Abstract
We reported a case of an 11-year-old girl admitted to our hospital for goiter, tachycardia, sweating, and visible and palpable thyroid. Thyroid function tests revealed a low thyrotropin level (<0.004 mIU/L) and elevated free thyroxine level (3.4 ng/ dL) diagnosed with Graves’ disease and treated with methimazole. This anti-thyroid drug is recommended as first-line treatment in children with Graves’ disease because it produces minor adverse effects with respect to propylthiouracil. She developed a lateralized exanthem mimicking figurate inflammatory dermatosis of infancy after methimazole therapy. The symptoms resolved after discontinuation of methimazole and treatment with an antihistamine and a corticosteroid. Furthermore, the treatment was changed to propylthiouracil without any adverse effects. According to current literature this is the first case of cutaneous figurate erythema related to methimazole, different from other well-known reactions such as skin eruption or urticaria.
Introduction
Anti-thyroid drugs (ATDs) are usually recommended as the initial treatment in children and adolescents for various hyperthyroid conditions, especially for Graves’ disease (GD). The most commonly used ATDs are thionamides: methimazole (MMI) and propylthiouracil (PTU).1,2
The two drugs partially differ in molecular structure and certain aspects of clinical pharmacology, with implications in routine practice. MMI is usually preferred over PTU because it reverses hyperthyroidism more quickly and has fewer side effects than PTU. Due to its better safety profile, MMI represents at present the treatment of choice for GD, which is the most common cause of hyperthyroidism in the pediatric population.1,2 Additionally, this drug is effective when given once daily, thus improving patient’s adherence. 3
Another key point is that safety information related to anti-thyroid treatment in the pediatric population is often extrapolated from data in adults. Moreover, several reports regarding children with GD involved cohorts of patients treated with PTU. Only recently, few observational studies described comparative results between treatments with MMI or PTU for children and adolescents with GD.4,5 As MMI has become the first-line therapy in children and adolescents, efforts should be taken to improve the knowledge about safety of this medicine during pediatric use.
ATDs are generally considered safe and well tolerated. As reported by early investigators, minor adverse reactions of ATDs are encountered in 4–6% of treated patients. Minor side effects encompass itching, rash, hives, joint pain and swelling, fever, altered taste sensation, nausea, and vomiting. Moreover, they could rarely cause serious adverse reactions, of which hematopoietic organ toxicity is particularly well known. Other major rare side effects, including drug-induced hepatitis and antibody-positive related vasculitis, are more commonly observed with PTU than with MMI treatment. 1 Cutaneous toxicity from ATDs is a little-known complication and its management remains to be determined, in particular in pediatric patients. Dermatological adverse events such as maculopapular rashes, skin hyperpigmentation, urticaria, exfoliative dermatitis, and toxic epidermal necrolysis have been reported in the literature with MMI use. 1
Here we present the first case of an erythema annulare mimicking a figurate inflammatory dermatosis of infancy in an 11-year-old girl with GD treated with MMI.
Case report
An 11-year-old girl was admitted to our pediatric department for goiter, tachycardia, and sweating. Physical examination revealed the following findings: bodyweight, 30 kg; height, 141 cm; heart rate, 140 beats per minute; sweat and warm extremities; and visible and palpable thyroid. Laboratory test results revealed: decreased thyroid-stimulating hormone (TSH) <0.005 µIU/mL (normal range, 0.2–4.2 µIU/mL) levels, increased free thyroxine T4 (FT4) 55 pmol/L (normal range, 12–22 pmol/L), elevated thyroid stimulating thyrotrophin receptor antibody (TRAb) 22.4 IU/L (normal range, <2.0 IU/L), and thyroid peroxidase antibody (TPOAb) 549 IU/mL (normal range, 0–34 IU/mL). Hematological and biochemical investigations including liver function tests, antinuclear antibodies, anti-extractable nuclear antigen antibodies, anti-Scl-70 antibodies, and antineutrophil cytoplasmic antibodies gave normal results. Microbiological evaluations for bacterial and viral infections (adenovirus, cytomegalovirus, Epstein-Barr virus, herpes virus, parvovirus, toxoplasma, tuberculosis, Borrelia burgdorferi, staphylococcus, and Group A streptococcus) were negative. These included blood culture, urine culture, throat and nasopharyngeal culture, and serological tests. The ultrasound images of thyroid showed enlarged lobes (4.5 cm), some degree of inhomogeneity was also present, and color Doppler revealed markedly increased vascularity throughout the thyroid gland parenchyma.
She was diagnosed with GD and treated with MMI at 0.7 mg/kg daily given in three divided doses. Fifteen days after MMI initiation, a generalized itching erythematous rash developed on her legs, arms, and body. The rash, characterized by erythematous annular and polycyclic lesions with central clearing (Figure 1), had begun in his lateral thoracic wall and spread centrifugally along his left axilla. The trunk had been the first involved site, but subsequently new lesions had appeared on the limbs and thereafter spread over the body (then root of the arm, extending to the whole limb, and successively involved the root of the leg.). A skin biopsy showed non-specific findings consisting of a mild perivascular and interstitial inflammatory infiltrate of lymphocytes and neutrophils (Figure 2) Desquamation and vesicles were absent. MMI was discontinued and betamethasone (0.1 mg/Kg) twice a day and cetirizine (10 mg) 15 drops daily were started. Erythema disappeared gradually after MMI withdrawal and 5 days of corticosteroid and antihistamine therapy. Because of the development of the rash, MMI therapy was switched to propylthiouracil 150 mg/daily without side effects. According to the literature and clinical conditions PTU therapy was gradually decreased to 50 mg/daily.
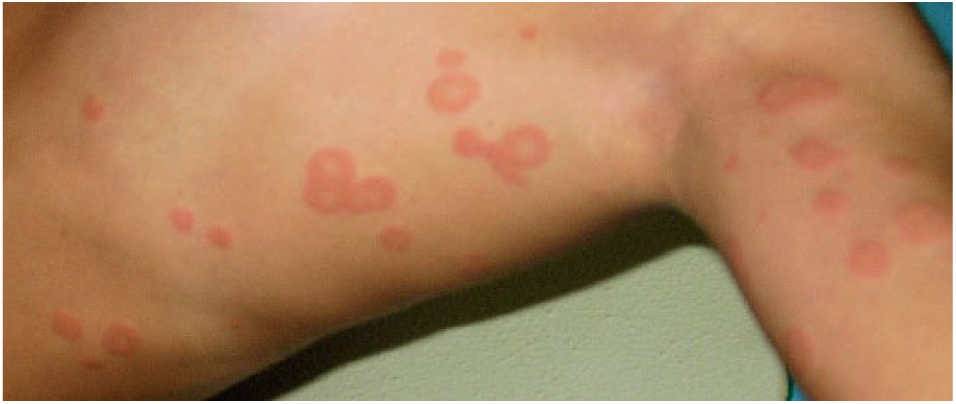
Image of an 11-year-old girl with erythematous, annular, and polycyclic lesions with central clearing without scaling, vesicles, or crusts.

Histopathological examination showing non-specific findings consisting of a mild perivascular and interstitial inflammatory infiltrate with lymphocytes and neutrophils. (Hematoxylin-eosin stain. Original magnification 10×).
A written informed consent for patient information and images to be published in the study was provided by the patient’s parents.
Discussion
Cutaneous manifestations are a key factor in the diagnosis of a drug-related exanthem, but they are usually non-specific and include scarlatiniform, morbilliform and urticarial rashes, and erythema multiforme-like (targetoid) lesions. To our knowledge, this is the first case of an adverse reaction to MMI in which the cutaneous manifestations are exclusively annular lesions with central clearing and erythematous, firm, and raised borders, without scaling, vesicles, or crusts, which mimics figurate inflammatory dermatoses of childhood.
Annular or figurate erythema of infancy includes reactive vascular dermatoses which are characterized by primary lesions with an annular, oval, or polycyclic feature. The diagnosis of these lesions is difficult because only minor differences exist in clinicopathologic symptoms. Annular erythema may be associated with various inflammatory and infectious disorders or with drug hypersensitivity reactions. 6
Figurate inflammatory dermatoses of infancy include: neonatal lupus erythematous, erythema marginatum rheumaticum, erythema chronicum migrans, erythema gyratum atrophicans transiens neonatal, and drug-related exanthems, which are of known etiology, and some dermatoses of unidentified origin (i.e. erythema annulare centrifugum, familial annular erythema, eosinophilic annular erythema, annular erythema of infancy, neutrophilic figurate erythema of infancy). 6
The pathogenesis of annular lesions can be explained with different mechanisms, which also involve an altered immune response, when the reaction is related to a drug. Molecular mimicry has been proposed to explain an autoimmune reaction that occurs simultaneously to or immediately after infections or drug administration. This pathogenic model clarifies the mechanism for autoimmune and reactive skin diseases.7–11 In particular, homologies between microbiological proteins and skin component would cause the activation of autoreactive T-lymphocytes which, together with other important actors of the immune response, contribute to the development of reactive diseases via the molecular mimicry mechanism.7–11
Recently, the lateralized involvement has been explained by the hypothesis that an early postzygotic mutation has rendered the skin on one side of the body more reactive. Furthermore, a superimposed segmental manifestation of a polygenic skin disorder has been demonstrated in many common dermatoses associated with viral infections or drugs.12,13
The lesions on our patient were probably due to MMI administration. This conclusion was based on the examination of the essential criteria to define the case-causality assessment between the drug intake and the appearance of the adverse event, including the time relationship, a response to drug withdrawal plausible (pharmacologically, pathologically), and the exclusion of alternative explanations (i.e. other diseases or other drugs).
In our case, other potential causes of annular erythema, such as metabolic or infective causes, have been ruled out by appropriate laboratory analyses. From a clinical point of view, the temporal association of MMI exposure with adverse effect, clinical improvement soon after discontinuation of MMI, and absence of other concomitant medications or pathological conditions support the hypothesis that the drug played a role in the development of our patient’s cutaneous manifestations. Moreover, Naranjo algorithm evaluation obtained a score of 7, which indicates a high probability that the adverse reaction was due to the drug. 14
To date, the majority of publications related to medical therapy for GD have focused on children treated with PTU. Cohort studies describing adverse events related to MMI are few.
The most common side effects reported in literature from use of MMI include fever, pruritus, and nausea, while less frequent but serious reactions are agranulocytosis and severe arthralgia. Moreover, MMI has been associated with dermatological events and allergic reactions. 2
As regards cutaneous toxicity, the most common reaction associated with MMI is a mild, occasionally purpuric urticarial papular rash. Other minor dermatologic effects, such as rash (unspecified), alopecia, skin hyperpigmentation, urticaria, and pruritus have been observed in approximately 3–5% of patients receiving this drug. To our knowledge, the diagnosis of annular erythema due to ATDs has not been described in the worldwide literature to date.
Severe skin reactions, including exfoliative dermatitis, have been reported with MMI use. Toxic epidermal necrolysis has been also described in a 12-year-old-girl with hyperthyroidism treated with MMI. 15 Various cases of methimazole-induced hypersensitivity syndrome and immunologic side effects were reported, although the precise mechanisms were not elucidated.16–18 An observational clinical study showed that nearly 20% of 100 children treated with MMI developed adverse effects, mainly skin eruptions and arthralgia. Stevens-Johnson syndrome was diagnosed in three of these patients, one of which required hospitalization.19,20
Another study, focusing on hepatic and cutaneous side effects of ATDs, found an increase in the frequency of dermatological reactions in patients taking 30 mg/day MMI as compared to those taking MMI at lower dosages and PTU 300 mg/day. 21 The authors also showed that patients who experienced side effects with an ATD did not have an increased tendency to develop adverse reactions after switching to another medication of the same class.
In our patient, MMI therapy was switched to PTU without reappearance of symptoms. There was no cross-reaction with PTU, which probably reflected the differences in molecular structure between the two medications. There is evidence that cross-reactivity between PTU and MMI mainly occurs for severe side effects, such as agranulocytosis or vasculitis, but not with mild adverse reactions.22,23
In conclusion, the choice of ATDs used to treat hyperthyroidism in children, which results from the autoimmune condition such as GD, is still controversial.4,5 Given that all these compounds have similar efficacy, the optimal choice may depend largely on their safety profile.
We reported the first case of erythema annulare triggered by methimazole in a child with GD. However, it is difficult to assess causality because there are no similar cases reported in the literature. Nevertheless, erythema annulare is rare and clinicians should be aware of the possible association in pediatric patients. More investigations are needed to clarify the pathogenesis of the eruption, which may be either through cytokine imbalance or altered immunity due to several medications.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
