Abstract

Conventional surgical outcome measures have focused on mortality and postoperative complications from a biological perspective.1,2 However, fundamental concerns for patients relate to how they feel and function after an anaesthetic and operation and these outcomes have become an essential measure of quality of perioperative care.3,4 Patient-centred care requires clinicians to recognise patient outcomes that are most valued and most important to the patient themselves. 3
A classification of measures of perioperative patient-centred outcomes includes recommendations for the use of a life-impact measure (Days Alive and at Home up to 30 days post-surgery—DAH30), 5 a health-related quality of life measure (EuroQol 5 Dimension—EQ-5D), 6 and a functional status measure (World Health Organization Disability Assessment Schedule 12-question version—WHODAS 2.0). 7 We performed a survey at Wollongong Hospital in the Illawarra Shoalhaven Local Health District (ISLHD) network in New South Wales, Australia, to quantify the relative value given to the importance of these distinct validated outcomes from the perspective of the surgical patient themself.
The study was approved by the ISLHD Low Risk Negligible Risk Research (LNR) Review Committee on 15 November 2022 (ISLHD/LNR/2022-195). We developed a questionnaire to evaluate the patient-valued importance on the postoperative outcomes, consisting of questions listed in the EQ-5D, the WHODAS 2.0 and DAH30 measures. Duplicate questions were listed only once. The questionnaire asked respondents to rate the importance of each item using an interval rating scale of 1–10.
We included adult inpatients within 30 postoperative days who could answer the questionnaire themselves. A total of 106 patients were approached with an invitation to participate in the study, with 100 participants consenting and completing the questionnaire. Descriptive statistics were applied to the interval data to determine the central scores and distribution for each item of the questionnaire.
The surveys were completed between November 2022 and March 2023. Participants ranged in age from 24 to 104 years, with a median age of 69.5 years. Fifty-one percent were male. The types of surgery undergone by participants included general surgery, orthopaedic, plastic and reconstructive surgery, urology, gynaecology, gastroenterology, and vascular surgery. As almost every question returned a median and mode score of 10/10, mean scores were also calculated to provide more discrimination. The 15 items were then ranked in order of mean score (Table 1).
Questions ranked according to mean participant scores.
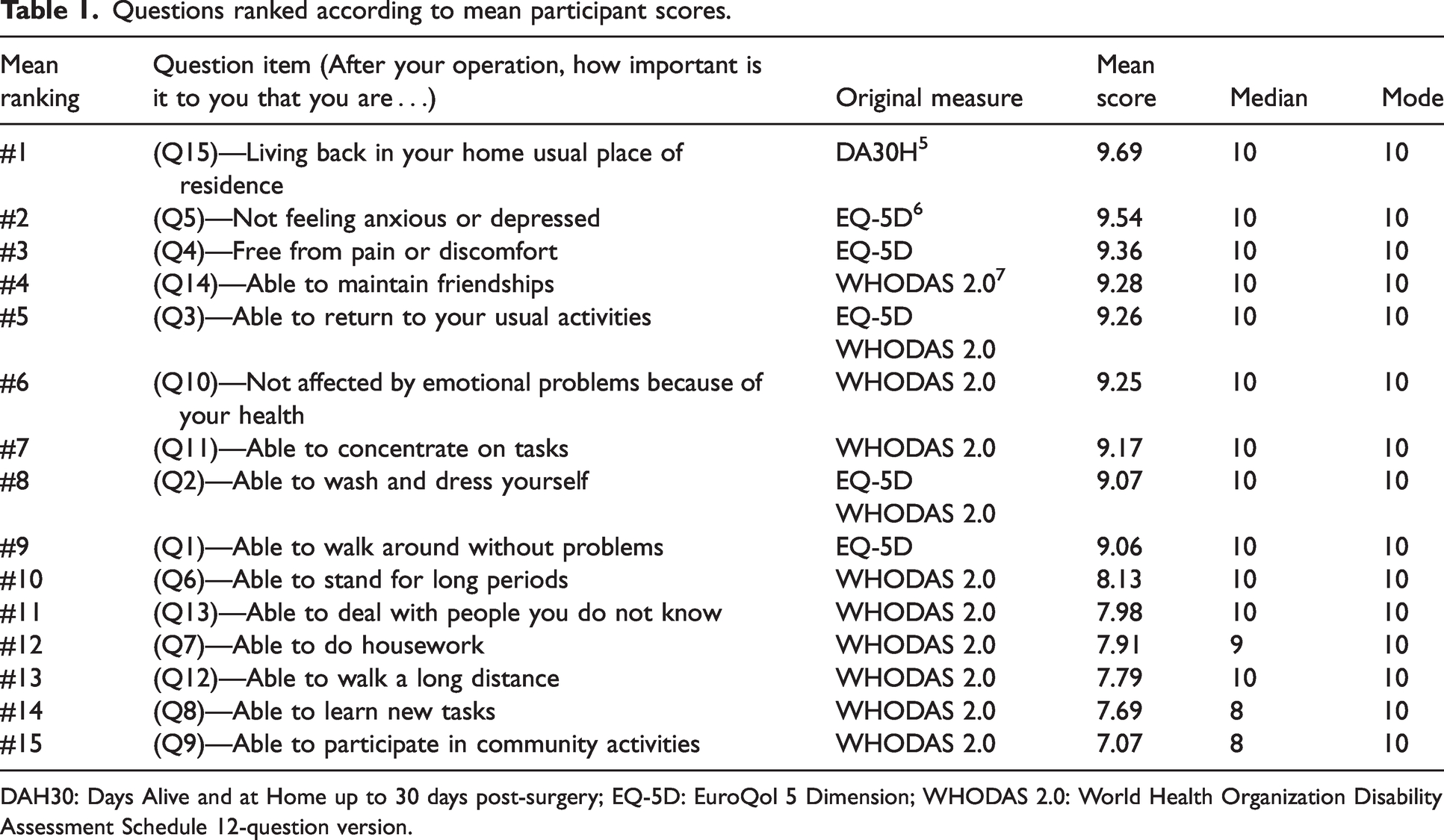
DAH30: Days Alive and at Home up to 30 days post-surgery; EQ-5D: EuroQol 5 Dimension; WHODAS 2.0: World Health Organization Disability Assessment Schedule 12-question version.
The highest ranked question was the importance of returning to living back at the participant’s usual residence, which reflects the DAH30 concept. Participants aged over 70 years gave slightly higher mean scores to all items apart from three of the five lowest ranked items.
One hundred postoperative patients rated all questions in the DAH30, 5 EQ-5D 6 and WHODAS 2.0 7 tools as being very important to their postoperative recovery. The mode for each question was 10/10, with means greater than 7 for all items. The highest ranked outcome was for patients to be back living in their own home, which supports the use of the DAH30 as a single outcome measure. Most of the EQ-5D items scored more highly than most of the WHODAS 2.0 items. Our small real-world survey reinforces the value of using these tools to rate patient satisfaction and recovery.
Measures of physical, emotional and social outcomes are clearly an addition to traditional morbidity and mortality outcomes. Patient age did not appear to impact the importance of most outcomes, though most outcomes were scored as being slightly more important to older compared with younger participants. Only one item, ‘ability to learn new tasks’, was deemed less important for older participants. These results suggest that the recommended domains have utility across a broad range of adult ages.
Ladha and Wijeysundera noted the utility of understanding patients’ preferences and values in the perioperative period, and the need for data on how patient-centred outcomes may change after a surgical procedure. 1 The recommendations from the standardised endpoint in perioperative medicine core outcome measures for perioperative and anaesthetic care (StEP-COMPAC) group are supported by our results, signifying that these domains were all outcomes that patients rated as important in the postoperative period. 5 Our data support the validity and relevance of these models towards patient-centred care, emphasising the importance of incorporating these patient-centred outcomes into postoperative measures.
In summary, we investigated the patient-centred perioperative measures that are most important from the patient perspective. We found that all questions in the DAH30, WHODAS 2.0 and EQ-5D tools were rated as important, with return to home as the most highly rated single measure. The results emphasise the importance of a range of patient-valued outcomes in the postoperative period that include measures related to physical, social and mental wellbeing.
Footnotes
Author Contribution(s)
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
