Abstract
Abstracts are published as supplied and have not been subject to editorial review or correction.
5
OUTCOMES AND DETERMINANTS OF IN-HOSPITAL CARDIOPULMONARY RESUSCITATION IN THE GENERAL WARDS OF A CARIBBEAN TERTIARY CARE TEACHING HOSPITAL
1The University Of The West Indies, Trinidad, Trinidad and Tobago
Introduction
The outcomes following in-hospital cardiopulmonary resuscitation (CPR) are variable in accordance with many factors including the resources and processes adopted.
Methods
This was a prospective observational study. Data recorded included patient demographics, comorbidities, reasons for CRASH, onset and duration of CPR, drugs and equipment utilized, availability of CRASH cart, return of spontaneous circulation, hospital length of stay and outcomes of patients.
Results
A total of 53 CRASH calls were studied. 77% of crashes occurred between 3 pm to 7 am. One-third of patients were 61–70 years old; 40% had ≥3 pre-existing co-morbidities. Vital signs were checked 0–4 h prior to CRASH calls in 68% of the patients. Despite the presence of red-flags, only 15% of patients were reviewed prior to CRASH. 45% patients had new symptoms prior to CRASH call, but half of them received no intervention. 90% of CRASH calls were responded in ≤10 minutes. Cause of 72% of crashes were recorded as “unknown”. Asystole was the presenting cardiac rhythm in 70%; 70% of patients were resuscitated for 10–20 min. Return of spontaneous circulation was achieved in 13% of patients; the overall survival rate >24 hours was 3.7%. However, no patients survived to discharge. Prognosis was already deemed poor in 36% of patients. 11 patients had palliative care documented in their notes, yet 9 of these patients were resuscitated. Issues recorded included unavailable ECG (17%), NIBP (9%), pulse oximetry (13%), suction apparatus (94%) and oxygen (4%).
6
WHICH AGE CONFERS AN INDEPENDENT RISK OF MORTALITY IN ICU PATIENTS AT A LARGE TEACHING HOSPITAL IN SINGAPORE?
1Changi General Hospital, Singapore, Singapore
Introduction
Previous studies have demonstrated conflicting results regarding age as an independent predictor of mortality in critically ill medical patients.
Methods
Retrospective review of consecutive patients admitted to the MICU over a 5 month period. We analyzed 5 age cut-offs (60, 65, 70, 75 and 80 years) to determine if any of these conferred an independent risk of mortality. Modified APACHE II score was used to assess the severity of illness.
Results
A total of 211 patients were included in the study. Patients aged ≥65 years were more likely to die during the hospital admission compared to < 65 years. Even after adjustment made for APACHE II score, age ≥65 remained an independent risk factor for hospital mortality; 38.9% vs 22.4% (OR 2.7, 95% CI 1.3–5.7, p = 0.008). Modified APACHE II scores, ICU length of stay (LOS), hospital LOS and MICU readmission rates were not statistically different at any age cut-off. Patients aged ≥65 years were more likely to have DNR orders put in place after their admission to the ICU.
Conclusion
Age ≥65 years is an independent risk factor for mortality in MICU patients. This information may be useful for physicians while triaging patients for admission to ICU and for communication with family members. This is important in a country like Singapore, which has advanced healthcare and a rapidly ageing population.
7
DO PROCALCITONIN LEVELS PREDICT THE SEVERITY OF ILLNESS AND RISK OF DEATH IN PATIENTS WITH SEVERE SEPSIS?
1Changi General Hospital, Singapore, Singapore
Introduction
High procalcitonin (PCT) levels are seen in systemic bacterial sepsis and there is some evidence that the levels correlate with disease severity, mortality and presence of bacteremia. There is a paucity of such data from South East Asia for the critically ill patients.
Objectives
We examined these correlations at our hospital, which is a 1000 bedded teaching hospital in Singapore.
Methods
Chart review of consecutive patients admitted to the medical intensive care or high dependency units with a diagnosis of severe sepsis (as defined by the 2012 Surviving Sepsis guidelines). The cut-off value for high PCT levels used in our lab is >0.5 ng/ml. Patients were divided into 3 groups A) levels <0.5 ng/ml B) 0.5 to 2 (mild elevation) and C) > 2 (moderate to severe elevation). SOFA score was used to assess disease severity on admission. Between the 3 groups, we examined the SOFA scores, hospital mortality and the yield of blood cultures.
Results
129 patients were included. Most (61%) were men, median age 62 years, median SOFA score on admission 12 and median PCT value 11.7 ng/ml (range < 0.5 to 100).
Group A had 12 patients, median SOFA score 10, mortality 16%, positive blood cultures 0%.
Group B had 14 patients, SOFA score 12.5, mortality 7%, positive blood cultures 7%.
Group C had 103 patients, SOFA score 12, mortality 29%, positive blood cultures 42%.
There was no significant difference in SOFA score between the 3 groups (p value 0.07). Mortality rates were considerably higher in Group C as compared to the other 2 groups, but did not achieve significance (p value 0.16). The yield of blood cultures were higher in Group C (p value <0.001).
Conclusion
The vast majority (80%) of patients had moderate to severe elevations of PCT. Higher PCT levels had significant correlation with blood culture positivity, but no correlation with disease severity on admission. Although high levels were associated with higher mortality, it did not reach statistical significance. This could have been influenced by the small number of patients in Groups A and B.
9
SOCIAL DETERMINANTS OF RESUSCITATION STATUS (“DO NOT RESUSCITATE” VS. “FULL CODE”) IN CRITICALLY ILL PATIENTS >70 YEARS
1Desert Regional Medical Center, Palm Springs, United States
Introduction
We set out to investigate whether race, religion, education level, occupation, income, patients’ age, gender, etc, influenced one’s resuscitation decision. Prior studies by Jorge, et’al (2000) and Dong, et’al (2014) investigated some associations but were limited to patients with acute myocardial infarction and to hospitalized septic patients, respectively.
Methods
n = 77: We included all patients 70years and older who were inpatient on Saturday August 4th, 2018. This “entire-hospital-on-a-single-day” approach was designed to eliminate selection and sampling biases. Interested participants (52/77) were consented and given English or Spanish questionnaires. 25/77 patients were excluded due to: “confused or sedated” (3/25), “off floor for procedure” (9/25), “sleeping” (1/25), “deceased” (1/25), “discharged” (1/25) and “declined” (10/25).
Results
14
INTRAOSSEOUS VERSUS ARTERIAL BLOOD SAMPLING IN HAEMORRHAGIC SHOCK
1Uppsala University Hospital, Uppsala, Sweden
Introduction
Shock is frequently associated with difficulties in obtaining vascular access. Intraosseous (IO) administration of fluids and drugs may contribute to survival. Blood sampling is necessary in order to steer therapeutic interventions. Aspiration of bone marrow through an IO needle may potentially damage conventional laboratory equipment. Point-of-care testing (POCT) allows the sample to be analyzed within a cartridge.
Objectives
To compare IO versus arterial blood samples, analyzed by POCT, in an experimental model of haemorrhagic shock, corresponding to ATLS shock class 2 and 3–4.
Methods
Twelve anaesthetised pigs were included in this experiment, which was approved by the local ethics committee (C155/14; 20141024). Arterial, pulmonary arterial, and central venous catheters were inserted. IO access was obtained through tibial insertion of 15 G EZ-IO needle. POCT was performed using an i-STAT equipped with EG7+ and CG4+ cartridges. Exsanguination of 20% and 40%, respectively of the blood volume was performed during the 6h experimental procedure.
Results
Progressive hypotension and decreasing cardiac index occurred. Analyses of blood gases showed acceptable precision between the two kinds of POCT cartridges. Overall, differences between IO and arterial samples tended to increase over time as exsanguination became more expressed. pH was approximately 0.1 higher in arterial blood than in IO samples. PO2 was considerably higher in arterial blood compared to IO samples. PCO2 was between 7.5–15 mm Hg lower in arterial versus IO samples. Potassium was nearly 0.5 mmol/L higher in IO samples compered to arterial samples. Base excess, sodium, haemoglobin, and lactate were essentially in the same range.
Conclusions
Except for PO2, the difference between IO and arterial samples was limited in this shock model. However, dispersion must be taken into account. It is deduced that in an emergency, IO samples may help to guide initial therapy until reliable vascular access is achieved.
299 ord.
28
RISK OF SPINAL HAEMORRHAGE IN NEURAXIAL BLOCKS GIVEN TO CRITICALLY ILL PATIENTS TREATED WITH NEW DIRECT ORAL ANTICOAGULANTS
1Paediatric Anaesthesia and Intensive Care, SUS Lund University Hospital, Sweden, Lund, Sweden
2Intensive and Perioperative Care, SUS Lund University Hospital, Lund, Sweden
3Anaesthesia and Intensive Care, Institution of Clinical Sciences, University of Lund, Lund, Sweden
Introduction
neuraxial blocks may reduce morbidity and mortality in patients with various critical conditions, including orthopaedic injuries and abdominal emergencies requiring laparotomy. Patients treated with New/Direct-acting Oral Anti-Coagulants (NOACs or DOACs) present for intensive care more often now that these drugs are routinely prescribed as thromboprophylaxis.
Objectives
to present and evaluate current guidelines concerning the management of patients treated with DOACs requiring a neuraxial block, especially how hepatic and renal insufficiency affect DOACs’ elimination and thereby risk of spinal haemorrhage from neuraxial block.
Methods
A review was conducted using PubMed and known existing guidelines.
Results
Current guidelines pertain mainly to elective neuraxial blocks and not those in the critically ill. They rely on data concerning elimination half-lives: after 5 half-lives, 97% of a drug should be eliminated. Dabigatran’s half-life is significantly increased by renal failure.
aPTT and PT/INR are not recommended for monitoring DOACs. Dabigatran can be monitored by anti-IIa assay, diluted thrombin time and ecarin based assays, while apixaban, rivaroxaban and edoxaban can be monitored by anti-Xa assays. Whether these tests can be used to exclude significant risk of neuraxial haemorrhage is controversial.
NOAC’s have several clinically relevant interactions: e.g. clarithromycin, amiodarone and verapamil prolong dabigatran’s half-life. Case-reports describe dabigatran being eliminated by continuous renal-replacement therapy. At present dabigatran is the only NOAC with a specific antidote.
Limited previous experience of ‘non-complicated blocks’ in patients recently treated with NOAC may give a false sense of confidence, since the statistical upper-limit of the 95% confidence interval for the actual risk of an event that has not yet been observed in a series of n observations is 3/n.
Conclusions
In order to assess when it is safe to administer a neuraxial block, clinicians should be well-acquainted with NOACs’ pharmacology, and be aware of how this is affected by critical illness.
31
Successful management of severe diabetic ketoacidosis in a type-2 diabetes patient with insulin allergy
1Emergency Department, Bach Mai Hospital, Hanoi, Viet Nam
2Department of Emergency and Critical Care Medicine, Hanoi Medical University, Hanoi, Vietnam
3Allerology and Clinical Immunology Center, Bach Mai Hospital, Hanoi, Vietnam
4Department of Internal Medicine, Hanoi Medical University, Hanoi, Vietnam
5Endocrinology and Diabetes Department, Bach Mai Hospital, Hanoi, Vietnam
6Department of Allergy and Clinical Immunology, Hanoi Medical University, Hanoi, Vietnam
Introduction
Diabetic ketoacidosis (DKA) is an acute, major, life-threatening complication of diabetes mellitus (DM) that requires immediate treatment. The clinical presentation of insulin allergy can range from minor local symptoms to a severe generalized allergic reaction, especially anaphylaxis.
Methods
Case report.
Conclusions
In this patient, SIA caused an allergic reaction in contrast to continuous IV insulin infusion, for which allergic symptoms did not appear. Thus, identical insulin molecules could behave in markedly different ways depending on the route of injection.
32
Factors relating to mortality in patients with acute respiratory distress syndrome (ARDS) in Vietnam
1Emergency Department, Bach Mai Hospital, Hanoi, Viet Nam
2Teikyo University School of Medicine, Tokyo, Japan
3Department of Internal Medicine, National Defense Medical College, Saitama, Japan
4Department of Medical Risk Management and Infection Control, National Defense Medical College Hospital, Saitama, Japan
5Intensive Care Unit, Bach Mai Hospital, Hanoi, Vietnam
6Department of Emergency and Critical Care Medicine, Hanoi Medical University, Hanoi, Vietnam
7Yurin Hospital, Tokyo, Japan
8Waseda University, Tokyo, Japan
Introduction
Understanding the factors for mortality in acute respiratory distress syndrome (ARDS) is crucial for reducing mortality along with developing effective clinical management strategies. However, risk factors relating to mortality have not yet been fully elucidated in Vietnam.
Methods
We conducted a retrospective observational study in a national tertiary hospital in Hanoi, Vietnam. Participants were adult patients (age ≥18 years), admitted and diagnosed with ARDS during 2015–2017. Data on patients’ general and clinical conditions, radiographic findings, ventilator settings, gas exchange, and treatment methods were collected and compared between survivors and non-survivors and between days 1 and 3 after admission. Risk factors for mortality were assessed using a logistic regression analysis.
Results
Among 126 eligible patients (mortality, 57.1%), 94% were transferred from local hospitals. At the time of admission, the difference in mean (±SD) of PaO2/FiO2 between non-survivors (102.1 ± 52.5 mmHg) and survivors (120.0 ± 66.7 mmHg) was not significant (p = 0.079); however, PaO2/FiO2 on day 3 was improved in both nonsurvivors (126.3 ± 79.9 mmHg) and survivors (183.9 ± 98.9 mmHg), with statistical significance (p = 0.002). Multivariate logistic regression revealed that PaO2/FiO2 [odds ratio (OR), 1.010; 95% confidence interval (CI), 1.003–1.017] and length of stay in a local hospital before admission to the central hospital (OR, 1.122; 95% CI, 1.042–1.210) were independent factors for patient survivability.
Conclusions
Improvement in PaO2/FiO2 within 3 days of hospital admission (PaO2/FiO2 ≥150 mmHg) was crucial for reducing hospital mortality in patients with ARDS. In Vietnam, early transfer to a central hospital that could initiate appropriate treatment in early stages of ARDS was crucial for better outcome.
33
SURVIVAL TO HOSPITAL DISCHARGE: OR JUST OUT ONE DOOR, IN ANOTHER?
1Monash University, Bendigo, Australia
2Bendigo Health, Bendigo, Australia
Introduction
A common metric used to record survival following an in-hospital cardiac arrest (IHCA) is survival to hospital discharge. However, the use of this outcome may not be valid when the patient is discharged to another hospital, as opposed to home. Previous research has found that only a small proportion of IHCA survivors (15%) are discharged to a location other than home. However, this work has only been conducted in large metropolitan hospitals.
Methods
Data from a prospectively collected IHCA dataset in a regional hospital, 2000–2017, was linked to the state death registry and analysed using Cox survival analysis.
Results
During the study period, 225 adult patients who suffered an IHCA survived to discharge and were subsequently included. Of these patients only 94 (42%) were transferred home, with 107 (48%) transferred to another hospital. The remainder were transferred to rehabilitation facilities, aged care facilities or had missing data. Of the patients transferred to another hospital, the majority went to large metropolitan hospitals, likely for ongoing acute care (78/107; 73%). When long-term survival was compared between patients discharged home and those transferred to metropolitan hospitals there was no significant difference (p = 0.148) between the groups. The median follow-up in this study was 4.4 years’ post-arrest.
34
Effectiveness of combined external ventricular drainage with intraventricular fibrinolysis for the treatment of intraventricular haemorrhage with acute obstructive hydrocephalus
1Emergency Department, Bach Mai Hospital, Hanoi, Viet Nam
2Department of Neurology, Bach Mai Hospital, Hanoi, Vietnam
3Poison Control Centre, Bach Mai Hospital, Hanoi, Vietnam
4Department of Emergency and Critical Care Medicine, Hanoi Medical University, Hanoi, Vietnam
5Department of Neurology, Hanoi Medical University, Hanoi, Vietnam
6Emergency and Critical Care Department, Hanoi Medical University Hospital, Hanoi, Vietnam
7Department of Science Management, Thai Binh University of Medicine and Pharmacy, Thai Binh, Vietnam
8Epidemiology Department, Thai Binh University of Medicine and Pharmacy, Thai Binh, Vietnam
9Undergraduate Training & Management Department, Thai Binh University of Medicine and Pharmacy, Thai Binh, Vietnam
10Department of Postgraduate Management, Thai Binh University of Medicine and Pharmacy, Thai Binh, Vietnam
11Department of Neurosurgery II, Viet Duc Hospital, Hanoi, Vietnam
12Department of Neurosurgery, Caen University Hospital, Caen, France
13University of Caen Normandy, Caen, France
Introduction
Intraventricular haemorrhage (IVH) patients with acute obstructive hydrocephalus (AOH) who require external ventricular drainage (EVD) are at high risk for poor outcomes. Intraventricular fibrinolysis (IVF) with low-dose recombinant tissue plasminogen activator (rt-PA) can be used to improve patient outcomes.
Methods
This prospective cohort study included IVH patients with hypertensive intracranial haemorrhage complicated by AOH who required EVD. We evaluated the risk of death and the functional outcomes at one month and three months, with a specific focus on the impact of combined EVD with IVF by low-dose rt-PA.
Results
Between 2011 and 2014, eighty patients were included. Forty-five patients were treated with EVD alone (EVD group) and thirty-five received IVF (EVD+IVF group). The 30- and 90-day mortality rates were lower in the EVD+IVF group than in the EVD group (42.2% vs 11.4%, p = 0.003 and 62.2% vs 20%, p < 0.001; respectively). The Graeb scores were significantly lower in the EVD+IVF group than in the EVD group (p ≤ 0.001) during the first 3 days and at day 7 after assignment. The 30-day good functional outcome (mRS, 0 to 3) was also higher in the EVD+IVF group than in the EVD group (6.7% vs 28.6%; p = 0.008). However, the 90-day good functional outcome (mRS, 0 to 3) did not significantly increase in the EVD+IVF group (30.8% in the EVD vs 51.6% in the EVD+IVF group; p = 0.112).
Conclusions
In our prospective observational study, EVD+IVF was associated with a lower risk of death in IVH patients. EVD+IVF improved the chance of having a good functional outcome at one month; however, this result was no longer observed at three months.
35
Clinical outcomes in patients with acute respiratory distress syndrome (ARDS) in Vietnam according to severity of the Berlin definition
1Emergency Department, Bach Mai Hospital, Hanoi, V Nam
2Teikyo University School of Medicine, Tokyo, Japan
3Department of Internal Medicine, National Defense Medical College, Saitama, Japan
4Department of Medical Risk Management and Infection Control, National Defense Medical College Hospital, Saitama, Japan
5Intensive Care Unit, Bach Mai Hospital, Hanoi, Vietnam
6Department of Emergency and Critical Care Medicine, Hanoi Medical University, Hanoi, Vietnam
7Yurin Hospital, Tokyo, Japan
8Waseda University, Tokyo, Japan
Introduction
The burden of mortality of ARDS according to the Berlin definition has not ever been reported from Vietnam.
Methods
We conducted a retrospective chart review on patients who admitted and were diagnosed ARDS in Bach Mai Hospital (a national tertiary care hospital), Hanoi, Vietnam between 2015 and 2017. The data on ventilator settings and conditions on gas exchange were collected at the time of 1st day and the 3rd day of admission. The primary outcome was hospital mortality. The secondary outcomes included comparisons of respiratory conditions among three groups of ARDS severity on the Berlin definition.
Results
In 126 eligible patients, the median age was 53 (IQR, 39–63) years and 66% was male. 93% of direct risk for ARDS was pneumonia. Overall hospital mortality was 57.1%. In total patients, the period prevalence of severe ARDS on Day 1 was 53.0%; of moderate ARDS 37.3%; and of mild ARDS 9.5%. The ARDS severity changed on Day 3 due to improvement/deterioration of PaO2/FiO2 in each patient. Of the total patients on Day 3, severe ARDS was 27%; moderate ARDS, 35.7%; and mild ARDS, 12.7%. In addition, 6.3% of patients showed an improvement of over 300 of PaO2/FiO2. The hospital mortality did not differ significantly among three groups of ARDS severity on Day1 (p = 0.163), but when compared among three groups of ARDS severity on Day3, it was significant (p = 0.017). In the length of hospitalization using the Kaplan-Meier method, the survival time of severe ARDS was significantly shorter among three groups of ARDS severity on Day 3 (p = 0.030).
Conclusions
Our study demonstrated that the clinical outcome of ARDS patients in Vietnam depends on the improved ARDS severity within three days from the hospital admission. In Vietnam, the mortality of ARDS can be verified by the Berlin definition.
43
RISK FACTORS OF EXTUBATION FAILURE AFTER NEONATAL CARDIAC SURGERY ARE AIRWAY DISEASES AND PROLONGED MECHANICAL VENTILATION
1Royal Children’s Hospital, Parkville, Australia
2Shizuoka Children’s Hospital, Shizuoka, Japan
Introduction
Extubation failure (EF) is associated with the increased mortality. Younger age groups, especially neonates, are at risk of EF, ranging 6% to 21%. The epidemiologic knowledge of EF in these patients is crucial, and few data have been published.
Objectives
The primary aim of this study was to explore the incidence, etiology, and risk factors of EF. The secondary aim was to investigate outcomes of subsequent extubation and need for surgical reinterventions in EF cases.
Methods
Neonates (≤30 days old) who underwent cardiac surgery and were admitted to an intensive care unit from September 2010 to February 2016 were included. The prevalence and etiology of EF, defined as reintubation within 48 hours, were reviewed. Demographic, operative, and peri-operative data were retrospectively collected. Multiple logistic regression models were constructed to identify the risk factors for EF.
Results
EF occurred in 25 of 156 cases (16.0%; 95% confidence interval (CI) 10.6–22.7%). The etiology was respiratory dysfunction (n = 16), hemodynamic instability (n = 4), upper airway obstruction (n = 4), or gastrointestinal bleeding (n = 1). Subsequent extubations were successful in 17 (68%) cases because of medical optimization of the causes of reintubation. The remaining 8 cases needed surgical re-intervention including tracheostomy and cardiac surgery. The in-hospital mortality rate was 2.6%. In a bivariate analysis younger age, airway diseases, pre-surgery ventilation, prolonged mechanical ventilation, and delayed sternal closure were associated with EF. The multivariable analysis identified airway diseases (adjusted odds ratio 18.2, 95%CI 3.8–88.6, p = .0003) and mechanical ventilation >7 days (adjusted odds ratio 8.2, 95%CI 1.9–34.9, p = .0046) as risk factors for EF.
Conclusion
The prevalence of EF was high after neonatal cardiac surgery. The etiologies can be diverse. Extubation of neonates at high risk after cardiac surgery, based on these possible risk factors, requires more diligent approaches.
45
LONG-STAY PATIENTS UTILIZE SUBSTANTIAL RESOURCES AND BEDS IN PICU AND CARRY HIGH RISKS OF INFECTIOUS COMPLICATIONS: A SINGLE-CENTER COHORT STUDY
1Saitama Children’s Medical Center, Saitama, Japan
Introduction
Although few patients require a prolonged length of stay (PLS) in the pediatric intensive care unit (PICU), these patients account for considerable numbers of ICU bed days. In PICU settings, PLS is considered a critical issue because the affected children face higher risks of comorbidities, mortality, and a poor quality of life and consume substantial patient care and financial resources. Therefore, it is imperative to balance the needs of patients in this population with available resources to optimize the efficiency and quality of critical care. However, few has been studied.
Objectives
This study aimed to describe the prevalence, characteristics, resource consumption, and complications of long-stay patients in a PICU.
Methods
This was a single-center retrospective, descriptive cohort analysis of 1309 patients admitted to the PICU from January to December 2017. The main outcome was the ICU length of stay, and patients were divided into PLS and non-PLS groups if they had a length of stay of ≥28 or <28 days, respectively. Univariate analyses were conducted to characterize PLS.
Results
Thirty-two (2.4%) patients had a PLS and utilized 33% of PICU bed days. Factors associated with PLS included a young age (neonate, p < 0.001 and infants, p = 0.04), admission for respiratory (p = 0.003) or cardiovascular dysfunction (p < 0.001), post-cardiac operation (p = 0.003) or post-cardiopulmonary arrest (p = 0.01), and transfer from another facility (p = 0.001). PLS patients more frequently developed nosocomial infections and disproportionately received monitoring and therapeutic resources.
51
ULTRASOUND MEASURED LEAN QUADRICEP MUSCLE THICKNESS FOR ASSESSMENT OF NUTRITION IN CRITICALLY ILL: A PROSPECTIVE OBSERVATIONAL STUDY
1Sanjay Gandhi Post Graduate Institute Of Medical Sciences, Lucknow, India
Introduction
Nutritional assessment in critically ill ICU patients is challenging.
Methods
Prospective observational study was conducted in a mixed adult ICU. Patients 18 years age and admitted more than 24 hours in ICU were studied. Bilateral LQMT, using POCUS multi-frequency linear transducer probe was measured within 48 hours of ICU admission, and then serially on days- 4, 7, 14, 28. NUTRIC score, calorie deficit, nitrogen balance and mortality were also recorded.
Results
Ninety two (M/F: 55/37) patients with mean age of 50 years and predominantly medical illness (87/92, 94.6%) were studied. 80.4% (74/92) had two or more organ failures. 42.4% (39/92) died. LQMT changes showed a decreasing trend with length of ICU stay, at a lesser rate among survivors (Ss) compared to non-survivors (NSs) [0.99 ± 0.25%/day in Ss vs 1.49 ± 0.42%/day in NSs, p, <0.001]. The calorie & nitrogen deficit were higher in NSs on all days. However, it differed significantly only on the first day [(−745 ± 293 Kcal in NSs vs. −506 ± 345 Kcal in Ss; p, 0.001) & (−5.96 ± 3.45 in NSs vs. −2.46 ± 3.32 in Ss; p, 0.003)]. Higher proportion of patients with positive nitrogen balance survived (p, <0.001). Patients with NUTRIC score ≥5 had a proportionally greater decrease in LQMT (1.31 vs. 1.13%/day with NUTRIC score < 5; p, 0.04). LQMT change had a good overall accuracy to predict mortality [AUC, 0.82 (95%CI, 0.73–0.91); p, <0.001].
55
PATTERN OF ANALGESIC USE IN A RESOURCE LIMITED ICU IN NORTHERN NIGERIA
1Department Of Anaesthesia, Abu Teaching Hospital, Shika-zaria, Nigeria, Kaduna, Nigeria
Introduction
Moderate to severe pain is common in the intensive care unit (ICU). Origin of pain varies from post-traumatic causes, acute post-operative pain, ICU procedure related sources and pain from diseases among others. Inadequate pain treatment has been shown to cause prolonged stay in the ICU, produce distress, anxiety and sleep disturbance. Systemic opioids and other components of multimodal analgesic techniques are being used to improve pain management in the ICU.
Methods
Study was an audit of all ICU admissions that occurred over a 12-month period from July 2016-June 2017 in a tertiary hospital in Zaria, Nigeria. Data on age, sex, indication for admission (medical/surgical) and types of analgesics were retrieved and analyzed using SPSS version 21. Continuous data were summarized as mean ± standard deviations while qualitative data were summarized as proportions. Fisher’s Exact Test (FET) was computed. Level of significance was set at p≤0.05.
Results
There were 98 admissions out of whom 94(95.9%) received analgesics. Females constituted 42(44.7%). The mean age was 35.4 ± 18.4years. Most of the admissions were surgical 86(91.5%). Paracetamol, diclofenac, pentazocine and tramadol were used in 20(21.3%), 15(16%), 54(57.4%), and 2(2.1%) patients while pethidine and morphine were administered in 1(1.1%) and 2(2.1%) patients respectively. There was no statistical relationship between types of analgesics used and indication for admission (medical/surgical) p = 0.422 (FET).
60
MEASUREMENT OF CITRATE CONCENTRATION IN HUMAN BIOFLUIDS USING ULTRAVIOLET SPECTROPHOTOMETRY: MODIFICATION OF A COMMERCIAL TWO-STEP ENZYMATIC KIT
1Sunshine Coast University Hospital, Nambour, Australia
Introduction
The use of citrate as an anticoagulant during renal replacement therapy is increasing and the ability to measure its simultaneous concentration in both blood and ultrafiltrate would assist with the management of the dialysis regimen.
Methods
Vertical path length was determined ratiometrically. Next, to test the assay sensitivity to plasma proteins, samples of plasma with added citrate were prepared. One sample was centrifuged and microfiltered to remove molecules under 10kDa while the other was not. Throughout, citrate concentration was determined in duplicate using the test procedure. Sample colour sensitivity due to protein content was tested separately by filtering the plasma prior to addition of the citrate. Difference in citrate concentration between the two samples was measured. Last, accuracy and linearity of the method was tested by constructing a standard curve using pH-adjusted solutions of sodium citrate.
Results
Pathlength was 4.39mm giving a final total sample volume of 150µl with a plasma sample volume of 15µl or an ultrafiltrate sample volume of 4µl. Neither protein content nor sample colour had any significant effect. Data for the standard curve obeyed the Beer-Lambert Law and there were no significant differences between measured and calculated concentrations. At all dilutions, the absorbance difference between the two steps of the enzymatic method (ΔA) was always well above the lower limit of discrimination for the kit (ΔA > 0.005).
61
PLASMA CITRATE CONCENTRATION AND ITS CORRELATION WITH TOTAL TO IONISED CALCIUM RATIO IN PATIENTS RECEIVING RCA DURING CVVHDF
1Sunshine Coast University Hospital, Nambour, Australia
Introduction
Continuous veno-venous haemodiafiltration (CVVHDF) with regional citrate anticoagulation (RCA) is now commonly used to treat acute kidney failure in the ICU with citrate toxicity primarily assessed using the total to ionised calcium ratio (CR).
Methods
After meeting inclusion criteria, blood was sampled from twenty patients before, during and after episodes of filtration. Using spectrophotometry, samples were tested for citrate concentration. Demographic and other clinical and biochemical data were also collected. Throughout, a 15mmol/l solution of trisodium citrate was used as the prefilter anticoagulant. Results were analysed using STATA (v15.0) and presented as mean (SD), median [IQR] or simple proportion. Comparisons were made using either the Student t-test or the Wilcoxon rank-sum test. Correlation was assessed using Pearson’s r.
Results
Twenty patients (17 males) were enrolled in the study. Mean age was 63.7years (9.9). Median ICU length of stay was 281hours [199, 422] with 85% undergoing IPPV. Median APACHE 3 score was 95 [87, 117] with a 30% mortality rate. Median filtration time was 85hours [46, 149]. No difference was found between pre and post filtration plasma citrate concentrations (79µmol/l (50) vs 71µmol/l (42), p = 0.65). Mean citrate concentration during filtration was 508µmol/l (221) with a maximum of 1070µmol/l. This was significantly higher than the pre/post levels (p < 0.001). Mean calcium ratio was 1.88 (0.27) with several values > 2.10. There was poor correlation between plasma citrate concentration and calcium ratio (r = +0.32).
65
CLINICALLY SIGNIFICANT PLEURAL EFFUSIONS IN INTENSIVE CARE: A MULTICENTRE, PROSPECTIVE EVALUATION OF THE RISKS AND BENEFITS OF EARLY DRAINAGE
1St John of God Midland Public and Private Hospital, Midland, Australia
2Royal Perth Hospital, Perth, Australia
3Fiona Stanley Hospital, Murdoch, Australia
4Sir Charles Gairdner Hospital, Nedlnads, Australia
Introduction
Pleural effusions affect 62% of patients in intensive care. The prevalence and optimal management of clinically significant pleural effusion in the critically ill is unknown. Pleural drainage can improve respiratory mechanics and diagnostic accuracy, but may result in complications. The alternative, expectant medical management without drainage, may delay treatment optimisation. No prior studies have compared drainage with expectant management.
Methods
Consecutive patients with clinically significant pleural effusions (depth ≥2cm and significantly affecting patient-care according to treating intensivist) who underwent drainage or expectant management in four ICUs over 28 months were recruited. Primary outcome was the change in PaO2 to FiO2 (P:F in mmHg) ratio within 24 hours. Changes in diagnosis and treatment whilst in intensive care, as well as pleural effusion related serious adverse events (PERSAEs) up to 90 days were recorded.
Results
Of the 7342 patients screened, 300 clinically significant pleural effusions were diagnosed in 226 patients (3.1%); 76 patients had early drainage within 24 hours of enrolment and 150 did not. Drainage of effusion significantly improved oxygenation (P:F ratio: 203 (148 to 285) at baseline vs 263 (217 to 352) at 24 hours, 29.6% increment from baseline; p < 0.01) compared to without drainage (P:F ratio: 250 (176 to 325) at baseline vs 268 (190 to 323) at 24 hours, 7.2% increment from baseline; p = 0.44). Improvements in diagnosis were noted in 91 initial (non-repetitive) drainages (76.5% out of 119); treatment strategy was optimised in 80 drainage episodes (59.7% out of 134). PERSAEs were not different between the two groups (drainage: 10.5% vs non-drainage: 16.0%, p = 0.32).
68
EARLY INTENSIVE REHABILITATION DOES NOT AFFECT RESPIRATORY OR HAEMODYNAMIC PARAMETERS IN PATIENTS REQUIRING EXTRACORPOREAL MEMBRANE OXYGENATION
1Physiotherapy Department Alfred Hospital, Melbourne, Australia
2Discipline of Physiotherapy La Trobe University, Melbourne, Australia
3Intensive Care Department Alfred Hospital, Melbourne, Australia
4Australian and New Zealand Intensive Care Research Centre, Department of Epidemiology and Preventive Medicine Monash University, Melbourne, Australia
Introduction
The number of publications investigating rehabilitation of patients whilst on extracorporeal membrane oxygenation (ECMO) has increased over the past decade. Early rehabilitation in the intensive care unit (ICU) is recognised as safe and feasible in other ICU populations, but little is known about the respiratory and haemodynamic effects of rehabilitation in patients on ECMO.
Objective
The primary objective of this study was to describe the respiratory and haemodynamic effects of early intensive rehabilitation compared to standard care physiotherapy over a 7-day period in patients requiring ECMO.
Methods
Single-centre randomised controlled trial. Consecutive patients undergoing ECMO were recruited within 72 hours of ECMO commencement. These patients formed part of a larger multicentre randomised safety and feasibility trial evaluating early intensive rehabilitation versus standard care physiotherapy in patients on ECMO (NCT03328767). Respiratory and haemodynamic parameters, along with ECMO settings, were recorded 30 minutes pre and post each session, and continuously during the session (minimum and maximum values). In addition, the minimum and maximum values for these parameters were recorded outside of the rehabilitation or standard care sessions for each 24-hour period over the 7 days. The number of minutes of exercise was recorded per session.
Results
Fifteen patients (age 51.5 ± 14.3 years, 80% male) received ECMO. The intensive rehabilitation group (n = 7) spent more time exercising per session than the standard care group (n = 8); mean 28.7 versus 4.2 minutes respectively, p < 0.0001. Three patients (43%) in the intensive rehabilitation group versus none in the standard care group mobilised out of bed during ECMO. There was no difference between the groups for any of the respiratory, haemodynamic or ECMO parameters. The minimum and maximum values for each parameter occurred outside of the rehabilitation or standard care sessions.
Conclusion
Early intensive rehabilitation of patients on ECMO does not affect acute physiological parameters.
71
RISK FACTORS AND OUTCOMES OF POST-TRAUMATIC ACUTE KIDNEY INJURY REQUIRING RENAL REPLACEMENT THERAPY: A MATCHED CASE-CONTROL STUDY
1All India Institute Of Medical Sciences, New Delhi, Delhi, India
Introduction
Acute kidney injury following severe trauma is common and an independent risk factor for increased morbidity and mortality. However, most patients with raised creatinine or decreased urine output following trauma recover well while a few require renal replacement therapy (RRT).
Methods
This retrospective case-control study was conducted on patients admitted to the Trauma ICU at a Level I trauma center admitted for at least 24 hours following severe trauma. The primary outcome measure was requirement of RRT. Univariate comparison and multiple logistic regression analyses were done to identify risk factors associated with requirement of RRT and mortality outcome.
Results
Presence of crush injury and elevated serum creatinine on arrival were identified to be independent risk factors for RRT requirement. Hypotension on presentation, pre AKI sepsis and exposure to nephrotoxic agents or radiocontrast exposure were not found to be associated with need for RRT. AKI requiring RRT resulted in significantly increased ICU length of stay (15 vs. 5 days, P < 0.001) and mortality (OR 12.1, 95% CI [3.84–38.17]; P < 0.001).
72
Preoperative High coronary artery calcium score may be associated with long-term Cardiovascular morbidity in patients who underwent living-donor liver transplantation
1Asan Medical Centre, Seoul, South Korea
Introduction
Coronary computed tomographic angiography (coronary CT) is a non-invasive test for diagnosis of cardiac function. Coronary calcium scores determined by coronary CT are associated with cardiovascular risk factors. However, no studies have investigated the association between coronary calcium scores and long-term cardiovascular complications within 5 years after living donor liver transplantation (LDLT).
Methods
Between 2008 and 2012, 628 LDLT recipients were analyzed retrospectively. Preoperative cardiovascular assessments, including coronary CT, were performed. A coronary calcium score > 400 was defined as a positive finding. Predictive factors of long-term cardiovascular complications were evaluated by univariate and multivariate analyses. Major cardiovascular complications were evaluated up to 5 years after LDLT.
Results
Of the 628 patients, 48 patients (7.6%) experienced one or more major cardiovascular complications. Positive coronary CT findings were seen in 26 patients (4.1%). In the multivariate analysis, a coronary calcium score > 400 [odds ratio (OR) = 4.045, 95% confidence interval (95% CI): 1.519–10.771, P = 0.005], age (OR = 1.062, 95% CI: 1.011–1.115, P = 0.016), Diabetes mellitus (OR = 2.739, 95% CI: 1.424–5.628, P = 0.003), Creatinine (OR = 1.201, 95% CI: 1.001–1.003, P = 0.049), and brain natriuretic peptide (OR = 1.002, 95% CI: 1.001–1.462, P = 0.049) were associated with long-term cardiovascular complications.
73
DEMAND ON ICU BEDS BY POST SURGICAL PATIENTS
1Sri Jayewardenepura General Hospital, Colombo, Sri Lanka
Introduction
Sri Lanka is a lower middle income country having 2.5 ICU beds per 100000 population. It has a total of 500 critical care beds with around 38000 admissions annually, with a high demand for beds.
Methods
The study was prospectively done at Sri Jayewardenepura General Hospital for a period of 220 days.
All post surgical patients admitted electively or as emergency from the operating theatre or the wards were analyzed. Procedures which routinely require ICU were not considered.
Results
This hospital has 1061 beds and the general multidisciplinary ICU with 10 beds caters for 897 beds. This is a ratio of 1.1%. The average occupancy was 92%. 75 post operative patients out of 383 total admissions accounted for 19% of the total. This accounted for 6.8% of the total bed hours.
40% were in the 60–80 age group and 19% in the over 80. ASA III and IV accounted for 56%. Pre operatively 45% had cardiovascular issues while 19% had diabetes 10% had CKD. The majority of admissions were following orthopedic surgery accounting for 36% while 27% were abdominal surgery and 20% urology.
38% were admitted electively while 62% were due to problems occurring in the operating theatre or post operatively in the ward. The emergency problems were, 30% due to ischaemic events, 16% for respiratory events and 9% for excessive bleeding.
90% required interventions. 29% required inotropes, 19% ventilation, 21% blood transfusions, 15% invasive renal support.
There were (8%) deaths.
82
Cairns Sepsis Models (CSM-4 and CSM-24) – Improved prediction of adult sepsis mortality at ICU admission
1Cairns and Hinterland Hospital and Health Service, Queensland Health, Cairns, Australia
2Department of Public Health and Community Medicine, Institute of Medicine, The Sahlgrenska Academy, University of Gothenburg, Sweden
3Deputy State Medical Director, DonateLife
4Adjunct Senior Lecturer, James Cook University College of Medicine and Dentistry, Australia
5Associate Professor at Cairns Clinical School, James Cook University, Cairns, Australia and Department of Surgery, Cairns Hospital, Australia
6Adjunct Professor in General Practice, Research and Development Unit, Primary Health Care and Dental Care, Narhalsan, Southern Alvsborg County, Region Vastra Gotaland, Sweden
Introduction
Sepsis is a common presentation and
Methods
We performed a case-control study of 500 patients admitted to the Cairns Hospital ICU in Queensland, Australia between 2013–2017. Data was obtained from the Cairns ICU “metavison” database for patients that met our inclusion criteria of age ≥18 on ICU admission and a primary diagnosis of sepsis as per sepsis-3 definitions. 168 independent variables were then assessed against ICU episode mortality. We performed a multivariate backwards logistic stepwise regression to derive our own MPM which we assessed on discrimination, as measured by area-under-receiver-operator curve (AUROC), calibration as measured by the Hosmer-Lemeshow goodness-of-fit (HLGOF) and model fit with Nagelkerke R2 (NR2).
Results
The 4-hour Cairns Sepsis Model (CSM-4) contained 10 variables and had an AUROC of 0.90, NR2 of 0.51 and HLGOF of 0.081 with a specificity of 0.94 and NPV of 0.98. The 24-hour Cairns Sepsis Model (CSM-24) contained 7 variables and had an AUROC of 0.87, NR2 of 0.40 and HLGOF of 0.35 with a specificity of 0.91 and NPV of 0.97. Both CSM models outperformed existing MPM’s tested on our dataset. Both CSM models also performed similarly to the latest MPM’s in their derivation papers.
89
IMPACT OF CORRECTIVE AUDITING ON THE PREVALENCE OF VENTILATOR-ASSOCIATED PNEUMONIA
1Hospital Caxias Dor, Duque de Caxias, Brazil
Introduction
Ventilator
Methods
A study conducted with data collected prospectively from june 2013 to january 2019 with a total of 6428 patients included. The intervention was performed in September 2016, totaling 3361 patients before the intervention and 3076 patients after it. The utilization rate of mechanical ventilation, incidence of ventilator-associated pneumonia and mortality rate standardized BY the SAPS3 were compared.
Results
We observed before the intervention 55 events of pneumonia associated with mechanical ventilation. The utilization rate of mechanical ventilation was 32.46% with an incidence density in the period of 9.65. The mean SAPS3 of these patients reached 62.9 points with a probability of death of 42.8%. The standardized hospital mortality rate(observed/expected) was 1.4. After the intervention, 13 pneumonia events were observed. The utilization rate of mechanical ventilation observed was 30.25% with an incidence of 2.39. The mean SASPS3 score in this period was 76.2% with a standardized mortality rate(observed/expected) equal to 1.
96
FUNCTIONAL OUTCOME OF CHILDREN DISCHARGED FROM A PEDIATRIC INTENSIVE CARE UNIT – A COHORT STUDY
1JIPMER, Puducherry, India, Puducherry, India
Introduction
The focus on assessing the PICU outcome should be survival with good functional outcome. Currently there is a paucity of data especially from developing countries like India regarding the functional outcome of children discharged from PICU.
Methods
Over the study period of one year, all children were assessed at the time of PICU admission regarding their pre admission health status using mGOS questionnaire. Data regarding diagnosis and management was collected. Following discharge from the PICU, caregivers of the children were contacted after 6 months through telephone and the functional outcome was assessed using the study questionnaire.
Results
Out of 420 children enrolled, 384 (91.4%) could be contacted 6 months after discharge. The median age observed was 24 months. Infants (39.1%) constituted the majority. The primary organ system involved was respiratory in 23.2%, followed by CNS (13.8%), bites/poisoning (12.2%) and CVS (8.9%). The median duration of PICU stay was 5 days and the median PRISM score was 8. Hemodynamic instability and need for mechanical ventilation was observed in 26.4% and 25% of children respectively during the PICU stay. On follow up, 77% had favorable outcome. On multivariate analysis, only higher PRISM score during admission and unfavorable pre admission status were independently associated with poorer outcome.
104
PREDICTORS OF MAJOR ADVERSE KIDNEY EVENTS IN SURVIVORS OF ACUTE KIDNEY INJURY
1Austin Health, Richmond, Australia
Introduction
Acute kidney injury is a common complication of critical illness and survivors remain at heightened risk of chronic kidney disease, end-stage kidney disease and death.
Methods
We conducted a retrospective study of adult patients admitted with acute kidney injury between 1 January 2012 and 31 December 2016. Cox regression models were performed to examine the primary outcome, which was the development of a major adverse kidney event in the first year following hospital discharge. The secondary outcomes (chronic kidney disease, end-stage kidney disease, and death) were studied using Cox and competing risk regression models. Patients were followed for up to 12 months. Predictors included demographic, comorbidity, and laboratory variables available at the time of hospital discharge.
Results
Of 2,101 patients included in the study (mean age 69 years, 58% male, baseline estimated glomerular filtration rate 72 mL/min/1.73m2), 767 patients developed a major adverse kidney event within the first year. Major adverse kidney events occurred more frequently in patients who were older and in those with a history of chronic heart failure, liver disease, and either non-metastatic or metastatic malignancy. They were also more common in patients with a greater severity of acute kidney injury and in those with a higher serum creatinine level at discharge. Female sex and hypertension were additional risk factors for the development of chronic kidney disease and end-stage kidney disease.
106
RELATIONSHIP BETWEEN BETA-LACTAMS CONCENTRATIONS AND DEVELOPMENT OF RESISTANCE IN CRITICALLY ILL PATIENTS
1Erasme Hospital – Ulb, Brussels, Belgium
Introduction
Antimicrobial resistance is a worldwide problem. Multidrug resistant bacteria (MDR) are associated with high morbidity and mortality rates. Critically ill patients have altered pharmacokinetics of antibiotics and underdosing is frequent. This could lead to treatment failure and increased selection of MDR. We hypothesized that insufficient doses of beta-lactams would be associated with an increased risk of MDR acquisition.
Methods
Retrospective single-center cohort study including patients admitted to the ICU who were treated with a broad-spectrum beta-lactam and had a concomitant therapeutic drug monitoring (TDM). Patients were classified as having insufficient beta-lactam levels when their minimal drug concentrations were below 4 times the MIC of Pseudomonas aeruginosa as for EUCAST breakpoints. The development of bacterial resistance was based on available microbiological cultures from any site within 15 days from TDM; previous MDR carriage was not considered. A logistical regression analysis was performed to identify the variables independently associated with MDR acquisition.
Results
We studied 291 patients with a total of 704 TDM levels. Patients who presented with insufficient beta-lactam levels (n = 203, 69,8%) were less severely ill than patients with adequate serum levels [SOFA score 8 (4–11) vs. 10 (8–14), p = 0.001; APACHEII score 18 (13–18 vs 22(16–28), p = 0.001]. Ninety eight (33.7%) patients acquired a new resistant pathogen; the most common pathogens were: Pseudomonas aeruginosa [32 (32.6%)], Escherichia coli [17(17.3%)] and Staphylococcus aureus [15(15.3%)]. The acquisition of resistance [64(31.5%) vs. 34(39.1%); p = 0.23) and the number of days to resistance acquisition (12 days in both groups) were similar in patients with insufficient and adequate drug levels. The only independent factor associated with MDR acquisition was the use of renal replacement therapy (OR 1.93 CI 95% 1.12–3.33).
108
THE SUCCESSFUL DEVELOPMENT OF A MULTIDISCIPLINARY IN-SITU SIMUALTION PROGRAMME IN CARDIOTHORACIC INTENSIVE CARE
1Mater Hospital, Sydney, Australia
Introduction
The introduction of ICU In-Situ Simulation Club along with the development of easy to use emergency guidelines has drastically increased staff confidence and knowledge in managing emergences which occur in General and Cardiothoracic ICU.
Methods
The ICU in-situ Simulation program occurs every 2 weeks. The simulation scenarios are high fidelity, have specific learning objectives and run in real time with the use of emergency equipment and guidelines available in ICU. Members of the MDT work in their usual roles and expected ability.
After the scenario, time is taken to sit down with participants and observers for a formal debrief. Feedback forms are collected after each session.
Results
We have collated over 140 individual feedback forms and have shown that staff confidence at managing the emergency identified in the scenario increased from 6/10 before the simulation scenario to 8.5/10 after the simulation scenario. Confidence in locating vital emergency equipment increased from 7/10 to 9.5/10.
We are very proud to have increased staff engagement and confidence with simulation training from 6.5/10 to 9.5/10.
The ICU Simulation Program, nicknamed ‘SIM Club”, has been very successful. To quote a staff member (Registered Nurse) after a recent airway emergency- “I didn’t find that very stressful and I knew where everything you asked for was as it was just the same as SIM Club a couple of weeks ago”.
114
THE INCIDENCE, CLINICAL OUTCOMES, AND RISK FACTORS OF POST EXTUBATION DYSPHAGIA IN AN AUSTRALIAN REGIONAL CRITICAL CARE SETTING
1Bendigo Health, Bendigo, Australia
2Flinders University, Adelaide, Australia
3University of Melbourne, Melbourne, Australia
4University of Queensland, Brisbane, Australia
Introduction
Swallowing impairment after mechanical ventilation (known as post extubation dysphagia, PED) has been shown to increase rates of aspiration pneumonia and hospital length of stay. A recent meta-analysis demonstrated that 49% of all intubated patients present with PED.
Methods
Retrospective clinical coding data from the Victorian Admitted Episodes Database, identified the incidence, risk factors, and clinical outcomes for patients with PED over a 5-year period. Patients with a tracheostomy or pre-existing dysphagia were excluded. The data were linked to the Victorian Cost Data Collection records to identify cost per episode.
Results
822 patients were included, of which 7% (n = 58) developed PED. Despite traditional beliefs of prolonged endotracheal intubation increasing the risk of PED, 53% (n = 31) of cases occurred within less than 48hrs of ventilation. Patients with PED had a longer mean ICU length of stay (168.79 hours vs. 97.55 hours; p < 0.001). 21% (n = 12) of patients with PED developed a hospital acquired pneumonia. Average cost per episode (AUD$64,190) was double (51%) that of extubated patients without dysphagia. This represents an increase of AUD$32,776 per patient.
117
PERCEIVED DISCOMFORT IN CRITICALLY ILL PATIENTS BEFORE AND AFTER TRANSITIONING TO A NEW INTENSIVE CARE UNIT A PROSPECTIVE OBSERVATIONAL STUDY
1The St George Hospital NSW, Sydney, Australia
2University of New South Wales, Sydney, Australia
3The Canberra Hospital, Canberra, Australia
Introduction
Discomfort experienced by patients admitted to ICU is an important indicator of quality of care. Discomfort may be due to environmental factors.
Objectives
To compare discomfort perceived by patients admitted to an open plan ICU (cohort 1) with those admitted to a new ICU (all single rooms) (cohort 2). To identify factors that may reduce discomfort.
Methods
The study was conducted over 15 months (6 months in old ICU, 6 months in new ICU after a 3 month settling in period). All eligible patients (>18 years, GCS 15, off sedation, English speaking) were surveyed. A validated English version of the French discomfort questionnaire (IPREA) was used. Patients were asked to score discomfort caused by 16 items on a scale of 0 (no discomfort) to 100 (maximum discomfort). An overall discomfort score was computed as the mean score of the 16 item scores. The mean total discomfort score from the 2 cohorts were compared using unpaired t test or Wilcoxon rank sum test. Performance-Importance plots were plotted to identify important contributory items.
Results
A total of 317 patients were studied (168 patients in cohort 1, 149 patients in cohort 2). Overall response rate was 98.8%. The mean age was similar. The mean APACHE II was significantly higher in cohort 2 (15.5 ± 5.6 vs. 13.8 ± 5.6, P = 0.01). The mean total discomfort score was similar (18.4 ± 12.5 vs. 19.1 ± 12.8, P = 0.62). Compared to cohort 1, the median discomfort scores in cohort 2 for 8 of 16 items were higher. Noise and anxiety were less. Using Bonferroni correction for multiple testing, only discomfort from isolation [median(IQR): 1(1–2.5) vs. 4(1–22), P<0.0001] and absence of phone [median(IQR): 0(0–0) vs. 0(0–5), P = 0.0001] were significantly higher.
Conclusion
Transitioning to a new ICU did not reduce overall perceived discomfort. Discomfort from isolation was higher in the new ICU. Factors other than environmental factors influence discomfort in ICU patients.
119
BURNOUT, PROFESSIONAL QUALITY OF LIFE, AND WORPLACE STRESSORS IN INTENSIVISTS IN AUSTRALIA AND NEW ZEALAND
1Intensive Care Unit, Gold Coast University Hospital, Southport, Australia
2Faculty of Medicine, University of Queensland, Brisbane, Australia
3Paediatric Intensive Care Unit, Queensland Children’s Hospital, Brisbane, Australia
4Professional Activities and Welfare Committee, Australia and New Zealand Intensive Care Society
5Intensive Care Unit, St. Vincent’s Hospital, Sydney, Australia
6Department of Critical Care Medicine, Royal Hobart Hospital, Hobart, Australia
7Intensive Care Unit, The Townsville Hospital, Townsville, Australia
8Paediatric Critical Care Research Group, Queensland Children’s Hospital, Brisbane, Australia
9Department of Intensive Care, Austin Hospital, Melbourne, Australia
Introduction
Burnout is one of several interrelated concepts that influence doctor wellbeing. The health and wellbeing of doctors has a significant impact on the quality of the healthcare they provide. It has been proposed that burnout is one of the links between organisational culture and quality of care.
Methods
Australian and New Zealand (ANZ) intensivists were invited to participate in an online survey. The Professional Quality of Life scale, version 5 (ProQOL-5) was used to measure (1) compassion satisfaction, (2) burnout and (3) secondary traumatic stress. Several a priori defined socio-organisational factors designed to assess (1) interpersonal interactions and workplace relationships, (2) leadership and governance, and (3) self-determination and control, all of which have previously been associated with workplace stress and burnout, were also measured. Finally, we conducted thematic analysis on intensivists’ perspectives on workplace stressors.
Results
Very few participants (0.8%) demonstrated high scores (>75th centile) for burnout and 70.9% scored in the average range for burnout. 98.1% participants scored in the average to high range for compassion satisfaction. No association was found between gender, age, or years of practice with level of burnout or compassion satisfaction. Seven major themes for intensivists’ work stressors were: (1) interpersonal interactions and workplace relationships; (2) workload and its impact; (3) resources and capacity; (4) health systems leadership and bureaucracy; (5) end-of-life issues and moral distress; (6) clinical management; and (7) job security and future uncertainty.
121
APTA-1, A NOVEL RNA APTAMER, IMPROVES OUTCOME IN AN ANIMAL MODEL OF SEPSIS
1Medical Faculty, Uppsala University, Uppsala, Sweden
2Medical Faculty, Gothenburg University, Gothenburg, Sweden
3Aptahem Ltd, Malmoe, Sweden
Introduction
Sepsis/septic shock is one of the major causes of death worldwide. Sepsis/septic shock is frequently mimicked in animal models by injection of endotoxin, the toxic moiety, found in the cell wall of gram-negative bacteria.
A novel RNA aptamer, Apta-1, belonging to a class of fluorinated modified oligonucleotides, has anticoagulant properties. Aptamers have high affinity to specific target molecules and may act as antagonists of disease-associated proteins.
Objectives
To evaluate the potential effects of Apta-1 in an endotoxemic mouse model.
Methods
Sixty female C57BL/6 mice, weighing 19–23 g, where injected intraperitoneally with endotoxin (E. coli O111:B4) at 10 mg/kg. Groups of twenty mice were, after endotoxin challenge, 15 and 60 minutes later injected intravenously with saline, Apta-1 50mg/kg or Apta-1 100mg/kg, respectively.
The experiment was terminated 72h after the endotoxin injection. Another 5 mice served as non-endotoxemic controls. The study was approved by IACUC.
Results
Mortality was significantly reduced in both groups of Apta-1 treated endotoxemic mice compared to saline-injected endotoxemic mice. Median survival time for endotoxemic mice injected with Apta-1 at 50 mg/kg and 100 mg/kg, respectively were >71h, whereas median survival time for saline injected endotoxemic mice was 47h. Survival rates were 100%, 90% and 44%, respectively.
At 28h, TNF-alpha, IL-6 and IL-1beta were significantly lower in serum from both groups of Apta-1 treated endotoxemic mice, as compared to saline-injected endotoxemic mice. Similar significant findings were obtained for AST, ALT, creatine kinase and BUN.
Conclusions
Mice challenged with endotoxin, in order to replicate sepsis/septic shock, thereafter treated with Apta-1, a novel RNA aptamer exhibited lower mortality rate and decreased serum levels of proinflammatory cytokines. Furthermore, Apta-1 also reduced serum levels of several markers of organ damage. These results point towards the possibility that Apta-1 may turn out to be a drug candidate against human sepsis/septic shock.
122
GENOME WIDE EXPRESSION IN INFECTION AND SEPSIS: A PILOT PROSPECTIVE COHORT STUDY
1Department of Anaesthesia and Intensive Care, The Chinese University Of Hong Kong, Hong Kong, China
2Accident and Emergency Medicine Unit, The Chinese University Of Hong Kong, Hong Kong, China
Introduction
Sepsis affects an estimated 31.5 million people globally each year with mortality of up to 50%. Pathogenesis from infection to development of dysregulated host response and organ dysfunction in sepsis remains unclear.
Objectives
Determine the feasibility of using genome wide expression in peripheral blood mononuclear cells (PBMC) to study the differences between simple infection and sepsis.
Methods
We prospectively recruited 13 adults hospitalized for community acquired pneumonia. All patients had positive bacterial or viral pathogens. Blood samples for RNA sequencing were taken within 24 hours of admission. After sequencing, we normalized expression with log and quantile transformation. We used Wilcox test (p < 0.05) and 20th percentile of >15 transcripts per kilobase million as cutoffs for significant expression. The Boruta algorithm was used to find important differential gene expressions.
Results
After quality control, PBMC mRNA from 12 patients (6 with uncomplicated pneumonia, 6 with pneumonia related sepsis) were fully sequenced. The median sequential organ function assessment (SOFA) score (without respiratory component) of pneumonia patients with and without sepsis were 5 (range 2 to 10) vs 0 (range 0 to 1) (p = 0.002). We found 33 differentially expressed genes between patients with infection versus sepsis. Expression levels of 8 genes were correlated >0.85 (each with p < 0.0005) with SOFA score. NBR1, CARD16, DOCK8, RABGAP1L, APEX1, CD300A, PRKAG2, and SERPINB9 each have an AUC of ≥0.97 to differentiate infection and sepsis. These genes encode proteins involved in response to bacterial lipopolysaccharide, autophagy, immune signaling and cellular stress.
Conclusion
Our results show that PBMC genome wide expression can potentially be used to differentiate simple infection and sepsis. Expression levels of specific genes encoding proteins involved in inflammation are correlated with changes in organ function in sepsis. The results will inform larger prospective studies, with discovery and validation cohorts, using similar study protocols.
124
GOING HOME TO DIE FROM THE INTENSIVE CARE UNIT. EXPERIENCES FROM DENMARK
1Lillebaelt Hospital, Denmark, Kolding, Denmark
Introduction
Given the right help and assurance that they will have sufficient palliative care most elderly or sick people want to die in their own home, However, only 23% of Danes die at home and dying at the hospital, especially dying in the ICU is reported to be a stressful and anxious filled experience. Up to 90% of patients dying in the ICU die after withdrawal of treatment, potentially 20% of these could go home to die.
Methods
In 2013, the option of going home to die from the ICU was initiated. For the fully awake patient, where ongoing treatment was futile, the patient and the relatives were informed about the possibility to die at home. As the primary care team could not be there 24/7, It necessitated the family’s presence. The ICU took care of all practical arrangements, followed the patient home and were there to hand over the patient to primary care. Afterwards, the families were interviewed and asked to share their experiences and give insight about this experience. Pain treatment and relief of anxiety and breathing difficulties were addressed as main topics.
Results
From 2013–2019 we transferred 21 patients to their own home. The patients were from 59–87 years old, 45% were women, length of ICU stay was 1–103 days, and the patients died between a few hours up to four days after ICU discharge. Families found that it had been a very valuable experience and reported that the patients had received sufficient palliative care and died peacefully.
126
DEXMEDETOMIDINE REDUCES NORADRENALINE REQUIREMENTS AND PRESERVES RENAL MICROCIRCULATORY PERFUSION, OXYGENATION AND FUNCTION IN OVINE SEPTIC ACUTE KIDNEY INJURY
1Preclinical Critical Care Unit, Florey Institute of Neuroscience and Mental Health, University of Melbourne, Victoria, Australia, Melbourne, Australia
2Cardiovascular Disease Program, Biomedicine Discovery Institute and Department of Physiology, Monash University, Clayton, Australia
3Centre of Integrated Critical Care, School of Medicine, University of Melbourne, Melbourne, Australia
Introduction
Noradrenaline remains the primary vasopressor used to restore mean arterial blood pressure (MAP) in patients with sepsis. However, restoration of blood pressure with noradrenaline can worsen underlying renal medullary hypoperfusion and hypoxia in experimental gram-negative hyperdynamic sepsis associated with acute kidney injury (AKI).
Methods
Sheep were instrumented with pulmonary and renal artery flow probes, and laser Doppler and oxygen-sensing probes in the renal cortex and medulla. Conscious sheep received an infusion of live Escherichia coli for 30 h. Sheep were randomized to receive either noradrenaline or noradrenaline with dexmedetomidine or dexmedetomidine alone or vehicle-saline from 24–30 h of sepsis (all N = 8).
Results
Sepsis reduced MAP (84 ± 3 to 67 ± 4 mmHg), renal medullary perfusion (1250 ± 256 to 730 ± 176 perfusion units), medullary tissue oxygenation (40 ± 6 to 21 ± 6 mmHg) and creatinine clearance (2.50 ± 1.10 to 0.78 ± 0.40 mL/Kg/min) (P < 0.01). Noradrenaline restored baseline MAP (to 83 ± 6 mmHg) but worsened medullary hypoperfusion (to 330 ± 150 perfusion units) and medullary hypoxia (to 9 ± 5 mmHg). Dexmedetomidine (0.5 µg/kg/h) co-administration reduced the noradrenaline dose (0.8 to 0.4 µg/kg/min; P < 0.001) required to restore baseline MAP, attenuated medullary hypoperfusion (to 606 ± 300 perfusion units; P = 0.001), decreased medullary tissue hypoxia (to 29 ± 7 mmHg; P = 0.001), and progressively increased creatinine clearance (to 1.8 ± 0.4 mL/Kg/min; P < 0.001). Compared with vehicle time-control, dexmedetomidine given alone prevented the temporal reduction in MAP (P = 0.004) but had no significant effects on medullary perfusion and oxygenation or creatinine clearance.
137
UTILISATION OF A DATATHON TO EXPLORE DYSPHAGIA POST INVASIVE MECHANICAL VENTILATION
1Bendigo Health, Bendigo, Australia
2Department of Health and Human Services, Melbourne, Australia
3Monash University, Bendigo, Australia
4Monash Health, Melbourne, Australia
Introduction
A datathon is an event designed to bring researchers, clinicians, and data scientist together. Machine learning enables exploratory data analysis and hypothesis generation for clinically relevant questions in a collaborative environment. At present, it is unclear which patients are at greatest risk of dysphagia post invasive mechanical ventilation in an Australian population. A recent international meta-analysis demonstrated that 49% of all intubated patients present with dysphagia.
Methods
This pilot study occurred at a regional critical care datathon. The data have been extracted from the Victorian Admitted Episodes Database, using minimal data entry fields and ICD 10–AM codes. All results presented are preliminary findings based on trend analysis.
Results
In 2017 across Victoria, 15,033 patients underwent invasive mechanical ventilation. Of these 1,221 (8%) were identified as dysphagic. Incidence of dysphagia was noted to increase with length of ventilation, however plateaued at 24% after 4 days. 18% of patients with dysphagia were ventilated for less than 48 hours. Patients with delirium were more likely to present with dysphagia (23.5% vs. 5.5%). Based on data visualisation age did not appear to increase the risk of dysphagia until 70+ years.
138
DISCHARGE DELAY FROM INTENSIVE CARE UNITS IS ASSOCIATED WITH BETTER PATIENT OUTCOMES
1Flinders Medical Centre, Adelaide, Australia
2Women’s and Children’s Hospital, Adelaide, Australia
3Monash University, Melbourne, Australia
4Alfred Hospital, Melbourne, Australia
Introduction
Discharge delay is common in Australian and New Zealand intensive care units (ICU). The effects of these delays on patient related outcomes is unclear.
Methods
Data were accessed from the Australian and New Zealand Intensive Care Society (ANZICS) Adult Patient Database on all patients discharged alive from an ICU to a ward at contributing hospitals between 2010–2018 and in whom ‘time ready to leave ICU’ was recorded. Logistic regression was used to examine the association between discharge delay and mortality or readmission. Patients were further stratified and analysed by categories of mortality risk at ICU admission.
Results
919,289 patients from 186 hospitals were examined. Mean age was 61.8 (±17.9) years. Most patients were in tertiary hospitals (38.5%). Mean Apache II score was 14.6 (±6.8). 693,638 (75%) of patients were discharged within 6 hours, with 119,938 (13%) discharged in the next 6 hours. 15,927 (2%) of patients were delayed 48–72 hours. 29,201 (3.2%) died and 41,610 (4.5%) patients were readmitted to ICU. Risk adjusted mortality declined with increasing discharge delay and was lowest at 48–72 hours (OR 0.84, 95% CI 0.76–0.92). This effect was greatest in the sickest cohort of patients (OR 0.74, 95% CI 0.67–0.81) at 48–72 hours of discharge delay. Similarly, readmission risk was lowest at 48–72 hours of discharge delay (OR 0.75, 95% CI 0.70–0.82).
Conclusions
Adjusted hospital mortality declines with increasing discharge delay in ICU, particularly for the sickest cohort of patients. Further studies should evaluate potential causes for this. Consideration should be given to delaying the discharge of patients who have a high risk of death on initial ICU admission.
140
LOST IN RELOCATION: LESS THAN OPTIMAL MEDICAL HANDOVER OF PATIENTS DISCHARGED FROM INTENSIVE CARE
1Royal Adelaide Hospital Intensive Care Unit, Adelaide, Australia
2The University of Adelaide, Adelaide, Australia
Introduction
Poor quality communication and lack of standardized handover practices contribute to adverse patient events. Intensive care organisations recommend standardized, structured written and verbal handover. Large, complex health services with ever-changing workforces provide challenges to the process of handover of patients discharged from the Intensive Care Unit (ICU) to the ward.
Objectives
Investigate the effectiveness of ICU verbal and written patient handover at ward discharge.
Methods
Surveys were undertaken amongst ICU and ward-based doctors at a large, adult, university affiliated, Australian tertiary hospital. Survey 1 was completed verbally with a ward doctor, assessing the handover received for a specific patient discharged from ICU on the previous day. Invitations to online surveys ascertaining opinions of, and preferences for, handover processes were sent to ward (Survey 2) and ICU (Survey 3) doctors.
Results
Of 40 ward doctors completing Survey 1, 28 (70%) had received no verbal or written handover. Verbal handover was received in 5 (13%) discharges. Eighty-seven ward doctors completed Survey 2; 39 (45%) were unaware of the existing written discharge summary and 66 (76%) would prefer both written and verbal handover. Fifty-eight (67%) were unaware of how to contact the ICU doctor who discharged their patient. Of 39 ICU doctors completing Survey 3, 30 (77%) were unaware of the hospital’s verbal handover policy at ICU discharge and 38 (97%) believed verbal handover would be useful. However, 36 (92%) reported difficulties contacting the ward team as a barrier to effective handover. Handover quality was rated poor by 38 (44%) ward doctors and 14 (36%) ICU doctors.
Conclusions
Despite a preference for verbal handover of patients discharged from the ICU to the ward, this is often not achieved. Barriers such as education of handover policies and ease with which doctors are identified, and communicated with, can impede verbal and written handover procedures.
144
INFLUENCE OF BALANCE BETWEEN CALORIE AND PROTEIN INTAKES ON PHYSICAL OUTCOME IN CRITICALLY ILL PATIENTS
1Kochi Medical School, Nankoku, Japan
Introduction
Nutritional therapy is an important management tool in an intensive care unit (ICU). Recently, timing of calories and protein administration has received a lot of attention. However, an optimal balance between calorie and protein regarding physical outcome remains unclear.
Methods
This is a post-hoc analysis of a previous observational study. The study population comprised consecutive patients in 13 hospitals who were in the ICU for > 6 days with mechanical ventilation for at least 24 hours and no oral intake. The primary outcome was physical status at ICU discharge. We defined good physical status as more than end sitting (Good group) and poor physical status as bed rest and sitting (Poor group). We evaluated nitrogen/non-protein calorie (N/NPC) ratio as balance between calorie and protein, and compared N/NPC ratio on days 3 and 7 and at ICU discharge between both groups. Data were expressed as median [interquartile range].
Results
In total, 158 patients were included. The physical status of 60 and 98 patients was good and poor, respectively. The caloric and protein intakes on day 3 were significantly higher in the Poor group than in the Good group (10.8 [6.0, 17.2] vs 5.1 [2.4, 9.8] kcal/kg/day, p < 0.001; 0.5 [0.3, 0.8] vs 0.4 [0.2, 0.7] g/kg/day, p = 0.03, respectively). The protein intake on day 7 was significantly higher in the Poor group than in the Good group (0.7 [0.5, 1.0] vs 0.5 [0.3, 0.9] g/kg/day, p = 0.01). The caloric and protein intakes at ICU discharge in both groups were similar. The N/NPC ratio on days 3, 7, and at ICU discharge in both groups were similar.
146
CORRELATION OF CENTRAL CATHETER THROMBOSIS WITH INSERTION SITE IN ADULT TRAUMA INTENSIVE CARE UNITS
1Shiraz University Of Medical Sciences, Shiraz, Iran
2Anesthesiology and Critical Care Research Center, Shiraz University of Medical Sciences, Shiraz, Iran, Shiraz, Iran
3Medical imaging research center, department of radiology, Shiraz university of medical sciences, Shiraz, Iran, Shiraz, Iran
Introduction
Among central catheter-related complications, thrombosis is a common issue especially in trauma patients.
Methods
As a cohort observational follow up survey, using color doppler ultrasonography, 82 adult patients with central venous catheter were evaluated for the existence of catheter related thrombosis (CRT) at four time points (1st, 3rd, 7th and 14th day after insertion of catheter) . Demographic data, site of catheter insertion, history of smoking, aspirin and anti-coagulant consumption, among other factors, were recorded simultaneously.
Results
Nine patients (10.9%) developed CRT during the course of study, eight in internal jugular and one in femoral vein . There was no sonographic evidence of thrombosis in any patient with subclavian catheter. The use of aspirin, subclavian site of insertion, and previous smoking were associated with reduced CRT incidence. In contrast, internal Jugular catheter and catheterization time over 7 days, were associated with an increased CRT incidence. Heparin and enoxaparin had no effect on CRT.
150
LEAN TOOLS IMPROVING INTENSIVE CARE PROCESSES: USING A3 IN BRAZILIAN ICUs
1Imed Group Brasil, Sao Paulo, Brazil
Introduction
During the last two decades health care sector is progressively using concepts born in the industrial sector to reorganize production processes, to enhance the efficiency and the performance of services and organizations. Some of these changes are based on the fundamentals of the Toyota Production System (TPS) and focus on eliminate waste, generate value and continuous improvement. This approach is conventionally called “Lean”. The intensive care unit is a complex system suitable for frequent actions of development. There are no standards of care that cannot be driven to a better level. A3 is a powerful and comprehensive tool to address complex problems and reach improvement in many instances.
Methods
Problem 1: Increase the discharge rate at 10 am from ICU to hospital bed to 70% (previously 55%) Countermeasures: Distribute the morning work of the clerks in order to prioritize the discharges of the unity . Create specific function at the close of the care transfer document, completed by the doctor, that directly signals the "discharge" of the ICU patient.
Problem 2: Achieve catheter related bloodstram infection rate reduction of 30% in 6 months.
Countermeasures: Review the service level agreement with the hemodynamics team to modify the preferential access of transvenous pacemaker insertion through the femoral to jugular. Review of the process of care of the hemodialysis team using as a reference the intensive care unit’s standard catheter care.
Results
Problem 1: Discharge rate went up to 80% in 4 months and stayed that way since then. Problem 2: bloodstram infection rate decreased by 40% in 6 months and is still going down.
151
DEVELOPMENT OF A CLINICAL PRACTICE GUIDELINE FOR THE PHYSIOTHERAPY MANAGEMENT OF INVASIVELY VENTILATED ADULTS WITH COMMUNITY ACQUIRED PNEUMONIA
1The University of Notre Dame Australia, Fremantle, Australia
2Fiona Stanley Hospital, Perth, Australia
3Curtin University, Perth, Australia
Introduction
Community-acquired pneumonia is a common cause for ICU admission requiring invasive ventilation. Physiotherapists working in ICU are involved in the respiratory care of these patients during the intubated period, however there is clinical variability regarding mode and dosage of intervention, and evidence to guide what should be best practice is limited.
Methods
A program of mixed-methods research was conducted. This involved a national survey of clinical practice and systematic literature review to inform development of a series of expert consensus statements using an e-Delphi method. These expert consensus statements were then peer-reviewed by multidisciplinary clinical stakeholders for validity and applicability within the ICU setting. Modification of the consensus statements by clinical stakeholders was undertaken where necessary to facilitate clinical application. Final recommendations were synthesized into draft guidelines using the JBI approach for guideline development.
Results
A total of 34 recommendations for physiotherapy practice were developed. There were 26 strong recommendations (76%) addressing six domains of assessment (n = 13), selection and prioritization (n = 4), positioning (n = 3), hyperinflation (n = 3), normal saline instillation (n = 1), and active treatment and mobilization (n = 2). Eight conditional recommendations (24%) were made across four domains of positioning (n = 2), manual chest wall techniques (n = 4), normal saline instillation (n = 1), and active treatment and mobilization (n = 1). Conditional recommendations were made for areas of practice where there is limited or conflicting empirical evidence, lack of expert concurrence and/or variation in clinician values and preferences, such as with use of head down tilt positioning and saline instillation. Clinical stakeholders concurred that patient safety, interprofessional communication and culture were integral to effective practice and should form an overarching preamble to the guideline.
Conclusion
A draft guideline was developed for trial in Australian ICUs. Further stakeholder feedback from patients and staff is now required.
152
INCIDENCE OF ANTITHROMBIN DEFICIENCY AND ANTI-CARDIOLIPIN ANTIBODIES AFTER SEVERE TRAUMATIC BRAIN INJURY: A PROSPECTIVE PILOT STUDY
1Department of Intensive Care Medicine, Royal Perth Hospital, Perth, Australia
Introduction
Animal studies suggested that traumatic brain injury (TBI) can damage cerebral mitochondria, and release mitochondrial cardiolipin phospholipid into the systemic circulation, inducing a prothrombotic state through platelet activation.
Objectives
To determine the incidence of detectable anti-cardiolipin antibodies after severe TBI, and whether this was related to abnormal coagulation parameters within 7 days of TBI.
Methods
Serial anti-cardiolipin antibodies, anti-thrombin levels and viscoelastic testing were measured on admission, day-1, and between day-5 and day-7 in patients with severe TBI requiring intracranial pressure monitoring.
Results
Of the 37 patients (87% male and median age: 42 years-old) included in the study, 6 patients (16.2%) had a newly developed Ig-G or Ig-M anti-cardiolipin antibody titer after TBI. Anti-thrombin levels were below the normal level — especially on day-0 and day-1 — in 15 patients (40.5%), and 14 patients (37.8%) developed a prothrombotic state due to an elevation in fibrinogen concentration and platelet count according to the viscoelastic test. Anti-thrombin levels and the maximum clot firmness both increased significantly over the first 7 days after severe TBI (both p < 0.001). Four patients (10.8%) developed deep vein thrombosis and nine patients (24.3%) died, both of which and also the highest intracranial pressure within the first 24-hours after TBI were not statistically significantly related to development of anti-cardiolipin antibodies (p = 0.619, p = 0.638 and p = 0.491, respectively).
Conclusions
A prothrombotic state after severe TBI involves multiple mechanisms at different phases; suppression of antithrombin production and release of cerebral cardiolipin phospholipids are common initially followed by an elevation of fibrinogen and platelet count. A larger clinical study is needed to confirm the pathogenic relationships between severity of TBI, mitochondrial cardiolipin release from the brain, and development of thromboembolism.
159
FACTORS ASSOCIATED WITH SUCCESSFUL EARLY AND LATE TRACHEOSTOMY DECANNULATION
1Department of Speech Pathology, Austin Health, Heidelberg, Australia
2Tracheostomy Review and Management Service, Austin Health, Heidelberg, Australia
3Global Tracheostomy Collaborative, Boston, USA
4Department of Intensive Care, Austin Health, Heidelberg, Australia
5Department of Respiratory and Sleep Medicine, Austin Health, Heidelberg, Australia
Introduction
Factors associated with successful early and late tracheostomy decannulation in adults have not yet been definitively established in the literature. Identification of these factors would enable health care professionals to inform patients of the likely course of care, enable appropriate resource allocation and follow up care using best available evidence, and ascertain targets for intervention.
Methods
Retrospective descriptive observational cohort study using data extracted from the Global Tracheostomy Collaborative database and the medical record of 120 patients who had their tracheostomy inserted and were decannulated at Austin Health between August 2015 – July 2017. Twenty parameters were examined using Cox Proportional Hazards Model analysis and Kaplan-Meier survival analysis to determine an association between the variables and time to decannulation. Statistically significant variables were then analysed with univariate logistic regression.
Results
Five factors were associated with early decannulation. Tracheostomy insertion due to a loss of upper airway indicated a high likelihood of early successful decannulation. Two or more medical complications, duration of intubation over twelve days, duration of invasive mechanical ventilation via the tracheostomy over fifteen days and duration of ICU admission over twenty days indicated a low likelihood of early decannulation. Seven factors were associated with a high likelihood of late decannulation including an ICU admission over thirty-one days, two or more medical complications, an abdominal/GIT-related admission, major surgery, intubation for more than twelve days, invasive mechanical ventilation via the tracheostomy for more than twenty-four days and having a tracheostomy-related adverse event.
Conclusion
This project suggests that individuals requiring tracheostomy for loss of upper airway can be targeted for early decannulation, while those with prolonged ventilatory support needs and major abdominal surgery require acute care and resource allocation for prolonged periods. Tracheostomy adverse events were related to a high risk of late decannulation, offering a potential intervention target.
162
PREDICTIVE VALIDITY OF A QT PROLONGATION RISK SCORE IN A MEDICAL INTENSIVE CARE UNIT
1Surrey Memorial Hospital, Surrey, Canada
2Monash University, Parkville, Australia
3Royal Columbian Hospital, New Westminster, Canada
Introduction
Torsades de pointes (TdP) is a polymorphic ventricular tachycardia associated with QT interval prolongation. With approximately 24–61% of critically ill patients experiencing QT prolongation, a QT prolongation predictive tool to identify high risk patients could assist in monitoring and management in the intensive care unit (ICU). The Tisdale et al. Risk Score (TRS) is one such tool; developed and validated in a cardiac critical care unit.
Methods
This was a retrospective, cohort study of consecutive patients who met the inclusion criteria from 1st October 2017 until a sample size of 264 patients was achieved. Baseline characteristics and risk factors based on the TRS were collected. First occurrence of QTc interval >500ms or >60ms above baseline was recorded. Sensitivity, specificity, and likelihood ratios were calculated.
Results
Of the 264 patients enrolled, 88 patients and 3 patients in the moderate-high and low risk categories experienced QT prolongation, respectively. No QT prolongation was experienced in 145 moderate-high risk patients and 28 low risk patients. The sensitivity and specificity of the TRS for low risk patients against the moderate-high risk patients was 97% (95% CI 91–99%) and 16% (95% CI 11–23%), respectively. This corresponded to a positive likelihood ratio of 1.15 (95% CI 1.07–1.24) and a negative likelihood ratio of 0.20 (95% CI 0.06–0.65). A post-hoc multivariate logistic regression identified baseline QTc interval >450ms, use of ≥2 QT prolonging medications and sepsis as independent predictors of QT prolongation.
163
ANTIMICROBIAL DOSING IN CRITICALLY ILL PATIENTS REQUIRING CONTINUOUS RENAL REPLACEMENT THERAPY
1Surrey Memorial Hospital, Surrey, Canada
2Monash University, Parkville, Australia
3University of British Columbia, Vancouver, Canada
Introduction
Acute kidney injury (AKI) requiring continuous renal replacement therapy (CRRT) is common in patients with septic shock. Early, appropriate antimicrobial therapy can decrease mortality in septic patients. Clinicians may reduce the dose of antimicrobials in response to the AKI or during CRRT; however, this may not be necessary.
Methods
This is a retrospective chart review of eligible patients admitted to a tertiary care medical-surgical ICU between October 2017 and September 2018. Included patients received CRRT for 24-hours or more and at least one antimicrobial requiring dose adjustment in renal impairment. Information on baseline characteristics, CRRT, antimicrobials and culture results were collected. Descriptive statistics were used to analyze the data.
Results
Seventy-four patients were included in the study. The mean age was 61.3 ± 15 years, with 67.6% being male. The mean APACHE II score was 28 ± 7 and sepsis/septic shock was the most frequent admitting diagnosis. Thirty-six patients (49%) in the cohort died during their hospitalization. CRRT was administered as continuous venovenous hemodiafiltration at a mean effluent rate of 32+/-2.6 mL/kg/hr. According to hospital standards, 31 (41.9%) patients received at least one under-dosed antimicrobial. When reviewing the most frequently prescribed antimicrobials, the percentage of patients under-dosed were as follows: 25% on piperacillin/tazobactam, 66.7% with a vancomycin loading doses, and 29.2% on The median number of doses administered below the hospital standard for piperacillin/tazobactam and meropenem were 1 (1–2) and 2 (1–3), respectively.
169
MANNITOL PLUS HYPERTONIC SALINE DOES NOT INCREASE RISK FOR ACUTE KIDNEY INJURY AFTER TRAUMATIC BRAIN INJURY
1University of Sydney School of Pharmacy, Sydney, Australia
2The Royal Prince Alfred Hospital, Sydney, Australia
3University of Sydney School of Nursing, Sydney, Australia
Introduction
Mannitol and hypertonic saline are treatment options for intracranial pressure reduction in patients with traumatic brain injury. It is unknown if patients who receive these hyperosmolar agents in combination during critical illness are at an increased risk for renal dysfunction.
Objectives
To compare the effect of mannitol plus hypertonic saline combination (MHS) versus hypertonic saline monotherapy (HS) on renal function in patients with traumatic brain injury.
Methods
This was a secondary analysis of data from the Resuscitation Outcomes Consortium (ROC) Hypertonic Saline Trial Shock Study and Traumatic Brain Injury Study, which were randomized controlled trials conducted in the United States. Patients with traumatic brain injury who received MHS were selected. Patients were matched using propensity scores to those who received HS alone. The primary outcome measure was the maximum serum creatinine value during critical illness. Secondary outcome measures were stage 2 or 3 acute kidney injury as defined by the Kidney Disease Improving Global Outcomes guidelines.
Results
After propensity score matching, the cohort consisted of 152 patients in each group (304 total). The overall sample had a mean age of 33 ± 15 years and 23% (n = 69) were female. The mean Injury Severity Score was 34 ± 11. The MHS and HS groups were balanced with regard to demographic and clinical characteristics. The maximum serum creatinine value reached was 82 ± 49 µmol/l in the MHS group and 80 ± 28 µmol/l in the HS group (p = 0.525). Stage 2 or 3 acute kidney injury occurred in 1.3% (n = 2) patients in the MHS group and 0.7% (n = 1) patients in HS group (p = 1.000).
Conclusion
The combination of mannitol with HS did not increase the risk of renal dysfunction compared to HS alone in patients with traumatic brain injury.
172
DETERMINING THE INCIDENCE OF DELIRIUM AND THE DETECTION OF RISK FACTORS USING CAM-ICU AND ICDSC
1Pamukkale university medicine faculty, Denizli, Turkey
Introduction
Delirium is one of the common situations in intensive care.
Methods
125 adult patients who were admitted into Pamukkale University hospital Intensive Care Unit, aged over 18 years, who had no communication problems, RASS scale -3 and above, and were in intensive care for at least 24 hours were included in the study. The ICDSC in the evening between 16:00 and 18:00 patients went through psychiatric assessment according to DSM-V criteria by an assistant from the Department of Psychiatry at the same 24-hour timeframe. When delirium was detected in the first assessment, the follow-up of those patients were terminated. Patients went through assessment CAM-ICU in the morning between 09:00 and 12:00 The effect of possible risk factors on delirium was investigated.
Results
The incidence of delirium according to DSM-V was 32% (n = 40) in our study. The sensitivity of the CAM-ICU scale to DSM-V was 90%, the selectivity was 97.6% and the kappa value was 0.89. The sensitivity of the ICDSC scale according to DSM-V was 92.5%, the selectivity was 96.5% and the kappa value was 0.89. According to our study, the sensitivity of the ICDSC scale was higher and selectivity of the CAM-ICU scale was higher, with both of the scales showing high sensitivity and selectivity. In our study, older age, higher APACHE-II score, hypotension, electrolyte imbalance, mechanical ventilation, and infection were found to be risk factors for delirium.
174
PROPHYLACTIC USE OF PLATELETS IN CRITICALLY ILL PATIENTS WITH THROMBOCYTOPAENIA: A RETROSPECTIVE OBSERVATIONAL STUDY USING THE PICRAM DATABASE
1Nuffield Department of Clinical Neurosciences, University Of Oxford, Oxford, United Kingdom
2University of Melbourne, Melbourne, Australia
Introduction
Thrombocytopaenia is found in 8.3–67.6% of patients treated in ICU. It is commonly defined by a platelet count under 150 x 10^9/L. Guidelines reporting thresholds for platelet transfusion are lacking. We hypothesise that this would lead to a wide range of platelet transfusion triggers.
Objectives
We reported current practices of prophylactic platelet transfusions for critically ill thrombocytopaenic patients, and their effect on platelet counts. We compared these between patients with and without bone marrow failure as a cause of their thrombocytopaenia.
Methods
We conducted a retrospective analysis of the PICRAM database, covering 13,439 patients admitted to three ICUs in the United Kingdom between 2008 and 2016. We identified thrombocytopaenic patients who received a prophylactic platelet transfusion. We separated these into those with bone marrow failure, defined by a WCC < 1.0 x 109/L prior to transfusion, and those without. We assessed the transfusion trigger, defined by the last platelet level prior to transfusion, and the increment in platelets following transfusion. These outcomes were compared between groups.
Results
Of 13,439 patients, 591 (4.4%) received a prophylactic platelet transfusion for thrombocytopaenia during admission. Platelet levels before and after transfusion were available for 513 patients. The trigger for platelet transfusion was 42.3 ± 27.7 x109/L overall. When comparing those with and without primary bone marrow failure, the trigger was 22.6 ± 17.9 for those with marrow failure and 47.9 ± 27.4 for those without (p < 0.01). The increment in platelets following transfusion was significantly reduced in patients with bone marrow failure (11.4 ± 26.4 x 109/L) compared with those without (30.6 ± 36.4 x 109/L) (p < 0.01).
Conclusions
There appear to be different practices in managing thrombocytopaenic patients with bone marrow failure compared to those without. Platelet transfusions appeared to be less efficacious in critically ill patients with bone marrow failure.
178
Correlation analysis and expression parameters of miRNA-125 in sepsis shock patients with acute kidney injury
1ICU, Chengdu, China
Introduction
Acute kidney injury(AKI) is a frequent and serious complication of septic shock. Currently, the diagnosis of AKI is based on changes in serum creatinine, which is a late marker. We need find a new biomarker for the prediction of AKI in patients with septic shock.
Results
A total of 256 patients (134 patents with AKI and 122 patients without AKI) were enrolled. The levels of miRNA-125, NGAL, IL-6, APACHE II score and creatinine in AKI group were significantly higher than those in non-AKI group. Multivariate regression analysis showed the creatinine, APACHE II score, miRNA-125 and NGAL were independently associated with AKI(P < 0.05). The level of TNF-a in mild-AKI group was 82.3 ± 21.2ng/ml and 171 ± 23.5 ng/ml in severe AKI group (P < 0.05). The level of miRNA-125 in mild-AKI group was 29.5 ± 6.9 and 39.8 ± 9.2 in severe AKI group(P = 0.01). The area under curve of miRNA-125 and NGAL was 0.80 and 0.75.
Conclusion
The level of miRNA-125 is associated with occurrence of AKI in septic shock patients and could predict the incidence rate of AKI.
179
A SCOPING REVIEW OF ACCELEROMETRY IN INTENSIVE CARE UNITS: PRESENT AND FUTURE OF MOVEMENT ASSESSMENT
1Servicio de Medicina Física y Rehabilitación, Departamento de Medicina Interna, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
2Critical Care Departament, Clínica Alemana Universidad del Desarrollo, Santiago, Chile
3School of Physical Therapy, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
Introduction
Immobility is a risk factor for developing long-term functional impairments. Since 90’s decade accelerometry has been used in Intensive Care Units (ICU) in order to measure movement continuously and objectively.
Methods
Scoping review according to the Joanna-Briggs-Institute methodology. Search was conducted from inception to 15 June, 2017 in MEDLINE, EBSCO, Health BVS and Clinical Trials, using MeSH keywords and terms related to “Intensive Care Unit” and “Accelerometers”. Articles in English and Spanish were selected reporting the use of accelerometry during ICU stay. A qualified researcher performed the search, article selection and data extraction. A senior researcher performed a quality control during selection by title, abstract and full text according to the eligibility criteria.
Results
Overall, 22 of the 162 articles found were analyzed. According to the ICU setting, 17 studies were found in the Adult-ICU, 3 in the Neonatal-ICU and 2 in the Pediatric-ICU. The accelerometry studies have been conducted in United States (36.4%), Israel (18.2%), Canada (9.1%), Holanda (9.1%), Inglaterra (4.5%), Australia (4.5%), Brazil (4.5%) China (4.5%), Italia (4.5%) and Japón (4.5%). Accelerometers are mainly used in wrist (59%), ankle (14%), wrist and ankle (18%) and hip (5%). Accelerometry has been used to measure the sleep-wake cycle (59%), movement level (36%) and physical activity (5%) in the ICU. No study reported adverse events with the use of accelerometry in the ICU.
180
PHYSICAL FUNCTIONING MEASUREMENT INSTRUMENTS THAT MEASURE THE MOBILITY DOMAIN DESIGNED FOR THE ICU SETTING
1Servicio de Medicina Física y Rehabilitación, Departamento de Medicina Interna, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
2Critical Care Departament, Clínica Alemana Universidad del Desarrollo, Santiago, Chile
3Department of Clinical Sciences, Brunel University London and The Royal Brompton and Harefield NHS Foundation Trust, London, UK
4School of Physical Therapy, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
Introduction
Mobility is an essential basic-activity-of-daily-life and an important component of rehabilitation in ICU. The use of physical functioning measurement instruments (PFMI) in ICU has increased with multiple tools now available; this can make it difficult to select the most appropriate measure fit for purpose.
Methods
A secondary analysis of a scoping review based on the Joanna-Briggs-institute methodology. A systematic search was conducted from inception to 05–17-2017 in Cochrane-CENTRAL, PubMed, CINAHL, LILACS and hand search, using key words and MeSH (“measurement instrument”, “Intensive Care Units” and “Physical Function”). All types of articles that used or named at least one PFMI in ICU-setting were screened. An expert analysis selected the International Classification of Functioning, Disability and Health domains included in the PFMI.
Results
We included 181 articles of 4434 identified. We found 38 instruments that measure the mobility domain, of which 13 were designed for ICU-setting. The mobility-instruments with the highest frequency of use in scientific articles were Physical Function in Intensive care Test-scored (9.4%, n = 17), Functional Status Score for the ICU (8.8%, n = 16), ICU Mobility Scale (6.6%, n = 12), Perme ICU Mobility Score (3.9%, n = 7), Chelsea Critical Care Physical Assessment Tool (3.3%, n = 6) and Surgical ICU Optimal Mobilisation Score (2.8%, n = 5). Of the 13 mobility-instruments designed for the ICU setting, 7 exclusively measure mobility and 6 measure additional domains (e.g., muscle function, movement function, respiration function, exercise tolerance functions). The mobility-activities most frequently used in the instruments were maintaining-a-sitting-position (69%, n = 9), standing (69%, n = 9) and walking-short-distances (69%, n = 9).
181
MOVEMENT BEHAVIOR OF PATIENTS WITH SEVERE ACQUIRED WEAKNESS DURING INTENSIVE CARE UNIT STAY
1Servicio de Medicina Física y Rehabilitación, Departamento de Medicina Interna, Clínica Alemana Universidad del Desarrollo, Santiago, Chile
2Critical Care Departament, Clínica Alemana Universidad del Desarrollo, Santiago, Chile
3School of Physical Therapy, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
Introduction
The severity of the critical illness is associated with prolonged periods of immobility causing intensive care unit acquired weakness (ICUAW). The movement behavior of critically ill patients during whole ICU-stay is still unknown.
Methods
A secondary analysis of a prospective study approved by the Clínica Alemana Universidad del Desarrollo ethics committee (N°2017-104) was conducted in a 12-beds academic medical-surgical ICU. Adult patients with mechanical ventilation were selected, who on awakening had a Medical Research Council Sum-Score lower than 36-points. Awakening was defined as patient answered 5-simple questions for first time. A triaxial-accelerometry (Actigraph® GT9X-Link) was installed in the right ankle to measure movement during 24-hours-day throughout ICU-stay. All patients received standard physiotherapy including multimodality-respiratory-physiotherapy, passive-range-of-motion, neuromuscular-electrical-stimulation, cycling and progressive-mobility. REDcap® was used to capture the patients characteristics. The accelerometry variables were: immobility time and amount of movement (counts) measured from ICU-admission to awakening (before awakening) and from awakening to ICU-discharge (after awakening).
Results
Of 29 patients who completed the accelerometry measurement during ICU-stay from October-2018 to January-2019, 6 had severe ICUAW. Fifty-percent were female and their characteristics (median [RIQ]) were: age = 77 (68–79) years old, body mass index = 27 (26–29), APACHE II = 19 (16–24) points, mechanical ventilation days = 6 (6–10), ICU length of stay = 11 (10–16), Functional Status Score for the Intensive Care Unit on awakening = 7 (5–10) points and at ICU discharge = 18 (15–22) points. The immobility per hour was 40 (24–55) and 24 (22–50) minutes before and after awakening, respectively. The amount of movement per hour was 1048 (251–1881) and 889 (308–2000) counts before and after awakening, respectively.
182
A FRAMEWORK TO PROMOTE LOCAL BIOETHICAL CAPACITY DEVELOPMENT IN GLOBAL INTENSIVE CARE
1Boston Children’s Hospital, Boston, United States
Introduction
Intensive care is expanding in developing countries, often in collaboration with foreign partner institutions. As new technologies are deployed, bioethical concerns naturally arise. Ethical clinical decision making demands a deep understanding of local cultural constructs. Instead of aiding partner institutions to develop a local ethical framework, foreign institutions often dictate standards based off western practices. Global health practitioners experience moral distress at the perceived differences, and lack the tools to facilitate a conversation about ethical differences.
Methods
The Harvard Center for Bioethics convened an Organizational Ethics Consortium. The Consortium examined the case of the first pediatric ventilator donated to a tertiary referral center in Malawi and the experiences of practitioners surrounding decisions of resource allocation. Following this meeting, the author reviewed the available literature, evaluated benefits and limitations, and ultimately generated an actionable framework.
Results
The rubric describes five discrete points: i) Time out – declare the emergence of an ethical concern; ii) Gather information – outline ethical issue, identify stakeholders; iii) Evaluation – describe stakeholder’s ethical frameworks; iv) Decision making – explore options within ethical frameworks, identify preferences, examine legal ramifications; v) Resolution – make clinical decision transparently and collaboratively.
186
WHICH IS THE MOST EFFECTIVE METHOD OF TEACHING THE FORCE OF CRICOID PRESSURE TO APPLY DURING RAPID SEQUENCE INDUCTION?
1The Queen Elizabeth Hospital, Adelaide, Australia
2Royal Adelaide Hospital, Adelaide, Australia
3University of Birmingham, Birmingham, UK
4Sandwell & West Birmingham NHS Trust, Birmingham, UK
Introduction
Cricoid pressure is theoretically used to reduce the risk of aspiration during rapid sequence induction. The recommended force applied to the cricoid is 10–20 newtons (N; 1.020–1.040kg) on awake patients and 30–40N (3.060–4.080kg) on anaesthetised patients, however it is difficult for staff to accurately estimate this required force in clinical practice.
Methods
30 nurses/doctors from two hospitals with clinical experience of applying cricoid pressure were included. Baseline cricoid pressure force measurements were taken from all participants using an airway model attached to measuring scales for “awake” and “anaesthetised patients”, with the participants blinded to the actual force. Participants were taught one of three teaching methods: biofeedback, bridge of nose analogy and 50ml syringe method. Post-teaching, force measurements were repeated with the participants again blinded to the actual force. Data analysis was performed using a linear mixed model.
Results
Model estimates and marginal predictions of post-teaching forces in newtons between the teaching methods and “awake” vs “anaesthetised patients” yielded various differences. For the “awake patients” biofeedback teaching method lead to predicted forces on the upper limit of those recommended (mean 21.6N, 95% CI 16.7–26.4), nose analogy method lead to forces within the recommended range (14.6, 9.7–19.4), whilst the 50ml syringe method forces were much greater than recommended (29.0, 23.9–34.0). For “anaesthetised patients”, biofeedback teaching method lead to predicted forces within the recommended range (33.4, 28.4–38.3), the nose analogy method lead to predicted forces less than recommended (26.3, 21.6–31.1), whilst the 50ml syringe method caused predicted forces above those recommended (40.8, 35.8–45.8).
198
HAEMOGLOBIN ESTIMATION BY NON-INVASIVE PULSE CO-OXIMETRY OR ARTERIAL BLOOD CO-OXIMETRY ARE INFERIOR TO ARTERIAL HEMOCUE™ ESTIMATION DURING INTRA-OPERATIVE HAEMORRHAGE
1Tata Memorial Hospital, Mumbai, India
Introduction
Non-invasive, continuous spectroscopic haemoglobin monitoring using pulse oximetry (SpHb) may be advantageous during major surgical haemorrhage.
Methods
60 adult patients undergoing elective oncosurgery with anticipated blood loss > 21ml/kg wore a Rainbow ReSposable Sensor (R-25a) with a Masimo Radical-7™ Pulse CO-Oximeter (SpHb). Arterial blood samples were analysed with a Siemens laboratory analyser (HbLab), a Roche COBAS-B221co-oximeter (HbABG), and HemoCue™ haemoglobinometer (HbHC). SpHb, HbABG and HbHC were compared with HbLab at T1, prior to surgical incision; T2, prior to transfusion of packed red blood cells (PRBCs); T3, after transfusion of two units of PRBCs; and T4, after completion of surgery. Agreement was analysed by the Bland–Altman method and and Morey’s error grid was plotted. Trend accuracy was determined by the mean difference between HbLab and other methods at each time point (paired ‘t’ test).
Results
183 measurements were obtained from 54 patients. Median (interquartile range) blood loss was 2500 (1600–3425) ml. Compared with HbLab, bias (precision) and [Limits of agreement] were −0.23 (1.64) gm/dl, and [+2.99, −3.44] gm/dl, respectively, for SpHb. Corresponding values for HbABG and HbHC were −0.84 (1.29), [+1.69, −3.37] gm/dl, and 0.29 (1.19), [+2.62, −2.04] gm/dl, respectively. On error-grid analysis there were no values in the critical error Zone C with any method. There was a significant difference between mean SpHb and mean HbLab at T2, and between HbABG and HbLab at all points, while there was no difference between HbHC and HbLab at any point.
220
RISK FACTORS FOR PROLONGED MECHANICAL VENTILATION IN PATIENTS WITH LEFT VENTRICULAR ASSIST DEVICES
1Department Of Anesthesiology And Intensive Care, Osaka University Graduate School Of Medicine, Suita, Osaka, Japan., Suita, Japan
Introduction
Prolonged mechanical ventilation (PMV) after cardiovascular surgery is associated with increased patient morbidity and mortality. However, there are only limited data on patients requiring left ventricular assist device (LVAD) implantation as a bridge therapy to heart transplantation.
Objectives
We aimed to identify perioperative predictors of PMV after LVAD implantation and its impact on patient outcomes. PMV was defined as the need for intubation and mechanical ventilation for more than 144 hours.
Methods
From April 2012 to March 2017, adult patients admitted to the intensive care unit (ICU) after LVAD implantation were consecutively included. We reviewed the baseline characteristics, operative data and the variables at ICU admission retrospectively.
Results
A total of 91 patients, 68.1% male, were enrolled. The median age was 47 [37 – 58] years. PMV occurred in 38 (41.8%) patients, and 17 (44.7%) of these underwent tracheostomy. The multivariable logistic regression identified mechanical ventilation prior to the LVAD implantation (OR = 4.62, 95% CI = 1.13 – 18.87), increased central venous pressure (CVP) (OR = 1.22, 95% CI = 1.03 – 1.44), administration of dopamine (OR = 14.16, 95% CI = 2.18 – 98.77) and administration of inhaled nitric oxide (iNO) (OR = 14.16, 95% CI = 3.46 – 57.95) as independent predictors of PMV. Moreover, extended ICU length of stay (23 vs. 6 days, P < 0.001) and higher ICU mortality (7.9 vs. 0%, P = 0.07) were observed among patients requiring PMV.
Conclusions
PMV after LVAD implantation is associated with patient worse outcomes. Our results suggest that LVAD recipients previously supported on mechanical ventilation, those with higher CVP, and requiring dopamine or iNO at ICU admission have an increased risk of PMV. Further studies in larger cohorts are necessary to confirm these findings for the optimal clinical management.
235
ACCURACY OF FOUR SUBCUTANEOUS CONTINUOUS GLUCOSE MONITORING SYSTEMS IN CRITICALLY ILL PATIENTS WITH HYPERGLYCAEMIA
1University Of Melbourne, Parkville, Australia
2Department of Critical Care Medicine, St Vincent’s Hospital Melbourne, Melbourne, Australia
Introduction
Intermittent blood glucose monitoring may miss episodes of hyper- and hypoglycaemia in critically ill patients. Subcutaneous continuous glucose monitors (CGMs) may improve glycaemic control and patient safety. Few studies have evaluated multiple CGMs in the same population of ICU patients. It is therefore unknown which device is most accurate and by what factors accuracy may be affected.
Methods
In our prospective, observational study, we applied one subcutaneous CGM to the abdomen or upper arm of 41 hyperglycaemic ICU patients. Readings were recorded hourly and time matched reference measurements were taken from arterial or capillary blood. This produced 1588 paired measurements for analysis. Accuracy was assessed using the median absolute relative difference (MARD) between paired measurements and Bland Altman analysis. Factors associated with device accuracy were identified using univariate and multivariate analysis.
Results
Devices differed significantly in their accuracy (P < 0.001). The Medtronic Guardian Connect (Guardian Sensor 3) (MARD 9.39%, interquartile range 4.03–19.05%, mean bias 0.27 mmol/L, limits of agreement, –6.37− 6.91 mmol/L) and the Dexcom G4 (MARD 11.05%, interquartile range 5.33–21.33%, mean bias 0.22 mmol/L, limits of agreement, –6.74 – 7.19 mmol/L) demonstrated superior accuracy. Several factors were associated with decreased sensor accuracy, including hyperthermia, hypoglycaemia and receiving paracetamol. Wearing a subcutaneous continuous glucose monitor was associated with a 40% reduction in the frequency of hypoglycaemia, relative to historical data (p = 0.002).
236
0.9% SALINE BOLUS ADMINISTRATION LEADS TO PERMEABILITY PULMONARY OEDEMA IN HEALTHY VOLUNTEERS
1Flinders Medical Centre, Intensive & Critical Care Unit, Bedford Park, Australia
2Flinders University, Department of Critical Care Medicine, Bedford Park, Australia
3Flinders Medical Centre, Respiratory Function Laboratories, Bedford Park, Australia
Introduction
Bolus intravenous administration of 0.9% saline has been associated with the development of pulmonary oedema and increased mortality. We have previously showed in an animal model that rapid administration of 0.9% saline was associated with non-hydrostatic lung injury with increased lung lavage protein. We hypothesised that this non-hydrostatic effect would also be present in human volunteers.
Objective
To demonstrate non-hydrostatic lung injury due to bolus fluid administration in healthy human volunteers.
Methods
In a randomised, cross-over study of 14 healthy male subjects, we compared the lung lavage protein concentration and cardiorespiratory effects of rapid (100ml/minute) intravenous administration of 30 ml/kg of 0.9% saline with no fluid bolus. Bronchoalveolar lavage (BAL) was performed after fluid administration, while doppler echocardiography, lung ultrasound, lung function tests, blood gases and Borg’s dyspnoea scale were performed before and after each intervention. Data was analysed with repeated measures ANOVA with the fluid effect examined as an interaction effect.
Results
All 14 subjects completed both study days. None of the subjects reported dyspnoea after 0.9% saline administration (modified Borg scale = 1). BAL protein concentration was higher after 0.9% saline than no fluids (196.1(87.6) vs. 129.8(55.4) µg/ml, p = 0.002). There was an increase in ultrasound lung B lines (1(0–3) to 3(1–6), P = 0.03), and decrease in FEV1 (4.55(3.17–5.24) to 4.25(3.35–4.94), p < 0.01) after 0.9% saline administration. There was an increase in stroke volume (58(51–74) to 66(58–74), p = 0.045) and Doppler echocardiography left ventricle E/e’ ratio (5.0(4.5–6.0) to 5.7(5.3–6.3), p = 0.007), but no difference in IVC maximum diameter (p = 0.34) or tricuspid annular plane systolic excursion (p = 0.06).
Conclusion
Rapid intravenous administration of 0.9% saline leads to non-hydrostatic pulmonary oedema in healthy human volunteers. While this may underlie the development of lung oedema during fluid resuscitation, relevant disease orientated research is needed.
242
DENGUE COMPLICATING PREECLAMPSIA LEADING TO MARTENAL MORTALITY. TWO CASES FROM HOSPITAL OF TROPICAL DISEASES HO CHI MINH CITY, VIETNAM
1Hospital Of Tropical Diseases Ho Chi Minh City, Ho Chi Minh City, Viet Nam
Introduction
Dengue, a mosquito borne viral infection is common in Vietnam. The clinical manifestations range from arthralgia, fevers, malaise to multi organ failure and in particular severe haematological abnormalities. Mortality from dengue is low in the general population, however infection during pregnancy increases the risk of death.
Methods
We report on cases of preeclampsia and superimposed dengue in two women.
Results
Case One: 23 yo G1P0 with mild preeclampsia presented with high fevers at 37 weeks gestation. Dengue was confirmed on admission. On day 4 of, an emergency Caesarean section was performed for severe hypertension and foetal distress. Following delivery, she was transferred to the tertiary hospital. On admission the patient was noted to have features of HELPP (haemolysis, elevated liver enzymes, thrombocytopenia) as well as acute renal failure. The patient rapidly deteriorated, requiring intubation and commenced on continuous renal replacement therapy. Her clinical course was complicated by ongoing coagulopathy, severe purpeural sepsis and persistent coma. She died three weeks after admission. Case Two: 29yo G1P0 admitted at 31 weeks gestation with fevers and vomiting and diagnosed with dengue. On Day 4, she developed severe preeclampsia. Following an emergency Caesarean section, the patient had severe lactic acidosis, thrombocytopenia and acute renal failure. Despite maximal supportive therapy, the patient had persistent acidosis and coagulopathy and died on day 4 of her intensive care admission.
244
The therapy to incarcerated obturator hernia after reduction under ultrasonography
1Tokai Hospital, Nagoya, Japan
Introduction
Obturator hernia is a relatively rare pelvic hernia which can cause bowel obstruction and usually occurs in elderly women. Despite improved imaging techniques which can allow us to make a preoperative diagnosis, emergent operation is still often carried out. It is very risky because the patients are elder.
Methods
At first, we examine intestinal perforation by Computed Tomography (CT). When we suspect intestinal perforation, we consider emergent operation. When we don’t find perforation and just incarceration, we try to reduce under ultrasonography. If we can’t reduce, we consider emergent operation.
Results
We have been able to reduce all six cases until now. It took 4.2 sec as mean time. After reduction, they are admitted to hospital conservatively. In the hospital, we pay attention to delayed intestinal perforation and examine their general conditions. According to their conditions, we can safely choose the anesthetic method (local or general) and operative method (laparotomy or laparoscopy).
246
REDUCING INAPPROPRIATE ARTERIAL BLOOD GAS TESTING IN A QUATERNARY INTENSIVE CARE UNIT
1Royal North Shore Hospital, Sydney, Australia
2The University of Sydney, Australia
Introduction
Arterial blood gas (ABG) analysis is the most frequently ordered pathology test in the Intensive Care Unit (ICU), carrying a high cost and contributing to iatrogenic anaemia. Ordering is largely driven by cultural factors and a significant proportion of tests are not clinically indicated.
Objectives
To identify the indications for ABG analysis in the ICU and reduce the number of inappropriate ABGs without compromising patient care.
Methods
The indications for ABG analysis were surveyed at a 58-bed quaternary ICU during fortnightly periods before and after a multifaceted intervention consisting of education of medical and nursing staff and the introduction of a clinical guideline. The number of ABGs performed in the second half of 2017 was compared with the number performed in the second half of 2018 (post-intervention). Tests were defined as inappropriate if performed at regular time intervals in a stable patient, at change of shift, when taken concurrently with other blood tests, in response to a decrease in ventilation or oxygen delivery, or after a treatment was ceased in a stable patient. The study was enrolled on the local Quality Improvement Projects Register and ethical approval waived by the local ethics committee.
Results
The proportion of inappropriate ABGs decreased from 54.2% to 28.6% between the two surveys. The number of ABGs decreased from 33,005 in the first six-month period to 22,408 in the second (a 31.3% reduction when adjusted for ICU bed-days, p < 0.001). This represents an annual saving of approximately A$750,000 and 100L blood. There was no significant difference in the standardised mortality rate (APACHE III) between the two periods (0.65 vs 0.63, p = 0.22).
Conclusion
Clinician education and the implementation of a clinical guideline resulted in a substantial decrease in both the proportion of inappropriate ABGs and the total number performed, resulting in significant cost savings.
248
PHARMACOKINETIC DATA SUPPORT 6-HOURLY DOSING OF INTRAVENOUS VITAMIN C TO CRITICALLY ILL PATIENTS WITH SEPTIC SHOCK
1Department of Medicine and Radiology, Melbourne Medical School, Royal Melbourne Hospital, Parkville, Australia
2Department of Intensive Care, Alfred Health, Melbourne, Australia
3Australian and New Zealand Intensive Care Research Centre, Melbourne, Australia
4School of Health and Biomedical Sciences, RMIT University, Bundoora, Australia
5RCPAQAP Vitamins Advisory Committee, St Leonards, Australia
6Victorian Clinical Genetics Services, Murdoch Children’s Research Institute, Parkville, Australia
7Department of Intensive Care, Austin Health, Heidelberg, Australia
Introduction
Intravenous vitamin C is a potential treatment for septic shock but there are no pharmacokinetic data in this population.
Methods
This was a prospective observational study. After informed consent, patients with septic shock had arterial blood sampled at four timepoints: at baseline and 1, 4 and 6 hours post initial intravenous administration of 1.5 grams of vitamin C. Samples were collected in chilled tubes and immediately centrifuged and plasma stabilised with diethylenetriamine pentaacetate/perchloric acid solution. Samples were analysed with Chromsystems vitamin C kits using high-performance liquid chromatography with ultraviolet detection. Pharmacokinetic parameters were calculated using PKSolver. Data are presented as median (interquartile range).
Results
Twelve patients (7 women, age 60.5 (57 – 72.8) years, weight 75 (69 – 81) kg, eGFR 49.5 (30.8 – 62.3 mL/min/1.73 m2, noradrenaline rate 9 (6.5 – 17.5) microgram/min) participated. Pre-dose vitamin C concentration in serum was 29.5 (10.8 – 50.3) micromol/L. One patient died prior to the 6-hour timepoint. Calculated vitamin C plasma half-life was 4.4 (3.4 – 5.7) hours, volume of distribution 27.8 (22.4 – 37.4) L, and clearance 5.2 (3.5 – 5.8) L/h.
250
A REVIEW OF THE WITHDRAWAL OF TREATMENT WITHIN 24 HOURS OF REFERRAL TO STARSHIP PICU TRANSPORT SERVICE IN NEW ZEALAND
1Starship Paediatric Intensive Care Unit, Auckland, New Zealand
Introduction
The Starship PICU transport service is the only dedicated paediatric retrieval service in New Zealand. Often due to severity of illness, a proportion of children referred will have life sustaining treatment withdrawn. The decision whether to transfer a child with a non-survivable condition miles away by air to PICU and separating them from their whānau (family unit) is a difficult one that can be supported by the transport service.
Methods
A manual and electronic search of referrals (2016–2018) that received withdrawal of life sustaining treatment within 24 hours of referral was conducted. Data including age, inotropic support, pupils, suspected cause of death and location was analysed.
Results
A total of 29 referrals met the above criteria. Of these, 11 patients had withdrawal of life sustaining treatment at the local hospital after discussion with the retrieval team. 8 of those received advice via telephone and 3 received face-to-face support. Patients ranged between 1 day to 10 years of age and 45% of these patients had significant co-morbidities. 18/25 patients were retrieved to PICU prior to withdrawal of treatment.
252
4% SUCCINYLATED GELATINE IS ASSOCIATED WITH INCREASED RENAL OXIDATIVE STRESS IN CARDIAC SURGICAL PATIENTS: A PILOT RANDOMISED CONTROLLED TRIAL
1Murdoch University, Murdoch, Australia
2Centre for Clinical Research in Emergency Medicine, Perth, Australia
3Fiona Stanley Hospital, Murdoch, 6150
4University of Western Australia, Perth, Australia
5Royal Perth Hospital, Perth, Australia
Introduction
Patients admitted to the intensive care unit (ICU) after cardiac surgery frequently require intravenous fluid resuscitation and are at risk of developing postoperative acute kidney injury (AKI). Colloids, including 4% succinylated gelatine (GEL), are used commonly but their safety is uncertain.
Methods
Patients who required at least 500mL fluid bolus after cardiac surgery were randomised to receive GEL or CSL as the ongoing fluid for bolus therapy for 24 hours. Urinary F2-isoprostanes concentration, a measure of renal oxidative stress, was measured by gas-chromatography-mass-spectrometry at baseline, one hour, five hours and 24 hours after enrolment. Difference in concentrations over time between groups was assessed using a mixed-effects regression model. A p < 0.05 for the interaction between time and treatment allocation was considered significant.
Results
Of the 40 participants recruited (mean age 64 years), 31 (78%) were male and 29 (73%) had on-pump surgery. Median EuroSCORE II-predicted mortality was 1.09% (Q1-Q3 0.80–1.82). There was no significant difference between groups in these baseline variables. The total median study fluid administered within 24 hours of enrolment was similar (GEL 1250mL, Q1-Q3 500–1750 vs CSL 1000mL, Q1-Q3 500–1375; p = 0.42). Patients who received GEL had a significantly higher urine concentration of F2-isoprostanes over time (p = 0.036) compared to those who only received CSL, with a significant post-hoc pair-wise difference at 24 hours (GEL geometric mean 37.3 nmol/L, 95% confidence interval [CI] 20.4–68.0 vs CSL geometric mean 8.6 nmol/L, 95% CI 5.0–14.8; p = 0.002).
Conclusion
Compared to using CSL for fluid resuscitation, use of GEL was associated with an increase in renal oxidative stress within 24 hours after its administration in postoperative cardiac surgical patients.
254
HIGHER SKIN FLOW REACTIVITY INDUCED BY A THERMAL CHALLENGE PREDICTS AN IMPROVEMENT IN ORGAN FUNCTION IN OUT-OF-HOSPITAL CARDIAC ARREST PATIENT
1Intensive Care Department, Erasme University Hospital, University Libre Bruxelles, Belgium, Brussels, Belgium
Introduction
Skin blood flow (SBF) is rapidly altered during shock and the last to recover after resuscitation.
Objectives
SBF alteration is associated with organ dysfunction in patients after out-of-hospital cardiac arrest (OHCA).
Methods
In 29 OHCA patients under targeted hypothermia (TH) (33 ˚C) for 24 hours, SBF was measured (Periflux 5000, Perimed; index finger, Perfusion unit: PU) at basal temperature (BT) and at 37 ˚C (SBF37) (thermal challenge (TC)) at the begining of TH (T0), and 6 (T6) and 24 (T24) hours later. The response of TC was defined by the ratio SBF37-SBF/37-BT (ΔSBF/ΔT). Systemic parameters, lactate levels were obtained concurrently. An improvement in organ function (IMP) was defined as a reduction in SOFA scores (ΔSOFA) by ≥2 within 48 hours after T0. Patients were IMP were compared to those without IMP (non-IMP). A receiver operating characteristic (ROC) curve was performed and the area under the curve (AUC) was calculated to evaluate the predictive values of baseline ΔSBF/ΔT on a IMP.
Results
Organ function improved in 12 of the 29 patients. At T0, MAP and CI were similar, but SOFA scores and lactate concentrations were lower in the IMP than the non-IMP group (SOFA; 10 (6–12) vs 15 (12–18),p = 0.03, Lactate; 2.6 (2–3.7) vs 4.9 (3.3–6.2) mmol/L, p = 0.03). SBF didn’t differ (18 (13–83) vs 13 (11–18) PU, p = 0.2), but ΔSBF/ΔT was higher in IMP than in the non-IMP group (8 (3–12) vs 0.9 (0.3–1.3), p < 0.01).
SBF and ΔSBF/ΔT increased in the IMP group over the period of TH but remained lower in non-IMP group. ΔSBF/ΔT at T0 had a AUC of 0.93 (0.83–1.0) with a cut-off value ≥1.26 (Sensitivity 89%; Specificity 76) to predict IMP.
256
TRACHEOSTOMY TRAINING IN CAMBODIA – A NEW COURSE FOR MANAGING SWALLOWING PROBLEMS
1Wythenshawe Hospital, Manchester University NHS Foundation Trust, MFT, Manchester, United Kingdom
2Barking Havering and Redbridge University Hospitals, Barking, UK
3Manchester Royal Infirmary, Manchester University NHS Foundation T, Manchester, UK
4Speech Therapy Cambodia, Phnom Penh, Cambodia
Introduction
Tracheostomy services are significantly less developed in Cambodia. Under-resourced hospitals have inadequate or non-existent tracheostomy equipment. Basic care, tube changes and weaning are limited. Staff lack opportunities for familiarity, knowledge and skills growth. A non-government organisation (NGO) ‘Speech Therapy Cambodia’ (STC) trains medics, nurses and physiotherapists in dysphagia in the absence of Cambodian Speech Therapists. Tracheostomy training had not previously been delivered in Cambodia.
Methods
A 3 day course was delivered at Calmette hospital, Phnom Penh by a UK team of 3 Speech Pathologists in February 2019. Lectures, videos, decannulation checklists, local case studies and hands-on instructional activities were devised taking a culturally sensitive, problem solving approach. Topics covered; tracheostomy basics, indications, tubes, dysphagia, cuff management, prevention and management of complications. STC organised executive hospital buy-in and local logistics and Interpreters rehearsed with the UK trainers pre-teaching. The UK National Tracheostomy Safety Project donated equipment for training. Learner needs were investigated by completion of pre and post course questionnaires exploring experience, knowledge and confidence.
Results
A course handbook was produced and duplicated in English and Khmer. Trainees were enthusiastic and engaged throughout. Self-rated knowledge grew (Table 1) and confidence in dealing with tracheostomy patients increased (mean 4.5 to 7.5/10) post training. Quality of teaching was rated 9.6/10 and likelihood of clinical application of knowledge 9.5/10. In follow-up, STC shared case studies illustrating improvements in care with ripple-effect to other hospital staff.
257
RETROSPECTIVE REVIEW STUDY OF EPIDURAL-GENERAL ANESTHESIA AFFECTING POST-RESECTION HYPOTENSION OF PHEOCHROMOCYTOMA AND PARAGANGLIOMA
1Department of Anesthesia and Pain Medicine, Medical Research Institute, Pusan National University Hospital, Busan, South Korea
2Department of Dental Anesthesia and Pain Medicine, School of Dentistry, Pusan National University, Dental Research Institute, Yangsan, South Korea
Introduction
During resection surgery of catecholamine-secreting tumors (e.g. pheochromocytoma or paraganlioma), hemodynamic instability episodes can arise and be life-threatening.
Methods
Patients medical record was collected who had undergone resection surgery for pheochromocytoma or paraganlioma from January 2000 to December 2008. The primary predictor variable was the anesthetic technique (GA vs. GE) and primary outcome variable was the presence of post-resection hypotension. Post-resection hypotension was defined as mean blood pressure (MBP) < 60mmHg or > 30% reduction in systolic blood pressure (SBP) from baseline. Abstracted multiple covariates also included baseline patient characteristics, preoperative CT findings, preoperative levels of catecholamine, premedications, intraoperative data, tumor weight, and hemodynamic data.
Results
A total of 104 patients were identified, 53 (51.0%) had surgery with GE technique, and 51 (49.0%) with GA. Post-resection hypotension occurred in 80 (76.9%) patients. On multivariate analysis, independent risk factors of post-resection hypotension were increased HU at unenhanced CT (adjusted OR [95% CI]: 1.112 [1.009–1.226], p = 0.033), increased MBPb (adjusted OR [95% CI]: 1.063 [1.012–1.117], p = 0.015), and GE techniques (adjusted OR [95% CI]: 5.439 [1.410–20.977], p = 0.014). Alpha-blocker premedication was included in the final model, but was not statistically significant (adjusted OR [95% CI]: 5.459 [0.937–31.805], p = 0.059).
258
MITOCHONDRIAL FUNCTION DIFFERS BETWEEN MILD INFLAMMATORY DISEASE STATE AND CRITICAL ILLNESS WITH MULTIPLE ORGAN DYSFUNTION SYNDROME
1Liverpool Hospital, Sydney, Australia
2University of Auckland, Auckland, New Zealand
Introduction
MODS is the predominant cause for death in ICU and the pathophysiology is not well understood. Recently, it has become evident that impaired use of oxygen by mitochondria play a important role in MODS. Understanding mitochondrial function (MF) in a mild inflammatory disease and comparing it with MODS has the potential to lead to future treatments.
Methods
In patients with MODS, blood was taken six times over a period of 1 week. In patients with AP, blood was taken for the first three days and at discharge. Blood was taken once from healthy volunteers (n = 15). Assays of mitochondrial electron transport system (ETS) were done using a multiple substrate inhibitor titration protocol.
Results
In mild AP (n = 18), MF was significantly raised early in the disease course in order to keep up with the cell’s energy demands. This is in contrast with MODS (n = 27) where no significant increases in MF were seen early in the disease state. The pattern of MF in AP differed significantly from MODS. In contrast to AP where there were no depression in MF as patients recovered, MODS had significant mitochondrial depression from day 3 onwards. The trough in MF at days 3 and 4 correlated with SOFA and thus the severity of MODS. Additionally, compensation of ETS by Complex I was present from day 2 in AP whereas there was no such compensation in MODS.
259
GIVING VENTILATED TRACHEOSTOMY PATIENTS A VOICE: A SURVEY OF THE USE OF ABOVE CUFF VOCALISATION (ACV) IN THE UK
1Wythenshawe Hospital, Manchester University NHS Foundation Trust, UK, Manchester, United Kingdom
Introduction
Above Cuff Vocalisation (ACV) is a technique to enable cuff inflated tracheostomised ventilated patients to speak, utilizing insufflation of an external gas flow via the subglottic suction port. The benefits of ACV for enabling earlier speaking reducing psychological distress and for swallow stimulation have been described but protocols and guidance are lacking. Speech Language Pathologist (SLP) presence in ICUs is variable in the UK but vitally important for ACV trials. More widespread adoption of subglottic suction tubes is increasing staff awareness of ACV but extent of use and SLP involvement is currently unknown.
Methods
SLPs attending a national tracheostomy clinical excellence network meeting undertook a real-time voting exercise using interactive presentation software (mentimeter). 7 questions examined ACV use, SLP involvement, reasons why ACV was not used and suggestions for features that would improve an ACV system. Response rate varied between 34 and 69 SLPs per question.
Results
SPs reported ACV use in 53% of their hospital ICUs and 13% outside of ICUs. Only 60% of first ACV trials and 62% of subsequent ACV trials were performed with SLP involvement. Reasons for lack of ACV use included insufficient SLP staff, no access to subglottic suction tracheostomy tubes, lack of knowledge and training, inconsistent MDT approach and safety concerns. Suggestions for ACV system improvements focused on humidification, equipment, ventilator synchronisation and education.
265
ONCOSTATIN M DEFICIENCY RESULTS IN DISTINCT HEMODYNAMIC PROFILE IN NON-SEPTIC AND SEPTIC MICE
1Royal Alexandra Hospital, Edmonton, Canada
2University of Alberta, Edmonton, Canada
Introduction
Sepsis is a leading cause of death worldwide. Oncostatin M Receptor (OSMR) is highly expressed on vascular endothelial cells. Evidence suggests septic OSMR deficiency may improve survival.
Methods
Studies were in accordance with Canadian Council on Animal Care guidelines. Young (3–4 months) male C57Bl/6 and OSMR-/- mice were instrumented for hemodynamic assessment under anesthesia following randomization. Fecal slurry (or vehicle) was administered (1.3mg/g intraperitoneally). Mice received methacholine (1µg/kg intravenously) to assess vasodilatory function every 30 minutes.
Results
Non-septic OSMR-/- mice displayed elevated systolic blood pressure (p = 0.02), diastolic blood pressure (p = 0.02), and heart rate (p = 0.03).
OSMR-/- mice displayed a higher systolic blood pressure (p = 0.003) and diastolic blood pressure (p = 0.005) than C57Bl/6 mice throughout the septic time-course (maximum 600 minutes). Heart rate was not different (p = 0.05). Elevated OSMR-/- septic systolic blood pressure and diastolic blood pressure did not improve median survival (248.5 minutes (C57Bl/6); 226.5 minutes (OSMR-/-) (p = 0.38)).
Methacholine decreased systolic blood pressure in non-septic C57Bl/6 mice by 15.29% ± 2.20% mmHg and 7.41% ± 1.60% mmHg (p = 0.03) in OSMR-/- mice and decreased diastolic blood pressure in non-septic C57Bl/6 mice by 19.93% ± 1.88% mmHg and 9.89% ± 2.05% mmHg (p = 0.04) in OSMR-/- mice. Methacholine elevated heart rate (p = 0.04) in both non-septic genotypes.
In sepsis, methacholine decreased systolic blood pressure in both genotypes (p = 0.0007) but more in OSMR-/- mice (p < 0.0001). Septic diastolic blood pressure response did not decrease in either genotype (p = 0.82), however the OSMR-/- response remained decreased compared to C57Bl/6 mice (p = 0.003). Heart rate response in septic mice did not decrease over time in either genotype (p = 0.44).
266
ONCOSTATIN M DEFICIENCY IN SEPSIS ALTERS EX-VIVO VASCULAR FUNCTION
1Royal Alexandra Hospital, Edmonton, Canada
2University of Alberta, Edmonton, Canada
Introduction
Sepsis is a leading cause of death worldwide. Preliminary evidence demonstrates Oncostatin M receptor (OSMR) deficiency of the vascular endothelium may improve sepsis-related vascular dysfunction.
Methods
Studies were in accordance with Canadian Council on Animal Care guidelines. Young (3–4 months) male C57Bl/6 and OSMR knockout (OSMR-/-) mice were instrumented for hemodynamic assessment under anesthesia following randomization. Fecal slurry (or equivalent volume of vehicle) was administered (1.3mg/g intraperitoneally). Mice were euthanized 120 minutes post-slurry administration to assess vascular function and tone of isolated mesenteric arteries using wire and pressure myography. Cumulative concentration response curves were generated for phenylephrine and the endothelial-dependent and endothelial-independent vasodilators methacholine and sodium nitroprusside in the presence and absence of the non-selective NOS inhibitor L-NG-nitro-arginine-methyl ester (LNAME).
Results
Phenylephrine contractile sensitivity was similar in septic arteries of both genotypes (p = 0.21). However, increased sensitivity to phenylephrine when incubated with LNAME is lost (p = 0.09) in OSMR-/- mice. An interaction between genotype and LNAME exists regarding methacholine response in septic arteries (p = 0.007). C57Bl/6 septic mice required increased concentrations of methacholine to produce vasorelaxation in the presence of LNAME (p = 0.0008) while OSMR-/- septic mice did not (p = 0.98). Genotype did not alter sodium nitroprusside vasorelaxation (p = 0.18).
Sepsis increased passive artery diameter (p = 0.03) in C57Bl/6 mice but decreased OSMR-/- artery diameter (p = 0.009). C57Bl/6 active tone was unaffected by sepsis (p = 0.12) however OSMR-/- arteries lost their active contraction response compared to the non-septic (p = 0.0003). Non-septic OSMR-/- myogenic tone was increased (p = 0.005) but diminished in the septic OSMR-/- mice, whereas sepsis did not alter myogenic tone in C57Bl/6 mice (p = 0.42).
267
TRACHEOSTOMISED PATIENTS WITH A PRIMARY NEUROLOGICAL DIAGNOSIS: A RETROSPECTIVE OBSERVATIONAL STUDY
1Flinders University, Adelaide, Australia
2Royal Adelaide Hospital, Adelaide, Australia
Introduction
Patients with severe neurological disease frequently exhibit neuromuscular ventilatory insufficiency, failure of secretion clearance or inadequate airway protection requiring endotracheal intubation. Prolonged endotracheal intubation is associated with discomfort, increased sedation requirement, laryngeal dysfunction and tracheal injury and tracheostomy insertion may be considered to mitigate these complications.
Methods
We undertook a retrospective, observational analysis of patients admitted to the RAH ICU between 2013 and 2018 with a primary neurological diagnosis who received a tracheostomy for medium to long-term airway support. Data was collected from the local Tracheostomy and ICU Adult Patient Databases. Patients were further stratified by primary neurological diagnosis.
Results
A cohort of 279 patients were studied. The median time to tracheostomy was 9 days, with tracheostomy remaining in-situ for a median 20 days. 37 patients were discharged without decannulation. The median length of stay in RAH ICU and RAH was 17 and 46 days respectively.
A substantial proportion of patients were discharged to other hospitals (34.4%) or chronic/palliative care (39.8%); only 8.24% of patients directly return home upon discharge.
Conclusion
The substantial percentage of patients discharged to sites other than home, especially with tracheostomy in-situ, suggests there is reason to further explore when, why and if we offer tracheostomy to those with a primary neurological diagnosis, however without correlation to functional outcome data, current collection is inadequate to definitively comment. The existing data should be made available to substitute decision makers when considering informed consent for tracheostomy.
268
The utility of TEG 6s (Thromboelastgraphy system) in pediatric cardiac surgery
1Jichi Medical University, Shimotsuke-shi, Japan
Introduction
Thromboelastgraphy(TEG) system is a device that can analyze comprehensive coagulation functions quickly and accurately. Several studies have been reported about the utility of TEG system in the perioperative management of cardiac surgery. TEG® 6s (HAEMONETICS Inc.) is a new TEG device and it enables multiple assays to be performed simultaneously from a single blood sample inserted into a cartridge containing four assays. However, there have been few clinical studies about TEG® 6s, especially in pediatric heart surgery.
Methods
We investigated the analysis results of TEG® 6s in pediatric patients who undergone cardiac surgery at our institution form September 2016 to April 2019. Retrospective chart review was performed.
Results
TEG® 6s were used in 26 patients, and 23 patients of those were tested during operation. The patients age ranged from 10 days to 11 years (median: 20.0 month). TEG® 6s test were performed right after cardiopulmonary bypass (after administration of Protamine). In all cases TEG tracing curves were clearly formed except one patient. The TEG results demonstrated extremely poor coagulation. MA (Maximum Amplitude) of CK (Kaolin TEG) were 31.4 ± 6.9 mm (Mean ± SD), MA of CRT (RapidTEG) were 30.9 ± 8.7mm, and MA of CFF (Functional Fibrinogen) were 3.8 ± 3.0mm. The difference of R (Reaction time) between CK and CKH(Kaolin TEG with heparinase) were 4.3 ± 10.2 min, and heparin were not antagonized by protamine in only two patients. MA of CFF correlated with plasma fibrinogen levels (Correlation Coefficient = 0.499, p = 0.049). The difference of MA between CRT and CFF also correlated with platelet count (Correlation Coefficient = 0.542, p = 0.030).
272
TARGETING THE NO-sGC AXIS TO MONITOR AND TREAT VASCULAR DYSFUNCTION AND VASOPLEGIA IN SEPSIS
1University of Alberta, Edmonton, Canada
2Royal Alexandra Hospital, Edmonton, Canada
Introduction
Vasoplegic blood vessels contribute to hypotension and disturbed regional blood flow as sepsis progresses to septic shock. Perturbed nitric oxide signaling contributes to the pathophysiology of vasoplegia. Oxidative stress damages soluble guanylate cyclase (sGC), the downstream mediator of nitric oxide, resulting in impaired organ blood flow.
Methods
Studies were in accordance with Canadian Council on Animal Care guidelines. Male C57Bl/6 mice (10–12 weeks of age) were instrumented for direct blood pressure and regional blood flow measurements under anesthesia. Sepsis was induced by fecal slurry injection (1.3mg/g intraperitoneally). Bolus doses of phenylephrine (10µg/kg intravenously) and sodium nitroprusside (5µg/kg intravenously) were injected to assess in-vivo vascular function. In a separate series of experiments, mice were treated with cinaciguat (0–90µg/kg intravenously) 30 minutes post fecal slurry injection and survival time monitored.
Results
Blood pressure in septic mice reduced over time (44% ± 4% after 4h of fecal slurry injection) compared to controls (p < 0.01), but no changes in heart rate (p>0.05) were noted.
Blood flow in the carotid, superior mesenteric, and renal arteries reduced at 47 ± 4%, 71 ± 8%, and 57 ± 13% respectively, 4h after fecal slurry injection.
Vessel reactivity to phenylephrine and sodium nitroprusside was reduced by 36 ± 9% and 53 ± 7% respectively, in septic mice compared to controls (p < 0.01), suggesting impaired regional vascular function.
Administration of low dose (15µg/kg intravenously) cinaciguat 30 minutes after fecal slurry injection provided the best survival outcomes in our model. While sGC activity was impaired in septic mice, cinacigaut administration restored its activity by 87 ± 2% (p < 0.05).
274
NEURO INTENSIVE CARE UNIT IMPROVES QUALITY INDICATORS IN NEUROLOGICAL INPATIENTS IN BRAZIL
1Hospital Caxias Dor, Rio De Janeiro, Brazil
Introduction
It is well established internationally that neuro intensive care units (ICU) are the best place to treat neurological patients. But it is important to prove it in different countries, as regional issues might not be the same everywhere.
Methods
We compared quality indicators of neurological patients admitted in our general ICU (before we had a neuro ICU), from June 2013 to July 2015; and the same quality indicators in patients admitted to the neuro ICU, from August 2015 to December 2018.
Results
272 patients with neurological diagnosis were admitted to general ICU from June 2013 to July 2015 (mean 10.46 patients per month) and 658 neurological patients were admitted after we started neuro ICU, from August 2015 to December 2018 (mean 16.04 patients per month); which means a 53.34% improve in admissions. Mortality rate was 8.82% in general ICU and 8.05 in neuro ICU, while expected mortality from SAPS 3 was 15.10 and 24.25 respectively, showing greater severity among neuro ICU admitted patients. Mean length of stay was 4.07 days in general ICU and 6.74 days in neuro ICU, probably because of greater severity among neuro ICU patients. Other quality indicators also improved. Ventilator-associated pneumonia rate was 8.26 events/1000 days in general ICU and was 4.92 events/1000 days in neuro ICU. Blood stream infection due to central line rate was 5.41 in general ICU and 0.70 in neuro ICU. Urinary catheter related infection rate was 3.13 in general ICU and 1.21 in neuro ICU.
275
REDUCTION OF INTENSIVE CARE UNIT READMISSION RATE AFTER THE INTRODUCTION OF A SPECIFIC PROTOCOL
1Hospital Caxias Dor, Rio De Janeiro, Brazil
Introduction
Intensive care unit (ICU) early readmission is an important quality indicator widely used. Implementation of specific protocols may improve this indicator.
Methods
We started a protocol in order to reduce early readmission in our ICU in July 2016. In this paper, we compare ICU readmission rate before and after this protocol. The protocol included Fugulin score applied by nurse personal, in order to verify the patient dependency of care. Additionally we improved the communication process before ICU discharge, with a whatsapp group, including all ICU and ward doctors. In this group, ICU doctors summarize patients data before discharge, as well as ward doctors communicate patients data before readmit them to ICU, when necessary.
Results
3229 patients were admitted to ICU before the protocol, from June 2013 to July 2016; and 3200 patients were admitted after the protocol, from August 2016 to December 2018. Severity of diseases were similar, with SAPS 3 score 42.56 (+/− 15.29) before the protocol and 49.92 (+/− 18.86) after the protocol. Total readmission rate was 11.33% before and 8.64% after the protocol. Readmission before 24 hours was respectively 0.90% and 0.47%; and readmission before 48 hours were respectively 1.80 and 0.50. Mean length of stay in ICU was 5.29 days before the protocol and 5.85 days after the protocol. And the mortality rate was 8.81% before and 8.73% after the protocol.
277
A SINGLE DOSE OF FUROSEMIDE REDUCED RENAL MEDULLARY AND CORTICAL OXYGENATION IN HEALTHY SHEEP
1Osaka University Graduate School Of Medicine, Ibaraki-shi, Japan
2University of Melbourne, Melbourne, Australia
3Monash University, Melbourne, Australia
4Austin Hospital, Melbourne, Australia
Introduction
Furosemide, the most commonly used loop diuretic, reduces sodium transport in the ascending limb of the loop of Henle, which would be expected to increase renal medullary tissue oxygen tension (PO2). Considering the evidence that medullary hypoxia contributes to the development of acute kidney injury, furosemide may have beneficial effects on renal oxygenation. However, in healthy subjects furosemide has been shown to have harmful renal effects.
Methods
Studies were performed on eight conscious sheep, previously instrumented under general anaesthesia with a renal artery flow probe and fibre-optic probes to measure renal medullary and cortical perfusion and PO2. The renal vein was cannulated to determine renal oxygen delivery (RDO2) and consumption (RVO2). Intravenous furosemide (20 mg bolus) was given after baseline recording and measurements were continued for 8 h.
Results
By 3 h after bolus administration of furosemide, renal medullary and cortical PO2 significantly decreased (from 47 ± 5 to 31 ± 8 and 45 ± 5 to 10 ± 2 mmHg, respectively) (both p < 0.05) and returned to baseline levels by 8 h. Furosemide did not significantly alter renal blood flow (244 ± 19 to 247 ± 20 ml/min), medullary and cortical perfusion (1145 ± 227 to 1348 ± 257 and 1973 ± 268 to 2028 ± 290 blood perfusion units, respectively), RDO2 (29 ± 2 to 29 ± 2 mLO2/min) or RVO2 (3.4 ± 0.5 to 2.9 ± 0.3 mLO2/min). Furosemide caused transient increases in urine flow (74 ± 16 to 253 ± 15 mL/h, p < 0.01) and fractional excretion of sodium (0.7 ± 0.1 to 6.6 ± 0.5%, p < 0.001).
280
EFFECTS OF CARBON DIOXIDE LEVEL AND POSITIVE END EXPIRATORY PRESSURE ON INTRA-RENAL OXYGENATION AND PERFUSION IN SHEEP
1Osaka University Graduate School of Medicine, Suita, Japan
2University of Melbourne, Melbourne, Australia
3Saiseikai Senri Hospital, Suita, Japan
4Monash University, Melbourne, Australia
5Austin Hospital, Melbourne, Australia
Introduction
Acute kidney injury (AKI) is a prevalent complication of major surgery. There is compelling evidence that renal medullary hypoxia contributes to the pathogenesis of AKI. However, the effects of arterial carbon dioxide level and positive end expiratory pressure (PEEP) during general anaesthesia on intra-renal perfusion and oxygenation are unknown.
Methods
In Merino ewes, surgery was performed to implant pulmonary and renal artery flow probes and laser-Doppler and oxygen-sensing probes in the renal medulla and cortex. In anaesthetised sheep (isoflurane 2.5%), FiO2 was held at 0.4 and respiratory rate was changed to achieve target PaCO2 (normocapnia 35–45, mild hypercapnia 45–55 and severe hypercapnia 55–65 mmHg) for periods of 20 minutes, in random order. PEEP was held at (0, 5, 10, 15 and 20 cm H2O) for periods of 15 minutes during normocapnia and mild hypercapnia.
Results
Increases in PaCO2 from normocapnia, to mild and severe hypercapnia significantly increased medullary PO2 (39.1 ± 5.5, 48.6 ± 4.2 and 51.9 ± 4.8 mmHg, respectively) and perfusion (336 ± 66, 449 ± 72 and 453 ± 82 blood perfusion units (BPU), respectively). There were no changes in cortical perfusion or PO2, or renal blood flow (RBF). During normocapnia, PEEP decreased cardiac output (CO), RBF, medullary perfusion (342 ± 101 to 243 ± 64 BPU) and medullary PO2 (33.5 ± 5.4 to 22.6 ± 8.9 mmHg). Mild hypercapnia, for 30 min before and during PEEP, prevented the PEEP-induced decreases in medullary perfusion (to 491 ± 93 BPU) and PO2 (to 57.4 ± 7.6 mmHg).
281
UTILITY OF THE HOSPITAL FRAILTY RISK SCORE IN AN AUSTRALIAN HOSPITAL PATIENT COHORT
1St Vincent’s Hospital Melbourne, Fitzroy, Australia
Background
Frailty in a hospitalised patient is increasingly recognised as risk factor for long hospital stay and poorer clinical outcome and many frail patients are being referred for intensive care. The Hospital Frailty Risk Score uses administrative data to calculate a score which compares reasonably well with classical frailty scales.
Objective
To investigate the utility of the Hospital Frailty Risk Score (HFRS) in an Australian hospital population.
Methods
Retrospective cohort study of all patients discharged alive from St Vincent’s Hospital for the first time in 2010. The HFRS was calculated from the diagnostic codes (ICD-10AM) recorded during the index admission. The impact of HFRS on length of stay, discharge to locations other than home, and their medium term survival was assessed with logistic and poisson regression adjusting for demography, type of illness and comorbidity scores. Follow-up extended to 31 July 2018.
Results
The cohort comprised 25210 individuals median age 56.7 years (38.4–71.6 IQR), 53.4% male, 44.6% same day admissions. 20.4% had at least one Charlson comorbidity. Overall, 11.1% of the cohort were known to have died. Scores ≥5 (intermediate to high risk) were noted in 7.26%. Higher scores were associated with longer length of stay (relative risk ratio 1.093, 1.091–1.094 95% CI), discharge to locations other than home (odds ratio 1.170, 1.155–1.185 95% CI) and increased chance of mortality (odds ratio 1.04, 1.02–1.06 95% CI).
Conclusions
Hospital Frailty Risk Score can be estimated on Australian administrative data and higher scores are associated with worse outcomes. The HFRS provides a useful tool to estimate the prevalence of frailty within an inpatient service and provides a tool to monitor interventions to reduce the impact of frailty on patient outcomes.
283
PAEDIATRIC NATIONAL TRACHEOSTOMY SAFETY PROJECT-GLOBAL LAUNCH OF MULTIMEDIA EDUCATIONAL RESOURCES
1Royal Manchester Children’s Hospital, Macclesfield, United Kingdom
2University of Manchester, Manchester, UK
3Boston Childrens Hospital, Boston, USA
4Royal Melbourne Childrens Hospital, Melbourne, Australia
5Our Ladys Hospital for Sick Children, Dublin, Ireland
6Manchester University Hospitals NHS Foundation trust, Manchester, UK
Introduction
The national tracheostomy safety project (NTSP) is a multi-disciplinary group of healthcare professionals that aims to develop guidance and resources to improve the quality and safety of care. It is often difficult due to time and budgets to keep up to date. Accessing resources on social media platforms is inexpensive, always available and unrestricted by training budgets or work schedules.
Methods
20 families and 30 staff members interviewed. Open questions about what they would find useful in accessible resources. Concerns: skill retention in both basic/emergency care, budgets, time, decannulation and tube selection. Using competitive grant from the Health Foundation we commissioned a multimedia company FeedFirst, to design educational assets with a marketing campaign to target staff/carers with NTSP resources.
Results
The videos were planned by a multidisciplinary working party. Assets filmed over four days, using consenting staff and patients. The 25 films were split into basic care, emergency care, indications for tracheostomy, and parental support films. Disseminated via the GTC and ITC community and global feedback has been extremely positive supported by short “thumbs up” video clips. They were launched as a “global collaborative” at Royal Manchester Children’s’ Hospital May 24th with live streaming to Dublin, Boston and Melbourne.
285
20 YEAR AUDIT OF GLYCAEMIC CONTROL IN AN INTENSIVE CARE UNIT
1St Vincent’s Hospital Melbourne, Fitzroy, Australia
Introduction
Controversy remains as to the best target for blood glucose in critically ill patients. Studies of tight control (4.5–6.0) have shown conflicting results and recent studies suggest higher targets in diabetic patients.
Objectives
Assess measures of glycaemic control in critical care patients over 20 years spanning different clinical guidelines (tight control, less tight control, relaxed control).
Methods
The study was performed at a tertiary referral hospital with a single intensive care unit that has used a clinical information system for 25 years. All laboratory measurements of glucose between 1999 and 2019 were extracted. Linkage to patient information was available from 2004 onwards. Glycaemic control was measured during four 5-year time periods and consisted of mean glucose (central tendency), standard deviation and coefficient of variation of glucose (dispersion) and hypoglycaemic events <4.0 (percentage and rate/100 measurements). Results are expressed as median (interquartile range) and odds ratios (95%CI).
Results
Overall, 617978 samples were recorded.
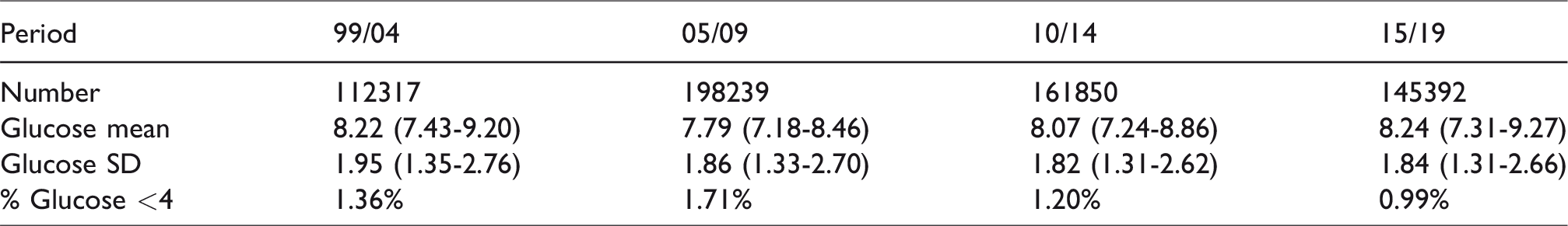
Since 2004, 19366 patients have been discharged: age 65 (52–74), 64% male, 26.7% diabetic, 11.5% mortality. One third had cardiac surgery. Odds ratios for mortality (adjusted for diabetes) were mean glucose 1.1 (1.07–1.12), glucose SD 1.17 (1.14–1.20) and rate of hypoglycaemia 1.04 (1.04–1.05).
Conclusions
Mean glucose levels tended to follow prevailing guidelines and are increasing whereas glucose variability has improved, and rates of hypoglycaemia continue to fall. Each metric (central tendency, dispersion and low events) is associated with an increased risk of mortality. All metrics should be assessed in future studies of glucose management.
286
REDUCTION IN HARM FROM PAEDIATRIC TRACHEOSTOMY SAFETY INCIDENTS FOLLOWING MULTIFACETED INTERVENTIONS OVER 10 YEARS: EXPERIENCE FROM A TERTIARY PAEDIATRIC HOSPITAL
1Royal Manchester Children’s Hospital, Macclesfield, United Kingdom
2University of Manchester, MANCHESTER, UK
3Manchester University Foundation NHS Trust, MANCHESTER, UK
Introduction
Paediatric patients with a tracheostomy are subject to morbidity and mortality as a result of pathology and tracheostomy-specific complications. Aim to improve safety and quality of care, by introducing resources of the Paediatric National Tracheostomy Safety Project.
• Weekly MDT 2016.
• GTC 2016.
• Improving Tracheostomy Care Project 2016.
• Mandatory tracheostomy annual BLS 2017.
• Monthly tracheostomy study days 2017.
• 2 tracheostomy champions/ward 2017.
• Change to Marpac tapes 2018.
• Central tracheostomy store cupboard £23,000 savings 2018.
• Risk stratification tool for post op care of new tracheostomies reducing critical care admissions 2018.
Methods
Previously demonstrated a significant and sustained reduction in harm 2010–2015. We have now looked at impact of interventions from 2015–2019 on harm data. Retrospective review of incidents 2016–2019. Anonymised reports analysed assessing harm, category, frequency.
Results
162 incidents. Exclusions: 31 incidents unrelated to tracheostomy patients; 49 ward staffing. 82 remained showing there was a significant trend towards reduction in harm (
287
IMPROVING THE QUALITY AND SAFETY OF PAEDIATRIC TRACHEOSTOMY CARE: IMPLEMENTATION OF A WEEKLY MULTIDISCIPLINARY WARD ROUND
1Royal Manchester Children’s Hospital, Macclesfield, United Kingdom
2University of Manchester, Manchester, UK
3Manchester University Foundation NHS Trust, Manchester, UK
Introduction
Globally there are considerable patient safety risks associated with children who have tracheostomies. (1). Within our institution, concerns were noted regarding the risk of serious avoidable tracheostomy morbidity. The Paediatric Working Party of National Tracheostomy Safety Project (NTSP) was established in 2014.
Methods
Incident data reviewed 2016–2019. Tracheostomy patients electronically tracked. The weekly MDT round includes Anaesthesia, ENT, SLT, Tracheostomy Nurses, Critical Care, physio. We review each patient and make a documented plan for the week. The team has developed a central tracheostomy store and a risk stratification tool for post operative care of new tracheostomies. We observed LOS, time to decannulation, use of one-way valves, routine admission to critical care and stoma issues.
Results
Further significant reductions in harm from 26% to 6% from reviewed incidents 2016–2019. Reduction in length of stay after a new tracheostomy excluding LTV cases to 24 days, reduction in admission to critical care after a new tracheostomy to <20%, earlier decannulation and earlier use of one way valve. The central store has reduced waste and saved which has saved £23,000.
290
TREM-1 GENETIC VARIABILITY DOES NOT INFLUENCE SEPSIS RISK AND OUTCOME
1Infectious Diseases Clinic, University of Medicine, Pharmacy, Science and Technology, Targu Mures, Romania
2Advanced Medical and Pharmaceutical Research Center, University of Medicine, Pharmacy, Science and Technology, Targu Mures, Romania
3Department of Genetics, University of Medicine, Pharmacy, Science and Technology, Targu Mures, Romania
4Department of Epidemiology, University of Medicine, Pharmacy, Science and Technology, Targu Mures, Romania
5Johns Hopkins School of Medicine, Baltimore, United States
6Department of Anesthesiology and Intensive Care, University of Medicine, Pharmacy, Science and Technology, Targu Mures, Romania
Introduction
Genetic variability in genes that mediate sepsis has been shown to influence sepsis susceptibility and outcomes, but the influence of specific polymorphisms is not well understood.
Methods
We performed a prospective study on 246 adult patients admitted to the ICU that met sepsis criteria at their admission. Based on the severity of the disease, they were assigned to 2 groups: sepsis patients (n = 146) and septic shock patients (n = 100); additionally, patients were assigned to either survivors (n = 61) or deceased (n = 185). Measurements were reported to a control group (n = 232). Plasma levels of TREM-1 were determined in the first 24 hours after sepsis diagnosis and participants in both study and control groups were genotyped for the rs2234246 and rs2234237 TREM-1 polymorphisms.
Results
Median TREM-1 values were significantly higher in patients with septic shock compared to septic patients (984.7 pg/mL vs 485.5 pg/mL, p < 0.0001), as well as in deceased versus survivors (684.8 pg/mL vs 440.4 pg/mL, p = 0.0048). No significant differences in genotype distributions of the two SNPs (CC/CT/TT of rs2234246; AA/AT/TT of rs2234237) were observed between any groups. AUC for TREM-1 was 0.621 (95%CI, 0.560–0.682), the cutoff value for mortality being 410.9 pg/mL with 80.43% (95%CI, 0.74–0.859) sensitivity and 48.33% (95%CI, 0.352–0.616) specificity. The OR for death is OR = 3.84 (95%CI = 2.06–7.17) for patients with TREM-1 values above the cutoff (n = 148, 80.4% of deceased).
293
INTENSIVE CARE UNIT BEREAVEMENT FOLLOW-UP: AN OVERVIEW OF THE FIRST YEAR OF SERVICE
1Addenbrooke’s Hospital, Cambridge, United Kingdom
2Royal Adelaide Hospital, Adelaide, Australia
3DonateLife South Australia, Adelaide, Australia
Introduction
Death in the intensive care unit (ICU) is common, often unexpected and can be associated with marked psychopathology among bereaved families. Good end-of-life (EOL) care is crucial.
Methods
This was a prospective, single-centre observational study, conducted in an Australian tertiary adult ICU. All deaths in the ICU were included and referrals made upon medical consensus on EOL care. After each patient’s death, the nominated family member received information about bereavement and details of the follow-up telephone interview. Calls were made at 4 weeks by trained clinicians, with questions based on a modified CAESAR Tool, evaluating the experience of patient and family around the EOL. Responses were recorded as Likert score (1, least satisfied, to 5, most satisfied) and qualitative feedback.
Results
From 1 February 2018 to 1 February 2019, 215 out of 241 ICU deaths were enrolled. 185 calls were finalized while the remainder 30 calls were still in progress. Of the 185 finalized calls, 109 (59%) families completed the follow-up interviews. Areas with median score of 5 (most satisfied) (IQR 5–5) were: support for family, attention to patient, maintaining patient’s dignity and quality of communications with nurses. The perceived pain control, quality of medical care, quality of communication with the doctors, opportunity to discuss patient’s wishes and say goodbye were given median score of 5 (IQR 4–5). The lowest median score, 4 (IQR 3–5) related to clarity of family being informed that patient was dying. Qualitative feedback indicated that humanization of patient was viewed positively, whilst ambiguity in communication and time away from patient were sources of dissatisfaction.
Conclusion
Bereavement follow-up in ICU is feasible and calls were well received. Overall EOL care was good but areas for improvement were identified, particularly in relation to communication.
294
THE IMPACT OF MEAN ARTERIAL PRESSURE CHANGES ON CEREBRAL AUTOREGULATION DURING SEPSIS
1Erasme University Hospital, Brussels, Belgium
Introduction
The Surviving Sepsis Campaign recommends targeting a mean arterial pressure (MAP) of at least 65 mm Hg during initial resuscitation of patients with septic shock. However, the impact of such MAP target on cerebral perfusion remains unknown.
Objective
To assess the effects of changes in MAP on cerebral autoregulation (CAR) in septic patients.
Methods
Prospective study of 39 patients with septic shock without intracranial disease severe arrhythmias treatment with extracorporeal membrane oxygenation or supra-aortic arteriopathy. MAP was progressively increased with a noradrenaline infusion at three levels: 70 ± 5 mmHg (low-target group), 80 ± 5 mmHg (middle-target group) and 90 ± 5 mmHg (high-target group). Transcranial Doppler (DWL, Germany) was performed at each target group, insonating the left middle cerebral artery with a 2MHz probe. The «blood flow velocity» and «arterial blood pressure» signals were simultaneously recorded for at least 6 minutes Pearsońs correlation coefficient between both signals (Mxa) was calculated using MATLAB (MathWorks, USA). Impaired CAR was defined as Mxa > 0.3.
Results
In the 39 patients (median age: 66 [53-73] years), actual MAP were 70 (range: 55–94), 78 (63–88) and 91 (80–103) mmHg in the low-, middle- and high-target group, respectively. At different time-points, mean Mxa was 0.29 (±0.34), 0.28 (±0.34) and 0.21 (±0.35), respectively (p = 0.48). In patients with intact CAR (n = 21), increasing MAP resulted in a significant increase of Mxa over time (ANOVA; p = 0.02), in particular from low- to middle-target levels (p = 0.01). In patients with altered CAR (n = 18), increasing MAP resulted in a significant decrease of Mxa over time (p = 0.002), in particular from low- to high-target levels (p = 0.006).
Conclusion
Targeting higher MAP in septic shock patients can improve cerebral autoregulation when it is altered at baseline.
297
A SINGLE CENTRE AUDIT COMPARING CITRATE AND NON-CITRATE DIALYSIS DOSE IN CRITICALLY ILL PATIENTS
1Princess Alexandra Hospital, Brisbane, Australia
Introduction
Current guidelines recommend a prescribed effluent dose of 25ml/kg/hr for critically ill patients requiring continuous renal replacement therapy (CRRT). At Princess Alexandra Hospital, Brisbane, the dose of dialysis delivered by the citrate protocol was largely determined by blood flow and the amount of citrated fluid required to anticoagulate the blood whilst a 2 litre exchange was usually prescribed in the non-citrate group.
Objectives
We performed an audit of CRRT comparing citrate and non-citrate dialysed patients. The primary outcome of interest was the adequacy of dialysis prescription with secondary outcomes including dose delivered and ICU outcomes.
Methods
We audited 97 patients who underwent CRRT between August 2017 and Sept 2018. Adequacy of dialysis prescription was defined as ≥25ml/kg/hr.
Results
The citrate group (n = 36) had a higher proportion of surgical patients and a lower illness severity (median APACHE III scores 83 vs 96, p = 0.004). In the citrate group 92% of the patients were prescribed a dose of 25ml/kg/hr and 62% were delivered this dose compared with 50% and 22% respectively in the non-citrate group. Over 45% of citrate dialysis patients were prescribed a dose greater than 40ml/kg/hr. The citrate group had a higher median ICU length of stay (10.5 versus 5 days, p = 0.02) but a lower hospital mortality (28% vs 48%, p = 0.055). The average cost of dialysis fluid in the citrate group was $4281 per patient ($31.1/hr) compared to $1038 ($11.6/hr) in the non-citrate group.
Conclusion
The current protocol for non-citrate CRRT led to inadequate dialysis dose prescription in half of patients whilst the citrate protocol delivered higher volumes of dialysis than necessary with its associated cost and nursing resource implications.
300
HETEROGENEITY IN BURNS MANAGEMENT. A RETROSPECTIVE REVIEW OF FOUR YEARS OF INTENSIVE CARE ADMISSIONS TO A QUATERNARY BURNS UNIT
1The Royal Brisbane And Women’s Hospital, Hendra, Australia
2The Prince Charles Hospital, Chermside, Australia
Introduction
A review of the demographics of admissions and care delivered to one hundred and fifty-three patients admitted over four years (2015–2018) to a quaternary burns unit.
Methods
Ethically approved retrospective chart review of all patients admitted to intensive care with a primary diagnosis of a burn.
Results
One Hundred and Fifty-three patients were admitted over four years 76% were male, 24% female. The admission rate fell in the last two years p = <0.001. An accidental mechanism was recorded for 116 (71%) whilst 47(29%) resulted from self harm. Twenty-four patients died (mortality rate 12.8%) with mortality associated with an act of self harm (p = 0.0013), a parkland calculation greater than twenty liters (p = <0.05), age >80 years, female gender, a TBSA >80%, a low pH and Hypothermia on linear regression models.
A documented Parklands Calculation on the first day fell from 66% in 2015 to 38% 2018 (p = 0.00133). Still 66% of patients received more fluid than a calculated Parklands in 2015, rising to 93% in 2018 (p = 0.00005). Predominantly patients were primarily resuscitated with Hartmanns however there were six different fluid resuscitation regimens used. There were 21 different sedation/analgesic regimens commenced on admission ranging from one to five agents. Eighty-two percent had a benzodiazepine infusion on admission (2015) which fell to 70% 2018 p = 0.025. Conversely discharge prescribing of Benzodiazepines increased from 13.8% (2015) to 44% (2018) p = 0.0003. For serial debridement’s patients received eight times the analgesic dose in their second debridement to their first (p = 0.0085). There was significant variation in discharge prescribing of analgesics and antipsychotics.
308
HAEMODYNAMIC RESPONSE TO FLUID BOLUSES IN CHILDREN IN INTENSIVE CARE OCCURS AND DISSIPATES RAPIDLY
1Royal Children’s Hospital, Melbourne, Australia
2Murdoch Children’s Research Institute, Melbourne, Australia
3University of Melbourne, Melbourne, Australia
4Austin Hospital, Melbourne, Australia
Introduction
Fluid boluses (FB) are a ubiquitous therapy in critically unwell children. The haemodynamic response to FB in children in intensive care is not well described.
Objectives
We sought to describe the minutely haemodynamic response to FB in children in a paediatric intensive care unit (PICU). We also aimed to assess the effect of FB duration on haemodynamic response.
Methods
We conducted a prospective, observational study of FB in children in the PICU, Royal Children’s Hospital, Melbourne. Administration of FBs were at the clinician’s discretion. Minutely haemodynamic data were collected from bedside monitors (Phillips Intellivue, Amsterdam, The Netherlands). Mean Arterial Pressure responsiveness (MAPr) was defined as a 10% increase in MAP from baseline and dissipation as a subsequent fall below this level. FB were compared for MAPr based on duration (≤10 vs >10 minutes).
Results
One hundred FBs were observed in 65 children; predominantly following cardiac surgery (50/65(77%)). The median age was 267 days [IQR:12,2251]. The median FB volume and duration was 5.0ml/kg [IQR:4.8; 5.6] and 12 minutes [5; 27] respectively. Fluid composition was 4% albumin in 57/100(57%). Main indications were hypotension(75%) and low filling pressure(45%). MAPr occurred in 56/100(56%) of FB at a median time of 6 minutes [IQR:4,12]. Dissipation occurred in 36/56(64%) of responders at a median time of 5 minutes [IQR:2,12]. Fluid boluses administered for hypotension had a shorter duration (10minutes [IQR:4;23] vs 25[IQR:8;29];p < 0.02) and more commonly had a MAPr; 50/75(66%) vs 6/25(24%);P < 0.001. There was no difference in MAPr based on FB duration; (≤ 10 mins 29/48(60%) vs >10 minutes 27/52(52%) p = 0.39). After adjustment for age and FB volume, FB duration was not significantly associated with a change in MAP; coeff = −0.22(95%CI;-0.46,0.02; p = 0.07).
309
GENDER DIFFERENCES IN ICU ADMISSIONS IN AUSTRALIA AND NEW ZEALAND
1Austin Health, Heidelberg, Australia
2ANZIC-RC, Australia
3Alfred Health, Melbourne, Australia
4Public and Preventative Medicine, Monash University, Australia
5Department of Critical Care, University of Melbourne, Australia
Introduction
Fewer women than men are admitted to intensive care units (ICU) worldwide: between 38% and 45% of all ICU patients are women.
Objectives
To quantify the relative contribution of each major diagnostic category to the overall proportion of women admitted to ICU in Australia and New Zealand. Additionally, to describe how the gender balance varied over time, with patient age, and between regions.
Methods
Retrospective review of ICU admissions in the ANZICS Adult Patient Database between 2005 and 2018. Multivariate logistic regression considered the explanatory variables APACHE III-J diagnostic category, patient age, admission year, geographic region and hospital type.
Results
42.3% of 1,616,856 ICU patients were women. There were 247,988 more men than women.
A gender imbalance was observed across most diagnostic categories, with less than 48% women in 12 of 20 diagnostic categories and greater than 52% women in 3 categories (p < 0.001). Admissions following cardiovascular surgery accounted for over half of the overall preponderance of men. After removing cardiovascular operative admissions, women comprised 45.7% of remaining patients.
The percentage of ICU patients who are women is steadily increasing, from 40.8% in 2005 to 43.6% in 2018. The percentage of women was higher among younger patients aged under 50 (47.7%) than patients aged 50 and over (40.6%, p < 0.001).
In multivariate analysis, the factors most predictive of ICU patient being a man were:.
• trauma diagnosis.
• non operative OR 3.18, (95% CI 2.69–3.74).
• operative OR 2.41 (95% CI 2.04- 2.85).
• cardiovascular operative diagnosis OR 2.51 (95% CI 2.13–2.96).
• respiratory operative diagnoses OR 1.61 (95% CI 1.37–1.9).
• Age 60 to <70 years old OR 1.49 (95% CI 1.47–1.51).
Conclusion
A gender imbalance across most diagnostic categories of ICU admission. Cardiovascular and trauma admissions contribute most to the observed preponderance of men. The proportion of female ICU patients is steadily increasing.
310
ADDITIONAL VALUE OF LABORATORY RESULTS FOR A MACHINE LEARNING ALGORITHM TO PREDICT IN-HOSPITAL CARDIAC ARREST: A SINGLE-CENTRE RETROSPECTIVE COHORT STUDY
1Frankston Hospital, Frankston, Australia
2Kameda Medical Center, Kamogawa, Japan
3Austin Hospital, Heidelberg, Australia
4Australian and New Zealand Intensive Care Research Centre, School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia
5The Alfred, Prahran, Australia
6The University of Tokyo, Chiyoda-ku, Japan
Introduction
In-hospital cardiac arrest (IHCA) is a global burden and associated with poor outcome. Machine learning techniques can facilitate development of simple prediction models which identify patients at risk of IHCA.
318
REQUIREMENT FOR ONGOING ORGAN SUPPORT IN PATIENTS WITH PERSISTENT CRITICAL ILLNESS IS ASSOCIATED WITH POOR OUTCOME
1St Vincent’s Hospital, Sydney, Australia
2University of New South Wales, Sydney, Australia
Introduction
Persistent critical illness is associated with significant prognostic uncertainty while carrying an enormous burden for patients, their families, and healthcare providers. It has been demonstrated that, as ICU stay progresses, diagnostic category and severity of illness scores on admission become less predictive of outcomes than antecedent characteristics such as age and chronic health status. The role of specific organ support interventions in persistent critical illness remains ill-defined.
Methods
Demographic data, illness severity parameters, details of organ support and 30-day post-hospital discharge mortality were collected in adult patients admitted to a mixed ICU in a tertiary university-affiliated centre for ≥28 days between 2012 and 2018.
Results
During the study period, 8328 patients were admitted to the ICU, of whom 81 (1%) stayed ≥28 days and met inclusion criteria. This group had a median (interquartile range, IQR) age of 49 (IQR 39–59) years and APACHE III score of 67 (IQR 57–80). 70% of these patients required organ support on day 28. Overall, 30-day post-hospital mortality was 22% (30% for those requiring organ support versus 4% for those who did not [P = 0.03]).
On multivariate analysis, age (OR 1.1, CI 1–1.11) and a requirement for more than one organ support (OR 17.2, CI 1.6 – 185.9 for two organ support modalities, OR 58.9, CI 3.5 – 995.4 for three organ support modalities) were independently associated with 30-day post-hospital discharge mortality. The association with APACHE III score, and admission diagnosis was not found to be significant.
Conclusion
Presence of organ support and the number of modalities required were, independently of acute and antecedent factors, associated with early post-hospital mortality.
319
A LUNG COMPARTMENT MODEL BASED ON RESPIRATORY DYNAMICS OBTAINED THROUGH THE LUNG COMPLIANCE MODEL
1Jeju National University Hospital, Jeju National University School of Medicine, Jeju, South Korea
Introduction
Inhalation anesthetics have long been used in the field of anesthesia, and they are one of the most familiar and easy-to-use drugs for anesthesiologists. However, the mechanisms of action of these inhalation anesthetics in the lungs remain unclear.
Methods
Lung models were designed to simulate one lung and two lungs. The lung model was composed of one or two test lungs, and the compliance was changed variously using a rubber band. Respiratory variables were measured with the model trachea by using spirometry. The lung model was mechanically ventilated, and the airway internal diameter was changed to reflect the degree of airway obstruction.
Results
The change in compliance did not show a significant effect on the dynamic compliance of the one-compartment model until it reached a specific resistance value (internal diameter 5.5 mm). On the other hand, the increase in the resistance of one side of the lung affected the opposite side of the lung and did not change the measured value in the trachea.
Conclusion
The compartment model (which can be simulated) can be used to explain the effects of respiratory dynamic variables on both the lungs.
323
SURVIVORS OF INTENSIVE CARE WITH TYPE 2 DIABETES AND THE EFFECT OF SHARED CARE FOLLOW-UP CLINICS: THE SWEET-AS FEASIBILITY STUDY
1Intensive Care Unit, Royal Melbourne Hospital, Parkville, Australia
2Discipline of Acute Care Medicine, University of Adelaide, Adelaide, Australia
3Department of Medicine and Radiology, University of Melbourne, Parkville, Australia
4Endocrine and Metabolic Service, Royal Adelaide Hospital, Adelaide, Australia
5Discipline of Medicine, University of Adelaide, Adelaide, Australia
6Intensive Care Unit, Royal Adelaide Hospital, Adelaide, Australia
Introduction
There are no data to support the use of Intensive Care Unit (ICU) follow-up clinics. This is potentially because existing studies have evaluated heterogeneous cohorts and utilised physicians who are not trained in ambulatory care.
Methods
This was a prospective, randomised, single-centre study with blinded assessment. After informed consent, participants were randomised to shared-care clinic one month after discharge or usual care. Six months after discharge, all participants were assessed for glycated haemoglobin, neuropathy, nephropathy, quality of life (QOL), frailty and healthcare utilisation. The primary outcome was recruitment and retention at 6 months. Data are mean (SD) and differences between groups were analysed using Student t-tests.
Results
42 of 82 (51%) eligible patients (age 66 (10) years) were recruited over the 18-month study period. Patients declining to participate most often reported competing medical appointments. 11/42 (26%) patients died after hospital discharge but before 6 months. 16/21 (76%) participants allocated to the intervention attended the clinic. Complete 6-month outcome data were available for 26 patients (62%). There was no difference in QOL scores between intervention and control groups [Short Form-36 physical summary score: 32 (9) vs. 32 (7), P = 0.997]. Only 12/42 (29%) were alive and living independently without supports and 24/42 (57%) required at least one hospital admission in addition to the index admission.
327
DATATHON MODEL: THE AUSTRALIAN EXPERIENCE
1Intensive Care Unit, Austin Health, Heidelberg, Australia
2Intensive Care Unit, Bendigo Health, Bendigo, Australia
3Monash Rural Health, Bendigo, Australia
4Monash University Clinical Skills and Simulation Centre, Bendigo, Australia
5Heath and Bioinformatics Centre University of Melbourne, Melbourne, Australia
6Institute for Medical Engineering and Science, Massachusetts Institute of Technology, Cambridge, USA
7Patient Care Analytics Philips Healthcare, Baltimore, USA
8Department of Pharmacy Practice and Science, University of Maryland School of Pharmacy, Baltimore, USA
9The Australian and New Zealand Intensive Care Society Centre for Outcome and Resources Evaluation, Camberwell, Australia
10The Australian and New Zealand Intensive Care Research Centre School of Public Health and Preventative Medicine Monash University, Prahran, Australia
11Wellington Public Hospital, Wellington, New Zealand
12Quality Improvement and Patient Safety, Capital and Coast District Health Board, New Zealand
13Laboratory for Computational Physiology, Massachusetts Institute of Technology, Cambridge, USA
14Department of Intensive Care, Alfred Health, Prahran, Australia
15Research and Innovation, Bendigo Health, Bendigo, Australia
Introduction
The utility of large clinical datasets is increasingly recognised in intensive care research. Advantages include access to high volume data-points from an environment that reflects true practice. To navigate the complexity of these data, inform quality improvement and test clinical hypotheses, a multi-disciplinary approach is essential. One method of achieving this is the ‘Datathon’. Together with the Australian and New Zealand Intensive Care Society (ANZICS) Centre for Outcome and Resource Evaluation, clinician researchers and data scientists from Massachusetts Institute of Technology, we introduced a multi-disciplinary Datathon model into Australia.
Methods
Datathons were planned by multi-disciplinary teams including senior and junior clinicians, researchers, data scientists, administrators and data custodians as well as representatives from technology platforms and universities. Planning covered key areas of sponsorship, logistics, technical factors, ethics requirements, confidentiality and data privacy. Datathon impact was measured by numbers of participants and teams, participant satisfaction, subsequent presentations at scientific meetings and publications, and through senior health sector engagement.
Results
Three critical care Datathons took place in Australia over 2017 and 2018; all free to attend. Participants had access to datasets including ANZICS, MIMIC-3, Philips eICU and Victorian administrative data. 352 participants formed 52 teams working over a weekend to formulate research plans, extract and analyse data, before concluding with brief oral presentations of key findings. Participant feedback showed high levels of satisfaction. Nineteen projects have been presented at conferences with 12 submitted or published in peer-reviewed journals indicating collaborative partnerships extending beyond the datathon. The events led to the creation of bi-national research collaborations to investigate obstetric and indigenous critical care outcomes.
329
CHANGING FROM A 32–34°C TO 36° TARGETED TEMPERATURE MANAGEMENT PROTOCOL IS ASSOCIATED WITH INCREASED COMPLIANCE WITH TARGET TEMPERATURES
1Melbourne Medical School, The University of Melbourne, Parkville, Australia
2Department of Critical Care Medicine, St Vincent’s Hospital Melbourne, Fitzroy, Australia
Introduction
Targeted temperature management (TTM) is proven to improve survival and neurological outcome in post cardiac arrest patients. In 2013, a landmark trial demonstrated no difference in outcomes when managing patients with TTM at 36°C compared to the previous standard of 33°C. Consequently, many critical care units have adopted a 36°C TTM protocol.
Methods
We conducted a retrospective cohort study of post cardiac arrest patients admitted to the Intensive Care Unit of an Australian tertiary referral hospital. The two cohorts were separated by time, the first group managed with a 32–34°C TTM protocol (2010–2013) and the second group managed with a 36°C TTM protocol (2015–2019). We compared compliance with target temperatures and patient outcomes, between these two groups. Patients undergoing active cooling and out-of-hospital cardiac arrest patients were analyzed as subgroups.
Results
The study comprised 335 patients (156 before and 179 after the protocol change). Patient demographics and arrest characteristics were similar between the two groups. After the protocol change a lower proportion of temperature recordings breached temperature targets in the first 24 hours post arrest (55.4% vs 17.4% p < 0.05) and breached 37.5°C between 24–72 hours post arrest (30.6% vs 15.9% p = 0.005). There was no significant difference in rates of fever between the groups. Interrupted time series analysis showed continuous improvement in compliance rates over time across both protocols. There was no significant difference in patient outcomes between the two groups, with similar numbers of patients being discharged with a good neurological outcome and surviving to discharge.
334
PROCESS MEASURES RELATED TO THE TREATMENT OF INFECTIONS IN INTENSIVE CARE AND THEIR ASSOCIATION WITH HOSPITAL MORTALITY
1The Department of Intensive Care, Alfred Health, Melbourne, Prahran, Australia
2The Australian and New Zealand Intensive Care Society (ANZICS) Centre for Outcome and Resources Evaluation, Melbourne, Camberwell, Australia
3The Australian and New Zealand Intensive Care Research Centre, School of Public Health and Preventive Medicine, Monash University, Melbourne, Prahran, Australia
4Safer Care Victoria, Melbourne, Australia
5Fiona Stanley Hospital, Intensivist and Director of ICU Research, Perth, Australia
Introduction
Intensive care unit (ICU) antibiograms, routine rounds by Infectious diseases (ID) specialists and antibiotic stewardship programs are aimed at improving patient care. Their impact on patient centred outcomes in Australian and New Zealand ICUs is uncertain.
Methods
The Australian and New Zealand Intensive Care Society Adult Patient Database and Critical Care Resources registries were used to extract patient-level factors including illness severity, ventilation status, length of stay and in-hospital mortality. ICU-level factors included type and location of hospital, and the year in which the process of care intervention took place. Descriptive statistics and mixed effects logistic regression were used to determine the relationship between the three process measures and in-hospital mortality.
Results
The study included 799,901 adults admitted to 171 ICUs from July 2009 to June 2016.
The number of patients admitted to an ICU where antibiograms, ID rounds and antibiotic stewardship occurred were 301,346 patients (38.7%), 584,212 patients (74.0%) and 606,695 (77.5%) respectively. In-hospital mortality of patients in ICUs conducting these three processes compared to ICUs that weren’t was 8.9% vs. 8.7%, 9.7% vs. 6.4% and 9.2% vs. 7.5% respectively (P < 0.001).
After adjusting for confounders, the use of ICU specific antibiograms was associated with a reduction in hospital mortality (OR 0.96 {95%CI 0.93–0.98} P 0.002). This finding persisted in multiple sensitivity analyses. There was no overall correlation between the two other processes of care and in-hospital mortality.
335
EFFICACY OF MEROPENEM-EDTA COMPARED WITH MEROPENEM IN TREATMENT OF COMPLICATED URINARY TRACT INFECTIONS-ROLE OF ANTIBIOTIC RESISTANCE BREAKER
1Apollo Hospital, Bhubaneswar, India
Introduction
Multidrug resistance gram-negative infection is a big challenge globally in most of the Critically ill patients. With not much of newer antibiotics options left in the horizon, different therapeutic strategies that could be employed in conjunction with antibiotics to increase the effectiveness of these life saving drugs. Antibiotic resistance breakers are compounds which may not have any antibacterial effect of its own, but can increase the effectiveness of antibiotics by combating the resistance mechanisms employed against them.
Methods
This was a retrospective observational analysis of outcome measures in patients treated with meropenem EDTA for complicated UTI compared with similar group of patients treated with meropenem. Over a study period of 6 months 50 patients treated in each cohort was analyzed. The primary end point was composite cure rate (clinical response and bacterial eradication). Clinical and microbiological outcomes were assessed in both the cohorts across 2 study point (End of treatment [EOT] and Test of cure [TOC]).
Results
Out of 100 cases analyzed, primary endpoint (TOC visit), the composite cure rate was higher in Meropenem EDTA treatment arm compared to Meropenem arm i.e. 85% (42/50) vs 78% (39/50) (treatment difference 12.6%; 95% CI: 5.9% to 26.4%). The clinical cure rate observed in Meropenem EDTA arm was 87% (43/50) compared to 80% (40/50) in Meropenem arm at EOT visit (treatment difference 7.01%; 95% CI: 2.99% to 17.3%).
336
DIAGNOSTIC ACCURACY OF CSF PRESEPSIN FOR SUSPECTED NOSOCOMIAL BACTERIAL MENINGITIS IN NEUROSURGICAL PATIENTS
1Apollo Hospital, Bhubaneswar, India
Introduction
External ventricular drainage (EVD) used in intensive care unit for variety of neurosurgical conditions; which also kept over 3–5 days to achieve therapeutic goals. Like all invasive catheters, there is an increased risk of infection leading to meningitis, but blood contaminated CSF makes biochemical tests unreliable in diagnosing infection.
Methods
We conducted a prospective study of 80 episodes of suspected bacterial meningitis in 66 patients having EVD placed for different reasons. CSF samples were examined from the EVD site with all aseptic precautions. Parameters measured were Presepsin in CSF along with cell count, differential count, glucose, protein.CSF was also taken for culture in microbiological lab along with BIOFIRE® FILMARRAY® Multiplex Real-Time PCR Systems examining various bacterial,viral and fungal causes of meningitis.
Results
Infection was microbiologically confirmed in 48(60%) out of 80 suspected cases. Diagnostic accuracies presented as area under the curve for presepsin, leukocytes, and proteins measured in CSF were 0.905 (95% confidence interval [CI], 0.853 to 0.961), 0.738 (95% CI, 0.657 to 0.820), and 0.657 (95% CI, 0.549 to 0.764), respectively. Sensitivity and Specificity were 91.2% and 85.1% for presepsin and 65.4% and 62.3% for leukocytes in CSF. There were 37 culture positive samples for meningitis along with 43 cases came positive with Filmarray PCR systems.
337
Etiology, Clinical profile and Outcome of ARDS patients in Eastern Nepal
1Birat Medical College And Teaching Hospital, Biratnagar, Nepal
Introduction
Adult Respiratory Distress Syndrome is an inflammatory disease of lungs characterized by acute onset of refractory hypoxia, bilateral chest infiltrates with significant morbidity and mortality. The etiology and prognostic factors for the disease may be different in the tropical areas. We aimed to study the etiology, clinical characteristics and outcome of patients with ARDS.
Results
The mean age of our cohort was 38.15 years with male predominance. Majority of the patients presented with shortness of breath and fever. 40.6% of patients had mild ARDS as compared to 23.2% as severe ARDS. Similarly, initial SOFA scoring was 8.56 with majority of patients had lung injury score less than 2.5. Pneumonia was the most common etiology followed by sepsis syndrome and tropical infections. 61.6% of patients had different organ dysfunction. The patients requiring invasive ventilation had significantly poor ventilator parameters (P < 0.05). The overall mortality in our study was 41.8%.
Conclusion
Pneumonia was the most common cause of ARDS in our set up. The Pa02/FiO2, lung injury score, non-respiratory organ failure and infectious etiology had significant influence on the mortality of ARDS patients.
339
CENTRAL VENOUS OXYGEN SATURATION IS CORRELATED WITH AN INCREASE IN SKIN BLOOD FLOW AFTER TRANSFUSION
1Erasme Hospital, Brussels, Belgium
Introduction
Red blood cell transfusion (RBCT) increases tissue oxygen delivery (DO2) and may improve microcirculation. However, the effects on blood flow have been found to be inconsistent.
Methods
We studied ICU patients with stable hemodynamic status (mean arterial pressure (MAP) ≥65 mmHg for at least 6 hours) and without active bleeding, who received a RBCT. Skin blood flow (SBF) was determined (Periflux System 5000, Perimed, index finger; perfusion unit, PU) together with MAP, heart rate (HR), hemoglobin (Hb), lactate levels and ScvO2 before and after RBCT. SBF was measured before RBCT (T0) and after (T1) for each 3 min. According to previous data indicating the lowest SBF value founded in non-infected ICU patients was 151 PU, all patients were analyzed according to the baseline SBF (i.e. <151 PU – low SBF vs. ≥151 PU – high SBF). The relative change of SBF (ΔSBF) was calculated after RBCT and the responders were defined by the function of >10%.
Results
54 ICU patients were studied. RBCT was associated with increases in MAP and ScvO2 but no change in SBF. At baseline, ScvO2 was lower in the responders than in the non-responders (p = 0.03) and somewhat lower in patients with low SBF than in the high SBF (p = 0.05). There was no difference in Hb, MAP, and lactate, between the patients with low and high SBF. After RBCT, MAP (p = 0.004) and SBF (p = 0.001) rose only in patients with low SBF. There was a negative correlation between baseline ScvO2 (r = -0.402, p = 0.003) or baseline SBF (r = -0.611, p < 0.01) and the relative increase in SBF after RBCT.
341
INTENSIVE CARE THERAPY IN CHILDREN FOLLOWING A MEDICAL EMERGENCY TEAM EVENT
1Royal Children’s Hospital, Melbourne, Australia
2Murdoch Children’s Research Institute, Melbourne, Australia
3University of Melbourne, Melbourne, Australia
Introduction
Medical emergency teams (MET) reduce cardiorespiratory arrest and death in hospitalized children. Risk factors for intensive care support following a MET are less well understood.
Objectives
To describe the characteristics and outcomes of children following a MET event; specifically the need for intensive care therapy (ICT) in a quaternary paediatric hospital.
Methods
We conducted a retrospective study of children who received a MET event at the Royal Children’s Hospital from July 2017 to March 2019. MET characteristics were recorded electronically by intensive care staff immediately following the MET. We defined ICT as positive pressure ventilation or vasoactive support in the paediatric intensive care unit (PICU) within 12 hours of the MET event. Its association with age, time of day and previously defined significant event were examined.
Results
There were 891 MET events in 567 patients over 632 admissions. The median age was 2.4 years (IQR[0.53, 9.9]). Seventy percent of MET events occurred after hours. Common reasons for a MET were desaturation (33%), tachypnoea (26%) and staff concern (26%). Respiratory infections/conditions, congenital heart disease and seizures were the most common hospital admission diagnoses; 25%, 21% and 11%, respectively. PICU admission followed 183(21%) MET events, of which 76(9%) required ICT. The predicted probability of ICT in children <1 year old was 0.13(95%CI[0.10, 0.17]), approximately twice that of older children; 1–5 years 0.07(95%CI[0.04, 0.10]), >5 years 0.05(95%CI[0.03, 0.08]). A significant event increased the risk of ICT by 15% (95%CI[5.3%, 25%], p = 0.002) compared to no significant event (7.2%). The proportion requiring ICT for MET in and out of hours was similar; 22/265(8%) and 54/626(9%), respectively. The risk difference for PICU mortality in those requiring ICT vs not was 9.5% (95%CI[2.4%, 17%], p = 0.009).
344
HIGH VENOUS-TO-ARTERIAL CARBON DIOXIDE DIFFERENCE ASSOCIATED WITH LOW CARDIAC INDEX DURING RESUSCITATION: SYSTEMATIC REVIEW AND META-ANALYSIS
1Peking Union Medical College Hospital, Beijing, China
Introduction
Although septic shock is usually a hyperdynamic state, patients may also present impaired cardiac function, which can influence CO2 production and elimination. Recent reports have shown venous hypercarbia, resulting in a widening of venous-to-arterial carbon dioxide difference (Pv-aCO2) is related to systemic hypoperfusion. Proper way to evaluate tissue perfusion when resuscitate patients is crucial.
Methods
We systematically reviewed observational cohort studies published from January 1966 to May 2019, retrieved from Pubmed, Embase and Cochrane Library. The search yielded a total of 1516 articles, of which 1492 were excluded on the basis of the title and summary. 8 articles, involving 454 adult patients with severe sepsis or septic shock, both Pv-aCO2 and CI recorded during the 24h of resuscitation were meta-analysed.
Results
Level of Pv-aCO2 lower than 6mmHg were associated with increased CI (mean difference (MD) -0.78, 95% (confidence interval (CI) -0.9 to -0.67), P < 0.00001).
348
EVALUATION OF CALLING CRITERIA FOR THE RAPID RESPONSE SYSTEM UTILISING SINGLE VERSUS MULTIPLE PHYSIOLOGICAL PARAMETER DISTURBANCES
1Department Of Health WA, Rivervale, Australia
Introduction
The Adult Deterioration Detection System (ADDS) for Medical Emergency Team (MET) activation is widely used and includes single parameter disturbance (SP-MET) and multiple parameter disturbances (MP-MET). Whether the patient characteristics, interventions and outcomes differ for SP-MET compared with MP-MET is uncertain.
Aim
To describe the patient characteristics, interventions and outcomes associated with single versus multiple parameters MET activation in the Acute Medical Unit (AMU) of a tertiary care hospital in Perth Western Australia.
Methods
Retrospective audit of MET calls over six months in 2017. SP-MET and MP-MET groups were compared.
Results
SP-METs constituted 65% (171) of 265 MET calls initiated in AMU, most commonly for hypotension (36%) and tachycardia (14%). Resuscitation status was documented in 55 patients (20.75%) prior to the MET activation. There was no significant difference between patient’s demographic and disease characteristics between the SP and the MP-MET groups. Common interventions included fluid and electrolyte replacement in 139 (52%), oxygen therapy in 46 (17.35%), and non-invasive ventilation in 33 (12.5%) patients. After MET intervention, 83% patients stayed on the ward, 8.3% either died or were palliated, 6% were transferred to the ICU, and 2.6% patients required urgent transfer to the theatre for cardiology, gastroenterology, or surgical intervention. End of life care was initiated in 14 (5.24%) patients by the MET. SP-METs were more likely to receive ward-based interventions (OR 3.62; 95% CI 2.01–6.57; p-value <0.0001), remain on the ward after the MET (OR 3.22; 95% CI 1.68–6.19; p-value 0.0004), and had lower risk of death or palliation (OR 4.45; 95% CI 1.74–11.34; p-value 0.0018).
Conclusion
SP-METs identifies a cohort of patients at lower risk of requiring escalation of care and ICU admission. Given the resource intensity of MET activation, further research is warranted to determine whether alternative response strategies are appropriate for selected single parameter disturbances.
350
THIS IS HOW WE TAKE PATIENTS OUTDOORS: “MEANINGFUL INTERACTIONS” WITH FAMILY FOR EARLY MOBILISATION
1Department of Critical Care Medicine, Nagoya City West Medical Center, Nagoya, Japan
2Department of Anesthesia, Nagoya City West Medical Center, Nagoya, Japan
3Department of Rehabilitation, Nagoya West City Medical Center, Nagoya, Japan
Introduction
Post-intensive care syndrome greatly affects patients’ and their families’ QOLs after discharge. To minimize the symptoms, the ABCDEF bundle was implemented. Early mobilization and family engagement are very important for better outcomes of critically ill patients. We implemented “outdoor stroll” activity as an early rehabilitative intervention for ICU patients. We select the type of wheelchair to use based on how the patient performed while sitting on the edge of the bed the previous day. At least, one physician, 2 nurses, 2 physical therapists, and a clinical engineer accompany the patient outside. We also encourage the patients’ families to participate in the activity when possible.
Methods
We retrospectively investigated the cases of critically ill patients who sat in a wheel chair in our ICU for early rehabilitation between January 2015 and May 2019. We defined “critically ill” as being on a ventilator for ≧3 days.
Results
There were 82 critically ill patients. 62 patients, of whom the average SOFA score was 10.7, sat in a wheelchair. The median day for the patients to sit on the edge of the bed was day 3, and to sit in a wheelchair was day 4. 43 patients (69%) went for a stroll outdoors, 20 of which went with family members. No unscheduled extubation or accidental removal of vascular access occurred, and no severe deterioration of vital signs was observed.
351
The incidence and outcome of patients admitted with sepsis to an ICU in a Middle Income Country
1Department of Intensive Care, Oshakati, Namibia
Introduction
The highest burden of sepsis occurs in low- and middle-income countries (LMIC), but nearly all research on both the epidemiology of sepsis and optimal treatment come from high-income countries (HIC). Assuming that adopting guidelines developed in HIC will lead to better outcomes in LMIC has been shown to be ill-advised. LMIC face many challenges in managing critically ill septic patients and the first step to improve care is to collect data on the incidence and outcome of these patients.
Methods
Single center, retrospective, observational cohort study over a 12 month period. The following information will be collected; age, sex, diagnosis, outcome, department and nature of admission (elective vs emergency), nationality. Local research committee and hospital management approval will be obtained. No external funding has been received for the study, and the authors have no conflicts of interest.
Results
There were 341 admissions of whom 51 had sepsis (15%). A total of 24 septic patients died giving a crude ICU mortality of about 50%.
353
LONG-TERM SURVIVAL AFTER DISCHARGE FROM PUBLIC INTENSIVE CARE UNITS IN VICTORIA
1Alfred Health, Commercial Road, Prahran 3004, Australia
2ANZICS Centre for Outcome and Resource Evaluation, Camberwell 3124, Australia
3Safer Care Victoria, Melbourne 3000, Australia
4The ANZIC-Research Centre, Monash University, St Kilda Road 3004, Australia
5St. Vincent’s Hospital, Fitzroy 3065, Australia
6Department of Intensive Care, Eastern Health, Box Hill, Australia
Background
Long-term survival after an index admission to an Intensive Care Unit (ICU) is rarely reported except in small studies examining specific subgroups. More comprehensive estimates of survival require linkage of clinical, administrative, and death registries.
Objective
To identify determinants of long-term survival after discharge alive from ICU.
Results
Of 228,912 adult ICU admissions reported to ANZICS, 183,635 (80.2%) were matched. 15,931 (8.7%) died in hospital during their index admission, leaving 167,704 ICU admissions involving 136,954 patients (mean 1.22 admissions per patient) over the study period.
Survival at five and ten years was 67% and 53%, respectively (without adjustment for right-censoring). Survival ranged from as high as 85% and 81% in those aged under 50 years, to 44% and 22% at five and ten years in those aged over 75 years at the time of index ICU admission (P < 0.001).
Shorter long-term survival was associated with increasing age (Hazard Ratio (HR) 1.050, 95%CI 1.048–1.051, P < 0.001), male sex (HR 1.18, 95%CI 1.16–1.21, P < 0.001), metastatic cancer (HR 3.79, 95%CI 3.64–3.95, P < 0.001), chronic liver disease (HR 2.54, 95%CI 2.38–2.70, P < 0.001) and admission diagnoses such as chronic obstructive pulmonary disease (HR 3.25, 95%CI 2.84–3.72, P < 0.001) and acute neurological conditions (HR 2.29, 95%CI 2.00–2.63, P < 0.001) including stroke (HR 2.38, 95%CI 2.05–2.77, P < 0.001).
Conclusion
Ten-year survival rates after the index ICU admission appear to exceed 50%. Linkage between clinical registries and administrative datasets may provide vital information to clinicians and patients about prognosis and determinants of long-term survival after critical illness.
358
CAN EARLY FUNCTIONAL ELECTRICAL STIMULATION-ASSISTED CYCLE ERGOMETRY (FESCE) REPLACE INSULIN INFUSION IN ICU PATIENTS?
1Charles University, Fac Med 3, FNKV University Hospital, Prague, European Union
Introduction
Insulin used to control blood glucose in ICU patients is not without risks. Glycogenolysis is coupled with muscle contraction and it can be hypothesized that active exercise can improve insulin sensitivity. FESCE is a novel way how to deliver active exercise early to sedated critically ill patients.
Methods
In a prospective randomized-controlled trial (NCT02864745), out of 1838 screened, we randomized 128 ICU patients within 48 hours of admission to receive intervention (FESCE) or no intervention on top of standard of care that included 30 min of goal-directed rehabilitation. Nutrition and blood glucose control measures were prescribed by clinicians not involved in the trial. We have monitored continuously (MetaVision, IMD Soft) and compared, blood glucose levels, glucose intake and daily insulin dose. In a subset of 30 patients we have performed hyperinsulinaemic clamps (insulin dose 120 mIU/m2 BSA.min) at baseline and after 7 days.
Results
FESCE group (n = 62) received 68 ± 35 min of exercise as opposed to controls (n = 66) who received 36 ± 16 min (p < 0.01). Blood glucose levels (n = 12640 values, both groups 8.7 ± 2.6 mmol/L) and carbohydrate intake (149 ± 99 vs. 146 ± 89 g/day, p = 0.73) were not different. Insulin requirements were 15 ± 28 IU/day in intervention vs. 21 ± 38 IU/day in controls (p = 0.37). In the subset of patients (n = 14 + 16) insulin clamp data confirmed no difference in insulin sensitivity (glucose disposal changed from 1.7 ± 1.1 to 2.6 ± 1.0 mg/kg.min in interventional group and from 1.2 ± 0.9 to 2.0 ± 0.8 mg/kg.min in controls).
359
ANALYSIS OF DOSAGE PATTERNS OF ANESTHETICS IN PATIENTS WHO RECEIVED RIGID BRONCHOSCOPY WITH TOTAL INTRAVENOUS ANESTHESIA
1Jeju National University Hospital, Jeju, South Korea
Introduction
Recently, palliative procedures have been widely used as treatment methods for central airway obstruction, as well as flexible and rigid bronchoscopy. Since rigid bronchoscopy is an invasive procedure and requires strong stimulation, it is difficult to perform smoothly with only light sedation, thus requiring general anesthesia.
Methods
We reviewed the electronic medical records of patients who had undergone rigid bronchoscopy with total intravenous anesthesia under general anesthesia between April 2015 and March 2019. A total of 81 patients were enrolled in this study. For maintenance of anesthesia, the patient received propofol (target plasma concentration 2.0–6.0 µg/ml) and remifentanil (target plasma concentration 2.0–6.0 ng/ml). Generally, 100% oxygen was applied in high flow manual bagging during the procedure.
Results
The amount of propofol administered per minute to maintain anesthesia was inversely correlated with the total operation time (r2 = 0.355, β = −0.067, p < 0.000). Remifentanil did not show significant differences when the procedure was repeated in the same patient. However, the amount of propofol administered per minute was significantly correlated to the number of times the procedure was repeated (r2 = 0.507, β = 0.449, p = 0.006).
Conclusion
The dose of propofol tended to decrease over time, and the amount administered per minute was significantly correlated to the number of times the procedure was repeated in the same patient.
362
A RETROSPECTIVE STUDY TO EVALUATE ICU OUTCOMES OF CANCER PATIENTS WITH ACUTE KIDNEY INJURY (AKI) REQUIRING RENAL REPLACEMENT THERAPY (RRT)
1Tata Memorial Hospital, Homi Bhabha National Institute, Mumbai, India
Introduction
AKI is a common in ICU patients. AKI needing RRT occurs in 5–6% general ICUs. AKI needing RRT is more frequent (9–27%) in cancer patients due to infections, treatment of cancer and cancer itself. Morbidity and mortality (43 to 77%) increase in cancer patients in ICU with AKI who require RRT.
Methods
We conducted a retrospective analysis of all cancer patients admitted to ICU requiring RRT over 2 years (2016 and 2017). We attempted to identify prognostic indicators to predict outcomes. The outcomes studied were ICU mortality, Hospital mortality, need for RRT at discharge.
Results
243/1791 cancer patients (mean APACHE II 21.22 ± 9.1) in ICU required 812 sessions of RRT.SLEDD was the most common initial modality (64.2%) but, overall, IHD was the most common modality. Hyperkalemia (55.1%) and metabolic acidosis (27.2%) were the commonest indications for initiation of RRT. In patients requiring RRT, ICU mortality was 59.3% and hospital mortality was 63.8%. Septic shock (76.1%) was the most common admission diagnosis. On univariate analysis, several parameters such as need for vasopressors, mechanical ventilation, APACHE II score, hepatic dysfunction, thrombocytopenia, etc. were associated with mortality. However; on multivariate analysis only mechanical ventilation, APACHE II score and occurrence of RRT associated complications were independently associated with mortality.34.57% patients had complete recovery of renal function while 6.17% patients became dialysis dependent. Complications occurred during 328/812 (40.4%) sessions. Hypokalemia (17.7%), hypotension (16.9%) and hypophosphatemia (13.3%) were the most common complications.
370
RICHMOND AGITATION-SEDATION SCALE: A RETROSPECTIVE AUDIT OF SCORING COMPLIANCE IN A LARGE REGIONAL HOSPITAL ICU
1Central Coast Clinical School, University of Newcastle, Gosford, Australia
2Gosford Intensive Care Unit, Gosford, Australia
Introduction
Sedation of ICU patients can have significant impacts on their clinical outcomes, with adverse outcomes associated with both over and under-sedation. Regular assessment of sedation levels in ICU patients is therefore vital in ensuring that appropriate sedation is achieved for critically ill patients. The Richmond Agitation-Sedation Scale (RASS) is a validated tool for monitoring sedation in ICU patients.
Objective
To determine compliance with RASS guidelines within Gosford Hospital ICU. Current nursing guidelines in Gosford Hospital ICU advise that RASS scoring should be performed on intubated patients I) at the beginning of every shift; II) every four hours; and III) with changes of sedation levels, aiming for a target sedation range of between +1 and -2.
Methods
A retrospective audit of all patients intubated for >48 hours over a six-month period from July to December 2018 in Gosford Hospital ICU was conducted. RASS frequency and scores were recorded from each patient’s “ICU Flowchart” paper observation charts.
Results
Of the total RASS scores recorded, 85% were taken within four hours of the previous score. Of the remaining 15% of scores, 28% were taken greater than eight hours following the previous score. Only 35% of recorded RASS scores were within the target sedation range of +1 to -2. Of the remaining scores, 30% indicated the patient was under-sedated and 35% indicated the patient was over-sedated.
Conclusion
Compliance with RASS scoring frequency was high. However, large gaps in scoring frequency highlights the need for improvement. Interventions should aim to target these large gaps, such as focusing on consistent afterhours scoring. Percentage of scores within the target sedation range was low and there appeared to be no bias towards over or under-sedation. Establishing a nurse-initiated protocol for modification of sedation levels based off RASS scores could potentially improve scores within the target sedation rage.
371
PREDICTORS OF NEPHROLOGY FOLLOW-UP AFTER ACUTE KIDNEY INJURY IN CRITICALLY-ILL PATIENTS
1Department of Intensive Care, Austin Hospital, Heidelberg, Australia
2School of Medicine, University of Melbourne, Melbourne, Australia
3Department of Intensive Care, Royal Melbourne Hospital, Parkville, Australia
Introduction
Acute Kidney Injury (AKI) is a frequent complication of critical illness and carries important prognostic and therapeutic significance. International data indicate a high risk of progression to chronic kidney disease (CKD) after AKI and consensus guidelines therefore recommend that patients are evaluated at 3 months to assess for the development of this complication.
Methods
A retrospective study of all critically ill adults admitted with AKI between 1 January 2012 and 31 December 2016 was conducted. Eligible patients were required to have a baseline eGFR >30 mL/min/1.73m2 and to be alive and independent of renal replacement therapy for 30 days after hospital discharge. Logistic regression models were used to examine the primary outcome, which was nephrology review within the first year. Candidate predictors were screened for inclusion using univariable models and a backward stepwise elimination approach was used to remove covariates whose multivariable p value was >0.2.
Results
Of 702 critically ill patients with AKI (mean age 66 years, 64% male, baseline eGFR 78 mL/min/1.73m2), 43 (6%) patients received nephrology follow up at 3 months, with only 63 patients (9%) being seen within the first year. The median time to nephrology review was 41 days (interquartile range 23–136). Nephrology follow up occurred more frequently in patients with a higher baseline creatinine, a higher discharge creatinine, and a greater severity of AKI. Traditional risk factors for CKD, including older age and a history of hypertension, diabetes, or cardiovascular disease, did not prompt specialist referral.
376
AUSTRALIAN INTENSIVE CARE IS COSTLY, INCREASED ICU SIZE AND OCCUPANCY ARE ASSOCIATED WITH REDUCED COSTS
1Fiona Stanley Hospital, Perth, Australia
2ANZICS CORE, Melbourne, Australia
3Alfred Hospital, Prahan, Melbourne, Australia
4Wellington Hospital, Wellington, New Zealand
Introduction
The provision of intensive care is expensive. Generalisable cost estimates are lacking and must account for variations in size, admission number, service provision and geographical distribution of Australian intensive care units (ICUs). The aim of this study was to estimate the financial costs of providing care to patients admitted to an ICU in Australia from an operational perspective and the association with bed number, occupancy and ICU type (tertiary, metropolitan, rural/regional, private).
Methods
A retrospective, multicentre cohort study using data from the Australian and New Zealand Intensive Care Society Centre for Outcomes and Resources Evaluation (ANZICS CORE) Critical Care Registry (CCR) in financial year 2013/14. Questions about ICU expenditure were developed using cost block methodology. ICUs in Australia were contacted and asked about ICU expenditure. All patients admitted to participating ICUs over the study period were included. Cost per patient day, annual costs per ICU bed and total annual ICU costs. The impact of ICU size and occupancy was also examined.
Results
The study included 36 ICUs (14 tertiary, 5 metropolitan, 10 rural/regional, 3 private). The median cost per patient day was AU$4,221 (IQR AU$3,436 – AU$5,286). The median annual cost per ICU bed was AU$1,114,557 [interquartile range (IQR) AU$900,455 – AU$1,368,277]. Increasing numbers of ICU beds and increasing ICU occupancy were associated with reduced costs per patient day (R2 0.23, P = 0.004 and R2 0.28, P = 0.002, respectively). ICU costs were estimated to account for over AU$2 billion annually, 1.4% of all health care expenditure, 0.15% of Australian gross domestic product and the equivalent of AU$92 per capita.
385
Current clinical practices, immediate complications and associated risk factors of emergency tracheal intubation in a tertiary-care hospital in Sri Lanka
1University Hospital, Kotalawala Defence University, Werahera, Sri Lanka
2Teaching Hospital Anuradhapura, Anuradhapura, Sri Lanka
Introduction
Emergency tracheal intubation in critically ill patients pose a challenge to clinicians. Patients may be hypoxaemic, hypotensive, cope poorly with induction agents and neuromuscular blocking drugs. Life threatening complications may occur in up to 40% critically ill patients.
Objectives
To determine the clinical practices, immediate complications and risk factors associated with tracheal intubation performed during emergencies at ICUs, emergency therapeutic unit and acute wards by doctors at a selected tertiary care hospital in Sri Lanka.
Methods
A prospective observational study was carried out in the surgical, medical, neuro surgical ICUs, surgical and medical casualty wards and ETU in a teaching hospital over a six month period. Demographic data, pre induction physical state, doctors training, intubation technique, medication used and the complications which occurred immediately after intubation was recorded.
Results
Data from 179 intubations were analysed. Fifty eight intubations occurred in ICUs, 54 in ETU and 67 in acute wards. Majority (59.2%) intubations occurred out of working hours, 53.6% were emergency intubations and 34% urgent intubations. Only 44% of doctors had >6 months training in anaesthesia. Pre-oxygenation and cricoid pressure were used in 76.5% and 55.3% respectively. Midazolam was used by 69.2% as an induction agent while 83.2% of time muscle relaxant was used. First attempt success rate was 71%, while only 3 patients required more than three attempts. Severe hypoxaemia (SpO2 <80%) occurred in 30.7% and severe hypotension (Systolic blood pressure <70mmHg) in 14%, oesophageal intubation 3.3%, damage to teeth 5% and Vomiting and regurgitation 7.2%. The duration of doctors training had no association with incidence of mechanical complications and number of attempts for successful intubation.
Conclusion
Intubation in emergency situations had considerable complications. Patients presenting complications, training received, technique used, preparation by the doctor and the availability of equipment are important factors contributing to immediate complications.
393
NIGHT-TIME DISCHARGE FROM PICU INCREASES THE RISK OF UNPLANNED READMISSION: AN ANALYSIS OF THE ANZPIC REGISTRY
1Royal Children’s Hospital Melbourne, Parkville, Australia
2Murdoch Children’s Research Institute, Parkville, Australia
3Sydney Children’s Hospital, Randwick, Australia
4Queensland Children’s Hospital, South Brisbane, Australia
5Starship Children’s Hospital, Grafton, New Zealand
6Perth Children’s Hospital, Nedlands, Australia
7Women’s and Children’s Hospital, North Adelaide, Australia
8ANZICS, Camberwell, 3124
Introduction
Night-time discharge from adult intensive care unit (ICU) is associated with high readmission rates and in-hospital mortality. There are limited data regarding the influence of night-time discharge from paediatric ICU (PICU) on readmission and mortality.
Methods
Data from the Australian and New Zealand Paediatric Intensive Care Registry (January 2000 to December 2017) were analysed. All children who survived PICU admission and were discharged to the ward were included. A propensity score methodology (utilising inverse probability of treatment weighting) was used to control for the following covariates between day-time and night-time discharges: age, gender, PIM2 score, elective admission, site, year of discharge (2000–08 vs 2009–17), and length of PICU stay.
Results
We included 150,460 discharges of 108,442 children over an 18 year period. The prevalence of night-time discharge declined (p trend < 0.001) during the study period: 6.7% (2604 out of 38979) in 2000–05, 6.1% (2946 out of 48428) in 2006–11 and 5.7% (3566 out of 63053) in 2012–17. Overall, the unplanned readmission rate was 1.9% for day-time discharge and 2.4% for night-time discharge. In a controlled analysis, night-time discharge was associated with higher odds for unplanned readmission [OR (95% CI): 1.45 (1.14–1.85), p = 0.002]. There was no significant association between night-time discharge and hospital mortality [OR (95% CI): 1.41; (0.80–2.49), p = 0.23].
397
THE USE OF ANTHROPOMETRY TO DETERMINE SAFE TIDAL VOLUMES IN ICU PATIENTS
1Ballarat Health Services, Ballarat, Australia
Introduction
Mechanical ventilation is a commonly employed therapy in ICU patients. It is well established that the use of low tidal volumes (VT) between 4–8ml/kg of ideal body weight (IBW) reduces the risk of lung injury in mechanically ventilated patients. IBW can be estimated from vertical standing height, however this is often unknown and not feasible in critically ill patients. Several different anthropometric measurements have been proposed to estimate standing height, however there is no current consensus on the best measurement to estimate height when this is unknown.
Methods
Structured review of research papers relating to anthropometric measurements in the ICU. Papers were included if they were in English and evaluated adult patients (≥18 years), and compared anthropometric measurements to a gold-standard vertical height.
Results
10 studies fulfilled our search criteria. 6 were excluded as they did not compare anthropometric measurements with vertical height. Ulnar length, knee length and demispan were considered for use in the ICU.
Demispan.
2 studies evaluated demispan as a measurement tool. One paper (n = 82) observed good agreement between demispan and vertical height, while the other paper (n = 49) observed that male patients were potentially under-ventilated if demispan was used to estimate VT.
Ulnar and knee length.
1 study (n = 100) utilising ulnar tape measures showed that VT was within 95% limits of agreement; however, this study only focused on volunteers below 65 years old.
Another study looked at supine measurement, ulnar length and knee length against vertical height (n = 100). Supine measurement yielded overestimations of VT by almost 150ml, with ulnar length and knee length causing overestimations between 73–87ml.
399
IMPROVED CONTACT WITH POSTOPERATIVE PATIENTS USING THE “PATIENT ASSISTANT” GRAPHIC TABLE
1Dnipropetrovsk Regional Clinical Center Of Cardiology And Cardiac Surgery, Dnipro, Ukraine
2 State Institution “Dnipropetrovsk Medical Academy of the Ministry of Health of Ukraine”, Dnipro, Ukraine
Introduction
Most patients after cardiac surgery need prolonged mechanical lung ventilation making it difficult to have productive contact with medical staff and thus reducing the comfort of staying in a medical facility. Therefore, at the moment it is relevant to search for new methods of communication.
Methods
80 patients were divided into two groups, which were matched by sex, age and type of surgery. Group 1: 40 patients, 15 of them were women (37.5%). The average age was 57.57 ± 9.39. “Patient Assistant” graphic table were used to make a contact with patients from this group. Group 2: 40 patients, 13 of them were women (32.5%). The average age was 55.3 ± 8.64. Another non-verbal methods were used for communication with this group. Evaluation of the effectiveness of the means of communication used was carried out on the basis of the patient’s subjective assessment 2 hours after extubation by a scale from 1 to 5 points. For processing the results, the methods of descriptive and non-parametric statistics were used.
Results
Patients from group 1 rated the effectiveness of using additional communication tools as follows: 4 [3; 5] points; Patients in group 2: 2 [2; 4] points. Statistically significant differences were found between the results in groups 1 and 2 (p = 0.000725 according to the Mann-Whitney test).
407
PREDICTORS OF MEDICAL EMERGENCY TEAM ATTENDANCE AFTER SURGERY
1Intensive Care Unit, Alfred Hospital, Alfred Health, Melbourne, Australia
2Medical Services, Alfred Hospital, Alfred Health, Melbourne, Australia
3Australian and New Zealand Intensive Care Research Centre, School of Public Health and Preventive Medicine, Monash University, Melbourne, Australia
4Department of Anaesthetics and Perioperative Medicine, Alfred Hospital, Alfred Health, Melbourne, Australia
5Department of Radiology, Alfred Hospital, Alfred Health, Melbourne, Australia
Introduction
The Medical Emergency Team attendance (METs) serve as a rapid response system when a patient’s vitals become abnormal.
Methods
Demographic, diagnostic, operative and biochemical data were extracted for all in-patients who underwent a surgical procedure in 2016 at The Alfred Hospital, Melbourne. Patients with one or more METs within 48 hours of discharge to a general ward were identified. Only the first procedure was considered for each patient. Patients admitted directly to ICU from the operating theatre, or patients who had a MET after an ICU admission post operatively were excluded.
Results
Of 10,098 patients, 6.9% (697/10098) had one or more METs in the 12-month study period. METs were most commonly called for hypotension of <90mmHg (244/697 – 35.0%) and for decrease in Glasgow Coma Scale (GCS) of more than 2 points (88/697 – 12.6%).
METs most commonly occurred following endoscopy procedures (130/697 – 18.7%) and major orthopaedic surgery (109/697 – 15.6%), following emergency procedures as compared to elective procedures (383/4810 – 8.0% vs 314/5288 – 5.9%, p < 0.001) and longer surgical procedures (127 [71-202] vs 106 [59-187] mins, p < 0.001) 1 .
Patients who had METs were older (62.5 [18.6] vs 54.5 [19.7] years, p < 0.001) 2 , had lower haemoglobin levels (125 [21] vs 133 [18] g/L, p <0.001)2 and higher level of urea (7.8 [4.8] vs 6.9 [4.3] mmol/L, p = 0.004)2.
Patients who had METs had longer hospital stays (12 [5-23] vs 3 [1-8] days, p < 0.001)1 and higher mortality (5.3% vs 1.6%, p < 0.001).
Notes
Median [interquartile range].
Mean [standard deviation].
408
PROBIOTICS FOR THE PREVENTION OF ANTIBIOTIC-ASSOCIATED DIARRHOEA: A SYSTEMATIC REVIEW AND META-ANALYSIS
1University Of Notre Dame Australia, Sydney, Darlinghurst, Australia
Introduction
Antibiotics disturb normal gastrointestinal flora leading to diarrhoea in up to 35% of users. Antibiotic-associated diarrhoea (AAD) has a significant impact on hospital length of stay, morbidity and mortality. Probiotics are thought to protect against AAD by reducing colonisation by pathogenic bacteria.
Methods
The electronic databases MEDLINE (Ovid), CINAHL Plus, Web of Science, and Google Scholar were comprehensively searched for randomised controlled trials investigating the use of probiotics for the prevention of AAD. The search was limited to adult subjects and included only English language literature. Data extraction followed PRISMA guidelines. The primary outcome was AAD incidence. Sub-group analyses evaluated species-specific and dose-specific responses. Dichotomous outcomes were pooled using a random-effects model to calculate odds ratio (OR) and 95% confidence interval (95% CI).
Results
Twenty-nine of 849 identified studies met inclusion criteria (total 8218 participants). Meta-analysis of pooled data suggests that probiotics reduce the incidence of AAD by 47% (OR = 0.53, p < 0.001). Compared with placebo, probiotics reduce the incidence of AAD by 43% (OR = 0.57, p < 0.001), whilst compared with no treatment, probiotics reduce incidence of AAD by 77% (OR 0.33, p < 0.001). AAD incidence was reduced with probiotic species: L. acidophilus (13 studies: OR 0.51, p < 0.001), Bifidobacterium spp. (8 studies: OR 0.57, P < 0.01), and Lactobacillus spp. (22 studies: OR 0.51, P < 0.0001). A dose-response effect was observed, with a greater reduction in AAD in those receiving high versus lower doses (OR 0.53, p < 0.01).
*Updated review due mid-2019.
414
THE ASSOCIATION BETWEEN MELATONIN AND DELIRIUM: A SYSTEMATIC REVIEW
1The University Of Notre Dame Australia, Sydney, Australia
2Werribee Mercy Hospital, Werribee, Australia
Introduction
The pathogenesis of delirium is yet to be fully elucidated. One hypothesis proposes that disruptions in circadian rhythms are complicit in the development of delirium. Measuring melatonin levels provides information about the state and regularity of the circadian clock.
Methods
We systematically searched PubMed, CINAHL, EMBASE, PsychINFO, Web of Science, MEDLINE, and the Cochrane Library, and hand-searched relevant references for studies published from 2000–2019 in English. Inclusion criteria were original research investigating an association between measured melatonin levels and delirium in hospitalised patients with a recognised method of delirium diagnosis. Extraction data included population characteristics, delirium diagnosis tool and subtype, melatonin measurement method and timing, and main study findings.
Results
A total of 10 studies met the inclusion criteria for data extraction. This resulted in a sample size of 614 patients, of which 262 had a delirium diagnosis. Various delirium diagnostic tools were used and melatonin was measured in serum, urine, saliva, and cerebrospinal fluid samples. Each study measured melatonin at different timepoints during admission. 8 studies reported a significant association between changes in melatonin levels and delirium, this association was different in each case. Broadly, in delirious patients, 4 studies reported significantly lower levels of nocturnal or 24-hour melatonin secretion, 2 studies reported significant disruption of rhythmic secretion patterns only, and 2 studies reported significant changes in daytime levels. 1 study also reported significantly higher levels of 24-hour melatonin secretion in hypoactive delirium.
416
COAGULATION ABNORMALITIES AND ASSOCIATED MANAGEMENT IN PATIENTS WITH SEVERE ACUTE LIVER FAILURE IN AUSTRALIA AND NEW ZEALAND
1Austin Health, Heidelberg, Australia
2The University of Melbourne, Heidelberg, Australia
3Epworth HealthCare, Box Hill, Australia
4Australian and New Zealand Intensive Care Research Centre, Clayton, Australia
5Department of Critical Care Medicine, Auckland City Hospital, Auckland, New Zealand
6South Metropolitan Health Service, Rockingham, Australia
7Department of Intensive Care, Sir Charles Gairdner Hospital, Perth, Australia
8Department of Intensive Care, Princess Alexandra Hospital, Brisbane, Australia
9Department of Intensive Care, Flinders Medical Centre, Adelaide, Australia
10Department of Intensive Care, Royal Prince Alfred Hospital, Sydney, Australia
11Department of Anesthesiology and Pain Medicine, Hospital Santa Creu i Sant Pau, University of Barcelona, Barcelona, Spain
12Data Analytics Research and Evaluation (DARE) Centre, Austin Hospital and University of Melbourne, Melbourne, Australia
Introduction
Acute Liver Failure (ALF) causes a complex critical illness with high mortality. Deranged haemostatic parameters are a defining characteristic, however little is known about how these are assessed or managed and how this affects outcomes.
Methods
We obtained and analysed data on key baseline characteristics, aetiology, coagulation and haematological tests, utilisation of blood products and outcomes during the first week in ICU.
Results
We studied 62 ALF patients, with 60% fulfilling King’s College Criteria (KCC) for transplantation. The median initial (first 24 hours) highest INR was 5.5 (IQR 3.8–8.7) and the median longest aPTT was 62 seconds (IQR 44–77 seconds). Fibrinogen was not measured in 15% of patients (p < 0.001 compared with other tests), although median concentrations were lower in patients with bleeding (p < 0.006). Initial median lowest platelet count was 83 (IQR 43–122) x 109/L, and patients who experienced bleeding had worse thrombocytopaenia (p < 0.008). 58% received FFP (peak INR of 5.7); 40% received cryoprecipitate (nadir fibrinogen of 0.9 g/L) (p = 0.001 compared with untreated patients) and 35% percent received platelets (nadir count of 44 x 109/L (p = 0.004 compared with untreated patients), (p < 0.01). 15% received prothrombin complex concentrate (PCC) for a median amount of 2500 units at a median peak INR of 10.1 (IQR 5.4–10.7) (p = 0.02 compared with untreated patient). Finally, 47% received a blood transfusion.
426
ASSOCIATION BETWEEN PREMORBID METFORMIN USE AND SEPSIS OUTCOMES
1Nepean Clinical School Sydney Medical School, The University Of Sydney, Penrith, Australia
2Department of Intensive Care Medicine, Nepean Hospital, Penrith, NSW, Australia, Penrith, Australia
3Yale University, New Haven, USA
4Medistra Hospital, Jakarta, Indonesia
Introduction
Recent data showed that premorbid metformin usage is associated with decreased mortality in sepsis. However, the effect of metformin on other sepsis outcomes remain unknown.
Methods
Retrospective cohort study on patients with sepsis between January 1, 2014 and December 31, 2017. Eligible patients were admitted to intensive care unit (ICU) with sepsis or septic shock. Premorbid metformin use was identified via medical records. Propensity score matching (PSM; 1:2 ratio) was performed using optimal matching without replacement and a caliper size of 0.25. Variables adjusted for include age, gender, APACHE IV score, premorbid β blocker usage, other premorbid anti-hyperglycemic agent usage, and source of infection.
Results
410 patients, including 63 (15%) with premorbid metformin use were identified. Overall ICU mortality rate was 23.4%. After PSM, comparing between no premorbid metformin use vs premorbid metformin use there were no differences in age (68 vs 66, p = 0.14), gender (males, 73% vs 67%, p = 0.052), median Apache IV score (75 vs 79, p = 0.47), median SOFA score difference (day 1 vs day 3; 0 vs 0, p = 0.24), median ICU length of stay (hours; 93 vs 125, p = 0.13), mechanical ventilation requirements (24% v 12%, p = 0.87), and renal replacement therapy requirements (15% v 14%, p = 0.73). Median total intubation time (hours; 45 v 88, p = 0.03) significantly higher with premorbid metformin usage. Premorbid metformin use was not significantly associated with ICU mortality (16.9% vs 6.9%; adjusted risk ratio = 0.83; 95% confidence interval (CI) 0.50–1.39; p = 0.48).
427
ASSOCIATION BETWEEN PREMORBID BETA BLOCKERS USE AND SEPSIS OUTCOMES
1Nepean Clinical School, Sydney Medical School, The University Of Sydney, Sydney, Australia
2Department of Intensive Care Medicine, Nepean Hospital, Penrith, NSW, Australia, Penrith, Australia
3Yale University, New Haven, The United States of America
4Medistra Hospital, Jakarta, Indonesia
Introduction
Elevated adrenergic response is a hallmark of early sepsis. β-adrenergic blockade is a potential treatment modality as β blockers (BB) exhibit multiple modulatory effects on cardiogenic, immunologic, metabolic, and coagulopathic derangements in sepsis.
Methods
Retrospective cohort study on patients with sepsis between January 1, 2014 and December 31, 2017. Eligible patients were admitted to intensive care unit (ICU) with sepsis or septic shock. Premorbid BB use was identified via medical records. Propensity score matching (PSM; 1:2 ratio) was performed using optimal matching without replacement and a caliper size of 0.25. Variables adjusted for include age, gender, APACHE IV score, premorbid metformin usage, other premorbid anti-hyperglycemic agent usage, and source of infection.
Results
410 patients, including 99 (24%) with premorbid BB use were identified. Metoprolol (46.5%) and bisoprolol (17.2%) were most commonly used. Overall ICU mortality rate was 23.4%. After PSM, age was not statistically different (no premorbid BB use vs premorbid BB use; 68 v 68, p = 0.91). There were no differences in gender (males, 55% vs 58%, p = 0.56), median APACHE IV score (77 vs 77, p = 0.82), median SOFA score difference (day 1 vs day 3; 3 vs 2, p = 0.13), median ICU length of stay (hours; 113 vs 117, p = 0.82), median total intubation time (hours; 60 v 48, p = 0.47), mechanical ventilation requirements (37% v 20%, p = 0.32), and renal replacement therapy requirements (15.7% v 15.2%, p = 0.91). Premorbid BB use was not significantly associated with ICU mortality (12% vs 6.6%; adjusted risk ratio = 1.09; 95% confidence interval (CI) 0.76–1.56; p = 0.64).
431
PHYSICAL ACTIVITY LEVELS OF MECHANICALLY VENTILATED PATIENTS FROM AWAKENING TO INTENSIVE CARE UNIT DISCHARGE
1Servicio de Medicina Física y Rehabilitación, Departamento de Medicina Interna, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
2Critical Care Departament, Clínica Alemana Universidad del Desarrollo, Santiago, Chile
3School of Physical Therapy, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
Introduction
The time that patients spend in different physical activity (PA) intensity levels and sedentary behavior (SB) are still unknown in the intensive care unit (ICU) stay.
Methods
A secondary analysis of a prospective study approved by the Clínica-Alemana-Universidad-del-Desarrollo ethics committee (N°2017-104) was conducted in a 12-beds academic medical-surgical ICU. Data was analyzed from awakening (defined as: patient answered 5-simple questions for first time) to ICU discharge in patients >18 years old who received mechanical ventilation. A triaxial accelerometer (Actigraph®GT9X-Link) was installed on the right ankle to measure the time spent in PA and SB from awakening to ICU discharge. All patients received bath-twice-day, positioning each 2-hours and standard physiotherapy including multimodality-respiratory-physiotherapy, passive-range-of-motion, neuromuscular-electrical-stimulation, cycling and progressive-mobility.
Results
Twenty-nine patients completed the accelerometry record from awakening to ICU discharge. Fifty-percent were female and their characteristics (median [RIQ]) were: age = 77(68–79) years old, APACHEII = 19 (16–24) points, mechanical ventilation days = 6(6–10), ICU length of stay = 11(10–16), FSS-ICU on awakening = 7(5–10) points and at ICU discharge = 18(15–22) points. Patients spent from awakening-discharge a total of 58.7(56.5–59.8) minutes per hour in SB. The total time patients spent on PA were 0.98(0.94–1) minutes per hour, which represent the 4.9% of the total time. This 4.9%, correspond to light PA (92.5%), moderate PA (7.1%) and vigorous and very vigorous PA (0.4%).
432
Feasibility of Actigraphy measurement in mechanically ventilated patients from ICU admission to ICU discharge
1Servicio de Medicina Física y Rehabilitación, Departamento de Medicina Interna, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
2Critical Care Departament, Clínica Alemana Universidad del Desarrollo, Santiago, Chile
3School of Physical Therapy, Facultad de Medicina Clínica Alemana Universidad del Desarrollo, Santiago, Chile
Introduction
Accelerometry measurement has been used for up to 5 continuous days in the intensive care unit (ICU), however, this movement monitoring throughout the whole ICU stay has not been rigorously evaluated.
Methods
A prospective study was conducted in a 12-beds academic medical-surgical ICU. Adult mechanically ventilated patients were included to measure movement daily with a triaxial accelerometry (GT9X Link ActiGraph®, Pensacola, Florida) during 24-hours a day. Twenty accelerometers were available for their potential installation and when the battery-level was less than 10%, were replaced. The accelerometers were installed in the right ankle, using a 5-second epoch and a 90-hertz sampling frequency. ICU-staff was trained in the device-care and the accelerometer functioning was daily monitored by two researchers. Data extraction was performed using “Low-frequency-extension” of Actilife 6.0. The activity time, immobility time and amount of movement were analyzed.
Results
Seventy of ninety-one eligible patients were enrolled from October-2018 to January-2019, installing 81 accelerometers. Thirty patients were analyzed; one was excluded due to miss of accelerometer information. The maximum numbers of accelerometers operated simultaneously were 7. The median (minimum-maximum) delay time between the ICU admission and the accelerometer installation was 128.5 (0–711) minutes. The median (minimum-maximum) duration of measurement was 5.5 (2.3–29.5) days. Only one patient refused to participate in the study due “device would interfere clinically”, and no patient reported discomfort or injury. There was always at least one accelerometer available for installation and there was no loss of any device.
433
EMERGENCY CALLS TO PATIENTS UNDERGOING IN-HOSPITAL PROCEDURES
1St Vincent’s Hospital Melbourne, Fitzroy, Australia
Background
Many hospital patients undergo procedures which have the potential to lead to clinical deterioration ending in an emergency call.
Objective
To investigate the incidence and causes of emergency calls to patients within 48 hours of an in-hospital procedure.
Methods
All patients undergoing procedures in 2017 and 2018 in a tertiary referral hospital were linked to a database of emergency calls. Timing of the call was divided in early (0–6 hours), intermediate (7–24 hours) and late (25–48 hours) post procedure. Data are expressed as median (interquartile range) and percentages.
Results
43,881 procedures were performed on 29,467 patients and there were 1593 emergency calls for the 2 years. 511 events (32.1% of all calls, 1.7% of all procedures) were recorded. 12 patients had a cardiac arrest (4 died) all within the first 6 hours; 4 post coronary intervention arrests survived. Patients were aged 68.4 (55.6–77.3) years and 50% were female. Early calls (n = 148) were due to hypovolaemia (42.0%), vasovagal events (9.0%) and narcosis (4.6%). Intermediate calls (n = 196) were for hypotension (26%), respiratory problems (15.8%), bleeding (7.1%) and altered conscious state (9.7%) while the late calls (n = 167) were for abnormal rhythm (25.0%), hypotension (22.8%), respiratory problems (15.0%) and pulmonary oedema (6.0%). Approximately 20% of calls resulted in transfers (ICU 48%, OR 22%).
Conclusions
While emergency calls are infrequent after procedures, they account for almost one third of emergency calls. Early calls are related to the procedure and anaesthesia, while later calls result from surgical (bleeding) and medical issues (rhythm, pulmonary oedema).
434
UPWARD TREND IN SEPSIS-RELATED ICD-10 CODED HOSPITALISATIONS AND AR-DRGs IN AUSTRALIA DURING 2002–17: AN AIHW DATABASE ANALYSIS
1The George Institute For Global Health, Sydney, Australia
2University of New South Wales, Sydney, Australia
3Royal North Shore Hospital, Australia
4Sydney Medical School, Australia
5Bankstown Hospital, Australia
Introduction
In 2017, the WHO recognised sepsis as a global health priority and urged improved use of International Classification of Disease (ICD) coding to estimate the global burden of sepsis. However, the true burden of sepsis remains largely unknown.
Methods
A retrospective analysis of the publically available Australian Institute of Health and Welfare (AIHW) database was undertaken to identify all sepsis-related hospitalisations in Australia between 01 July 2002 and 30 June 2017. The sepsis ICD-10 codes used were A40 (Streptococcal sepsis); A41 (other sepsis) including sepsis by Staphylococcus (A41.0–41.02) and unspecified gram-negative organisms (A41.5), other specified sepsis (A41.8) and unspecified sepsis (A41.9), and uncommon sepsis due to other organisms. The AR-DRGs used to estimate sepsis-related hospital resource use included septicaemia, with (T60A) or without (T60B) catastrophic outcomes.
Results
Sepsis-related hospitalisations increased from 13,004 in 2002 to 46,267 in 2017. Unspecified sepsis (A41.9) was the most commonly coded subgroup followed by sepsis due to unspecified gram-negative organisms (A41.5), staphylococci (A41.0–41.2) and streptococci (A40.0). The proportion of unspecified sepsis increased from 43.35% to 54.15%, showing an increase of 33%, whereas proportion of A41.5, A41.0–41.2 and A40 reduced from 26.15%, 14.76% and 9.45% to 20.92%, 8.13% and 7.31%, respectively, during 2002–17. Sepsis-related AR-DRGs increased from 11,830 to 39,292 in the 15-year study period with T60B showing steeper rise compared to T60A.
444
UNPLANNED ICU ADMISSIONS TO SIRIRAJ SURGICAL INTENSIVE CARE UNIT
1Department Of Anesthesiology Faculty Of Medicine Siriraj Hospital, Bangkok, Thailand
Introduction
Intensive care bed booking for all surgical patients who need access to Siriraj surgical intensive care unit (SICU) must be given to the SICU in advance by the surgical team. However, there are some unexpected SICU patients, and we would like to evaluate this unplanned ICU admission as a quality control.
Methods
We retrospectively analyzed of prospective collecting data of unplanned for ICU admission patients in Siriraj surgical ICU from 1st August 2010 – 31st January 2011. From 19,687 patients received anesthesia services, and 16,360 patients who were eligible to gain access to our Siriraj surgical ICU. We analysed these patients to learn what the reasons were, where they came from, and how big the anesthesia-related reasons can be.
Results
There were 469 admissions to Siriraj surgical ICU during study period, and 51 episodes of unplanned patients were reported (10.9%) that was less than the previous study (15%). The incidence of unplanned Siriraj SICU admission patients was 31: 10,000. The major source of these patients were from the operating theatres, followed by the recovery rooms and surgical wards. The main reasons were cardiac complications (33), the respiratory and airway complications (6), while 9 patients were admitted for close observations. Two cases of unplanned ICU admission were noted to cause early SICU discharge without haemodynamics stability.
450
INTERNET IS A FREQUENT AND TRUSTED SOURCE OF HEALTH INFORMATION AMONGST YOUNGER NEXT-OF-KIN OF PATIENTS IN THE INTENSIVE CARE UNIT
1Fiona Stanley Hospital, Willetton, Australi
2Royal Perth Hospital, Perth, Australia
3St John of God Subiaco Hospital, Subiaco, Australia
4Sir Charles Gairdner Hospital, Nedlands, Australia
5Royal North Shore Hospital, St Leonards, Australia
6Armadale Hospital, Armadale, Australia
7Royal Prince Alfred Hospital, Camperdown, Australia
8Royal Darwin Hospital, Tiwi, Australia
9University of Western Australia, Nedlands, Australia
10St John of God Midland Hospital, Midland, Australia
11Peninsula Private Hospital, Frankston, Australia
12University Notre Dame Fremantle, Fremantle, Australia
13St John of God Murdoch Hospital, Murdoch, Australia
14Cabrini Private Hospital, Malvern, Australia
15Canberra Hospital, Garran, Australia
Introduction
Next-of-kin (NOK) of patients admitted to the intensive care unit (ICU) are often involved in decision-making. This requires obtaining and understanding appropriate information. However, the frequency and associated trust of internet use and other sources of health-related information is uncertain.
Objectives
To describe the sources of health information and associated trust, reported by NOK of patients admitted to the ICU.
Methods
After development, piloting and human research ethics approval, a structured survey was administered in 13 Australian adult ICUs. Eligible participants were the NOK and first survey respondent for a patient admitted to the ICU for more than 24 hours. In addition to internet use, sources assessed were family, others in the waiting area, ICU doctors, ICU nurses, non-ICU doctors, General Practitioners, television, books and newspapers.
Results
Of the 473 study participants, the median duration of ICU stay and number of ICU visits at the time of survey completion were 3 days [interquartile range (IQR) 2–6] and 4 visits (IQR 2–7) respectively. The median number of sources used frequently or very frequently was 3 (IQR 2–4). The sources with the highest proportion of very frequent or frequent use were the ICU nurse (84.8%), ICU doctor (74.0%), non-ICU doctor (44.4%), family (37.9%) and the internet (19.2%). On multivariable analysis, lower respondent age was independently associated with more frequent internet use (odds ratio if less than 50 years old, 2.7 (95% confidence interval 1.7–4.4), P < 0.001). Of the 84 respondents reporting very frequent or frequent internet use, 49% completely or mostly trusted the internet compared with 98% trusting the ICU nurse (P = 0.001).
Conclusions
NOK in the ICU frequently used multiple health information sources to inform decision-making. ICU nurses were the most frequently used source and were highly trusted. The internet was a trusted source by a substantial proportion of younger surrogate decision-makers.
454
IMPACT OF INITIAL FIBRINOLYTIC MARKERS ON THE NEUROLOGICAL OUTCOME OF PATIENTS WITH TRAUMATIC BRAIN INJURY
1Hyogo emergency medical center, Kobe, Japan
Introduction/Objectives:
Acute coagulopathy is a well-known predictor of poor outcomes in patients with traumatic brain injury (TBI). However, the role of fibrinolytic markers in TBI remains unclear. We analyzed initial fibrinolytic abnormalities in relation with outcome in patients with TBI.
Methods
In this single center, retrospective study from January 2013 to May 2019, we identified 96 patients of isolated TBI (Abbreviated Injury Score –head of 3–5) with initial blood sample obtained no more than 1 hour after injury. We divided into two groups in plasma of D-dimer (D-D) level, which is low (<40µg/ml:L) or high (≧40:H). Patients with GCS≦10, transfusion within 3h after injury, under anti-coagulation or anti-platelet therapy were excluded. Measurement of plasma fibrinogen and D-D levels were done on arrival and 3 hours after injury. In GOS, GR/MD at 1 month was defined as favorable neurological outcome, SD/VS/D as unfavorable.
Results
Group L was 27, and Group H was 15 patients. Initial plasma level of D-D was 14.8 (7.0–19.7) in Group L and 65.9 (52.9–86.7) in Group H. Initial plasma level of fibrinogen was not significantly different between either groups (L:236 mg/dl (211–270), H:260 (234–286), P = 0.49). In Group H, the change of plasma level of fibrinogen from initial to 3h after injury (fibrinogen) was lower than in Group L (L:−20 (−36− −6.2), H:−63 (−81− −57), P = 0.42). There was a significant correlation between initial plasma level of D-D and fibrinogen (R2 = 0.55, P < 0.05). Group L had a higher rate of favorable neurological outcome than Group H (L:92% (25/27), H:53% (8/15)) (p < 0.05).
Conclusion
Fibrinolytic abnormalities are useful parameter for patients in acute phase of TBI, initial low plasma D-D may be a predictor of favorable neurological outcome.
473
MANAGEMENT OF HYPERAMMONAEMIA IN ACUTE LIVER FAILURE: THE EFFECT OF CRRT TIMING, INTENSITY AND DURATION
1Austin Health, Heidelberg, Australia
2The University of Melbourne, Heidelberg, Australia
3Epworth HealthCare, Box Hill, Australia
4Data Analytics Research and Evaluation (DARE) Centre, Heidelberg, Australia
Introduction
Acute Liver Failure (ALF) causes severe hepatic encephalopathy (HE), cerebral oedema and high risk of death. Hyperammonaemia is a key contributing factor and continuous renal replacement therapy (CRRT) has been proposed to achieve safer levels (<150 µmol/L); however, the optimal timing, mode, intensity and duration of treatment is unknown.
Objective
We aimed to study CRRT use in ALF patients and its impact on hyperammonaemia.
Methods
Data were obtained and analysed for patient characteristics, CRRT use, ammonia dynamics and outcomes.
Results
We studied 54 ALF patients, of whom 81% had high grade HE. The median time to initiation of CRRT was 4 hours (IQR 2–4.5) with 78% treated with CVVHDF and 22% with CVVH. The median hourly dose of CRRT was 43 ml/kg (IQR 37–62). The median ammonia concentration reduced every day during treatment: day 1; 151 µmol/L (IQR 110–204), day 2; 107 µmol/L (IQR 84–133), day 3; 75 µmol/L (IQR 63–95), day 5; 52 µmol/L (IQR 42–70), p < 0.0001). The number of patients with ammonia >150 µmol/L also fell: day 1;26, day 2;9, day 3; 2, day 5;0. There was a correlation between higher early treatment dose and greater reduction in ammonia concentration (p = 0.03). This was attributable to the duration of therapy (p = 0.01), rather than hourly dose (p = 0.24). Reductions in ammonia were similar regardless of the mode of CRRT provided (p = 0.429). 65% achieved ELT-free survival.
Conclusion
CRRT reduces ammonia concentrations in ALF, rapidly achieving safe levels for most patients. There is an initial dose effect that is mainly due to the duration of therapy. These findings suggest that CRRT should be initiated early in ALF patients and that reducing ammonia may be an important therapeutic goal.
474
SOCIAL DETERMINANTS OF A CRITICAL CARE READMISSION TO HOSPITAL OVER ELEVEN YEARS
1Alfred Health, Prahran, Australia
2ANZICS Centre for Outcome and Resource Evaluation, Camberwell, Australia
3Safer Care Victoria, Melbourne, Australia
4The ANZIC-Research Centre, Monash University, Prahran, Australia
5Department of Intensive Care, Monash Medical Centre, Clayton, Australia
6Department of Intensive Care, Eastern Health, Box Hill, Australia
Introduction
Socio-economic factors may influence long term health outcomes. Approximately 5% of patients are readmitted to an Intensive Care Unit (ICU) following their initial discharge to a medical ward but prior to their hospital discharge. However, readmissions to an ICU during subsequent hospitalisations have rarely been investigated.
Methods
Patients admitted to 23 adult public ICUs in Victoria, Australia between July 2007 to June 2018, were extracted from The Australian and New Zealand Intensive Care Society Adult Patient Database. De-identified data was matched using probabilistic methods and statistical linkage keys to the Victorian Admitted Episodes Database, to the Victorian Death Index and to socio-economic data from the Australian Bureau of Statistics linked by residential area.
Results
Of 228,912 ICU admissions examined, 183,635 (80%) were matched. 15,931 died in-hospital during their first admission, leaving 136,954 patients who accounted for a total of 167,704 ICU admissions. 21,650 (16%) patients had at least one more ICU admission over the eleven-year study period. Mortality on 1st, 2nd and 3rd readmissions were 11.4%, 10.1% and 8.2% respectively. After adjusting for age, acute and chronic illnesses, patients were less likely to be readmitted if from a higher socio-economic area (OR 0.976, 95%CI 0.971–0.982, P < 0.001), mandarin was listed as preferred language (OR 0.57, 95%CI 0.41–0.78, P = 0.001), in a married/defacto relationship (OR 0.92 95%CI 0.88–0.96, P < 0.001) or widowed (OR 0.74, 95%CI 0.69–0.79, P < 0.001). Readmissions were more likely in men (OR 1.07, 95%CI 1.04–1.11, p < 0.001) and separated/divorced patients (OR 1.17, 95%CI 1.10–1.24, p < 0.001) and those with chronic obstructive pulmonary disease (OR 2.32, 95%CI 2.08–2.60, p < 0.001).
475
THE UPTAKE OF LIAISON SERVICES IN AUSTRALIA AND NEW ZEALAND AND ITS IMPACT ON READMISSION TO INTENSIVE CARE
1Lyell Mcewin Hospital, Adelaide, Australia
2BAC Partners, Sydney, Australia
3Fiona Stanley Hospital, Perth, Australia
4Alfred Hospital, Melbourne, Australia
5School Of Public Health And Preventive Medicine, Monash University, Melbourne, Australia
6Anzcis Core, Melbourne, Australia
Introduction
There is limited data on the uptake of liaison services in Australian and New Zealand intensive care units (ICU) and its effect on clinical outcomes.
Methods
Retrospective analysis of the Australian and New Zealand Intensive Care Society (ANZICS) Adult Patient Database and Critical Care Resources registries from financial years 2006–7 till 2015–16. Proportion of patients discharged from ICU [in total, over time and at hospital level (tertiary, metropolitan, rural/regional and private)] with and without liaison services were determined. The association [(Odd’s ratio (OR) with its 95% confidence interval (CI)] between ICU readmission and liaison service along with multiple covariates was determined by mixed effect logistic regression.
Results
Of 716194 patients studied at 176 ICUs, 308537 patients (43%) were discharged from ICUs that provided a liaison service. The proportion of ICUs with a liaison service increased from 22% (20/90) in 2006–7 to 34% (44/129) in 2015–16 (P = 0.02). Liaison services were most common in tertiary compared to metropolitan, rural/regional and private hospital ICUs (73%, 43%, 40%, 10% respectively, P < 0.001). Patients exposed to liaison service were younger (mean years 62 vs. 60, P < 0.001), more frequently ventilated (43% vs. 34%, P < 0.001), had higher severity of illness (mean APACHE II score 15.3 vs. 14.6, P < 0.001), higher mortality (4.0% vs 3.0%, P < 0.001) and higher proportion of ICU readmission (5.0% vs. 4.6% P < 0.001). After adjusting for covariates, a liaison service was associated with increased likelihood of ICU readmission (OR 1.13, 95% CI 1.08–1.18, P < 0.0001).
477
A SINGLE INJECTION OF SAPHENOUS NERVE BLOCK IN OSTEOARTHRITIS PATIENTS AFFECTED THE REDUCTION OF POSTOPERATIVE BLEEDING
1Jeju National University Hospital, Jeju, South Korea
Introduction
In elderly patients, the vital sign tends to fluctuate according to the volume status, which may cause sudden hypovolemic shock if postoperative bleeding continues. Elderly patients, especially those who undergo surgery for arthritis, need more attention because the bleeding may persist over the joints after surgery. The appropriate pain control is related with postoperative blood loss.
Methods
We reviewed the electronic medical records of patients who had undergone uni-knee total arthroplasty with spinal anesthesia between January and May 2016. A total of 51 patients were enrolled in this study. All patients were treated with intravenous patient-controlled analgesia for postoperative pain control, and additional analgesic agents were administered at VAS above 6 score. In 25 patients, saphenous nerve block was performed using ultrasound with 0.75% ropivacaine 15ml before surgery.
Results
Patients administed additional analgesics during the maintenance period of intravenous patient-controlled analgesia were significantly lower in the nerve block group (p = 0.007). In addition, the volume of blood loss from catheter drainage was significantly less at 2 and 3 days postoperatively (p = 0.013, p = 0.041, respectively) in the nerve block group.
Conclusion
In patients who underwent total arthroplasty with osteoarthritis, even if only single injection of nerve block, it is helpful postoperative pain control and the reduction bleeding.
480
TIME FOR A CULTURE CHANGE: PEER-ON-PEER (POP) ENTRANCE AND EXIT INTERVIEWS – IMPROVING THE WORKING ENVIRONMENT FOR TRAINEES IN ICU
1Birmingham Children’s Hospital, Birmingham, United Kingdom
Introduction
Peer-on-peer (POP) entrance and exit interviews have been used in business to determine reasons why people leave employment. The hypothesis: high staff turnover correlates with poor performance.
In medicine, these interviews have had a positive affect on trainees in an emergency medicine department. After employment of this novel method, staff became net promoters for the department, trainees became more engaged and problems within the department were highlighted early on.
1. Will it help the trainees get more out of their rotation through PICU?.
2. Can the information collected contribute to a positive sustainable change within the department?.
Methods
Interviews were conducted using an open source proforma with a variety of trainees within the PICU department; including trainees from emergency medicine, anaesthetics, intensive care and paediatrics. PICU fellows and registrars conducted the interviews. The findings were analysed using thematic analysis and presented in word cloud format.
Results
12 entrance interviews and 7 exit interviews were conducted within a six month period.
Entrance interviews highlighted that trainees wanted their PICU experience to include friendship and being part of a team as well as gaining clinical experience.
Exit interview highlighted issues with bedside teaching and feedback processes. Trainees highlighted excellence in team working, allied health professional roles and clinical experience.
Results were fed back to consultant meetings and have been a factor in the implementation of a new teaching programme.
Conclusion
The use of POP interviews highlights problems and excellence within the training rotation. Time taken to conduct the interviews could be a barrier to this process. Understanding issues within a department and flattening hierarchy can aid positive change.
482
PATTERNS OF 4% ALBUMIN FLUID BOLUSES IN A PAEDIATRIC INTENSIVE CARE UNIT
1Royal Children’s Hospital, Melbourne, Australia
2Murdoch Children’s Research Institute, Melbourne, Australia
3University of Melbourne, Melbourne, Australia
Introduction
In the paediatric intensive care unit (PICU) 4% Albumin is the preferred colloid for fluid boluses (FB). Patterns of administration have not been well categorized.
Objectives
We sought to describe the patterns of 4% Albumin FB administration in patients in a PICU.
Methods
We conducted a retrospective study of 4% Albumin FB in children admitted to the PICU, Royal Children’s Hospital, Melbourne between January 1 2017 and December 31 2018. Fluid boluses of interest were those between 2–25ml/kg and administered in less than 2 hours. We described demographic and clinical characteristics of patients as well as FB characteristics such as timing, dose and duration. We described the patterns of administration within the first 72 hours of PICU admission.
Results
During the study period, 212/2659(8.0%) of admitted patients received 359 FB over 223 admissions. The median age at admission was 120 days [IQR;8,1664] and the most common admission diagnoses were congenital heart disease (54.7% of admissions), cardiac medical disorders (14.8%) and sepsis (9.4%). The most common FB volumes were 5ml/kg and 10ml/kg; (median 10.0ml/kg [IQR;5.1,12.5]). The median duration was 58.0 minutes [IQR;29.5,65.0]. For 194/212(91.5%) of patients, 3 FB or less were administered. Time from PICU admission to administration of the first FB occurred at a median of 24 hours [IQR;7.0, 88.0]. At 24, 48 and 72 hours, 112/223(50.2%), 142/223(63.7%) and 163/223(73.1%) of included PICU admissions received a FB. By 72 hours, 207/359(57.7%) of all FB had been administered. The median volume per 24-hour period for the first 72 hours were 5.9ml/kg [IQR;0.0,11.8], 9.8ml/kg [IQR;4.9,14.70] and 10.0ml/kg [IQR;5.4,16.95] respectively.
483
CIRCUIT HAEMODYNAMICS DURING CITRATE ANTICOAGULATION IN CONTINUOUS RENAL REPLACEMENT THERAPY AT TWO MAJOR ICUS IN VICTORIA
1The Royal Melbourne Hospital, Parkville, Australia
2The Alfred, Melbourne, Australia
3The Austin, Heidelberg, Australia
4The University of Melbourne, Parkville, Australia
5Monash University, Melbourne, Australia
Introduction
Regional citrate anticoagulation (RCA) has become standard of care during CRRT. Practices are likely to vary by institution, although little has been described regarding circuit haemodynamics during RCA.
Methods
Retrospective analysis of non-ECMO CRRT minutely circuit data at two major mixed adult ICUs in Victoria over a year (May 2018 – May 2019) representing more than a quarter of all CRRT done in Melbourne, Australia.
Results
1150 circuits representing 1.9 million minutely recordings were analysed. RCA was used in 69% of cases and median circuit life was 21.0 (11.4–39.5) hours. CVVHDF with 50:50 dialysis to filtration (predominantly pre-dilution) was commonly utilised (84% of cases). RCA was employed in 77% and 50%. Blood flows were different (200mL/min, 130mL/min) as well as preferred access site (femoral, internal jugular). Citrated circuits failing due to clotting (47%, 54%) had circuit lives of 31.8 (16.7 – 52.8) and 38.6 (28.8 – 56.4) hours. Effluent dose differed, 40.3 and 33.5mL/kg/hr. Fluid removal was more aggressive at one site (145 and 109mL/hr). Clotted non-citrate circuits (64.1%, 64.7%) lasted 23.8 and 19.3 hours. Circuits that did not fail due to clotting, had a shorter circuit duration (16.9, 12.5 hours. The higher blood flow (and higher pre-dilution) centre had higher filter pressure (131mmHg, 94mmHg), more negative access pressure (−86mmHg, −30mmHg), higher return pressure (69mmHg, 40mmHg), but lower transmembrane pressure (105mmHg, 124mmHg).
485
HYPOXIC HEPATITIS IN CRITICALLY ILL PATIENTS; INCIDENCE, CAUSES, MORTALITY
1Division of pulmonology and critical care medicine, Department of internal medicine, Gangnam Severance Hospital, Seoul, South Korea
2Department of internal medicine, Gangnam Severance Hospital, Seoul, South Korea
Introduction
Hypoxic hepatitis (HH) characterized by centrilobular necrosis, and mainly diagnosed based on the following three criteria: (1) reduced oxygen delivery to liver cell or utilization by the liver, (2) rapid increase in serum aspartate aminotransferase (AST) level, (3) exclusion of other causes of liver injury. It is caused by variety conditions inhibiting the oxygen delivery to the liver cell. HH is reported to be related to an in-hospital mortality.
Methods
Among patients admitted ICU at Gangnam Severance Hospital from January 1 to March 31, 2018, we included the patients with a rapid increase in AST level above 5 times of the upper limit of normal after exclusion of other liver disease, and investigated the incidence and causes, in-hospital mortality of HH.
Results
For 3 months, among 721 ICU patients, HH occurred in 51 patients (7.0%). Most common cause of HH was cardiac failure (47.1%), followed by septic shock (33.3%) and respiratory failure (9.8%). All cause in-hospital mortality rate in 48 hours and 28 days was 35.3% and 54.9%, respectively. Factors significantly related with 48 hours and 28 days mortality were comorbidity of chronic kidney disease, blood urea nitrogen, creatinine, AST, alanine aminotransferase, total bilirubin, and C-reactive protein level on peak AST day. Especially, peak AST level above 800 IU/L was significantly related with in-hospital mortality at 48 hours and 28 days (Hazard ratio 3.696 and 2.207, respectively, p < 0.05).
487
CONTINUOUS RENAL REPLACEMENT THERAPY CIRCUIT HAEMODYANAMICS DURING EXTRACORPOREAL MEMBRANE OXYGENATION
1The Alfred, Melbourne, Australia
2The Royal Melbourne Hospital, Melbourne, Australia
3The Austin, Melbourne, Australia
4The University of Melbourne, Melbourne, Australia
5Monash University, Melbourne, Australia
Introduction
Up to 50% of patients undergoing extracorporeal membrane oxygenation (ECMO) require continuous renal replacement therapy (CRRT). There is a paucity of published studies of ECMO-CRRT. Excessively negative access pressures (APs) have been identified as an issue in non-ECMO circuits, however it is thought that excessively positive APs may be problematic in ECMO-CRRT. This relationship has not been well established or quantified.
Methods
Retrospective analysis of CRRT circuit pressures and events of patients undergoing veno-arterial and veno-venous ECMO at two mixed adult ICUs in Victoria, Australia between August 2016-May 2019. The distribution of circuit failure was visualised and on this basis four failure groups were established, <12hours (early), 12–24hours (intermediate), 24–48hours (late), >48hours (very late). Classification and regression tree (CART) analysis was performed on summary measures of pressures recorded during the first two hours. A CART-generated outcome variable was used as a time-varying covariate in an unadjusted Cox-proportional hazards model.
Results
90 patients underwent 231 CVVHDF (50:50 dialysis to filtration) treatments with 489,561 minutely recordings. Median circuit life was 29.0 [13.4–64.8] hours. Blood flow was 190mL/min, effluent rate 38.7mL/kg/hr and fluid removal 134 mL/min. CART analysis demonstrated a maximum AP ≥245mmHg to have 81% probability of failure within 24 hours, maximum AP <245mmHg in the first two hours gave 83% probability of failure after 12 hours and 59% chance of failure after 24 hours. Using first incidence of an AP of ≥245 mmHg as a time-varying covariate in an unadjusted Cox-proportional hazards model, the incidence of such an AP increases the hazard of failure by 89%, HR 1.89 [1.37 to 2.59] p <0.0001.
492
A SYSTEMATIC REVIEW OF THE USE OF INTRAVENOUS VITAMIN C IN THE TREATMENT OF SEPSIS AND SEPTIC SHOCK
1St George’s, University of London, London, United Kingdom
2Adult Critical Care, St George’s University Hospitals NHS Foundation Trust, London, United Kingdom
Introduction
Recent evidence proposes the use of intravenous (IV) vitamin C as adjunctive therapy in the treatment of sepsis and septic shock. Given that vitamin C deficiency is common in the critically ill, this approach seems plausible. However, vitamin C’s ability to reduce mortality in the critically ill remains unclear.
Methods
We performed a systematic review of the literature using PubMed, MEDLINE and Cochrane Library up to 10/06/2019. Relevant papers were hand searched for additional studies. Studies were screened based on inclusion and exclusion criteria. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines were adhered to. Studies were graded for risk of bias. The primary outcome measured was mortality at final follow-up. Secondary outcomes included duration of vasopressor support and length of stay (LOS) in intensive care unit (ICU).
Results
A total of 7 studies were eligible (3 randomised controlled trials (RCT’s) and 4 cohort studies). Overall, 4 studies showed no statistically significant difference in mortality when compared to controls, whilst 2 studies showed reduction in mortality. 3 studies (2 of which were RCT’s) reported statistically significant reduction in vasopressor support in favour of vitamin C, whilst 2 studies did not (both retrospective cohorts). 3 studies directly measured ICU LOS, and all showed no significant difference.
499
SEASONAL VARIATION IN SEVERE INFLUENZA REQUIRING EXTRACORPOREAL MEMBRANE OXYGENATION: A BINATIONAL, OBSERVATIONAL STUDY
1The Alfred Hospital, Melbourne, Australia
2Queensland Children’s Hospital, Brisbane, Australia
3St Vincents Hospital, Sydney, Australia
4The Prince Charles Hospital, Brisbane, Australia
5Fiona Stanley Hospital, Perth, Australia
6Geelong Hospital, Geelong, Australia
7The Royal Childrens Hospital, Melbourne, Australia
Introduction
The 2009 H1N1 influenza pandemic saw unprecedented numbers of patients with severe respiratory failure requiring extracorporeal membrane oxygenation (ECMO). However seasonal variation in the influenza phenotype is common, and little is known how this might impact outcomes in patients on ECMO.
Methods
This binational, multicenter, observational study was conducted in seven Australian and New Zealand adult and paediatric centers who had confirmed influenza patients on ECMO in 2017. Data were collected on the clinical syndrome and patient outcomes, and were compared to a previous database of the 2009 H1N1 outbreak.
Results
In 2017, 29 patients were commenced on ECMO as compared to 68 in 2009. The H3N2 strain was more common in 2017 compared to 2009 (14.2 vs 0%), and a venoarterial ECMO mode was used more commonly (14 vs 4%). Patients in 2017 were older (47 vs 30 years), had higher plasma lactate levels (5.8 vs 2.4 mmol/L) and had higher creatinine levels (144 vs 83 umol/L) on initiation of ECMO, however they were less hypoxic (PaO2:FiO2 ratio 76 vs 51 mmHg) (p < 0.05 for all). Proning was less common in 2017 than in 2009 (19.7 vs 7.1%). The duration of ECMO in 2017 was similar (10 vs 12 days), however mechanical ventilation duration was shorter (14 vs 26 days). Hospital mortality was higher in 2017 compared to 2009 (34.5 vs 22.1%).
Conclusion
Significant seasonal variation exists between different strains of Influenza virus, phenotypes and outcomes. These factors should be considered when weighing the potential benefit of ECMO.
500
CARDIAC TAMPONADE DURING VENOARTERIAL EXTRACORPOREAL MEMBRANE OXYGENATION. PREVALENCE, ECHOCARDIOGRAPHIC DIAGNOSIS, AND OUTCOMES
1The Alfred Hospital, Melbourne, Australia
Introduction
Cardiac tamponade during venoarterial ECMO (V-A ECMO) is a potentially life threatening complication; however, little is known about distinguishing this from asymptomatic pericardial effusion. On one hand, echocardiographic features of decompression of the right heart during V-A ECMO can result in over diagnosis of cardiac tamponade and unnecessary interventions, while on the other hand, delays in the diagnosis can lead to inadequate V-A ECMO flow with profound haemodynamic instability.
Methods
This retrospective, observational study included all V-A ECMO patients at a high volume ECMO center in Australia. All patients with large pericardial effusions were identified from prospectively collected ECMO and echocardiography databases. Patients who underwent surgical pericardial drainage were divided into those with a significant haemodynamic improvement (defined as a post-operative reduction in noradrenaline ≥10mcg/min compared to pre-operative rate) and those without a significant hemodynamic improvement. These groups were compared using standard statistical tests.
Results
From 2011 to 2017, 205 V-A ECMO patients were identified. 43/205 (21%) patients had large (>2cm) pericardial effusions, of which 28 underwent surgical drainage. 8/28 (29%) patients showed significant post-operative haemodynamic improvement. These patients were more likely to have larger pre-operative effusions (2.9 vs 2.1 cm, p < 0.01), higher lactates (3.3 vs 2.5, µmol/L p = 0.04), higher pre-operative noradrenaline doses (27 vs 14 mcg/min, p < 0.01), and were more likely to have right ventricular collapse on echocardiogram (88 vs 45%, p = 0.04). No significant differences in mortality or hospital length of stay were demonstrated between the two groups.
Conclusion
This study provides clinicians clear factors to assist in the diagnosis of pericardial tamponade during V-A ECMO. Further prospective studies will be needed to validate this approach.
504
THE GLOBAL NEED FOR ESSENTIAL EMERGENCY AND CRITICAL CARE
1Karolinska Institutet, Stockholm, Sweden
2Karolinska University Hospital, Sweden
3College of Medicine, Blantyre, Malawi
4Uppsala University, Sweden
5MUHAS, Dar es Salaam, Tanzania
Introduction
Critical illness is common globally and can occur in anyone – irrespective of age, gender or underlying diagnosis. Patients with critical illness require care, and require it quickly, anywhere in the hospital. This care is “Emergency and Critical Care” and is, at its core, the close observation, continual assessment and frequent treatment modifications required to manage critical illness. In hospitals throughout the world, emergency and critical care is neglected due to (i) the “vertical” disease-based and specialty-based approach used by health services; and (ii) a lack of commonly agreed definitions and criteria for the identification of critical illness and the provision of care.
508
SKIN BLOOD FLOW AND THENAR TISSUE OXYGENATION ARE NOT CORRELATED TO SYSTEMIC HEMODYNAMIC VARIABLES IN PATIENTS WITH CIRCULATORY SHOCK
1Department of Intensive Care, Erasme Hospital, Brussels, Belgium
Introduction
Despite hemodynamic stabilization after resuscitation, tissue hypoperfusion may persist in circulatory shock patients. The ultimate goal of therapeutic interventions – such as volume expansion (VE) and red blood cell transfusion (RBCT) – is to improve oxygen delivery in order to correct tissue hypoxia.
Methods
Hemodynamically stabilized patients with circulatory shock undergoing VE or RBCT were included. Circulatory shock was defined as the presence of norepinephrine to maintain MAP ≥65 mmHg with ≥1 signs of tissue hypoperfusion (oliguria, alteration of consciousness, mottled skin) or lactate ≥2 mmol/L.
SBF (Periflux 5000, Perimed; index finger, Perfusion unit) and StO2 (near-infrared spectroscopy; InSpectra TM Model 325) were measured before and after VE or RBCT. A vaso-occlusive test was also performed to calculate the StO2 ascending slope (AscStO2) (%/min) following the end of the vaso-occlusion. Systemic hemodynamic parameters such as mean arterial pressure, cardiac index, lactate and ScvO2 were obtained at the same time as SBF and StO2 measurements. Changes in variables were calculated as relative percent changes.
Results
24 circulatory shock patients (VE = 9, RBCT = 15) were studied. After interventions AscStO2 increased in VE patients (p = 0.04) but did not change in RBCT patients. RBCT was associated with increased MAP (p = 0.01). There were no changes in other examined parameters following interventions.
Changes in SBF did not correlate to changes in MAP (r = 0.41 p = 0.3), cardiac index (r = 0.10 p = 0.3), ScvO2 (r = 0.07 p = 0.24) or lactate (r = −0.18 p = 0.9). Also, AscStO2 did not correlate to changes in MAP (r = 0.36 p = 0.9), cardiac index (r = 0.56 p = 0.1), ScvO2 (r = −0.08 p = 0.9) or lactate (r = −0.12 p = 0.9).
513
CENTRAL LINE INFECTION PREVENTION IN ICU PATIENTS: AN OPEN LABEL RANDOMIZED PILOT TRIAL OF A CHLORHEXIDINE LOCKING DEVICE
1Mcmaster University, Hamilton, Canada
2Hamilton Health Sciences, Hamilton, Canada
Introduction
Critically ill patients are at risk for central-line associated bloodstream infection (CLABSI) with an incidence up to 6.9 per 1000 catheter days. CLABSI impacts patient mortality, increasing a) hospital length of stay and b) risk of readmission. Our preclinical work demonstrated a device that diffuses the anti-microbial agent, chlorhexidine gluconate into the intravenous (IV) lock solution decreased bacterial growth. We designed and implemented a clinical trial to test this device.
Methods
Patients admitted to 3 ICUs at a single academic hospital with a central venous catheter were randomized to device or usual care within 72 hours of ICU admission. Exclusion criteria included treatment for infection, chronic indwelling catheters and chlorhexidine allergy. Blood cultures were collected every 48 hours. A survey was developed to assess the device acceptance by ICU nurses. The device sponsor, ICU Medical had no input into study design or analysis.
Results
Between November 2017 and May 2019, 169 (4.9%) of the 3462 patients screened met our eligibility criteria and 90 (83%) of the 109 patients and substitute decision makers approached consented to randomization. We randomized 1.2 patients/week. Survey respondents indicated “Urgent IV access required” was the most common reason for failing to adhere to the protocol. Patients had a venous catheter in situ for a mean (SD) of 10.4 (4.7) days, giving a total of 933 catheter days for all patients and 65 positive blood cultures were collected from 29 patients.
514
USE AND IMPACT OF SOCIAL NETWORKS BY CRITICAL AND INTENSIVE CARE JOURNALS
1Medical Internist, Cardiologist. Intensive care unit. University Hospital San Ignacio., Bogotá DC, Colombia
2Internist, Fellow, critical medicine and intensive care. Pontifical Javeriana University. Intensive care unit. Department of Internal Medicine. University Hospital San Ignacio., Bogotá DC, Colombia
3Internist, Clinical Epidemiologist, Department of Internal Medicine, University Hospital San Ignacio., Bogotá DC, Colombia
4Medical Internist, Rheumatologist. Rheumatology Unit. University Hospital San Ignacio., Bogotá DC, Colombia
Objetive
The growing use of social networks has changed the way of acquiring and taking advantage of knowledge, but the current metrics of scientific articles do not allow to properly know the use of forms of knowledge dissemination. This study aims to evaluate the correlation between the activity in social networks of journals of critical care and ntensive medicine, and traditional metrics.
Methods
We carried out a correlation study, between SCImago Journal Rank (SRJ), SJR quartile, H index and the activity on Twitter, Facebook, Youtube and Instagram. Data from the The intensive care journal database of the SCImago Journal & Country portal was consulted. The correlation between the metrics of dissemination in social networks and the Scimago Journal Rank and H index was evaluated through the Spearman correlation coefficient.
Results
We included 91 journals, of which 26 (28%) had social networks, the SJR of journals with networks was significantly higher than those that did not (n = 0.94 Vs 0.19 p = 0.0002). The most used social network was Twitter with 23 magazines (25%), followed by Facebook with 15 magazines (16.6%). We found a good correlation with the number of followers both on twitter (r = 0.7 p <0.05), and on Facebook (r = 0.56 p <0.05) and with the number of publications on twitter (r = 0.64 p <0.05) and.
Conclusion
The use social networks correlates directly and significantly, with the impact factor in intensive care journals. Despite the above, there is a underutilization of the same by intensive care journals. However, the use of social networks by intensive care journals is limited.
519
APPROACES FOR AN EFFICIENT USE OF DONATED EQUIPEMENT IN A NEONATAL ICU (NICU) FROM DEVELOPING COUNTRY
1Neonatal Reanimation Unit no.1, Perinatal Center, Clinical Municipal Hospital No.1, Chisinau, Moldova (the Republic of)
Introduction
Survival of critical ill or very premature newborns nowadays relies a lot on medical staff skills to use divers complicated equipment. Perinatal centers in developing countries (as neonatal ICU in our hospital) may receive this equipment through donation projects, their sustainability depending (after donors leaves) on local management and maintenance.
Methods
1) Observation of use/misuse during utilization of equipment, noticing the variety and frequency of equipment-induced complications as – baro-volutraumas on ventilators, hyper/hypothermia, skin injuries, frequency of blurred alarms on screens. 2) Accuracy of inscriptions in the registry of technical problems. 2) Weekly staff (medical team +/- bioengineers) meetings. 3) Pre-post evaluation of internal teachings.
Results
More frequent noticed errors/misuse moments were: for ventilation devices – not using correct Tidal Volumes; for thermoregulatory equipment (incubators, radiant warmers) – using mostly “air mode” instead of “skin mode”; for probes – checking the skin status where sensor is fixed more rarely that every 6 hours; for alarms – setting dangerously low limits for extremely premature babies; for the registry – verbal reporting leads to late solving of the problem, but writing reporting (even considered too bureaucratic at the beginning) – to an earlier damage repair.
