Abstract
Background
Irradiation, which affects cytokine secretion, is used to treat cancer patients. Cytokine levels have correlations to disease parameters, serving as biomarkers for patients. We aim to explore the effect of irradiation on cytokine production both in vitro (using lymphocytes from healthy donors) and in vivo (using serum levels of head and neck cancer patients following irradiation) and correlating them to mucositis severity/need for percutaneous endoscopic gastroscopy (PEG) tube installation.
Methods
Cytokine production by cultured lymphocytes from healthy donors, in vitro, following irradiation of 5 or 10 Gy. In addition, blood from 23 patients with head and neck cancers, irradiated by 60–72G in vivo, were assessed for inflammatory cytokines (tumor necrosis factor (TNF)α, interleukin (IL)-6, IL-8, IL-18), the anti-inflammatory cytokine IL-10, and the general marker sIL-2R. Following radiation, selected patients who were developing mucositis were treated by PEG tube installation. Changes in cytokine levels were studied as predictive biomarkers of response to therapy/PEG tube installation. Cytokine production levels were measured using ELISAs kits.
Results
Irradiation decreased the levels of all tested cytokines, most notably IL-6 and IL-8, proportional to irradiation dose. In patients, increases in cytokine levels, correlated with mucositis severity and potentially the need for PEG tube installation.
Conclusions
Irradiation decreased the levels of all cytokines of healthy lymphocytes in a dose-dependent manner, especially those of IL-6 and IL-8. This study shows a correlation between high and increasing levels of inflammatory cytokines, sIL-2R, plus radiation toxicity and the need for PEG. The reduction of cytokine levels after radiotherapy predicts that PEG will not be required. Thus, our study shows that cytokine changes are predictive biomarkers in head and neck cancer patients.
Introduction
Radiation therapy (RT) is a treatment used for many types of cancer in more than 50% of patients, and its direct effects in reducing cancer cell viability may induce modifications in local microenvironments. RT, and in particular high ionizing radiation (IR) treatments, activate both pro- and anti-proliferative signaling pathways.1–3 IR exposure in response to stress causes tumor cells to modulate their own cytokine secretion and therefore control cancer therapy outcomes.4,5
Cytokines function as indicators of inflammation or disease progression and provide a means of manipulating cellular responses both in vivo and in vitro. In healthy individuals, cytokines are expected to have low or undetectable circulating levels as they are minimally secreted by healthy cells.6–8
However, in diseased states, cytokines have been shown to be elevated. As a result, the ability to detect and evaluate cytokine levels has become increasingly important for both researchers and clinicians alike. Peripheral blood is the most common source of mononuclear cells (PBMC) for in vitro cultures. Purified PBMCs are used to evaluate various sub-classes of cytokines, including their production and roles.6–13 Changes in circulating cytokine levels have been associated with many human diseased states. Patient serum samples are simple to obtain with small amounts being sufficient for a number of cytokine level evaluations. Therefore, evaluating serum cytokines is an efficient approach for monitoring patients and predicting disease severity and response to therapies, such as irradiation.5,14–16 Multiple sub-classes of cytokines, such as pro-inflammatory6,13,14,17–20 and anti-inflammatory cytokines,21,22 have been reported in various diseased states.5,8,10,11 Cytokines are rapidly expressed in response to stimuli such as microbes, viruses, stress, or irradiation.
Cytokines are known to influence the process of cancer initiation, pathogenesis, and the therapeutic outcome of various anti-cancer treatments.4,5 Cytokine levels have a significant correlation to disease parameters and can be used as biomarkers for insight into a patient’s physiological state.4,5 Evaluation of cytokine levels during therapy and throughout clinical follow-ups can be useful in predicting clinical response and potential relapse earlier than other conventional clinical parameters or laboratory tests.
We previously demonstrated that circulating levels of the interleukin (IL)-1 family in hairy cell leukemia (HCL) HCL is correlated to disease activity and response to therapy. 19 We have also documented that interferon levels in breast cancer patients could be correlated to disease stage and response to therapy. 8
We showed also that in melanoma, where patients presenting with or without redness, presented differences in cytokine levels. 10 Pro-inflammatory cytokine levels (tumor necrosis factor (TNF)-α, IL-6, IL-8) are extremely high in autoimmune diseases, such as in primary biliary cirrhosis, 11 graft-versus-host disease or graft rejection, 20 while anti-inflammatory cytokines, such as IL-10, have a protective inhibitory effect on autoimmunity.21–24
Study aims
The primary aim of this study was to assess the role of three groups of cytokine levels as predictive immune biomarkers of response to irradiation in head and neck cancer patients:
Group 1: Inflammatory cytokines (TNF-α, IL-1, IL-6, IL-8, IL-18)
Group 2: The anti-inflammatory cytokine IL-10
Group 3: The general immune activation cytokine sIL-2R.
The secondary aim was to ensure that the results were not only unique to cancer patients but also to the general population, including healthy donors. Therefore, the effects of irradiation on the production of cytokines in those three groups in healthy donors was assessed and compared to those of the cancer patients’ serum levels.
Patients and methods
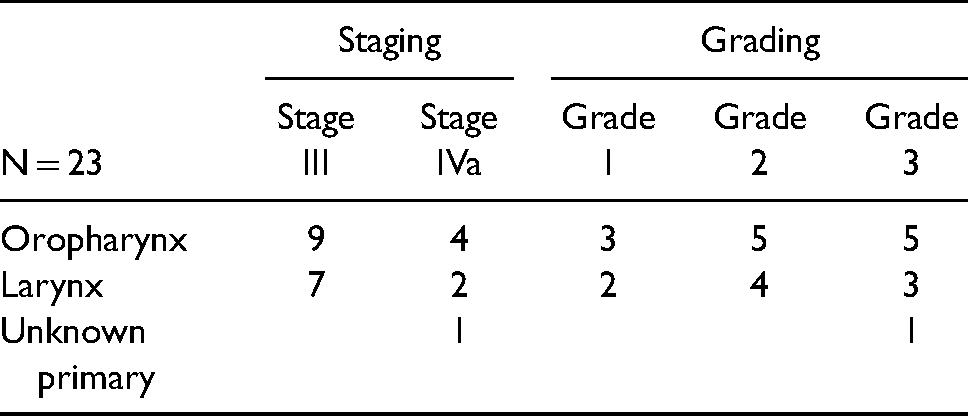
Of the 23 head and neck cancer patients in this study, the primary sites of disease included the oropharynx (13 patients), the larynx (9) and unknown primary cancer of the head and neck (1).
All patients had squamous cell carcinomas (see Table 1 for patient details).
Tumor primary site, staging, and grading of study cohort.
In order to assure that the effect of irradiation is the same in both normal controls and cancer patients, 1 we used blood samples for cytokine production from controls and compared the irradiation effect with that of cancer patients.
We cultured lymphocytes from the blood samples of 10 healthy donors that were used as controls and were then irradiated (5 and 10 Gy)—in vitro evaluation
We obtained blood from 23 patients with head and neck tumors who were treated with radiation therapy (60–72 Gy) using standard protocols. These were assessed for the inflammatory cytokine levels (TNFα, IL-1, IL-6, IL-8, and IL-18), the anti-inflammatory cytokine IL-10, and the general immune activation cytokine sIL-2R—in vivo evaluation.
Following radiotherapy, some patients developed mucositis (the main side effect of irradiation in head and neck cancers) according to the World Health Organization’s common toxicity criteria and percutaneous endoscopic gastroscopy (PEG) tube installation 25 was performed accordingly.
Changes in the cytokine levels of patients during treatment were studied to see if they can be predictive biomarkers for toxicity, leading to PEG tube installation.
Cytokine production8,12 levels were evaluated using ELISA kits (ABBOTT, Wiesbaden, Germany).
Statistical tests were performed using the SPSS statistical package (Chicago, IL, USA). Statistical difference was defined as P < 0.05.
Results
Effect of irradiation on cytokine levels produced by lymphocytes from healthy donors as controls, in vitro
In order to be sure that changes in levels of cytokines are not correlated with the cancer process, and that the effect of irradiation will be similar in healthy donors compared to that of head and neck cancer patients, we studied this comparison.
Lymphocytes from healthy donors were cultured in vitro, and the production of all cytokines was assessed. Cultures without irradiation served as controls and were compared to those with irradiation. Evaluation of the irradiation (5 and 10 Gy) effect on the inflammatory cytokines production (TNF-α, IL-6, IL-8), the anti-inflammatory cytokine IL-10, and the general immune activation cytokine sIL-2R, were compared to those of the head and neck cancer patients (Figure 1).
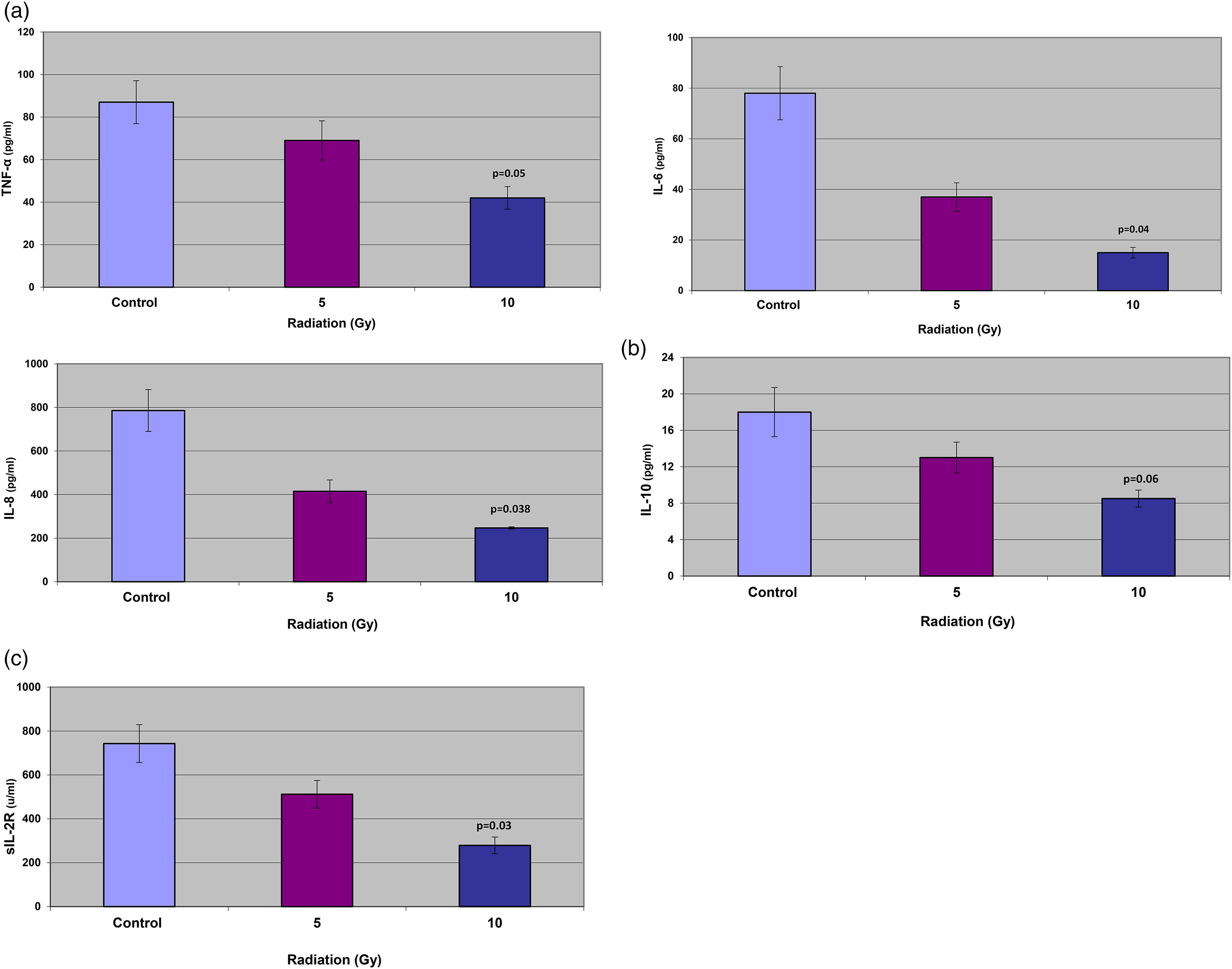
(a) Effect of irradiation on inflammatory cytokines production (healthy donors). (b) Effect of irradiation on IL-10 production (healthy donors). (c) Effect of irradiation on sIL-2R production (healthy donors).
Summary of Figure 1
Overall, irradiation decreased the levels of all tested cytokines produced by lymphocytes from healthy donors. The percentage of reduction was proportional to the irradiation dose:10 Gy caused approximately a two-fold decrease compared to 5Gy. The largest reductions were found in IL-6 and IL-8 (by the two-sample t-test), which showed significant decreases (P < 0.05) following 10Gy relative to the control.
Effect of irradiation on cytokine production in cancer patients
We examined the effect of irradiation in vivo by evaluating serum levels of the cytokines IL-6, IL-10, IL-18, sIL-2R, and TNFα in head and neck cancer patients with severe mucositis. Patients received radiotherapy to the head and neck region, with doses ranging from 50 to 70 Gy. All patients had clinical evaluations before, during, and after treatment (weeks 0–8). We collected blood samples at 2-week intervals from 23 patients, and following the evaluation of serum cytokine levels, the samples were examined for any potential correlation to clinical status and to radiation toxicity—especially with respect to the need for PEG tube installation.
Figures 2 to 4 show a correlation in the majority of patients between high inflammatory and low anti-inflammatory cytokine levels and the need for PEG tube installation (and vice versa).
Increases in the tested cytokines over time correlated with a need for PEG tube installation, while decreases correlated with no need for PEG tube installation (according to the Mann-Whitney U test) (Figure 2).
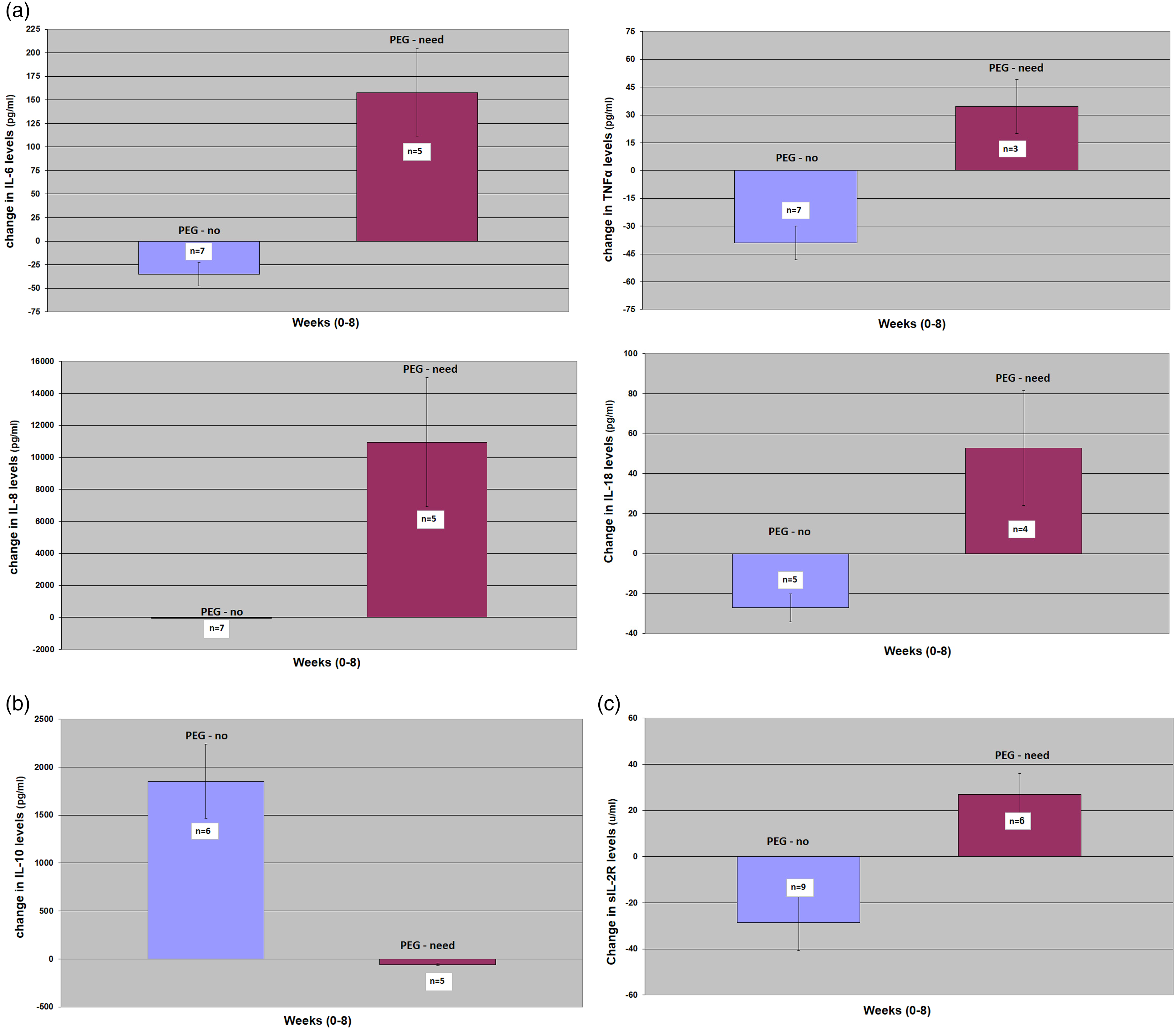
(a) Effect of irradiation on inflammatory cytokine production (cancer patients). (b) Effect of irradiation on the production of IL-10. (c) Effect of irradiation on the production of sIL-2R.
Decreasing levels of cytokines in individual patients (with no need for PEG)
To better understand the correlation between decreasing levels of inflammatory cytokines and the clinical parameter need for PEG tube installation, Figure 3 shows individual decreases over the duration of radiation therapy in representative patients.
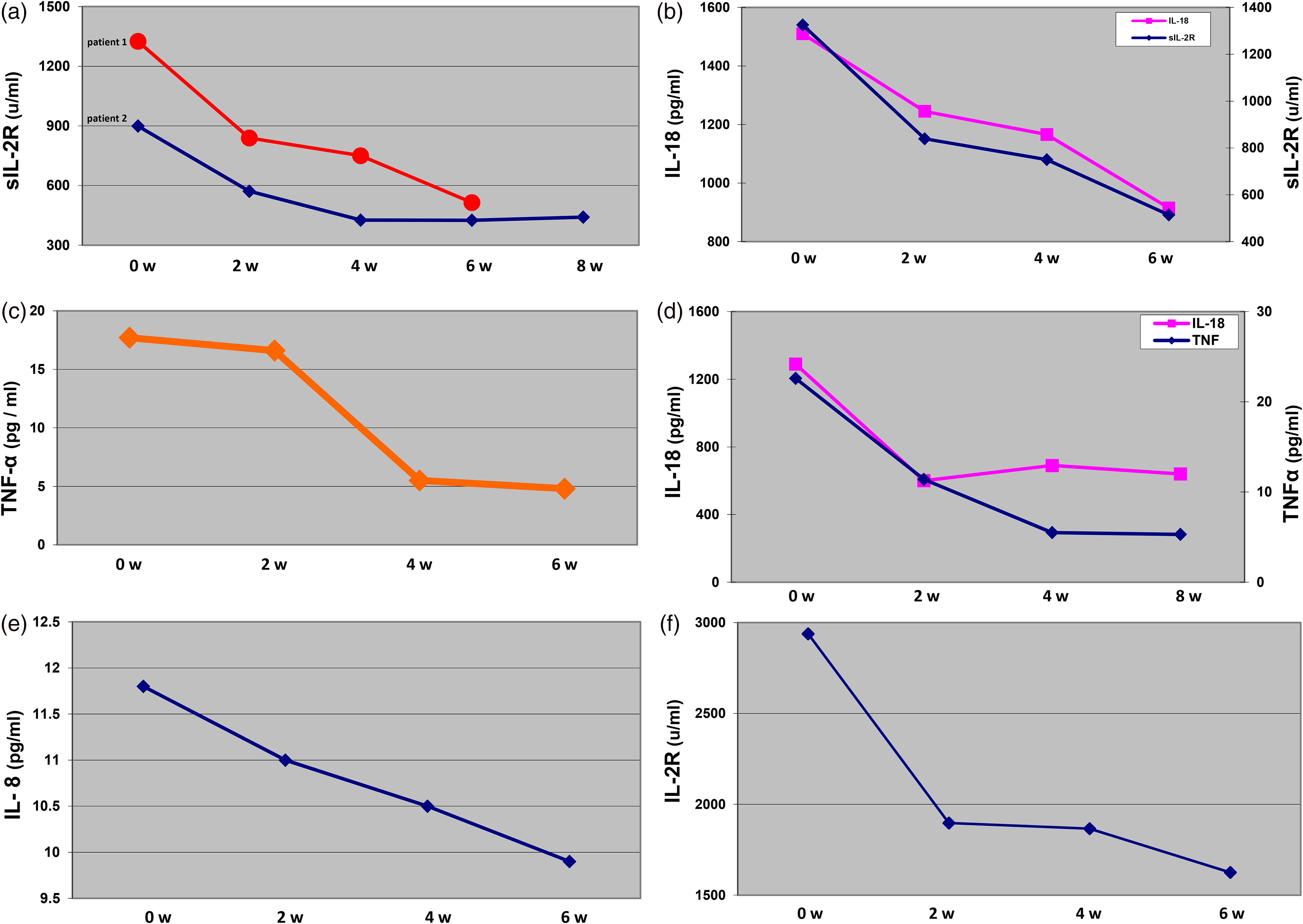
(a) Decreases in sil-2R serum levels. (b) Decreases in IL-18 and sIL-2R levels. (c) Decreases in TNFα serum levels. (d) Decreases in IL-18 and TNFα serum levels. (e) Decreases in IL-8 serum levels. (f) Decreases in IL-2R serum levels.
Increasing levels of cytokines in individual patients (with a need for PEG)
Figure 4 shows increases in inflammatory cytokine levels correlated to metastases formation and aggravation of clinical status of patients, leading to PEG tube installation.
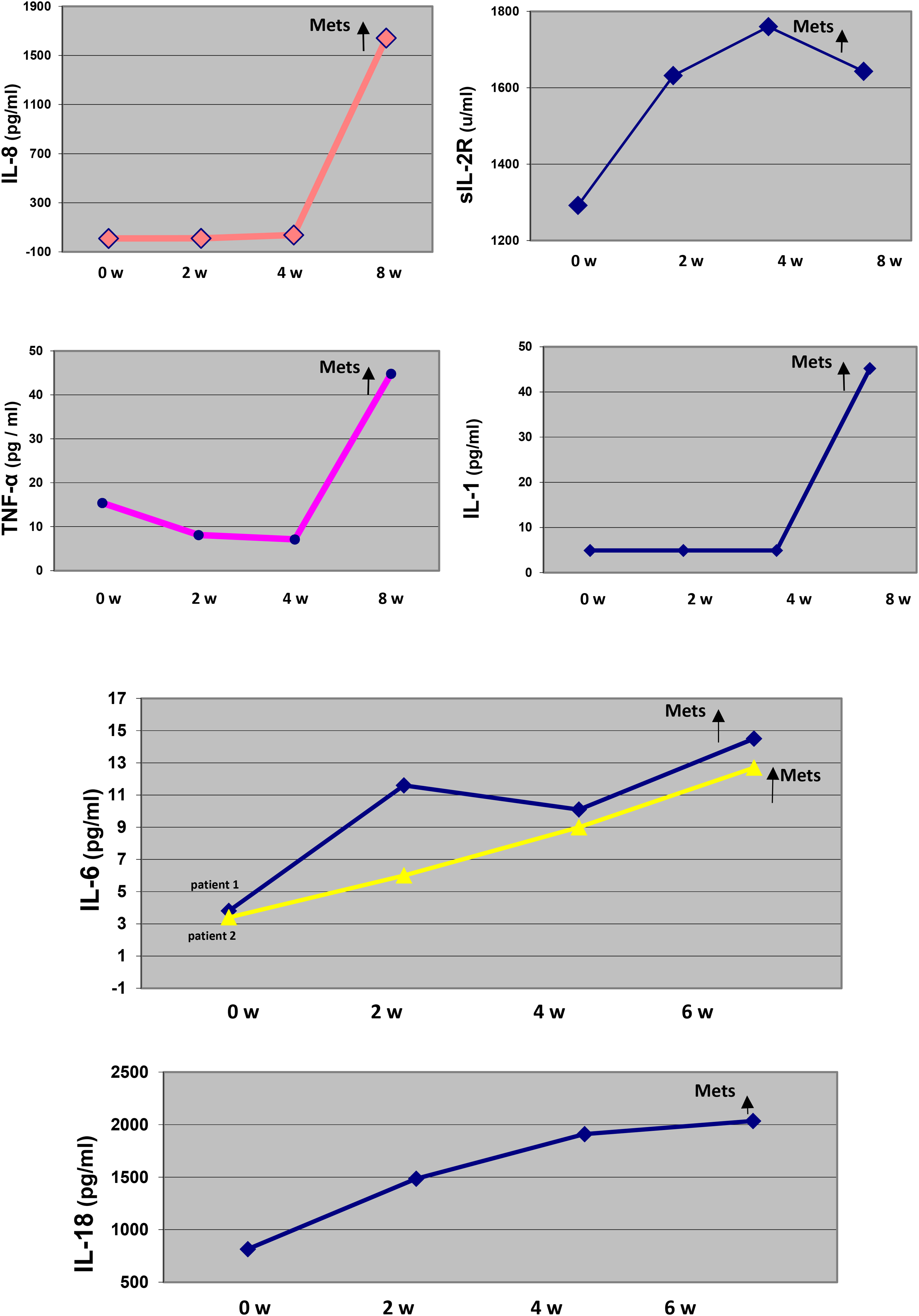
Increases in cytokine patients’ serum levels.
Discussion
Most head and neck cancers are treated with various forms of irradiation and are occasionally combined with chemotherapy. 26 One of the most common side effects of head and neck radiation therapy is mucositis, which ultimately may require treatment using PEG tube installation, which is an uncomfortable treatment for patients. The early detection of patients at high-risk for developing mucositis is important for optimal treatment intervention and the prevention of unnecessary PEG tube installation.
Cytokine levels are already known to be highly variable in the dynamic tumor microenvironment prior to any radio therapeutic intervention. This study reveals not only how radiotherapy has a direct effect on cytokine levels but also how monitoring the increasing levels of certain pro-inflammatory cytokines may be utilized as a predictive tool for the development of mucositis severity and ultimately the need for PEG tube installation.
PEG tube installation 25 plays an important role in providing nutrition to patients who require alternative methods of nutritional delivery, and circumvents the need for invasive, surgical gastrostomy insertions and general anesthetic exposure. Despite the advantages of PEG tube installation, the procedure carries serious risks, side effects, and contraindications; therefore, every effort should be made in patient care to avoid it.
This study provides a means to predict the need for PEG tube installation in head and neck cancer patients being treated with radiotherapy through the tracking of cytokine serum levels and the incidence of mucositis. The ability to predict this in a clinical setting is of vital importance as it would allow for early intervention treatment, thus preventing mucositis development and ultimately the need for PEG tube installation. This would not only reduce patient suffering and improve quality of life but also contribute to faster recovery times post-irradiation.
In both our preliminary study 27 and this study, we show that cytokine levels may be utilized as insightful biomarkers where a correlation between changes in cytokine levels and the ultimate need for PEG tube installation was found. Increases in inflammatory cytokine levels were associated with a need for PEG tube installation, while decreases were associated with no need for it.
The present study shows a strong correlation between IL-6, IL-8, sIL-2R, and severe mucositis. Similarly, other studies have shown a correlation between high IL-6 levels and cancer therapy resistance, cancer recurrence, and metastases, especially in head and neck cancer. 26 Another study, published in Cancer, supports our conclusions—higher levels of the inflammatory IL-1 and IL-6 are correlated with mucositis severity, while the anti-inflammatory IL-13 correlates with reduced mucositis severity. 26 An additional paper also found that the inflammatory cytokine IL-8 is an indicator of mucositis severity.
Multiple studies have recently shown that the immune biomarker sIL-2R, correlates with disease state in many types of cancer including HCL, 19 breast cancer, 8 peripheral blood cells (PBC), 18 head and neck cancer,28,29 lymphoma,30,31 and melanoma. 32 High sIL-2R levels or serial increases predict recurrence and metastases formation,30–33 which enable earlier treatment with improved patient outcomes.
This study predicts the need for PEG tube installation—a procedure that is not only unpleasant for the patient but also carries potentially serious side effects within itself. Using the prediction tools of this study in the form of tracking cytokine levels and monitoring for the presence and severity of mucositis allows for early treatment intervention and the prevention of PEG tube installation in the future.
Conclusions
The main findings of this study contribute to the differentiation of head and neck cancer patients with regard to potential mucositis severity and the need for PEG tube installation.
Cytokine kinetics in head and neck cancer patients have the potential to serve as prognostic factors to predict the requirement for PEG tube installation prior to the development of complications, enabling earlier treatment. Decreases in sIL-2R and inflammatory cytokines were associated with less radiation cytotoxic effects in terms of mucositis; therefore, there was no need for PEG tube installation. In contrast, increases and high levels in sIL-2R and inflammatory cytokines were correlated with a need for PEG tube installation.
However, future, more complex studies including larger numbers of patients are warranted to confirm the results of this study before introducing these cytokine biomarkers into routine oncology and irradiation care.
Footnotes
Acknowledgements
We thank Kim Sheva for editing this paper.
Author contributions
BV: Project PI and paper preparation; MA and GM: Clinical Principal Investigators; CS: Technical assistance; MA and GM contributed equally to this paper.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
