Abstract

Introduction
The association between urbanicity and an increased risk of developing schizophrenia has been replicated in many jurisdictions; however, the mechanisms underlying this association are not clear. There has been increasing interest in the study of novel environmental risk factors. 1 A recent population-based study in Denmark found that cumulative childhood exposure to green space is a protective factor that reduces the risk of developing schizophrenia during adolescence and adulthood. 2 These findings have yet to be replicated, nor have they been assessed solely in the context of an urban environment. This study explores the association between green space and the incidence of schizophrenia in a large Canadian urban center, while adjusting for known socioenvironmental risk factors.
Methods
We used a subset of a population-based cohort of people between the ages of 14 and 40 years residing in one of the 140 Toronto neighbourhoods (identified by six-digit postal code), who were followed over 10 years (1999–2009). Details on the larger cohort and data sources are described elsewhere.3,4 The primary outcome was incident cases of schizophrenia or schizoaffective disorder identified from administrative health data using a validated algorithm. Considering this was an incidence cohort, we removed all prevalent cases which were identified based on any previous contact with the provincial health system for a psychotic disorder up to 10 years prior to the cohort inception. A composite measure of marginalization and green space quintiles at the neighbourhood level was identified based on the Ontario Marginalization Index and the Urban HEART, 5 respectively. The Urban HEART measure of neighbourhood-level green space is based on the calculation of the average amount of green space per km2 in a 1 km circular buffer from each residential block in the neighbourhood based on geospatial data of all public parks and green spaces in the city obtained from Open Data Toronto. We calculated adjusted incidence rate ratio (IRR) estimates using multilevel Poisson regression models adjusting for age, sex, neighbourhood-level marginalization, and neighbourhood-level green space. The 140 neighbourhoods were fit as a random intercept to account for variability across neighbourhoods. Model fit was compared to an intercept-only model based on Bayesian information criterion values. Results are presented as IRRs with associated 95% confidence intervals and are considered to be significant when the 95% CI does not cross unity. All analyses were performed using Stata version 13. This study received research ethics approval from the Centre for Addiction and Mental Health.
Results
We identified 4,841 cases in a cohort of 649,020 people. The baseline characteristics of the cohort are presented elsewhere. 3
Exposure to the lowest amounts of green space was associated with a higher risk of developing schizophrenia independent of age, sex, and neighbourhood-level marginalization (Table 1). People residing in neighbourhoods with the lowest amount of green space had a 24% higher risk of developing schizophrenia (Q1 adjusted IRR = 1.24, 95% QI 1.06, 1.45), compared to people residing in neighbourhoods with the highest amount of green space (Q5), after adjusting for age, sex, and neighbourhood-level marginalization. The risk of developing schizophrenia was not elevated in areas with intermediate levels of green space (Q2–Q4).
Multilevel Poisson Model with Incidence Rate Ratio Estimates of Schizophrenia in Toronto, Canada Accounting for Age, Sex, Marginalization and Green Space.
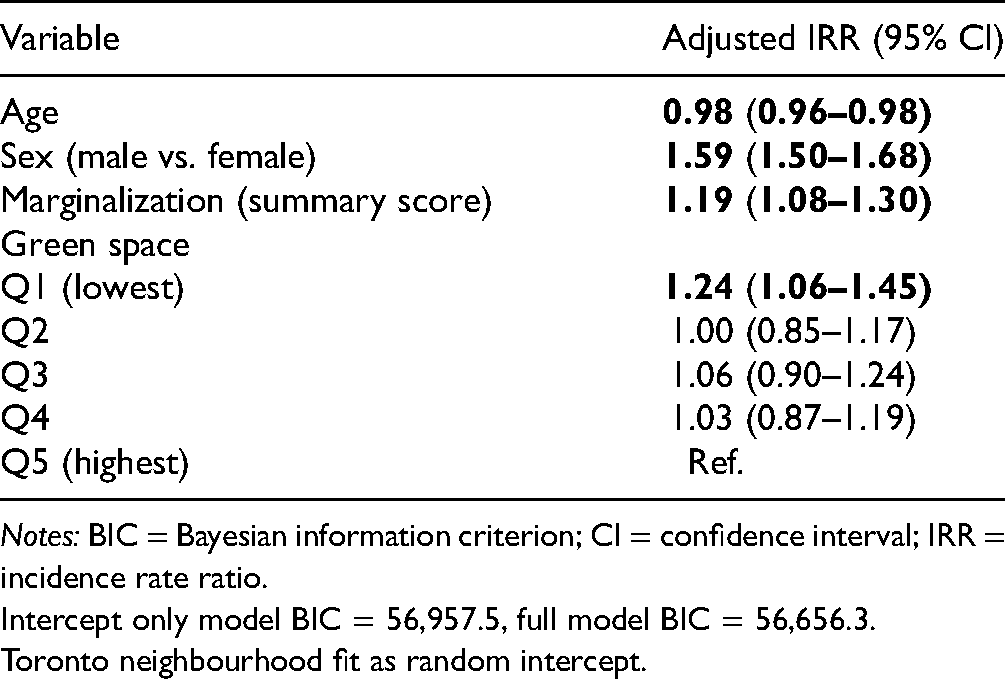
Notes: BIC = Bayesian information criterion; CI = confidence interval; IRR = incidence rate ratio.
Intercept only model BIC = 56,957.5, full model BIC = 56,656.3.
Toronto neighbourhood fit as random intercept.
Discussion
We found that residing in an area with the lowest amount of green space was associated with an increased risk of developing schizophrenia, independent of other sociodemographic and socioenvironmental factors. These findings are consistent with a study from Denmark that examined this association across the entire country, finding a 52% higher risk of psychotic disorder among people exposed to the lowest amounts of green space during childhood. 2 The current study builds on this international work, as we found a similar albeit modest association to be present in a diverse urban city in Canada. These findings contribute to a growing evidence base that environmental factors may play a role in the etiology of schizophrenia. The underlying mechanism at play is unknown and requires further study. It has been hypothesized that green space may reduce exposure to air pollution and noise and also increase opportunities to engage in outdoor activities for stress reduction. 2
Our findings are limited by the fact that exposure is defined at the time of cohort entry, and we are unable to account for changes in exposure over the course of the follow-up period, as well as lifetime green space exposure. Moreover, data on other potentially important confounding factors including a family history of mental illness and substance use were not available. Although these data are getting older, it is unlikely that the level of green space in Toronto has changed significantly, and further replication is warranted.
Future studies should build on the initial associations we have described and further examine how people's access and engagement with both natural (i.e., green space, blue space – which include areas with marine, coastal or inland water) and built environments (i.e., access to natural environments, walkability), as well as other environmental factors (i.e., air pollution), impacts the risk of developing schizophrenia and other psychoses. 1 Specific focus on the potential underlying mechanisms which may be at play which may relate to opportunities for stress reduction and exposure to different forms of pollution is also warranted. The role of these factors could also be further examined in the context of prevention strategies.
Footnotes
Acknowledgements
This study contracted ICES Data & Analytic Services (DAS) and used de-identified data from the ICES Data Repository, which is managed by ICES with support from its funders and partners: Canada's Strategy for Patient-Oriented Research (SPOR), the Ontario SPOR Support Unit, the Canadian Institutes of Health Research and the Government of Ontario. This study was supported through provision of data by ICES and Cancer Care Ontario (CCO) and through funding support to ICES from an annual grant by the Ministry of Health and Long-Term Care (MOHLTC) and the Ontario Institute for Cancer Research (OICR). The opinions, results and conclusions reported in this paper are those of the authors. No endorsement by ICES or any of its funders or partners is intended or should be inferred. Parts of this material are based on data and information compiled and provided by CIHI. However, the analyses, conclusions, opinions and statements expressed herein are those of the author, and not necessarily those of CIHI.
Data Access
The dataset is held at ICES and may be accessible with appropriate permission via a DAS data request. The Urban HEART Toronto is accessible online via http://www.torontohealthprofiles.ca/urbanheartattoronto.php. The Ontario Marginalization Index is accessible online via: ![]() .
.
Authors’ Note
This study was approved by the Centre for Addiction and Mental Health's research ethics board.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
