Abstract
Background:
Previous literature has demonstrated that an increased number of preoperative anterior shoulder instability episodes is associated with recurrent anterior shoulder instability after arthroscopic Bankart repair (ABR). However, a threshold for the number of preoperative instability episodes that increases the risk of recurrent anterior shoulder instability is not well established.
Purpose:
To establish a threshold value for the number of preoperative instability episodes that predicts recurrent anterior shoulder instability after ABR and to compare glenoid bone loss, the Hill-Sachs interval, and the distance to dislocation between patients who have surpassed the threshold and those who have not.
Study Design:
Retrospective cohort study; Level of evidence, 3.
Methods:
This retrospective review included consecutive patients with “on-track” Hill-Sachs lesions who underwent primary ABR for anterior shoulder instability at a single institution between 2007 and 2019. Patients with an unknown number of preoperative instability episodes, >20% glenoid bone loss, <2 years’ follow-up, or age >40 or <14 years were excluded. Logistic regression assessed associations between preoperative anterior shoulder instability episodes and recurrent anterior shoulder instability after ABR, defined as a recurrent subluxation or dislocation. Receiver operating characteristic analysis determined the optimal threshold of preoperative anterior shoulder instability episodes to predict recurrent anterior shoulder instability. Significance was set as
Results:
A total of 151 patients (mean age, 20 ± 5 years; mean follow-up, 6.0 ± 3.1 years) were included, of whom 28 (19%) experienced recurrent anterior shoulder instability. Multiple thresholds showed increased odds of recurrent anterior shoulder instability: ≥2 preoperative anterior shoulder instability events (odds ratio [OR], 9.70 [95% CI, 2.63-35.70];
Conclusion:
A threshold of ≥2 preoperative anterior shoulder instability episodes best predicted recurrent anterior shoulder instability after ABR. Stratification beyond 1 versus ≥2 preoperative anterior shoulder instability episodes did not increase predictive ability. This finding may help surgeons to counsel patients and consider earlier surgical stabilization in those who have sustained anterior shoulder instability episodes.
Keywords
Arthroscopic Bankart repair (ABR) is a commonly utilized procedure for anterior shoulder instability, particularly in patients with minimal glenoid bone loss (GBL) and “on-track” Hill-Sachs lesions (HSLs).6,19 However, recurrent anterior shoulder instability remains a common complication after ABR, with reported rates exceeding 30% in young athletic cohorts.19,22,23,29
Previous literature has identified multiple preoperative anterior shoulder instability episodes as a risk factor for recurrent anterior shoulder instability after ABR.4,8,11,24 The number of preoperative instability episodes has been associated with progressive GBL and damage to soft tissue of the labrum and anterior shoulder capsule, which may contribute to the increased risk of recurrent anterior shoulder instability. 3 Fox et al 10 found that patients with >1 preoperative dislocation had higher rates of recurrent shoulder instability after ABR compared with those who experienced a single preoperative dislocation. However, the optimal threshold of multiple preoperative instability episodes that predicts recurrent anterior shoulder instability in “on-track” HSLs is unclear. Establishing a threshold for the number of preoperative instability episodes that best predicts recurrent anterior shoulder instability after ABR may improve risk stratification, enhance preoperative patient counseling, and inform the timing of surgical interventions to optimize outcomes after ABR.
Thus, the primary purpose of this study was to investigate the relationship between the number of preoperative anterior shoulder instability episodes and recurrent anterior shoulder instability after ABR and to establish a threshold value for the number of preoperative anterior shoulder instability episodes that best predicts recurrent anterior shoulder instability after ABR. We hypothesized that a threshold of ≥2 preoperative anterior shoulder instability episodes would have the greatest predictive capability for recurrent anterior shoulder instability after ABR. A secondary aim of this study was to compare anatomic characteristics including GBL, Hill-Sachs interval (HSI), and distance to dislocation (DTD) between patients above and below the threshold of ≥2 preoperative anterior shoulder instability episodes. We hypothesized that patients above the threshold of ≥2 preoperative anterior shoulder instability episodes would have greater GBL, a larger HSI, and a smaller DTD compared to patients below the threshold.
Methods
Study Population
Institutional review board approval was obtained from the University of Pittsburgh (No. STUDY20030061). A retrospective review was conducted of consecutive patients who underwent ABR for shoulder instability at a single institution by 5 sports fellowship–trained orthopaedic surgeons between 2007 and 2019. First, nonanterior stabilization procedures were excluded. Before database creation, initial exclusion criteria included revision procedures, prior ipsilateral shoulder surgery, open surgical stabilization, multidirectional or concomitant posterior instability, connective tissue diseases, uncontrolled seizure disorder or seizures within 2 years of surgery, concomitant greater tuberosity or proximal humerus fractures, inadequate preoperative imaging including no available magnetic resonance imaging (MRI) scans, MRI performed >6 months before surgery, poor MRI quality or inadequate sagittal sequences precluding accurate humeral bone loss and/or GBL measurements, and ABR performed with <2 anchors. Furthermore, any patients who had a concomitant procedure performed, such as remplissage augmentation to ABR, were excluded. After database creation, patients were excluded if they had an unknown number of preoperative anterior shoulder instability episodes, had >20% GBL, underwent revision ABR, had <2 years of follow-up, or were aged >40 or <14 years.
Data Collection
A chart review of the electronic medical record was used to extract demographic variables including patient age, sex, sport type (stratified into collision, contact, and/or overhead sport), laterality of injury, number of anchors placed intraoperatively, presence of glenohumeral capsuloligamentous hyperlaxity, and number of preoperative anterior shoulder instability episodes. Competitive athletes were defined as patients actively participating in organized sports at a competitive level, including high school, club, collegiate, or professional play. A preoperative anterior shoulder instability episode was defined as sustaining either a glenohumeral subluxation or dislocation event. A subluxation was defined as a self-reported sensation of anterior shoulder instability not requiring manual reduction, while a dislocation was defined as anterior shoulder instability requiring manual reduction. Preoperative glenohumeral hyperlaxity was determined during an examination under anesthesia and was defined as external rotation >85° with the arm at the side and/or grade 2 to 3 humeral head translation relative to the glenoid on all anterior, posterior, or inferior load-and-shift tests at 90° of abduction. 3 Grade 2 humeral head translation was defined as humeral head translation over the glenoid rim with spontaneous reduction, and grade 3 humeral head translation was defined as humeral head translation without spontaneous reduction. 1
The primary outcome of this study was recurrent anterior shoulder instability, defined as sustaining at least 1 postoperative glenohumeral subluxation or dislocation event. This outcome was collected via a review of the electronic medical record. All patients who met inclusion criteria but did not have at least 2 years of follow-up in the electronic medical record were contacted by telephone. After informed consent was obtained, patients were asked if they had sustained a glenohumeral subluxation or dislocation event in the time after index ABR as well as any revision procedures or subsequent ipsilateral shoulder surgery since their index ABR.
MRI Measurements
All MRI measurements were performed by 2 sports fellowship–trained orthopaedic surgeons. Anatomic measurements obtained from preoperative MRI included GBL, HSI, and DTD. GBL was measured as a percentage of anterior GBL relative to the total glenoid width utilizing the perfect-circle method on T2-weighted sagittal MRI sequences. 15 The HSI was measured on T2-weighted axial MRI sequences as the distance from the most medial aspect of the HSL to the infraspinatus insertion site laterally. The glenoid track (GT) was calculated using the formula GT = 0.83 * D – d, where “D” is the diameter of the glenoid best-fit circle and “d” is the width of anterior GBL. 30 The DTD could then be calculated with the HSI and GT using the formula DTD = GT – HSI. 16 The HSL was then categorized as “on-track” if the DTD was >10 mm or “near-track” if the DTD was between 0 and 10 mm. 16
Surgical Technique and Postoperative Care
All ABR procedures were performed in either the lateral decubitus or beach-chair position, according to surgeon preference. ABR was performed using a standard suture anchor technique with a minimum of 3 anchors. All patients then underwent a standard postoperative protocol consisting of restricted motion in a sling for 4 weeks, followed by supervised physical therapy focused on increasing range of motion and isometric rotator cuff exercises beginning at 4 weeks, and finally dynamic strength training beginning at 12 weeks. Athletes were cleared to return to sport at around 24 weeks based on shared decision-making and criteria-based return-to-sport testing described by Drummond et al. 9
Statistical Analysis
An independent-samples
A post hoc sensitivity analysis was conducted among patients with ≥2 preoperative anterior shoulder instability episodes, comparing the proportion of patients with recurrent anterior shoulder instability (n = 28) with the proportion of patients without recurrent anterior shoulder instability (n = 123). With an alpha of 0.05 and 80% power, the study was sufficiently powered to detect a minimum effect size (Cohen
Results
There were 181 patients who were identified for an initial evaluation; 21 were excluded for missing data on the number of preoperative anterior shoulder instability episodes, 1 for <2 years of follow-up, 4 for >20% GBL, and 4 for age >40 or <14 years (Figure 1). A total of 151 patients were included for final analysis, with a mean age of 20 ± 5 years and a mean follow-up time of 6.0 ± 3.1 years.
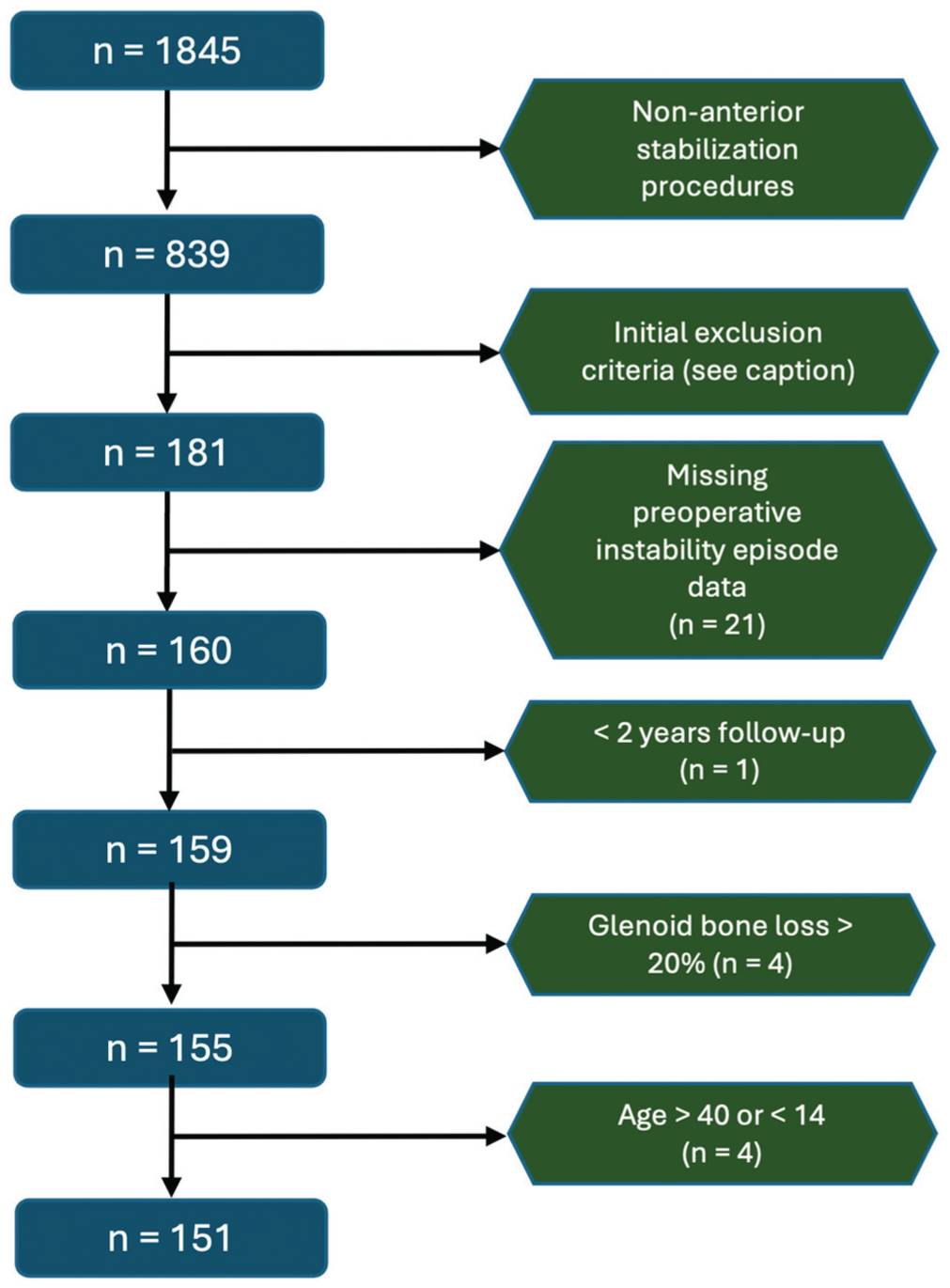
Patient selection flowchart. Initial exclusion criteria included revision procedures, prior ipsilateral shoulder surgery, open surgical stabilization, multidirectional or concomitant posterior instability, connective tissue diseases, uncontrolled seizure disorder or seizures within 2 years of surgery, concomitant greater tuberosity or proximal humerus fractures, inadequate preoperative imaging including no available magnetic resonance imaging (MRI) scans, MRI performed >6 months before surgery, poor MRI quality or inadequate sagittal sequences precluding accurate humeral and/or glenoid bone loss measurements, and arthroscopic Bankart repair performed with <2 anchors.
Overall, 28 patients (19%) experienced recurrent anterior shoulder instability after ABR. Patients who experienced recurrent anterior shoulder instability after ABR were younger (18 vs 21 years, respectively;
Baseline Characteristics of Patients
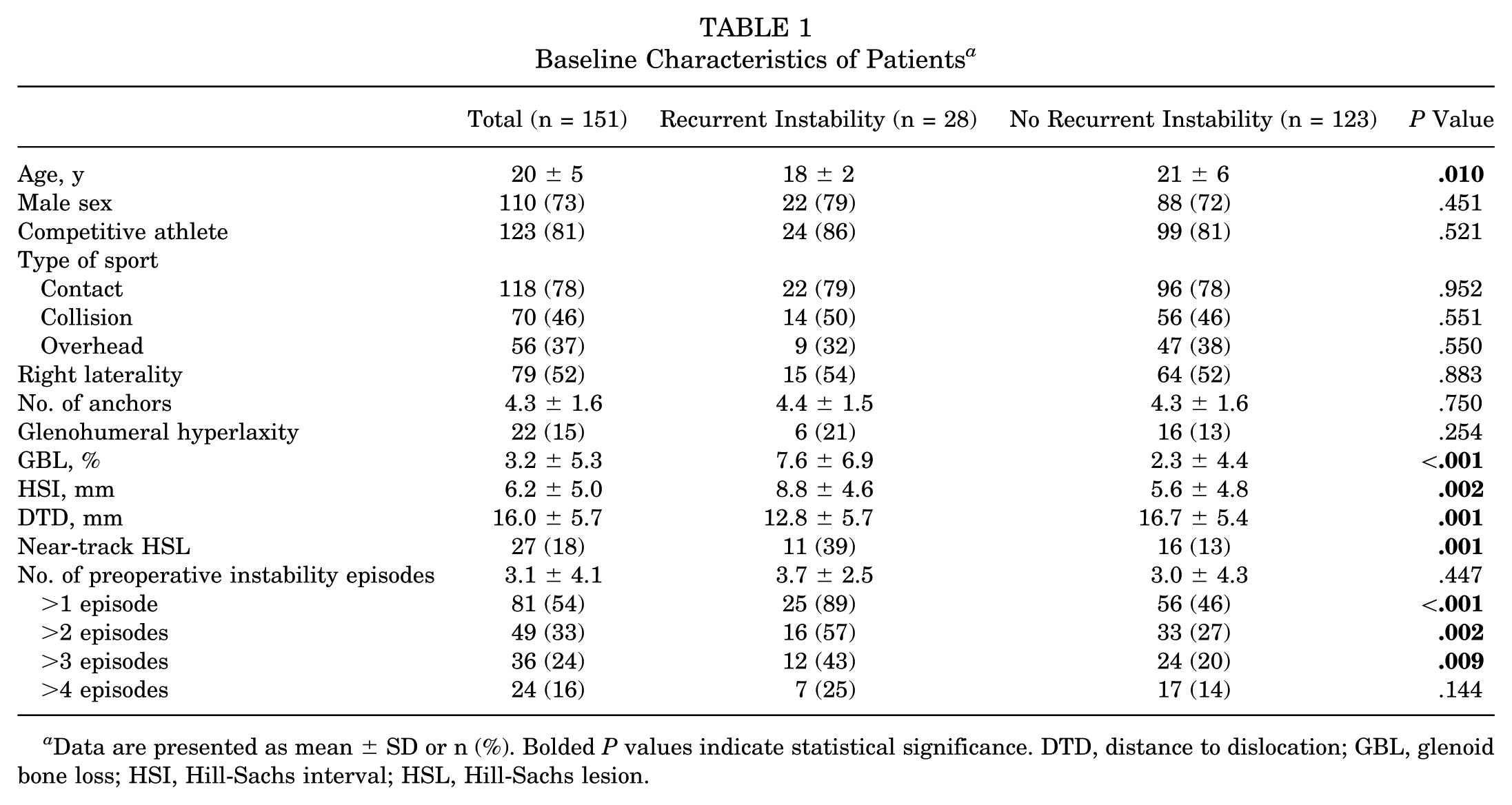
Data are presented as mean ± SD or n (%). Bolded
Multivariable Predictors of Failure After Arthroscopic Bankart Repair
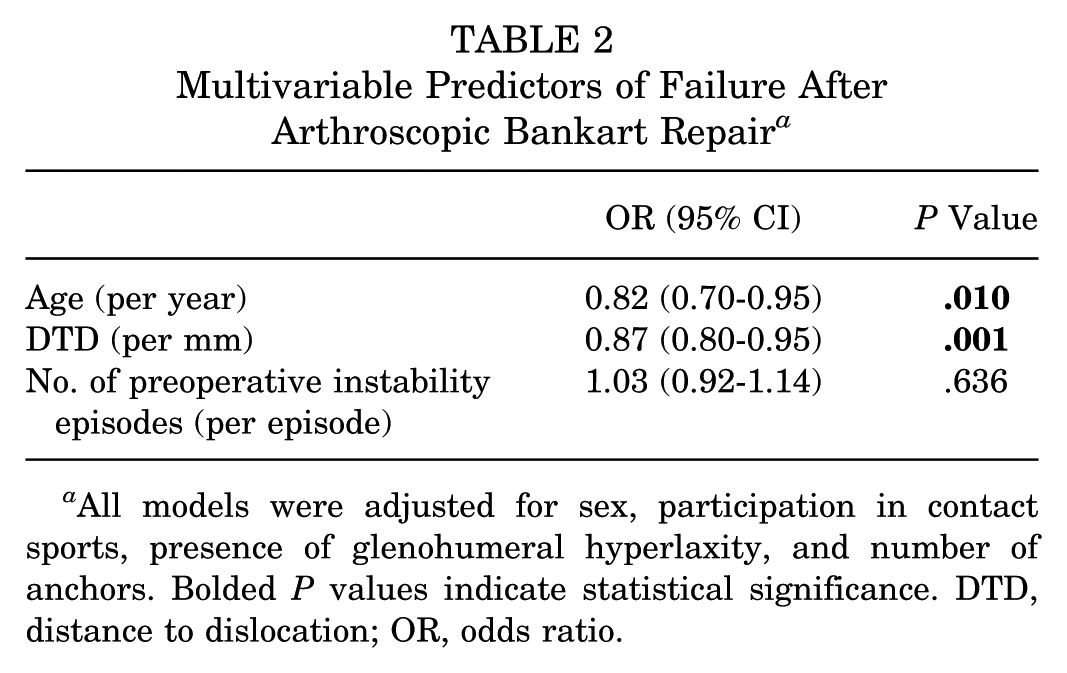
All models were adjusted for sex, participation in contact sports, presence of glenohumeral hyperlaxity, and number of anchors. Bolded
When the number of preoperative anterior shoulder instability episodes was analyzed in a categorical manner and the model was adjusted for confounders, patients who had ≥2 preoperative anterior shoulder instability episodes had 9.70 times the odds of experiencing recurrent anterior shoulder instability after ABR compared to patients who sustained only 1 preoperative anterior shoulder instability episode (
Multivariable Predictors of Failure After Arthroscopic Bankart Repair Based on Number of Preoperative Instability Episodes
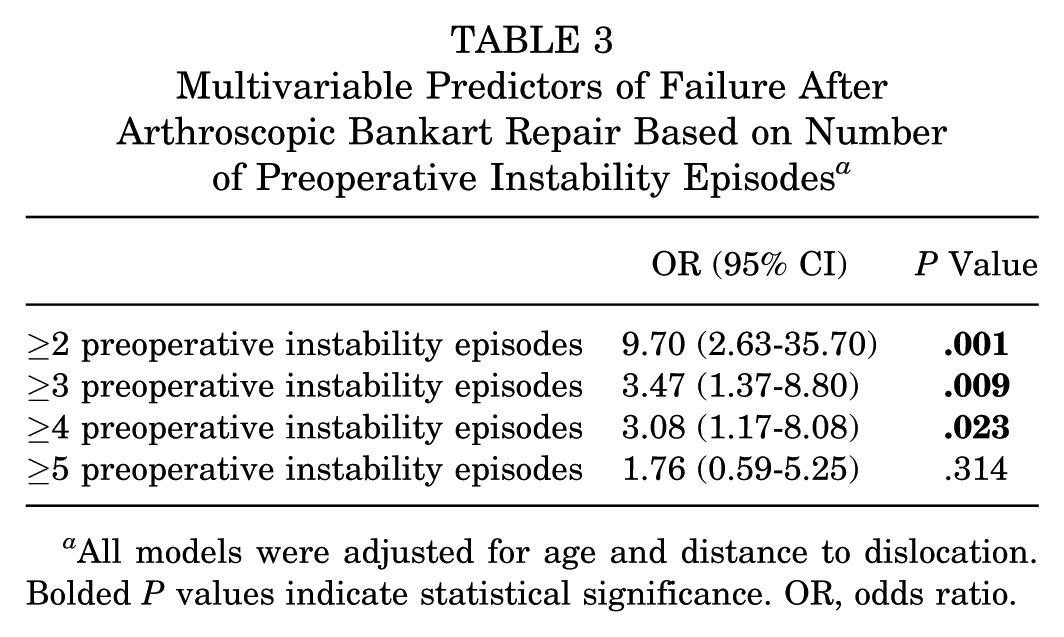
All models were adjusted for age and distance to dislocation. Bolded
Using the Youden index, the optimal cutoff value for preoperative anterior shoulder instability episodes to predict recurrent anterior shoulder instability was ≥2 preoperative anterior shoulder instability episodes (Youden index = 0.44), corresponding to a sensitivity of 89%, specificity of 55%, and AUC of 0.72, indicating good discriminative ability (Figure 2). Increasing the threshold to ≥3, ≥4, or ≥5 preoperative anterior shoulder instability episodes reduced the sensitivity for detecting patients at risk for recurrent anterior shoulder instability, with corresponding AUCs of 0.65, 0.62, and 0.56, respectively.
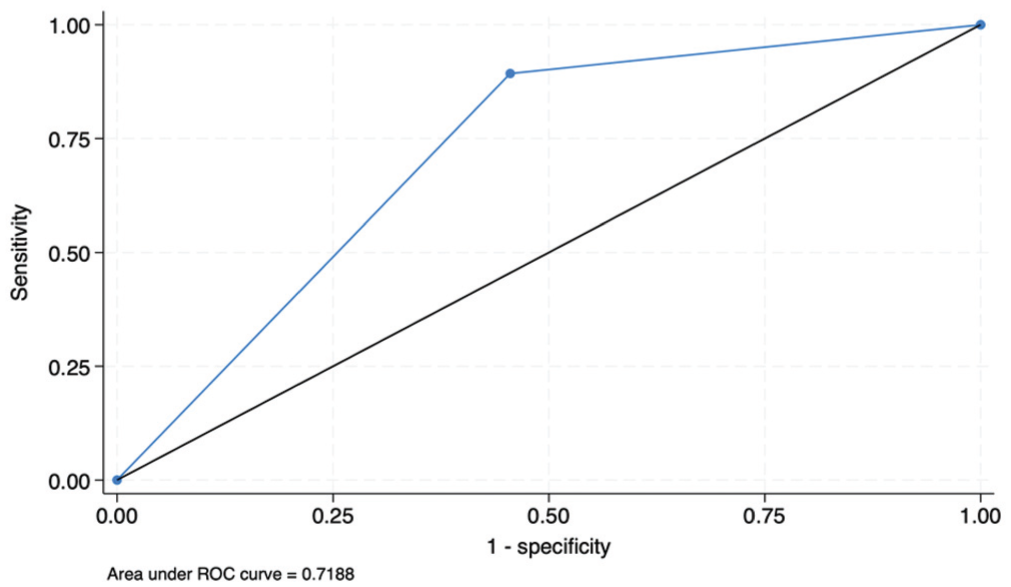
Receiver operating characteristic analysis with the Youden index was conducted to determine the optimal threshold for predicting recurrent anterior shoulder instability in the entire cohort. The optimal cutoff value to predict recurrent instability was ≥2 preoperative anterior shoulder instability episodes (Youden index = 0.438 [standard error = 0.074]), corresponding to a sensitivity of 89%, specificity of 55%, and area under the curve (AUC) of 0.72.
Anatomic characteristics were then compared between patients above and below the threshold of ≥2 preoperative anterior shoulder instability episodes. Patients with ≥2 preoperative anterior shoulder instability episodes had greater GBL (4.4% vs 2.0%, respectively;
Anatomic Characteristics Between Patients With ≥2 and 1 Preoperative Instability Episodes
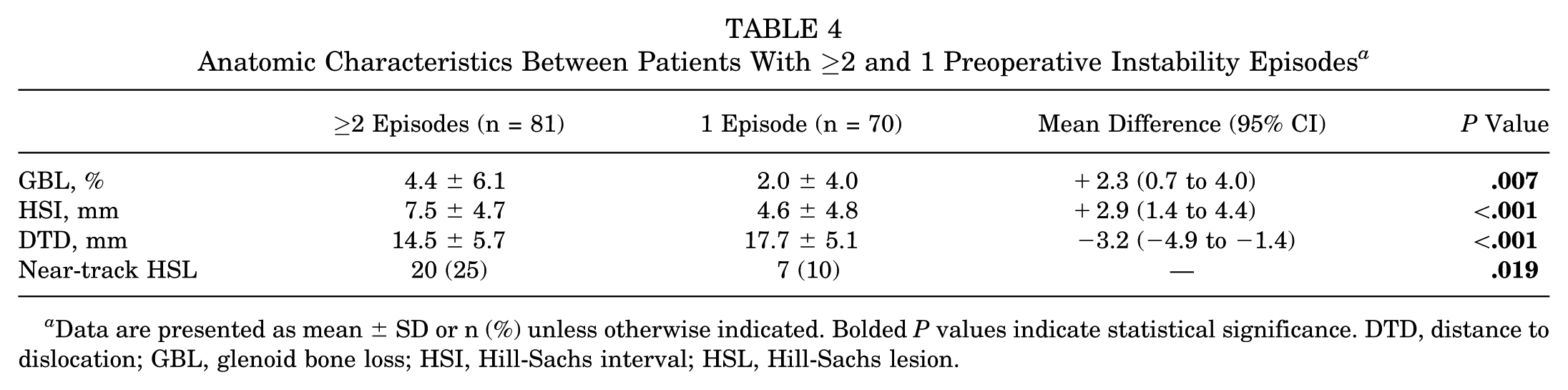
Data are presented as mean ± SD or n (%) unless otherwise indicated. Bolded
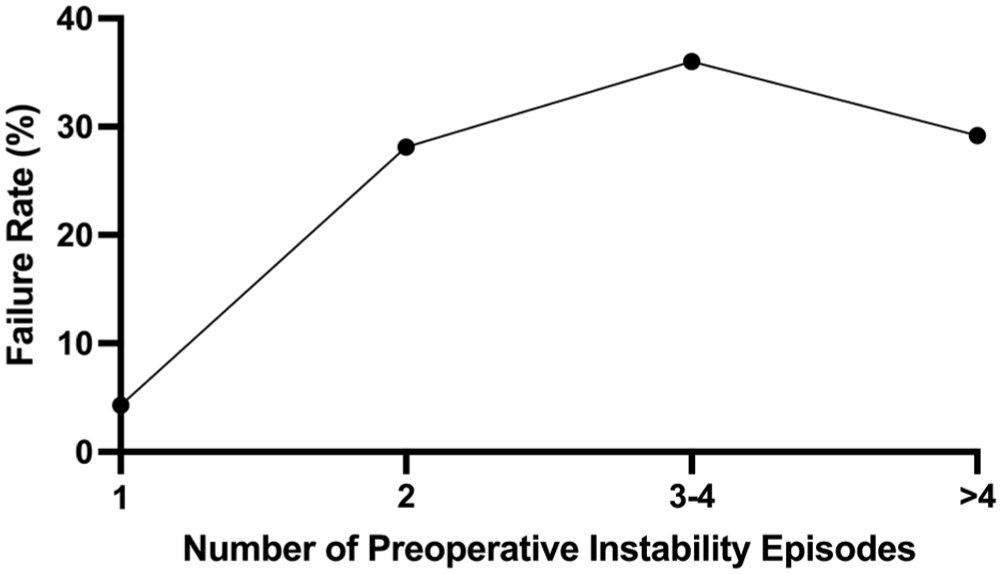
Preoperative anterior shoulder instability episodes were divided into different numbers of preoperative instability episodes (1, 2, 3-4, or >4 episodes). The rate of recurrent anterior shoulder instability was calculated for each group.
Discussion
The present study identified that a threshold of ≥2 preoperative anterior shoulder instability episodes best predicted patients who would experience recurrent anterior shoulder instability after ABR. Increasing the threshold beyond ≥2 preoperative anterior shoulder instability episodes reduced sensitivity for predicting recurrent anterior shoulder instability, indicating that fewer patients who ultimately experienced recurrent anterior shoulder instability were correctly identified as being at risk when using thresholds higher than ≥2 preoperative anterior shoulder instability episodes. Patients with ≥2 preoperative anterior shoulder instability episodes had greater GBL and a larger HSI than those with only 1 preoperative anterior shoulder instability episode, suggesting that repeated anterior shoulder instability episodes after an initial episode lead to progressive structural damage and further predispose patients to recurrent anterior shoulder instability after ABR. Recognizing this threshold can help to consider earlier surgical stabilization and avoid unnecessary stratification beyond this critical cutoff.
The findings of this study align with prior literature, which has identified that sustaining >1 preoperative anterior shoulder instability episode is a risk factor for experiencing recurrent anterior shoulder instability after ABR.8,10,11,24 Kay et al 13 analyzed 488 adolescent patients and found that those with multiple preoperative dislocations faced a markedly higher risk of recurrent anterior shoulder instability requiring revision stabilization surgery compared to those with a single episode. Specifically, only 3.2% of patients with a single preoperative dislocation required revision stabilization surgery versus 24.2% with 2 dislocations and 33.5% with ≥3 dislocations, underscoring the potential value of earlier surgical interventions before repeated dislocations lead to increased GBL and progressive soft tissue damage to the anterior labrum and anterior shoulder capsule. 13 Warner et al 28 also conducted a systematic review across 11 studies involving 767 patients, observing that patients with >1 preoperative dislocation were consistently shown to have an elevated risk of recurrent anterior shoulder instability after ABR. Finally, Charles et al 4 evaluated 170 patients undergoing either ABR or ABR with remplissage augmentation and found that patients who experienced >1 preoperative anterior shoulder instability event had a >3-fold increased risk of recurrent anterior shoulder instability compared with those who presented after a single episode. The findings of this study add to the present literature, identifying that a threshold of ≥2 preoperative anterior shoulder instability episodes best predicted recurrent anterior shoulder instability after ABR and indicating that further delineation of the number of preoperative anterior shoulder instability episodes beyond this threshold might not impact clinical outcomes after ABR.
A secondary finding of this study was that patients with ≥2 preoperative anterior shoulder instability episodes had a significantly larger HSI and greater GBL compared to patients with only 1 preoperative anterior shoulder instability episode. It is well established in scientific literature that an increased number of preoperative anterior shoulder instability episodes is the factor most strongly associated with GBL, the presence of HSLs, and the presence of combined glenoid and humeral head bone loss.12,17,18 Dickens et al 7 found that a single preoperative anterior shoulder instability episode resulted in an average GBL of 6.8% but was 22.8% in patients with recurrent anterior shoulder instability. In a multicenter study of over 892 patients with anterior shoulder instability, for each additional dislocation, the odds of having combined GBL and HSLs nearly doubled, underscoring the cumulative risk of repeated anterior shoulder instability events. 12 This progressive bone loss is clinically significant, as it is a major predictor of recurrent anterior shoulder instability after ABR and may necessitate more complex surgical interventions, such as the Latarjet procedure. This study builds upon these previous studies by showing that sustaining ≥2 preoperative anterior shoulder instability episodes was the most sensitive threshold for predicting recurrent anterior shoulder instability after ABR when compared to sustaining only 1 preoperative anterior shoulder instability episode. This suggests that an earlier surgical intervention (ie, before sustaining ≥2 preoperative anterior shoulder instability episodes) may be indicated after a first-time anterior shoulder instability episode, as delaying ABR until even the occurrence of a second preoperative anterior shoulder instability episode may allow cumulative structural damage that predisposes patients to experience recurrent anterior shoulder instability. The findings of the present study reinforce the importance of considering early surgical stabilization in high-risk patients to minimize the chance of recurrent anterior shoulder instability and protect glenoid and humeral bone integrity.
With regard to the recurrence rates in the present study, the overall rate in the entire cohort was 19%, which is consistent with previously reported outcomes after ABR.26,27 The relatively higher failure rates observed in certain subgroups likely reflect the evolving understanding of appropriate indications for isolated ABR during the study period rather than deficiencies in the surgical technique, as factors such as the number of preoperative anterior shoulder instability episodes were not yet widely recognized as key determinants of surgical decision-making between ABR alone versus adjunctive or alternative procedures. With a mean follow-up of 6.0 years, these findings also align with longer term outcome data, including reports of failure rates approaching 30% at 10 years, supporting the interpretation that recurrent instability is more closely related to patient selection and the natural history of shoulder instability than to the technical failure of isolated ABR. 19 Over the study period, the recognition of recurrence risk factors and indications for remplissage augmentation to ABR evolved, allowing the inclusion of patients treated with isolated ABR who would now likely undergo concomitant remplissage. At present, we favor remplissage augmentation for patients with on-track HSLs in the setting of subcritical (≤20%) GBL who carry additional risk factors for recurrence, including participation in contact sports, near-track lesions, generalized hyperlaxity, multiple preoperative instability episodes, and age <25 years, and have an acceptable risk of recurrence based on the number of these risk factors. 4
This study is not without limitations. First, the present study's retrospective design may lead to selection bias, incomplete data, and potential misclassification of the number of preoperative anterior shoulder instability episodes based on patient recall. Additionally, because of the limitations in data granularity, we were unable to differentiate between subluxation and frank dislocation events when characterizing preoperative instability. However, prior studies have demonstrated that patients with recurrent subluxations and those with recurrent dislocations exhibit similar pathoanatomy and comparable outcomes after ABR, suggesting that this limitation may have a minimal impact on the validity of our findings.20,21 Furthermore, because our definition of recurrent anterior shoulder instability relied, in part, on patient-reported symptoms, this may also introduce reporting bias into this study. Our multivariable logistic regression models, while accounting for key confounders, do not capture the influence of unmeasured variables such as rehabilitation compliance, which may have influenced postoperative outcomes. Although the “on-track” classification was applied retrospectively using available MRI scans, 5 which is consistent with prior studies,2,16 this approach may be subject to inherent measurement imprecision and limited imaging standardization. The use of the conventional MRI method to measure the HSI may have overestimated off-track lesions, potentially biasing the cohort toward minimal GBL. 14 Finally, it is not immediately clear why a threshold of ≥5 preoperative anterior shoulder instability episodes was not a significant predictor of recurrent anterior shoulder instability after ABR. While this finding is counterintuitive, it may be a result of diminished statistical power, as only 24 patients (16%) reported ≥5 dislocations.
Conclusion
A threshold of ≥2 preoperative anterior shoulder instability episodes best predicted recurrent anterior shoulder instability after ABR. Increasing the threshold beyond ≥2 episodes did not increase predictive ability, indicating that stratification beyond 1 versus ≥2 preoperative anterior shoulder instability episodes may not be warranted. Surgeons may utilize this finding to counsel patients and consider earlier surgical shoulder stabilization.
Authors
Ryan T. Lin, BS, Ryan Gilbert, BA, Sahil Dadoo, MD, Amin Karimi, MD, Noah Feder, BS, Abigail Balsan, BS, Ehab M. Nazzal, MD, Shaquille Charles, MD, Jonathan D. Hughes, MD, PhD, Pittsburgh Shoulder Institute, Adam Popchak, DPT, PhD, Bryson P. Lesniak, MD, Mark Rodosky, MD, Jenna L. Dvorsky, MS, Asher Mirvish, BS, Sophia McMahon, BS, and Albert Lin, MD (Department of Orthopaedic Surgery, UPMC Freddie Fu Sports Medicine Center, University of Pittsburgh, Pittsburgh, Pennsylvania, USA).
Footnotes
Submitted January 2, 2026; accepted February 6, 2026.
One or more of the authors has declared the following potential conflict of interest or source of funding: J.D.H. performs professional activities for Smith & Nephew; serves on the Education Committee of American Shoulder and Elbow Surgeons (ASES), the Team Physician and Athlete Advocacy Committee of AOSSM, the Sports Medicine/Arthroscopy Program Committee of the American Academy of Orthopaedic Surgeons, and the Innovations and New Technology Committee of the International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine (ISAKOS); and serves on the editorial or governing board of
