Abstract
Background:
A discoid lateral meniscus (DLM) is the most common meniscus variant and is commonly treated with arthroscopic saucerization. There are mixed data regarding long-term results after surgery, especially in terms of radiological parameters.
Purpose/Hypothesis:
The aim was to evaluate the functional and radiological results of patients who underwent arthroscopic saucerization for a symptomatic DLM. It was hypothesized that successful outcomes can be achieved by avoiding excessive resection while reshaping only to an extent that prevents mechanical symptoms.
Study Design:
Case series; Level of evidence, 4.
Methods:
This study retrospectively analyzed pediatric and adult patients who had a symptomatic discoid meniscus between 2000 and 2018, who underwent arthroscopic saucerization with at least 10 mm of peripheral length, and who had at least 5 years of follow-up. Radiological parameters were measured on both preoperative and follow-up radiographs. Patient-reported outcome measure scores were recorded at follow-up.
Results:
The study included 57 knees of 53 patients (mean age, 27.6 years [range, 6-65 years]). The mean follow-up duration was 12.1 years (range, 5.0-23.1 years). There were 31 knees in the pediatric group and 26 knees in the adult group. No significant difference was found between the groups or between preoperative and follow-up values for the femorotibial angle (P > .05). When the preoperative and follow-up Kellgren-Lawrence grades were compared, no change was observed in the pediatric group (P = .125), while grades were shown to progress in the adult group (P < .001). The mean Lysholm score was 94.61 ± 7.61 and 84.23 ± 14.90 for the pediatric and adult groups, respectively (P = .001). Overall, 2 patients underwent arthroscopic surgery because of a symptomatic recurrence of symptoms, and 2 patients underwent arthroplasty because of osteoarthritis. The 10-year survival rate was 90.6%.
Conclusion:
Limited saucerization of a DLM helped to preserve coronal-plane knee joint alignment. Functional and radiological results were superior in the pediatric patients. Even when alignment was more varus in older patients, preoperative and follow-up femorotibial angles were not statistically significant. This outcome may be used to guide treatment in appropriately selected cases.
A discoid lateral meniscus (DLM) is the most common morphological meniscus variant. It involves alterations in meniscus shape and stability.7,31 There are many theories, but the exact cause of a discoid meniscus remains unknown. 30
Nonoperative treatment has been found to produce unfavorable clinical outcomes in cases of a symptomatic DLM and thus is not recommended.17,23 The current treatment of choice for a DLM is saucerization with arthroscopic partial meniscectomy.4,16,18,20 When there is a tear necessitating repair or when peripheral instability is present, it is imperative to incorporate repair techniques into the surgical procedure. 12
The age of the patient has been highlighted as a prognostic factor in cases treated with arthroscopic surgery, and clinical results worsen as the follow-up period lengthens.17,28 Long-term follow-ups typically show poor radiological outcomes; however, the degenerative process may not reflect clinical results. 1 The need for revision procedures is another factor to be considered in the long-term follow-up of patients with a DLM. 22
The traditionally recommended amount of an intact peripheral rim remaining after saucerization is 6 to 8 mm. 13 Excessive removal of the DLM is regarded as a cause of instability. 10 Moreover, a decrease in meniscal width has been reported to occur even after surgery. 26 This should be kept in mind when determining the amount of resection, especially in the pediatric population.
The aim of the present study was to thoroughly investigate and analyze the preoperative and midterm to long-term clinical and radiological outcomes of patients with a symptomatic DLM who underwent arthroscopic saucerization with or without meniscal repair. We hypothesized that with the approach of conservation of a minimum of 10 mm of residual meniscal tissue, successful radiological and clinical outcomes would be achieved.
Methods
This study was approved by the local institutional ethical committee (GO 22/1169). The preoperative and postoperative clinical and radiological outcomes of patients with a DLM who underwent partial meniscectomy performed by a single surgeon (O.A.A.) at a single center were retrospectively analyzed.
Patients treated for a discoid meniscus at a tertiary reference hospital between January 2000 and January 2018 were retrospectively evaluated. Within the scope of the study, 138 knees from 129 patients were reviewed. The study included patients with a DLM who had been operated on by the senior author, had a preoperative physical examination record and a surgical report, had undergone standing knee anteroposterior (AP) radiography before surgery and at the end of follow-up, and had been followed up for a minimum of 5 years. Patients without appropriate radiographs, those with insufficient records, those with a discoid medial meniscus, those who had undergone subtotal or total meniscectomy, those who had undergone previous knee surgery, and those who underwent knee surgery during the follow-up period for a cause other than osteoarthritis or meniscal injuries were excluded from the study. After the criteria were applied, the study was conducted with 57 knees of 53 patients. After primary surgery for a DLM, the patients who underwent a reoperation because of inadequate resection (n = 1) or a rerupture of the lateral meniscus (n = 1) and knee arthroplasty because of osteoarthritis (n = 2) were recorded, and survival analysis was performed. These 4 patients were excluded from the main analysis, and statistical analysis was performed with 53 knees (Figure 1).
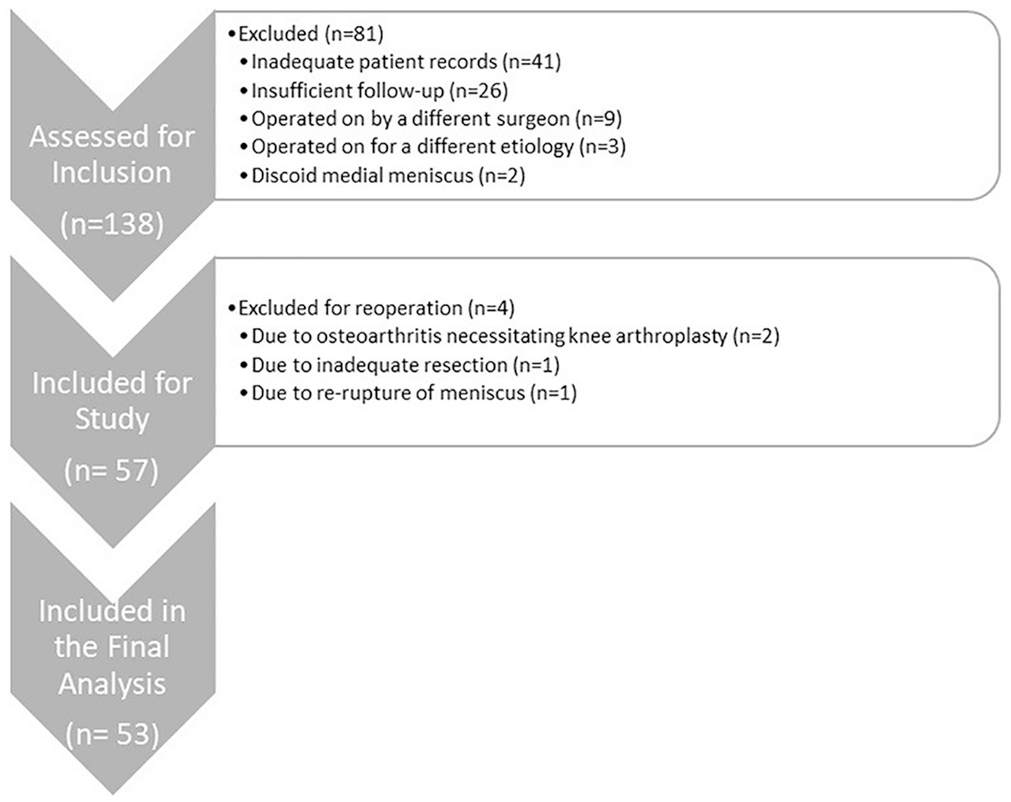
Flowchart of the participants included in the study cohort.
The patients were classified as pediatric if they were aged ≤18 years and as adults if they were aged >18 years, according to their age at the time of surgery. In addition, those in the pediatric group were divided into subgroups of ≤12 and ≥13 years of age for further evaluation.
Data Collection
Age at the time of surgery, follow-up duration, age at the time of the latest follow-up, sex, laterality, and discoid meniscus localization of the patients were recorded. On the preoperative evaluation form, the initial complaints were categorized according to pain, catching, locking, giving way, and swelling, and how the complaints emerged were categorized according to daily activity, sport, and trauma.
Surgical Technique
During surgery, tears in the white-white zone were debrided. Tears in the peripheral zone were repaired. The discoid structure of the meniscus was saucerized by avoiding excessive resection. The length of the retained meniscus to the periphery was at least 10 mm after resection. This was confirmed with arthroscopic probe measurements in all patients. The Watanabe classification of a discoid meniscus, the presence of a meniscal tear, the type of meniscal tear (if any), and the treatment method applied were evaluated using the surgical report form completed by the primary surgeon immediately after surgery.
Radiological and Clinical Evaluations
The preoperative and final follow-up medial joint space (MJS; in mm), lateral joint space (LJS; in mm), and femorotibial angle (FTA; in deg) as well as changes in parameters were noted during the radiological evaluation. The Kellgren-Lawrence classification was used for the assessment of knee osteoarthritis.
The FTA was defined as the angle formed by the anatomic axes of the femur and tibia on standing knee AP radiography. Positive FTA values indicated valgus alignment, while negative values indicated varus alignment in the coronal plane.
Radiographic variables were measured by 2 observers using a picture archiving and communication system. Measurements were made blind to information regarding the cases and were repeated after 2 weeks. In this way, 4 measurement sets from 2 observers were used for statistical analysis.
At the last follow-up, patient-reported outcome measures (PROMs) including the Lysholm Knee Scoring Scale, International Knee Documentation Committee (IKDC) subjective knee evaluation form, and Short Form–12 (SF-12) were administered and their scores noted. Lysholm Knee Scoring Scale scores were categorized as follows: ≥95 excellent, 85-94 good, 65-84 fair, and <65 poor. SF-12 scores were divided into mental component summary and physical component summary scores.
Statistical Analysis
The data were analyzed with SPSS (Version 23; IBM). Compliance with a normal distribution was examined using the Shapiro-Wilk test and Kolmogorov-Smirnov test. The chi-square test, Yates correction, Fisher exact test, and Fisher-Freeman-Halton test were used to compare categorical variables according to groups. Multiple comparisons of proportions were examined with the Bonferroni-corrected Z test. The independent 2-sample t test was used to compare normally distributed data according to binary groups, and the Mann-Whitney U test was used to compare nonnormally distributed data. The paired 2-sample t test was used to compare normally distributed data within groups according to binary time. The McNemar test, McNemar-Bowker test, and Wilcoxon test were used to compare dependent categorical variables within groups according to binary time. Relationships between nonnormally distributed data were examined with the Spearman rho correlation coefficient. Interobserver and intraobserver agreement were examined using the kappa coefficient and intraclass correlation coefficient. For the intraclass correlation coefficient, values <0.50 indicated poor reliability, 0.50-0.75 indicated moderate reliability, 0.76-0.90 indicated good reliability, and >0.90 indicated excellent reliability. Linear regression analysis was used to examine the effect of independent variables on Lysholm Knee Scoring Scale and IKDC subjective knee evaluation form scores. The results of analysis are presented as the mean ± standard deviation for continuous variables and the frequency (percentage) for categorical variables. P values <.05 were considered significant.
Results
There were 31 female and 22 male patients included in the study. The mean follow-up period of the patients was 12.1 years (range, 5.0-23.1 years). Patient information is shown in Table 1.
Characteristics of Patients a
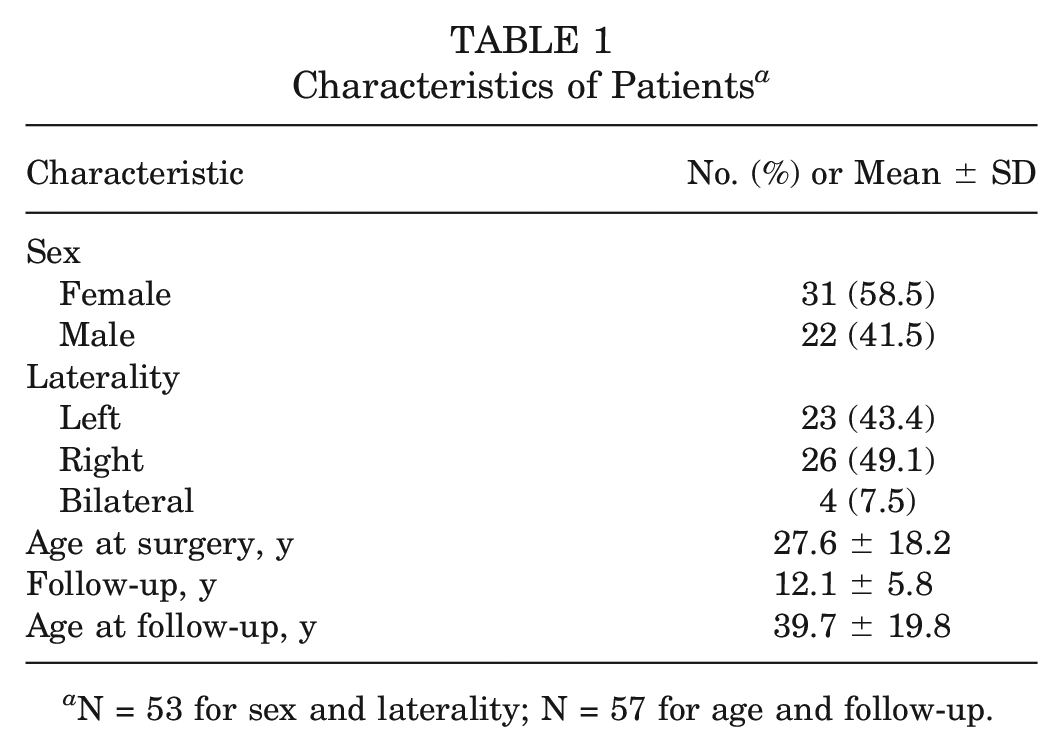
N = 53 for sex and laterality; N = 57 for age and follow-up.
When the patients were evaluated according to their age at the time of surgery, there were 31 knees in the pediatric group and 26 knees in the adult group. A statistically significant difference was found between the groups according to the Watanabe classification (P = .023). Diagnosis and treatment information by age group is shown in Table 2.
Diagnosis and Treatment According to Age Group a
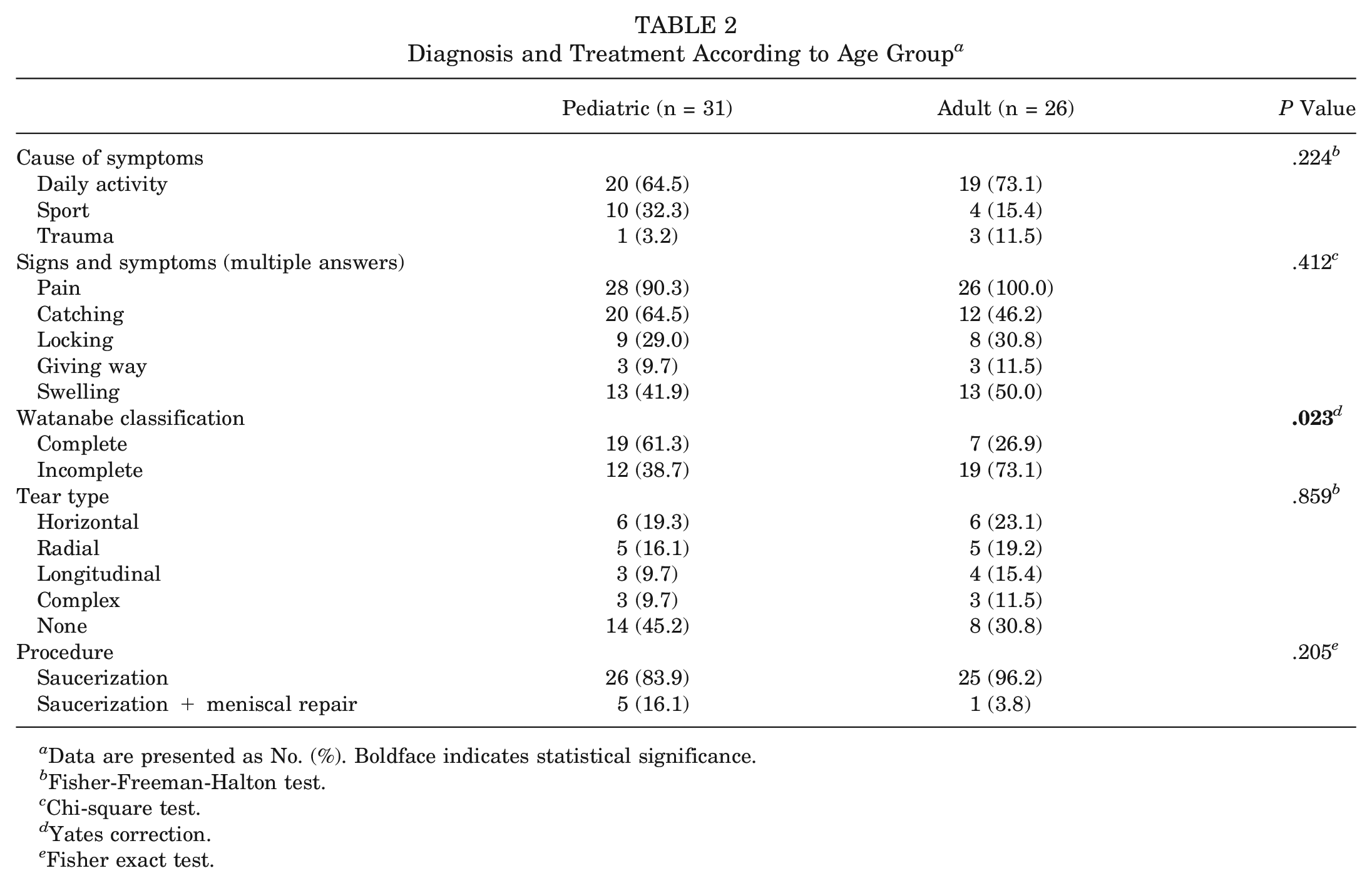
Data are presented as No. (%). Boldface indicates statistical significance.
Fisher-Freeman-Halton test.
Chi-square test.
Yates correction.
Fisher exact test.
Interobserver and intraobserver intraclass correlation coefficients for MJS, LJS, and FTA as well as kappa coefficients for Kellgren-Lawrence grades are given in Tables 3 and 4, respectively.
Interobserver Agreement for Radiological Parameters a
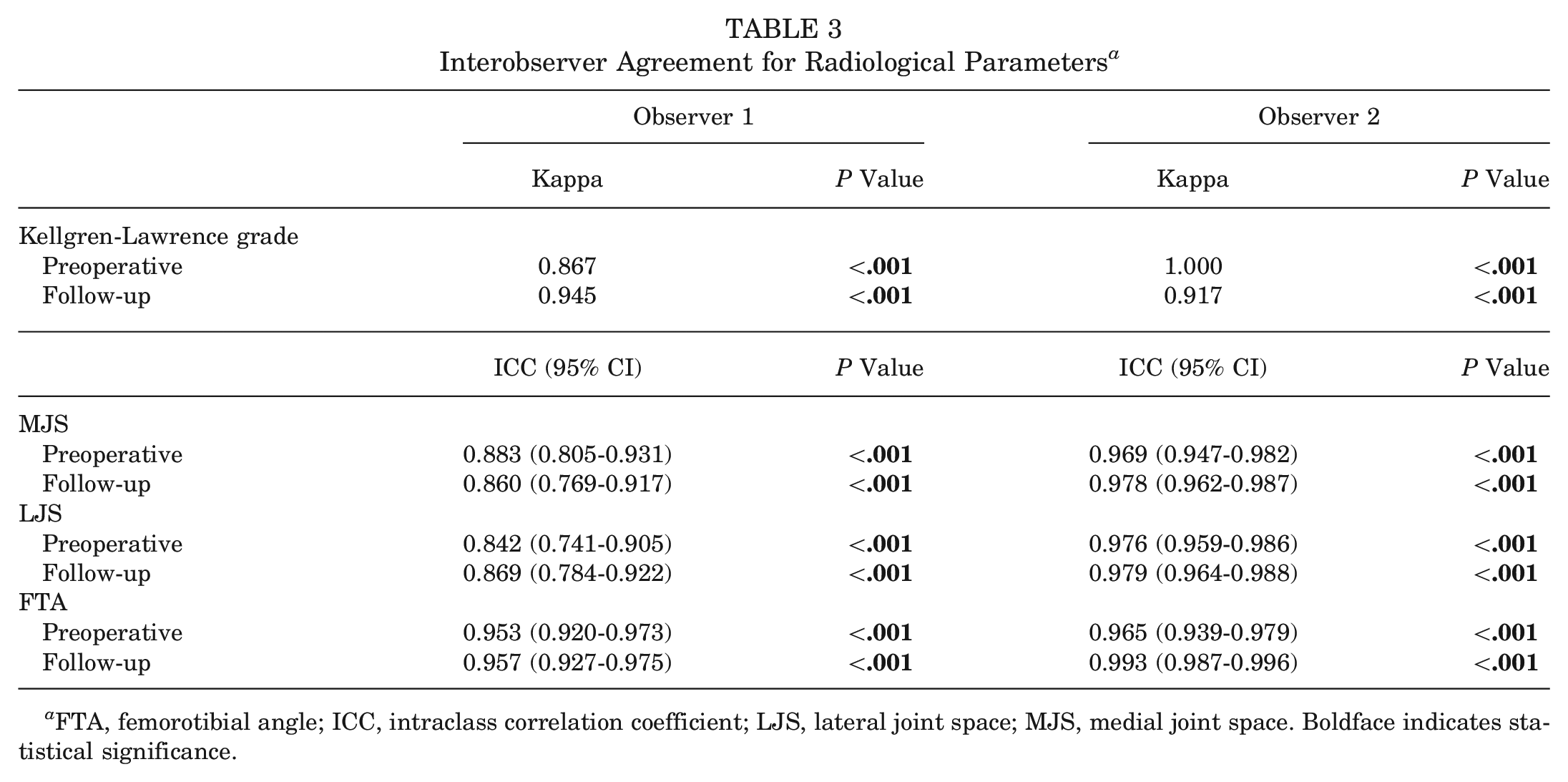
FTA, femorotibial angle; ICC, intraclass correlation coefficient; LJS, lateral joint space; MJS, medial joint space. Boldface indicates statistical significance.
Intraobserver Agreement for Radiological Parameters a
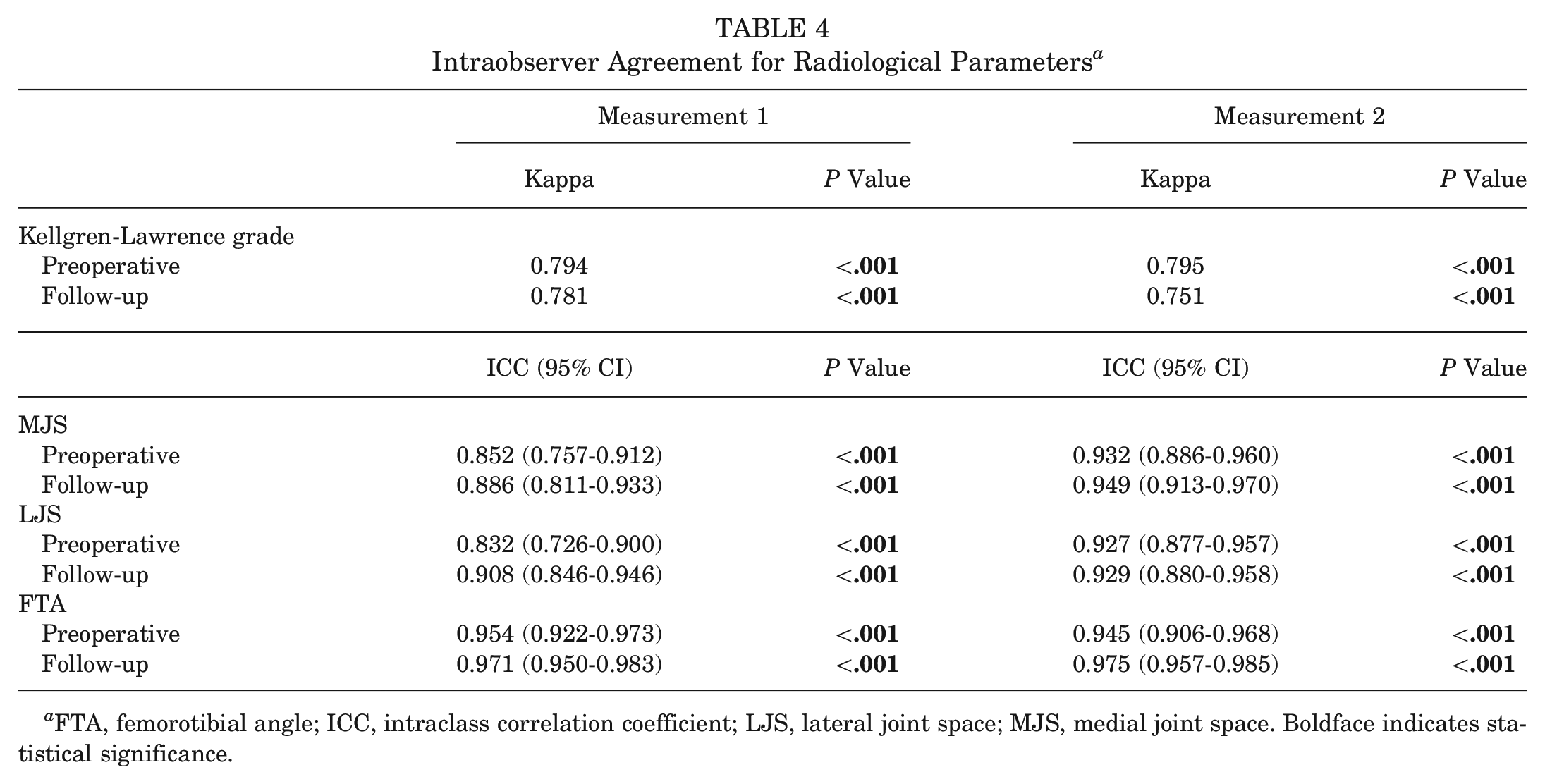
FTA, femorotibial angle; ICC, intraclass correlation coefficient; LJS, lateral joint space; MJS, medial joint space. Boldface indicates statistical significance.
Significant differences were observed between the pediatric and adult groups according to the MJS and LJS both preoperatively and at follow-up. There were also significant differences between the preoperative and follow-up MJS and LJS in both the pediatric and adult groups. For the FTA, no statistically significant difference was found between the groups or between preoperative and follow-up values. When the Kellgren-Lawrence grades before surgery and at follow-up for the pediatric and adult groups were compared, there was a significant difference in their distribution (P < .001). There was no difference between the distributions of preoperative and follow-up Kellgren-Lawrence grades in the pediatric group (P = .125) (Table 5).
Radiological Outcomes According to Age Group a
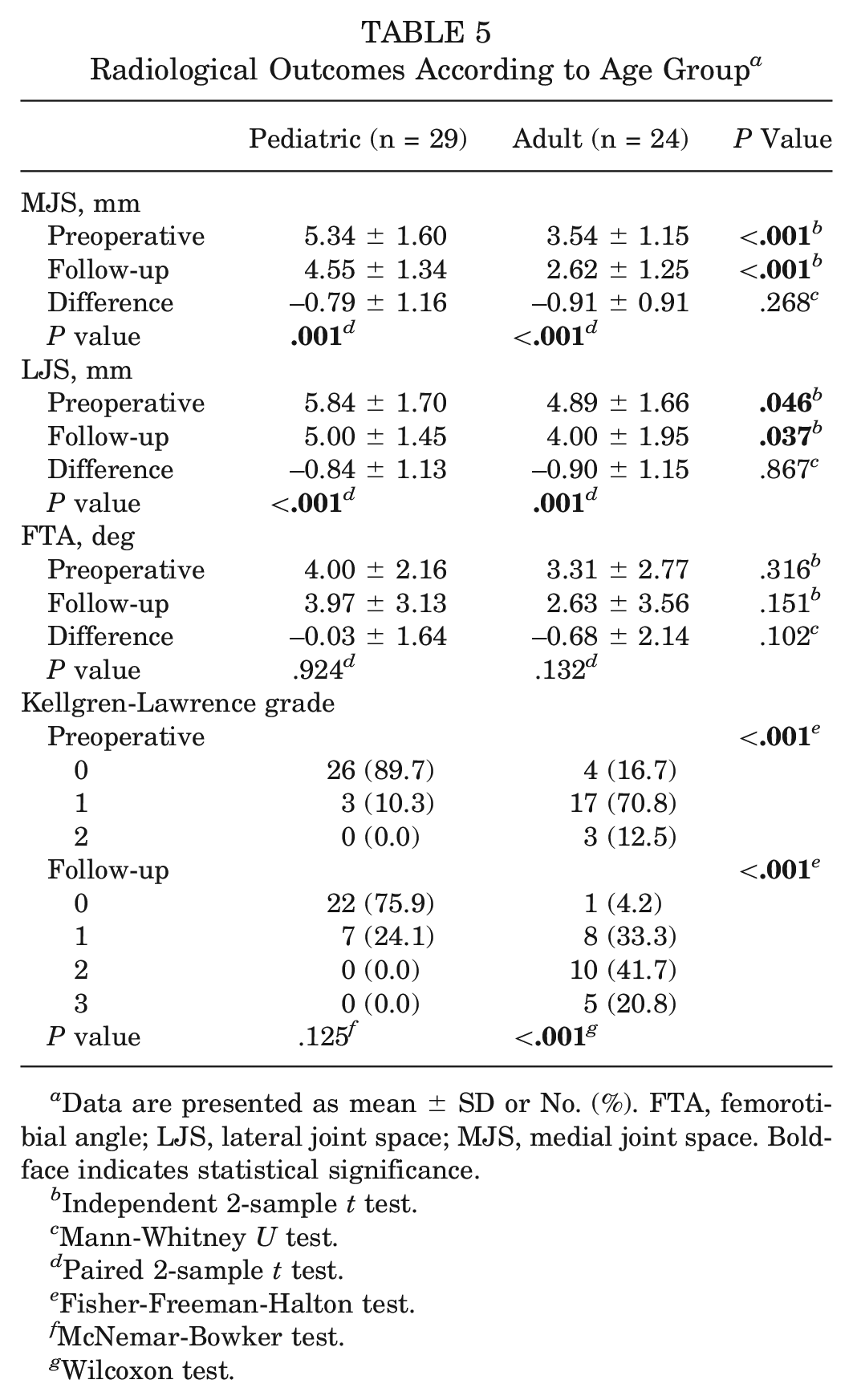

Data are presented as mean ± SD or No. (%). FTA, femorotibial angle; LJS, lateral joint space; MJS, medial joint space. Boldface indicates statistical significance.
Independent 2-sample t test.
Mann-Whitney U test.
Paired 2-sample t test.
Fisher-Freeman-Halton test.
McNemar-Bowker test.
Wilcoxon test.
Patients in the pediatric group were evaluated by dividing them into 2 subgroups. There were significant differences between the preoperative and follow-up MJS and LJS in both subgroups (Table 6).
Radiological Outcomes of Pediatric Group a
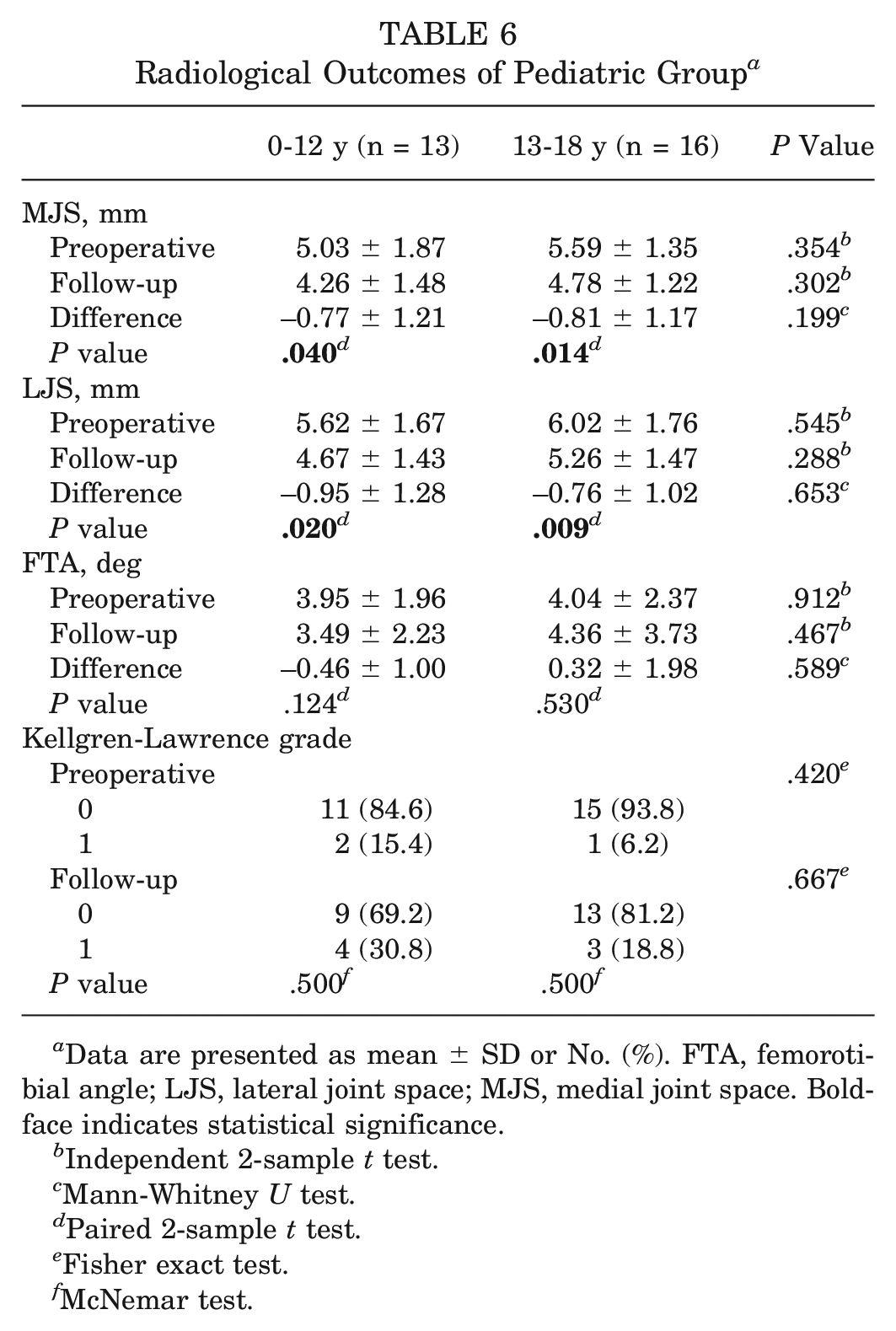
Data are presented as mean ± SD or No. (%). FTA, femorotibial angle; LJS, lateral joint space; MJS, medial joint space. Boldface indicates statistical significance.
Independent 2-sample t test.
Mann-Whitney U test.
Paired 2-sample t test.
Fisher exact test.
McNemar test.
The relationships between surgical age and radiological variables were analyzed. There was a weak but statistically significant negative relationship between age at the time of surgery and preoperative FTA (r = −0.299; P = .030) (Figure 2) and between age at the time of surgery and follow-up FTA (r = −0.337; P = .014) (Figure 3). All correlation values are presented in Table 7.
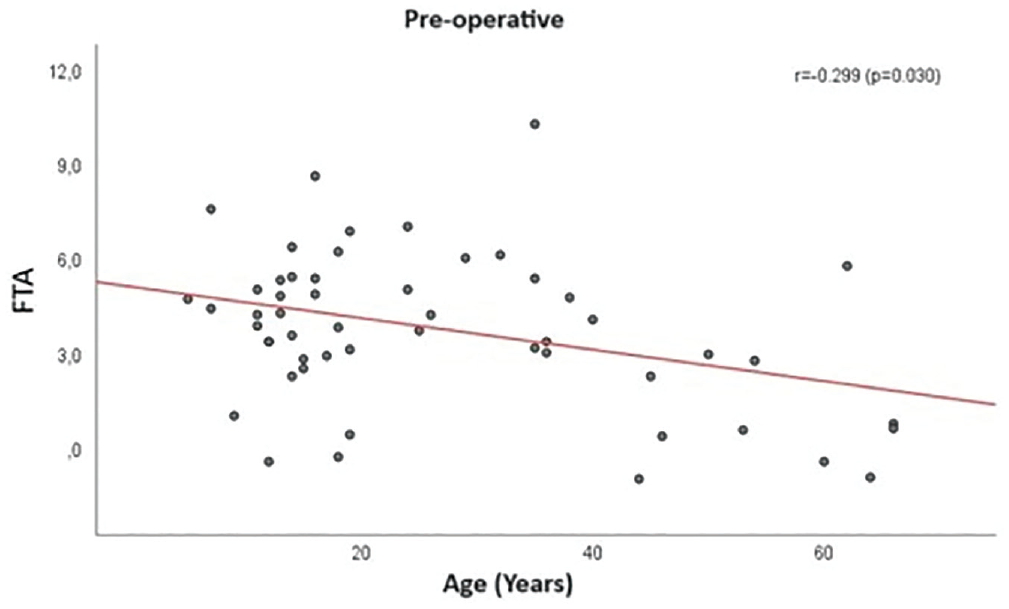
Relationship between surgical age and preoperative femorotibial angle (FTA).
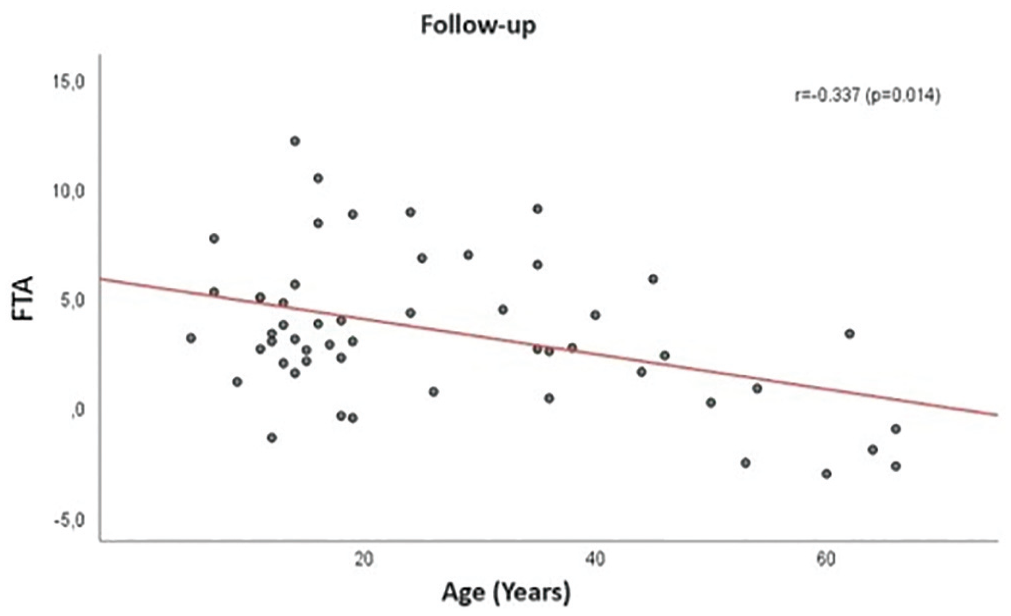
Relationship between surgical age and follow-up femorotibial angle (FTA).
Relationship Between Surgical Age and Radiological Variables a
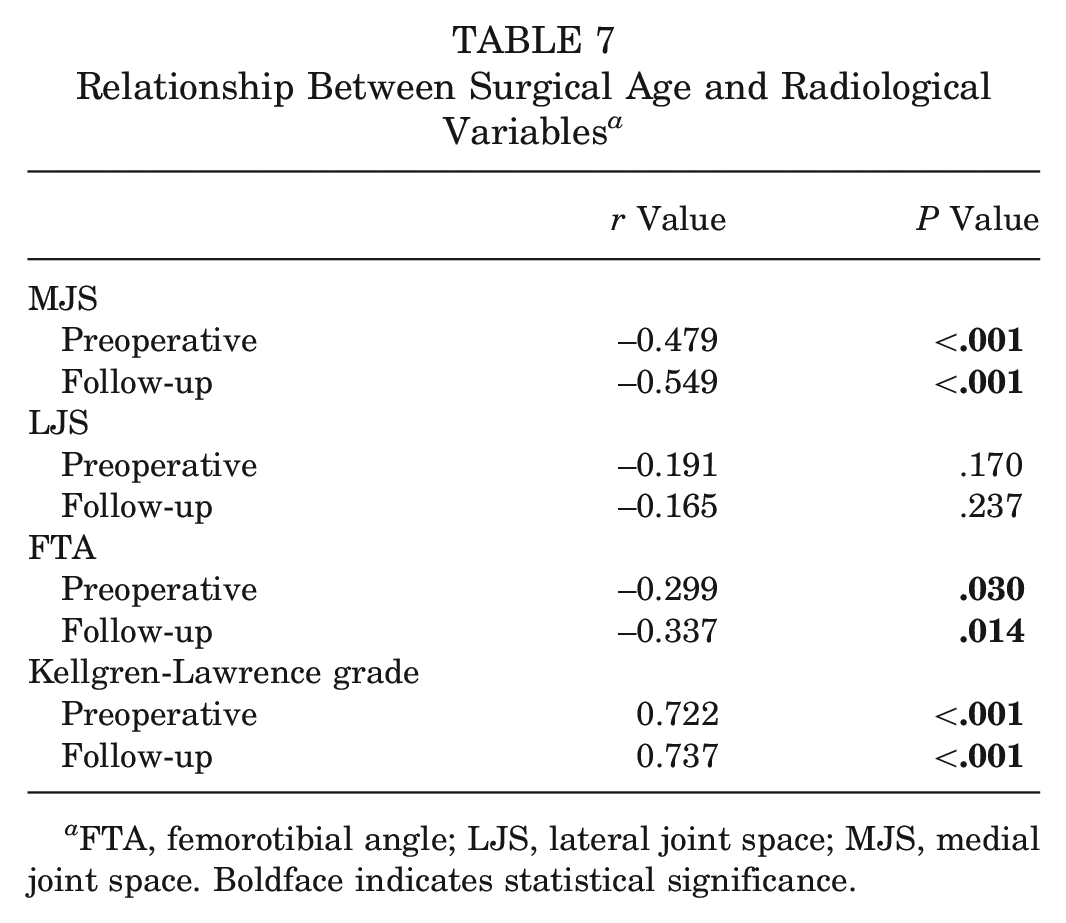
FTA, femorotibial angle; LJS, lateral joint space; MJS, medial joint space. Boldface indicates statistical significance.
PROM scores were analyzed between the pediatric and adult groups (Table 8).
PROM Scores at the Final Follow-up a
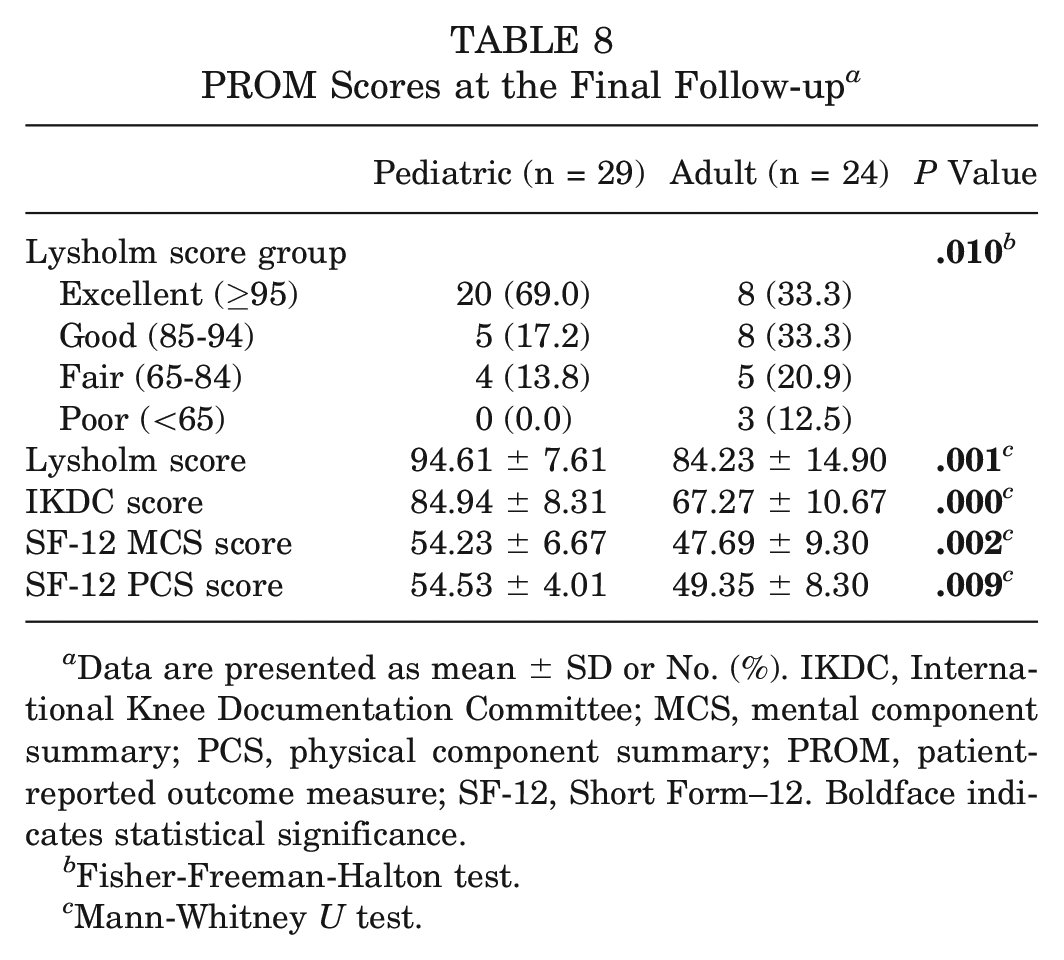
Data are presented as mean ± SD or No. (%). IKDC, International Knee Documentation Committee; MCS, mental component summary; PCS, physical component summary; PROM, patient-reported outcome measure; SF-12, Short Form–12. Boldface indicates statistical significance.
Fisher-Freeman-Halton test.
Mann-Whitney U test.
The regression model established to examine the effect of independent variables on the Lysholm score found the effect to be statistically significant (F = 3.39; P = .025) (Table 9). Increasing the age at the time of follow-up by 1 unit reduced the Lysholm score by 0.243 units (P = .012). The established regression model explained 11.4% of the Lysholm score. The regression model established to examine the effect of independent variables on the IKDC score found the effect to be statistically significant (F = 9.486; P < .001) (Table 10). Increasing the age at the time of follow-up by 1 unit reduced the IKDC score by 0.383 units (P < .001). With the established regression model, 31.3% of the IKDC score was explained.
Influence of Independent Variables on Lysholm Score Using Linear Regression a
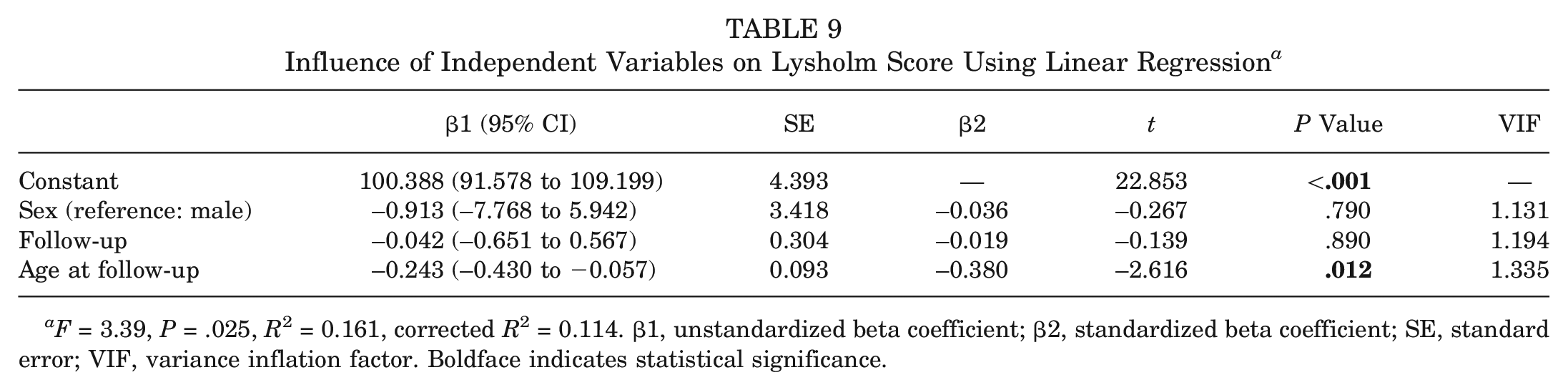
F = 3.39, P = .025, R2 = 0.161, corrected R2 = 0.114. β1, unstandardized beta coefficient; β2, standardized beta coefficient; SE, standard error; VIF, variance inflation factor. Boldface indicates statistical significance.
Influence of Independent Variables on IKDC Score Using Linear Regression a
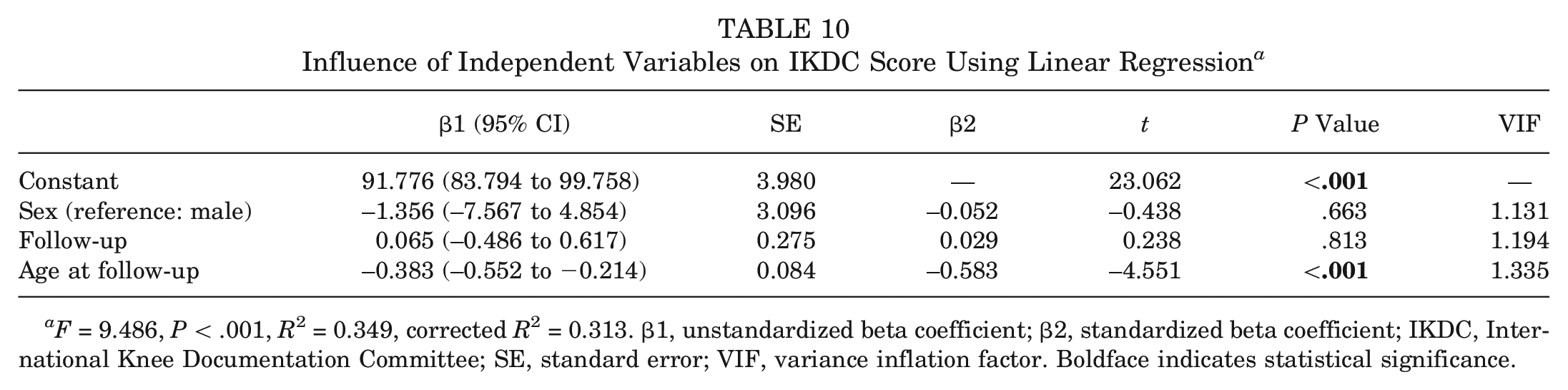
F = 9.486, P < .001, R2 = 0.349, corrected R2 = 0.313. β1, unstandardized beta coefficient; β2, standardized beta coefficient; IKDC, International Knee Documentation Committee; SE, standard error; VIF, variance inflation factor. Boldface indicates statistical significance.
Overall, 2 patients underwent partial meniscectomy because of a symptomatic recurrence of a discoid meniscus, while 2 other patients received a total knee prosthesis because of osteoarthritis. The mean reoperation time was 5.7 years (range, 1-10 years) (Figure 4). The 5-year survival rate was 96.5%, and it decreased to 90.6% at 10-year follow-up.
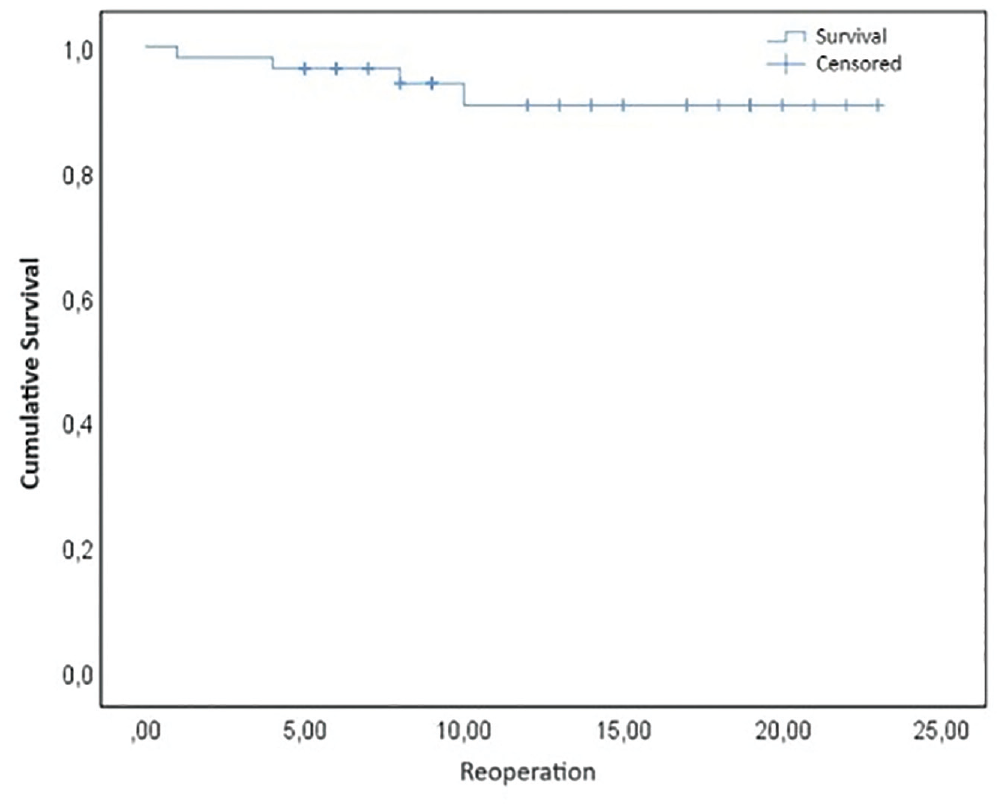
Survival analysis for time to reoperation.
Discussion
In the present study, the outcomes of patients with a DLM who underwent arthroscopic saucerization were examined, with a focus on midterm and long-term results. It was determined that the participants spanned a wide range of ages. While this finding aligns with the literature, it is possible to argue that a discoid meniscus, particularly in its complete form, presents at a younger age, tends to cause symptoms more frequently, and is the primary reason for seeking medical attention rather than accompanying injuries to other structures in the knee joint. A discoid meniscus typically manifests in older patients and is accompanied by concurrent intra-articular abnormalities and symptoms that may be coincidental or a result of deterioration in the meniscus structure. The higher clinical scores observed in the pediatric group in this study can be attributed to these factors. Similarly, although saucerization in the adult group did not prevent the progression of Kellgren-Lawrence grades, no significant distinction was observed between the preoperative and follow-up grades in the pediatric group. These may be considered to reflect the significance of a prompt surgical intervention.
The microscopic morphology of a discoid meniscus differs from that of a healthy meniscus. This distinction makes patients with a DLM more susceptible to injuries. Differences in force distribution produced by load bearing can lead to further degeneration and tears. The condition in question is especially important for young patients. It must be kept in mind that most tears in the meniscus among patients younger than 10 years originate from a discoid meniscus. 32 Given the delicacy of this particular age group, the effect of optimum care cannot be overstated.
When the radiological findings were evaluated based on age at the time of surgery, it was evident that the MJS and LJS values exhibited a large disparity. In addition, a weak negative correlation was demonstrated between age and FTA. When the radiological outcomes of the subgroups within the pediatric group were evaluated, no statistically significant difference was observed between the subgroups. This phenomenon might be attributed to the limited number of cases as well as to continuing maturation and the remarkable capacity to adapt during the course of growth. It has been reported that this adjustment could even potentially result in regeneration of the discoid meniscus.3,29 This disparity further underscores the significance of treatment in patients of a pediatric age.
It is important to consider the relationship between alignment and the extent of meniscal resection when assessing coronal-plane alignment of the knee joint. Additionally, it is necessary to provide a specific time frame for evaluation. Therefore, the outcome of a surgical intervention cannot be adequately revealed by cross-sectional investigations and studies with short follow-up periods.14,21 Research on alignment has shown that patients who underwent arthroscopic surgery had a higher incidence of valgus alignment and subsequent degeneration in the lateral compartment compared with those who underwent nonoperative treatment.5,14 According to another study, patients with varus alignment exhibited elevated clinical scores. 19 In the present cohort, the patients who underwent surgery at an older age tended to have their preoperative and follow-up FTAs shift toward varus alignment. This finding was consistent with the literature and indicates that patients who receive the optimum treatment for a DLM may expect a course of knee alignment similar to that of their healthy peers. 15
Declines in clinical scores have been reported at long-term follow-up of an arthroscopically treated DLM. 12 In our series, an increased follow-up duration was not associated with worse Lysholm or IKDC scores. Although patient numbers were limited, patient age had a negative influence on PROM scores, as would be expected from a naturally aging knee joint. These findings emphasize the positive effect of our surgical technique utilizing limited resection.
The surgical technique used in the present study involved reshaping the torn and degenerative discoid meniscus in a manner that did not compromise mechanical function. Additionally, efforts were made to maintain a wide peripheral rim of the meniscus. The objective was to provide specialized treatment for the discoid meniscus, which has a distinct collagen fiber arrangement that differs in structure and quantity from the typical meniscus. 2 Given that the average midlevel body width of a typical lateral meniscus is documented to be 8.3 mm, it is evident that a discoid meniscus with a body width of 6 mm after excision cannot perform at its best.8,10 Preserving the maximum amount of meniscal width may be of even greater importance in torn DLMs. 6 Moreover, postoperatively, the width of the discoid meniscus is subject to change. The height of the meniscal segments increases, and therefore, the width decreases. 25 These findings may be a result of compression and clumping of meniscal tissue during the follow-up period. This width decrease was related to meniscal extrusion and deformation. 24 An assessment of all the pertinent factors led to the conclusion that extensive resection should be avoided and sensitive meniscal tissue should be preserved to the greatest extent possible. 11 Therefore, valgus alignment, and thus lateral compartment degeneration, can be prevented.9,33 On the other hand, larger meniscal remnants were reported to be associated with increased tear rates. 13 In the present study, only 1 patient had a retear during the follow-up period, and no significant disparity was seen between preoperative and follow-up FTAs, thereby signifying a noteworthy outcome. However, we did not perform a risk analysis for a cut-off value of the remaining meniscal rim. Therefore, while promising, it is important to keep in mind that these data should be interpreted cautiously because 10 mm is not a definite cut-off value that leads to better outcomes.
The patients in the present study were categorized into 2 primary groups based on age and subsequently compared. The purpose of this grouping was to ensure a fair and balanced comparison of as many cases as possible. Observable disparities in radiological and clinical measurements were evident between the groups categorized as ≤18 and >18 years. Nevertheless, it is important to note that within both groups, there were varied presentations. Several factors such as skeletal development, age, reason for admission, and lower limb alignment exhibited a heterogeneous distribution. Each patient needs to be evaluated individually, regardless of age.
In the present study, the outcomes of patients who underwent arthroscopic treatment by a single surgeon utilizing the same technique and instruments were analyzed, with a focus on midterm and long-term follow-up. Thus, a conventional study protocol was established. Nevertheless, there are certain limitations in our study. It was conducted in a retrospective manner and lacks a control group. The study’s statistical power is limited because of the small sample size. Some of the surgically treated patients could not be analyzed because of the lack of follow-up. Selection bias arises for this particular reason. Lower extremity coronal-plane alignment was evaluated using standing knee AP radiographs. Full-length lower extremity radiographs were not used. This might have affected alignment-related outcomes because alignment and orientation are best assessed with full-length lower extremity AP radiographs. 27 To ensure more consistent results, the knee radiographs obtained before surgery and at the last follow-up were compared. Also, the majority of the operative notes lacked documentation of joint cartilage status, and hence, it was not included in the analysis. This is a limitation and could have an effect on the outcomes. Finally, a total of 6 menisci was repaired but not included in the comparisons or regression analyses as a subgroup because of the relatively low number of procedures. This potentially creates a confounding bias. Future studies addressing these shortcomings are essential to draw more evidence-based conclusions.
The reliability of the recorded data in this study is high. The patients completed translated and validated PROMs, and the senior author, as the sole medical provider, filled out standardized examination reports and operative charts immediately after each surgical procedure. This minimized the likelihood of recall bias.
A timely intervention is crucial when managing a symptomatic discoid meniscus. Current research has demonstrated that clinical and radiological outcomes are more unfavorable in patients who undergo surgical treatment during adulthood. With that being said, this finding may be attributed to patient age rather than the delay in treatment. Nevertheless, monitoring is still recommended in asymptomatic cases. During arthroscopic surgery, it is vital to thoroughly assess all components of the knee joint using the appropriate technique. While it is necessary to remove culprit meniscal tissue to decrease symptoms and ensure proper joint function, efforts should be made to preserve the meniscal width as much as possible. It is crucial to recognize that extensive excision of meniscal tissue might change its already sensitive microstructure and negatively affect its functionality.
Conclusion
This study suggests that saucerization of a DLM, while preserving a 10-mm peripheral rim, helped to preserve knee joint alignment in the long term. Functional and radiological outcomes were superior in pediatric patients. Future studies with higher quality evidence are warranted to guide individualized patient management.
Footnotes
Submitted July 10, 2024; accepted November 14, 2024.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
