Abstract
Nitrous oxide (N2O) is a potent greenhouse gas used to provide analgesia and anaesthesia in healthcare. Leaks from the manifold-pipeline systems may result in significant losses of N2O before delivery to the patient. The provision of N2O by cylinder at point-of-care is proposed as a leak-reducing alternative to manifold-pipeline systems. The primary endpoint of this study was to determine the percentage of anaesthetists who considered it acceptable for N2O to be supplied by cylinder rather than a manifold-pipeline system. It also explored the current application of N2O and prevailing attitudes toward its environmental impact and future role in anaesthetic practice. A cross-sectional survey was administered in 2023 among anaesthetists working across seven metropolitan hospitals in New South Wales, Australia. Participants provided self-reported information on demographics, practice characteristics, views on climate change, the role of anaesthetists in addressing environmental concerns, routine N2O usage, and the potential shift to cylinder supply of N2O. Among the 287 respondents, the majority (n=241, 84.6%) were current users of N2O, although most administered it infrequently (71.5% used it in less than 25% of cases). Attitudes regarding N2O’s environmental impact varied irrespective of career stage. Notably, 219 of 287 (76.3%) favoured using cylinders over the manifold-pipeline network. These findings indicate a decreasing trend in N2O usage, especially among early career anaesthetists, and suggest that transitioning to cylinder supply is acceptable, provided that strategies are in place to manage supply disruptions without compromising patient care.
Introduction
Climate change is the most significant global challenge facing the modern world. Nitrous oxide (N2O) is one of the four long-lived greenhouse gases created by human activities. 1 The amount of atmospheric heat absorbed by a given substance per kilogram is called its global warming potential (GWP). The reference gas for this metric is carbon dioxide (CO2), which has a GWP of 1. Nitrous oxide has a GWP of 265. 2
Approximately 7% of Australia’s total carbon footprint comes from the healthcare sector, of which 44% is generated by hospitals. 3 Approximately 92% of emissions in the healthcare sector are indirect and are the result of ‘supply chains involved in the manufacture, distribution and supply of health care goods and services’. 4 Approximately 8% of emissions in the healthcare sector are direct and are the result of ‘stationary fuel use, anaesthetic gases, or fuel use in vehicles owned or leased by the health system’. The use of N2O constitutes a direct emission and accounted for 2.19% of Australia’s total healthcare sector emissions in the 2021/2022 financial year. 4
In Australia, between 2017 and 2022, the annual data for N2O procurement in public hospitals were obtained. The total annual procurement of N2O was 242,054 kg and is equivalent to the annual carbon emissions of over 36,000 cars. 5
An estimate from the UK indicated that N2O may have accounted for up to 80% of National Health Service (NHS) England’s anaesthetic greenhouse gas emissions in 2017. 6 In Australia, N2O is estimated to account for 93% of the health system’s anaesthetic gas emissions. 4 Studies in Scotland, New Zealand, and Australia have all shown that up to 75 to 95% of stored N2O escapes from manifold-pipeline networks before delivery to the patient.7–9 A quality improvement project at a large New South Wales (NSW) tertiary children’s hospital found an approximately 50% leakage/wastage rate of N2O, contributing 621 tonnes of CO2 equivalents annually. 10
Portable cylinders attached to anaesthetic machines are an alternative to hospital manifold-pipeline networks for supplying N2O for use with patients. The UK NHS’s Nitrous Oxide Project and the American Society of Anesthesiologists have both advocated for this approach.11,12
Previous studies have examined the use of N2O by anaesthetists.13,14 However, the perspectives of anaesthetists regarding modifications to their practice or their views on N2O, administration, and the challenges associated with transitioning to alternative supply methods have not been documented in NSW.
The objectives of this study were to 1) determine the percentage of anaesthetists who considered that it was acceptable for N2O to be supplied by cylinder rather than by a manifold-pipeline system, 2) understand changes in N2O use by NSW anaesthetists, 3) identify attitudes about the GWP of N2O and the future of N2O use in anaesthetic practice in NSW, and 4) gauge whether career stage affected these attitudes.
Materials and methods
Study design
This survey employed a cross-sectional study design. In 2023, an invitation to participate in the survey was distributed using the routine mailing list of each department of anaesthesia at seven NSW hospitals: Royal Prince Alfred Hospital, Concord Hospital, Canterbury Hospital, Royal North Shore, Ryde Hospital, Hornsby Ku-ring-gai Hospital and The Children’s Hospital at Westmead. A follow-up reminder email was distributed after 2 and 4 weeks. No incentives were offered to participants to complete the survey. These hospitals were chosen because they were in three different local health districts, one of which was a paediatric hospital, and four contained birthing units. The number of hospitals chosen was limited due to delays in obtaining individual hospital site-specific ethics approval.
Participants
The inclusion criteria for this study were employment as a trainee- or consultant anaesthetist at one of the seven selected hospitals. The total number of recipients on each routine mailing list formed the denominator.
Variables
The survey consisted of 16 questions (Appendix 1). Questions 1 to 4 collected information about individual anaesthetist’s demographics (including age and years of training), and their volume of clinical practice (sessions of anaesthetic practice per week, total number of cases per week). Age and years of training were presented as 10-year groups in the questionnaire. Questions 1 to 4 were compulsory for all respondents. Questions 5 to 10 collected information on individual anaesthetist’s use of N2O (use in the last 12 months, percentage of cases N2O is used, use at different stages of anaesthesia, and any changes in current practice). Respondents who answered ‘No’ to Question 5 (Have you used N2O within the last 12 months?) were directed to Question 11 (respondent’s opinion about N2O’s role in modern anaesthetic practice). Questions 12 to 16 collected information about respondents’ opinions on climate change, the role of anaesthetists in climate action, N2O’s use in anaesthesia, and its future use in NSW. Questions 10, 11 and 15 allowed multiple responses to be recorded. Questions 10, 15 and 16 allowed a free-text response. The principal site of practice for each respondent was not collected.
Quantitative variables
The respondents’ level of training was dichotomised into early career anaesthetists (ECAs, i.e. trainees and consultant anaesthetists practising for up to 10 years) and mid-to-late career anaesthetists (MLCAs; consultant anaesthetists practising for 11 years or more).
Data sources/measurement
Data were collected and managed using Research Electronic Data Capture (REDCap), a secure web platform hosted by the Sydney Local Health District. 15
Statistical methods
All data analysis was undertaken using IBM SPSS Statistics (IBM Corp. Released 2023. IBM SPSS Statistics for Windows, Version 29.0.2.0, Armonk, NY). Respondents’ demographics, N2O use, and opinions about N2O categories were analysed descriptively; categorical data are presented as frequencies (percentage) and continuous data as mean, range and standard deviation (SD). Differences in distribution for categorical data were analysed using a chi-square or Fisher’s exact test. In all instances, differences in distribution for categorical data were compared between ECAs and MLCAs. Bonferroni correction was used in cases of multiple comparisons to control for type 1 error. The adjusted P-value was calculated by multiplying the P-value by the number of comparisons. For example, a P-value of 0.02 with four comparisons would have an adjusted P-value of 0.02*4=0.08. The adjusted P-value was capped at 1.00. A P-value less than 0.05 was considered statistically significant.
Ethics
The Sydney Local Health District ethics committee approved this study (2023/ETH00181 and X23-0026).
Results
Participants
The survey was distributed to 499 eligible staff. The response rate was 57.1% (285 of 499), with 285 complete surveys and two partially complete surveys available for analysis. The two partially complete surveys did not have responses to the questions relating to N2O use (Questions 5 to 10). All other questions were answered. A summary of the respondents’ demographics is shown in Table 1. ECAs were younger (25 to 34 years, n=33 (22.6%); 35 to 44 years, n=95 (65.1%); 45 to 55 years, n=18, (12.3%)) than MLCAs (35 to 44 years, n=7 (5.0%); 45 to 55 years, n=73 (51.8%); 55 to 64 years, n=52 (36.9%); 65 to 74 years n=9 (6.4%)). A summary of the average number of sessions (5 h) and the average number of cases respondents performed per week is shown in Table 2.
Years of training and age of anaesthetists.
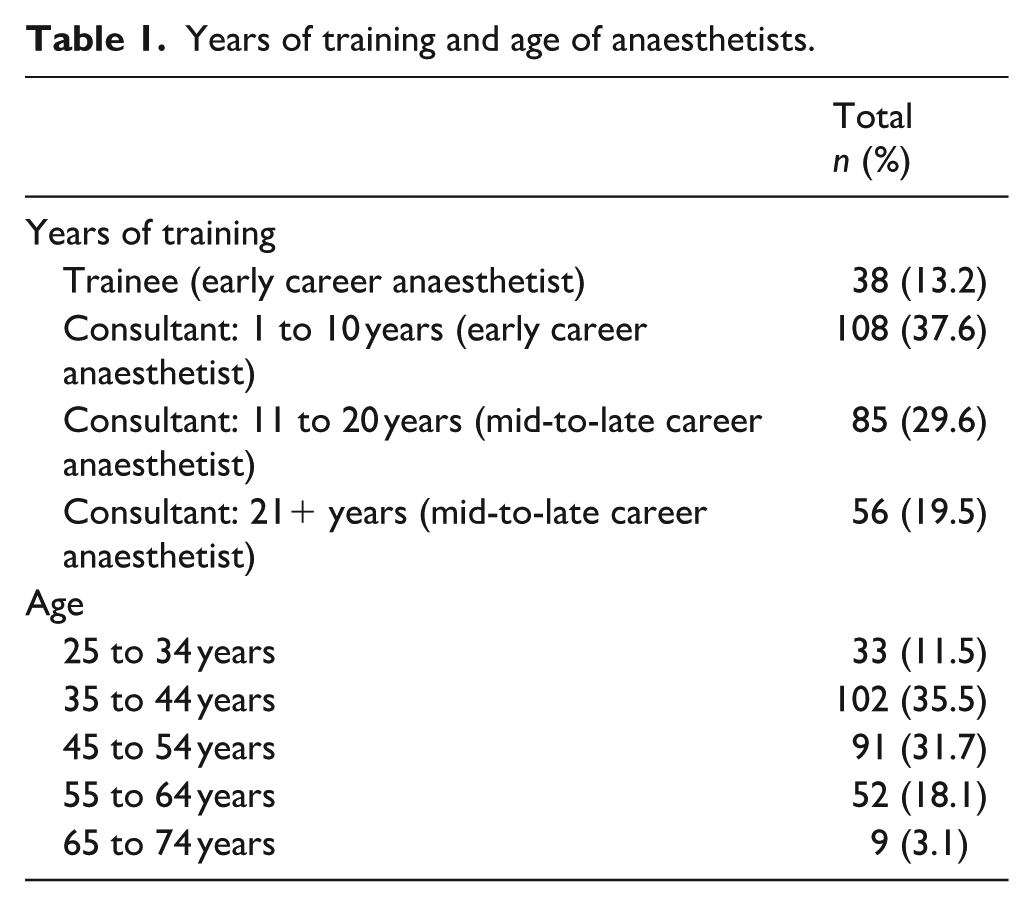
The average number of sessions (5 h) and cases performed per week by anaesthetists.
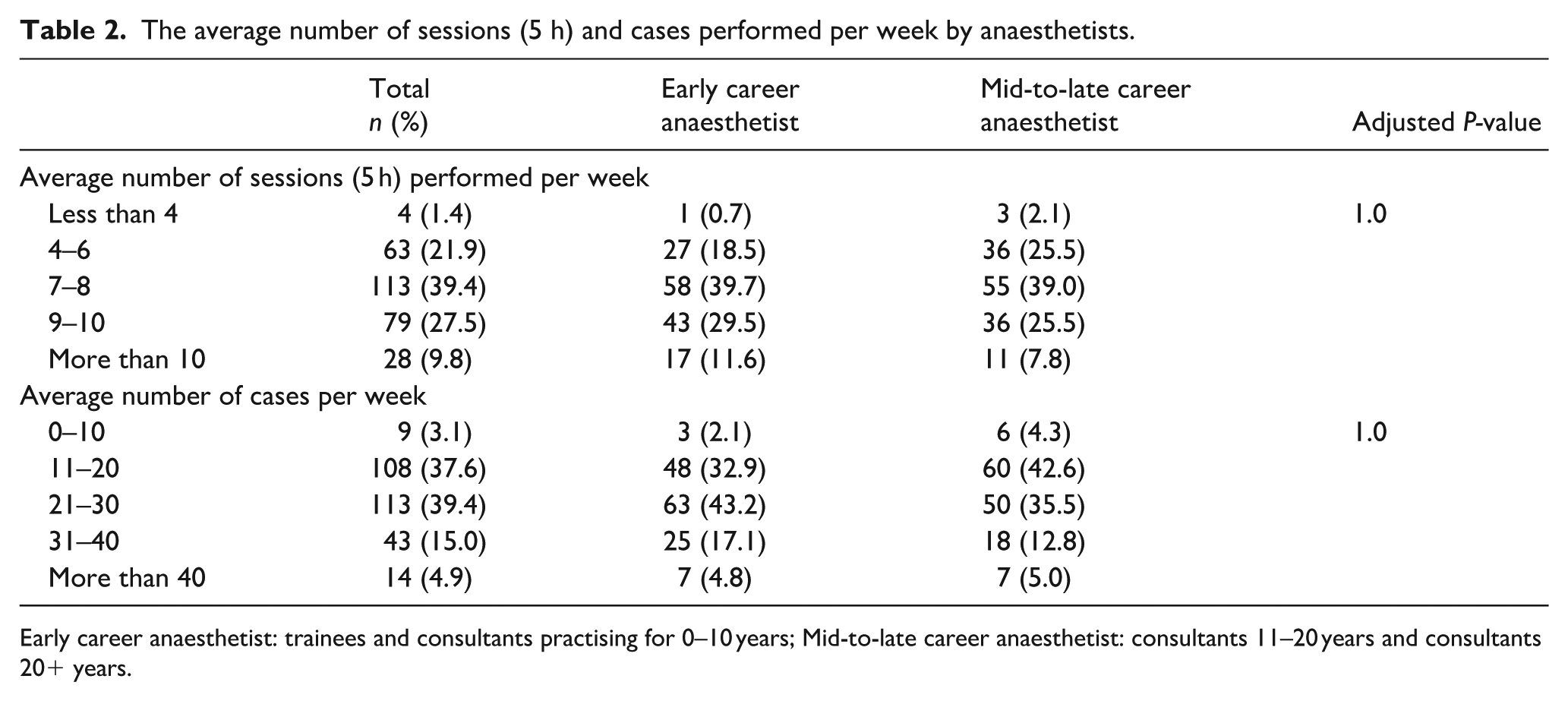
Early career anaesthetist: trainees and consultants practising for 0–10 years; Mid-to-late career anaesthetist: consultants 11–20 years and consultants 20+ years.
NSW anaesthetists’ opinions about N2O supply
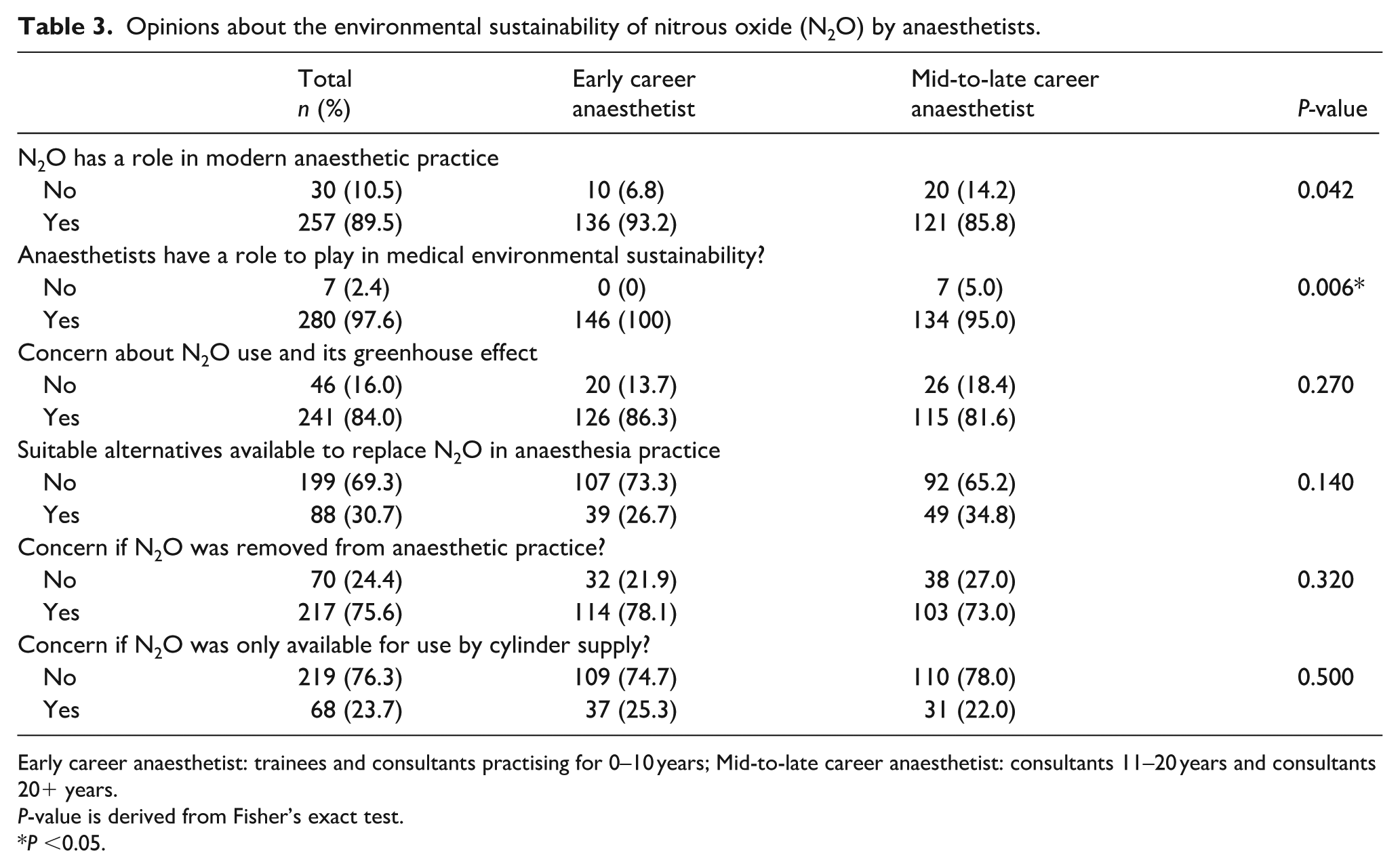
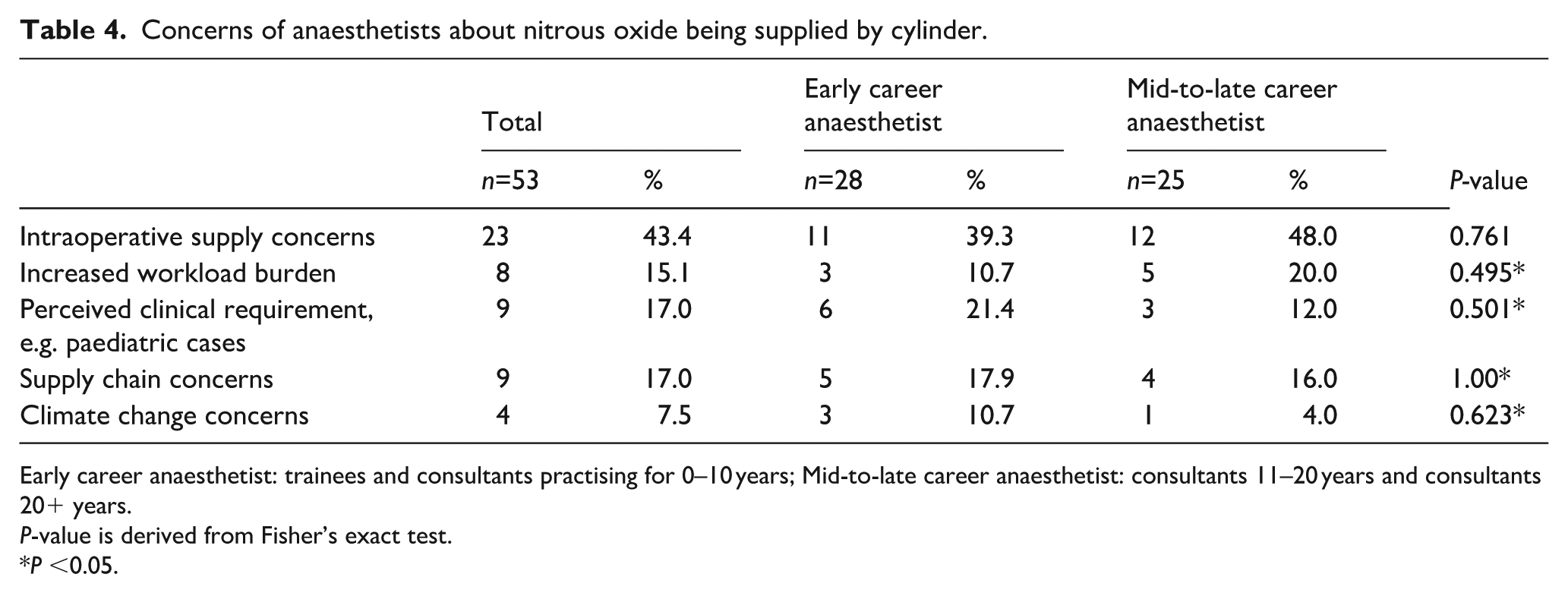
A summary of the respondents’ opinions about N2O is shown in Table 3. Anaesthetists were mostly not concerned about N2O being provided for use by cylinder supply (219 of 287 (76.5%), χ2 (1, n=287)=0.45, P=0.504). Of the 68 respondents expressing concerns if N2O was only available for use by cylinder supply, 53 (77.9%) provided comments detailing their concerns. These concerns were grouped into common themes, and the results are shown in Table 4. The primary concern was that the supply would run out during an operation.
Opinions about the environmental sustainability of nitrous oxide (N2O) by anaesthetists.
Early career anaesthetist: trainees and consultants practising for 0–10 years; Mid-to-late career anaesthetist: consultants 11–20 years and consultants 20+ years.
P-value is derived from Fisher’s exact test.
P <0.05.
Concerns of anaesthetists about nitrous oxide being supplied by cylinder.
Early career anaesthetist: trainees and consultants practising for 0–10 years; Mid-to-late career anaesthetist: consultants 11–20 years and consultants 20+ years.
P-value is derived from Fisher’s exact test.
P <0.05.
N2O use by NSW anaesthetists
Two respondents did not answer Questions 5 to 10, leaving 285 of 287 responses for analysis. Table 5 summarises how respondents use N2O in their current practice. Most respondents had used N2O in the last 12 months. ECAs and MLCAs were equally likely to have used N2O in the previous 12 months (χ2 (1, n=285)=3.12, P=0.077). ECAs were more likely to use N2O in less than 25% of sessions than MLCAs (χ2 (3, n=241)=8.00, P=0.046). ECAs were more likely than MLCAs to have reduced their use of N2O in the past 12 months (χ2 (2, n=241)=9.61, P=0.006).
The use of nitrous oxide (N2O) by anaesthetists.
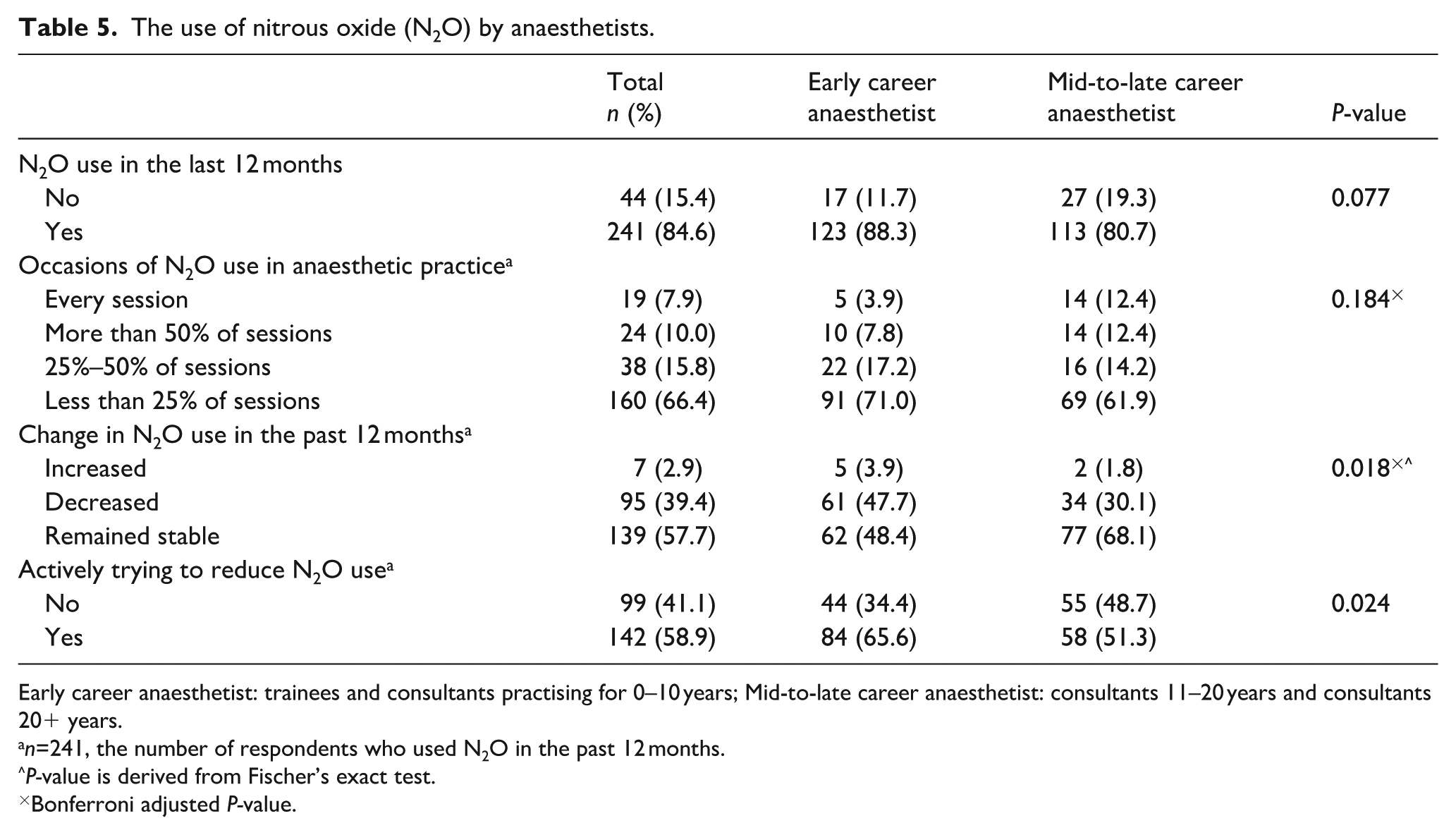
Early career anaesthetist: trainees and consultants practising for 0–10 years; Mid-to-late career anaesthetist: consultants 11–20 years and consultants 20+ years.
n=241, the number of respondents who used N2O in the past 12 months.
P-value is derived from Fischer’s exact test.
Bonferroni adjusted P-value.
Stage of anaesthesia
Respondents predominantly used N2O during the induction phase of anaesthesia (induction n=133, 55.2%; maintenance n=36, 14.9%; roughly equal induction and maintenance n=72, 29.9%). The mean flow rate for induction was 4.9 L/min (SD 1.8; range 0.5 to 12.0 L/min). The mean flow rate for maintenance was 1 L/min (SD 0.8; range 0.1 to 6.0 L/min). ECAs and MLCAs showed no statistical difference in regard to which stage of anaesthesia they used N2O (χ2 (2, n=241)=5.62, P=0.060).
The rationale for reducing or maintaining N2O use
Of the 241 respondents who had used N2O in the last 12 months, 142 (58.9%) had actively tried to reduce the amount of N2O they used. ECAs were more likely than MLCAs to have actively tried to reduce their N2O use (χ2 (1, n=142)=5.10, P=0.024). Overall, this was primarily through reduced utilisation in cases (n=121, 85.2%), followed by reduced flow rate (n=73, 51.4%) and reduced inspired fraction of N20 (n=23, 16.2%). For the respondents who were not actively trying to reduce their use of N2O (n=98), ‘already restricting the use of N2O to specific cases’ was listed as the most common reason (n=74, 75.5%). Of the total sample, 25% preferred not to change their anaesthetic practice, 6% did not believe N2O contributes to global warming, 4% were uncertain about the impact of N2O on global warming, and 1% did not believe humans contributed to global warming. Twelve respondents entered free-text comments about the reasons for not changing their practice. These fell into two main groups: seven respondents felt practitioners should have sole choice over the drugs they use, and five stated the impact anaesthetists had on global warming was negligible when compared to other sources of greenhouse gas emissions.
NSW anaesthetists’ opinions about N2O
ECAs were more likely than MLCAs to think that N2O has a role in modern anaesthetic practice (χ2 (1, n=287)=4.12, P=0.042). The areas of modern anaesthetic practice in which respondents believed N2O still had a place are summarised in Table 6. MLCAs were less likely to think that anaesthetists have a role to play in medical environmental sustainability, P=0.006. Overall, anaesthetists were concerned about N2O use and its greenhouse effect (χ2 (1, n=287)=1.20, P=0.274). As a group, anaesthetists felt no suitable alternatives were available to replace N2O in anaesthesia practice (χ2 (1, n=287)=2.18, P=0.140) and would be concerned if N2O was removed from anaesthetic practice (χ2 (1, n=287)=0.99, P=0.321).
The opinions of anaesthetists about the areas of modern anaesthetics in which nitrous oxide still has a role.
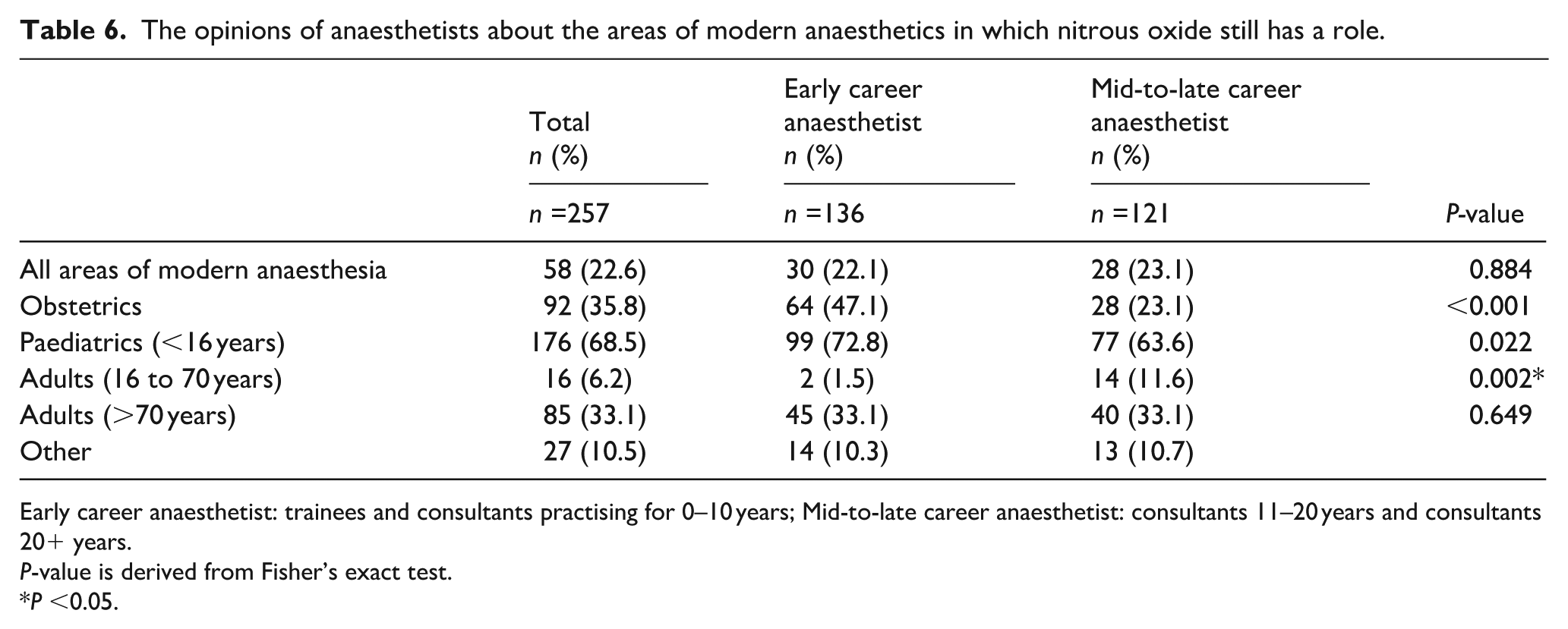
Early career anaesthetist: trainees and consultants practising for 0–10 years; Mid-to-late career anaesthetist: consultants 11–20 years and consultants 20+ years.
P-value is derived from Fisher’s exact test.
P <0.05.
Discussion
In this survey of trainee and qualified anaesthetists in 2023 in NSW, Australia, 76.3% stated they were willing to administer N2O supplied by cylinder rather than manifold-pipeline system. However, 23.7% of anaesthetists were not willing to administer N2O by cylinder. The study also found that ECAs used N2O less often than MLCAs. Most anaesthetists maintained that N2O still has a role to play in modern anaesthesia, particularly in paediatric and obstetric cases. Additional support may be required for anaesthetists who wish to change their practice to reduce their use of N2O, or for those who are ‘already restricting the use of N2O to specific cases’ and ‘trying to reduce their use of N2O’, to assist them with the transition.
Survey response rates exceeding 25% are considered excellent for online surveys. 16 Our study had a high response rate (285 of 499, 57.1%). This enabled the results to be interpreted with a 98% confidence interval and 5% margin of error. 16 The reason for the high response rate is unclear, however, it may be explained by the interest and strength of conviction currently seen in the Australian anaesthesia community regarding N2O use and its environmental sustainability. If so, this supports the value of the survey in characterising the attitudes to change and the use of N2O by anaesthetists.
The main limitations of this survey involved the questions that were asked. It would have been useful to collect data on the spectrum of anaesthetic cases undertaken by the respondents, for example, 20% obstetric/80% adult, or 100% paediatric. This would have allowed for an improved understanding of when and how N2O is used within NSW hospitals. If N2O is primarily used for paediatric induction, as was hinted at in the data, then consideration of Gordon et al.’s 17 arguments about alternatives to its use during mask induction, such as ‘preoperative preparation of children, use of preoperative anxiety scores, use of effective premedication, and ubiquitous distraction technology (screens)’, is warranted.
Another limitation was the inability to determine whether the respondents who considered that N2O did not contribute to climate change were referring to the medical use of N2O or all use of N2O. Five free-text comments for this question referred to the minimal impact that changing medical practices in the hospital would have when compared to the contribution of commuting. Question 13 was therefore excluded from the analysis. The responses to this question have been included in the raw response data presented in the supplementary documents (see Appendix 2). This survey only included seven hospitals because of delays with obtaining site-specific approval, which took almost 12 months. In the future, a similar survey could target more hospitals, including rural and private hospitals.
In the UK in 2023, a study by Thomas et al. 18 of 53 hospitals reviewed the trends in clinical usage of N2O and support for decommissioning the N2O manifold-pipeline system. Of 1445 potential respondents, 440 (28%) completed the survey. Seventy percent supported the removal of the N2O manifold-pipeline system in their hospital in favour of portable cylinders or cessation of the ongoing supply. 18 Furthermore, 47% of the cohort described by Thomas et al. 18 strongly supported decommissioning of N2O manifold-pipeline systems. In 2019, McGain et al. 13 surveyed Australian and New Zealand College of Anaesthetists’ fellows. This survey examined the use of general anaesthetic agents in Australia and New Zealand. Their results for N2O use were almost identical to those reported by the MLCAs in this study, suggesting little ongoing progress in this cohort. However, our study did highlight the change in practice by ECAs with an increased proportion using N2O less frequently than reported by McGain et al. (66% using N2O for 0 to 20% general anaesthetics versus 74% using N2O for 0 to 25% of sessions in this study). Our findings are also similar to Elliott and Pierce’s 19 survey, which found that 80% of clinicians and all trainees still use N2O. In future studies, it would be useful to understand the reasons for the changing trend in N2O use among ECAs. This change in practice may be due to clinical reasons, such as N2O contributing to postoperative nausea and vomiting, rather than ECAs being concerned about its GWP. 20
The use of N2O cylinders may have limitations or risks that should be explored to resolve the concerns expressed by some of the respondents. Anxiety about running out during a surgical procedure is understandable: implementing strategies to manage or prevent this may help alleviate these concerns. For example, approximately 25% of a cylinder’s contents remain when the pressure gauge falls into the red-shaded area suggesting the cylinder requires changing. 21 This allows for around 2 h of gas delivery at 6 L/min, ample time for a cylinder change to be completed. 21 Peyton and Leslie 22 identified and advocated using automatic low fresh gas flow anaesthesia delivery systems. This would further increase the time to empty a gas cylinder while reducing unnecessary use of N2O.
There is growing understanding among anaesthetists that a reduction in use and ultimately the decommissioning of manifold-pipeline systems for N2O supply are considered best practice. However, implementation of changes to N2O supply, delivery and alternative sedation techniques requires a multifaceted approach. Chesebro and Gandhi 23 recommend that change requires coordination and communication between multiple departments. Leadership in the education process should come from anaesthetists who have the potential to reassure other departments, for example, management and engineering, that changes to N2O supply are safe and will not impact patient care. 23
Several settings, including birthing units and paediatric hospitals, may still need N2O supplied by a manifold-pipeline network due to the high flow and high-volume use required. Further examination of these settings is important, as birthing suites and paediatric emergency departments have been shown to use more N2O than operating theatres when co-located in major hospitals. 24 Alternatives to N2O, such as those discussed by Gordon et al.,17,25 or use of dexmedetomidine for procedural sedation, are available in some settings and show comparable outcomes.
Changing to cylinder-only supply is not without its own sustainability issues. Large volumes of N2O can still be vented into the atmosphere from expended cylinders if suppliers do not capture the residual N2O before reprocessing. 21
It is essential that healthcare facilities that use a manifold-pipeline network regularly evaluate the system to detect leaks. Various methods may be used to do this, such as weighing methods similar to those used by Gaff et al. 7 This will ensure leaks are detected and rectified as soon as possible.
Finally, it would have been useful to determine any impact of local policies or guidelines on the changing use of N2O, particularly by ECAs. Repeating the survey to include anaesthetists with a non-metropolitan practice, and those working in other States and Territories, would be informative. Interestingly, McGarrigle et al. 26 found that patients were more inclined to seek alternatives to N2O after being advised about its greenhouse effect, and surveying patients to understand their priorities may be of value in progressing changes in practice.
Conclusion
The anaesthetic community continues to discuss and evaluate the use of N2O in modern anaesthesia practice. In NSW metropolitan anaesthesia practice, its use is decreasing, particularly among ECAs. Transitioning to the supply of N2O by cylinder would be acceptable to most anaesthetists, with strategies implemented to ensure that supply failure during surgery can be managed without compromising patient care. To reduce the overall environmental impact of N2O use in healthcare the following are required: (i) periodic assessment of manifold-pipeline networks for leaks and maintenance, (ii) responsible management of cylinder N2O reprocessing, (iii) improved N2O capture and destruction during clinical use, and (iv) development and/or use of clinically acceptable alternatives to N2O with a lower carbon footprint. To improve the health of all humans and the planet, all methods to mitigate the environmental impact of N2O must be explored.
Supplemental Material
sj-docx-1-aic-10.1177_0310057X251396232 – Supplemental material for A survey of nitrous oxide use, attitudes and environmental sustainability considerations by anaesthetists across metropolitan local health districts in New South Wales
Supplemental material, sj-docx-1-aic-10.1177_0310057X251396232 for A survey of nitrous oxide use, attitudes and environmental sustainability considerations by anaesthetists across metropolitan local health districts in New South Wales by Henry CM Clutterbuck, Timothy J Marshall, Sascha Karunaratne, Daniel Steffens, Michael Paleologos and Charlotte Johnstone in Anaesthesia and Intensive Care
Footnotes
Acknowledgements
The authors would like to pay special thanks to the following people for their contribution to the project: Dr Mincho Marroquin-Harris, Department of Anaesthesia, Ryde Hospital; Dr Elspeth Bright, Department of Anaesthesia, Hornsby Ku-ring-gai Hospital; Dr Penny Hodges and Dr Anthony Hull, Department of Anaesthesia, Royal North Shore Hospital; A/Prof Justin Skowno, Department of Anaesthesia, The Children’s Hospital at Westmead; Dr John Quoyle, Department of Anaesthesia, Concord Hospital; and Dr Beverley Correia, Department of Anaesthesia, Canterbury Hospital.
Author Contribution(s)
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
