Abstract

Awake fibreoptic intubation (AFOI) is an important technique for the management of difficult airways. Effective anaesthesia of airway structures minimises patient discomfort, improves patient cooperation, reduces the need for supplemental sedation and is thus critical to the safety and success of AFOI.
Many techniques for anaesthetising the airway have been described in the literature. These include direct application (e.g., gargling, soaked pledgets, etc), nebulisation and atomisation of local anaesthetics, the ‘spray as you go’ technique as well as regional anaesthesia. 1 These techniques are associated with varying efficacy, complexity and patient tolerability. Thus, there is unlikely to be an ‘one size fits all’ method for all patients. The proceduralist performing AFOI should be familiar with a range of topicalisation techniques, carefully selecting the most appropriate technique for each situation.
We report a case where topicalisation of the airway was achieved by directly injecting local anaesthetic into the lumen of high flow nasal oxygen (HFNO) tubing, which generated droplets that rapidly resulted in dense anaesthesia of the entire airway. Written informed consent was obtained from the patient for the report of this case.
An 83-year-old lady, who had a recent mandibulectomy for squamous cell carcinoma of her left parotid gland, presented for planned free flap repair of her neck defect. On airway examination, she was Mallampati class 4, with very limited mouth opening (2 cm) and tongue protrusion. Previous videolaryngoscopy was documented as ‘very difficult’. During her recent mandibulectomy, she underwent nasal AFOI after topicalisation with 2% lidocaine using the MADgic™ laryngotracheal atomisation device (Teleflex®, Morrisville, NC, USA), which was supplemented by the ‘spray as you go’ technique. She described the AFOI experience as ‘very uncomfortable’. For the present case, the decision was made to secure her airway again with nasal AFOI but using the HFNO topicalisation technique.
The patient was first premedicated with 200 μg intravenous glycopyrrolate and her nasopharynx was sprayed with a premix of 5% lidocaine and 0.5% phenylephrine (Co-Phenylcaine™ Forte, ENT Technologies®, Hawthorn East, Victoria). While the patient was in a semi-recumbent position, HFNO cannula was applied and oxygen flow rate was slowly increased to 50 l/min. The patient was instructed to take deep breaths through her nose. Next, 15 ml of 2% lidocaine was slowly injected over two minutes into the lumen of HFNO tubing near the nasal cannula using a 30G needle, angled towards the patient (Figure 1). The injection was synchronised to the patient’s inspiration. Tubing at the point of injection was elevated to facilitate egress of any lidocaine that pooled within the HFNO lumen. AFOI was subsequently performed using an aScope™ 5.0/2.2 fibreoptic bronchoscope (Ambu®, Warriewood, NSW). After visualisation of the carina, remifentanil target-controlled infusion was commenced with the effect site target set at 2 ng/ml, and a size 6.0 nasal tube was then railroaded. No additional topicalisation was required and the entire procedure was well tolerated by the patient. Once the tracheal tube position was deemed satisfactory, general anaesthesia was induced, the patient was paralysed and positioned supine. Her surgery proceeded uneventfully. On postoperative follow-up, the patient reported that AFOI using the HFNO topicalisation technique was more comfortable than her previous experience.
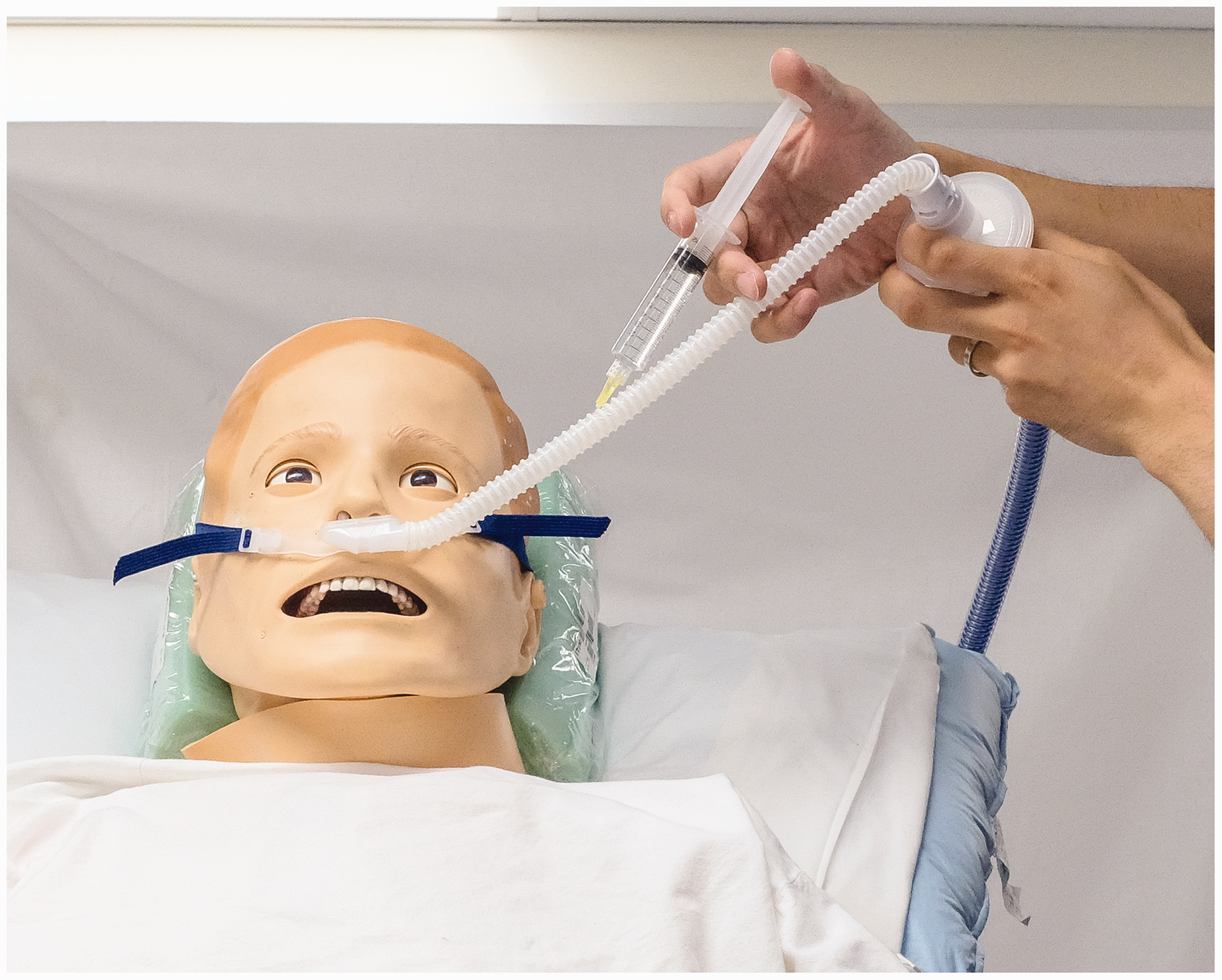
Setup for airway topicalisation via high flow nasal oxygen device.
The main advantages of the HFNO topicalisation technique are that it is simple, fast and non-invasive. This technique is particularly suitable in patients with a severely limited mouth opening, which precludes effective topicalisation via the oral route. Also, HFNO could be continued during AFOI, which may assist patients with reduced respiratory reserve (e.g., already dependent on HFNO support).
The main disadvantage of the technique is the inability to precisely control droplet size and consistent spread. Consequently, anaesthesia below the glottis may occasionally be unreliable and would require supplementation using the ‘spray as you go’ technique. Furthermore, local anaesthetic droplets seem to preferentially exit from the nasal cannula that is distal to the oxygen tubing, potentially resulting in uneven topicalisation of the nasopharynx. We find both disadvantages may be partly overcome by slowing the rate of injection (over at least two minutes) and using a finer bore needle (e.g., 27G or 30G), resulting in droplet sizes that optimise spread. The success of this technique also requires an adequate volume of local anaesthetic (at least 15 ml in our experience) as well as good inspiratory effort by the patient. Another disadvantage of this technique is the potential for increased aerosol generation associated with the use of HFNO devices, a particular concern during the current COVID-19 pandemic. 2
The HFNO topicalisation technique shares some similarities with the technique recently described by Bhalotra, 3 whereby 2% lidocaine solution is directly injected into the oropharynx via a carefully positioned nasopharyngeal airway. However, topicalisation through HFNO devices eliminates the risk of airway trauma associated with nasopharyngeal airway insertion as well as the risk of inadequate topicalisation associated with suboptimal nasopharyngeal airway placement.
We have now applied this topicalisation technique to more than 20 patients with good overall success and minimal discomfort being reported. Thus, we believe topicalisation via HFNO devices is another useful addition to the armamentarium of techniques for the management of the difficult airway.
Footnotes
Author contribution(s)
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
