Abstract
Over the course of the past six decades, liver transplantation has evolved to become the treatment of choice for chronic end-stage liver disease and some cases of acute hepatic failure. Currently, more than 34,000 liver transplants are conducted worldwide per annum, and overall one year survival rates exceed 90%. However, the early years of human liver transplantation were beset by failure. Eyewitness reports from this period make for tragic, yet compelling reading. Volume 12 of The History of Anaesthesia Society Proceedings contains one such account, written by Dr Elizabeth Gibbs. This outlined the experience of single-handedly anaesthetising the recipient of the first liver transplant to be undertaken at Addenbrooke’s Hospital, Cambridge, UK, in June 1967. Despite the best efforts of the team, the patient died from uncontrollable haemorrhage 19 hours after the start of the procedure. While this tragic outcome might have been expected in the early days of liver transplantation, Gibbs included an unsettling postscript in her paper. This stated that all of the patient’s records had apparently been ‘lost’, and the date of the first Cambridge liver transplant was publicly reported as 2 May 1968, some 11 months after the events described. This article outlines the results of research aimed at critically appraising this postscript. In doing so a number of unexpected discoveries were made. These highlight some important lessons for medical historians and demonstrate that if you look hard enough, there really are two sides to every story.
Only those who dare to fail greatly, can ever achieve greatly.
Robert F Kennedy, 1966 1
A triumph of modern scientific and clinical endeavour, liver transplantation has evolved to become the treatment of choice for chronic end-stage liver disease and some cases of acute hepatic failure. Currently, more than 34,000 liver transplants are conducted worldwide per annum, 2 and advances in surgical technique, anaesthetic management and immunosuppressive medication have resulted in overall one year survival rates that exceed 90%. 3 Despite this success, the early years of human liver transplantation were beset by failure. Eyewitness reports from this period make for tragic yet compelling reading, recording heroic surgical procedures in desperately ill recipients, along with vivid descriptions of the complications encountered.
Volume 12 of The History of Anaesthesia Society Proceedings contains one such account, written by the late Dr Elizabeth Gibbs. 4 This outlined the experience of single-handedly anaesthetising the recipient of the first liver transplant to be undertaken at Addenbrooke’s Hospital, Cambridge, UK, in June 1967. At the time, Gibbs was a newly appointed senior registrar and entirely unaware that such an operation was even possible. Arriving in theatre one morning, expecting to anaesthetise a patient for a cholecystectomy, she was informed that there had been a change of plan, and Professor (later Sir) Roy Calne would be attempting a liver transplant instead. Despite her best efforts, Gibbs was unable to obtain the assistance of a consultant anaesthetist, and met the patient, a jaundiced middle-aged man, for the first time when he appeared in her anaesthetic room. No specific preparation had been made for the operation and the anaesthetic technique used for renal transplants was hastily adapted. Physiological monitoring comprised her hands, eyes and a sphygmomanometer, and intravenous access consisted of two peripheral drips. Faced with massive intraoperative bleeding, Gibbs and her anaesthetic nurse transfused a total of 54 pints of citrated blood, which they attempted to warm by placing the tubing of the giving set in a bowl of hot water. Despite the best efforts of the team, the patient died from uncontrollable haemorrhage 19 hours after the start of the procedure.
While this tragic outcome might have been expected in the early days of liver transplantation, Gibbs included an unsettling postscript in her paper. This stated that all of the patient’s records had apparently been ‘lost’, 4 and the date of the first Cambridge liver transplant was publicly reported as 2 May 1968, some 11 months after the events described.
This article outlines the results of research aimed at critically appraising this postscript. Unfortunately, hopes of rapidly settling the matter were dashed when it indeed proved impossible to locate any of the clinical records relating to the case in the hospital archives. However, the archivist reported that this situation was far from unusual at Addenbrooke’s, and missing records have long proved to be a stumbling block for those attempting retrospective research projects within the institution. It was therefore necessary to assess the validity of Gibbs’ statements with reference to the widely accepted historiography of liver transplantation, before examining the accuracy of this body of work itself. In doing so, a number of unexpected discoveries were made. These highlight some important lessons for medical historians, and demonstrate that if you look hard enough there really are two sides to every story.
The established historiography of liver transplantation
The early history of liver transplantation has been documented in a number of books5 –11 and journal articles,12 –21 as well as several reputable sites on the world wide web.22 –25 Predominantly written by clinicians who were intimately involved in the evolution of the specialty, including Thomas Starzl,6,13,18 and Roy Calne,5,14,19 these accounts present a relatively standardised and seemingly incontrovertible version of events, which can be summarised as follows.
Three separate strategies for transplantation of the liver were developed in canine models during the 1950s. In 1952, Vittorio Staudacher, professor of surgery at the University of Milan and director of the Department of Emergency Surgery at the Policlinico of Milan, was the first to describe a technique for orthotopic transplantation, in which the donor organ was placed in the normal anatomical position following removal of the recipient’s liver. Three years later at Albany Medical College, New York, C Stuart Welch reported a method for heterotopic (also known as auxiliary, or accessory) transplantation. The native liver was left in place and the donor organ implanted in the right paravertebral gutter of the recipient. Finally, by late 1959, Starzl and colleagues from the Department of Surgery, Northwestern University Medical School, Chicago, had devised a multivisceral procedure, during which the liver, stomach, pancreas, spleen, small bowel, colon and omentum were removed en bloc, and replaced with comparable donor organs.
Experimental researchers including Starzl and Francis Moore, chief of surgery at Peter Bent Brigham Hospital, Boston, subsequently focused their attention on the orthotopic and heterotopic techniques, and after an extended period of work it became clear that total hepatectomy and orthotopic liver replacement, rather than engraftment of an auxiliary liver was the procedure that offered most hope of long-term survival, and thus clinical utility.
Between March and June 1963, Starzl conducted the first three human liver transplants in Denver, Colorado, using the orthotopic technique he had refined in dogs. This included the employment of external venovenous bypass circuits to decompress the inferior vena caval and splanchnic venous beds during the recipient hepatectomy (which required clamping of the intrahepatic vena cava and portal vein), because it had been found that failure to obtain satisfactory drainage of these venous pools proved fatal in canine experiments. Tragically, the first human recipient, a 3-year-old boy named Bennie Solis, bled to death on the operating table 4 hours after revascularisation of the transplanted liver. The recipients of Starzl’s second and third clinical transplants died 22 and 7.5 days postoperatively from massive pulmonary emboli. Although the Denver group attempted two further procedures in July and October 1963, and there were single attempts made by Moore in Boston, and Jean Demirleau at the Hôpital Saint-Antoine, Paris, in September 1963 and January 1964, respectively, survival among the recipients of the first seven human liver transplants ranged from zero to 23 days. As a result, there were calls for a worldwide moratorium on liver transplantation, and it is widely reported that all human liver transplant activity ceased until July 1967, when Starzl performed the world’s first successful procedure, judged by the extended survival of the recipient beyond 90 days. Calne meanwhile has frequently stated that he undertook the first liver transplant at Addenbrooke’s Hospital on 2 May 1968, and faced significant opposition from his peers, as the operation had never been attempted in the hospital, or the United Kingdom. The patient survived for 11 weeks postoperatively before succumbing to partial graft infarction.
This widely perpetuated historical narrative fails to reference the procedure in which Gibbs was involved in June 1967, and provides strong support for her suggestion that the events of that day were withheld from public scrutiny. However, before settling on this disturbing conclusion, it seemed important to examine the accuracy of this accepted historical record itself. Within the wider historiography of medicine, secondary historical accounts have previously been shown to promulgate omissions, myths and falsehoods, and in the case of human liver transplantation, a thorough search of the primary scientific literature was to yield an altogether different story.
Original reports of human liver transplantation in Cambridge
In November 1968 Roy Calne and Roger Williams, consultant physician and member of the Medical Research Council Group on the Metabolism and Haemodynamics of Liver Disease at King’s College Hospital, London, published two papers in the British Medical Journal detailing their initial experience of human liver transplantation in the collaborative Cambridge/King’s College Hospital programme.26,27 The authors included a detailed description of the transplant undertaken by Calne on 2 May 1968, but curiously, this was not the first case in the chronologically ordered series.
‘Case 1’ concerned a 47-year-old man with a history of decompensated alcoholic liver disease who had been admitted to Addenbrooke’s Hospital on 23 May 1967. 26 At the time of his admission, it is stated he was pale and jaundiced, with marked ascites. A spleno-portogram showed large gastro-oesophageal varices. The patient went on to have two episodes of haematemesis and melaena requiring transfusion, and was comatose for one week. Having recovered consciousness, his case was discussed and the consensus reached that his liver disease was beyond conventional therapy. The possibility of hepatic transplantation was discussed and the patient was anxious that it should be tried.
In June 1967, a donor organ suddenly became available when a 50-year-old woman was brought into the hospital following a severe head injury. Resuscitation efforts were made for half an hour before she was declared dead and her liver rapidly harvested. The recipient operation occurred under ‘light general anaesthesia’ 26 and the liver was inserted into the abdomen at around 11:30 hours, 3 hours after the death of the donor. Following formation of arterial and venous anastomoses the liver appeared to perfuse adequately. The bile duct was then ligated and the gall bladder joined to the end of a Roux loop of jejunum. The abdomen was subsequently closed in layers and, although no heparin had been administered, a steady but continuous loss of blood was noticed from the drains. Two hours after the operation, the bleeding became more profuse and blood oozed from the wound. This clotted and then underwent complete fibrinolysis after about 20 minutes. The abdomen was thus reopened and bleeding was seen to be coming from the whole operative site. Haemorrhage continued in spite of the administration of a total of 23 litres of blood, and the patient died at 05:30 hours the next morning.
This is undoubtedly the same case described by Gibbs, and its inclusion in the first high profile paper emanating from the Cambridge/King’s College Hospital group definitively refutes any suggestion that the procedure was covered up. However, it is also proof that the widely accepted history of liver transplantation is factually incorrect, and that the first procedure in Cambridge took place in June 1967, not May 1968 as stated.
Semantics and human nature
The reasons behind this apparent confusion lie partly in semantics, and partly in human nature. As outlined above, techniques for orthotopic and heterotopic liver transplantation were developed in canine models during the 1950s and early 1960s. As this research progressed, it became apparent there were advantages and disadvantages to both operations. Orthotopic transplantation made revascularisation and biliary drainage straightforward, but required preliminary hepatectomy in the recipient. Engraftment of an auxiliary liver, on the other hand, presented a much less serious surgical undertaking, and there was also the possibility that residual function in the recipient’s liver might prove life-saving if uncontrolled rejection or graft failure occurred. However, it was often difficult to site the donor liver ectopically and there was an ever-present danger that its vascular and biliary anastomoses could become kinked or otherwise compromised. By the early 1960s the orthotopic procedure had proved far superior in dogs, and each of first seven human liver transplants undertaken between March 1963 and January 1964 were orthotopic.28 –31 So too was the procedure undertaken in Denver in July 1967, which resulted in extended survival of the recipient, 32 and also the transplant undertaken by Calne on 2 May 1968.26,27
In contrast, in June 1967 Calne performed the less technically demanding heterotopic operation, in which the patient’s cirrhotic liver was left in situ, and the donor organ placed in the splenic fossa (Figure 1). 26 This was in fact the seventh case of human heterotopic liver transplantation reported in the world literature. Karel Absolon and colleagues performed the first in a 13-month-old boy with extrahepatic biliary atresia at the University of Minnesota in November 1964. 33 Starzl attempted three cases in Denver during 1965, 34 and the fifth and sixth reported auxiliary liver transplants were undertaken in late 1966 34 and early 1967. 35 Recipient survival was poor in all cases, and with the exception of a brief chapter in Starzl’s memoir The puzzle people, 6 these heterotopic procedures rarely appear in accounts outlining the history of human liver transplantation. Even more bizarrely, the first six heterotopic transplants were completed during the self-imposed moratorium on liver transplantation (January 1964—July 1967) at which time it is widely stated that all activity had ceased in human subjects worldwide.
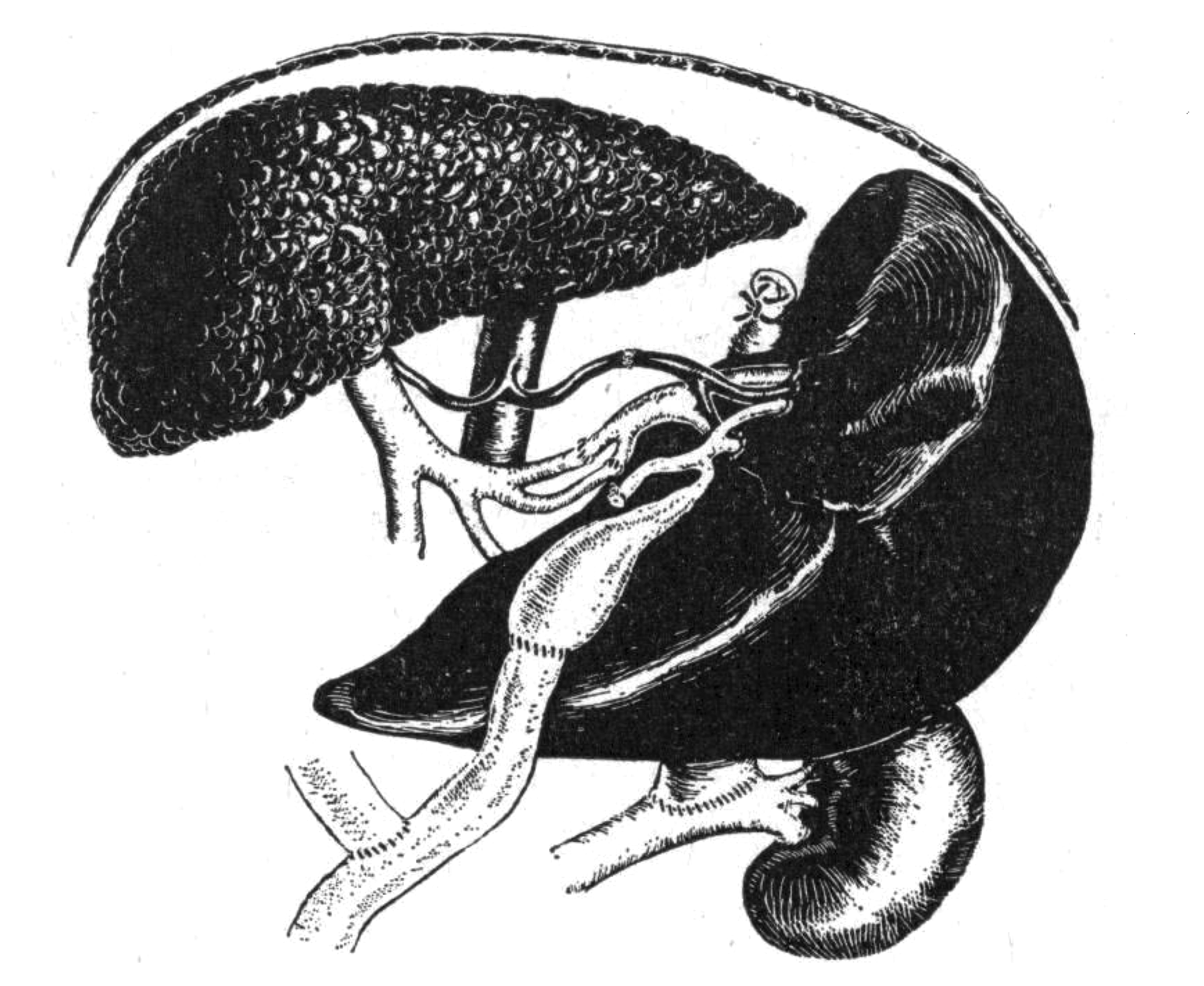
Diagram of operative procedure conducted in June 1967, showing heterotopic liver allograft in the splenic bed. 26 Reproduced with permission from BMJ Publishing Group Ltd.
By 1969 a total of nine heterotopic cases had been reported in the literature, and Starzl discussed these in his book Experience in hepatic transplantation, 31 published the same year. Somewhat shockingly, he noted that these documented efforts represented only a small fraction of the actual heterotopic transplant experience accrued; it was known by personal communication, newspaper reports and word of mouth that as many as 25 other unsuccessful trials had been made worldwide. A year later, Joseph Fortner and colleagues from the Memorial Hospital, New York City, were the first to report extended survival in six heterotopic liver transplants, but in spite of their success, the technique has never gained clinical acceptance. 36
Reviewing these findings, it is clear that attempts at human heterotopic liver transplant have largely been omitted from the body of work outlining the evolution of the specialty, and the established history of human liver transplantation has become exclusively that of the orthotopic procedure. Why might this be the case?
One appealing possibility revolves around the human preference to emphasise success, and avoid dwelling on failure. The surgical pioneers of liver transplantation were extremely driven, and dedicated themselves to mastery of a procedure that many told them would be ‘too difficult to ever be feasible’. 20 This they somehow achieved while transplanting recipients who were, at best, too ill for an independent existence outside of hospital, and often frankly moribund. 27 For those attempting the first procedures, in which there was little previous experience, mistakes were made at every stage, and death became a tragic, but all too common, conclusion. That is not to say, however, that those involved were not personally affected. Reflecting on the death of Bennie Solis following the first attempted orthotropic liver transplant in 1963, Starzl recorded: ‘Bennie was only three years old and had not enjoyed a trouble-free day in his life … his wound was closed and he was wrapped in a plain white sheet after being washed off by a weeping nurse.… The surgeons stayed in the operating room for a long time after, sitting on the low stools around the periphery, looking at the ground and saying nothing … It was not the last time I would see this scene, both in my dreams and in reality. I never heard anyone who was there describe this as “the Solis case”, or the first human liver transplantation. If they mentioned it at all, it was always just about Bennie.’ 6
In addition, more practical factors may have been at play during the 1960s. At the time Calne performed the heterotopic transplant in Cambridge, he was one of only three surgeons in the hospital, and Addenbrooke’s was little more than a district general hospital, with aspirations to become a teaching centre. Despite his success with kidney transplantation, Calne’s colleagues were largely sceptical of liver transplantation, and the establishment of a liver transplant programme required new infrastructure and funding, which was difficult to obtain. By highlighting success and downplaying failure, Calne could improve the standing of the operation among his peers, and bolster his chances of obtaining financial support.
In a letter to the author (written in September 2019), Calne confirmed: ‘The justification for reporting the first Addenbrooke’s case as 2 May 1968 was the perception that an orthotopic transplant was the procedure that eventually might help patients, whereas there was little to recommend the heterotopic operation. Thus, this was the beginning of a new and potentially valuable therapy.’
As a result, it appears the history of human liver transplantation, as documented by these pioneers, has focused exclusively on the path of progress—that is, the development of orthotopic transplantation, rather than the failure of the heterotopic procedure. Nevertheless, had the recipient of the heterotopic transplant in Cambridge survived for more than 90 days, it seems almost certain that this would have been recorded as the world’s first successful liver transplant.
Conclusion
Roy Calne performed the first heterotopic liver transplant at Addenbrooke’s Hospital in June 1967. The recipient was single-handedly anaesthetised by Elizabeth Gibbs. The first orthotopic procedure at Addenbrooke’s Hospital was undertaken on 2 May 1968. The widely reported worldwide moratorium on human liver transplantation existed only for attempts at the orthotopic operation, and early efforts at human heterotopic engraftment have largely been omitted from historical accounts, explaining the reasoning for the postscript in Gibb’s original paper. For medical historians, this reinforces the importance of always examining the original literature, and not relying on secondary accounts.
As for Dr Gibbs herself, it would appear she performed admirably in the face of adversity. In 1969 Antonio Aldrete and colleagues outlined the anaesthetic protocol which had been used for liver transplants in Denver since 1963. 37 This included a thorough preoperative evaluation and continuous intraoperative monitoring of invasive arterial and central venous pressures, as well as recording of the electrocardiograph, oesophageal temperature, urine output, acid-base status, and glucose and potassium levels. A similar setup was described in Cambridge in 1971, 38 where it was stated an experienced team consisting of at least two anaesthetists, a nurse and an operating theatre technician were always required.
Footnotes
Author Contribution(s)
Acknowledgements
The author gratefully acknowledges the assistance of Miss Hilary Ritchie, hospital archivist, Cambridge University Hospitals NHS Foundation Trust, who searched the hospital archives for any record of the heterotopic liver transplant undertaken in June 1967; Professor Sir Roy Calne, who corresponded with the author in 2019; and Dr Christine Ball, adjunct clinical professor, Department of Anaesthesia and Perioperative Medicine, Monash University, Melbourne, Australia, who discussed important aspects of this article during its preparation.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) received no financial support for the search, authorship and/or publication of this article.
