Abstract
Failing high-stakes examinations in specialist medical training has devastating effects on trainees, both personally and professionally, with some trainees requiring multiple attempts. Factors enabling the transition from failure to success are under-explored. This study aims to understand how intensive care trainees, taking multiple attempts at the final high-stakes exam for progression to specialist, made the transition from failure to success, and their lived experience of the journey. This qualitative study applied grounded theory design, conducting 11 in-depth interviews. All participants had had two or more failed attempts before achieving success in the final high-stakes examination, a critical hurdle in achieving Fellowship with the College of Intensive Care Medicine. Additional data included exam reports, an external review of the exam processes, and research notes. To achieve exam success participants needed to reconstruct their sense of self, develop a growth mindset and identify as a competent intensivist. The constructed theory, ‘Identifying as an intensivist’, relates to professional identity formation and ‘thinking, acting and feeling’ as an intensivist. ‘Identifying as an intensivist’ was integral to overcoming exam failure for intensive care trainees. Professional identity formation as an aspect of remediation for high-stakes assessments in medical specialty training has not been well described. Furthermore, assessment processes should be constructed to align with a professional identity reflecting the values and diversity of the specialty.
Keywords
Introduction
Despite criticisms regarding their reliability, validity and educational value,1–5 high-stakes examinations are a persisting feature of many medical specialist training programmes. Arguments for their use include acting as a driver for learning and shaping professional identity.1,6–8 However, exam failure has potentially devastating effects on trainees, affecting job prospects, home life, mental and physical wellbeing, and, in some instances visa status.9,10
The health professions education literature describes remediation programmes and learner characteristics associated with failure or success in high-stakes assessments,11–21 but there is little evaluating how learners make the transition from failure to success. The influence of assessments on professional identity formation is well recognised.6–8 The tension for the learner between assessment-driven performance and the development of the professional self is also described.22,23 Professional identity is a complex concept relating to the individual’s viewpoint of who they are as a professional, and, for this context, may be described as thinking, acting and feeling as an intensivist. Professional identity is shaped by self-efficacy, self-confidence and self-esteem, and negatively affected by exam failure. Despite this, there is a paucity of research addressing the role of professional identity formation in remediation in high-stakes assessments.
The purpose of this research was to add to the understanding of recovery from failure in academic achievement, specifically for intensive care medicine (ICM) trainees but also with implications for a wider learner context. A further aim was to gain a better understanding of the lived experience of trainees while undergoing the transition from exam failure to success, and the related psychosocial contexts. The research questions were as follows:
How do ICM trainees, who have had previous multiple attempts at the final high-stakes exam for progression to specialist, achieve success?
What is the meaning, for ICM trainees, of multiple poor exam results before achieving success?
Methods
This research was positioned in a constructivist-interpretivist paradigm, acknowledging there are multiple different realities, and that the researcher is not unbiased, and their own experiences and beliefs cannot be separated from the analysis. 24 Grounded theory methodology (GTM) after the teachings of Charmaz was selected as the methodological approach, aligning with the research team’s epistemological stance and world view.
Participants
The study population was defined as trainees and new Fellows of the College of Intensive Care Medicine of Australia and New Zealand (CICM) who had completed the final high-stakes examination within the preceding 5 years, after two or more unsuccessful exam attempts, an estimated pool of approximately 50 potential participants. These inclusion criteria ensured recency of the experience and excluded those for whom exam failure had been readily remediated. Purposive sampling was used to identify and recruit 11 participants who responded to an open invitation advertised in the CICM newsletter.
The participants were representative of the broader trainee population, coming from the three main geographical areas served by CICM: Australia, Aotearoa New Zealand and Hong Kong, from a background of both regional and major metropolitan intensive care units, and representing diversity in gender, age and country of primary medical degree. Participants had taken a minimum of four and a maximum of six exam attempts before achieving success. At the time of recruitment, they were within a few months to nearly 5 years from their successful exam attempt. Individual demographic data are not reported to preserve participant anonymity.
Ethics
Ethics approval was obtained from the University of Western Australia Human Research Ethics Committee, reference number RA/4/20/5988. Participants self-identified and gave informed consent prior to participation, and were able to withdraw from the study at any time. None of the 11 participants refused consent, declined to participate in or withdrew from the study at any stage.
Data collection
Data collection occurred between December 2020 and May 2021. In-depth, individual, interviews were conducted with the study participants via Zoom by MP, lasting 50–84 min (average 68 min). The initial interview structure was tested as a pilot with a senior colleague and evolved and developed with subsequent participant interviews as guided by concurrent data analysis. The final interview structure is set out as a checklist in Appendix 1. De-identified audio-recordings of the interviews were transcribed into text using NVivo software (QSR International). 25
A follow-up interview at 1–2 weeks was conducted by telephone to clarify points from the first interview, and for discussion of any additional information, either offered by the participant, or arising from initial data analysis.26,27 An important focus of this follow-up interview was participant wellbeing, recognising the initial interview may have been emotionally triggering.
The interview was a dynamic process, in keeping with GTM,26,28–30 and the questions were refined as the study progressed, based on data derived from earlier interviews. Additional data sources included memos, research notes, a reflective research diary, CICM exam reports and the findings of an external review of the exam processes. These secondary data sources facilitated reflexivity and contributed to research design, determining the scope and focus, but were not used in coding or theory development.
Data analysis
Data collection, coding and analysis occurred contemporaneously and was an iterative process following the framework of constructivist GTM.26,28–30 Open, focussed, theoretical and axial coding led to the development of categories and themes and the creation of an overarching theory. Recruitment for the study ceased when the research team considered adequate data had been collected to allow understanding of the themes and creation of a theory to answer the research questions, aligning with the concept of ‘information power’ and theoretical sufficiency as opposed to saturation.29,31 Recruitment of a relatively small number of participants was facilitated by sample specificity and the quality of dialogue in the interviews. 31
Reflexivity
The practice of reflexivity is integral to GTM and serves to acknowledge the effect of researcher experience and worldview on data collection and analysis. 32 In this instance, the research team comprised a novice qualitative researcher and experienced intensivist with in-depth knowledge of the intensive care training programme (MP), and two experienced qualitative researchers with non-medical backgrounds but experience in intensive care training and other health professional training programmes, both pre and post-registration (CID and SEC). These backgrounds influenced the researchers’ understanding of the study and their interpretations of the data. In particular, how they understood remediation in the context of exam failure. Only one member of the research team (MP) had an ongoing relationship with intensive care training which guided the design of the research and the potential for implications for future practice. Peer debriefing and memo-writing throughout the research process mitigated the influence of researcher experience on the interpretation of the data.
Results
Data analysis revealed that, in order to achieve success, the study participants needed to rebuild their professional identity; seeing themselves as an intensivist. This was achieved by acknowledging their competence and accepting self. Integral to these themes were reconstruction of their professional and personal self, exam preparedness (becoming ‘match-fit’), and reframing failure. These elements were inter-connected and inter-dependent (Figure 1). Accepting and acknowledging self as someone who was both good at their job and who had struggled to pass the exam was central to participants making meaning of failure and being able to identify as an intensivist, and contributed to achieving exam success. The theory generated through the data analysis was ‘Identifying as an intensivist’, relating to professional identity formation. The three key categories are described below.
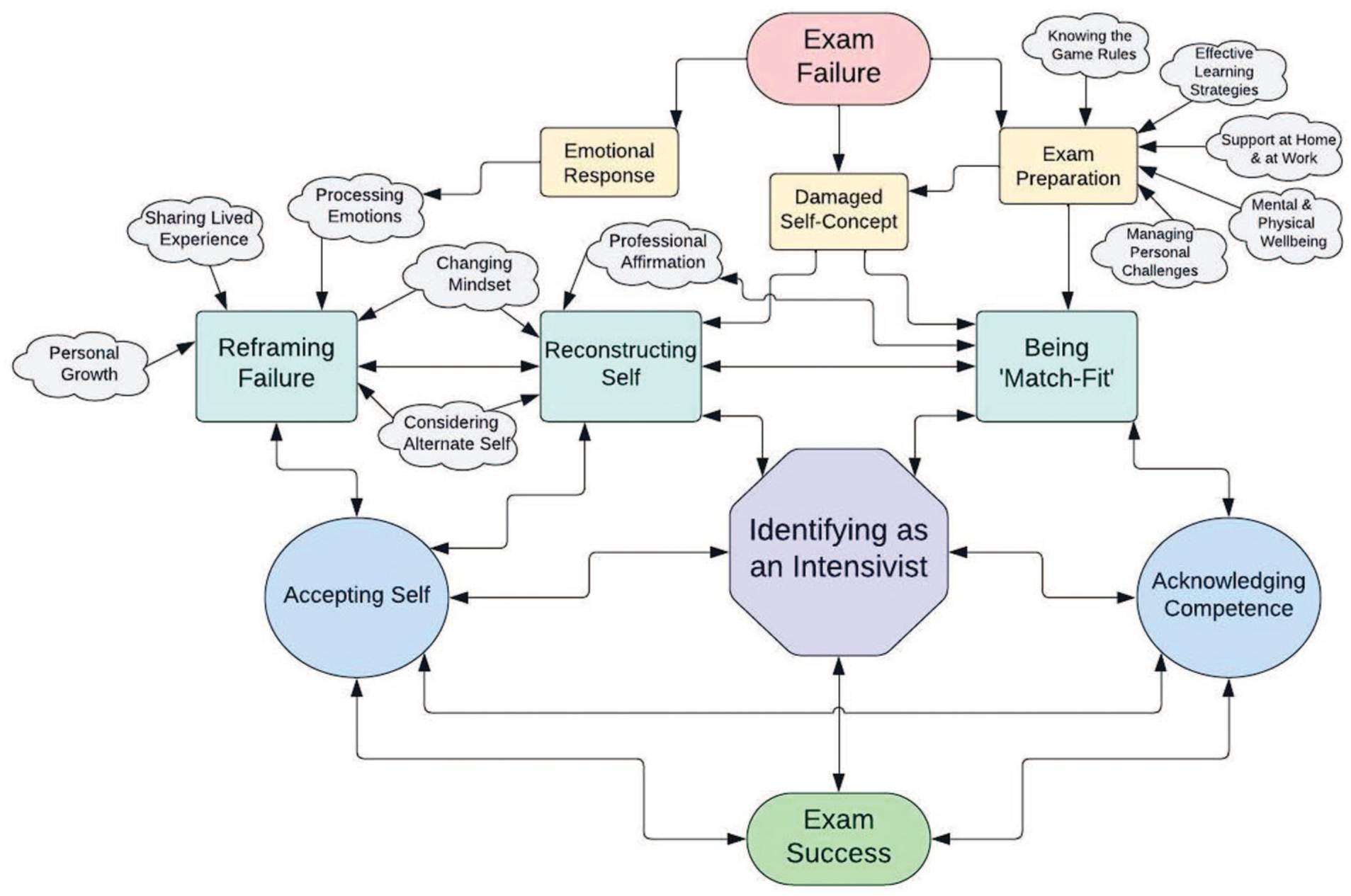
Concept diagram showing path from exam failure to success.
Becoming ‘match-fit’
Achieving a state of exam preparedness drew parallels with elite sports performance and being ‘match-fit’. Participants needed to acquire adequate knowledge with effective study strategies, and to optimise the mental, physical and emotional aspects of their game to be able to perform at their best. Participants also needed to understand the purpose and format of the assessment process and the required standard to pass, the ‘rules of the game’:
Participants identified having social and environmental enablers with support both at work, with trusted coaches and mentors, and at home as integral to exam preparedness: You can’t do this one alone. This is not an individual wolf against the world, lone wolf. Although there are people out there, I know, that just lock themselves in a room and manage to get through it, I think you need that support you need to be human. You need to acknowledge that humanness. (P4)
A pivotal point was adoption of a growth mindset with the recognition that the exam’s purpose was to drive the learning to help them become a better clinician and improve patient outcomes, and not just to pass the exam: [The exam] is to make sure that we learn what we need to learn. . . it’s like an opportunity to hopefully grow into the consultant you want to be. (P6) At the end, the important thing is the patient, and so, like, you know, connect it to the patient. And when I actually give the template away and then present and think, I’m really concerned about this patient. . . and then it actually comes all together for you. Like, I think the patient is the most important thing. (P2)
Attending to wellbeing during exam preparation, looking after both mental and physical health, was an important factor in exam success. Participants reflected that focusing on their own wellbeing not only facilitated deep learning and eased exam stress, but also helped them perform better in the workplace, feel more competent, and provide better care for their patients: As the time progressed by, I felt that I was coming back to normal, to what I was before. I felt that I was calmer and I felt that I lived for myself. And in that process I came to know that I still loved to read and learn and take care of my patients. (P1)
Becoming ‘match-fit’ also required achieving balance between the conflicting demands of work, study and family life. Participants each had their unique personal challenges and barriers to exam preparation to negotiate and mitigate. Unsuccessful exam attempts were often associated with emotional life events and personal tragedies: People who are doing exams are in a stage where they have to cater to multiple needs, the family, the personal or the unit, the job applications for the next year. Getting all that aligning with the exam goal and performing the exam is very hard. At least, it was very, very hard for me.. . . I think it was too much for my [partner] and we got separated. . . and then I got remarried and had a child who was sick and still with that I was able to write. . . . But once the child passed away, that was a big blow to me. (P1)
To be prepared for the exam, as in a sporting context, the study participants needed to believe they could ‘win the match’. Feeling prepared for the exam gave them the confidence that they could pass the exam and allowed them to acknowledge their clinical competence.
Reconstructing self
Seeing themselves as an intensivist was very important to the participants and to their identity, and failing the exam was a massive blow to their self-esteem and sense of self. Participants needed first to process their emotional responses to failure and then rebuild their self-image, seeing themselves as competent intensive care doctors, performing at the required standard to pass the exam, through affirmation of their clinical ability. Rebuilding their sense of self after failure was not just integral to exam success, it was an important step in forming their identity as an intensivist—the purpose of their training and key to making meaning of their exam experience.
Participants reflected on their emotional responses in the aftermath of a poor exam result and acknowledging these emotions was an important part of the process of reconstructing self. Participants’ reactions reflected grief and loss and included denial, anger and sadness, with even suicidal ideation expressed.
33
There was also frustration in not knowing how to improve their performance, guilt and disappointment, self-doubt and a sense of shame: And it was hard going back to work and realising that I should have got through when they had put so much time into helping me through that. (P6) I also felt really sorry for my family because my partner isn’t medical and my children are small and they had all invested so much in me passing. It was very hard to get up and keep going after that. (P3)
Participants relied on their support networks and the healing effect of time to help process their emotional responses. Working through these emotions and coming to a phase of acceptance was important in enabling participants to move on from failure, regain their sense of self, and have the right mindset to focus on the next exam attempt.
Affirmation of their clinical ability was a crucial step for participants in rebuilding their valued self. Participants needed to see themselves as equal to their peers, and to recognise their progression along the training pathway from novice to expert. This affirmation was external, through the opinions of trusted colleagues, and internal, through self-reflection. Entrustment that they could ‘do the job’ gave them the confidence that they could pass the exam. Knowing that their exam performance was not reflective of their clinical performance in the workplace was a critical step enabling participants to reconstruct their sense of self. The exam was then seen as an opportunity to demonstrate their clinical competence, rather than an insurmountable hurdle: [Supervising consultant] he called me, and he said to me, ‘Look, if I were to get sick, I’d want you to look after me. And you’re a good doctor. You’ve got knowledge. I’ll never, ever understand why you have failed’. That made me re-look at things, because [supervising consultant] is one of the most difficult people to please. He’s got a very, very high standard, and when he said that it’s made a big, big difference to the outlook. (P10)
Personal relational identities were realigned in the aftermath of exam failure, with examples of strained relationships and marital breakdown. However, for the most part, relational identities were maintained or even strengthened, with family and friends seen as understanding and supportive. Relational identity with children was enhanced by providing a living example of resilience and overcoming failure: From my daughter’s point of view, it does demonstrate resilience, people fail things that they shouldn’t fail, or they have failed things that they didn’t want to fail. . . and we just buckle down and get on with it again. (P9)
Professional relational identities were also affected, in some instances damaged irrevocably. Peers progressed ahead through the training pathway, and senior colleagues, previously seen as respected mentors, were perceived to provide inadequate remedial support and to lack empathy. Career prospects were jeopardised and job offers withdrawn. However, participants also described receiving affirmation and support from senior colleagues that was valuable in growing mutual respect and rebuilding their relational identity: What I found really nice was consultants coming out of the woodwork with things like, ‘I failed the exam first time and it doesn’t necessarily reflect on you as a person’. (P6)
Although their identity as an intensivist was valued, participants were prepared to consider an alternative self, had they continued to be unsuccessful in the exam, demonstrating resilience and adaptability and an element of pragmatism: I don’t like using the phrase, ‘wasting their lives’, but I will in this circumstance. As in, if you’re studying for an exam that you’ll never actually end up passing, what’s the point? You should actually be focussing on something else because you should be working to live, not living to work. (P4)
However, identifying as an intensivist remained their preferred self. This was a major driver in striving for, and ultimately achieving, exam success.
Reframing failure
Reframing failure enabled study participants to find meaning in the experience. Both exam failure and exam success were described as defining moments in their life. Contextualising failure, a change to a positive mindset, acknowledging the personal and professional growth that had occurred, and sharing the learning from their lived experience to help others were important factors in the healing process. However, some aspects of reframing failure were retrospective, and participants could not fully accept self until working as a consultant. As of the time of the interview, this was still a work in progress for some.
Participants felt stigmatised by their poor exam performance, and concerned they would always be marked as failures. Participants were able to move beyond this negative self-image by appreciating that colleagues they viewed as ‘incredibly smart’ and ‘excellent clinicians’ also failed the exam, and that they would not progress if they held onto feelings of inferiority. Participants put their desire to learn and to become their best self above a sense of feeling judged. An additional component of contextualising failure was acknowledging the limitations of the exam as a summative assessment process.
An important component of reframing failure was acknowledging the personal and professional growth the study participants had experienced through their exam journey. As well as knowing themselves to be better clinicians through the exam process, participants spoke of feeling they were a better person and more resilient as a result of their lived experience, and they felt grateful for having had this life lesson. Reminding themselves that the exam process was an opportunity for professional growth, and observing the changes in their performance over time with more practice, helped participants maintain their motivation. Participants learned to overcome challenges and personal issues through their exam journey. Strategies used to help improve exam performance had a lasting effect, teaching participants to reach inner calm and mindfulness, and to focus on their strengths: I learn a lot from the exam and both the knowledge and the skill and also how to face failure. (P5)
Study participants found that using their experiences to mentor junior colleagues, both in terms of strategies to pass the exam and lessons from their personal journey, was therapeutic. Demonstrating intellectual candour and vulnerability in sharing their exam journey with junior colleagues strengthened the supervisor–trainee relationship and assisted learning. This helped participants reframe failure and enhanced their self-belief in their competence as an intensivist: When I look back now with all those experiences, it’s not a waste, it’s still useful because I can talk to the registrars about my experience. . . not every consultant has this kind of experience. (P2)
Identifying as an intensivist
The theory generated from the data, ‘Identifying as an intensivist’, relates to the process by which the study participants came to think, act and feel like an intensivist, and so build their professional identity. Construction of this professional self was integral in making meaning of the journey from exam failure to success and assisted that transition.
Participants’ self-concept was mutable and the processes by which the participants were able to overcome failure and achieve success were foundational in rebuilding their sense of self. This is reflected in the two themes underpinning the emergent theory, acknowledging competence and accepting self. In order to achieve exam success, participants needed to reach acceptance of their valued self, as both someone who had overcome failure and who was a competent clinician. For the participants in this study, exam success was achieved by, and contributed to, the development of the professional self and the ability to ‘Identify as an intensivist’, the overarching theory generated from the data.
Discussion
The generated theory, grounded in the data, ‘Identifying as an intensivist’, relates to how the participants came to construct their professional identity, and make meaning of their journey from exam failure to success. This theory represents the social-psychological process of trainees undergoing this transition, and encompasses thinking, acting and feeling as an intensivist.
This research contributes to the conversation relating to high-stakes assessments in medical specialty training as previously little has been known about the processes of overcoming failure in this context. Identifying as an intensivist was integral to overcoming failure and making the transition to success. Although the connection between failure and professional identity formation has been shown in medical students,6–8 this theoretical construct has not been well researched in the context of the transition from failure to success in medical specialty training. Although the dominant theory constructed from the data relates to professional identity formation, the study participants’ transition from exam failure to success aligns with other foundational psychological theories underpinning achievement and motivation in education, and including both social and cognitive elements. 34
Exam failure had a devastating impact on the study participants’ sense of self, with a profound sense of loss, and a variable and changing effect on their individual, relational and collective identities. Study participants spoke of the stigma of failure and the importance of support from family and colleagues. There were positive experiences but some spoke of a lack of empathy shown by supervisors and a breakdown in previously collegial relationships, and exam stress contributed to marital breakdown and suicidal ideation.
The lived experience of the study participants described systemic factors contributing to exam failure. The barriers highlighted included variability in the quality of supervision and intensive care training experience, and bias in the assessment processes.
These findings resonate with those of other studies that have explored failure in high-stakes assessment in health professions education.35–37 These studies also demonstrated the dynamic interaction between meaning-making and action, describing the complexity of the learners’ experiences, their strong emotional response to failure and how this influenced remediation, and the variable effect on personal and professional relational identities.
The participants in this research were able to reframe failure, describing their exam journey as an opportunity for personal growth. As their exam preparedness developed and with external and internal affirmation of their knowledge and skill, they were able to rebuild their individual identity and acknowledge their competence as an intensivist. These perceptions were echoed in a study evaluating academic failure in dental students, who reported increased self-confidence from overcoming failure and recognised failure as a ‘turning-point’ in their life. 38
The collective identity of the intensivist is influenced by sociocultural, psychosocial and cognitive elements layered on the pre-existing self. 7 These elements encompass the culture of the intensive care community of practice, its role models and leaders, and by the assessment processes determining progression along the training pathway. Thus, CICM plays an integral role in shaping the collective professional identity of intensive care medicine specialists in its region by driving culture through trainee selection, the design and implementation of the curriculum and assessment processes for progression to becoming a specialist, and through the appointment of supervisors of training and examiners.
As participants moved from failure to success, they, at times, reflected on incongruence between their individual identity and the perceived identity of an intensivist. This can be understood as identity dissonance.7,8,39 It may be that the high-stakes assessment process for intensive care training promotes a professional identity that is not a true reflection of the specialty. This is an area that warrants further research and evaluation and has relevance for other medical specialty colleges and training programmes. Curriculum development must reflect the increasing diversity of the healthcare workforce and the wider community and acknowledge the tension that exists for minoritised clinicians between negotiation and dissonance of their professional identity. 39
Limitations of the study
Limitations of this study relate primarily to the study population, the relatively small sample size and methodological challenges. Firstly, this cohort may not have been representative of the wider population of trainees and fellows taking multiple exam attempts before achieving success. Secondly, as the study participants self-identified, this may have introduced bias, favouring participants who had processed their journey from failure to success more positively. However, the study population was a specific group comprising trainees and fellows from Australia, Aotearoa New Zealand and Hong Kong, from a background of both regional and major metropolitan intensive care units, and who represented diversity in gender, age, and country of primary medical degree. The participants were articulate and accustomed to reflective practice and discussion, and the interviews generated more than 12 hours of quality interview dialogue. These factors contributed to a sense that data sufficiency had been reached within the 11 interviews. 31
Thirdly, because of the small number of participants, the study was unable to identify themes or trends relating to a specific sub-group, for example, exam candidates needing multiple attempts at one section only; international medical graduates; rurally based candidates. Finally, as only trainees who were ultimately successful in the exam were interviewed, it is unknown whether there are others who are still unsuccessful, despite reaching a similar stage of professional identity development.
It should also be acknowledged that, in keeping with a constructivist worldview, the data from this study could give rise to different perspectives, interpretations and theories. However, as the chosen research paradigm is a grounded theory methodology, the theoretical framework was developed inductively from the contemporaneous data collection and analysis during the research process, and guided the direction of the research. Alternative theories and perspectives could be explored in future research evaluating the lived experience of exam failure.
However, despite these limitations, the findings of this study are believed to be of relevance to other learner contexts. As research conducted in alignment with a constructivist paradigm, the concepts arising from this study have theoretical generalisability, relating to professional identity formation and theories underpinning motivation and achievement in health professions education. 40
Conclusion
This study used grounded theory methodology to explore how intensive care trainees recovered from multiple failed attempts to achieve success in a high-stakes assessment and how they made meaning of the experience. Study participants described needing to acknowledge their competence as an intensive care clinician and to accept self as someone who had failed but gone on to succeed, growing professionally and personally through the experience. The generated theory grounded in the data, ‘Identifying as an intensivist’, related to the development of the professional self—a step that was integral in making meaning of their journey and in achieving exam success and, in turn, enhanced by that success. The importance of professional identity formation and the influence of the college’s processes, procedures and activities has hitherto been under-recognised in intensive care training.
The study has also highlighted systemic issues within the CICM training process. Future research and curriculum development should focus on systemic enablers and barriers to exam success, such as exam design, training culture and support infrastructure, and address identity dissonance.
The findings of this study align with those from other research evaluating the struggling learner in different healthcare contexts. This implies that the experience of academic failure and recovery from this has common features across all learner contexts and that the learnings from this research may be able to be extrapolated to other settings. These findings are of particular interest to other medical specialist training programmes in Australia and Aotearoa New Zealand with high-stakes summative assessments, and inform college educational programmes, and assist supervisors and trainees with exam preparation and recovery from failure. The findings also contribute to the broader discussion in the health professions literature of the role of high-stakes assessments in medical specialty training.
Footnotes
Appendix
Interview structure checklist.

| Interview structure checklist | |
|---|---|
| Introduction | Introduce research team Provide overview of project Explain structure of interview Explain data collection 3.3.4.1.1 Audio recording, written notes Explain data management 3.3.4.1.1 De-identification, confidentiality, encryption, secure storage 3.3.4.1.1 Results dissemination Follow-up post interview Potential for emotional triggering Counselling service details Informed consent and withdrawal |
| Areas explored | Experiences of training programme leading up to the FCICM Second Part Examination Mentors, role models and supervisors Feedback on performance Experience of the FCICM Second Part Examination and comparison with other exams/tests ○ ‘How have you found other tests and exams in the past?’ ○ ‘Tell me about your experience with this exam’ ■ What happened? ■ How did you feel then? ■ What did you do? ■ Why did you do it? ■ How do you feel now? Preparation and study strategies ○ What helped? What didn’t? ○ How much time did you spend studying? Challenges and barriers to exam preparation and performance ○ Personal and professional ○ Mitigating strategies Support systems ○ Mentors, peers, family and friends Response to unsuccessful exam attempts ○ ‘How did you feel when you got the result?’ ○ ‘What do you think your family/friends/colleagues would say if asked how you seemed?’ ○ ‘Why do you think you were unsuccessful?’ ○ ‘What feedback did you get?’ ○ ‘What changes did you make?’ ○ ‘If you hadn’t passed when you did, what were you going to do?’ ○ ‘What was the response of family/friends/colleagues?’ Response to successful exam attempt ○ ‘What was different about your preparation (work, home, study, stressors, support systems)?’ ○ ‘What was different about your performance?’ ○ ‘Why do you think you were successful?’ ○ ‘How did you feel at the time?’ ○ ‘What was the response of family/friends/colleagues?’ Self-reflection ○ ‘How do you feel about the exam now looking back?’ ○ ‘Since you have passed, what have you noticed that is different for you?’ ○ ‘What do you think your family/friends/colleagues may have noticed about you?’ ○ ‘What impact has the exam process had on your ability to work as a consultant?’ ○ ‘What advice would you give to junior colleagues preparing for the exam?’ |
| Conclusion | Invite any additional insights ○ ‘What haven’t we touched on that you would like to talk about?’ Welfare check Recap information re follow-up and counselling service details Contact details of research team |
| Follow-up phone call 1–2 weeks later | Welfare check Invite discussion of further reflections ○ ‘What have you thought of since we last spoke that you would like to say?’ Reminder of access to counselling service and contact details Updates on study progress and dissemination of findings |
Acknowledgements
The author(s) acknowledge Brid Phillips and Kelby Smith-Han for advice during data analysis; ‘K’ for being the inspiration for the study; and the study participants for their generosity in sharing their stories.
Author contributions
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
