Abstract
Background:
The clinical impact of coracoid graft resorption after the Latarjet procedure has been controversial and likely underestimated.
Purpose:
To (1) develop and validate a refined classification system—coracoid graft resorption based on degree and location (CRDL); and (2) correlate clinical and radiological outcomes with the CRDL classification system.
Study Design:
Cohort study; Level of evidence, 3.
Methods:
Between January 2015 and December 2018, 63 patients who underwent the arthroscopic Latarjet procedure were evaluated with computed tomography imaging preoperatively, immediately postoperatively, and at a minimum 5-year follow-up. According to the resorption location, the coracoid graft resorption was classified as grade 0 (no resorption), grade 1 (resorption on the proximal-medial and/or distal-medial part), grade 2 (resorption on the proximal-lateral part with no resorption on the distal-lateral part), and grade 3 (resorption on the distal-lateral part). Resorption severity was categorized as mild (grades 0 and 1) and severe (grades 2 and 3). The incidence, classification, and location of graft resorption were described. Intrarater and interrater reliability were calculated. Correlations between the classification and clinical and radiological outcomes were analyzed.
Results:
After a mean follow-up of 85.3 months, coracoid graft resorption was observed in 84.1% of cases: grade 0 in 15.9%, grade 1 in 47.6%, grade 2 in 30.2%, and grade 3 in 6.3%. Mild and severe resorption were found in 63.5% and 36.5% of patients, respectively. Resorption mainly occurred on the proximal-medial part of the graft. Intra- and interrater reliability of the classification system were both almost perfect (κ = 0.865 and 0.822, respectively). Significant differences were found in the postoperative American Shoulder and Elbow Surgeons (ASES) and visual analog scale for pain (VAS) scores among different grades and between mild and severe resorption. Correlation and multivariable regression analyses identified higher-grade graft resorption as a risk factor for worse postoperative ASES and VAS scores.
Conclusion:
CRDL classification is a reliable and clinically relevant classification system for coracoid graft resorption evaluation. Application of the CRDL system reveals that while high-grade resorption is a significant risk factor for postoperative shoulder pain, it has no major impact on shoulder function or stability.
Keywords
The Latarjet procedure is a well-established surgical intervention for recurrent shoulder instability, offering favorable clinical outcomes and low recurrence rates.19,39 However, complication rates of up to 26% have been reported, 20 with graft-related issues representing the most common category. 18 Among these, with a high incidence ranging from 7.5% to 100%, 20 coracoid graft resorption is a controversial issue because of the unclear clinical impact.
The coracoid graft resorption has been evaluated to determine whether it is acceptable in clinical practice. Evidence suggests that coracoid graft remodeling is largely complete within 1 year, resulting in a structure comparable to that of the native glenoid. 21 However, persistent pain and recurrent dislocation associated with graft resorption have been reported.13,26,41 Several studies have attempted to characterize the extent and location of graft resorption using 2-dimensional (2D) or 3-dimensional (3D) computed tomography (CT), yet none have proposed a standardized classification system.6,8,16,21 To address this gap, we developed a classification system—termed coracoid graft resorption based on degree (CRD)—to quantify the severity of resorption. 45 Because of its simplicity and reliability, the CRD classification has been widely adopted in subsequent research.32,36,42
Despite these efforts, the relationship between graft resorption and clinical outcomes remains unclear. Current evaluation methods, including the CRD classification, may underestimate the clinical impact of resorption, as they assess severity solely based on the degree of graft resorption without accounting for its anatomic location. Consequently, the potential influence of resorption site on clinical outcomes is often overlooked. Moreover, prior research has predominantly focused on short-term outcomes and the open Latarjet procedure, 45 leaving a limited understanding of graft resorption in the context of long-term follow-up after arthroscopic Latarjet surgery.
Therefore, this study aimed to (1) develop and validate a refined classification system—coracoid graft resorption based on degree and location (CRDL)—and (2) correlate clinical and radiological outcomes with the CRDL classification system. It was hypothesized that the CRDL classification system would be reliable and valid to grade the severity of coracoid graft resorption, and significant resorption would be correlated with poor clinical outcomes after the arthroscopic Latarjet procedure.
Methods
Study Design and Population
This retrospective cohort study was approved by the institutional review board (No. K2025027-00). The medical records of patients who underwent the arthroscopic Latarjet procedure for the treatment of recurrent anterior shoulder instability between January 2015 and December 2018 were reviewed. The decision to proceed with the Latarjet procedure was primarily driven by the extent of the glenoid defect, which was more precisely evaluated than lesions on the humeral head side. The size of any Hill-Sachs lesion was therefore not a major consideration. Indications for the arthroscopic Latarjet procedure included traumatic unidirectional anterior shoulder instability with a glenoid bone defect ≥15% on CT en face view or a defect <15% in patients participating in contact/overhead sports or requiring revision surgery after a failed Bankart repair. Contraindications were multidirectional instability, uncontrolled epilepsy, or psychological illness.
Patients who met the following inclusion criteria were included: (1) treatment with the arthroscopic Latarjet procedure, (2) a minimum 5-year follow-up, and (3) consent to participate in the study. Exclusion criteria were (1) incomplete clinical or radiological data and (2) concomitant musculoskeletal or neurovascular disorders of the ipsilateral shoulder. A total of 63 patients (63 shoulders) were finally analyzed (Figure 1).
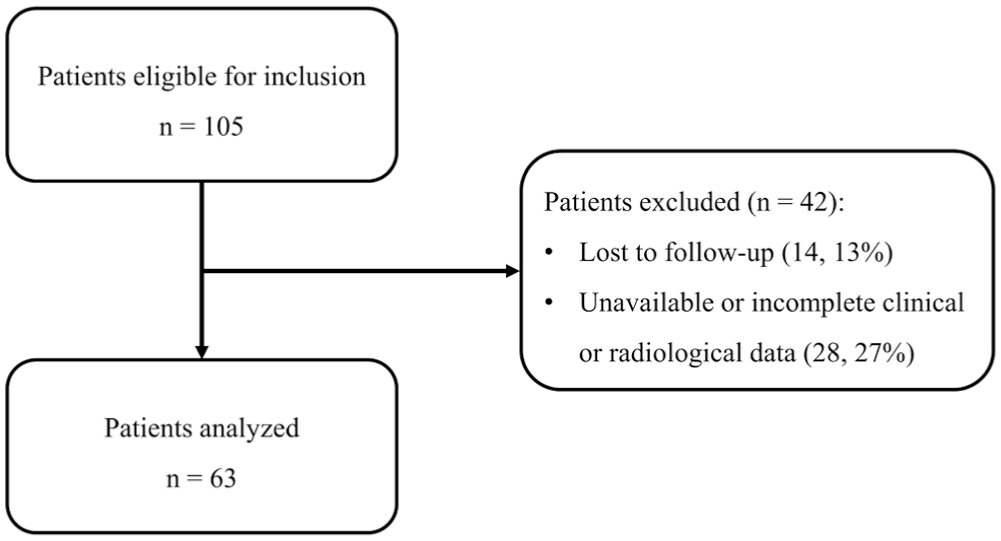
Flowchart of patient inclusion.
All procedures were performed at a single institution by the same surgical team using the arthroscopic Latarjet technique with screw fixation as previously described.25,44 Postoperatively, all patients followed the uniform and standardized rehabilitation guidelines. 44
Data Collection
Patient data, including age at surgery and at the first episode of dislocation, sex, body mass index, time from first episode to surgery, episodes of dislocation, revision surgery (failure after Bankart repair), and level of sport, were collected.
All patients were clinically assessed preoperatively and at the final follow-up (at a minimum of 5 years postoperatively). Patient-reported outcome measures were assessed using the Rowe score, American Shoulder and Elbow Surgeons (ASES) score, visual analog scale for pain (VAS) score, Constant-Murley score, and single assessment numeric evaluation (SANE) score. The evaluation of shoulder range of motion (ROM) consisted of forward flexion (FF), abduction (AB), external rotation at 0° of abduction (ER@0°), external rotation at 90° of abduction (ER@90°), internal rotation at 0° of abduction (IR@0°), and internal rotation at 90° of abduction (IR@90°). IR@0° was determined as the highest spine level that the thumb could reach on the back: 1 to 22 points for T1 to S5. 2 Because of the missing preoperative SANE score, AB, ER@90°, and IR@90° measurements, these data were excluded from the comparative analysis of preoperative versus postoperative values. The apprehension test and level and time of return to sports (RTS) 1 were also assessed.
Radiological assessments were performed via CT imaging with 3D reconstruction and radiographs preoperatively, immediately after the surgery (within 2 days), and at the final follow-up, including (1) the glenoid surface area ratio, defined as the ratio of the glenoid surface area to the best-fit circle of the inferior glenoid (glenoid bone defect was calculated as 1 minus the preoperative glenoid surface area ratio, along with the graft surface area extending beyond the best-fit circle30,31); (2) the superior-inferior and medial-lateral position of the coracoid graft 44 ; (3) bony union of the graft 17 ; (4) the screw orientation (alpha angle) 28 ; and (5) the grade, occurrence, and progression of glenohumeral osteoarthritis (OA) according to the Samilson and Prieto classification. 34
All clinical and radiological assessments were performed by 2 shoulder surgeons (P.L. and D.Z.) blinded to the surgery.
CRDL Classification System
This study proposed a refined classification system for coracoid graft resorption with 4 grades based on the axial CT scan. On the 2 slices where the 2 screws were the most visible, the coracoid graft was divided into 4 parts relative to the 2 screws: proximal-medial part, proximal-lateral part, distal-medial part, and distal-lateral part (Figure 2). 35 No resorption was defined as a condition that both the screw head and shaft were buried in the coracoid graft. Resorption was defined as a condition that only the screw head or both the screw head and shaft were exposed outside the graft. 45 The degree of graft resorption on each part was evaluated. The graft resorption was classified as follows:
Grade 0: No resorption on all 4 parts (Figure 3A),
Grade 1: Resorption on the proximal-medial and/or distal-medial parts (Figure 3B),
Grade 2: Resorption on the proximal-lateral part with no resorption on the distal-lateral part (Figure 3C), and
Grade 3: Resorption on the distal-lateral part (Figure 3D).
The grade was classified according to the highest grade when resorption occurred on multiple parts of the graft. The severity of graft resorption was categorized as mild (grades 0 and 1) or severe (grades 2 and 3). Coracoid graft resorption was classified according to both CRDL and CRD classification systems (grade 0: the screw head is buried in the coracoid bone graft; grade 1: only the screw head is exposed outside the bone graft; grade 2: part of the screw shaft is exposed outside the graft; grade 3: the screw head and shaft are both totally exposed, with all of the coracoid bone graft absorbed). 45 The incidence, classification, and location of graft resorption were analyzed.
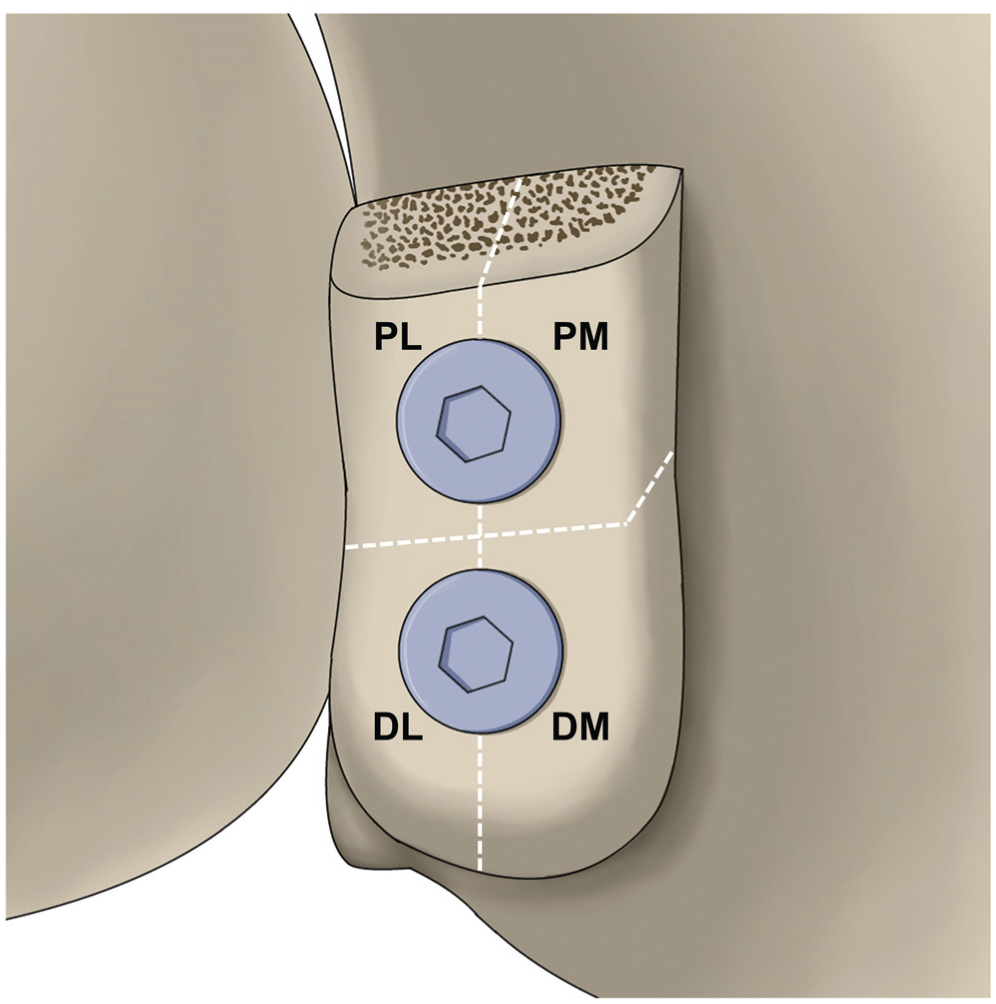
Location of coracoid graft resorption, consisting of the proximal-medial (PM) part, proximal-lateral (PL) part, distal-medial (DM) part, and distal-lateral (DL) part.
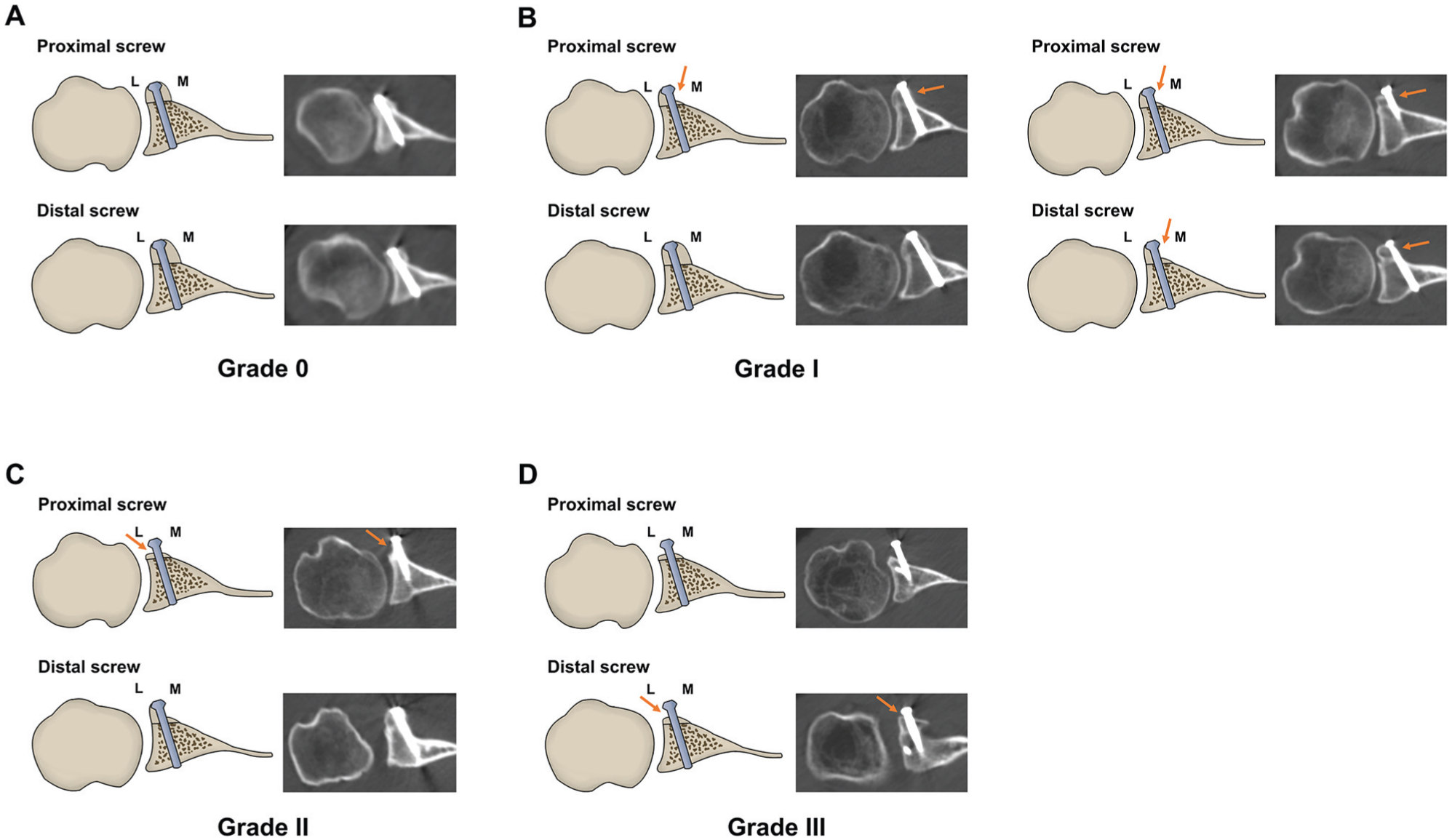
CRDL classification system for coracoid graft resorption. (A) Grade 0, no resorption occurred on the 4 parts. (B) Grade 1, resorption occurred on the proximal-medial and/or distal-medial parts. (C) Grade 2, resorption occurred on the proximal-lateral part with no resorption on the distal-lateral part. (D) Grade 3, resorption occurred on the distal-lateral part. The arrows represent the location of graft resorption. L, lateral; M, medial.
Statistical Analysis
All data were analyzed using SPSS Version 27.0 (IBM). Normal distribution was assessed using the Shapiro-Wilk test. Continuous variables are reported as mean ± standard deviation, and categorical variables are described as sample size and percentage. The paired Student t test, 1-way analysis of variance (ANOVA), Wilcoxon signed-rank test, and Friedman test were used to evaluate the intragroup differences. The independent Student t test, 1-way ANOVA, Mann-Whitney U test, and Kruskal-Wallis test were used to evaluate intergroup differences. The standard significant P value <.05 was used. The minimal clinically important difference (MCID) was determined using a distribution-based method: one-half the standard deviation of the difference between pre- and postoperative outcome scores. 24
The CRDL classification was performed by 3 observers (J.X., Z.W., and H.L.) at the same time and on the same day of the week. One observer (J.X.) performed the classification twice, 6 weeks apart. The weighted kappa (κ) and light kappa coefficients were used to calculate the intrarater and interrater reliability, respectively. The strength of agreement was categorized according to Landis and Koch 27 as follows: 0.00 to 0.20, slight; 0.21 to 0.40, fair; 0.41 to 0.60, moderate; 0.61 to 0.80, substantial; and 0.81 to 1.00, almost perfect. 27 Percent agreement was calculated for all pairs of graders.
The Spearman correlation coefficient (ρ) was used to evaluate the correlation between the grade and severity of graft resorption and clinical and radiological outcomes. According to Cohen, 5 a medium correlation is on the order of 0.30 with practical clinical significance. Univariable and multivariable regression analyses were used to identify whether the coracoid graft resorption was a risk factor for poor outcomes. In the univariable regression analysis, variables with P values <.1 were initially selected to account for potential confounders; subsequently, up to 4 variables with the smallest P values were retained for multivariable regression modeling.
A priori power analysis, using an estimated Spearman correlation coefficient of 0.40 and kappa coefficient of 0.60, found that to obtain 80% power, with an alpha level of .05, the inclusion of 51 patients was considered to be adequate.
Results
Overall Clinical and Radiological Outcomes
Patient characteristics are summarized in Table 1. The mean follow-up period for the 63 patients was 85.3 ± 14.8 months. At the final follow-up, no instances of recurrent dislocation or revision surgery were recorded. The rate of a positive apprehension test significantly declined, from 100.0% (63/63) preoperatively to 14.3% (9/63) postoperatively. The Rowe (90.1 ± 10.1 vs 40.2 ± 7.5), ASES (94.9 ± 7.7 vs 86.0 ± 12.8), and Constant-Murley (93.6 ± 4.0 vs 84.6 ± 9.0) scores were significantly improved postoperatively compared with preoperatively (P < .001 for all), and all achieved the MCID (Rowe score: 6.2; ASES score: 7.1; Constant-Murley score: 4.2). The VAS score was significantly increased without achieving the MCID (0.9 ± 1.5 postoperatively vs 0.4 ± 1.6 preoperatively; P = .011; MCID, 1.0). Postoperative ER@0° was significantly smaller than the preoperative value (55.0 ± 12.0 vs 58.3 ± 8.4; P = .045). No significant differences were found between pre- and postoperative values in FF and IR@0°. All patients returned to sports at 9.2 ± 6.7 months after surgery, and 41 (65.1%) cases returned at the same or higher level (Appendix Table A1, available in the online version of this article).
Patient Characteristics a
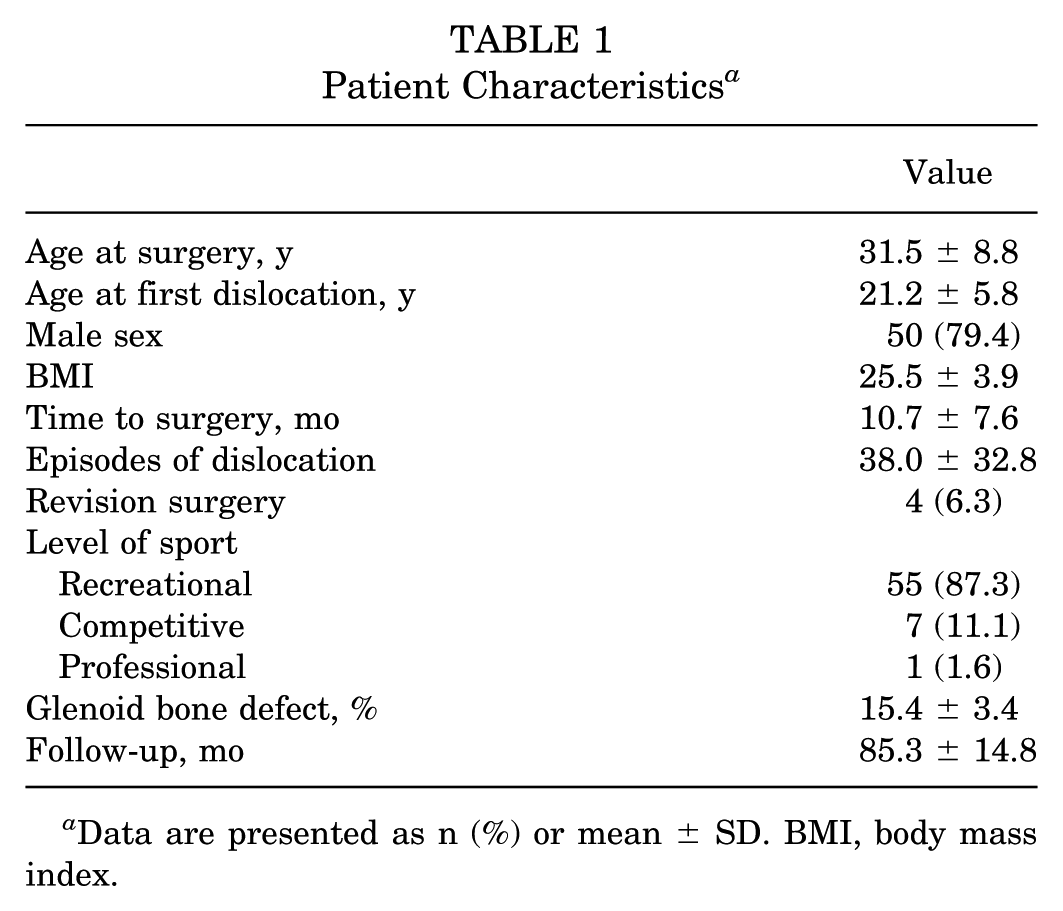
Data are presented as n (%) or mean ± SD. BMI, body mass index.
The coracoid graft was positioned flush with the glenoid surface medially-laterally in 59 (93.7%) shoulders and appropriate (below the equator) superiorly-inferiorly in 47 (74.6%) shoulders. The orientation of the screw was 26.5°± 9.1° superiorly and 28.7°± 10.1° inferiorly. Bony union was achieved in 98.4% (62/63) of the cases. The incidence of OA was 3.2% (2/63) preoperatively and 20.6% (13/63) at a mean follow-up of 7 years, and most cases were grade 1. Eleven (17.5%) cases showed signs of OA progression on the radiographs. Preoperative en face CT scans demonstrated that the affected glenoid occupied 84.6% ± 3.4% of the best-fit circle area, corresponding to a glenoid bone defect of 15.4% ± 3.4%. This value increased significantly to 126.3% ± 11.1% immediately after the surgery, indicating surgical overcorrection. However, a significant decrease to 108.0% ± 3.7% was observed at the final follow-up, attributable to resorption of the transferred coracoid graft. Furthermore, the graft surface area extending beyond the best-fit circle—initially 29.4% ± 9.6% of the circle’s area immediately after the surgery—declined significantly to 9.3% ± 2.7% at the final follow-up, indicating that bone resorption occurred predominantly outside this region (Appendix Table A2, available online).
Coracoid Graft Resorption Evaluation Using CRD and CRDL Classification Systems
At the final follow-up, the incidence of coracoid graft resorption was 84.1% (53/63) based on the CRD classification system. The graft resorption was classified as grade 0 in 10 (15.9%) patients, grade 1 in 7 (11.1%), grade 2 in 37 (58.7%), and grade 3 in 9 (14.3%). Minor and major graft resorption were found in 17 (27.0%) and 46 (73.0%) patients, respectively. The graft resorption mainly occurred on the proximal part of the graft (84.1% [53/63]) (Appendix Table A3, available online).
According to the CRDL classification system, the incidence of graft resorption was 84.1% (53/63), with grade 0 in 15.9% (10/63), grade 1 in 47.6% (30/63), grade 2 in 30.2% (19/63), and grade 3 in 6.3% (4/63). The severity of graft resorption was mild in 63.5% (40/63) and severe in 36.5% (23/63) of the cases. The graft resorption mainly occurred on the proximal-medial part of the graft (81.0% [51/63]), followed by the proximal-lateral part (34.9% [22/63]), distal-medial part (25.4% [16/63]), and distal-lateral part (6.3% [4/63]) (Appendix Table A4, available online).
The CRDL classification system demonstrated almost perfect intrarater (κ = 0.865; 95% CI, 0.766-0.963; P < .001) and interrater (κ = 0.822; 95% CI, 0.753-0.891; P < .001) reliability, with percentage agreements of 88.9% and 86.2%, respectively.
Correlation Between Classification for Graft Resorption and Clinical and Radiological Outcomes
There were no significant differences in clinical and radiological outcomes among graft resorption grades based on the CRD classification system preoperatively and at the final follow-up (Appendix Table A5, available online).
According to the CRDL classification system, the postoperative ASES score (P < .001) and VAS score (P < .001) significantly differed among graft resorption grades (Table 2). Pairwise comparisons revealed that patients with grade 3 had significantly lower ASES scores (80.8 ± 14.6) and higher VAS scores (3.5 ± 3.1) than those with grade 0 (ASES score: 97.2 ± 3.9, P = .049; VAS score: 0.4 ± 0.7, P = .025) and grade 1 (ASES score: 98.2 ± 3.3, P = .004; VAS score: 0.3 ± 0.6, P = .004). Additionally, patients with grade 2 showed significantly lower ASES scores and higher VAS scores than those with grade 1 (ASES score: 91.7 ± 8.3 vs 98.2 ± 3.3, P = .006; VAS score: 1.5 ± 1.6 vs 0.3 ± 0.6, P = .006) (Figure 4). No significant differences in the Rowe score, Constant-Murley score, apprehension test, SANE score, ROM, RTS level, or OA occurrence and progression were observed among different graft resorption grades (Table 2).
Differences in Clinical and Radiological Outcomes Among Graft Resorption Grades According to CRDL Classification System a
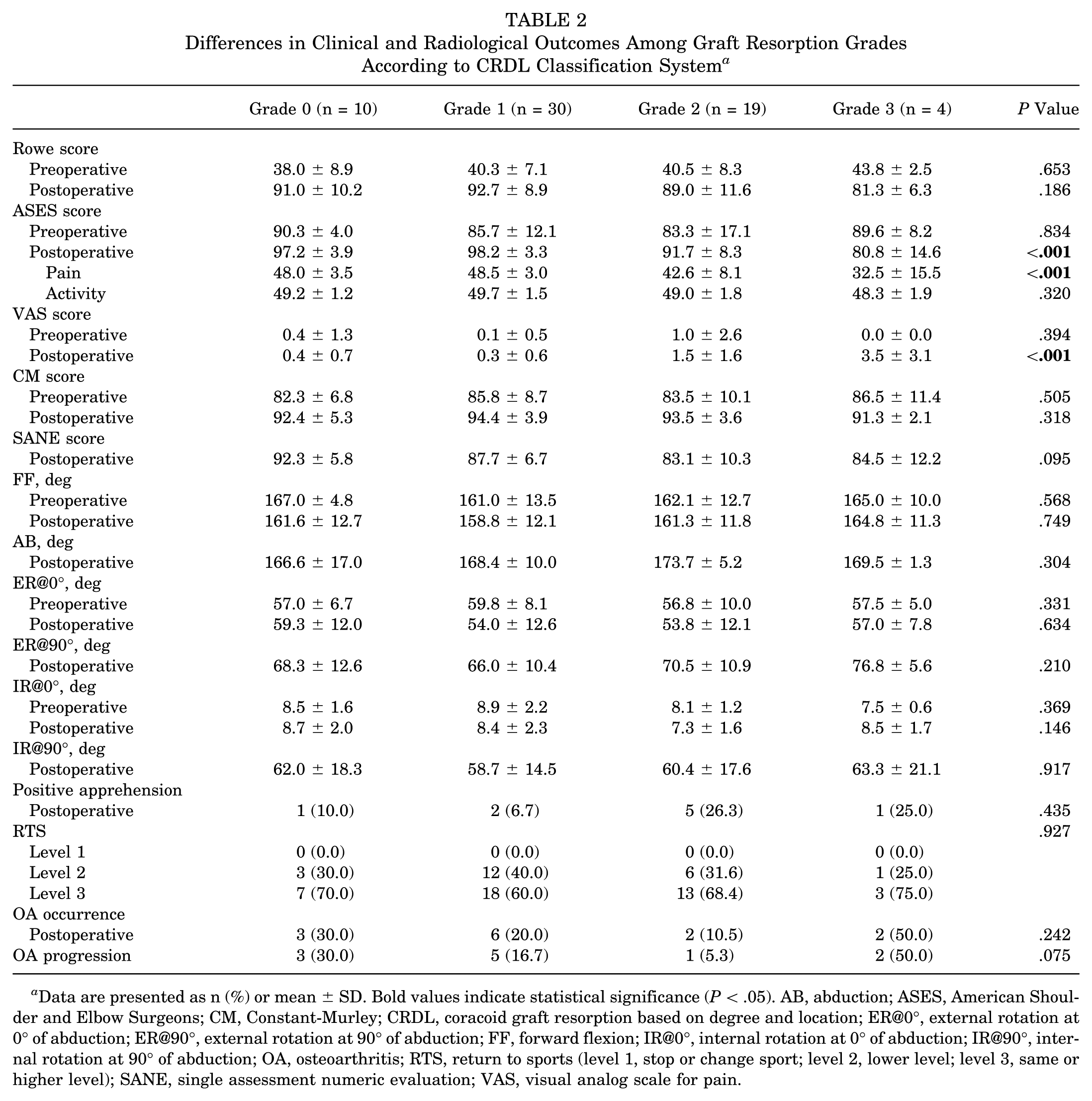
Data are presented as n (%) or mean ± SD. Bold values indicate statistical significance (P < .05). AB, abduction; ASES, American Shoulder and Elbow Surgeons; CM, Constant-Murley; CRDL, coracoid graft resorption based on degree and location; ER@0°, external rotation at 0° of abduction; ER@90°, external rotation at 90° of abduction; FF, forward flexion; IR@0°, internal rotation at 0° of abduction; IR@90°, internal rotation at 90° of abduction; OA, osteoarthritis; RTS, return to sports (level 1, stop or change sport; level 2, lower level; level 3, same or higher level); SANE, single assessment numeric evaluation; VAS, visual analog scale for pain.
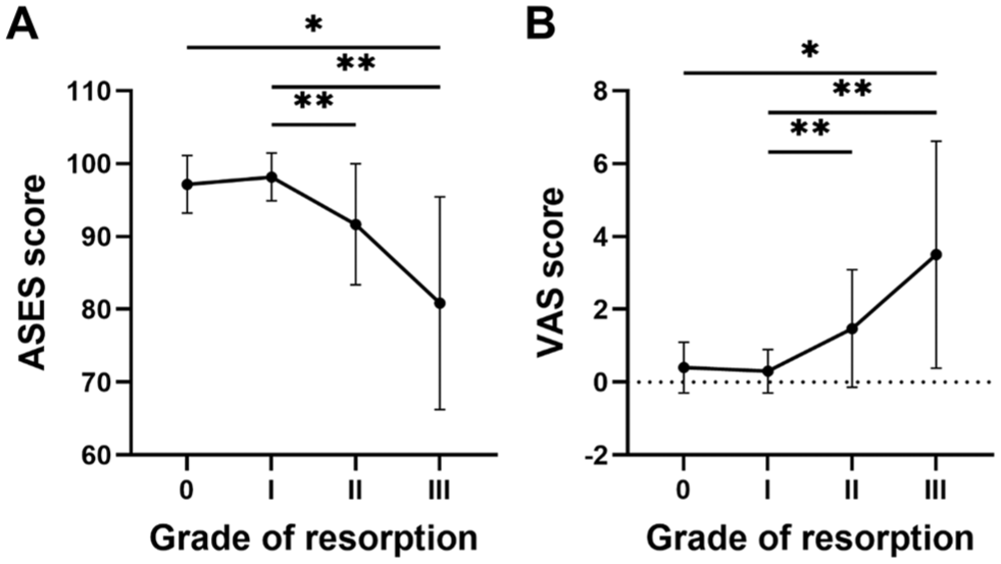
Pairwise comparisons of postoperative American Shoulder and Elbow Surgeons (ASES) and visual analog scale for pain (VAS) scores among graft resorption grades (coracoid graft resorption based on degree and location classification system). (A) Grade 3 had significantly lower ASES scores than grade 0 and grade 1; grade 2 had significantly lower ASES scores than grade 1. (B) Grade 3 had significantly higher VAS scores than grade 0 and grade 1; grade 2 had significantly higher VAS scores than grade 1. *P < .05; **P < .01.
Similarly, patients with severe graft resorption exhibited significantly lower ASES scores (89.8 ± 10.1 vs 97.9 ± 3.4; P < .001) and higher VAS scores (1.8 ± 2.0 vs 0.3 ± 0.6; P < .001) postoperatively than those with mild resorption. Other outcomes did not significantly differ between the 2 groups (Table 3).
Differences in Clinical and Radiological Outcomes Between Mild and Severe Graft Resorption According to CRDL Classification System a
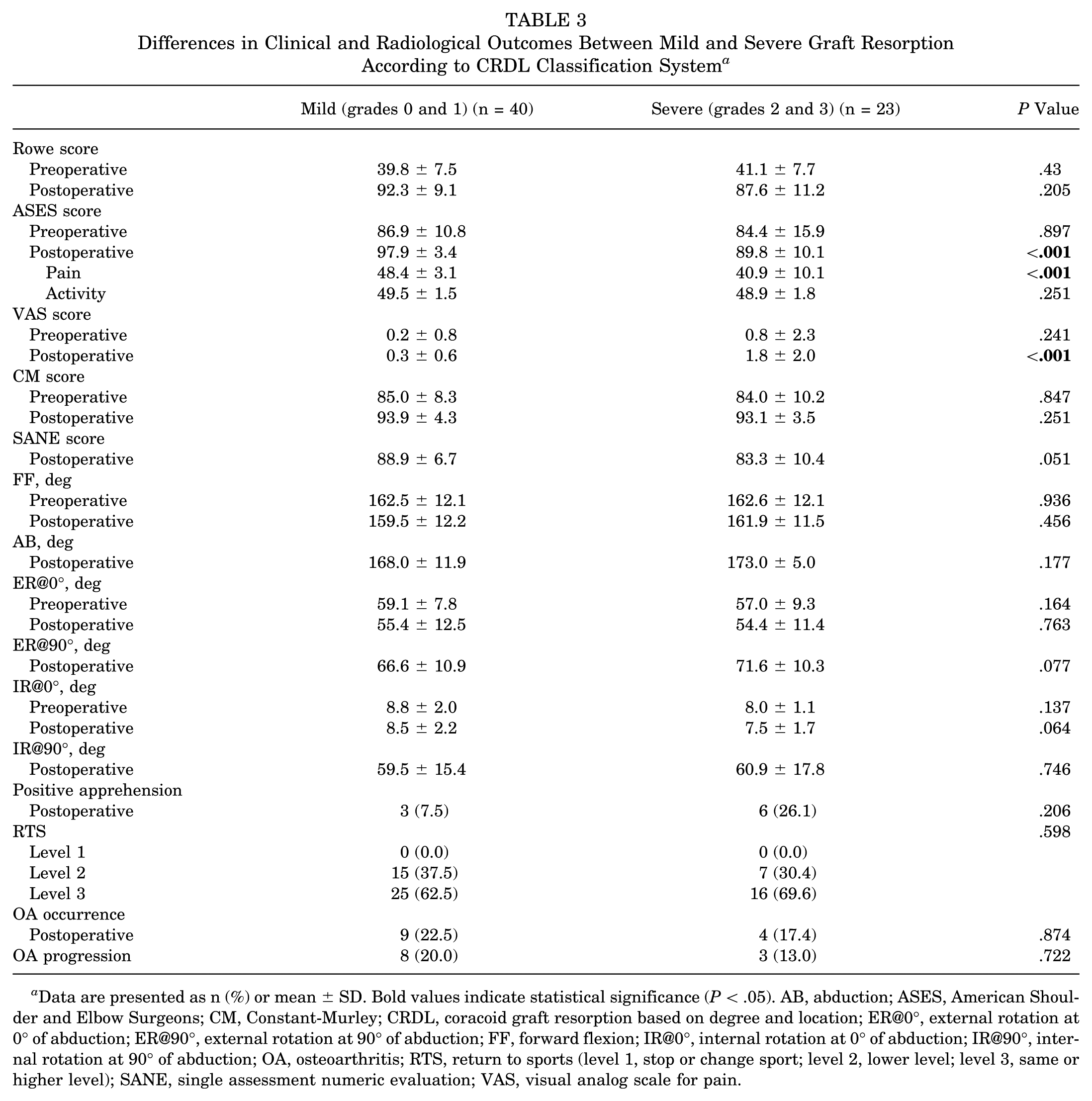
Data are presented as n (%) or mean ± SD. Bold values indicate statistical significance (P < .05). AB, abduction; ASES, American Shoulder and Elbow Surgeons; CM, Constant-Murley; CRDL, coracoid graft resorption based on degree and location; ER@0°, external rotation at 0° of abduction; ER@90°, external rotation at 90° of abduction; FF, forward flexion; IR@0°, internal rotation at 0° of abduction; IR@90°, internal rotation at 90° of abduction; OA, osteoarthritis; RTS, return to sports (level 1, stop or change sport; level 2, lower level; level 3, same or higher level); SANE, single assessment numeric evaluation; VAS, visual analog scale for pain.
All significant differences in the ASES and VAS scores achieved the MCID (7.1 for ASES score; 1.0 for VAS score), except for the difference in ASES scores between grade 2 and grade 1.
Given that the ASES score consists of 50 points from the VAS subscale and 50 points from the functional subscale, the significant differences in ASES scores among patients with varying degrees of coracoid graft resorption may be attributable to differences in the pain component. Therefore, the ASES score was further broken down into its pain and functional components for separate comparisons. The results confirmed that the significant differences in ASES scores were primarily driven by the pain subscale (grade 0 vs 1 vs 2 vs 3: 48.0 ± 3.5 vs 48.5 ± 3.0 vs 42.6 ± 8.1 vs 32.5 ± 15.5, P < .001; mild vs severe: 48.4 ± 3.1 vs 40.9 ± 10.1, P < .001), whereas differences in the functional subscale were not statistically significant (Tables 2 and 3).
The Spearman correlation analysis revealed that the grade of graft resorption was significantly negatively correlated with the ASES score (ρ = −0.450; P < .001) and positively correlated with the VAS score (ρ = 0.484; P < .001). Similarly, the severity of graft resorption was significantly negatively correlated with the ASES score (ρ = −0.507; P < .001) and positively correlated with the VAS score (ρ = 0.524; P < .001). No significant correlations were found between graft resorption and the Rowe score, Constant-Murley score, apprehension test, SANE score, ROM, RTS, or OA occurrence and progression (Table 4).
Correlation Between Graft Resorption and Postoperative Outcomes a
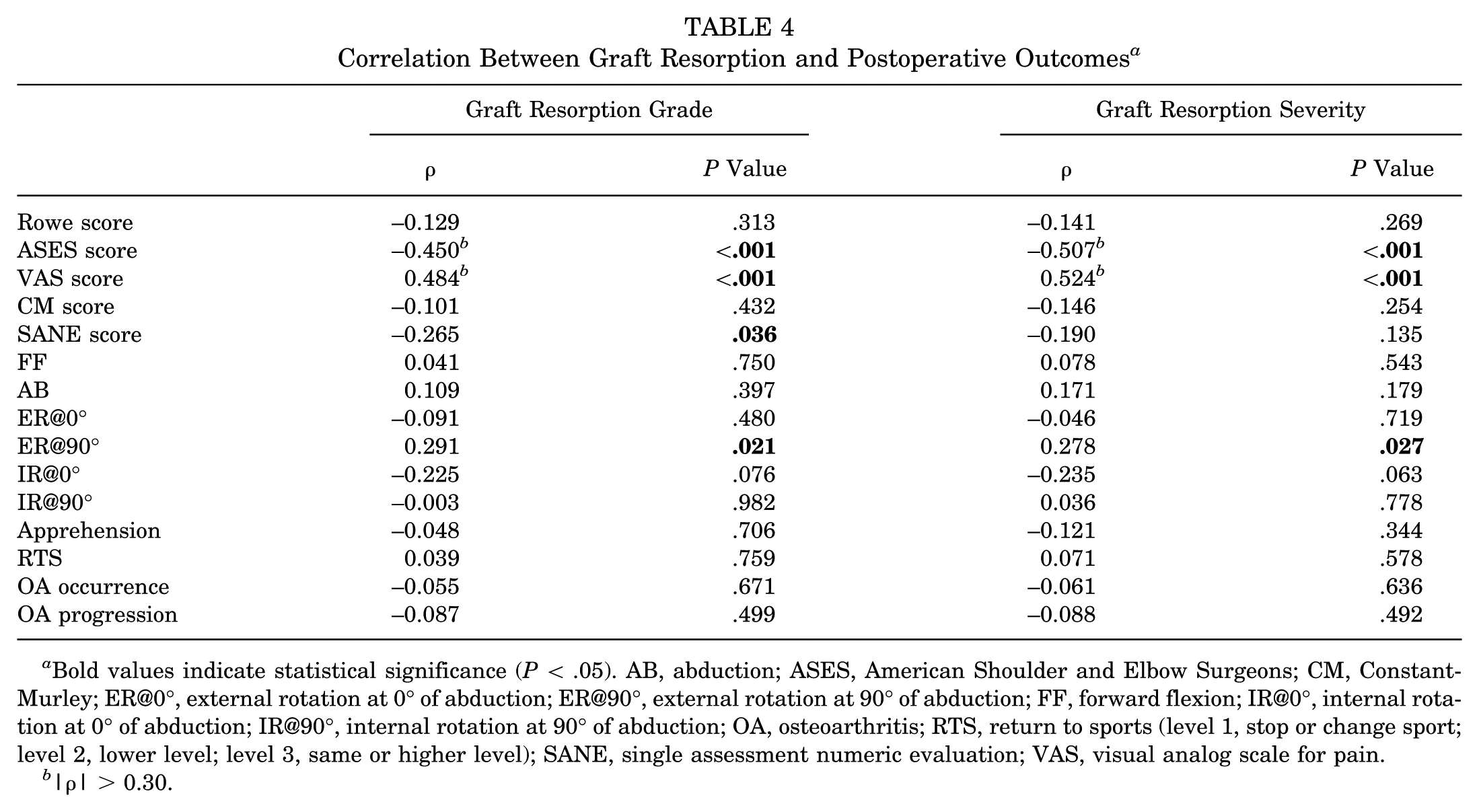
Bold values indicate statistical significance (P < .05). AB, abduction; ASES, American Shoulder and Elbow Surgeons; CM, Constant-Murley; ER@0°, external rotation at 0° of abduction; ER@90°, external rotation at 90° of abduction; FF, forward flexion; IR@0°, internal rotation at 0° of abduction; IR@90°, internal rotation at 90° of abduction; OA, osteoarthritis; RTS, return to sports (level 1, stop or change sport; level 2, lower level; level 3, same or higher level); SANE, single assessment numeric evaluation; VAS, visual analog scale for pain.
|ρ| > 0.30.
After the univariable regression analysis, age at surgery, age at first dislocation, BMI, episodes of dislocation, revision surgery, level of sport, level of RTS, glenoid bone defect, graft position, screw orientation, and occurrence and progression of OA were excluded from multivariable regression modeling (P≥ .1 for all). The grade and severity of graft resorption, time to surgery, and sex were finally retained for assessing risk factors associated with the ASES and VAS scores. The adjusted multivariable regression analysis revealed that grade 2 (B = −5.220; P = .043), grade 3 (B = −15.804; P < .001), and severe graft resorption (B = −6.692; P < .001) were significant negative predictors of the postoperative ASES score. Conversely, these 3 variables served as significant positive predictors of the postoperative VAS score (grade 2: B = 1.017, P = .045; grade 3: B = 2.993, P < .001; severe graft resorption: B = 1.255, P = .002). No significant associations were found for other variables (Tables 5 and 6).
Multivariable Regression Analysis of Risk Factors for ASES and VAS Scores (Resorption Grade) a
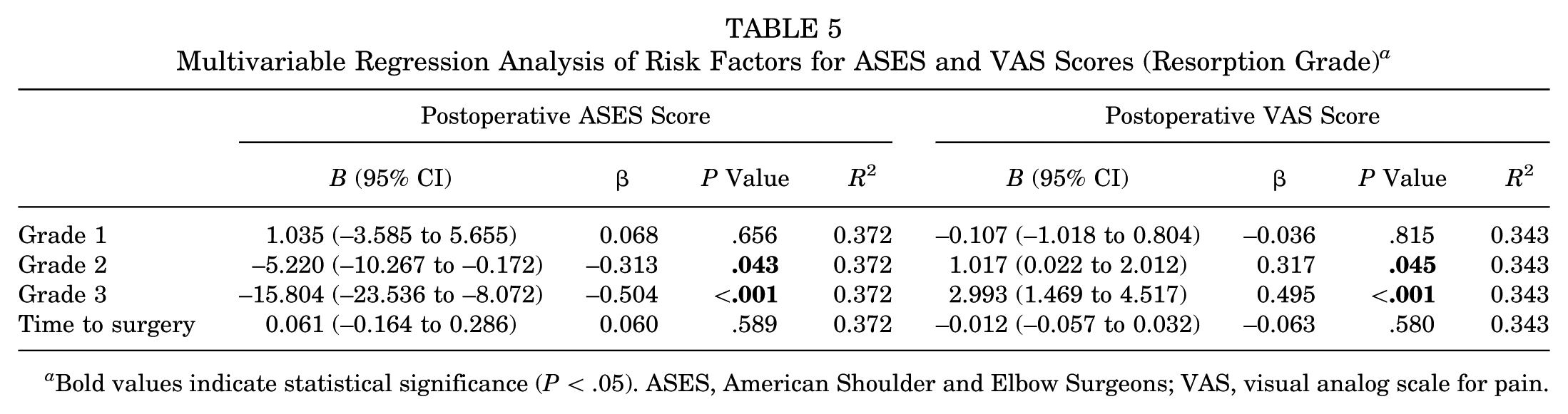
Bold values indicate statistical significance (P < .05). ASES, American Shoulder and Elbow Surgeons; VAS, visual analog scale for pain.
Multivariable Regression Analysis of Risk Factors for ASES and VAS Scores (Resorption Severity) a
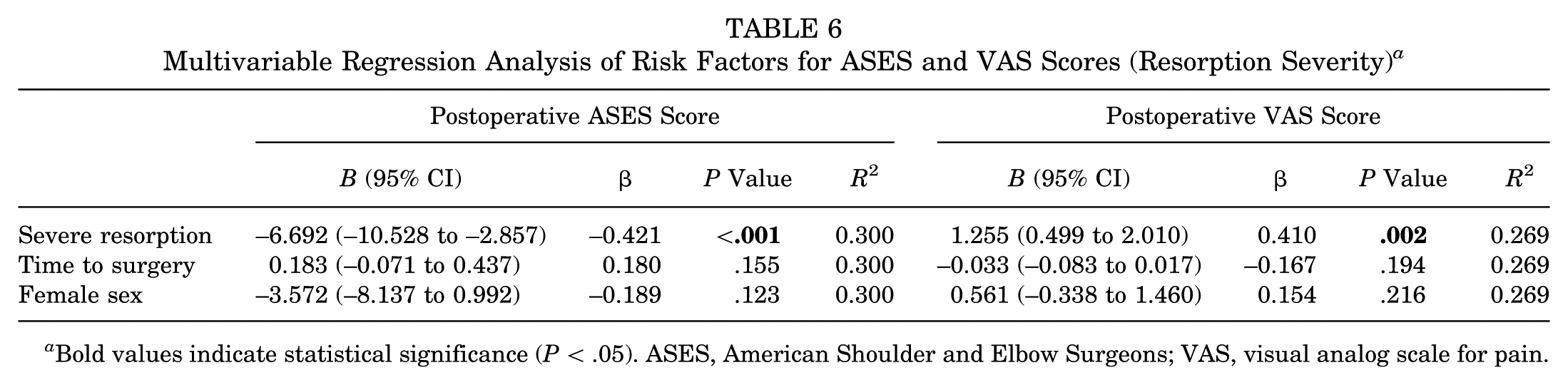
Bold values indicate statistical significance (P < .05). ASES, American Shoulder and Elbow Surgeons; VAS, visual analog scale for pain.
Correlation Between Preoperative Glenoid Bone Defect and Graft Resorption
No significant intergroup differences in preoperative glenoid bone defect size were observed, either across the CRDL coracoid graft resorption grades (grade 0: 16.2% ± 3.7%; grade 1: 15.8% ± 3.5%; grade 2: 14.8% ± 2.9%; grade 3: 12.6% ± 2.5%; P = .107) or between the mild (15.9% ± 3.5%) and severe (14.4% ± 2.9%) resorption categories (P = .050). Similarly, no significant correlation was found between the defect size and CRDL grade (ρ = −0.269; P = .033) or severity level (ρ = −0.248; P = .050).
Discussion
The key finding of this study is the establishment of a refined, reliable, and clinically relevant classification system for coracoid graft resorption—the CRDL (based on degree and location) classification. Application of the CRDL system revealed that while high-grade resorption is a significant risk factor for postoperative shoulder pain, it has no major impact on shoulder function or stability.
Coracoid graft resorption is a common complication after the Latarjet procedure with a high incidence.4,20,23,37 Most studies have suggested that graft resorption does not significantly affect clinical outcomes.8,10,21,45 Nevertheless, graft resorption has gained attention because it may give rise to shoulder pain (screw–subscapularis/humeral head impingement), humeral head chondral lesions (screw–humeral head impingement), and recurrent dislocation (absence of bony effect). 29 In the current patient series, graft resorption was found to occur only on the medial part or both the medial and lateral parts of the graft. The graft resorption limited to the medial part would not compromise clinical outcome, because the intact lateral portion of the graft would protect the screw from exposure to the humeral head. On the contrary, the graft resorption on the lateral part would likely lead to the symptoms mentioned above. Therefore, this study speculated that not only the degree but also the location could contribute to the clinical impact of graft resorption.
The degree and location of coracoid graft resorption have been evaluated by several studies to determine its clinical acceptability. Di Giacomo et al 8 first quantified and localized graft resorption using CT scans, reporting that the extensive graft resorption was not of any great clinical significance in terms of pain or recurrent dislocation. Although they divided the graft into 8 parts, the correlation between resorption location and clinical outcome was not investigated. And their method was too complicated to be widely used. We subsequently proposed a reliable and simple classification system—CRD—that graded the severity of graft resorption by semiquantifying the resorption around the screws. 45 However, the CRD classification system did not take resorption location into consideration and showed no significant correlation with functional outcomes.32,36,44,45 Recently, some studies have tried to accurately quantify the graft resorption degree by measuring the volume of the graft,6,11 and several authors have simply classified the graft resorption as partial or total,4,23 but they still have not identified the clinical impact of graft resorption. Therefore, the current evaluation and classification methods merely focusing on the resorption degree may conceal the influence of the resorption location, limiting the understanding of the clinical impact of graft resorption.
By combining the degree with location, the graft resorption was classified into 4 grades in the CRDL classification system. Consistent with previous studies11,37 and results based on the CRD classification, the CRDL classification system showed a high incidence of graft resorption (84.1%). It was also found that the graft resorption mainly occurred on the proximal and medial parts of the graft, as reported in other studies.8,16 Most cases classified as grade 2 (major) under the CRD system were categorized as grade 1 (mild) under the CRDL system. This discrepancy arises from their differing criteria: the CRD system emphasizes the degree of screw exposure, whereas the CRDL system emphasizes resorption location. In this study, although partial screw exposure (qualifying as CRD grade 2) was common, the exposed area was typically confined to the medial portion of the graft, corresponding to CRDL grade 1. Consequently, the incidence of severe resorption was lower under the CRDL classification. Furthermore, the CRDL classification system demonstrated almost perfect reliability, with intra- and interrater values of 0.865 and 0.822, respectively, and a high percentage agreement. This high reliability, which is comparable to that of the previously published CRD classification (0.898 and 0.856), 45 indicates that graft resorption can be reliably identified and classified using the CRDL system.
According to the CRD classification system, graft resorption did not significantly affect clinical outcomes. In contrast, the CRDL classification system identified high-grade and severe graft resorption as independent risk factors for poorer ASES scores and higher VAS scores. Further analysis, which divided the ASES score into its pain and functional subscales, confirmed that the observed differences in ASES scores across resorption grades were primarily attributable to the pain subscale. These findings suggest that patients with more advanced graft resorption are more likely to experience shoulder pain after the Latarjet procedure.
Several studies have pointed out that the screw exposure caused by graft resorption can lead to shoulder pain due to the impingement between the screws and subscapularis or humeral head.13,22,26 In the present study, resorption confined to the medial part (grade 1) did not appear to cause shoulder pain, regardless of its degree. In contrast, lateral resorption (grades 2 and 3), which exposes the lateral portion of the screw, was strongly associated with shoulder pain. Affected patients often reported pain or discomfort during shoulder AB and ER, although none required revision surgery. Given the high proportion of graft resorption limited to the medial part, pooling it with lateral graft resorption into a single category may obscure the true impact of lateral graft resorption, which potentially explains why the CRD classification system and other studies have failed to identify the clinical impact of graft resorption. Therefore, it is rational and necessary to classify the graft resorption based on both the resorption degree and medial-lateral resorption location.
Moreover, the distal-lateral graft resorption (grade 3) showed a lower ASES score and higher VAS score compared with the proximal-lateral graft resorption (grade 2), although no significant differences were found due to the small sample size in grade 3. This may be because the relationship between the humeral head and the coracoid graft is mostly on the distal part of the graft, 26 resulting in more impingement between the humeral head and the distal screw in grade 3. Therefore, the proximal-distal resorption location on the lateral part of the graft is also significant for clinical outcomes, but it needs to be further investigated with a larger sample size.
Despite a 14.3% rate of a positive apprehension test in this study, no recurrent dislocations occurred postoperatively. This can be attributed to 2 main factors. First, the graft’s structural integrity was largely preserved: most grafts achieved bony union without hardware failure or migration, and no case of complete resorption was observed, indicating that its essential bony effect was maintained. Second, even in cases of partial resorption, the sling effect of the conjoined tendon was likely to provide substantial stability, as supported by previous literature.12,43 This also explains why, in the present cohort, the resorption classification showed no significant association with the apprehension test or the Rowe score, which primarily assesses stability. Furthermore, the absence of significant differences in the ROM, Constant-Murley score, and RTS rates across different resorption grades demonstrates that coracoid resorption has no substantial impact on functional outcomes after the arthroscopic Latarjet procedure.
Graft resorption has been suggested to contribute to OA due to impingement between the screw and humeral head. 29 Although the present study found no association between graft resorption and OA, 50% (2/4) of patients in the grade 3 group had postoperative OA and OA progression. The short period of follow-up and small sample size of patients with high-grade graft resorption may have limited the statistical power of the correlation analysis. Patients with grade 3 graft resorption showed the highest OA incidence (50%) as well as the highest pain scores; however, regression analysis revealed no significant correlation between OA and pain. Therefore, the differences in pain scores among different graft resorption grades seem to be unrelated to OA.
Regarding the potential mechanism of bone resorption, numerous studies have suggested that the absence of biomechanical stimulation may be a contributing factor.7,9,21,35 Hachem et al, 15 in a recent study monitoring patients treated with arthroscopic iliac crest bone graft, reported that graft resorption primarily occurred outside the best-fit circle. A similar pattern was observed in this study: the glenoid surface area significantly decreased from 126.3% ± 11.1% immediately after the surgery to 108.0% ± 3.7% at the final follow-up due to bone resorption. Furthermore, resorption was found predominantly outside the best-fit circle. Di Giacomo et al 9 found that graft resorption was significantly associated with the absence of preoperative glenoid bone defects. They proposed that patients without bone defects have a larger area of the bone graft lacking mechanical stimulation compared with those with critical bone defects, thus leading to more significant bone resorption. However, consistent with the other 2 studies,6,33 the present study found no clinically significant correlation between the preoperative glenoid bone defect and graft resorption.
Since exposed fixation screws can cause postoperative pain and resorption outside the best-fit circle is often unavoidable, using a graft size individualized to the bone defect represents a rational strategy. This approach is particularly practical when using an allograft to address glenoid bone defect, as demonstrated in the study by Dawe et al. 7 In the Latarjet procedure, however, the limited ability to alter the dimensions of the coracoid graft precludes its practical application. In addition to mechanical impingement, local inflammation resulting from screw prominence—due to soft tissue irritation and metal ion release—can also contribute to shoulder pain. 40 Another alternative strategy to prevent screw-related irritation is the use of nonrigid fixation (suture buttons and suture anchors)3,38 or metal-free fixation (suture tape cerclage) techniques. 14 Nevertheless, the substantially different biomechanical properties of these alternative fixation methods necessitate further investigation to assess whether they might introduce new clinical complications.
Limitations
Some limitations still existed in the present study. First, the sample size of patients with grade 3 graft resorption was small, limiting the power of statistical analysis. Second, subgroup analysis of graft resorption degree was not performed for patients with grade 2 and grade 3 resorption, which limited the comprehensive understanding of high-grade graft resorption and resorption in the anterior-posterior plane. Future studies should enroll a larger number of patients with grade 2 and grade 3 graft resorption. Third, this study did not investigate the risk factors for the occurrence and severity of coracoid graft resorption, which will be analyzed in future research.
Conclusion
The refined classification system—CRDL—is a reliable and clinically relevant classification system for coracoid graft resorption evaluation. Application of the CRDL system reveals that while high-grade resorption is a significant risk factor for postoperative shoulder pain, it has no major impact on shoulder function or stability.
Supplemental Material
sj-docx-1-ajs-10.1177_03635465251408095 – Supplemental material for Impact of Significant Coracoid Graft Resorption on Clinical Outcomes After Arthroscopic Latarjet Procedure: Development and Validation of a Refined Classification System for Coracoid Bone Graft Resorption
Supplemental material, sj-docx-1-ajs-10.1177_03635465251408095 for Impact of Significant Coracoid Graft Resorption on Clinical Outcomes After Arthroscopic Latarjet Procedure: Development and Validation of a Refined Classification System for Coracoid Bone Graft Resorption by Qihuang Qin, Pinxue Li, Dan Zhang, Jianhao Xie, Zeyu Wang, Haoyue Li, Siyi Guo, Chunyan Jiang and Yiming Zhu in The American Journal of Sports Medicine
Supplemental Material
sj-docx-2-ajs-10.1177_03635465251408095 – Supplemental material for Impact of Significant Coracoid Graft Resorption on Clinical Outcomes After Arthroscopic Latarjet Procedure: Development and Validation of a Refined Classification System for Coracoid Bone Graft Resorption
Supplemental material, sj-docx-2-ajs-10.1177_03635465251408095 for Impact of Significant Coracoid Graft Resorption on Clinical Outcomes After Arthroscopic Latarjet Procedure: Development and Validation of a Refined Classification System for Coracoid Bone Graft Resorption by Qihuang Qin, Pinxue Li, Dan Zhang, Jianhao Xie, Zeyu Wang, Haoyue Li, Siyi Guo, Chunyan Jiang and Yiming Zhu in The American Journal of Sports Medicine
Footnotes
Submitted July 29, 2025; accepted December 1, 2025.
One or more of the authors has declared the following potential conflict of interest or source of funding: This study was funded by the National Natural Science Foundation of China (82372494) and the Natural Science Foundation of Beijing (7254371). AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
