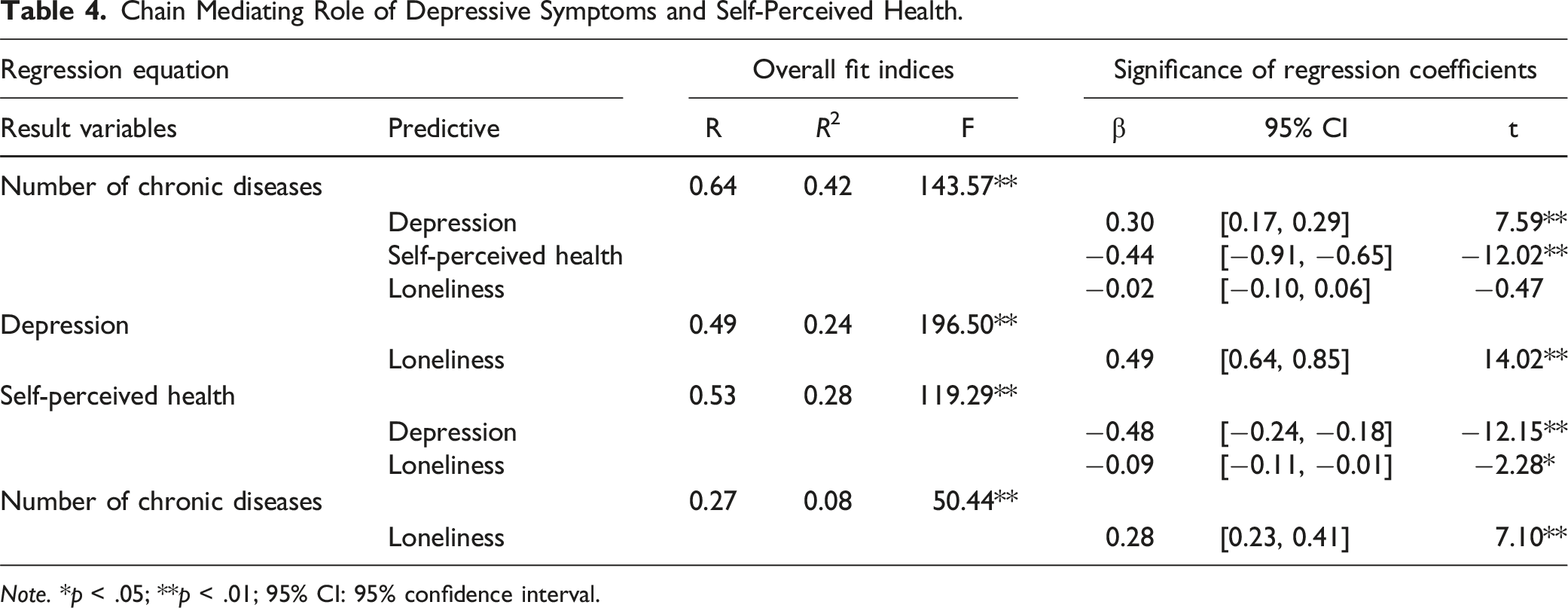
Note. *p < .05; **p < .01; 95% CI: 95% confidence interval.
Loneliness significantly predicted higher depression scores (β = 0.49, p < .01). Depression, in turn, was a strong predictor of poorer self-perceived health (β = −0.48, p < .01), while loneliness had a smaller but still significant direct effect on self-perceived health (β = −0.09, p = .02). In the final model predicting the number of chronic diseases, depression (β = 0.30, p < .001) and self-perceived health (β = −0.44, p < .001) were significant predictors.
Mediating Effect (Direct and Indirect) of the Model.
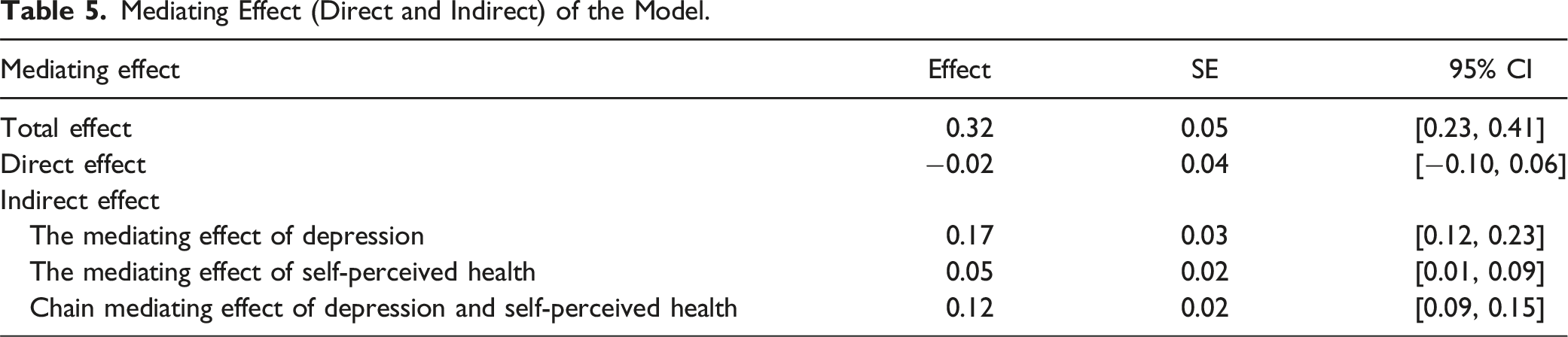
Table 5 presents the total effect of loneliness on chronic illness as 0.32 (SE = 0.05, 95% CI [0.23, 0.41]), indicating a significant overall relationship between the two variables. However, the direct effect of loneliness on chronic illness is −0.02 (SE = 0.04, 95% CI [−0.10, 0.06]), which was insignificant. This suggests that loneliness does not directly influence chronic illness when accounting for the mediating variables.
The indirect effects reveal that loneliness influences chronic illness through three pathways. First, loneliness has a mediating impact through depression, with an effect size of 0.17 (SE = 0.03, 95% CI [0.12, 0.23]). Second, loneliness has a mediating effect through self-perceived health, with an effect size of 0.05 (SE = 0.02, 95% CI [0.01, 0.09]). Finally, there is a chain-mediating effect of loneliness on chronic illness through depression and self-perceived health, with an effect size of 0.12 (SE = 0.02, 95% CI [0.09, 0.15]).
Conditional Indirect Effects of Loneliness on Chronic Illness Through Depression and Self-Perceived Health at Different Levels of Age.
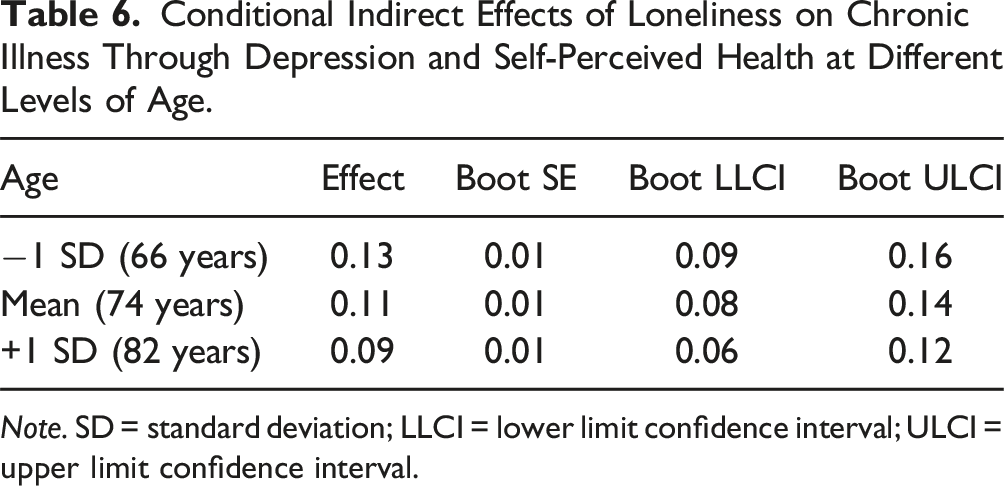
Note. SD = standard deviation; LLCI = lower limit confidence interval; ULCI = upper limit confidence interval.
Table 6 shows that the serial mediation effect was stronger at younger ages (1 SD below mean age: Effect = 0.13, 95% CI: 0.09, 0.16) compared to older ages (1 SD above mean age: Effect = 0.09, 95% CI: 0.06, 0.12).
Discussion
In this study, we strived to investigate the mediating series of roles of depression and self-perceived health on the relationship between loneliness and the number of chronic diseases and to examine how age moderates these relationships among older adults in Israel. It was found that the relationship between loneliness and the number of chronic diseases is mediated through depression and self-perceived health, with age moderating this mediation pathway. The relationship between loneliness and chronic illness, series mediated by depression and self-rated health, is stronger among younger elder adults compared to older. These findings contribute to the growing body of literature on the detrimental effects of loneliness on physical health outcomes (Lee et al., 2021; Nguyen et al., 2020).
The relationship between loneliness and the number of chronic diseases is consistent with recent research demonstrating that loneliness is a significant risk factor for various chronic conditions, such as cardiovascular disease, diabetes, and cognitive decline (Macdonald & Hülür, 2021). This study extends the understanding of this association by identifying the mediating roles of depression and self-perceived health in the pathway from loneliness to chronic diseases which are stronger among younger elder adults compared to older.
Depression emerged as a significant mediator in the relationship between loneliness and chronic diseases, aligning with current evidence suggesting that loneliness is a strong predictor of depressive symptoms (Lee et al., 2021). Loneliness may lead to depression through various mechanisms, such as reduced social support, increased stress, and negative self-perceptions (Domènech-Abella et al., 2019; Park et al., 2020; Shrira et al., 2020). In turn, depression has been linked to an increased risk of developing chronic diseases, possibly due to its impact on health behaviors, immune function, and neuroendocrine processes (Keenan-Miller et al., 2007; Penninx & Lange, 2018).
Self-perceived health also played as a mediating role in the pathway from loneliness to chronic diseases. This finding is consistent with recent studies showing that loneliness is associated with poorer self-perceived health (Nersesian et al., 2018; Richard et al., 2017). Loneliness may influence an individual’s perception of their health status through psychological and physiological pathways, such as increased stress, reduced self-efficacy, and altered immune function (Beller & Wagner, 2018; Luo et al., 2012). Poor self-perceived health, in turn, has been identified as a strong predictor of chronic disease development and mortality (Latham & Peek, 2013; Wuorela et al., 2020).
The series mediation pathway revealed in this study highlights the interconnectedness of loneliness, depression, self-perceived health, and chronic diseases. This innovative model suggests that loneliness may lead to depression in turn influences self-perceived health, ultimately increasing the risk of developing chronic diseases. The finding that the chain mediation effect is more pronounced among younger older adults may be attributed to age-related differences in social networks and coping mechanisms (Bruine de Bruin et al., 2020). Younger older adults may be more vulnerable to the negative effects of loneliness due to life transitions, such as retirement or the loss of social roles, which can lead to a reduction in social connections and support (Hawkley & Kocherginsky, 2018). Additionally, younger older adults may have less developed coping strategies to deal with the emotional and psychological consequences of loneliness compared to their older counterparts, who may have accumulated more resilience and adaptability over time (Ong et al., 2016). The identification of this complex pathway provides a more comprehensive understanding of the mechanisms through which loneliness affects physical health outcomes (Christiansen et al., 2016; Hawkley & Capitanio, 2015).
Also, the moderating effect of age on the mediation pathway emphasizes the importance of considering age-related differences in the impact of loneliness on health. The finding that the mediation pathway was stronger among younger older adults suggests that the negative consequences of loneliness may be more pronounced possibly due to age-related changes in social networks, coping mechanisms (Hawkley & Kocherginsky, 2018; Ong et al., 2016).
The pioneering nature of this study lies in its integration of multiple psychological and health-related variables into a comprehensive model, offering a novel perspective on the pathways linking loneliness to chronic diseases. By examining the mediating roles of depression and self-perceived health, as well as the moderating effect of age, this research provides valuable insights into the complex interplay between psychosocial factors and physical health outcomes among older adults.
Implications for Research and Practice
The findings of this study have important implications for both research and practice. From a research perspective, the innovative model presented in this study highlights the need for further investigation into the complex interchange between psychosocial factors and physical health outcomes. Future research should aim to replicate and extend these findings in diverse populations and cultural contexts, as well as explore additional mediating and moderating factors that may influence the relationship between loneliness and chronic diseases.
In terms of practice, the results underscore the importance of targeting loneliness, depression, and self-perceived health as key points of intervention to promote healthy aging and prevent chronic diseases. Healthcare professionals and policymakers should prioritize the development and implementation of evidence-based interventions that focus on enhancing social support, promoting social engagement, and providing mental health resources, particularly for older adults who may be more vulnerable to the negative consequences of loneliness (Briguglio et al., 2020; Shah et al., 2020). By addressing loneliness and its associated health risks, we can work towards improving the overall well-being and quality of life of older adults, ultimately contributing to the promotion of successful aging.
Limitations and Future Research
Despite the significant findings, this study has some limitations that should be addressed in future research. First, the cross-sectional design of the study impedes causal inferences, and longitudinal studies are needed to confirm the direction of the relationships between loneliness, depression, self-perceived health, and chronic diseases. Second, the limitation of the current study is the reliance on a single-item measure to assess self-perceived health. While this approach is common in large-scale surveys like SHARE and has been validated in previous research, it may not fully capture the multidimensional nature of individuals' health perceptions. Future studies could benefit from employing multi-item scales to provide a more comprehensive assessment of self-perceived health. Additionally, incorporating objective health measures, such as biomarkers or physician assessments, could complement self-report data and strengthen the robustness of the findings. Finally, the study was conducted in Israel, and the generalizability of the results to other cultural contexts should be explored in future research. Despite these limitations, the present study contributes valuable insights into the complex relationships between loneliness, mental health, and physical health among older adults in Israel, providing a foundation for future research to build upon using more comprehensive health assessments.
Conclusions
The study provides evidence for the pathway from loneliness to chronic diseases, mediated by depression and self-perceived health, and moderated by age among older adults in Israel. The findings suggest that loneliness leads to an increased risk of developing chronic diseases through its impact on depression and self-perceived health. Moreover, the study highlights the importance of considering age-related differences in the consequences of loneliness. The innovative model presented in this research contributes to a more comprehensive understanding of the complex relationships between psychosocial factors and physical health outcomes, highlighting the need for targeted interventions to address loneliness and its associated health risks in life.
Footnotes
Author Contributions
All authors contributed equally to the production of this manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
Data Availability Statement
The analyzed data will be made available to requesting researchers upon a reasonable request
