Abstract
Tinea faciei caused by zoophilic dermatophytes can simulate several facial inflammatory skin conditions, such as eczema, lupus erythematosus, and cellulitis, often leading to misdiagnosis or a delayed diagnosis. A young girl around primary school age developed inflammatory, favus-like lesions on the face after the purchase of a pet rabbit. The patient had been evaluated at a local clinic where she received treatment with dexamethasone acetate cream topically twice daily for suspected eczema. Mycological examination confirmed that both the patient and her rabbit were affected by tinea corporis, which was caused by Trichophyton mentagrophytes. This case underscores the importance of considering tinea faciei in children presenting with inflammatory facial rashes, especially when there is a history of contact with pets. Moreover, it is crucial to implement protective measures to prevent children from contracting zoonotic dermatophytosis through contact with domestic animals.
Introduction
Tinea faciei (TF) is a dermatophyte infection affecting the non-hairy skin of the face, accounting for approximately 3%–4% of tinea corporis cases. 1 It occurs across all age groups, with higher prevalence in children aged 2–14 years and adults aged 20–40 years. 2 The face is also a common site for tinea incognito (TI), a condition often exacerbated by corticosteroid misuse, which alters the clinical presentation of the infection.3,4 This report describes a case of TF caused by Trichophyton mentagrophytes, originating from a pet rabbit, which was initially misdiagnosed as eczema.
Case presentation
The reporting of this study conforms to the CARE guidelines. 5 Written consent for treatment and publication were obtained from the patient’s parents.
In April 2024, a female pediatric patient within the 6–8-year age range was brought to Department of Dermatology of Hangzhou Third People’s Hospital (West Lake Rd 38, Hangzhou, China) by her parents with complaints of a three-month history of progressively worsening, intensely pruritic facial erythema. The rash appeared shortly after her family acquired a pet rabbit. The patient had been evaluated at a local clinic where she received treatment with dexamethasone acetate cream applied topically twice daily for suspected eczema, but her condition failed to improve. Instead, the lesions expanded, developing papules, pustules, and crusts. Physical examination revealed severe erythematous plaques with yellow crusting on the face (Figure 1(a)). The rabbit exhibited similar symptoms, including erythematous papules, hair loss, and scaling on its ears and tail (Figure 1(b) and (c)). Following the patient’s presentation at our center, given her clear history of exposure to animals and the typical features of her lesions (well-defined margins, crusting, and scale), we performed a mycological evaluation to further confirm the possibility of fungal infection. Fluorescence staining of samples from both the child and the rabbit revealed septate hyphae (Figure 1(d)). Fungal cultures grown on Sabouraud dextrose agar at 25°C for 10 days yielded yellowish, powdery colonies (Figure 1(e)). Microscopic analysis identified spherical to pyriform microconidia (2–4 μm) and cigar-shaped macroconidia (20–50 μm) (Figure 1(f)). PCR amplification and sequencing of the rDNA internal transcribed spacer region (ITS) were performed with primers ITS1 and ITS4-R. Finally, ITS sequencing confirmed the isolates as T. mentagrophytes (GenBank accession: PP587399).
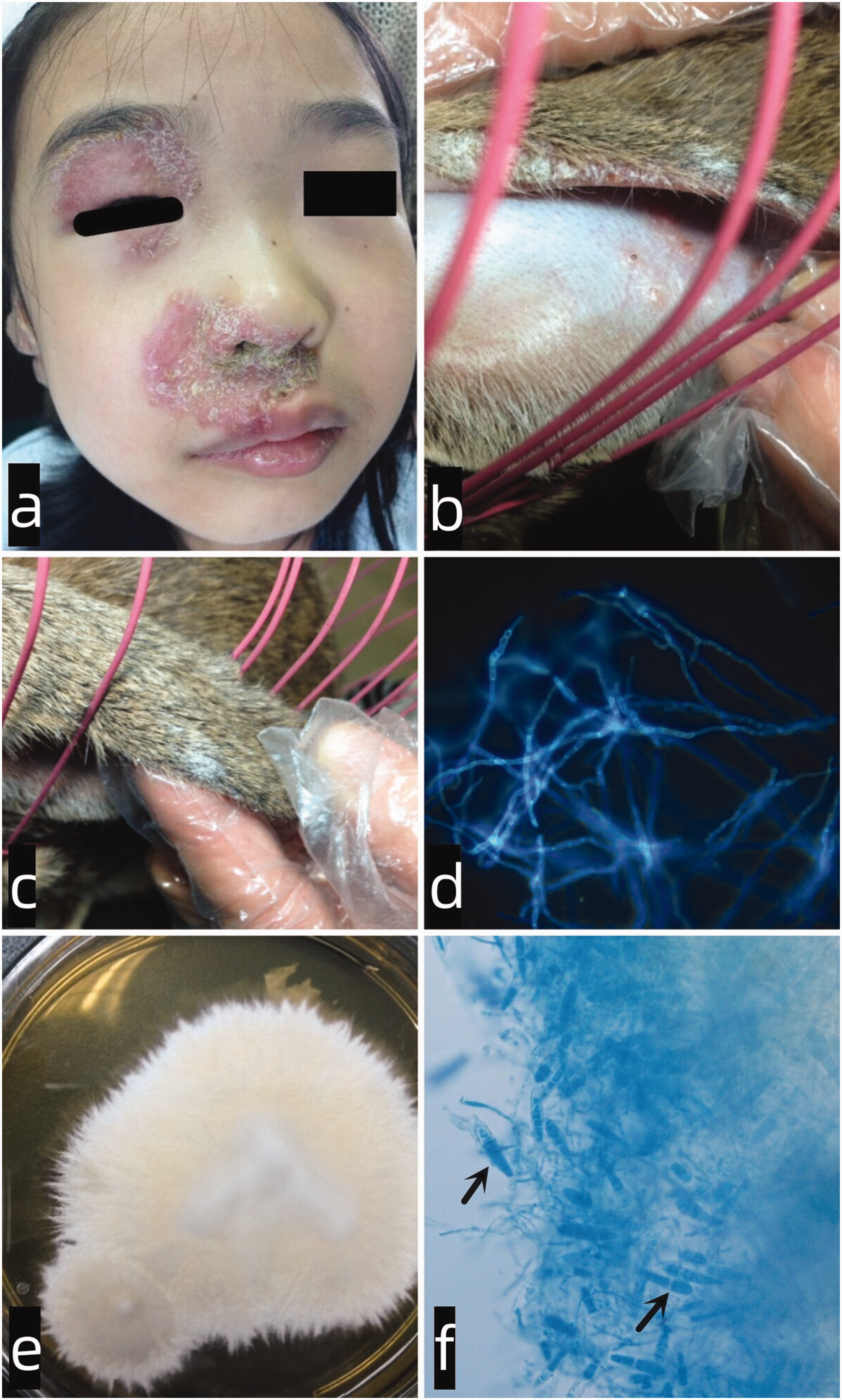
Clinical appearance of the child’s face (a). Clinical appearance of the rabbit’s ears (b) and tail (c). Fluorescence staining (40×) showing septate hyphae in the child’s sample (d). Colonies of T. mentagrophytes identified in the culture of a skin-scraping sample collected from the rabbit (e). Microscopic image of the isolated dermatophyte (f) (lactophenol cotton blue stain, 400×; cigar-shaped macroconidia (black arrow)).
The patient was diagnosed with TF caused by T. mentagrophytes and treated with oral terbinafine (125 mg daily) for one month, resulting in complete resolution. No recurrence was reported during a three-month follow-up.
Discussion
T. mentagrophytes is the second most common cause of dermatophytosis, following T. rubrum.6,7 It includes five species (T. mentagrophytes, T. interdigitale, T. erinacei, T. quinckeanum, and T. benhamie). Nine genotypes of T. mentagrophytes and T. interdigitale are morphologically similar but distinguishable through molecular analysis of the ITS1-5.8S-ITS2 region. 8 T. mentagrophytes is zoophilic, producing powdery colonies, while T. interdigitale is anthropophilic, characterized by aerial mycelium and abundant conidia. 9
Zoophilic dermatophytes, such as T. mentagrophytes and Microsporum canis, pose significant zoonotic risks, particularly in settings where humans and animals coexist. Infections often trigger strong inflammatory responses in humans. T. mentagrophytes is a leading cause of dermatophytosis in rabbits, commonly found in laboratories, veterinary clinics, pet stores, and farms.10–15 Zoonoses have emerged as a critical public health concern. This highlights the importance of the One Health concept, which emphasizes the interconnected health of humans, animals, and the environment. Supported by organizations such as the World Health Organization and the United Nations Children’s Fund, One Health aims to address zoonotic diseases and promote interdisciplinary collaboration. 16 Within family and pediatric care settings, stringent isolation protocols and comprehensive hygienic precautions must be implemented to mitigate the risk of zoophilic dermatophyte transmission and subsequent dermatophytosis development in children.
TI is a dermatophyte infection that loses its typical clinical features due to inappropriate steroid or calcineurin inhibitor use. Facial TI can mimic conditions such as eczema, lupus erythematosus, and cellulitis, often leading to diagnostic delays. 17 Favus, a dermatophytosis characterized by yellow scutula around hair follicles, is typically caused by T. schoenleinii and is more common in children.18,19 Favus-like TF is rare, emphasizing the need to consider TF in children with inflammatory or crusted facial eruptions. For unusual tinea corporis and TF, mycological screening is strongly recommended to exclude the risk of its exacerbation. 20
Conclusions
This case highlights TF caused by T. mentagrophytes in a child with a history of rabbit exposure, initially misdiagnosed as eczema. Clinicians should consider TF in children with inflammatory facial rashes, particularly those with pet contact. Mycological examination is essential for accurate diagnosis and appropriate treatment. It is crucial to implement protective measures to prevent children from contracting zoonotic dermatophytosis through contact with domestic animals.
Footnotes
Acknowledgements
The authors wish to thank the patient’s parents for their willingness to share their experience by providing informed consent for this case report.
Author contributions
Drafting of the manuscript: B.S and XK. X. Revision of the manuscript: XJ. X. Collection and/or analysis of the data: B.S, XK. X, and XJ. X. All authors read and approved the final manuscript.
Data availability statement
All data included in this study are available upon request from the corresponding author.
Declaration of conflicting interest
The authors declare that there is no conflict of interests.
Ethics statement
The study was approved by the Medical Ethics Committee at the Hangzhou Third People's Hospital (No. 2025KA151). The study was performed according to the Good Clinical Practice guidelines and the latest Declaration of Helsinki. The patient’s clinical data are kept in accordance with the EU General Data Protection Regulations, or other counterparts, on the processing of personal data and the protection of privacy (2016/679/EU). Written informed consent was obtained from the patient’s parents for publication of this case report and accompanying images.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
