Abstract
Background:
Arterial haemoglobin oxygen desaturation is common during gastroscopy and is associated with patient harm. Obesity increases the risk of desaturation during gastroscopy. High-flow nasal oxygen may reduce the risk of desaturation, but data are lacking.
Methods:
We conducted a single-centre, parallel group, randomised controlled trial of high-flow nasal oxygen at 50–70 l/min compared with oxygen via nasal prongs 4–10 l/min, enrolling adults having gastroscopy procedures who had a body mass index greater than 30 kg/m2. The primary outcome was the incidence of desaturation, defined as any peripheral oxygen saturation less than 90% during the procedure.
Results:
We recruited 150 participants (75 in each group). The mean body mass index was similar in each group (35 vs. 36 kg/m2). High-flow nasal oxygen reduced the incidence of desaturation compared with standard oxygen therapy (three (4%) vs. 14 (19%), P = 0.005), and increased the median minimum peripheral oxygen saturation (98% (interquartile range 92–97%) vs. 94% (interquartile range 97–100%), P < 0.001). Fewer patients administered high-flow oxygen required airway interventions (39 (52%) vs. 58 (77%), P < 0.001), while the number of patients requiring interruption to the procedure for airway management were similar in each group (seven (9%) vs. five (7%), P = 0.57). High-flow nasal oxygen was associated with a higher risk of apnoea compared with standard oxygen delivery (17 (23%) vs. six (8%), P = 0.013), and a similar risk of arrhythmias existed between the groups (two (3%) vs. one (1%), P = 0.56).
Conclusion:
High-flow nasal oxygen reduced the incidence of desaturation during gastroscopy in obese patients.
Introduction
Gastroscopy is a common procedure, with over 2 million procedures performed per year across the globe. 1 Deep sedation is commonly used to facilitate the procedure and is preferred by patients 2 and proceduralists.3,4 However, deep sedation is associated with adverse events including arterial haemoglobin oxygen desaturation (‘desaturation’), 5 interruption to the procedure caused by the need for airway intervention and extended duration of the procedure, which may increase costs, and can cause significant patient harm. 6 Patients with obesity are increasingly being offered deep sedation for their gastroscopy procedures and they are at higher risk of desaturation and procedural interruptions than non-obese patients.7,8 Desaturation during gastroscopy procedures places patients at risk of adverse cardiac events such as arrhythmias or myocardial ischaemia, which can potentially lead to hypoxic brain injuries, and cardiorespiratory arrest. 9 Comparative trials of interventions to reduce the risk of desaturation are important fot improving the safety of gastroscopy procedures in patients with obesity.
Conventionally, low-flow nasal oxygen is used to supplement inspired air during gastroscopy, a practice based on limited evidence.10–12 High-flow nasal oxygen is a recent innovation that may provide a greater margin of safety for these procedures,13,14 partly because of the very high fraction of inspired oxygen and partly because high-flow oxygen may offer some degree of ventilatory pressure support or positive end-expiratory pressure. 15 These advantages may be particularly useful in obese patients, and trials have demonstrated that sustained maintenance of peripheral oxygen saturation (SpO2) is possible with high-flow nasal oxygen even when the patient is apnoeic. 16 High-flow oxygen may be superior to low-flow oxygen in patients with obesity, and may reduce the incidence of clinically significant complications and reduce the interruptions to procedures required for airway management, 17 which may in turn reduce cost. However, evidence supporting this hypothesis is equivocal, particularly in terms of affecting the proportion of patients experiencing desaturation during procedures. 18 Despite these promising data, recent meta-analyses have called for additional evidence to resolve this question due to substantial heterogeneity of the evidence available, 19 and the strength of evidence is particularly lacking in patients with obesity. 16
We conducted a randomised controlled trial comparing high-flow nasal oxygen delivery against standard oxygen delivery to resolve this question. We hypothesised that high-flow nasal oxygen would reduce the incidence of desaturation during the procedure.
Methods
We conducted a single-centre, parallel group, randomised controlled trial. The trial received ethical approval from the Melbourne Health Human Research Ethics Committee (approval number 2019.221) and was conducted in accordance with the Declaration of Helsinki, the National Health and Medical Research Council Statement on Human Participation in Research and Good Clinical Practice principles. A detailed consolidated standards of reporting trials (CONSORT) statement is included in the supplementary materials.
The trial was conducted at the Royal Melbourne Hospital, a tertiary referral and trauma centre in Melbourne, Victoria, Australia. All procedures were conducted in the dedicated day procedure unit.
This work was supported by internal departmental funding.
Registration
The trial was prospectively registered on the Australian and New Zealand Clinical Trials Register, with the registration number of ACTRN12619000983101. We did not change the design of the trial after commencement of the trial. A copy of the trial protocol is available on request.
Participants
We recruited adult patients, who either weighed more than 100 kg or had a body mass index (BMI) of greater than 30 kg/m2, requiring deep sedation for a gastroscopy. We set the dual weight criteria because we observed anaesthetists using both cut-offs as part of their decision to use high-flow nasal oxygen. However, after recruitment was completed, we noticed that all recruited patients had a BMI above 30 kg/m2 and for the rest of the article we will refer to this as the primary inclusion criterion. Written informed consent was obtained from all patients before enrolment in the trial.
For the purposes of the trial a gastroscopy could be a stand-alone procedure, or in combination with colonoscopy or other diagnostic or interventional procedures, such as endoscopic ultrasound or oesophageal dilation.
We excluded patients who were younger than 18 years, who were unable to consent to participate in the research, were intubated or required intubation for the procedure, were pregnant, had active nasal bleeding or a base of skull fracture, or were planned for an endoscopic retrograde cholangiogram procedure.
Interventions
Participants were randomly assigned to two groups: patients in the high-flow oxygen delivery group were administered oxygen using an Optiflow THRIVE circuit (Fisher and Paykel Healthcare, Panmure, Auckland, New Zealand), which delivers heated humidified oxygen at 100% concentration via proprietary nasal cannulae. Flow was started at 30 litres/min (LPM) for at least 3 minutes before sedation was administered and increased to between 50 and 70 LPM in stages at the discretion of the anaesthetist. If the patient was not able to tolerate flows in this range, reduction in flow to 30 LPM was permitted. The anaesthetist could titrate the flow if desired during the procedure.
In the standard oxygen delivery group, patients were administered oxygen at a flow rate starting at 4 LPM via nasal prongs before sedation was given. The oxygen flow rate could be adjusted and increased up to 10 LPM by the treating anaesthetist.
Screening, enrolment and allocation concealment
A research nurse screened all patients planned for gastroscopy procedures during the periods the study was recruiting. An investigator from the trial approached participants, gained their consent and enrolled them in the trial. Allocations were concealed in sequentially numbered opaque envelopes which were opened once written consent was obtained.
Randomisation and blinding
A randomisation list was computer-generated by an independent statistician in permuted blocks of ten. Participants were allocated to groups in a 1:1 ratio in parallel. As the appearance and sound of the delivery devices in operation were substantially different, it was not possible to blind patients, anaesthetists or the research staff with respect to the intervention.
Uncontrolled aspects
As a pragmatic trial the study did not control the conduct of the gastroscopy procedure, nor the proceduralist conducting it. All anaesthetic care was led by consultant anaesthetic specialists. The study also did not direct the conduct of the anaesthetic, the selection or dosing of the anaesthetic medications, nor the use of airway adjunct devices, airway opening maneuvers or decisions to intubate. Cross-over between groups was permitted at the discretion of the anaesthetist but did not occur during the trial. An anaesthetic nurse and consultant anaesthetist jointly managed the airway for the duration of the procedure.
Outcomes of interest
The primary outcome was desaturation below a SpO2 of 90% at any time during the procedure.
Secondary outcomes included the number of desaturation events per patient, the proportion of patients in which jaw thrust or chin lift were used, the requirement for interruptions to the procedure for airway management, the lowest SpO2 level and the duration of desaturation when it occurred. Complications including apnoea and arrythmias (defined as any cardiac rhythm other than sinus rhythm that was not present before the start of the procedure) were assessed in each group. Satisfaction with the intervention was assessed for patients, proceduralists and anaesthetists using a five-point Likert scale (very dissatisfied, dissatisfied, neutral, satisfied, very satisfied). 20
Outcome assessment
Oxygen saturation was measured using a pulse oximeter placed on the fingertip attached to a General Electric B450 (General Electric, Chicago, Illinois, USA) patient monitor. An experienced research nurse monitored the pulse oximeter during the procedure and recorded the lowest value during the procedure on the case report form. Duration of desaturation was established from the electronic logs of the B450 monitor. In the cases in which the gastroscopy was combined with other procedures, the period of data collection for the purposes of the study was limited to the gastroscopy component, which was always undertaken first of the sequential procedures.
The application of chin lift, jaw thrust or interruption to the procedure was observed by the research nurse and recorded on the case report form. Similarly, the research nurse asked patients (once they had recovered from sedation), proceduralists and anaesthetists to rate their satisfaction on the Likert scale at the end of the procedure and record it on the case report form. A bite block was inserted to protect the gastroscope in both groups, and a carbon dioxide (CO2) sampling cannula was attached to this bite block to facilitate measurement of end-tidal CO2. Apnoea was assessed using capnography measured using a sampling line attached to the nasal outlet of the bite block connected to an infrared analyser in the gas analysis module of the B450 monitor and was declared when CO2 was not continuously detected in the absence of respiratory effort for at least 5 seconds.
Safety monitoring and consideration of early stopping
A trial safety monitoring committee comprising three experienced anaesthetists who were independent of the trial monitored the primary and safety outcomes after the recruitment of every 30 participants. Stopping was not recommended by the monitoring committee and the trial ran to the planned conclusion of recruitment without modification to the protocol.
Sample size calculation
In order to demonstrate a minimally clinically important difference in desaturation rate from a conservative estimate of 30% 7 to 10% 17 (assuming a minimally important difference of 20%) with 80% power to detect an effect at the 0.05 level of significance, allowing for a cross-over rate of 10% from control to intervention and 5% from intervention to control, along with withdrawal of up to 5% of patients, a total of 75 patients were required in each group, for a total study population of 150.
Statistical analysis
Statistical analysis was performed using Stata 13 (Stata Corp, College Station, Texas, USA). The primary outcome was assessed using a chi-square test, with a threshold of significance assigned at P < 0.05. The results were assessed on an intention-to-treat basis. Secondary outcomes were analysed using Pearson chi-square tests or Fisher’s exact tests for binary outcomes as appropriate and Mann–Whitney U tests for continuous outcomes as the distribution of results were non-normal as assessed using visual inspection of histograms. A threshold of significance was set at P < 0.05 initially, and a Bonferroni correction was applied with an adjusted threshold of P < 0.006 to account for eight hypothesis generating comparisons to control the risk of type I error. There were no pre-planned subgroup analyses.
Results
A total of 150 patients were recruited, with 75 being allocated to each treatment arm. Full baseline demographics are recorded in Table 1. The flow of participants through the trial is recorded in Figure 1. The first participant was enrolled on 13/2/2020 and the last on 15/3/2024. A significant period of interruption to recruitment occurred during the COVID-19 pandemic as the use of high-flow nasal oxygen was restricted in our institution at various periods due to concerns about aerosolisation of virus particles. Recruitment concluded in March 2024. Follow up concluded on the day of the procedure. The trial concluded once the planned population was recruited.
Baseline patient characteristics between the two groups.
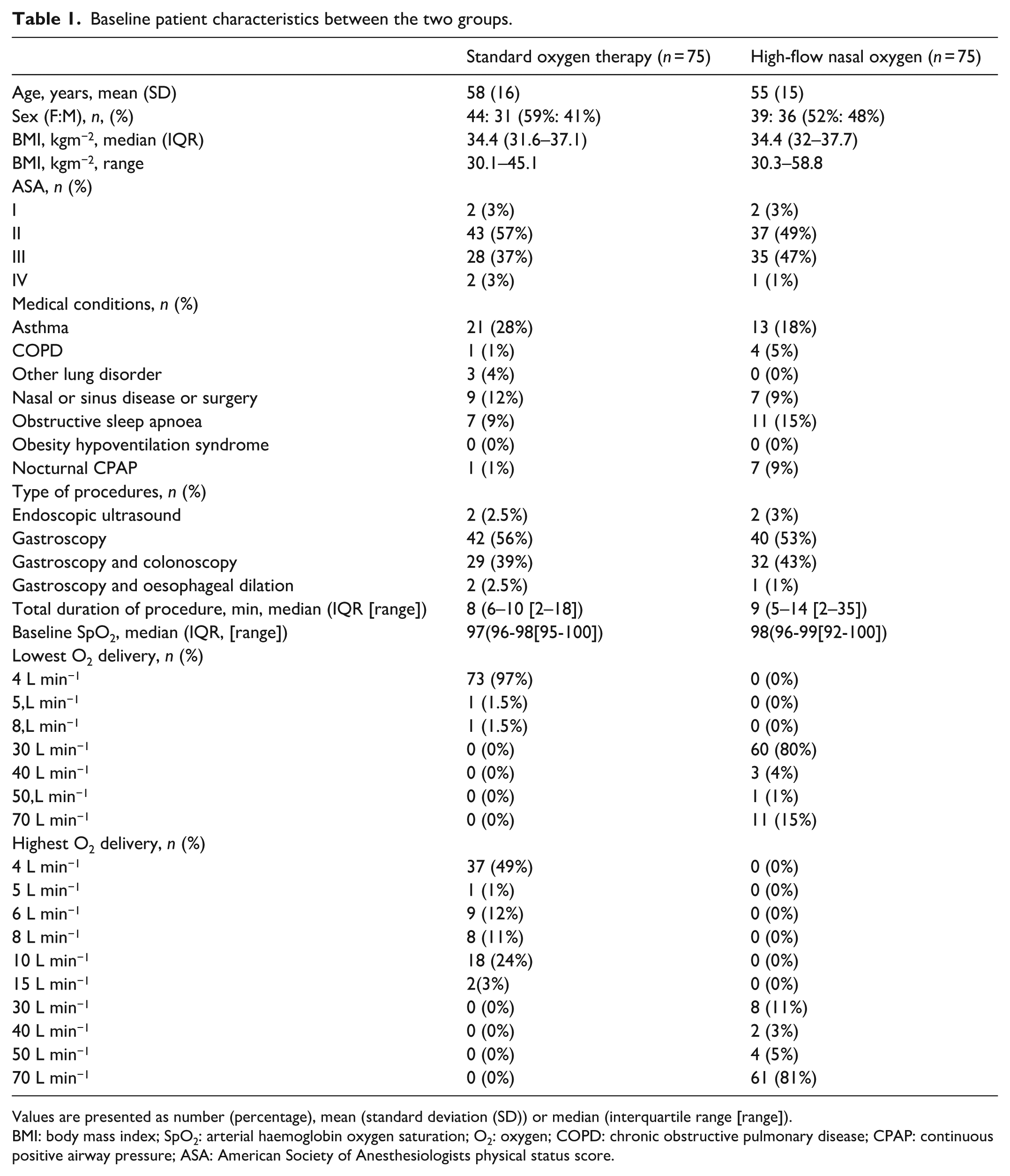
Values are presented as number (percentage), mean (standard deviation (SD)) or median (interquartile range [range]).
BMI: body mass index; SpO2: arterial haemoglobin oxygen saturation; O2: oxygen; COPD: chronic obstructive pulmonary disease; CPAP: continuous positive airway pressure; ASA: American Society of Anesthesiologists physical status score.
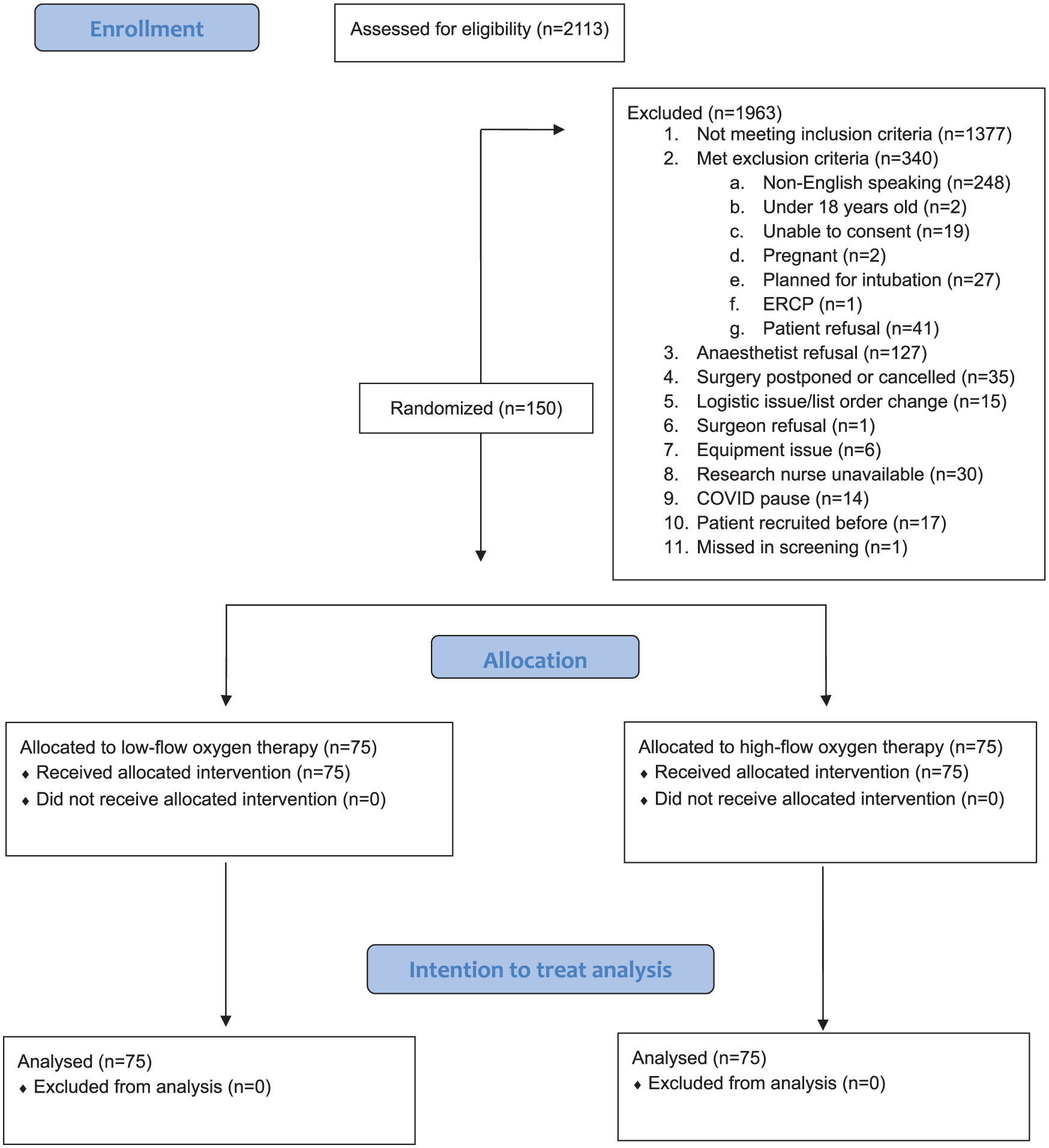
CONSORT (consolidated standards of reporting trials) diagram.
Significantly fewer patients administered high-flow nasal oxygen experienced the primary outcome of desaturation below 90% during their procedure (three (4%) vs. 14 (19%), P < 0.005). High-flow nasal oxygen reduced the incidence of desaturation by 15% in absolute terms, translating to a 79% reduction in relative terms and a number needed to treat of seven.
The median minimum SpO2 experienced during the procedure was higher in the high-flow nasal oxygen group (98% vs. 94%, P < 0.001). A lower proportion of patients administered high-flow oxygen required airway interventions during their procedure (39 (52%) vs. 58 (77%), P < 0.001); however, the number of patients requiring interruptions to the procedure for airway management problems was similar in each group (seven (9%) vs. five (7%), P = 0.57). No patients in either group required intubation for desaturation or laryngospasm. The median duration of desaturation when it occurred (30 s vs. 80 s) was not statistically significantly different (P = 0.069). The duration of the procedure was not different between the groups (8 min vs. 9 min, P = 0.57). High-flow nasal oxygen was associated with a similar incidence of apnoea compared with standard oxygen delivery (17 (23%) vs. six (8%), P = 0.013), and a similar incidence existed between the groups with regard to arrythmias (two (3%) vs. one (1%), P = 0.56). A detailed description of the secondary outcomes is contained in Table 2. The majority of patients and proceduralists were either satisfied or very satisfied with either oxygen delivery strategy. The proportion of anaesthetists who reported being satisfied or very satisfied after cases with the high-flow oxygen delivery strategy compared with the standard oxygen delivery (96% vs. 84%) was not statistically significantly different after Bonferroni correction (P = 0.008). A full description of the anaesthetists’ responses to the satisfaction scale is displayed in Figure 2. There were no significant differences in terms of medication selection or dose used for sedation between the two groups.
Outcome data between the two groups.
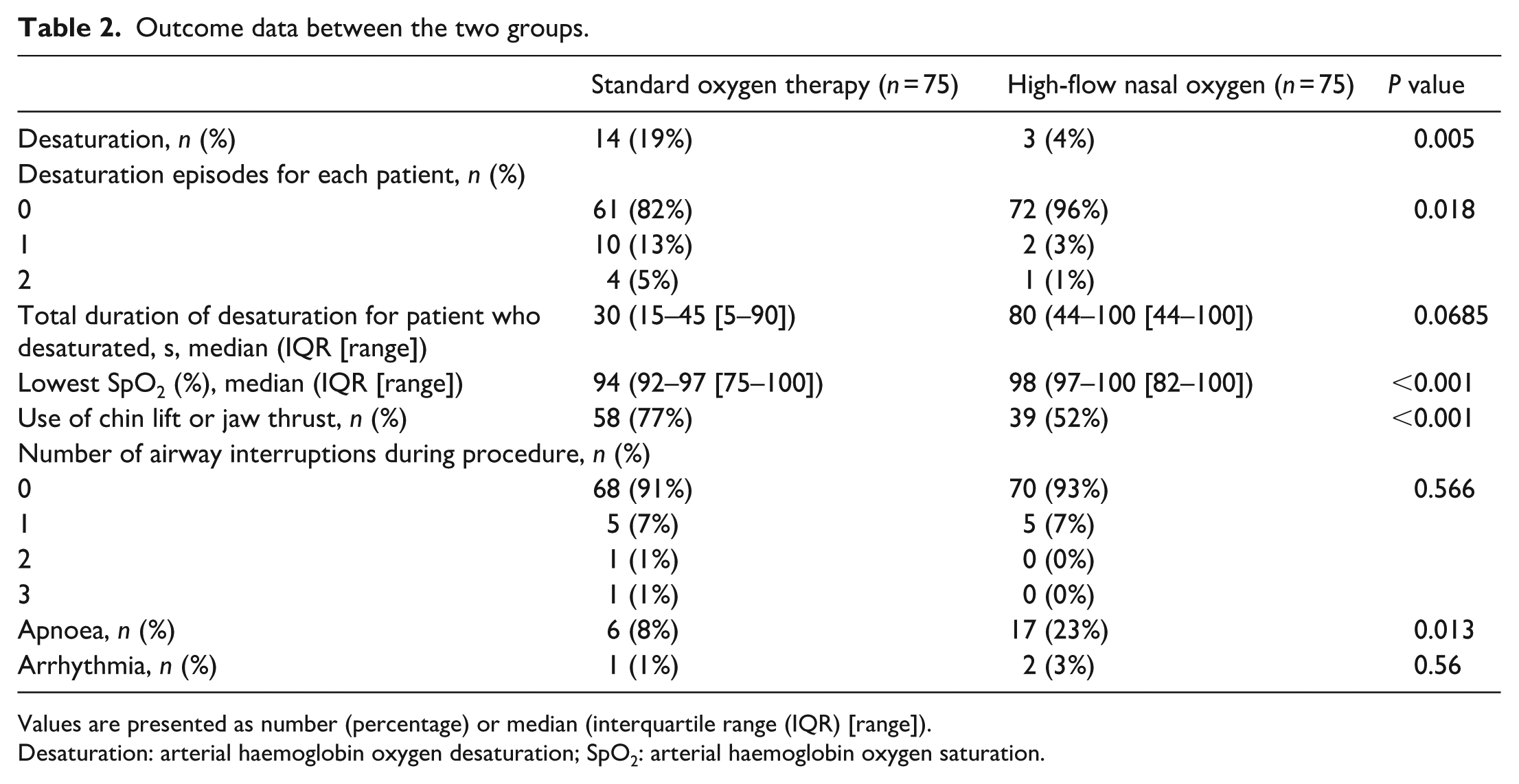
Values are presented as number (percentage) or median (interquartile range (IQR) [range]).
Desaturation: arterial haemoglobin oxygen desaturation; SpO2: arterial haemoglobin oxygen saturation.
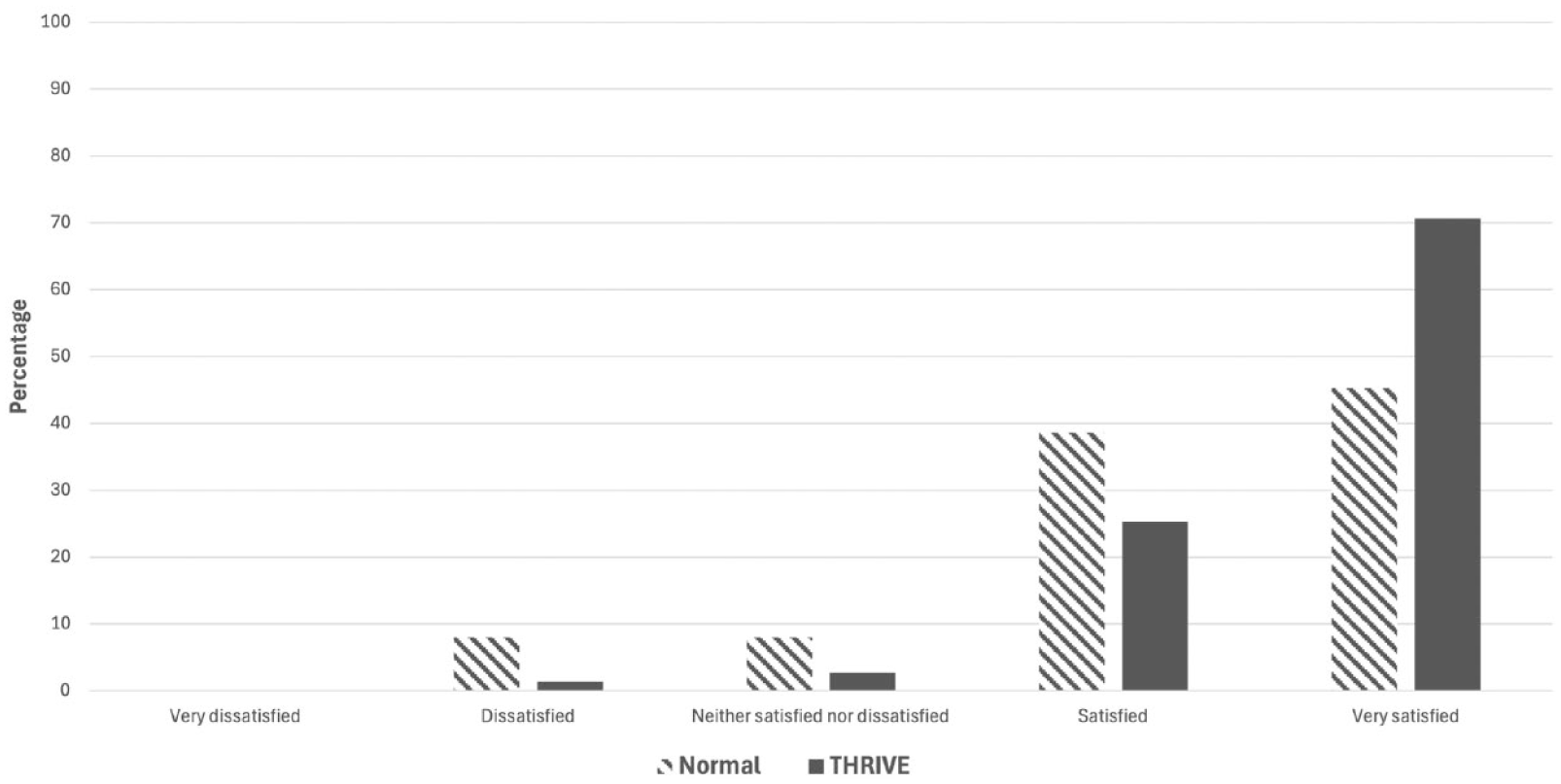
Anaesthetists’ satisfaction score results comparing the standard oxygen therapy group and the high-flow nasal oxygen group.
Discussion
This study supports the hypothesis that high-flow nasal oxygen reduces the incidence of desaturation during gastroscopy procedures in obese adult patients compared with low-flow nasal oxygen, with a number needed to treat of seven patients. The data provide some support to the idea that high-flow nasal oxygen reduces the need for airway interventions during gastroscopy in this patient population.
While not reaching statistical significance in our study, the finding that desaturation could be more prolonged in the high-flow nasal oxygen group is clinically concerning and requires investigation in larger studies that are adequately powered to examine this outcome. Potential explanations for the reduced incidence of desaturation despite the similar rate of apnoea in the high-flow nasal oxygen group include either the high fraction of inspired oxygen in this group achieving better pre-oxygenation at the onset of apnoea, 20 or the phenomena of apnoeic oxygenation. 21 Our data are unable to clarify which is the more important reason as we did not measure the relevant physiological variables.
The trend towards increased satisfaction reported by anaesthetists when patients were allocated high-flow oxygen compared with low-flow oxygen may reflect the lower incidence of desaturation, the lower use of airway interventions (and corresponding lower workload) or a greater perceived safety margin that may be independent of the physiological effects of the intervention. Significant complications were rare in both groups, although this trial did not have sufficient power to detect rare life-threatening complications of desaturation. A clinically significant effect of high-flow nasal oxygen in maintaining airway patency in obese patients appears unlikely, as 52% of the patients allocated to this group required airway maneuvers during the procedure, although the data are unable to clarify if these interventions were applied for a clinical indication or as part of anaesthetists’ routine practice. For obese patients who cannot tolerate even brief periods of desaturation (for example those with severe pulmonary hypertension), high-flow nasal oxygen may be helpful to allow them more safely to tolerate deep sedation for gastroscopy.
This trial joins several others recently examining the use of high-flow nasal oxygen in patients with obesity having gastroscopy or similar procedures.16,19 The study is concordant with these results and supports the overall hypothesis that high-flow oxygen may be helpful in reducing desaturation during these procedures in vulnerable adults. However, it stands in contrast to some other trials reporting negative outcomes, 13 the reasons for which are not immediately clear but may include differences in the degree of obesity seen in the various trials or other patient or procedure-specific factors. A formal diagnosis of obstructive sleep apnoea (OSA) was only noted in less than 12% of participants of our trial, which is markedly lower than in other populations of obese patients. 22 While it is difficult to establish if the true rate of OSA was higher in this group, a lower rate of OSA may have improved the efficacy of high-flow oxygen in maintaining airway patency in this trial.
A formal health economic evaluation of this intervention is needed to understand if the use of high-flow nasal oxygen can be justified on cost grounds. The use of high-flow nasal oxygen has been associated with a larger environmental impact compared with low-flow oxygen therapy, 23 although our study did not collect data relating to this outcome. Much larger studies will be required to understand the impact of high-flow nasal oxygen on life-threatening complications or mortality. Despite this, we observed increasing numbers of anaesthetists refusing to include patients in the trial due to a desire to use high-flow nasal oxygen as the oxygenation strategy during the trial period, suggesting that practice was changing ahead of the evidence that high-flow nasal oxygen reduced the incidence of desaturation.
Limitations
The trial has a number of limitations. The most important include the fact it was unblinded out of necessity and this may have introduced an element of performance bias although the primary outcome, being objectively measured, mitigates this risk. The use and dosing of sedative medications were not controlled; however, natural variation in practice ensured the groups were balanced. The generalisability of this trial may be limited by choices specific to the hospital (provision of sedation by specialist anaesthetists), and the choices of anaesthetic agents that may influence the risk of desaturation. High-flow oxygen may have diluted exhaled CO2, which may explain the higher incidence of apnoea observed in that group. The decision to apply a conservative correction for the multiple secondary analyses may limit the ability of the study to discover hypothesis-generating results from these analyses, although it does limit the risk of over-interpretation of the secondary outcomes, especially as the sample size calculation was based around the primary outcome rather than the secondary outcomes.
Conclusion
High-flow nasal oxygen resulted in fewer desaturation events per patient and reduced the degree of desaturation during the procedure compared with standard oxygen therapy. The need for airway intervention was also reduced. Life-threatening complications of sedation were rare in both groups and occurred at similar rates. Obese patients who cannot tolerate even brief desaturation may benefit from high-flow oxygen if deep sedation is required to facilitate gastroscopy procedures.
Supplemental Material
sj-docx-1-aic-10.1177_0310057X251382261 – Supplemental material for A randomised controlled trial of high-flow nasal oxygen compared with standard oxygen delivery in obese patients undergoing gastroscopy
Supplemental material, sj-docx-1-aic-10.1177_0310057X251382261 for A randomised controlled trial of high-flow nasal oxygen compared with standard oxygen delivery in obese patients undergoing gastroscopy by Ned Douglas, Reny Segal, Kane O’Donnell, Keat Lee, Roni Krieser, Paul Mezzavia, Shan Hung, Ying Wei Chen, Teresa Sindoni and Irene Ng in Anaesthesia and Intensive Care
Footnotes
Author contributions
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
