Abstract
Background:
The optimal treatment strategy for patients with an anterior cruciate ligament (ACL) rupture is still under debate. Different determinants of the need for a reconstruction have not been thoroughly investigated before.
Purpose:
To investigate why, when, and which patients with an ACL rupture who initially started with rehabilitation therapy required reconstructive surgery.
Study Design:
Case-control study; Level of evidence, 3.
Methods:
In the Conservative versus Operative Methods for Patients with ACL Rupture Evaluation (COMPARE) trial, 167 patients with an ACL rupture were randomized to early ACL reconstruction or rehabilitation therapy plus optional delayed ACL reconstruction. We conducted an exploratory analysis of a subgroup of 82 patients from this trial who were randomized to rehabilitation therapy plus optional delayed ACL reconstruction. The reasons for surgery were registered for the patients who underwent a delayed ACL reconstruction. For these patients, we used the International Knee Documentation Committee (IKDC) subjective knee form, Numeric Rating Scale for pain, and instability question from the Lysholm questionnaire before surgery. To determine between-group differences between the nonoperative treatment and delayed ACL reconstruction group, IKDC and pain scores during follow-up were determined using mixed models and adjusted for sex, age, and body mass index.
Results:
During the 2-year follow-up of the trial, 41 of the 82 patients received a delayed ACL reconstruction after a median time of 6.4 months after inclusion (interquartile range, 3.9-10.3 months). Most reconstructions occurred between 3 and 6 months after inclusion (n = 17; 41.5%). Ninety percent of the patients (n = 37) reported knee instability concerns as a reason for surgery at the moment of planning surgery. Of these patients, 18 had an IKDC score ≤60, 29 had a pain score of ≥3, and 33 patients had knee instability concerns according to the Lysholm questionnaire before surgery. During follow-up, IKDC scores were lower and pain scores were higher in the delayed reconstruction group compared with the nonoperative treatment group. Patients in the delayed reconstruction group had a significantly younger age (27.4 vs 35.3 years;
Conclusion:
Patients who experienced instability concerns, had pain during activity, and had a low perception of their knee function had unsuccessful nonoperative treatment. Most patients received a delayed ACL reconstruction after 3 to 6 months of rehabilitation therapy. At baseline, patients who required reconstructive surgery had a younger age and higher preinjury activity level compared with patients who did not undergo reconstruction.
Finding out who needs which treatment at what moment is the challenge we try to solve after each anterior cruciate ligament (ACL) rupture. Currently, which treatment would be best for every patient cannot be determined on a scientific basis, and we do not know what treatment is successful in what situation. In a randomized controlled trial (RCT) comparing 2 different treatment strategies for ACL rupture, we found that early surgical reconstruction, compared with rehabilitation therapy with optional delayed reconstruction, resulted in improved clinical outcomes at a 2-year follow-up that were significant but of uncertain clinical importance. 18 This study (Conservative versus Operative Methods for Patients with ACL Rupture Evaluation [COMPARE] trial) showed that half of the patients who started with nonoperative treatment had satisfactory clinical results and did not need a surgical reconstruction during the 2-year follow-up period. 18 However, the other half of the patients received a delayed ACL reconstruction when nonoperative treatment failed. In the current study, we are looking for why, when, and in which patients nonoperative treatment failed. This has not been thoroughly investigated, especially not in an RCT study population.
In most studies and guidelines, symptomatic instability concerns are an indication for an ACL reconstruction if these concerns are not reduced after a physical therapy–guided exercise program or after adjustment of activity.10-12,15 Nevertheless, despite many objective measures of knee stability, objectifying how a patient perceives the instability remains a challenge, especially during activities of daily living. 19 So, the existing instruments do not predict the necessity for a reconstruction. Functional outcome measures may give a better indication of which patients need an ACL reconstruction. 5
Furthermore, few studies have described the time between starting nonoperative treatment and receiving an ACL reconstruction.21,23 The 2 existing RCTs described the average time to delayed ACL reconstruction, but timing for each patient has not been described yet.10,18 Investigating individual timing can give more insight into the distribution of time to delayed ACL reconstruction.
Therefore, the aim of the present study is to explore why, when, and which patients with an ACL rupture who started with rehabilitation therapy eventually had reconstruction, using data of the COMPARE trial. In this exploratory analysis, we evaluated which and how knee concerns, symptoms, and patient-reported outcome measures (PROMs) relate to the need for a delayed ACL reconstruction after failed nonoperative therapy.
Methods
Study Design and Patients
We used data of the COMPARE trial, a multicenter randomized controlled trial that recruited patients with an acute ACL rupture at 6 hospitals in the Netherlands. The research protocol was approved by the Erasmus MC University ethics committee, and the trial was registered with trial No. NL2618 in the Dutch trial registry. All participants provided informed consent. In the COMPARE trial, patients aged 18 to 65 years with an acute ACL rupture confirmed via magnetic resonance imaging scans and physical examination were included. Main exclusion criteria were history of ACL injury and a bucket-handle lesion of the meniscus with an extension deficit. Additional information about the recruitment process and exclusion criteria has been described in more detail in the article about the COMPARE trial. 18
Treatment
Patients were randomly assigned to early ACL reconstruction or rehabilitation therapy with optional delayed ACL reconstruction. Patients who were randomized to rehabilitation therapy started with a 3-month supervised physical therapy program as recommended by the Dutch ACL guideline. 15 In case of symptomatic instability concerns or the inability to reach a desired activity level, patients could receive an ACL reconstruction after a minimum of 3 months of rehabilitation therapy. Of the 167 included patients, 82 were randomized to rehabilitation plus optional delayed ACL reconstruction. For the present study, we restricted our analyses to the group of patients who were randomized to rehabilitation therapy with optional delayed ACL reconstruction.
Outcomes
The primary outcome of the COMPARE trial was the patients’ perception of symptoms, knee function, and ability to participate in sports activities as measured via the International Knee Documentation Committee (IKDC) subjective form score. The IKDC score ranges from 0 to 100, with 100 as optimal score. It is a validated and appropriate outcome measure to evaluate the recovery of patients with an ACL rupture.13,24
In the COMPARE trial, other validated questionnaires were also used for secondary outcomes, including the Lysholm questionnaire. This is a validated outcome measure to evaluate the functional status of patients with an ACL injury. 8 As a reflection of experienced instability, question 5 of the Lysholm score was used. This question asks, “Do you experience instability of your knee?” Scores for this question range from 0 (experiencing instability with every step) to 25 (never experiencing instability).
Pain severity during activities of daily living was determined via the Numeric Rating Scale (NRS) score, ranging from 0 to 10 (0 is equivalent to no pain).
In the COMPARE trial, patients filled out questionnaires at baseline and 3, 6, 9, 12, and 24 months after randomization. Last-reported PROMs before surgery were determined for every patient.
For each of these patients, we registered the reason for surgery during follow-up, as well as any patient’s preference for a reconstruction.
Data Analysis
We described patients from the rehabilitation plus optional delayed ACL reconstruction group of the COMPARE trial in an “as-treated” analysis. In this post hoc comparison, this group was divided into nonoperative treatment and delayed ACL reconstruction. The nonoperative treatment arm consisted of patients who did not receive an ACL reconstruction during the 2-year follow-up period. The delayed ACL reconstruction group consisted of patients who received an ACL reconstruction during the 2-year follow-up.
Distribution of time between inclusion and surgery, as well as reasons for surgery, are described for patients of the delayed ACL reconstruction group.
To give an overview of PROM scores before patients received a reconstruction, we made Venn diagrams with IKDC score, pain score (NRS) during activity, and patient’s experienced instability as separate categories. We evaluated how many patients had a low to moderate IKDC score (0-60) (based on normative IKDC scores in men and women aged 18 to 65 years 1 ), NRS score during activity ≥3 (moderate to severe pain), and instability score on the Lysholm questionnaire ≤20 of 25 (minimally experienced instability during athletics or other severe exertion). A Lysholm score of 20 was selected to also identify patients with minimal instability concerns. Venn diagrams were also made for both treatment groups at baseline, with similar categories.
To determine between-group differences (nonoperative treatment vs delayed ACL reconstruction) of IKDC and pain scores during follow-up, we used mixed models. IKDC score and NRS scores during activity, at baseline and at 3, 6, 9, 12, and 24 months, were used as dependent variables. The treatment group (nonoperative or delayed ACL reconstruction) was used as the independent variable. The interaction between follow-up and treatment group was added to the model as a fixed factor. The analysis was adjusted for potential confounders: sex, age, and body mass index (BMI). Surgeon was added as random factor into the model since the randomization was stratified for orthopaedic surgeon. All 6 participating hospitals had 1 or 2 orthopaedic surgeons performing ACL reconstructions, and all surgeons had a minimum of 10 years’ experience in performing ACL reconstructions. The alpha level was set at 0.05. We performed statistical analysis using IBM SPSS Statistics version 25.
Results
Patients
Half of the patients (n = 41) in the rehabilitation plus optional delayed ACL reconstruction group received an ACL reconstruction during the 2-year follow-up. This resulted in 41 patients in both the nonoperative treatment group and the delayed ACL reconstruction group.
Baseline characteristics are shown in Table 1. At baseline, patients in the delayed ACL reconstruction group had a significantly younger age, lower BMI, and higher preinjury Tegner score compared with patients in the nonoperative treatment group. They also injured their ACL more often during sports.
Baseline Characteristics of Patients in the Rehabilitation Plus Optional Delayed ACL Reconstruction Group a
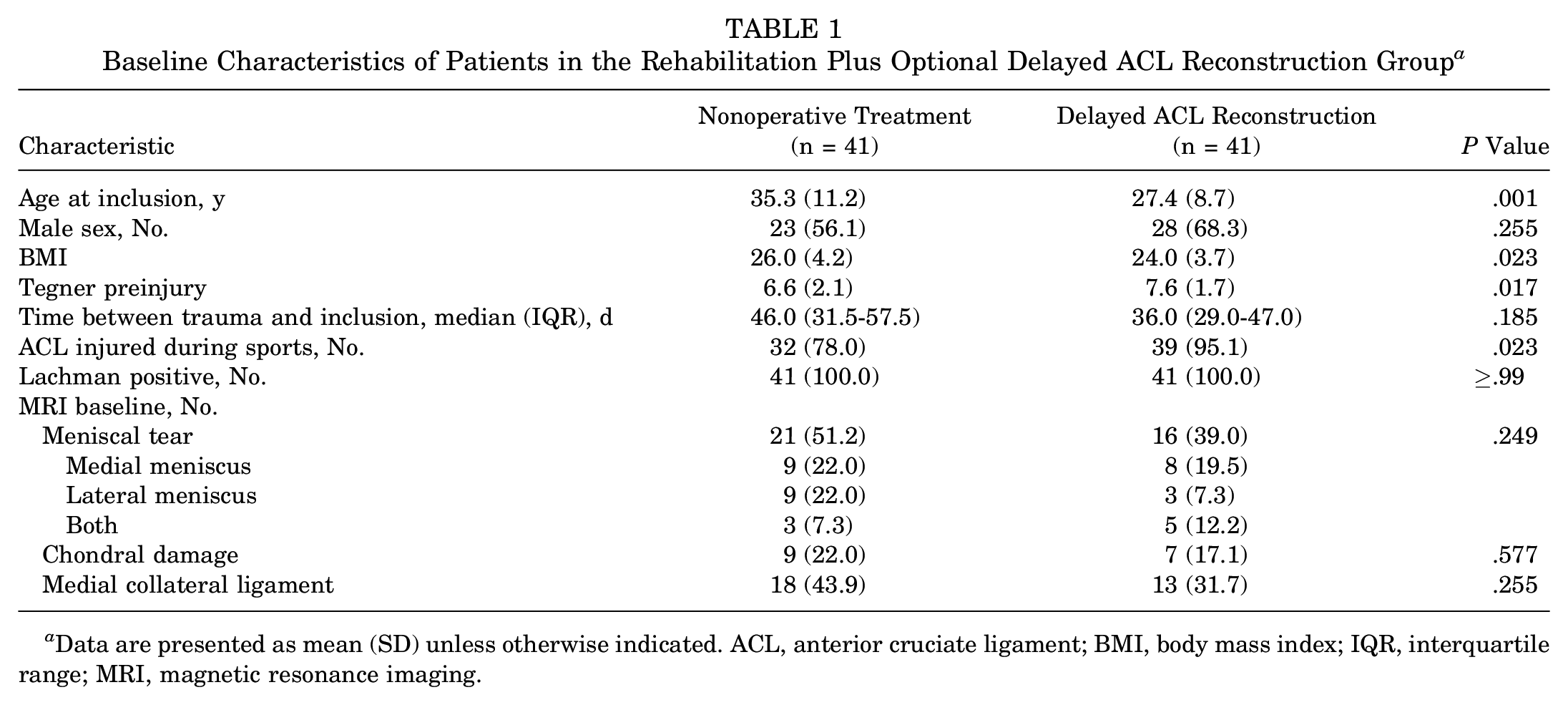
Data are presented as mean (SD) unless otherwise indicated. ACL, anterior cruciate ligament; BMI, body mass index; IQR, interquartile range; MRI, magnetic resonance imaging.
Delayed ACL Reconstruction Group
Median time from inclusion in the COMPARE study to delayed ACL reconstruction was 6.4 months (interquartile range, 3.9-10.3 months). Figure 1 shows the distribution of the time to surgery in months. Most patients (41.5%) underwent delayed ACL reconstruction between 3 and 6 months after inclusion (median, 3.8 months). One protocol violation occurred; 1 patient underwent ACL reconstruction 9 days after inclusion after receiving a second opinion from a surgeon at a nonparticipating private medical center who recommended and performed surgery within 2 days.
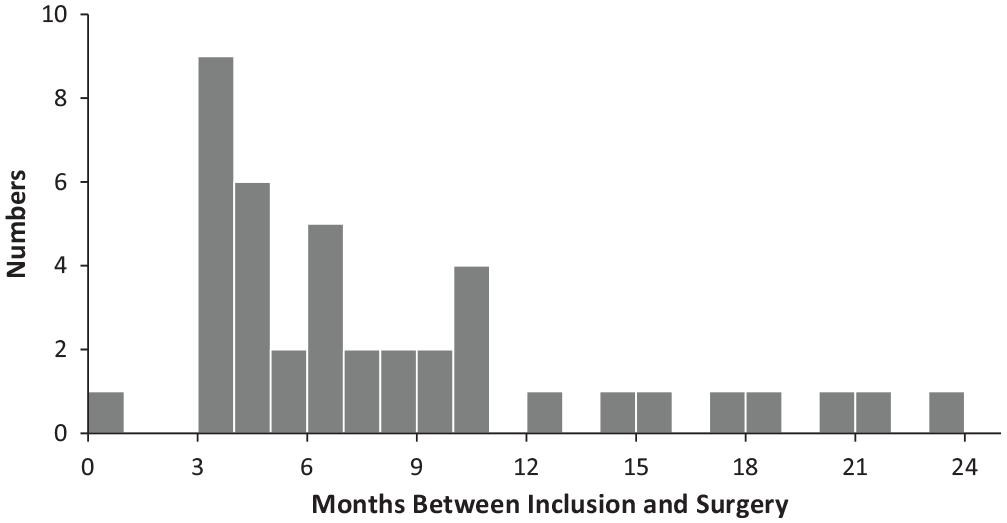
Time between inclusion and delayed anterior cruciate ligament reconstruction. “Numbers” represents number of patients.
Most patients (n = 37; 90.2%) reported knee instability concerns as the reason for surgery. Of these patients, 27% (n = 10) had a strong preference for surgery. Of the remaining 4 patients, 2 had a strong preference for surgery without instability concerns, 1 patient had a reason for surgery not reported in the medical records, and 1 patient went to another hospital where surgery was recommended (protocol violation mentioned earlier). In total, 29.3% (n = 12) of the patients had a strong preference for surgery, 9 of these patients (75%) underwent ACL reconstruction between 3 and 6 months after inclusion.
Figure 2 shows PROM scores of patients before they underwent a delayed ACL reconstruction. Of the 41 patients, 18 patients (43.9%) had a low to moderate IKDC score, 29 patients (70.7%) had a pain score of ≥3, and 33 patients (80.5%) reported instability in the Lysholm questionnaire. In total, 17 patients (41.5%) scored positive on all 3 items.
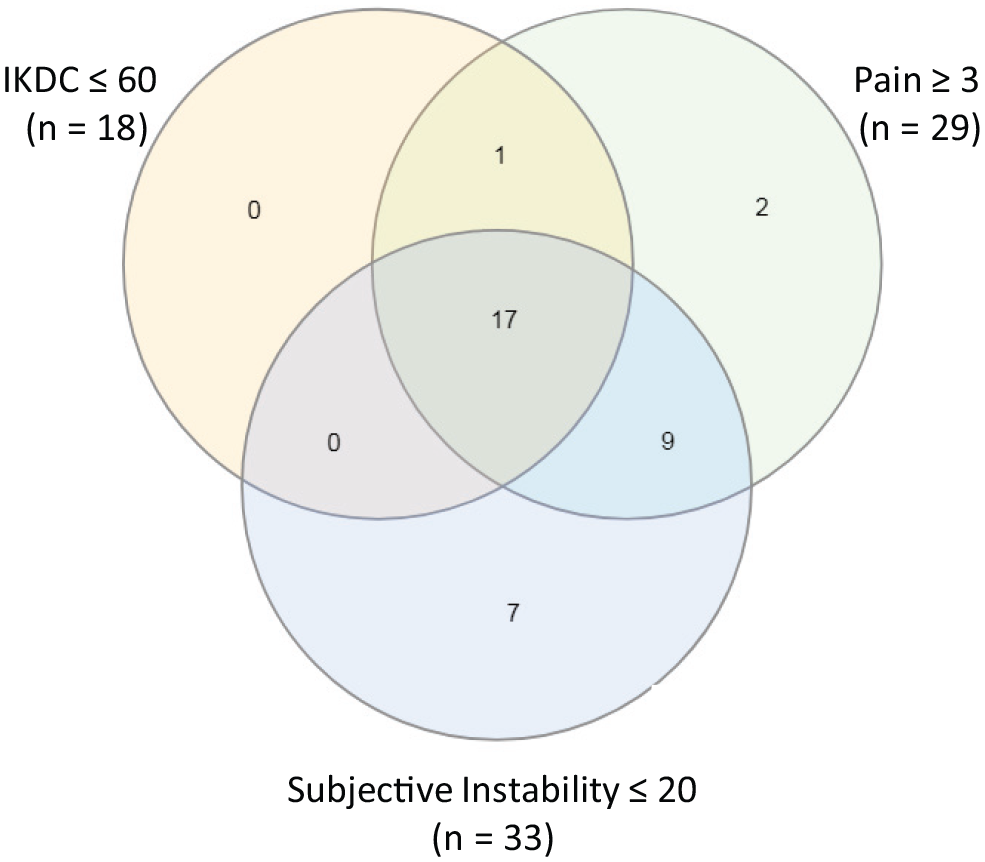
Delayed anterior cruciate ligament reconstruction group—patient-reported outcome measures before surgery. IKDC, International Knee Documentation Committee.
In the nonoperative treatment group, at baseline, 33 patients (80.5%) had a low to moderate IKDC score, 34 patients (82.9%) had a pain score of ≥3, and 33 patients (80.5%) reported instability. In the delayed ACL reconstruction group, the numbers of patients in these groups were respectively 27 patients (65.9%), 32 patients (78.0%), and 27 patients (65.9%), as shown in Figure 3.
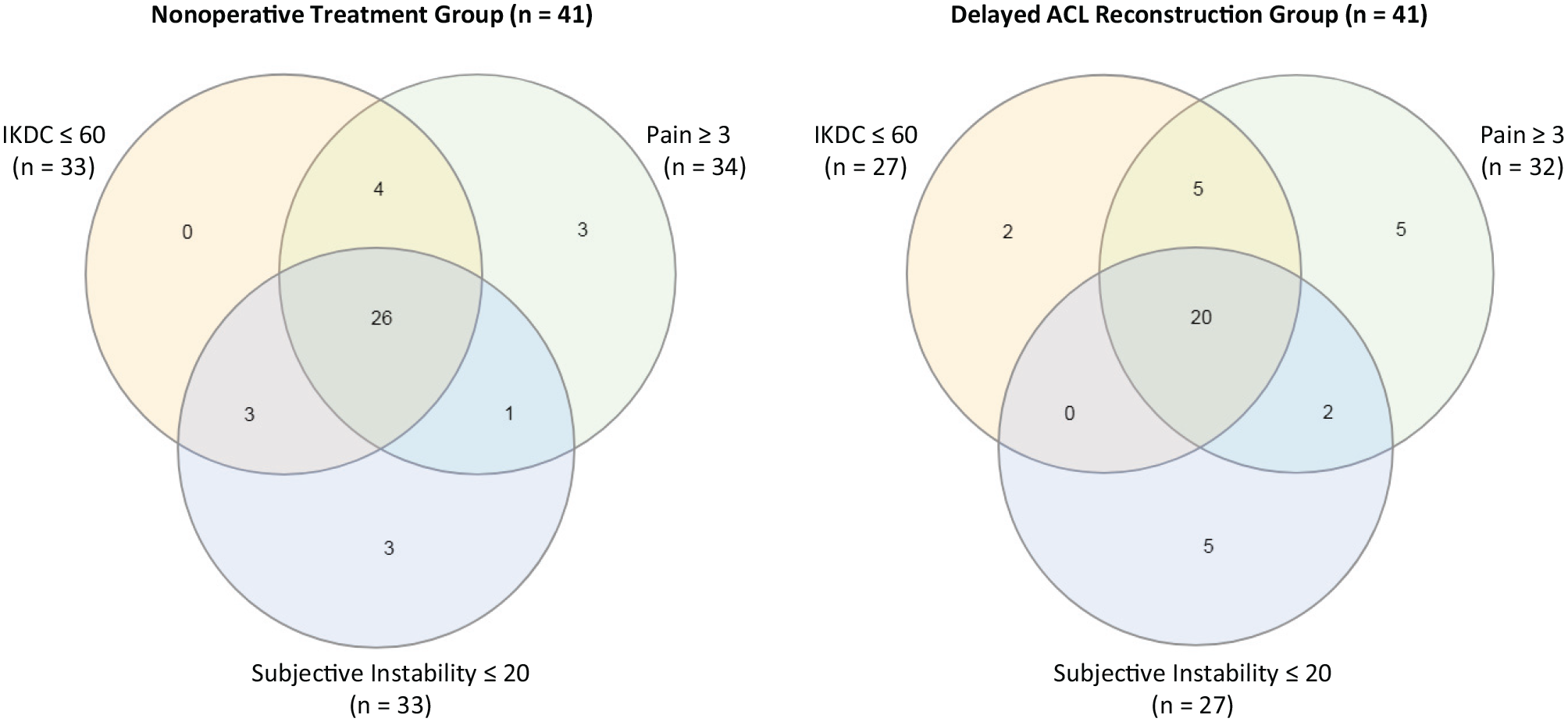
Baseline patient-reported outcome measures. ACL, anterior cruciate ligament; IKDC, International Knee Documentation Committee.
Of the 33 patients who experienced instability concerns according to the last PROMs before surgery, 39.4% (n = 13) had the same level of instability concerns at baseline, and 27.3% (n = 9) had no instability concerns at baseline but developed these during follow-up. The other patients had instability concerns at baseline that worsened (12.1%; n = 4) or improved (21.2%; n = 7) before surgery.
IKDC Score Over Time
Figure 4 and Table 2 show the IKDC score during follow-up for both as-treated groups. Patients of the delayed ACL reconstruction group were no longer included in the analysis from the moment of ACL reconstruction onward. Before patients underwent delayed ACL reconstruction, they had a decrease in IKDC score, while patients who did not undergo ACL reconstruction showed an increase in IKDC score over time. At 3, 6, 9, and 12 months, patients of the delayed ACL reconstruction group had a lower IKDC score compared with patients in the nonoperative treatment group. Because of potential indication bias and a decrease in the number of patients in the delayed reconstruction group, statistical analysis was not performed.
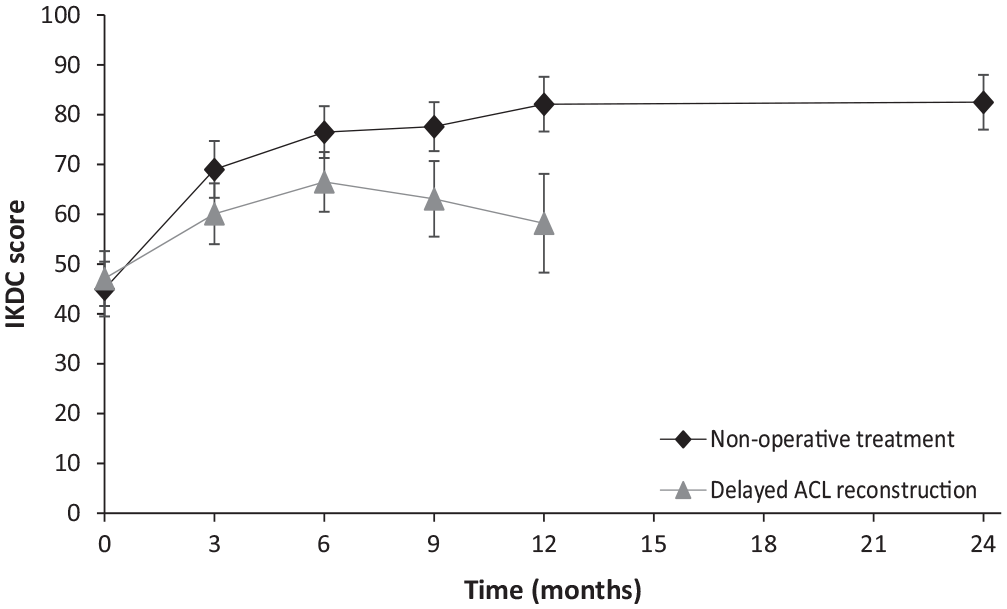
International Knee Documentation Committee (IKDC) score over time. ACL, anterior cruciate ligament. Bars represent 95% CIs.
As-Treated Analysis IKDC Score (Estimated IKDC) a
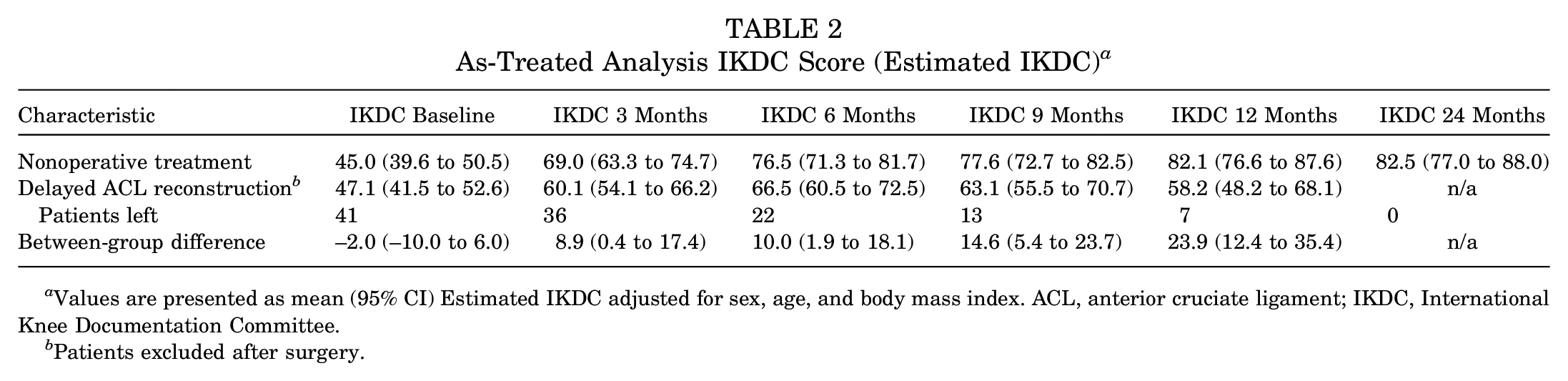
Values are presented as mean (95% CI) Estimated IKDC adjusted for sex, age, and body mass index. ACL, anterior cruciate ligament; IKDC, International Knee Documentation Committee.
Patients excluded after surgery.
Pain During Activity Over Time
The Appendix (available in the online version of this article) shows NRS pain scores during activity during follow-up for both as-treated groups. Patients of the delayed ACL reconstruction group were excluded from the analysis after they underwent reconstruction. Patients of the delayed ACL reconstruction group had a higher pain score before they underwent reconstruction compared with the nonoperative treatment group at 3, 6, 9, and 12 months of follow-up.
Discussion
In this exploratory analysis of data of the COMPARE trial, we described patients with an ACL injury who had unsuccessful nonoperative treatment. The symptoms these patients experienced before they received an ACL reconstruction were instability concerns, pain during activity, and a low perception of their knee function indicated by a low IKDC score. Furthermore, we found that 41.5% of the patients received an ACL reconstruction after 3 to 6 months of rehabilitation therapy. Patients with unsuccessful nonoperative treatment had a significantly younger age and higher preinjury activity level.
In our study, most patients who were randomly assigned to rehabilitation therapy plus optional delayed ACL reconstruction received surgery after 3 to 6 months of rehabilitation therapy. A possible explanation for this peak is the presence of a strong preexisting preference for surgery in 29.3% of the patients (n = 12). After the minimum period of 3 months of rehabilitation therapy according to the study protocol was completed, 9 of these patients (75%) underwent an ACL reconstruction within 3 months. Most patients reported instability concerns as the reason for surgical treatment. At baseline, not all of these patients experienced instability concerns according to their Lysholm score. This indicates that symptomatic instability can also become a problem later on during the nonoperative treatment period. After 1 year, patients still received an ACL reconstruction in our study. Frobell et al 11 reported similar results; in their study, some patients even received surgery after 2 years of nonoperative treatment because of new instability concerns.
At the last questionnaires before delayed ACL reconstruction, 43.9% of the patients experienced a low IKDC score, 70.7% reported moderate to severe pain during activity, and 80.5% experienced some degree of symptomatic instability. Patients in the delayed reconstruction group reported these 3 symptoms more often compared with patients in the nonoperative treatment group. Also during follow-up, patients who eventually received surgery showed worsening IKDC and pain scores.
Most patients received an ACL reconstruction after 3 to 6 months of nonoperative treatment, but we also found that some patients developed instability concerns after a longer period of nonoperative treatment and then received an ACL reconstruction. Furthermore, symptomatic instability concerns appear to be the main reason for patients to receive an ACL reconstruction, but patients also experience other symptoms, such as a less optimal knee function (IKDC score ≤60) and pain during activities of daily living (NRS ≥3).
In our study, symptomatic instability was the most important factor in receiving an ACL reconstruction after a period of nonoperative treatment. These instability moments and the consequent concerns could increase the risk for additional intra-articular damage in the ACL-deficient knee, but the evidence for this hypothesis is not conclusive. 6 There is also no consensus about which level of instability concerns is clinically acceptable. Different objective measures of knee instability have been developed over the past years.17,25 These measures include different techniques to quantify knee instability, such as imaging techniques to detect rotational and anterior-posterior instabilities, 16 devices to measure knee laxity, 22 and gait analysis.2,20 However, the question is to what extent these measures correlate with the amount of instability that is experienced by the patient. Objectifying knee instability that patients experience during daily living still remains a challenge. 19 Laxity in the knee joint measured via different diagnostic techniques is different from instability experienced by the patient.
In our study, we focused on instability experienced by the patient since this is in our opinion the best representation of how a patient experiences concerns in daily living. We found that patients with an ACL-deficient knee reported different levels of symptomatic instability and that even patients who rarely experienced knee instability also received an ACL reconstruction. It is possible that these patients have such a high desired activity level that they do not accept any experienced knee instability. Furthermore, we showed that in the delayed ACL reconstruction group, there were both patients who already had instability concerns at baseline and patients who developed instability concerns during follow-up. This could indicate that symptomatic instability of the knee is fluid or that instability concerns change over time because of changes in activity level or changes in desired knee function.
Besides symptomatic instability, patient preference also plays an important role in the decision-making process for surgery. This has evolved into more emphasis on shared decision making, which has been defined as “an approach where clinicians and patients share the best available evidence when faced with the task of making decisions, and where patients are supported to consider options, to achieve informed preferences.” 7 We tried to objectify as many of these parameters as possible in our study and are further developing this area, where patients’ and physicians’ preferences are part of the decision making.
At baseline, patients in the delayed ACL reconstruction group had a significantly younger age and higher preinjury Tegner score compared with patients in the nonoperative treatment group. Although we focused on PROMs at the moment of decision making for ACL reconstruction, these differences in baseline characteristics cannot be ignored. Activity level is probably the most important predictor for the necessity of an ACL reconstruction. 15 It is thought that the more a patient practices pivoting sports, the greater chance this patient needs a reconstruction.3,4,9,14 In our study, patients who needed a reconstruction also had a younger age compared with the patients who were successful with nonoperative treatment. This is similar to the study by Eitzen et al, 5 who also found a younger age in patients who needed an ACL reconstruction.
A limiting factor of this study is that deciding to perform an ACL reconstruction is a subjective decision of both the orthopaedic surgeon and the patient. In this study, we tried to objectify multiple aspects of this decision making, such as symptoms before surgery and time to surgery. However, it is hard to quantify and qualify all aspects of decision making. In clinical practice, patients visit the surgeon with specific concerns and wishes, but these are not always comparable with the filled-out questionnaires at each time point. We still aimed to cover all aspects of unsuccessful nonoperative treatment by investigating it from different perspectives; namely, why, when, and which patients needed an ACL reconstruction. Another limitation is the potential presence of recruitment bias in the COMPARE trial because 41% of the eligible patients declined to participate in the trial. Furthermore, the relatively small sample sizes in each group led to a higher fragility index.
In conclusion, our current study provides more insight in patients who have unsuccessful nonoperative treatment after an ACL injury. To our knowledge, this is the first study that describes why, when, and which patients with an ACL injury who started with nonoperative treatment received an ACL reconstruction in an RCT setup. We found that patients who received surgery experienced more knee instability, had lower IKDC scores, and reported more pain during activity compared with patients who followed a nonoperative treatment successfully. Most patients had unsuccessful nonoperative treatment after 3 to 6 months of rehabilitation therapy, but some, after a longer period of nonoperative treatment. Patients who received surgery had a younger age and higher preinjury activity level at baseline.
Supplemental Material
sj-pdf-1-ajs-10.1177_03635465211068532 – Supplemental material for Why, When, and in Which Patients Nonoperative Treatment of Anterior Cruciate Ligament Injury Fails: An Exploratory Analysis of the COMPARE Trial
Supplemental material, sj-pdf-1-ajs-10.1177_03635465211068532 for Why, When, and in Which Patients Nonoperative Treatment of Anterior Cruciate Ligament Injury Fails: An Exploratory Analysis of the COMPARE Trial by Sabine J.A. van der Graaff, Duncan E. Meuffels, Sita M.A. Bierma-Zeinstra, Eline M. van Es, Jan A.N. Verhaar, Vincent Eggerding and Max Reijman in The American Journal of Sports Medicine
Footnotes
Acknowledgements
The authors thank J.H. Waarsing for supporting the data analysis.
Submitted May 26, 2021; accepted November 1, 2021.
One or more of the authors has declared the following potential conflict of interest or source of funding: A grant for this study was received from ZonMw, a Dutch organization for health research and care innovation. The funder of the study had no role in study design, data collection, data analysis, data interpretation, or writing of the report. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
