Abstract
During the Syrian conflict, chlorine gas has increasingly been used as a chemical weapon, primarily causing acute respiratory injuries. However, chronic dermatological sequelae remain poorly documented, complicating long-term healthcare planning. A 70-year-old Syrian man developed pruritic ulcerative lesions on the scalp and exposed skin areas following chlorine gas exposure during a December 2016 airstrike. These lesions persisted for months after the initial exposure. Initial symptoms included ocular irritation, coughing, and dyspnea. These respiratory symptoms resolved within 48 hours; however, progressive skin changes developed. Physical examination revealed well-defined, erythematous, hyperkeratotic lesions exhibiting epidermal necrosis on the scalp and extremities. Associated findings included alopecia and hair follicle atrophy. Histopathological examination demonstrated epidermal hyperkeratosis, hypergranulosis, and dermal fibrosis with chronic perivascular inflammation. Based on clinical presentation, exposure history, exclusion of alternative etiologies, and histopathological findings, a diagnosis of chlorine-induced chronic dermatitis due to chemical warfare agent exposure was established. Treatment included oral cetirizine, prednisolone, and topical corticosteroids. At the 3-month follow-up, the chronic disease remained stable, with persistent hyperkeratotic lesions showing no significant improvement in size, erythema, or morphology. Clinicians should recognize chronic dermatopathology as an integral component of chemical warfare injuries. International health agencies should develop comprehensive registries to document long-term effects of gas exposure and to guide therapeutic strategies in conflict-affected populations.
Introduction
Chlorine (Cl2) is a yellowish-green gas with a characteristic pungent odor, resembling bleach, at room temperature. Cl2 exists as a clear to amber-colored liquid at temperatures below −30°F/−34°C or under elevated pressure conditions. 1 With a density approximately 2.5 times greater than air, Cl2 tends to accumulate in low-lying areas, making civilians in basements and shelters particularly vulnerable during attacks. Although Cl2 itself is noncombustible, it acts as a strong oxidizing agent that promotes combustion of other materials. 2
The risk of mass casualty exposure remains high due to the transport of Cl2 in large quantities through densely populated areas. 3 Cl2 exposure occurs through inhalation of elemental Cl2 gas or vapors from Cl2-releasing chemicals.4–7 Common exposure scenarios include transportation accidents,8,9 industrial leaks, malfunctions of the Cl2-disinfection system, 7 improper mixing of household bleach with acidic cleaners (producing chloramine gas), and laboratory accidents.8,10,11 However, Cl2’s toxic properties have led to its weaponization in chemical warfare, most notably documented in the Syrian conflict, where it has been systematically used against civilian populations. 1
Cl2 exposure produces multisystem toxicity, affecting the respiratory, cardiovascular, neurological, and psychiatric functions, with symptom severity correlating directly with both concentration and duration of exposure.1,12 The respiratory system bears the greatest burden of Cl2 toxicity, 13 with severe exposures causing immediate complications such as acute respiratory distress syndrome (ARDS), respiratory failure, pneumomediastinum, and death.14–18
Isolated case reports provide limited insights into cutaneous manifestations. The burn case reported by Norimatsu et al. 19 documented facial burns that resolved with residual hyperpigmentation. Pham et al. 20 reported reversible ARDS secondary to Cl2 inhalation during a pool-maintenance accident, with no documented cutaneous pathology. Papoff et al. 21 reported successful treatment of a 14-year-old patient with Cl2-induced pediatric ARDS using bronchoscopic lavage and surfactant therapy, and dermatological examination findings were normal. During household-cleaner incidents in China, seven adults demonstrated respiratory injury without cutaneous involvement, emphasizing the rarity of documented dermatological complications. 22 Collectively, these publications emphasize pulmonary toxicity while providing minimal insight into chronic dermatopathology. International health organizations recognize this knowledge gap; a 2023 systematic review concluded that no consensus exists for managing delayed Cl2 complications beyond general supportive care. 23
To our knowledge, our case represents the first documentation linking Cl2 warfare exposure with persistent, treatment-refractory dermatological lesions supported by histological evidence of epidermal hyperkeratosis, hypergranulosis, and perivascular fibrosis 8 years after exposure. By documenting alopecia and biopsy-confirmed chronic inflammation unresponsive to standard corticosteroid therapy, this report expands the recognized clinical spectrum of chemical weapon-induced injuries.
Case presentation
Chief complaints
A 70-year-old Syrian man from Aqirbat, in the eastern countryside of Hama, presented to the dermatology clinic with pruritic ulcerative lesions on the scalp and other exposed skin areas. These lesions had persisted for several months.
Personal and medical history
The patient had no significant medical history, was not taking medications, and reported no family history of cutaneous conditions, allergies, or chronic skin diseases. In December 2016, he was exposed to Cl2 gas during an airstrike on his village. He initially developed ocular and pharyngeal irritation, cough, and dyspnea, which resolved within 48 hours. However, progressive skin changes developed over the following months.
Physical examinations
Physical examination revealed well-defined, erythematous, hyperkeratotic lesions with epidermal and dermal necrosis affecting the scalp and exposed skin areas, including hands, forearms, legs, and neck. The lesions were painless and demonstrated a brown pigmentation pattern. Examination of the scalp revealed multiple areas of alopecia with hair follicle atrophy (Figure 1(a) to (d)). Vital signs remained stable, and systemic examination was unremarkable.

Baseline physical examination showing well-defined, erythematous, hyperkeratotic lesions with epidermal and dermal necrosis. Scalp involvement with alopecia and hair follicle atrophy (a, b). Lesions on hands, forearms (c), and legs (d).
Laboratory analysis and histopathological examination
Laboratory examinations, including complete blood count, hepatic and renal function tests, and inflammatory markers, were normal. Leishmania antigen testing was negative. Incisional biopsy of the scalp and dorsal hand revealed significant tissue fragility with suturing complications due to Cl2-induced dermal damage. Histopathological examination demonstrated epidermal hyperkeratosis, hypergranulosis, and dermal fibrosis with chronic perivascular inflammatory infiltrates. Mild edema was observed, with no signs of malignancy or granuloma formation (Figure 2).

Histopathological examination demonstrating epidermal hyperkeratosis, hypergranulosis, and dermal fibrosis with perivascular chronic inflammatory infiltrates.
Differential diagnoses
Four differential diagnoses were systematically evaluated based on clinical presentation patterns, histopathological characteristics, and exposure history.
Lichen simplex chronicus (LSC) was considered due to the hyperkeratotic morphology and its distribution on the scalp and extremities. However, exclusionary features included the absence of pruritus or scratching behavior, which represents the fundamental pathophysiological mechanism of LSC. Histopathology revealed hyperkeratosis and hypergranulosis but lacked the characteristic LSC triad: acanthosis with irregular elongation of rete ridges, compact orthokeratosis, and papillary dermal fibrosis with vertically oriented collagen bundles. The lack of lichenification patterns, the presence of painless lesions, and poor treatment response over 3 months further argued against this diagnosis.
Mycosis fungoides (MF) was also considered, given its ability to mimic chronic inflammatory dermatoses. However, histopathological findings excluded this diagnosis due to the absence of epidermotropism, a hallmark feature of early-stage MF. Atypical cerebriform lymphocytes and Pautrier microabscesses were absent. The poor response to 3 months of corticosteroid therapy, combined with negative histopathological findings, further reduced the diagnostic probability of MF.
Chronic contact dermatitis (CCD) was also considered due to the documented Cl2 exposure history. However, several factors argued against classic CCD: the lesions persisted for years after exposure, whereas allergic contact dermatitis typically resolves once the allergen is avoided. Histopathology showed a hyperkeratotic and fibrotic histological pattern, differing from the eczematous spongiosis changes characteristic of contact dermatitis. Additionally, the poor anti-inflammatory response over extended periods suggested mechanisms beyond standard contact hypersensitivity, further reducing the likelihood of CCD.
Cutaneous leishmaniasis (CL) was also considered because it is endemic in Syria. Negative Leishmania antigen testing excluded this parasitic infection. Histopathology showed no granulomatous inflammation or epithelioid cell granulomas, which are characteristic findings in chronic Old World CL. Clinical progression failed to follow the typical papule-to-nodule evolution pattern, and the stable hyperkeratotic morphology contradicted the expected ulcerative development of CL lesions.
Final diagnosis and therapeutic intervention
Clinical, histopathological, and temporal evidence support chronic Cl2-induced dermatosis with secondary hyperkeratotic changes. Five lines of evidence support this diagnosis: First, a well-documented temporal relationship exists between the December 2016 Cl2 gas exposure and subsequent progressive skin changes. Second, the initial acute presentation included ocular irritation, pharyngeal symptoms, and respiratory distress, characteristic of Cl2 toxicity. Third, the anatomical distribution of chronic lesions corresponds precisely to body surfaces exposed during the Cl2 gas incident. Fourth, histopathological findings demonstrate chronic inflammation and dermal fibrosis, consistent with postchemical injury tissue remodeling. Fifth, the treatment-refractory nature of these lesions, which showed minimal improvement despite appropriate anti-inflammatory therapy, aligns with documented cases of irreversible structural skin changes following severe Cl2 gas exposure. Tissue fragility during biopsy further supports chronic chemical-induced dermal damage. Cl2 causes direct cellular injury and subsequent fibrotic changes. These findings fulfill the established criteria for chemical-induced dermatoses, representing a chronic manifestation of Cl2 toxicity with persistent dermal remodeling.
Due to the absence of a specific Cl2 antidote, supportive therapy was initiated. Treatment consisted of oral cetirizine 10 mg daily, prednisolone 0.5 mg/kg daily for 3 weeks with gradual tapering, and topical corticosteroids twice daily to affected areas. Strict photoprotection was advised, including sun avoidance and broad-spectrum SPF 50+ sunscreen application.
Follow-up and outcomes
The 3-month follow-up revealed stable chronic disease, with persistent hyperkeratotic lesions and no significant improvement in size, erythema, or morphology (Figure 3). Pruritus symptoms persisted without significant improvement. No new lesions developed, and no adverse events occurred, demonstrating disease stability and treatment tolerability. Patient education emphasized the chronic nature of the condition, realistic treatment expectations, and the importance of protective measures and timely follow-up if symptoms worsen.
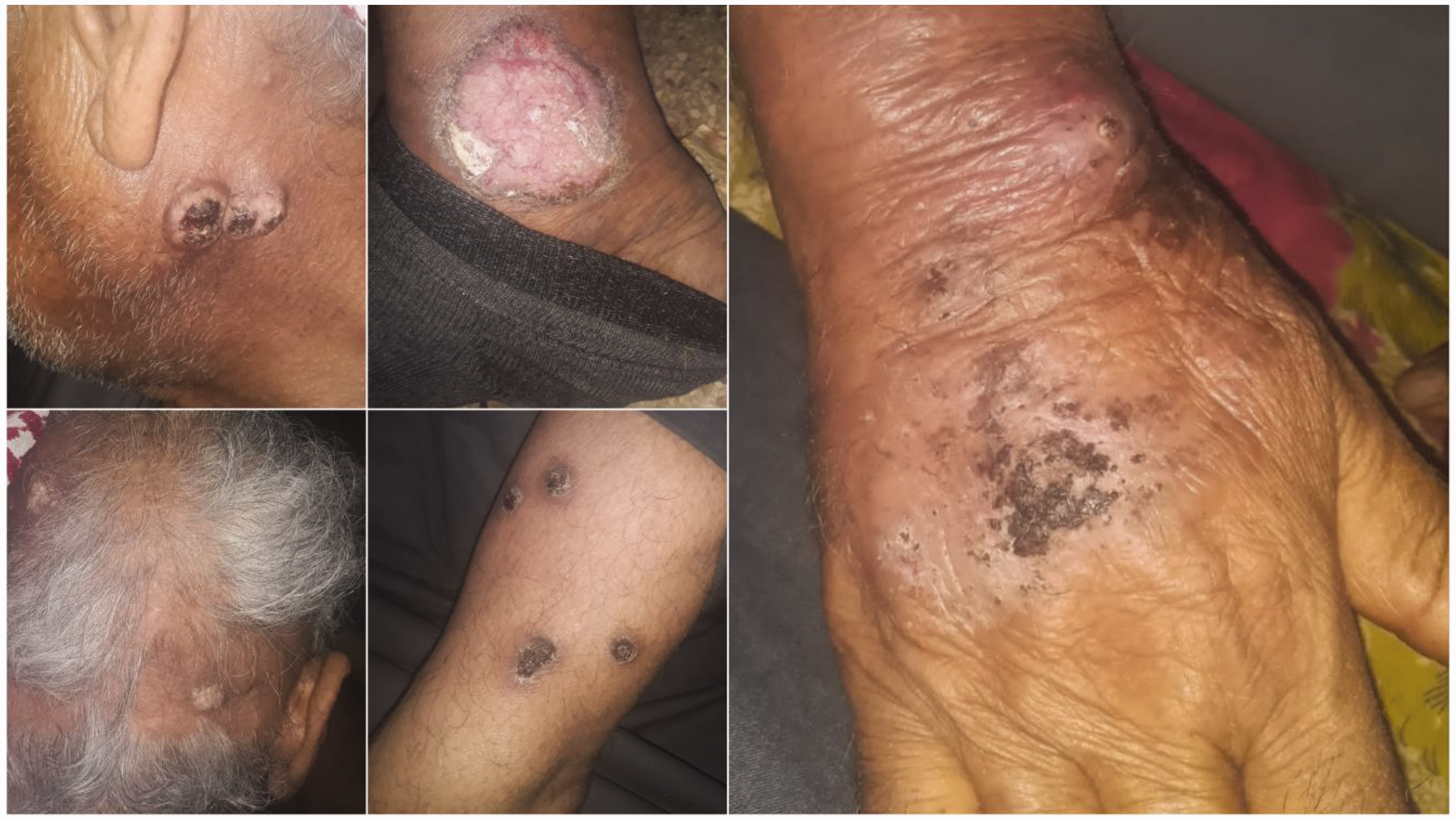
Three-month follow-up examination demonstrating persistent erythema and hyperkeratosis without significant improvement. No new lesions developed.
Discussion
Despite international prohibitions, Cl2 gas has been systematically employed as a chemical warfare agent throughout the Syrian conflict. The Organization for the Prohibition of Chemical Weapons fact-finding mission confirmed that the Syrian government used Cl2 against the civilian population,24,25 including documented attacks in Idlib and Sarmin during 2014–2015. 26 Analysis by Schneider and Lutkefend indicated that Assad’s regime utilized improvised Cl2 munitions in at least 89% of chemical attacks during the Syrian conflict. 27
Inhaled Cl2 gas reacts with mucosal water to form hydrochloric acid and hypochlorous acid. These acids generate reactive oxygen species, directly causing epithelial necrosis, vascular damage, and inflammatory responses. 1 Cl2 exposure causes immediate oxidative epithelial damage. Subsequently, activated neutrophils migrate to injury sites and release additional oxidants and proteolytic enzymes, amplifying tissue damage. The resultant oxidative injury affects the lower airways, upper respiratory mucosa, ocular surface, and skin. Damage is concentrated along the respiratory tract from the nasal cavity to the main bronchi, with severity escalating at higher concentrations. 5
Clinical manifestations of Cl2 gas exposure vary significantly based on exposure parameters (concentration and duration) and personal victim characteristics (age, gender, comorbidities, and smoking history).28–30 Cl2 gas concentration determines clinical manifestations and their severity. Low-level exposure (1–30 ppm) for up to 1 hour typically causes mild mucous membrane irritation. Higher concentrations (30–40 ppm) produce severe respiratory symptoms, including chest pain, dyspnea, and cough. Concentrations of 40–60 ppm characteristically cause acute pulmonary edema. 29 Concentrations exceeding 400 ppm typically cause death within 30 min, while exposure above 1000 ppm proves rapidly fatal.29,31 The patient experienced repeated Cl2 gas exposure during documented conflict-related chemical attacks. The delayed cutaneous manifestations suggest exposure concentrations below lethal levels, consistent with documented chronic effects of warfare-related chemical exposures.
Large-scale clinical studies have documented the spectrum of acute Cl2 toxicity following exposure incidents. Sever et al. 13 reviewed 39 victims of a Turkish water-purification tank explosion and reported cough (64.1%) and dyspnea (30.8%) to be the primary symptoms, with no documented persistent cutaneous complications. Similar findings emerged from Yunsur et al.’s 32 study, where coughing and dyspnea were the predominant symptoms in 18 patients (72%), with no mortality observed. An in vitro study by Sharyn et al. 33 demonstrated minimal Cl2 penetration through skin barriers up to 500 ppm, with slight enhancement observed with heavy cotton fabrics and oil-based sunscreens. However, comprehensive documentation of chronic dermatological sequelae remains notably scarce in the peer-reviewed literature. A systematic review by Govier et al. 34 analyzed Cl2 gas exposure in 1566 civilians across 37 incidents. The most common acute symptoms were cough (29%), dyspnea (22%), sore throat (16%), and eye irritation (12%). Chronic dermatological effects were not systematically addressed in this analysis, representing a significant literature gap. Although acute effects, including respiratory symptoms, ocular irritation, and immediate skin reactions, 35 are well-characterized, dermatological manifestations remain inadequately studied. Acute skin effects include irritation, pain, chemical burns, and blister formation, with severity dependent on exposure intensity. 1 Chronic cutaneous sequelae have received limited systematic investigation. This case report presents the first documented evidence of chronic, treatment-resistant dermatological sequelae following Cl2 gas exposure in a conflict setting. Our patient developed chronic cutaneous manifestations, including persistent ulcerative plaques, hyperkeratosis, alopecia, and perivascular inflammation on histopathology. Norimatsu et al. 19 described the case of a 40-year-old woman with 4.5 hours of Cl2 gas exposure in an enclosed space, who developed acute facial chemical burns and corneal erosion. Norimatsu et al. 19 reported prolonged enclosed-space exposure, but follow-up skin findings were unavailable, precluding comparison with our patient’s delayed chronic lesions. Our observations challenge the prevailing view that Cl2 causes only transient skin irritation. Delayed lesions after repeated low-dose exposure indicate that sublethal concentrations can still induce significant cutaneous injury.
Unlike the acute respiratory effects documented in the Douma and Saraqib Cl2 attacks,24,36 our case demonstrated potential chronic dermatological sequelae. This finding suggests the need for long-term monitoring of conflict-related chemical exposure survivors. The latency period of several months in our patient significantly exceeded the 24–72 hour onset observed in acute industrial Cl2 exposures.37,38 This extended timeline suggests distinct pathophysiological mechanisms in chronic low-level exposures. Moreover, the prolonged latency period complicates causal attribution, reflecting the diagnostic challenges inherent in conflict zone medicine, where documentation and follow-up are often limited. Despite these limitations, the temporal relationship and clinical pattern support Cl2 exposure as the likely cause.
Given the complexity of diagnosing Cl2 exposure, clinical evaluation requires integrating exposure history, symptomatology, available biomarker evidence, and radiological findings. Optimal assessment involves consultation with chemical, biological, radiological, and nuclear (CBRN)-trained physicians familiar with chemical warfare agent toxicology. 31 Metabolic acidosis secondary to hyperchloremia may develop after the absorption of hydrochloric acid when Cl2 reacts with water. Arterial blood gas analysis confirms this hypoxic state.39,40 Although chest radiographs are frequently normal, imaging should be obtained to exclude pulmonary edema, pneumonitis, or ARDS. Computed tomography and endoscopy assist in evaluating and managing severe injuries.41,42
Currently, no established biomarkers exist for detecting Cl2 exposure or locating Cl2 gas leaks and attacks. Moreover, the few candidate biomarkers under investigation remain confined to preclinical studies, rendering them unreliable for clinical diagnosis of Cl2 exposure. 31 Recent advances in exposure biomarkers have identified chlorinated phospholipids as promising indicators of Cl2 gas exposure. In vitro studies demonstrated chlorinated phosphatidylcholine formation in Cl2-exposed pig lung tissue, suggesting that similar compounds could potentially be isolated in human skin biopsies to confirm exposure history. 43 Although these biomarkers show promise for forensic verification of Cl2 exposure, they were not analyzed in our case due to the limited availability of specialized analytical methods.
Balakrishna et al. 44 demonstrated in murine models that Cl2 exposure causes significant vascular damage, as evidenced by elevated levels of vascular damage markers. These included serum amyloid P component, fibrinogen, adiponectin, and soluble vascular cell adhesion molecule 1. These vascular injury markers highlight Cl2’s ability to trigger prolonged systemic inflammation, potentially explaining the delayed dermatological manifestations observed in our patient. Histopathological examination revealed epidermal hyperkeratosis, dermal fibrosis, and chronic perivascular inflammation, consistent with prolonged oxidative tissue injury. Cl2-derived reactive oxygen species directly oxidize cellular lipids and proteins, triggering fibroblast activation and subsequent collagen synthesis. 43 These oxidative stress pathways explain both the delayed onset and persistent nature of the dermatological sequelae in our patient.
No specific antidote exists for those exposed to Cl2 gas. Treatment protocols for Cl2 exposure primarily focus on symptomatic management, addressing complications such as respiratory edema, bronchospasm, and upper and lower airway obstruction.5,18 Prehospital management of Cl2 exposure includes removing victims from the exposure site and providing supplemental oxygen. 1 Decontamination aims to minimize the risk of continued exposure to victims and protect healthcare workers from secondary contamination. Airway management is essential in the immediate treatment of any toxic inhalation. 13 Inhaled beta-agonists are administered to manage bronchospasm. 45 Patients experiencing ocular symptoms, including pain, photophobia, and vision changes, require immediate eye irrigation with water or saline solution. Ophthalmological examination should assess for corneal abrasions using fluorescein staining. For dermal injuries, contaminated clothing should be removed and the affected skin thoroughly irrigated with copious amounts of water. 13 Standardized triage protocols optimize the prioritization of therapeutic interventions, particularly during mass casualty events. 1
Hospital management includes humidified oxygen therapy and nebulized bronchodilators for symptomatic patients. 9 Intubation may be required for patients experiencing severe respiratory distress. Endotracheal intubation is indicated for severe respiratory distress, ARDS, or impending respiratory failure. Although animal studies demonstrate that corticosteroids reduce acute lung injury following Cl2 exposure, clinical evidence in humans remains limited.23,46,47 Evidence supporting nebulized sodium bicarbonate and corticosteroids is primarily anecdotal.48–50 Managing chronic skin lesions from Cl2 gas exposure presents significant challenges due to poorly defined protocols and limited evidence-based treatment strategies. Although the WHO chemical-incident guidelines comprehensively address respiratory complications, they provide no explicit protocols for long-term dermatological surveillance in follow-up care. Current guidelines recognize immediate skin contact risks and emphasize decontamination and acute care. However, they fail to establish systematic protocols for long-term dermatological monitoring. 51 Tissue fragility complicates suturing in severe chemical burn cases, particularly given limited research on Cl2-induced skin damage. Modified surgical approaches, such as tissue adhesives, specialized suturing techniques, and tissue engineering methods, may improve outcomes in severe cases.
This case report has inherent limitations, including a single-patient design, absent exposure dosimetry data, and potential confounding environmental factors. Future research priorities should include establishing population-based chemical weapon survivor registries, developing chronic exposure biomarkers, and investigating targeted therapies for treatment-resistant chemical dermatitis. Standardized diagnostic criteria for chronic chemical weapon injuries would facilitate case recognition and management. Antioxidant and antifibrotic therapies represent promising therapeutic avenues for Cl2-induced chronic skin disease.
Conclusion
This case demonstrates clinical significance through three key contributions to the field of chemical weapon medicine. First, this case provides the first documented histopathological evidence of Cl2-induced chronic dermatitis, a previously unreported long-term complication. Second, this case illustrates critical diagnostic challenges when differentiating chemical-induced chronic dermatitis from endemic diseases in conflict regions. Third, this case supports the implementation of long-term dermatological surveillance protocols for chemical weapon survivors. Persistent alopecia and scarring indicate irreversible follicular damage, necessitating specialized monitoring. This case demonstrates chronic dermatological sequelae of Cl2 gas exposure, expanding recognized toxicity patterns beyond acute respiratory effects. Systematic documentation of long-term cutaneous manifestations following Cl2 gas exposure will inform clinical guidelines and enhance therapeutic interventions for affected populations.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605251378697 - Supplemental material for Do Syrian conflict survivors show novel chronic cutaneous sequelae from chlorine gas exposure: A case report and literature review
Supplemental material, sj-pdf-1-imr-10.1177_03000605251378697 for Do Syrian conflict survivors show novel chronic cutaneous sequelae from chlorine gas exposure: A case report and literature review by Ayham Qatza, Nabeha Haytham Alibrahim, Mariam Shaaban, Omar Alsabbagh and Alae Aldin Almasri in Journal of International Medical Research
Footnotes
Acknowledgments
None.
Authors’ contributions
Ayham Qatza collected the data. Ayham Qatza, Nabeha Haytham Alibrahim, Mariam Shaaban, and Omar Alsabbagh drafted the manuscript and prepared the figures. Ayham Qatza and Nabeha Haytham Alibrahim revised the final manuscript. Alae Aldin Almasri supervised the study. Ayham Qatza submitted the final manuscript. All authors read and approved the final version of the manuscript.
Availability of data and materials
The data and materials used in this study are available upon request from the corresponding author.
Declaration of conflicting interests
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Ethics
This work has been reported in line with the Case Report (CARE) criteria. 52 Our institution does not require ethical approval for reporting individual cases or case series.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Informed consent
Written informed consent was obtained from the patient for publication of this case report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
