Abstract
Objective
Congenital megaprepuce (CMP) is a rare penile deformity that usually requires surgical correction. This study was performed to examine the efficacy of the modified Sugita procedure for repairing CMP in pediatric patients.
Methods
We retrospectively analyzed the clinical data of pediatric patients with CMP treated by a surgeon using the modified Sugita procedure in our hospital from January 2019 to April 2021.
Results
Twenty patients were enrolled, and their median age at surgery was 70.5 months (range, 60–96 months). All surgeries were successful, and no complications occurred during the operation. The postoperative foreskin had moderate edema in five patients, and soaking in 10% hypertonic saline resulted in disappearance of the edema within 4 to 8 weeks. The follow-up duration was 6 to 20 months (median, 10 months). No other complications occurred, such as dehiscence or hematoma.
Conclusions
The modified Sugita procedure for correction of CMP produces excellent cosmesis and a low complication rate. Our study indicates that the modified Sugita procedure is a safe and feasible treatment option.
Introduction
Congenital megaprepuce (CMP) is a rare genital deformity characterized by excessive redundancy of the inner preputial layer, phimosis, and deficient penile skin. Whether it is a unique subcategory of buried penis or a distinct condition separate from buried penis remains controversial.1–3 The malformation typically presents with urination difficulty and a poor urinary stream because of a confined preputial ring with inner preputial ballooning secondary to the hydrostatic pressure of accumulated urine, and hand-operated expression of stagnant urine is usually required. Therefore, surgical correction is necessary for children diagnosed with CMP.2,4,5
Several methods and techniques for the repair of CMP have been reported, and they have produced different levels of positive outcomes.5–7 However, severe complications requiring reoperation have also been described, including scrotal hematoma, wound dehiscence, urethral meatal stricture, and an unsatisfactory appearance, indicating that the achievement of an optimum result remains challenging.1,2,8–11 In a study of 52 cases, only 44% obtained very good postoperative outcomes and 48% obtained acceptable outcomes; the remaining 8% had disappointing results that required surgical revision of redundant inner foreskin and persistent secondary concealment. 1
In 2009, Sugita et al. 12 reported a new surgical procedure for repairing a concealed penis, and good cosmetic results were achieved. In the present study, we review and summarize our initial experience performing the modified Sugita procedure for treatment of CMP in children.
Materials and methods
This retrospective study was conducted by reviewing the clinical records of all children diagnosed with CMP. Children who had CMP with other concomitant genital deformities were excluded. The study group comprised patients who underwent penile correction with the modified Sugita approach by a surgeon from January 2019 to April 2021 at our center. Written and verbal consent for treatment was obtained from the patients’ parents or guardians, and verbal consent was obtained for publication of the report. The study was approved by the Medical Ethics Committee of Wuhan Children’s Hospital (approval no. 2019R020-F01). All procedures performed in studies involving human participants followed the ethical standards of the Medical Ethics Committee of Wuhan Children’s Hospital and the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
This was a retrospective clinical analysis, and all relevant information has been de-identified to ensure the protection of patient privacy. The reporting of this study conforms to the CARE guidelines. 13
All patients presented urination difficulty and preputial ballooning. Aside from CMP, their physical examinations were normal, and they had no associated deformities such as chordee or hypospadias. All patients received intravenous prophylactic antibiotics 30 minutes before the operation. We included data on intraoperative or postoperative complications, urination, and cosmesis. The cosmetic outcome was assessed both by the surgeon and by the parents or older children.
Surgical procedure
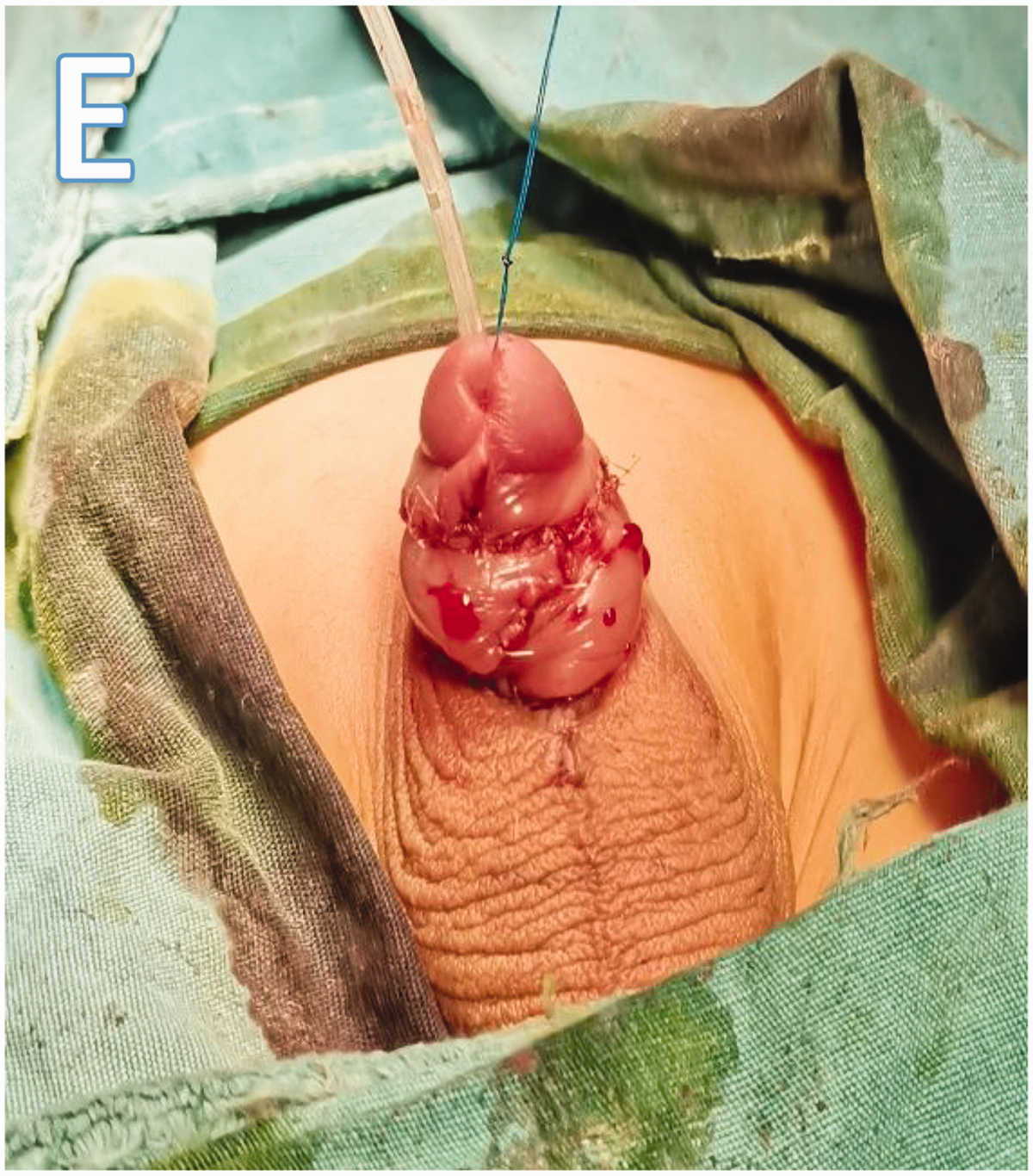
The key steps were performed as reported in the literature. 12 Briefly, a ventral longitudinal penile incision was made at the 6-o’clock position along a marked line down to the scrotum. The narrow ring of the prepuce was incised and the penile glans was exposed, creating a diamond-shaped skin defect. A 4-0 polypropylene suture was placed through the dorsal midline of the penile glans for traction. An 8-French Foley balloon urethral catheter was advanced into the bladder and retained for 3 to 5 days to allow continuous drainage (Figures 1–3). A circumferential incision was then made in the penile prepuce between two edges of the diamond-shaped skin defect, and a midline vertical incision was made in the dorsal inner prepuce to create two skin flaps that were sutured to the outer foreskin of the proximal glans without tension. The penile foreskin was degloved to the base of the penile shaft in the external surface of Buck’s fascia (Figure 4). Buck’s fascia at the penile root was anchored to the corresponding subcutaneous tissue with 4-0 absorbable sutures to reconstruct the penoscrotal angle at the 3- and 9-o’clock positions. The dorsal foreskin flaps were tailored and then transferred to cover the ventral skin defect, and the penile wound was closed with interrupted 5-0 absorbable sutures (Figure 5). The epidermal layer of the transferred flap was dissected to prevent swelling of the foreskin (Figure 6). Finally, the penile wound was dressed with Vaseline gauze and an elastic bandage.

Circumferential penile prepuce incision and manual anastomosis of the dorsal inner prepuce and outer foreskin of proximal glans without tension.
Tailoring of the dorsal foreskin flap with transfer to and coverage of the ventral skin defect.

Dissection of the epidermal layer of the transferred flap for reduction of anastomotic tension.

Typical appearance of congenital megaprepuce.
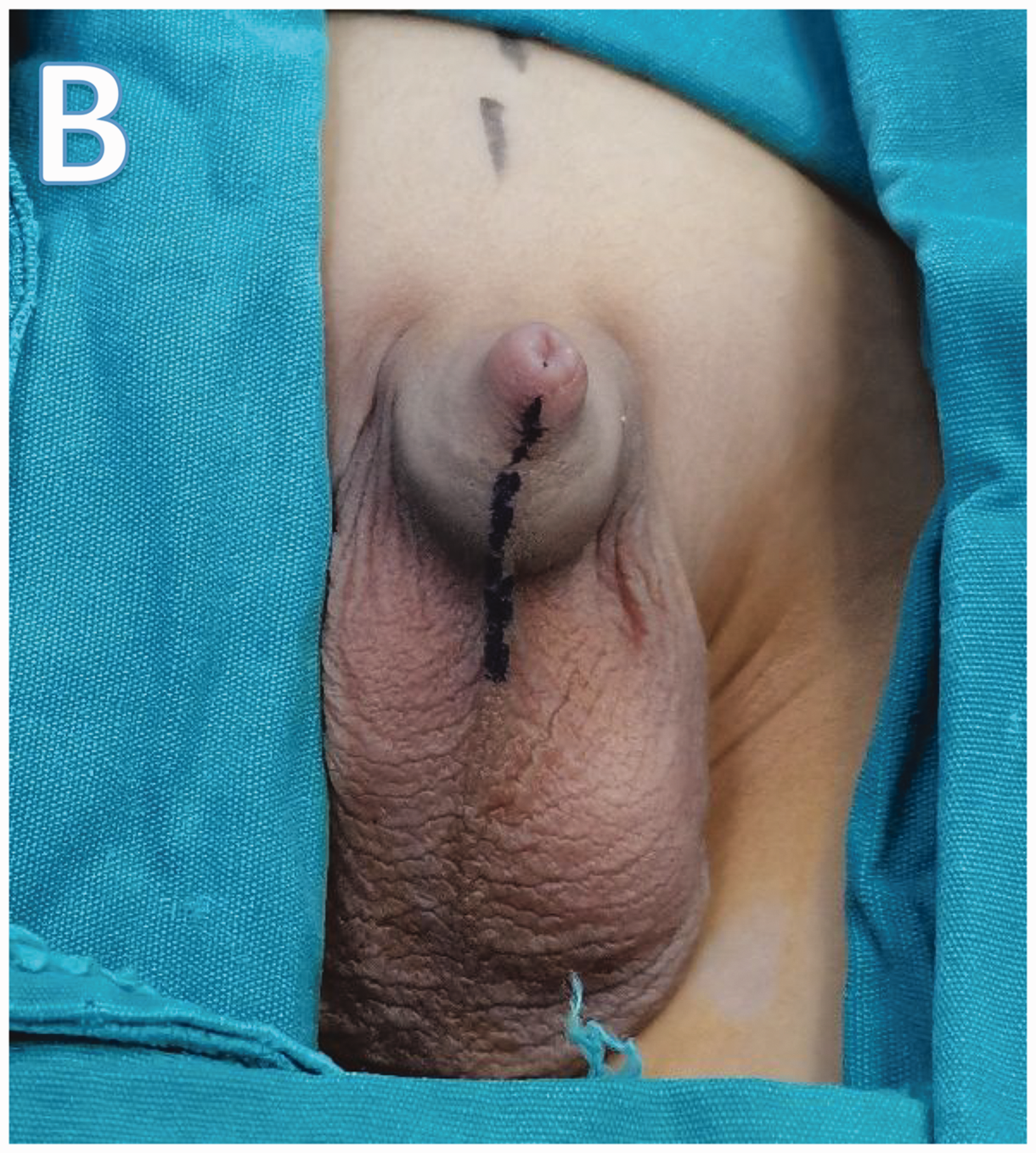
Line marking the site of the ventral longitudinal incision along the penis, extending down to the scrotum.

Traction of the penile glans; catheterization and marked line for penile longitudinal dorsal incision.
Results
Twenty patients were enrolled in the study, ranging in age from 60 to 96 months (mean, 75 months; median, 70.5 months). The operations were successful in all patients. The wound dressing and urethral catheter were removed from days 3 to 5 postoperatively. The preputial inner plate flap transferred to the penile ventral side healed well.
Five patients developed short-term complications in the form of moderate preputial edema, which was treated by soaking in 10% hypertonic saline and disappeared within 4 to 8 weeks. During 6 to 20 months of follow-up, no other complications such as wound dehiscence or urethral stricture occurred. The patients and their parents were satisfied with the penile appearance, and urination was unobstructed.
Discussion
CMP was first described in 1994, and its etiology is still unclear. A recent study showed that the etiology of CMP may be multifactorial, involving a genetic origin, deficient penile shaft skin, and severe phimosis.2,14 In addition, in cases of partial CMP accompanied by hypospadias or penile ventral curvature, the abnormities may be coincident or part of CMP; thus, further investigation of this condition is required.15,16 The preputial ring is narrow in patients with CMP, excessive hydrostatic pressure of urine accumulates during urination and leads to expansion of the inner prepuce, and the prepuce is not retractable. Therefore, a basal hemispheric ballooning appearance occurs during urination, leading to urination difficulty and the need for surgical treatment.1,2 Surgical repair often does not achieve the desired outcomes, and the proportion of complications requiring reoperation, such as wound dehiscence and an unsatisfactory appearance, remains high.1,8 Reducing the risk of surgery-related complications and achieving an ideal appearance are urgently needed.
In 2009, Sugita et al. 12 reported a new procedure for the repair of a concealed penis in 57 patients. The postoperative recovery of all patients was uneventful with the exception of two patients who developed persistent lymphedema caused by suture constriction that required reoperation during follow-up. Our institution first reported the modified Sugita procedure to repair pediatric CMP, and all patients or their parents were satisfied with the operative results. All patients in our study were school-age children (average age of 6.3 years), which is consistent with a study by Murakami et al. 17 (mean age at surgery of 5.9 years). Some researchers have reported their experience with this procedure in patients with a median age of approximately 6 months at the time of the operation.4,10,16 Currently, there is no consensus on the appropriate age for surgery, and research on whether age affects the outcome of a later operation is lacking. One point of consensus is that early surgical correction is recommended at diagnosis,2,5,7,16 and we strongly share this viewpoint.
All the operations in the present study were successful and acquired excellent results with the exception of moderate edema in five patients. However, the edema was successfully managed with nonsurgical measures, similar to the outcomes reported by Buluggiu et al. 5 Whether Buck’s fascia should be anchored to the penile skin shaft remains controversial. Murakami et al. 17 did not fix Buck’s fascia and found no evidence of penile retraction. Buluggiu et al. 5 reported their successful experience with the management of five cases of CMP, suggesting that there is no need for fixation of Buck’s fascia to the penile body to gain efficient, functional, and esthetic results without abnormal deep tissue attachments. In a report of a 12-year experience shared by Rod et al., 1 in which the authors restored the penopubic and penoscrotal angles by fixation of the penile skin with Buck’s fascia at the penile base, 16 patients presented with moderate penile retraction at the postoperative clinical follow-up. In the present study, however, we found no indications of penile retraction during the follow-up period, consistent with the findings reported by Alexander et al. 18 and Lin et al. 6
In 2018, Podestá and Podestá 8 described their 10-year experience treating CMP in 15 patients using the outer preputial layer to cover the ventral skin defects. During the mean follow-up period of 4.6 years, short-term complications appeared in three patients: scrotal hematoma in one and penoscrotal skin dehiscence in two.
During our clinical follow-up period, no adverse events such as penile retraction, redundant foreskin, hematoma, or wound dehiscence were observed. Our experience revealed three important aspects of this procedure. First, bilateral fixation of Buck’s fascia to the subcutaneous tissue at the base of the penile shaft reduces the occurrence of penile retraction, and fine tailoring avoids an abundant residual inner prepuce, thus maintaining an excellent penile appearance. Second, measures are adopted to ease wound tension on the penile ventral flap, alleviate the swelling of the prepuce, and prevent wound dehiscence. Third, the modified Sugita procedure weakens the effects of the transferred flap on the blood supply because of the shorter blood distribution distance and broad base. Thus, necrosis and infection of the transferred flap rarely occur.
Our study has two apparent limitations. First, the included patients were not representative enough to make definitive conclusions about the surgical results. Second, a standardized, validated questionnaire completed by both the surgeon and the patients (or their parents) would allow for a more impersonal evaluation of the procedure.
Conclusions
Our preliminary experience suggests that the modified Sugita procedure is safe and effective in treating CMP. The technique provides a satisfactorily cosmetic penile appearance with an initial low complication rate.
Footnotes
Acknowledgements
We would like to thank all the participants who took part in this study.
Author contributions
JY collected and analyzed the data, drafted the initial manuscript, and reviewed and revised the manuscript. HTC performed the data analysis and reviewed and revised the manuscript. SL performed the data analysis. All authors approved the final manuscript as submitted.
Availability of data and materials
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
Declaration of conflicting interests
The authors declare that they have no competing interests.
Funding
This work was supported by funding from the Clinical Medical Research Project of Wuhan Children’s Hospital (grant number 2019FE003).
