Abstract
Background
Individuals with psychosis are at risk for adverse sexual and reproductive health (SRH) experiences, and for receiving suboptimal SRH care. Early psychosis intervention (EPI) programs offer an opportunity to address SRH early in the illness course, yet SRH is not currently part of routine EPI care. This project sought to develop a SRH module for women, transgender, and gender-diverse individuals for delivery within EPI care.
Methods
To develop the SRH module, an integrated knowledge translation frame was used, informed by a community-based participatory action research approach. A working group was formed of diverse Youth Advisors (n = 3) and a Youth Engagement Specialist (n = 1) with lived experience with early psychosis, SRH experts (n = 3), mental health experts (n = 3), and research staff (n = 1). The working group met approximately biweekly to co-develop the module (January–October 2023). The module was formatted based on the NAVIGATE model of coordinated specialty care, and was informed by prior research on SRH and working group members’ lived and clinical experiences.
Results
The working group developed an interactive module covering five topics: (1) relationships, (2) sexual health, (3) reproductive health, (4) sexual orientation and gender identity, and (5) interpersonal violence. For each topic, client-facing materials (check-in questions, potential topics, worksheets) and clinician-facing materials (goals, handouts, suggested agendas, teaching strategies, tips for common challenges, evaluating gains and therapeutic goals, specific techniques, probes) were developed. SRH and mental health experts brought evidence-based content, and youth brought an affirming and youth-friendly lens to language and content.
Conclusion
The developed module covers a broad array of SRH topics important to youth. If implementation is successful, the module could improve SRH-related well-being and outcomes for women, transgender, and gender-diverse youth with psychosis. Including youth with lived experience as collaborators enhanced inclusivity and relevance.
Plain Language Summary Title
Addressing sexual and reproductive health for youth with early psychosis: description of a collaborative process to build a care module
Introduction
Sexual and reproductive health are important aspects of overall health and wellbeing, with wide-ranging needs and experiences across the lifespan. Psychosis impacts many aspects of sexual and reproductive health1,2; individuals with psychosis are at higher risk for negative reproductive outcomes, 3 sexually transmitted infections (STIs),4,5 sexual trauma, 6 sexual dysfunction, and relationship challenges.1,2,7 Psychotic disorders often have their onset during adolescence and early adulthood, 8 and youth with psychosis are at risk for STIs, higher-risk behaviours (e.g., inconsistent condom use), and sexual and relationship dysfunction.9–14 These negative sexual and reproductive health outcomes arise from an interplay of factors including the psychotic illness itself (e.g., impulsivity during acute psychosis, social cognition challenges), its treatments (e.g., antipsychotic-related sexual dysfunction), vulnerability to interpersonal violence (both prior to and after the onset of psychosis), comorbidities, stigma, and intersecting social determinants of health.1,15–17
Youth with psychosis are at risk of having inadequate sexual and reproductive health information and not receiving needed sexual and reproductive care,1,13,18,19 further setting them up for negative sexual and reproductive health outcomes. Youth with psychosis can face barriers when accessing general sexual and reproductive health services (e.g., mistrust of providers, diagnostic overshadowing leading to sexual and reproductive health being ignored) and may face additional barriers to accessing sexual and reproductive health information (e.g., psychosis may disrupt social support networks, which are frequent source of sexual and reproductive health information). 19 Previously developed sexual and reproductive health interventions for individuals with psychosis have generally not been youth-focused,20,21 meaning there is a gap for this population. Early psychosis intervention (EPI) programs offer comprehensive team-based care designed to improve functional outcomes for youth with psychosis. 22 EPI programs are typically offered for 2–5 years, and during that time clients see their EPI team more often than other providers (e.g., than their primary care provider). EPI programs do not usually include sexual and reproductive health as part of standard care, thereby missing an opportunity for early intervention.
In planning for the development of a new intervention in this area, members of our research team completed a set of qualitative studies that identified many unique sexual and reproductive health and healthcare needs of women, transgender and gender-diverse (TGD) youth with psychosis, and barriers they face to care.15,16,19 We chose to focus specifically on the needs of women, transgender, and non-binary youth as we expected there to be distinct considerations for those assigned female at birth (e.g., pregnancy) and related to gender (e.g., increased risk of sexual violence 23 ). Results of this qualitative research highlighted the importance of sexual and reproductive health for this population, the multitude in ways in psychosis impacts sexual and reproductive health (e.g., negative impacts on relationships, changes in sex drive, considerations for pregnancy planning), the barriers in access to sexual and reproductive health services faced by youth with psychosis, and the infrequency with which sexual and reproductive health was addressed in EPI care.15,16,19 Based on this research, in partnership with youth with lived experience of psychosis and clinicians with expertise in sexual and reproductive health and early psychosis, we developed a structured evidence-based sexual and reproductive health module. The module was based on NAVIGATE, a standardized, team-based program EPI model that is used widely. 24 Specifically, the module was based on NAVIGATE's ‘Individual Resiliency Training (IRT)’, 25 a manualized program that uses a strengths-based approach to help clients progress towards their individual recovery goals and improve their overall well-being. IRT includes clinician-facing guidelines (e.g., goals, suggested agendas, teaching strategies, tips for common challenges, evaluating gains, and therapeutic goals, specific techniques, and probes) and individual-facing hand-outs (e.g., educational materials, exercises) focused on helping clients achieve their individual goals. IRT covers diverse topics relevant to youth with early psychosis (e.g., relapse prevention, nutrition and exercise, substance use), but not sexual and reproductive health. NAVIGATE IRT was chosen as the model because the format lends itself well to a sexual and reproductive health focus and is used internationally, which could facilitate later widespread implementation of a sexual and reproductive module. Given that sexual and reproductive health needs differ by sex and gender, this first module was tailored for the needs of women (including cisgender and transgender women) and TGD individuals. The aim of this manuscript is to describe the development process for the module.
Methods
Project Design and Framework
The overall goal was to develop a sexual and reproductive health module that addresses the needs of women and TGD youth with early psychosis that could be delivered within an EPI context. Based on our prior qualitative work, sexual and reproductive health was defined broadly (e.g., including relationships). 15 To build a module that would meet the needs of youth with psychosis and their clinicians, an integrated knowledge translation framework was chosen, with collaboration between researchers and those impacted by the research (i.e., youth with psychosis and clinicians) as central to the module development process. 26 Central engagement of knowledge users, including service users can increase credibility and applicability of interventions.27,28 The approach was informed by community-based participatory action research, in particular the concepts of co-design, iterative processes, attention to power dynamics between researchers and knowledge users, and social justice.26,29,30
Setting
The project took place at the Centre for Addiction and Mental Health (CAMH), a psychiatric teaching hospital located in Toronto, Ontario. CAMH has a robust EPI clinical and research program, and houses the Slaight Family Centre for Youth in Transition, an outpatient EPI program that follows the manualized NAVIGATE program, 25 and a dedicated Youth Engagement Initiative. 31 The project was done in partnership with two community organizations, the Canadian Mental Health Association-Toronto, which houses a community-based EPI program, and Planned Parenthood Toronto, which provides community-based sexual and reproductive health care and education, and in collaboration with sexual and reproductive health experts from Women's College Hospital (WCH), an outpatient teaching hospital located in Toronto, Ontario. WCH houses several sexual and reproductive health programs including the Reproductive Life Stages Program (reproductive mental health), the Bay Centre for Birth Control, and the Sexual Assault and Domestic Care Centre.
Working Group Formation
To co-create the sexual and reproductive health module, a working group was formed. The group was led by a psychiatrist with clinical and research expertise in reproductive mental health from WCH, and consisted of 10 additional members: one Youth Engagement Specialist (YES) and three Youth Advisors (YAs) with lived experience of early psychosis; three sexual and reproductive health experts (two family physicians with clinical and research expertise from WCH and one expert from Planned Parenthood-Toronto); one mental health clinician (registered nurse) who delivers NAVIGATE-based early psychosis care at CAMH; one psychiatry resident; and one research analyst. YAs/YESs were already actively involved in shaping early psychosis care at CAMH's Youth Engagement Initiative, and were selected based on (a) identifying as a woman and/or TGD individual, (b) lived experience of psychosis, and (c) an interest in sexual and reproductive health. The YES joined the research team first, then recruited and acted as a mentor for the YAs for the project. The YES and YAs were compensated for their time on an hourly basis (including any time spent reviewing materials outside of the meetings), and other members were not directly compensated outside of their usual occupation roles. All working group members signed a project agreement form that outlined the project and expectations (e.g., respecting confidentiality of other group members, ability to withdraw from the project at any time).
Working Group Initial Processes
While the overall working group approach was to be determined by the working group itself, a plan was made a priori for the first working group tasks. Working group terms and values were to be discussed and agreed upon during this initial meeting. In keeping with the patient engagement literature, emphasis was placed on establishing terms that foster mutually respectful and reciprocal relationships, delineate expectations for group members, and incorporate flexibility for iterative feedback. 32 The working group lead presented the results, values, and preliminary recommendations from the prior qualitative study which predated this project.15,16,19 We discussed the NAVIGATE model. We discussed the initial module goals: (1) create a sexual and reproductive health module designed to address the needs of women and TGD people, (2) ensure the module follows the NAVIGATE framework, and (3) obtain input from interest holders to optimize the module for this population. We solicited opinions on group values, initially proposing inclusivity, intersectionality, patient-centred care, respectful and reciprocal relationships, and privacy with a plan to modify, remove, or add other values deemed to be important by the working group. Finally, we discussed meeting frequency and length (bi-weekly meetings for 1–2 h were proposed, to be modified at the group's discretion).
Data Collection
Formal data collection was not planned for the module-building process. Instead, detailed minutes were kept from each meeting (meetings were audio recorded to facilitate detailed minutes).
Analysis
Given the nature of the study, formal analyses were not planned and no formal analytic technique was used. Instead, working group detailed minutes and other module development-related documents (e.g., module, etc.) were reviewed in detail by LCB; she took notes on the module-building process (e.g., how personal experiences were shared, how the group interacted) and these were used to guide the description of the module development process. All working group members were invited to review the final manuscript for accuracy.
Reflexivity
Our working group (including clinicians, researchers, and individuals with lived experience) was comprised primarily of cisgender women, with some diversity with respect to gender (including cisgender men and transgender representation). There was some diversity with respect to sexual orientation (including heterosexual, bisexual, and questioning individuals) and race/ethnicity (including white, Asian-Canadian, Latina/é, and mixed race individuals). The working group included multiple members with lived experience of psychosis. Clinician members were motivated to participate due to the gaps they had noted in clinical care for this population, researcher members were motivated by wanting to create systems of care that included and centred clients voices, and service user members were motivated to participate from a place of healing, and wanting to advocate for compassionate care for others (which they themselves had often not received). Individuals brought their own personal and clinical experiences to the project, which led to focuses on trauma-informed care, inclusive and intersectionality-informed care, and the importance of respect and destigmatization. Additional study team members who did not participate in the working group brought varied lenses including additional clinical expertise and research expertise which shaped the study and module design (e.g., using a scalable NAVIGATE IRT model).
Results
Module Building
The module was built from January to October 2023. During this time, the working group met approximately biweekly for two-hour virtual meetings. Research staff ensured at least one YA or YES, one sexual and reproductive health expert, and one mental health expert (mental health clinician, psychiatrist, psychiatry resident) attended each meeting, in addition to at least one member of the core research team (research lead, research analyst, or psychiatry resident). One YA left their CAMH role partway through the process and was not replaced to maintain group cohesion; the other two YAs, the YES, and all other working group members were consistent throughout the process.
During the first working group session, members introduced themselves and the research lead/analyst presented an overview of the project, including the NAVIGATE program and existing IRT modules, and current project goals. Group values and expectations were also established; group members agreed upon the proposed values of inclusivity, intersectionality, patient-centred care, respectful and reciprocal relationships, and privacy, and added laughter, active listening, continuous mutual learning, sex-positivity, destigmatization, and supporting client goals to the working group values. The group also decided upon the following group expectations: acting in line with values, accountability, and respecting different ways of participating.
Within subsequent meetings, members collaboratively defined goals, and created and edited content. Informed by the prior qualitative research conducted by members of the team15,16,19 and lived and clinical/research expertise of working group members, the group decided to address five topics: (1) relationships, (2) sexual health, (3) reproductive health, (4) sexual orientation and gender identity, and (5) interpersonal violence (Figure 1). During meetings, working group members brainstormed the goals and worksheets for each topic. Between meetings, the research analyst and group lead drafted clinician-facing and individual/client-facing guidelines based on the structure of previous NAVIGATE IRT modules. Drafted guidelines were presented to the group for iterative feedback and collaborative edits. After each topic was completed, optional one-hour meetings were held to review the clinician and individual guidelines (working group members also had the option to review on their own). After 10 months of working group meetings, the group had developed a complete Sexual and Reproductive Health Module draft. The module was sent to the broader research team for feedback; no major revisions were made at this stage.
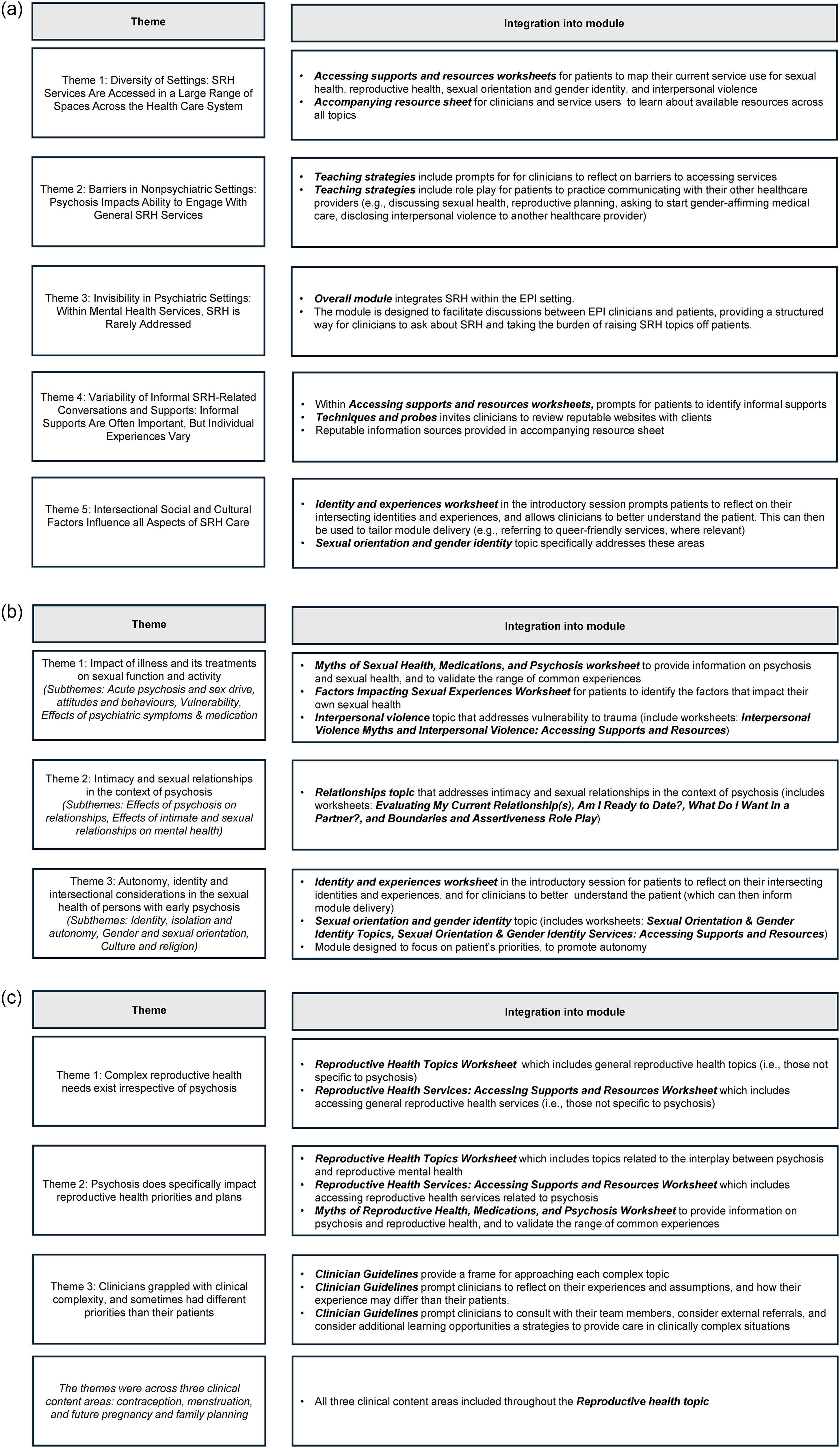
Final Module
The final module consists of an introductory session and five topics: (1) relationships, (2) sexual health, (3) reproductive health, (4) sexual orientation and gender identity, and (5) interpersonal violence (subtopics in Figure 2). The introductory session consists of an exploration of intersecting experiences and identities (to be able to tailor module delivery accordingly) and an overview of the module. During the introductory session, the individual reviews the topics and subtopics (Figure 2), selecting those that they would like to cover during the module (selections can be revisited at any point). Then, the clinician and individual can proceed with the selected topics in the order that best meets the individual's needs. Following the NAVIGATE IRT model, for each topic, clinician-facing materials consist of an overview, goals, handouts, suggested agenda, teaching strategies, tips for common challenges, approaches for evaluating gains, and a section on therapeutic goals, specific techniques, and probes. Similarly, for each topic, individual-facing materials consist of an overview, check-in questions, potential topics to discuss with their clinician, and worksheets. Examples of worksheets include role plays, fact sheets that dispel common myths, and tools to help identify and access needed resources. The materials were designed for delivery across approximately 3 to 17 clinical sessions (1–2 sessions for the introductory section and 0–3 sessions per topic). The final module was designed to facilitate improvement across a range of short-, medium-, and long-term outcomes (logic model in Figure 3).
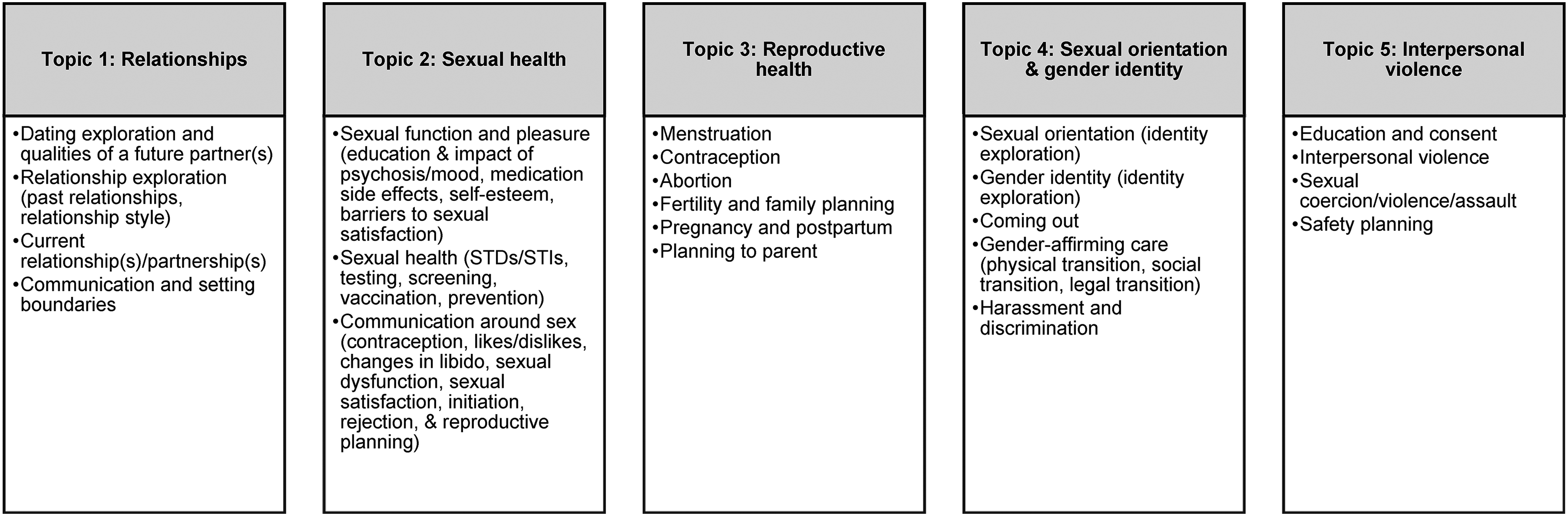
Topics and subtopics covered in the module.
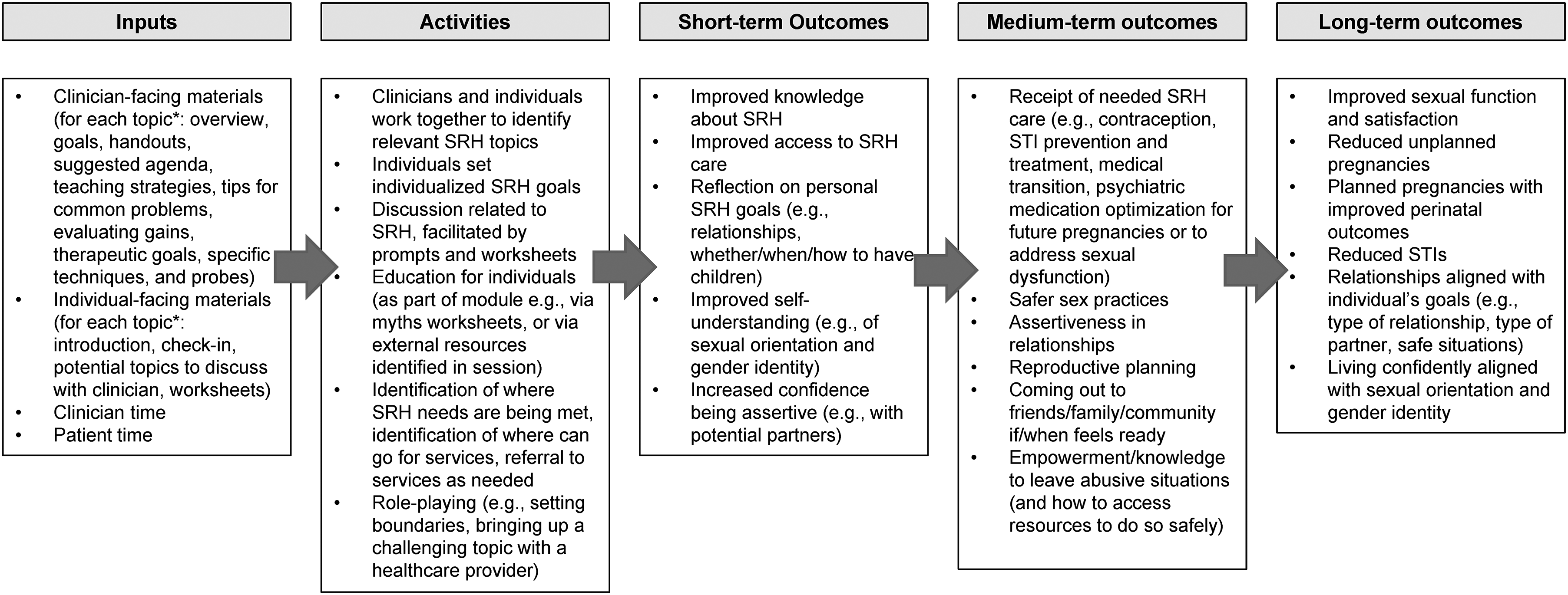
Logic model of how final module is expected to impact sexual and reproductive health outcomes.
Reflection on the Development Process
Reflections on the development process are described using review of detailed minutes. Minutes revealed that the longitudinal working group format allowed for a highly interactive process, with room for discussion, critique, and iterative change. Module content, format, and language were discussed among group members, and decisions were typically made by informal consensus. YA and YES members shared relevant personal experiences that were used to shape the module. Different topics were more relevant to some YA/YES members than others, and individuals typically provided the most feedback on topics that resonated most with their own experiences. YA and YES members brought an affirming and youth-friendly lens to language and content that reevaluated existing clinical and societal norms. For example, the module was designed to be relevant across relationship structures (e.g., monogamy, polyamory, etc.) and language aimed to be inclusive across sexual orientation and gender identities. YA and YES members flagged areas that could be distressing for some service users which led to change (e.g., changing the mention of alcohol in a scenario to a more neutral example).
Clinicians/experts shared relevant professional experiences and information from the medical literature. There was discussion amongst group members of how to present evidence-based information from the literature in a non-stigmatizing fashion (e.g., data related to the heritability of psychotic disorders). Members flagged areas where clinicians may not feel equipped or comfortable delivering content. Strategies that the group came up with to mitigate this included: (1) prompts for clinicians to examine their own experiences, assumptions, and biases; (2) prompts for clinicians to reflect on gaps in knowledge and pursue additional learning/skill-building opportunities or consult with their team members; (3) stating in both clinician- and individual-facing materials that the clinician (whose expertise is in psychosis) may not be an expert in sexual and reproductive health, and that referral to other services for sexual and reproductive health information and healthcare could be part of the care plan; (4) including glossaries of terms; and (5) preparing an accompanying resource sheet that clinicians can use when delivering the module.
Discussion
Through an iterative co-design process, a novel sexual and reproductive health module was created for women and TGD youth with early psychosis. The developed module covers five topics relevant to youth: (1) relationships, (2) sexual health, (3) reproductive health, (4) sexual orientation and gender identity, and (5) interpersonal violence. The co-design process allowed youth and clinician/expert experiences and perspectives to be incorporated into the module, ultimately enhancing inclusivity and relevance.
Prior interventions for sexual and reproductive health for those with severe mental illness have generally been designed for adult populations,20,21,33,34 and have not been youth-focused with few exceptions.35,36 Many of these interventions focused specifically on HIV risk reduction; while some have expanded scope to also include other sexual health topics and relationships.20,21,33,34 However, none to our knowledge have covered such a broad array of topics as our new module. With respect to format, many – though not all – prior interventions have been group-based and education-focused, with some also including more interactive components such as role-playing.1,20,33–35 The most similar intervention to ours is likely from the Randomised Evaluation of Sexual health Promotion Effectiveness informing Care and Treatment (RESPECT) study, an individually-delivered, manualized intervention that focused on knowledge, motivation, and behavioural intentions related to sexual health (including safer sex, contraception, and relationships) designed for adults with serious mental illness. 21 The intervention in RESPECT was also designed with extensive consultation with interest holders including those with lived experience, which likely contributed to similarities between their and our interventions. Differences between prior and our current intervention likely reflect our focus and process. For example, we were focused on youth and on women and TGD individuals, which guided topic selection (e.g., reproductive health, sexual orientation and gender identity, and interpersonal violence were all relevant topics). Modelling it after NAVIGATE IRT meant that it was designed for individual delivery, with patient- and clinician-facing materials. Our working group process, which involved extensive discussion and iterative revision, helped ensure that diverse lived experience, clinician, and expert perspectives were incorporated.
The community-based participatory approach facilitated a highly engaged process, with extensive dialogue between researchers, clinicians, and youth with lived experience.26,29 The social justice 30 orientation manifested both in the overall module goal (to reduce health disparities for women and TGD youth with early psychosis) and in the module's structure, content, and process (e.g., prompts for clinicians to reflect on how their own experiences and identities may inform their beliefs, prior to delivering content). Such processes can be applied in the development of other interventions for youth with psychosis to enhance inclusivity and relevance to diverse youth.
The module development process had several notable strengths. It involved an extensive co-design approach with youth with lived experience and clinicians/experts from diverse personal and professional backgrounds. It was based on an established evidence-based model (NAVIGATE IRT 25 ) and supported by existing evidence, including qualitative research conducted by members of the current project team that laid the groundwork for this module.15,16,19 The module is designed to be delivered in a collaborative manner by an existing care provider, an approach that is supported by the qualitative literature. 37 The main limitation of the current manuscript is that no formal module evaluation has yet been completed; an evaluation of feasibility is currently underway, with plans for a future effectiveness trial to evaluate the module's impacts on client knowledge, attitudes, and behaviours (e.g., seeking sexual and reproductive healthcare, practicing safer sex). Given that mental health clinicians often express discomfort with sexual and reproductive health topics, we will be incorporating a clinician training protocol and evaluating this as part of the project.38–41 If the module proves to be feasible and effective in follow-up research, it can be scaled up within EPI programs to improve sexual and reproductive health outcomes for a currently underserved group. A major limitation is that a formal evaluation of the co-creation process was not completed. Despite the lack of formal evaluation, we aimed for rigour by basing the description on a detailed review of minutes (as opposed to one individual's experience) and by offering all working group members the opportunity to review the full manuscript to confirm accuracy. In future such projects, more formal process evaluations can be considered (e.g., formal document review using qualitative methods, using independent raters). While our focus on the diverse needs of women and TGD is a strength, the needs of men and those assigned male at birth are not specifically considered. As men and those assigned male at birth make up a majority of EPI service users, 42 we are actively planning to adapt the sexual and reproductive health module for this population. Not all religious and cultural groups were represented in co-design process, and the evaluation will examine how the module addresses the needs of diverse service users. While the working group endeavoured to make the module inclusive, as understandings of social justice and language evolve over time, we expect that the module will need to be updated to reflect new best practices. Similarly, as evidence related to sexual and reproductive health evolves over time, materials will need to be updated.
In conclusion, through a highly engaged, iterative co-design process, we developed a novel sexual and reproductive health module for women and TGD youth with psychosis that can be implemented within EPI settings. If the module proves to be feasible and effective in follow-up research, it can be scaled up within EPI programs to improve sexual and reproductive health outcomes for a currently underserved group.
Footnotes
Acknowledgments
The authors thank Tallan Alexander and Erin Butler.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: RD reports honoraria from Merck, Searchlight, and Bayer. ANV currently receives grant funding from the National Institute of Mental Health, Canadian Institutes of Health Research, Canada Foundation for Innovation, CAMH Foundation, the University of Toronto, Brain Canada, and Wellcome Trust. SNV reports royalties from UpToDate Inc for authorship of materials related to depression and pregnancy.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by a womenmind grant from the Centre for Addiction and Mental Health. LCB is supported by an Academic Scholar Award provided by the Department of Psychiatry, University of Toronto and a PSI Graham Farquharson Knowledge Translation (KT) Fellowship. JSHL is supported by an Academic Scholar Award provided by the Department of Psychiatry, University of Toronto and the O'Brien Scholar program.
