Abstract
Background:
The medial patellofemoral ligament (MPFL) serves as a major stabilizer in the knee, providing restraint against lateral patellar translation. The optimal approach for treating patients with first-time MPFL injuries remains uncertain, as the choice between operative and nonoperative treatment depends on the risks and variability associated with individual patient anatomy, activity, and presentation.
Purpose:
To evaluate high-level literature on outcomes after operative and nonoperative treatment of MPFL injuries to guide decision-making.
Study Design:
Meta-analysis; Level of evidence, 1.
Methods:
This systematic review and meta-analysis utilized PubMed, CINAHL, MEDLINE, Web of Science, and SPORTDiscus through November 25, 2024, to find randomized controlled trials that assess the outcomes associated with operative versus nonoperative treatment for MPFL tears. The primary outcomes were rates of recurrent dislocation and patient-reported outcomes. Statistical analysis included relative risk (RR) with 95% confidence intervals (95% CIs) along with trial sequential analysis (TSA) and assessment of fragility index.
Results:
A total of 306 patients (55.9% female) had a frequency-weighted mean ± SD age of 19.68 ± 4.24 years (range, 9-40) and follow-up time of 21.61 ± 5.34 months and underwent nonoperative (n = 147) or operative (n = 159) treatment. When compared with nonoperative treatment, operative treatment had a significantly lower rate of recurrent instability (10.69% vs 29.93%; RR, 2.49; 95% CI, 1.34-4.61; P = .004) with robust evidence (fragility index, 7 patients) but no difference in Kujala scores (79.02 ± 10.71 vs 88.78 ± 2.91; overall mean difference, –9.32; 95% CI, –19.45 to 0.81; P = .071). Subgroup analysis showed that repair had a significantly lower rate of recurrent instability as compared with nonoperative treatment (15.74% vs 35.42%; RR, 1.87; 95% CI, 1.11-3.17; P = .019). Similarly, reconstruction showed a significantly lower rate of recurrent instability as compared with nonoperative treatment (3.92% vs 33.33%; RR, 6.80; 95% CI, 1.93-23.95; P = .003). TSA for all primary outcomes demonstrated that the Z curve did not cross the required information size, suggesting that the current volume of data is not sufficient to draw definitive conclusions for each comparison.
Conclusion:
Operative treatment of MPFL injuries resulted in a robust and significantly lower rate of recurrent instability when compared with nonoperative treatment, although there was no difference in Kujala scores. Given the current evidence, operative treatment appears to be the more ideal approach to treating first-time patellar dislocations. However, the key to these findings is the need for further studies, as TSA showed that the current level of evidence is insufficient to draw definitive conclusions.
The medial patellofemoral ligament (MPFL) serves as a major stabilizer in the knee, providing restraint against lateral patellar translation.8,16,24 Injury to the MPFL is associated with patellar dislocation or subluxation.2,4,7,13,26 MPFL tears typically occur in younger athletes and can result in recurrent instability, chronic knee pain, and functional limitations.12,24,40 Management of these injuries can be approached through either surgical or nonsurgical means, each with distinct outcomes and implications, which creates unclear indications for the optimal mode of treatment.
Patellofemoral articulation is complex, with many variables influencing the potential for first-time dislocation and recurrent instability, including containment of the patella, trochlear dysplasia, and patella alta.27,38 Previous studies have attempted to quantify measurements that are associated with patellar dislocation, such as tibial tubercle–trochlear groove distance and the amount of patellar tendon lateral to the lateral trochlear ridge, to better predict risk of patellar instability.27,38 Such attempts to identify anatomic risk factors for recurrent instability have been done in hopes of better determining optimal initial management based on the risk of recurrence.
Surgical treatment, primarily MPFL reconstruction, provides favorable outcomes, with 84.1% to 92.8% of patients returning to athletic activity.25,31,34 However, the incidence of complications after reconstruction ranges from 0% to 32.3% and includes patellar fractures, knee stiffness, and persistent anterior knee pain, which may affect recovery time and knee function.18,29,35 Although this can be mitigated by nonsurgical approaches, which offer lower cost and do not carry the risk of postoperative complications, studies have nonetheless demonstrated increased recurrence of dislocation, worse functional outcomes, and increased long-term instability with nonoperative approaches.5,10,19,22,41 Patients with recurrent patellar dislocation typically require operative treatment.
A systematic review by Hurley et al 17 compared outcomes after MPFL reconstruction, MPFL repair, and nonoperative treatment for patellar instability. While such studies have addressed this topic, our study incorporates trial sequential analysis (TSA) and an assessment of the fragility index (FI) to evaluate the robustness of the evidence and to provide an updated synthesis of the data to inform surgical decision making. The aim of our study is to analyze the existing randomized controlled trials (RCTs) that examine outcomes after operative and nonoperative treatments for this specific pathology. Our goal is to provide clear benefits and pitfalls of operative versus nonoperative management, while identifying areas for future research to improve care.
Methods
Study Creation and Initial Search
We performed a systematic review of RCTs comparing operative and nonoperative treatment of MPFL injury. All RCTs regarding MPFL were searched in PubMed, Cumulated Index in Nursing and Allied Health Literature, Medical Literature Analysis and Retrieval System Online, Web of Science, and SPORTDiscus from database inception until September 18, 2024. Search terms used in each database were as follows: (randomized) AND (nonoperative OR rehabilitation OR “physical therapy” OR brace OR bracing OR rehab OR nonoperative) AND (“medial patellofemoral” OR “patella dislocation” OR “patellar dislocation” OR MPFL). Guidelines of the most recent PRIMSA (Preferred Reporting Items for Systematic Reviews and Meta-analyses) were used for appropriate data reporting for this study. The study registration can be found within the PROSPERO registry at CRD42024592259.
Inclusion and Exclusion Criteria
Inclusion criteria were RCTs that compared any operative and nonoperative treatment of patients with MPFL injury. Exclusion criteria were nonrandomized studies, studies without MPFL injuries, studies not in English, and studies not comparing outcomes of operative and nonoperative treatment.
Article Screening Process
After the search algorithm was executed in each of the 5 databases for the initial search, all articles were uploaded into Rayyan, a public website used for systematic reviews. 28 One individual screener manually removed duplicates of articles and then performed article screening by title and abstract, followed by full-text screening based on inclusion and exclusion criteria. Last, the references of each article were manually searched for articles not initially captured. Any conflicts during the article screening process were resolved by another author.
Study Definitions
Patients undergoing nonoperative treatment were treated with no treatment, knee brace, or physical therapy. Those undergoing operative treatment had either MPFL repair or reconstruction.
Data Extraction
Two authors extracted data on multiple variables and outcomes, including journal name, publication year, treatment group, number of patients, patient age, male/female ratio, follow-up time, instability events, and patient-reported outcomes.
Article Risk Assessment
Risk of bias was assessed by the Cochrane Risk of Bias for Randomized Trials tool, which examines bias under the following categories: randomization process, deviations from intended intervention, missing data, measurement of the outcome, and selection of the reported result. 15 Each article is assessed and assigned a score of low risk, some concerns, or high risk of bias for each domain.
Statistical Analysis
This study utilized SPSS Version 29.0 (IBM Corp) for statistical analysis. Frequency-weighted means and other descriptive statistics were used to describe the data where no statistical significance could be calculated. A random effects binary outcomes meta-analysis was performed using relative risk (RR) and 95% confidence intervals (95% CIs) for effect size for statistical comparison among studies with binary outcomes. Where feasible, a forest plot was generated to depict the relationship between variables and was shown if a minimum of 4 studies were included in the analysis. For continuous outcomes meta-analysis, if reported mean scores did not have accompanying standard deviations, standard deviations were used from the closest study, as demonstrated by Furukawa et al. 14 Outcomes were reported as unstandardized mean difference. To address the issue of having a limited number of available trials, we performed TSA utilizing software from the Copenhagen Trial Unit. 37 Data were collected and TSA was conducted using the following parameters: α = 5%, power = 80%, and observed RR reduction of 20%, adjusted for heterogeneity from the meta-analysis. Using the O’Brien-Fleming α-spending function, we applied cumulative Z curve analysis to monitor the accumulating data. The incidence in the control arm, defined for the TSA as “nonoperative treatment,” was calculated before running each outcome and manually put into the TSA interface. 21 The FI is determined by converting 1 patient in the group (control or experimental) from a “nonevent” to an “event” outcome and recalculating a 2-sided Fisher exact test until the P value meets or exceeds .05.11,20 Outcomes were deemed robust if the FI was greater than the number of patients lost to follow-up/dropout and fragile if the number of patients lost to follow-up/dropout was greater than FI.
Results
Initial Search Results
The database search included 262 candidate articles, and 155 remained after duplicates were removed. After screening by title and abstract, 8 articles remained for full-text screening, as 149 were excluded owing to a lack of relevance. After review of the full texts, 6 articles met the inclusion criteria and were included in the data extraction process (Figure 1).3,5,6,9,30,36
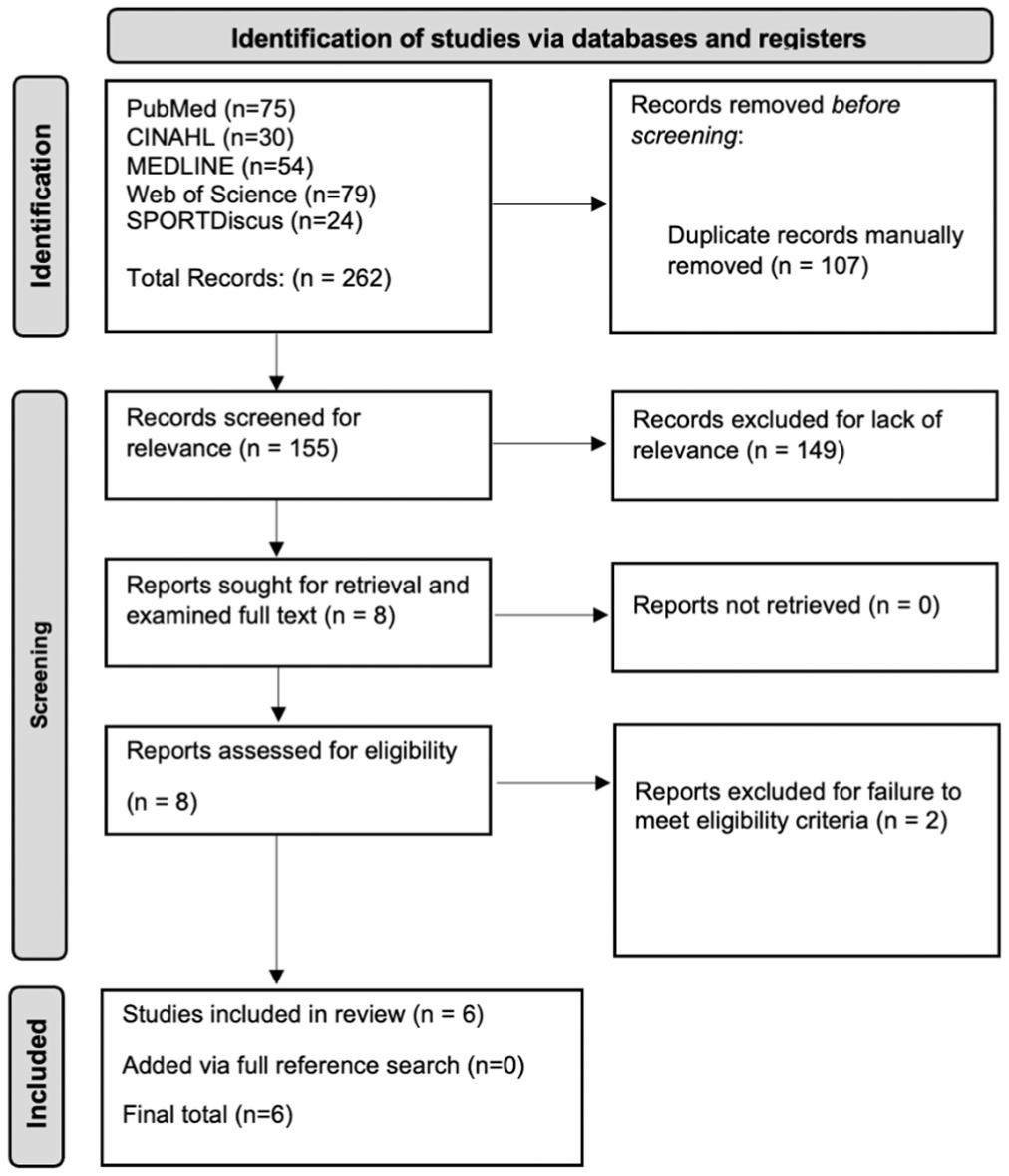
The PRISMA diagram (Preferred Reporting Items for Systematic Reviews and Meta-analyses) outlining the entire search progress, from initial search in 4 databases to final article inclusion.
Article Quality Results
All 6 RCTs had high risk of bias regarding blinding of outcome assessment and selective reporting, and all studies had a low risk of random sequence generation bias (Figure 2).
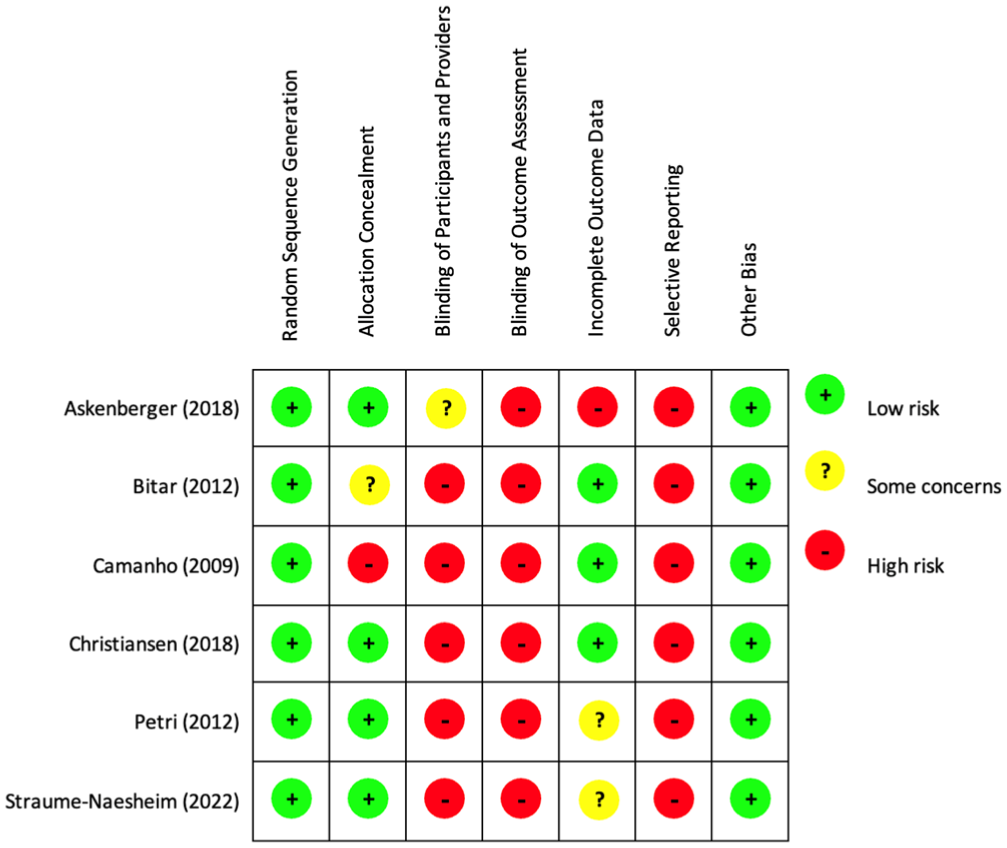

Outcomes of the Cochrane Risk of Bias 1.0 tool for randomized trials (n = 6 trials).
Descriptive Data
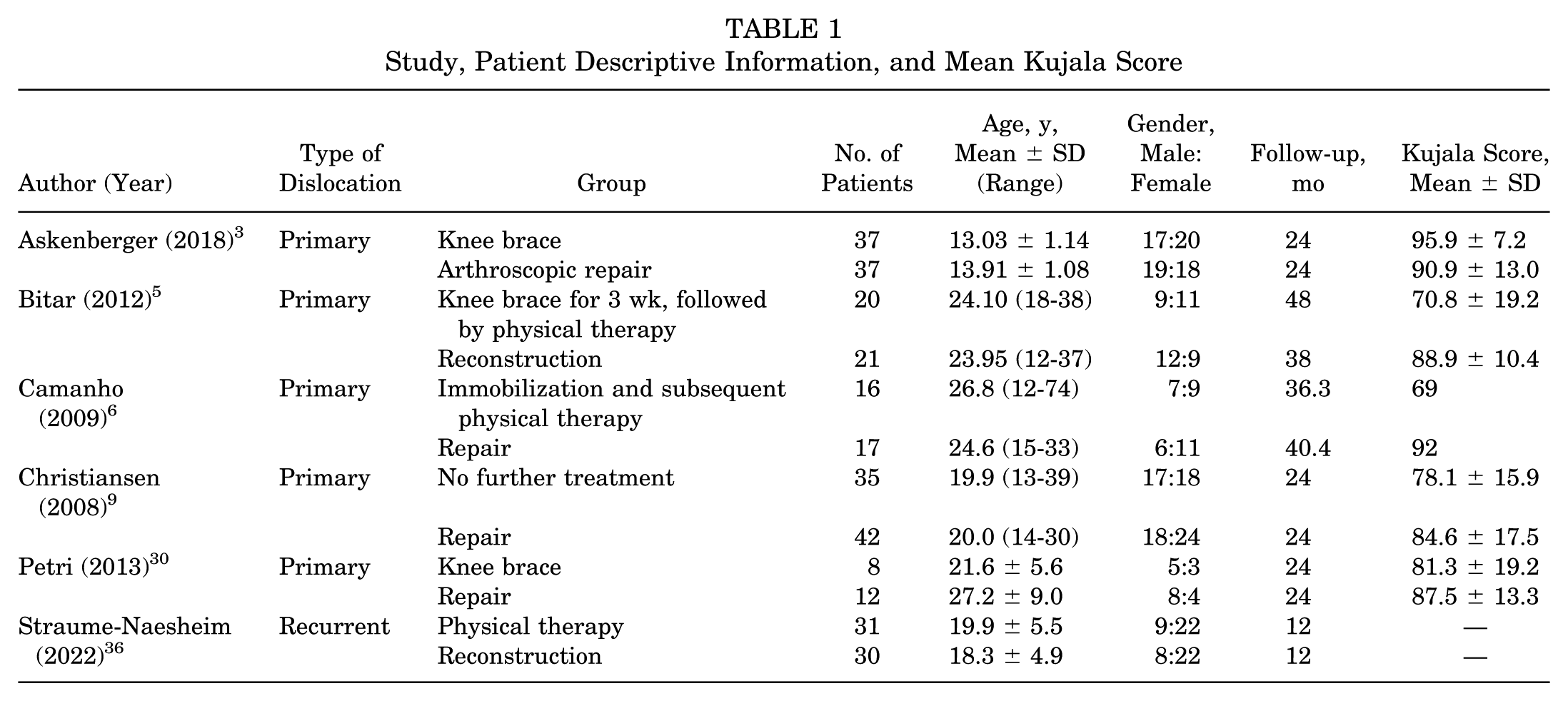
A total of 306 patients had a frequency-weighted mean ± SD age of 19.71 ± 4.24 years (range, 9-40) and follow-up of 21.61 ± 5.34 months. Females composed 55.9% of the patient population. From these studies, all patients had MPFL injury. Of these, 48.0% (n = 147) underwent nonoperative treatment with a brace and immobilization; 35.3% (n = 108), MPFL repair; and 16.7% (n = 51), MPFL reconstruction. A total of 159 patients underwent operative treatment. Of the 6 studies, 5 included patients with primary dislocation and 1 included recurrent dislocation (Table 1).
Study, Patient Descriptive Information, and Mean Kujala Score
Recurrent Instability After Nonoperative Versus Operative Treatment
Two studies reported isolated subluxation occurring in 22% (n = 8) of patients after nonoperative treatment. There were no reported isolated subluxation events after operative treatment. There was a statistically significant increase in recurrent instability after nonoperative treatment (44 of 147 cases; 29.93%) as compared with operative treatment (17 of 159 cases; 10.69%) via a random effects meta-analysis of 6 RCTs (P = .004; RR, 2.49; 95% CI, 1.34-4.61; Figure 3). This finding was robust, with an FI of 7 patients needed to alter the statistical significance of instability outcomes in those undergoing nonoperative versus operative treatment. TSA of recurrent instability after nonoperative and operative treatment for MPFL injuries determined a required information size of 1400 patients. At the current number of 306 patients, the cumulative Z curve crossed the significance boundary (P < .0001). However, it did not cross the required information size threshold, indicating that the current level of evidence is not yet sufficient to draw conclusions (Figure 4).
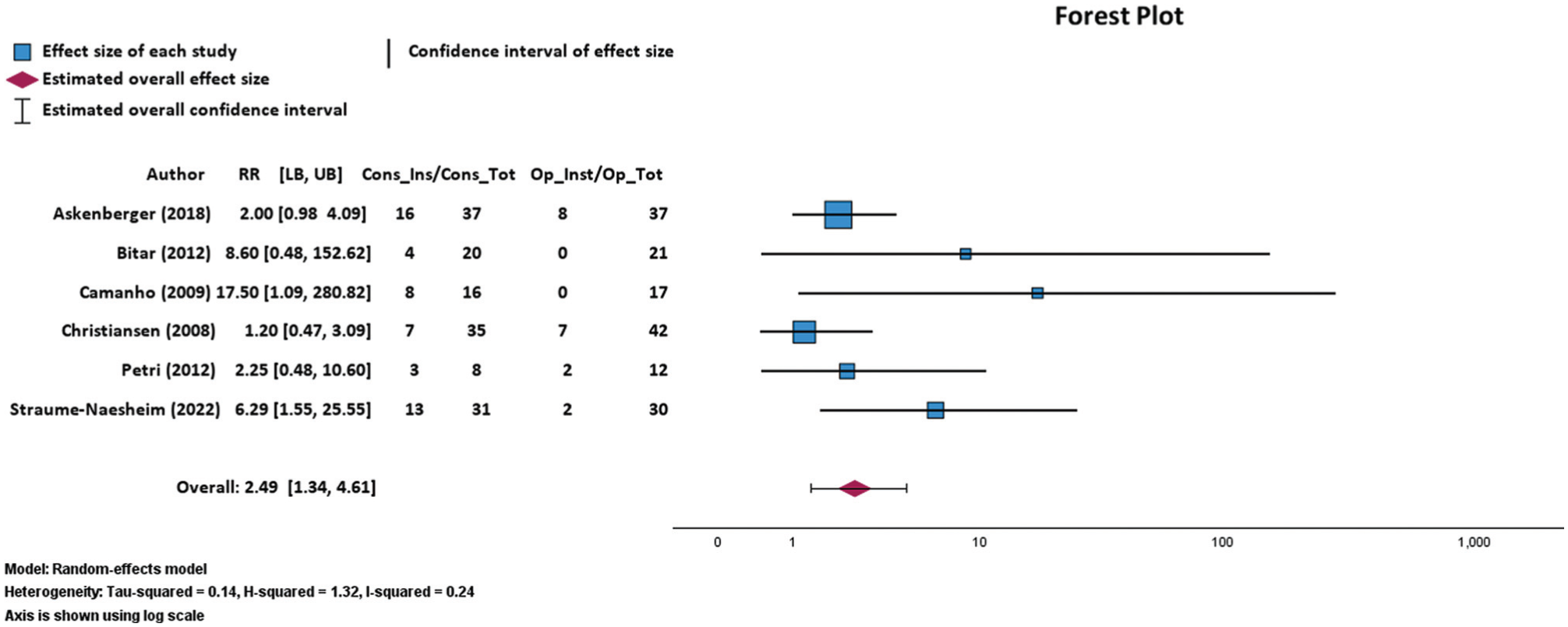
Random effects model forest plot demonstrating relationship between recurrent instability events and nonoperative or operative treatment for 6 RCTs. Effect measures used were relative risks (RRs) and 95% confidence intervals. Cons_Ins, patients with recurrent instability fusion treated nonoperatively; Cons_Tot, total number of patients treated nonoperatively; LB, lower bound; Op_Inst, number of patients with recurrent instability treated by operative repair or reconstruction; Op_Tot, total number of patients treated operatively; UB, upper bound. Heterogeneity: τ2 = 0.14, H2 = 1.32, I2 = 0.24. Axis is shown by log scale.
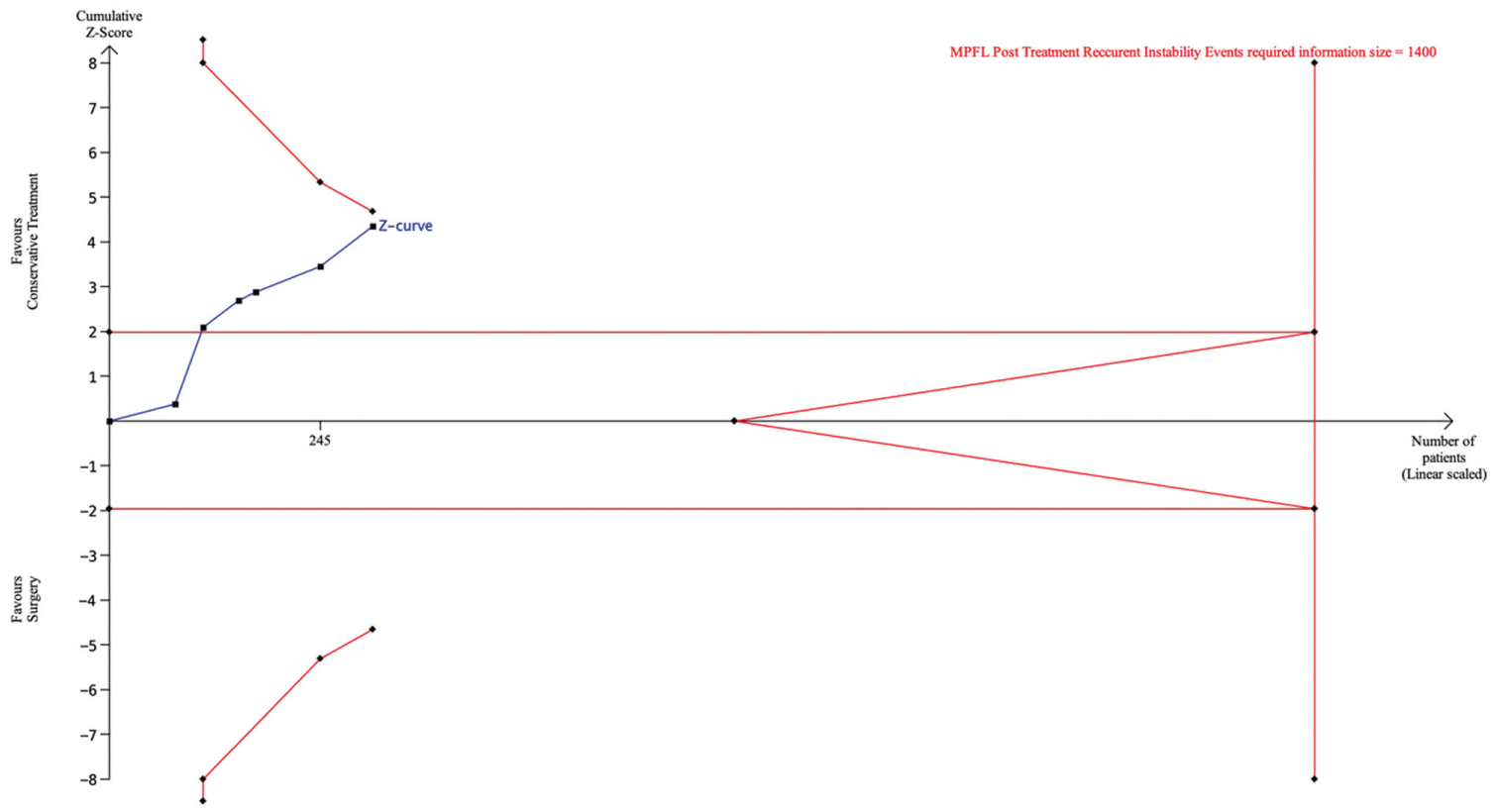
Trial sequential analysis comparing recurrent instability after nonoperative and operative treatment for medial patellofemoral ligament (MPFL) injuries with a 2-sided α of 5%, 80% power, and a relative risk reduction of 20%, adjusted for heterogeneity. A required information size of 1400 patients was calculated, with 306 included in the analysis. The cumulative Z curve (blue line) did not cross the required information size boundary (red line), indicating that the current evidence is not sufficient to draw conclusions.
Kujala Scores After Nonoperative Versus Operative Treatment
Five studies reported Kujala scores at final follow-up after each treatment. The mean Kujala score after nonoperative treatment was 79.02 ± 10.71 and the mean Kujala score after operative treatment fixation was 88.78 ± 2.91. Pooled findings of the 5 studies via a random effects meta-analysis found no significant differences of Kujala scores at final follow-up between nonoperative and operative treatment (P = .071; overall mean difference, –9.32; 95% CI, –19.45 to 0.81; Figure 5).3,5,6,9,30
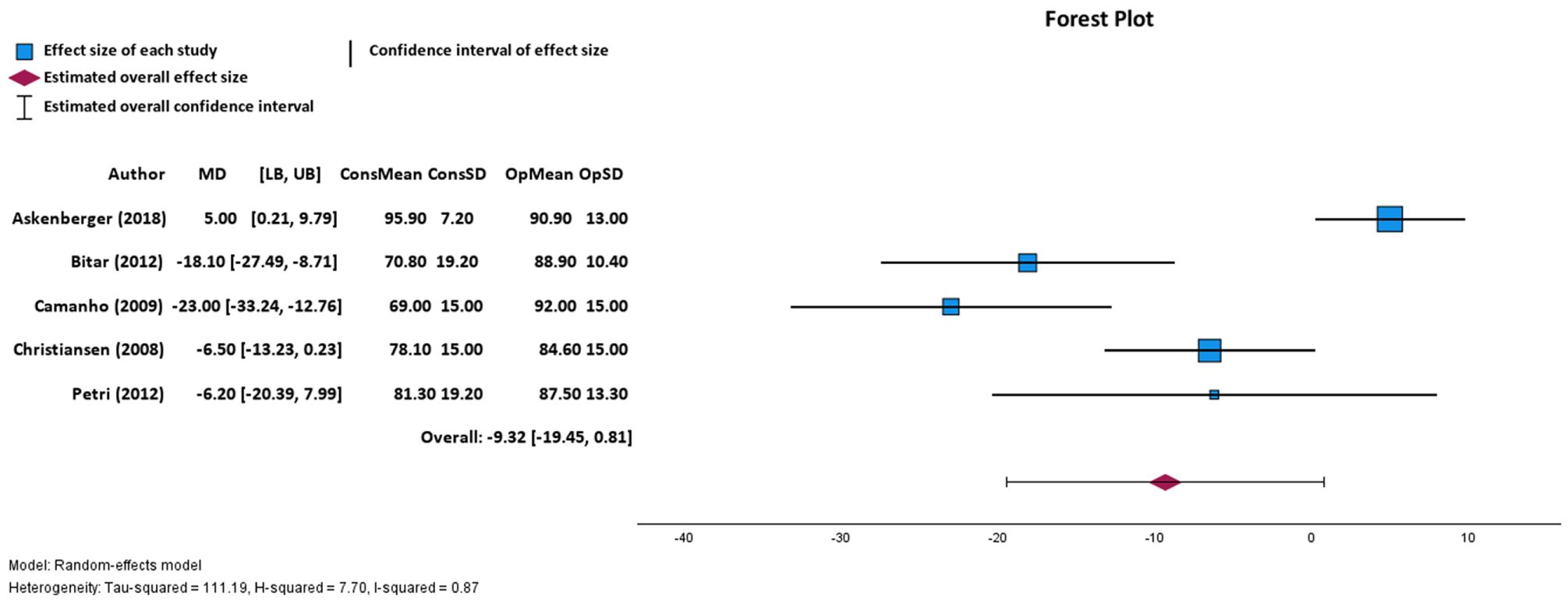
Random effects model forest plot demonstrating relationship between Kujala score and nonoperative or operative treatment for 5 studies. Effect measures and 95% confidence intervals were calculated for both individual study outcomes and reported as overall pooled outcomes. ConsMean, mean Kujala score after nonoperative treatment; ConsSD, standard deviation of mean Kujala score after nonoperative treatment; LB, lower bound; MD, mean difference; OpMean, mean Kujala score after operative treatment; OpSD, standard deviation of mean Kujala score after operative treatment; UB, upper bound. Heterogeneity: τ2 = 111.19, H2 =7.70, I2 = 0.67. Axis is shown by linear scale.
Subgroup Analysis of Recurrent Instability After Nonoperative Treatment Versus Repair
There was a statistically significant increase in recurrent instability after nonoperative treatment (34 of 96 cases; 35.42%) as compared with repair (17 of 108 cases; 15.74%) via a random effects subgroup meta-analysis of 4 RCTs (P = .019; RR, 1.87; 95% CI, 1.11-3.17; Figure 6). This finding was robust, with an FI of 8 patients needed to alter the statistical significance of instability outcomes in patients undergoing nonoperative versus operative treatment. TSA of recurrent instability after nonoperative treatment and repair for MPFL injuries determined a required information size of 1361 patients. At the current number of 204 patients, the cumulative Z curve crossed the significance boundary (P = .0027). However, it did not cross the required information size threshold, indicating that the current level of evidence is not sufficient to draw conclusions (Figure 7).
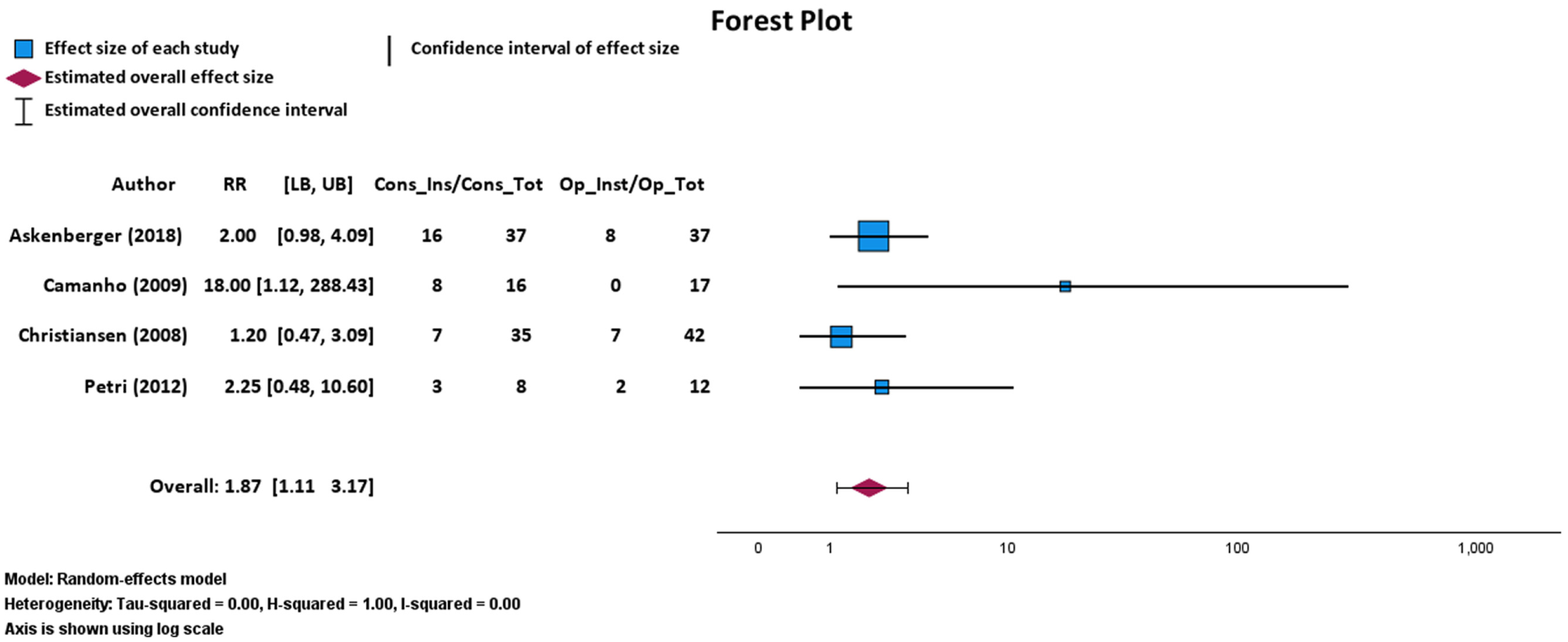
Random effects model forest plot demonstrating subgroup relationship between recurrent instability events and nonoperative treatment or repair for 4 randomized controlled trials. Effect measures used were relative risks (RRs) and 95% confidence intervals. Cons_Ins, patients with recurrent instability fusion treated nonoperatively; Cons_Tot, total number patients treated nonoperatively; LB, lower bound; Op_Inst, cases of repair with recurrent instability; Op_Tot, total number of cases of repaired; UB, upper bound. Heterogeneity: τ2 = 0.00, H2 = 1.00, I2 = 0.00. Axis is shown by log scale.

Trial sequential analysis comparing recurrent instability after nonoperative treatment and surgical repair for medial patellofemoral ligament (MPFL) injuries with a 2-sided α of 5%, 80% power, and a relative risk reduction of 20%, adjusted for heterogeneity. A required information size of 1361 patients was calculated, with 204 included in the analysis. The cumulative Z curve (blue line) did not cross the required information size boundary (red line), indicating that the current evidence is not sufficient to draw conclusions.
Subgroup Analysis of Kujala Scores After Nonoperative Treatment Versus Repair
Four studies reported Kujala scores at final follow-up after each treatment. The mean Kujala score after nonoperative treatment was 81.08 ± 11.17 and the mean Kujala score after operative treatment fixation was 88.75 ± 3.37. Pooled findings of the 4 studies via a random effects meta-analysis found no significant differences of Kujala scores at final follow-up between nonoperative treatment and repair (P = .228; overall mean difference, –7.17; 95% CI, –18.85 to 4.50; Figure 8).3,5,6,9,30,36
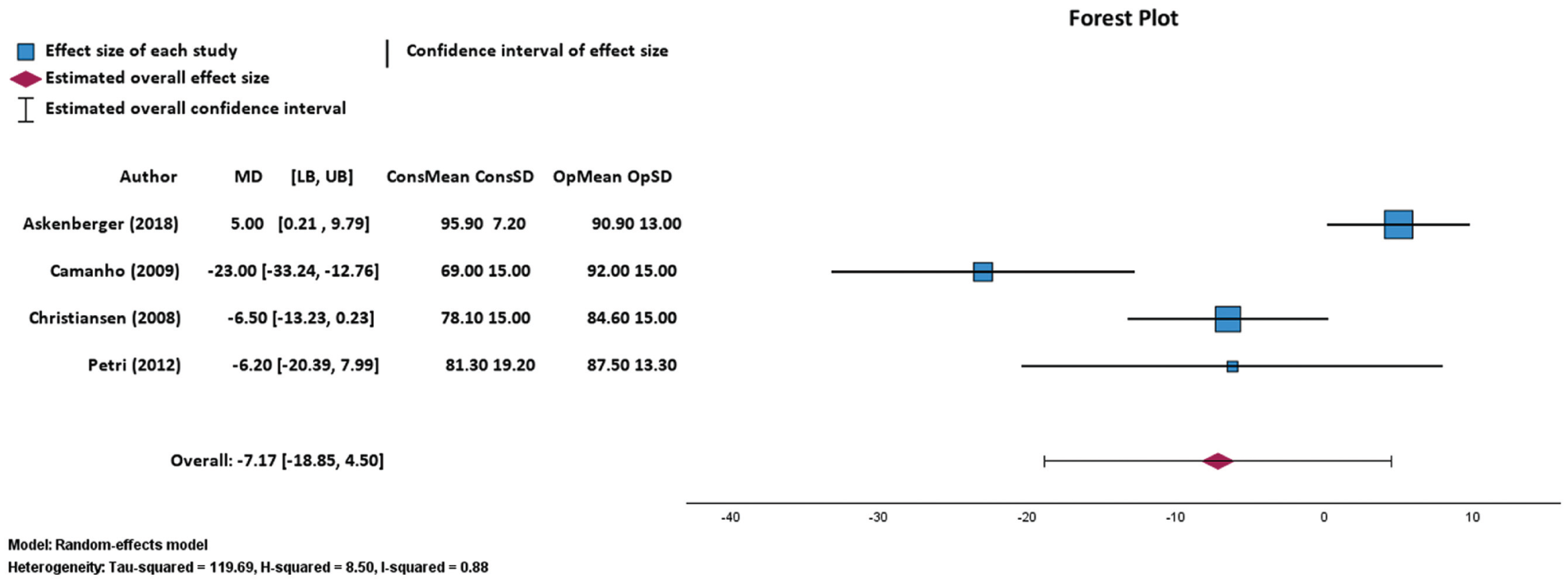
Random effects model forest plot demonstrating relationship between Kujala score and nonoperative or repair for 4 studies. Effect measures and 95% confidence intervals were calculated for both individual study outcomes and reported as overall pooled outcomes. ConsMean, mean Kujala score after nonoperative treatment; ConsSD, standard deviation of mean Kujala score after nonoperative treatment; LB, lower bound; MD, mean difference; OpMean, mean Kujala score after repair; OpSD, standard deviation of mean Kujala score after repair; UB, upper bound. Heterogeneity: τ2 = 119.69, H2 = 8.50, I2 = 0.88. Axis is shown by linear scale.
Subgroup Analysis of Recurrent Instability After Nonoperative Treatment Versus Reconstruction
There was a statistically significant increase in recurrent instability after nonoperative treatment (17 of 51 cases; 33.33%) as compared with reconstruction (2 of 51 cases; 3.92%) via a random effects subgroup meta-analysis of 2 RCTs (P = .003; RR, 6.80; 95% CI, 1.93-23.95).5,36 This finding was robust, with an FI of 4 patients needed to alter the statistical significance of instability outcomes in patients undergoing nonoperative versus operative treatment. TSA of recurrent instability after nonoperative and operative treatment for MPFL injuries determined a required information size of 1482 patients. At the current number of 102 patients, the cumulative Z curve crossed the significance boundary (P = .0029). However, it did not cross the required information size threshold, indicating that the current level of evidence is not sufficient to draw conclusions (Figure 9).

Trial sequential analysis comparing recurrent instability after nonoperative and reconstruction for medial patellofemoral ligament (MPFL) injuries with a 2-sided α of 5%, 80% power, and a relative risk reduction of 20%, adjusted for heterogeneity. A required information size of 1482 patients was calculated, with 102 included in the analysis. The cumulative Z curve (blue line) did not cross the required information size boundary (red line), indicating that the current evidence is not sufficient to draw conclusions.
Discussion
This systematic review and meta-analysis compares outcomes of operative and nonoperative management of MPFL injuries. A systematic review by Hurley et al 17 included a network meta-analysis to compare the outcomes of MPFL reconstruction, MPFL repair, and nonoperative treatment after patellar instability. Given the nature of a network meta-analysis and the broad inclusion criteria of any patients with patellar instability (not exclusively those with MPFL injury), it raises questions about the applicability of these results in determining whether operative or nonoperative treatment is more appropriate for patients with MPFL injury. Our findings indicate that recurrent instability occurred at significantly lower rates in patients undergoing operative treatment (10.69% vs 29.93%; P = .004), a robust finding, which was replicated in subgroup comparisons between MPFL repair and nonoperative treatment (15.74% vs 35.42%; P = .019) and, similarly, MPFL reconstruction and nonoperative treatment (3.92% vs 33.33%; P = .003). FI analysis highlights that these subgroup findings were robust; however, TSA demonstrates that the current evidence is not yet sufficient to draw definitive conclusions.
The findings in our study are supported by previous systematic reviews. Hurley et al 17 demonstrated that patients with patellar instability undergoing MPFL reconstruction and MPFL repair each had a decreased rate of recurrent instability as compared with nonoperative treatment. Similarly, Le et al 22 found that MPFL repair had a lower rate of recurrent instability when compared with nonoperative rehabilitation (7% vs 30%) after acute first-time patellar dislocation. Yoo et al 39 found MPFL reconstruction to have a lower rate of recurrence in patients with primary dislocation as compared with MPFL repair, proximal realignment, and nonoperative treatment. Alshaban et al 1 compared open reconstruction, arthroscopic reconstruction, open repair, arthroscopic repair, nonoperative treatment with immediate mobilization, and nonoperative treatment with partial mobilization and found arthroscopic repair to yield the lowest rate of redislocation in patients with primary patellar dislocation. Lee et al 23 found no significant difference in recurrent dislocation between patients undergoing nonoperative and operative treatment for primary patellar dislocation. These findings are important to consider because preventing recurrent instability can prevent the development of chronic pain, osteoarthritis, and functional limitations.
The decreased incidence of recurrent instability did not reflect an improvement in Kujala scores in the operative group (88.78 ± 2.91 vs 79.02 ± 10.71; P = .071). Askenberger et al 3 demonstrated an interesting relationship between patient-reported outcomes and rates of recurrence, as they did not find a difference in Kujala scores but reported a higher score on the Knee injury and Osteoarthritis Outcome Score quality of life subscale despite a higher frequency of recurrent instability in the group receiving nonoperative treatment. In contrast, Bitar et al 5 report an inverse correlation between Kujala scores and rates of recurrent instability, which would be the expected finding. Patient-reported outcomes are subjective and depend on many psychological factors, leading them to be unreliable when conflicting data are present. Furthermore, Kujala scores in the operative groups were mainly from patients undergoing MPFL repair, as there were insufficient data from studies analyzing MPFL reconstruction to perform a subgroup analysis. We performed a subgroup analysis comparing Kujala scores between the nonoperative group and MPFL repair group (81.08 ± 11.17 vs 88.75 ± 3.37; P = .228). The ambiguity of these findings is furthered by the TSA, which demonstrates an insufficient number of patients for comparison. This deepens the challenges in determining the effect of a lower incidence of recurrence on pain and quality of life using the current results given the nature of patient-reported outcomes.
Although our study focused on recurrent instability, it is important to consider other complications that may result from operative management. A substantial amount of data is currently available regarding complications after MPFL reconstruction. A systematic review by Jackson et al 18 reports up to a 32.3% incidence of complications in patients after MPFL reconstruction, including anterior knee pain, patellar fractures, stiffness, and range of motion deficits. Parikh et al 29 found a 16.2% complication rate in young patients undergoing MPFL reconstruction, including recurrent instability, stiffness, patellar fractures, and pain, with 47% of these complications being preventable—importantly, 89.4% of complications in this study were classified as being “major.” Shah et al 35 conducted a systematic review that reports a 26.1% complication rate. There were no nonoperative groups present for comparison in these studies, so more data are needed to determine the RR of performing MPFL reconstruction. Additionally, it is well known that recurrent instability significantly contributes to the development of osteoarthritis, but no studies have compared the incidence of patellofemoral osteoarthritis in patients undergoing operative versus nonoperative treatment.32,33 Knowing whether surgical treatment prevents osteoarthritis, while considering the effects of the timing of surgery and the significance of the injury, would provide better perspective on the exact benefits that come with surgical treatment.
To address the limited number of trials, TSA was conducted for all primary outcomes, revealing that the cumulative Z curve did not cross the required information size boundary for all primary outcomes. This indicates that the current evidence can be expanded on to further evaluate the primary outcomes. However, this must be weighed with the individual findings currently present in the literature and those present in the meta-analysis, which still provides evidence supporting operative treatment. This is arguably the most important finding of our study. Previous studies have found similar posttreatment outcomes, but none have provided insight on the strength of the evidence for their findings. The lack of sufficient RCT data strongly calls for further studies to add to the pool of data for more accurate clinical decision-making.
Our study has several strengths. It provides a thorough meta-analysis of randomized trials comparing operative and nonoperative treatment for MPFL injury, offering critical insights into postoperative outcomes such as recurrent instability and Kujala scores. The inclusion of TSA and FI also enhances the robustness of the conclusions, adding valuable quantitative tools to assess the sufficiency of existing evidence and help guide future research. By synthesizing data from multiple high-quality RCTs, this review reduces the risk of bias typically present in nonrandomized studies, thereby offering a stronger foundation for clinical recommendations. However, several limitations must be considered. While we aimed to focus on high-quality evidence, the heterogeneity in surgical techniques can introduce variability that could influence the outcomes. Additionally, the lack of blinding in these surgical trials increases the risk of performance and detection bias, which may affect the reported results, particularly for subjective outcomes such as pain and disability scores, as mentioned earlier. The mix of pediatric and adult populations in our data also opens the possibility of bias in Kujala scores and recurrence rates. Another limitation is that our study did not evaluate long-term outcomes to examine long-term function and development of osteoarthritis. Furthermore, the RCTs in the literature do not perform risk factor stratification, which limits the extent to which the results can be applied to a surgical practice. Additional RCTs analyzing complication rates and long-term implications after MPFL reconstruction, MPFL repair, and nonoperative treatment should be conducted to better understand the RRs of the various modes of treatment of MPFL injury. These studies should stratify outcomes by factors such as age and gender to inform which patients should receive certain treatments. Despite all studies in this systematic review being RCTs, the groups of patients being compared are not equal, as they have variations in anatomy that may deem them more viable candidates for certain modes of treatment. Therefore, there is a need for RCTs that compare operative and nonoperative treatment in patients with matched anatomic parameters. Additionally, future trials should examine adult or pediatric patients only.
Conclusion
This systematic review and meta-analysis provides a robust evaluation of operative versus nonoperative treatment in patients with MPFL injury. Operative treatment led to significantly decreased rates of recurrence, although this did not lead to a decrease in Kujala scores. TSA and FI analyses show that although the current evidence is robust, it is not sufficient to draw definitive conclusions regarding primary outcomes given the limited number of total patients across the RCTs in this study. The key to the findings in this study is the need for further RCTs to draw more definitive conclusions. These findings highlight the importance of cautious, individualized surgical planning, with concerns of recurrence guiding the decision between nonoperative and operative treatment. Importantly, it is necessary to consider that variations in anatomy play a role in recovery, which must be considered as a part of decision-making. Future large randomized trials should be conducted outlining and comparing complication rates after MPFL reconstruction, MPFL repair, and nonoperative treatment in patients with matched anatomic parameters along with risk stratification to provide further data for comprehensive guidance for optimizing patient care in management of MPFL injury.
Footnotes
Submitted March 15, 2025; accepted June 25, 2025.
The authors have declared that there are no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
An online CME course associated with this article is available for 1 AMA PRA Category 1 Credit™ at https://education.sportsmed.org/Public/Catalog/Home.aspx?CourseSearch=1&Criteria=9&Option=25. In accordance with the standards of the Accreditation Council for Continuing Medical Education (ACCME), it is the policy of The American Orthopaedic Society for Sports Medicine that authors, editors, and planners disclose to the learners all financial relationships during the past 12 months with any commercial interest (A ‘commercial interest’ is any entity producing, marketing, re-selling, or distributing health care goods or services consumed by, or used on, patients). Any and all disclosures are provided in the online journal CME area which is provided to all participants before they actually take the CME activity. In accordance with AOSSM policy, authors, editors, and planners’ participation in this educational activity will be predicated upon timely submission and review of AOSSM disclosure. Noncompliance will result in an author/editor or planner to be stricken from participating in this CME activity.
