Abstract
Abstract
Introduction: The friction generated during orthodontic treatment seems of concern in terms of anchorage and treatment duration. Different ligation methods have been developed to reduce the friction as compared with regular elastic modules. This study aimed to evaluate and to compare static and kinetic friction generated in ceramic brackets with metal slot and epoxy resin-coated stainless steel esthetic wire by using different ligation materials in wet condition (artificial saliva).
Materials and Methods: A total of 40 epoxy-coated stainless steel wires and metal slot ceramic brackets were divided into 4 groups of 10 each and ligated using 4 different methods as follows: (1) super slick elastic modules, (2) slide elastic modules, (3) Teflon-coated esthetic stainless steel wire, and (4) regular elastic modules. They were then immersed in artificial saliva for 1 hour before testing their static and kinetic friction using a universal testing machine.
Results: The intergroup comparison showed statistically significant differences for static and kinetic friction among all the 4 groups, where group 2 (slide modules) showed the least static as well as kinetic friction as compared with the other 3 groups.
Conclusions: (1) Slide modules produced the least amount of friction compared with all other methods of ligation when epoxy resin-coated stainless steel archwire was used in ceramic bracket with 0.22˝ metal slot in wet condition. (2) Super slick modules produced the least friction in comparison with regular elastomeric and Teflon-coated ligature groups but produced greater friction than slide modules. (3) Teflon-coated stainless steel ligature produced the highest friction; however, it was not statistically significant when compared with the conventional elastic ligature. (4) In all clinical situations during the retraction stage, a large amount of friction is created in the buccal segment; hence, it is advisable to use slide modules in the buccal segment to reduce static and kinetic friction.
Keywords
Introduction
The nature of friction in orthodontics is multifactorial, derived from a multitude of mechanical factors such as archwire material, cross-section shape and size, surface texture, stiffness, ligation of archwire to bracket, bracket material, slot width and depth, bracket design, and biological factors such as saliva, plaque, acquired pellicle, and corrosion. 1 The magnitude of friction depends on the amount of normal force pushing the 2 surfaces together, which is decided by the method of ligation, surface roughness, and nature of the surface material. The method of ligation is an important contributor to the frictional force generated at the bracket-archwire interface. Loosely tied stainless steel ligation is supposed to generate less friction. The new slick modules claim to reduce friction when compared with the regular elastic modules. 2 The self-ligating bracket generates lesser friction than the conventional bracket. 3
The chemical characteristics of alumina on a ceramic surface of the bracket can cause a metal wire to adhere to the alumina surface. A high friction can cause debonding of the brackets and can reduce the orthodontic force by 12% to 60%, making it difficult to apply optimal force. In an attempt to lessen the problems associated with friction, a combination bracket in which a metal slot was inserted into a ceramic bracket was introduced. 4 Coated metallic archwires are currently the only esthetic orthodontic archwires available for clinical use. Materials used in coating are plastic resin such as synthetic fluorine-containing resin or epoxy resin composed mainly of polytetrafluoroethylene to simulate tooth color. The epoxy coating is manufactured with a depository process that plates the base wire with an epoxy resin of approximately 0.002 thickness. Thus, a strong adhesion is achieved between the epoxy coating and the wire. When the frictional behavior of plastic-coated archwires was compared with noncoated reference wires by the same manufacturer, plastic coating was found to play a significant role in decreasing friction. 5
Ceramic brackets produced a higher frictional force than metal-insert ceramic brackets against polycoated and conventional NiTi wires; however, the frictional forces of epoxy resin wire against the 2 types of bracket during loading were not significantly different. 6
When these ceramic brackets were compared with the conventional ligation technique with low-friction ligature systems (Slide and Neo-Clips), a significantly greater amount of force was released with low-friction systems when compared with conventional elastomeric ligation systems. 7
Nowadays, there is an increasing demand of esthetic treatment especially in adult patients; there are some major issues such as friction when we use ceramic bracket, but many authors have concluded that there is less friction in ceramic bracket with metal slot compared with conventional ceramic brackets; hence, the purpose of this study was to evaluate the kinetic and static friction generated in 0.22″ metal slot ceramic bracket system (Clarity; 3M Unitek, Monrovia, CA, USA) with Ultraesthetic Tooth-Colored Archwires-Epoxy Coated; using 4 different ligatures, we evaluated which combination generated the least friction.
Slide modules had been compared with either stainless steel bracket or coated wire in the previous studies; however, in this study, a combination of slide modules with ceramic bracket, metal slot (0.022″), epoxy resin-coated (19″ × 25″) wire, and other ligation methods was analyzed, which till date has not been done.
Aim and Objective
Aim
The aim of this study was to evaluate and compare the static and kinetic friction generated in ceramic brackets with metal slot and epoxy resin-coated stainless steel esthetic wire using different ligation materials in wet condition (artificial saliva).
Objective
The objectives of this study were to
Evaluate the static and kinetic friction generated in ceramic brackets with 0.022″ metal slot and epoxy resin-coated 19 × 25 stainless steel esthetic wire using different ligation materials in individual groups in wet condition (artificial saliva). Compare the static and kinetic friction generated in ceramic bracket with metal slot bracket and epoxy resin-coated stainless steel esthetic archwire combination with super slick elastic module tie, slide module tie, steel ligation tie, and regular elastic module tie groups. Evaluate the static and kinetic friction generated in each group and compare between them.
Materials and Methods
A 0.019″ × 0.025″ epoxy-coated (G and H Ultraesthetic Tooth-Colored Archwires) stainless steel esthetic archwire of 30-mm size and preadjusted edgewise ceramic bracket with metal slot 0.022″ × 0.028″ of maxillary first premolar (Clarity™; 3M Unitek, Monrovia, CA, USA) were used for standardization as well as to simulate the buccal segment during the test.
8
The following ligation materials were used:
Super slick elastic modules (TP Orthodontics Inc, La. Porte, Indiana, USA). Slide elastic modules (Leone Orthodontics, Italy). Teflon-coated esthetic stainless steel ligature (Ortho-system). Regular elastic modules (Versa-Ties G and H).
A custom-made apparatus was constructed to hold the bracket wire assembly parallel to the universal strength-testing machine (model no. STS 248) (Figure 1), and artificial saliva was used to create a wet condition to simulate the oral environment while performing the test. 2 A total of 40 tests were performed in this study. For each group, 10 tests were performed, which are mentioned below.
Universal Testing Machine

Test Groups
Group 1: Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with super slick elastic module tie (Figure 2).
Group 2: Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with slide module tie (Figure 3).
Group 3: Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with Teflon-coated esthetic stainless steel ligation (Figure 4).
Group 4: Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with regular elastic modules (Figure 5).
Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with super slick elastic module tie

Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with slide module tie

Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with Teflon-coated esthetic stainless steel ligation

Ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire with regular elastic modules

Methods
Before tying modules, the bracket and archwire were cleaned with an alcohol wipe. Brackets were tied 25 mm from the upper end of the archwire to form the test unit. All the tests units were soaked in artificial saliva 1 hour before testing. Tests were performed on the universal testing machine with a crosshead speed of 20 mm/min over 10-mm slide of the bracket to form the test unit. The lower end of each test unit was attached to the heavy base block on the lower crosshead of the testing machine. 9
The bracket was pulled in the vertical direction with a special metal jig, which was fixed to the upper arm of the machine. Ten readings were taken per group. The force required for initiating the movement of bracket over the wire was measured as static friction. This was presented on the graph as the first peak during the test run. The force required for maintaining the movement over the 10-mm stretch was recorded as kinetic friction. This was measured as the mean value on the graph from 1 to 10 mm distance during the test run initially; the means and standard deviations (SDs) for all the values in each group were calculated.
Statistical Analysis
Descriptive and inferential statistical analyses were carried out in the present study. Results on continuous measurements were presented as mean ± SD.
The level of significance was fixed at P = .05, and any value ≤.05 was considered statistically significant.
Student’s t test (2-tailed, unpaired) was used to find the significance of study parameters on a continuous scale between 2 groups. The analysis of variance (ANOVA) was used to find the significance of the study parameters between 3 or more groups followed by post hoc analysis if the ANOVA values were significant.
The statistical software IBM SPSS statistics 20.0 (IBM Corporation, Armonk, NY, USA) was used for the analyses of the data, and Microsoft Word and Excel were used to generate graphs, tables, and so on.
Results
Table 1 shows the comparison of static friction (N) in terms of mean (SD) among all the 4 groups by using the ANOVA test. A statistically significant difference was observed (P < .001). Further using Tukey’s post hoc analysis, a significant difference was observed between group 1 and group 2 (P < .001), group 1 and group 3 (P = .028), group 2 and group 3 (P < .001), and group 2 and group 4 (P < .001).
Table 2 shows the comparison of kinetic friction (N) in terms of mean (SD) among all the 4 groups using the ANOVA test. A statistically significant difference was observed (P < .001). Further using Tukey’s post hoc analysis, a significant difference was observed between group 1 and group 2 (P < .001), group 1 and group 3 (P = .003), group 2 and group 3 (P < .001), and group 2 and group 4 (P < .001).
Comparison of Static Friction of All Groups Using ANOVA Test and Tukey’s Post Hoc Analysis
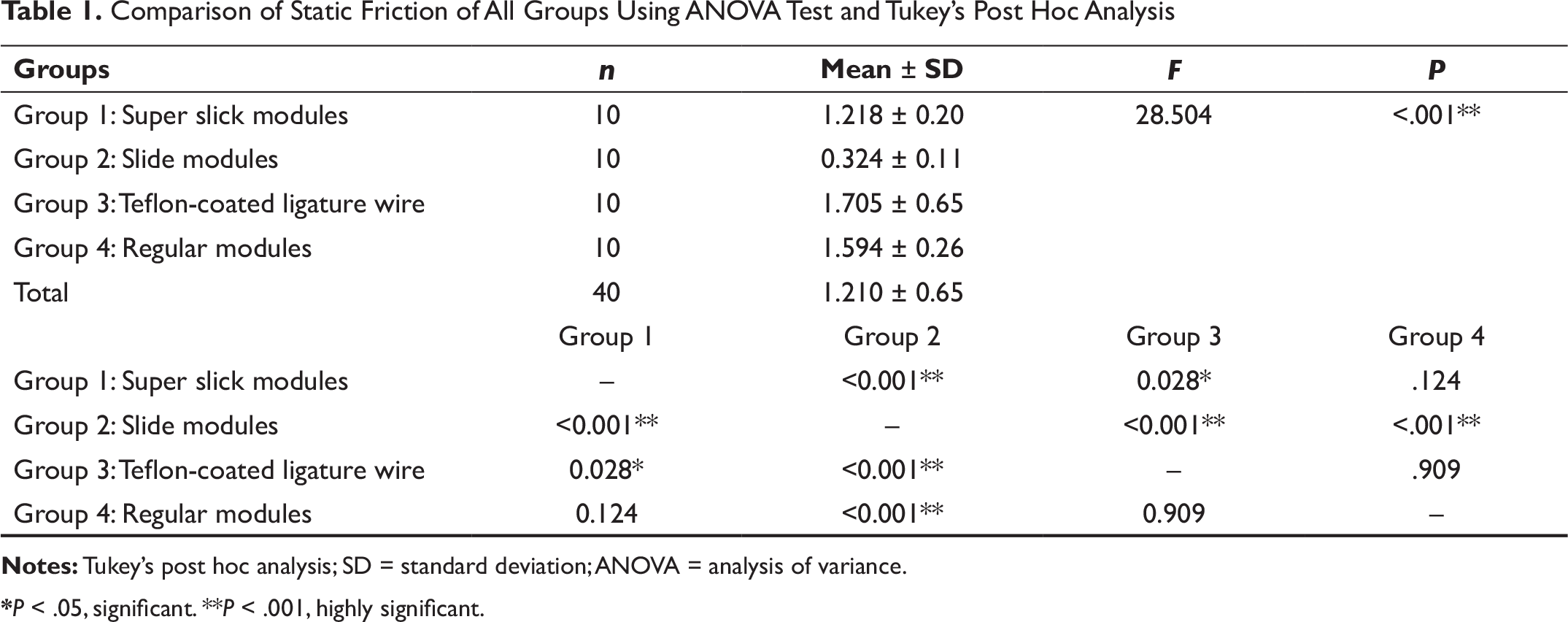
*P < .05, significant. **P < .001, highly significant.
Comparison of Kinetic Friction of All the Groups Using ANOVA Test and Tukey’s Post Hoc Analysis
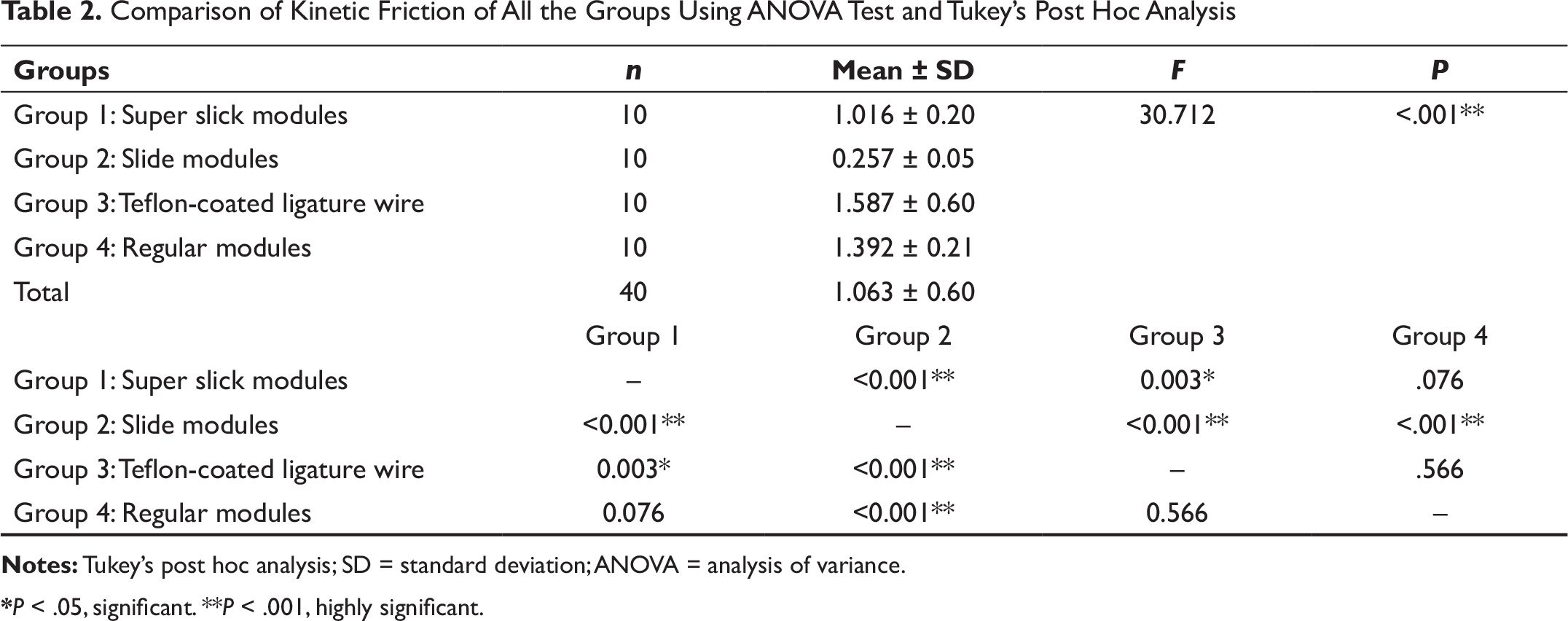
*P < .05, significant. **P < .001, highly significant.
Comparison of Static and Kinetic Friction Values Using Unpaired t Test
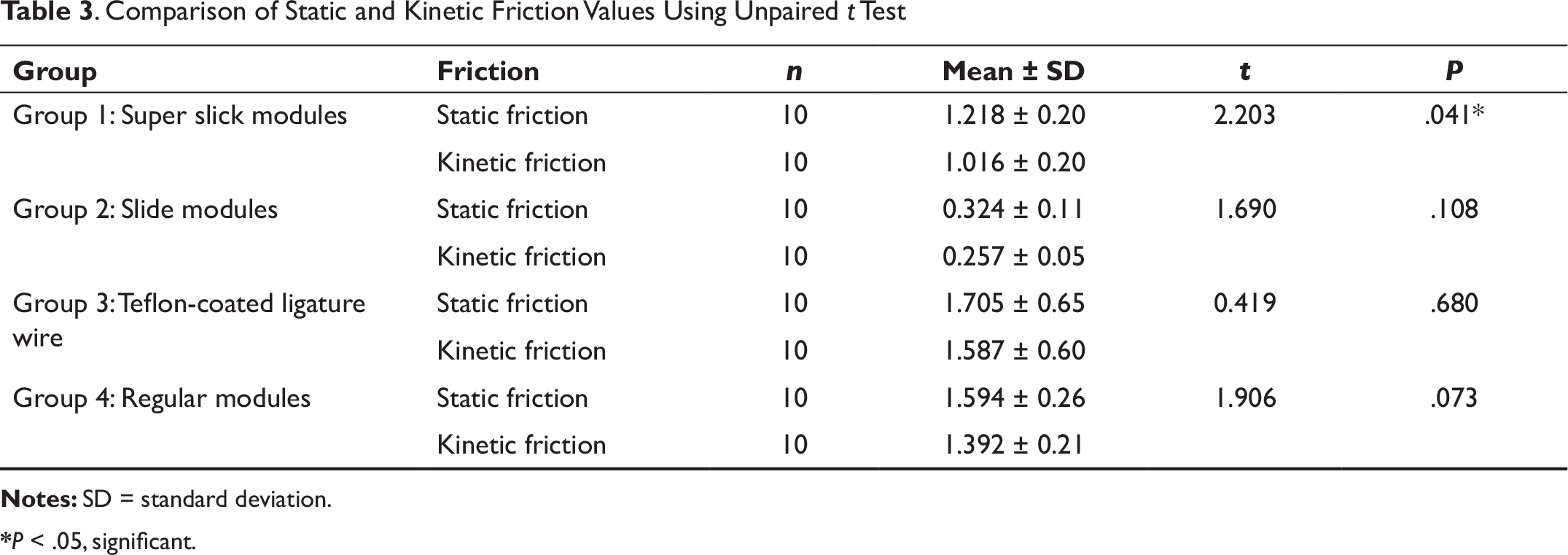
*P < .05, significant.
Discussion
Orthodontic tooth movement is objectively determined by friction between archwire and bracket interface. Mechanotherapy used for orthodontic tooth movement is always governed by the generation of friction between the bracket, wire, and ligature interface. It has been proven in previous studies that the material properties of the bracket, wire, and ligature and the amount of force by which the archwire is pressed against the bracket slot play important roles in the amount of friction generated. Tooth movement can occur only when tooth moving forces adequately overcome the friction at the bracket-wire-ligature interface. For these reasons, there is a continuous search for methods to reduce friction during tooth movement.
All materials have 2 coefficients of friction: static coefficient and kinetic coefficient. 10 Sliding between bracket and wire in the oral cavity occurs at a low velocity as a sequence of short steps rather than as a continuous motion. 11 In such conditions, Rossouw et al. found the distinction between static and kinetic frictional resistance is arbitrary because these 2 forms of friction are dynamically related. 12
In orthodontics, tooth moves through many tipping and uprighting cycles, moving in small increments during sliding movement. Therefore, as Oman et al. suggested, orthodontic space closure depends more on static friction than on kinetic friction. 13
When ligating the archwire to the bracket, friction produced by different methods varies because of different material properties and differences in the amount of force pushing the archwire against the slot surface. Iwasaki et al., 14 using an intraoral device, calculated that 31% to 54% of the total frictional force generated by a premolar bracket traveling along a 0.019″ × 0.025″ SS archwire was due to the friction of ligation. SS ligatures were used universally for the greater part of the 20th century until the introduction of elastomeric ligatures. Frank and Nikolai 11 compared the 2 ligation mechanisms and found that frictional resistance increased as the ligature applies greater force to the wire. They found that there was an insignificant difference between elastomeric ligation and a SS ligature tied with a force of 225 g.
Chimenti et al. 15 compared the frictional resistance seen with different-sized elastomeric ligatures. They concluded that there were no significant differences between small-sized (inside diameter 1.0 mm, outside diameter 2.6 mm, and thickness 0.85 mm) and medium-sized (inside diameter 1.3 mm, outside diameter 3.1 mm, and thickness 0.9 mm) ligatures. However, frictional force produced with large-sized elastomers was found to be 13% to 17% greater (inside diameter 1.6 mm, outside diameter 3.6 mm, and thickness 1.0 mm).
Polymeric-coated super slick ligatures were introduced in 2000. Manufacturers claimed that these ligatures generated lesser resistance to sliding than conventional elastomers. It was claimed that coated modules produced 50% less friction than all other ligation methods except self-ligating brackets.
De Franco et al. 16 suggested that recently Teflon-coated ligatures are being used with ceramic brackets to negate the esthetic problems associated with SS ligature wires and frictional disadvantages of transparent elastomers.
Fortini et al. 17 concluded that a new low-force ligation system made of special medical polyurethane, which was introduced recently, markedly reduces friction. The wire is free to slide as in a passive self-ligating bracket and it is claimed to cause lesser discomfort to the patient.
Drescher et al. 18 observed that the static friction and kinetic friction occurred at nearly the same time owing to the low crosshead speed of orthodontic tooth movement, and therefore, distinguishing between the static and kinetic frictional forces was difficult. Frank and Nikolai 11 used only the maximum kinetic frictional force because it was difficult to reproduce the kinetic frictional force in the oral cavity. Burrow 19 found that the static frictional force was more appropriate than the kinetic frictional force as orthodontic tooth movement is not continuous. On the other hand, Kusy and Whitley 20 measured both static and kinetic frictional forces. Tselepis et al. 21 used only the kinetic fictional force after the maximum static frictional force was reached because the static and kinetic frictional forces were constantly alternating as the tooth intermittently slide and bound along the archwire during orthodontic movements.
In this study, the maximum static frictional force and kinetic frictional force were measured because, logically, frictional values may vary for a given bracket–archwire combination.
The present study shows static friction to be significantly greater than the kinetic friction. Cacciafesta et al., 22 Taylor and Ison, 8 and Kapur et al. 23 also found similar results, with the static friction force always higher than the dynamic friction.
It was observed that friction for Teflon-coated ligature wire group was significantly higher than the other groups; however, there was no statistical difference when compared with the regular elastomeric ligatures group. De Franco et al., 16 Corbitt, 24 and Khamatkar et al. 25 have found that Teflon-coated ligation produced the least friction, which is in contrast to our study results; however, the frictional force found in the study by Khamatkar et al. 25 was comparable with that in our study. The possible reason for a higher static and kinetic friction obtained for Teflon-coated ligature wire group could be ligature tightening during every test, which cannot be standardized. Another reason could have been that in previous studies, different archwire bracket and ligation combinations were used, which could have affected the frictional forces.
In the present study, the “super slick” modules showed lesser friction than Teflon-coated ligation and regular elastomeric ligatures but produced more friction when compared with slide modules. Hain et al. 2 found that the recent “super slick” modules introduced by TP orthodontics produced less friction when compared with the regular counterparts, which is comparable with our study results. However, Griffiths et al. 26 compared “super slick” modules with round and rectangular modules and found that the frictional forces of slick modules are more than those of the regular round modules. The differences in values might be because of differences in the test apparatus of these studies and different inner diameters of modules.
Reduction in friction caused by slick modules has been explained on the basis of a polymeric coating on the module surface, which upon interaction with saliva becomes slippery and reduces friction at the archwire-bracket interface.
The present study shows that the slide modules produce the least amount of friction when compared with all other methods of ligation. Baccetti and Franchi 27 also found that the slide ligatures produced significantly lower levels of friction when compared with conventional elastomeric modules. This can be explained on the basis of the absence of normal force pushing the wire into the slot, which results in minimum friction at the bracket-wire interface, and module shape, which only produces force in the middle of the bracket. 28
The results obtained in the present study show that the slide modules introduced by Leone Orthodontics reduce friction significantly at the archwire-bracket interface. This could be very useful in the retraction stage of the treatment when the clinician wants minimum friction and full engagement of archwire in the bracket slot, especially in the buccal segment. The low-friction slide modules can reduce tissue damage, patient discomfort, and treatment time considerably.
The planning of orthodontic tooth movement is crucial because the use of proper bracket archwire and ligation technique can help to reduce frictional forces that occur between these interfaces; so, when we plan for esthetic orthodontic treatment, especially for adults, the ceramic bracket with metal slot bracket slide modules and epoxy resin-coated archwire combination should be used; we can use super slick modules only in the anterior segment to maintain torque and slide modules in the buccal segment during retraction.
Further investigations are required with a larger sample size to back up this study to compare the combination of wire, bracket, and ligatures with esthetic self-ligating bracket and also by simulating the oral condition.
This study shows that slide modules produce the least friction in the ceramic bracket with metal slot and epoxy resin-coated stainless steel esthetic archwire as these modules bind the archwire in the middle only. Other modules bind the archwire mesially and distally to the bracket, which probably produces more friction. This archwire binding force of modules is necessary in the initial phases of orthodontic treatment, such as alignment and leveling, rotation correction, and during torque expression as it requires complete wire engagement into the bracket slot. There is one more advantage of super slick modules: during individual canine retraction, we can use the same module as it helps in complete sitting of archwire and minimizes the rotational tendency of canine during retraction, which also helps to reduce the friction because of lubricious coating present on module; however, the force is much more than slide module.
As Patil et al. 28 conclude that slide module creates much less static and dynamic friction than other modules because of the shape of this module is different and it cannot bind the wire mesiodistally to the brackets; it only holds the wire passively into the bracket. Hence, depending on the treatment, we can use the low-friction module, such as during en masse retraction, using friction mechanics, we can use the super slick module in the anterior segment to avoid the torque loss by incomplete sitting of archwire into the brackets, and we can also use the slide module in the posterior segment to reduce the static and dynamic friction during the sliding of wire, and our study supports this suggestion. The system in the esthetic orthodontic treatment uses the conventional elastomeric module or Teflon-coated ligature wire. In this study, slide module was used, which is shown to produce less friction in combination with ceramic brackets with metal slot and epoxy resin-coated wire, as compared with the conventional elastomeric and Teflon-coated ligature wire ligation. It is the best alternative treatment modality against self-ligating ceramic bracket used for esthetic treatment or in adult patients, which will reduce cost burden on patients.
Conclusions
The conclusions of this study are as follows:
Slide modules produced the least amount of friction compared with all other methods of ligation when epoxy resin-coated stainless steel archwire was used in ceramic bracket with 0.22″ metal slot in wet condition. Super slick modules produced the least friction in comparison with regular elastomeric and Teflon-coated ligature groups but produced greater friction when compared with slide modules. Teflon-coated stainless ligature produced the highest friction, but it was not statistically significant compared with conventional elastic ligature. In all clinical situations, during the retraction stage, a large amount of friction is created in the buccal segment, and so, it is advisable to use slide modules in the buccal segment to reduce static and kinetic friction. It has other advantages such as it provides better tissue response, reduced root resorption, and less retraction time with faster space closure. It can be used as an option to self-ligating brackets, a more economical and clinical inventory.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
