Abstract
Objective
This study was performed to investigate the dynamics of intracranial pressure (ICP) alterations and bilateral transverse–sigmoid sinus morphologies in patients with venous pulsatile tinnitus (PT).
Methods
This retrospective study involved 27 patients with venous PT associated with sigmoid sinus wall anomalies. ICP and ICP metrics were measured by cerebrospinal fluid manometry and internal jugular vein compression tests. Correlation analysis was performed to determine the statistical correlation between ICP and the morphological metrics.
Results
The mean ICP was 212.5 ± 47.3 mmH2O. The median
Conclusions
Complete obstruction of flow patency should be avoided in patients with low ICP and large volumetric/patency differences in the bilateral transverse–sigmoid sinus systems.
Keywords
Introduction
Aberrant perception of vascular flow noises that are synchronized with cardiac rhythm is known as pulsatile tinnitus (PT) or pulse-synchronous tinnitus. 1 This type of tinnitus is categorized as objective tinnitus, in which an external examiner or acoustic sensor can determine or sense the acoustic origin of the PT.1,2 The most typical vascular source of PT is venous.3,4 Simple ipsilateral internal jugular vein (IJV) compression can halt venous PT by obstructing the flow of the ipsilateral venous return. 5 Because of the high rate of PT recurrence and its propensity to cause a detrimental increase in intracranial pressure (ICP), early IJV ligation is important to reduce PT perception. 6
Approximately 43% to 86% of patients with venous PT have sigmoid sinus wall abnormalities (SSWAs), sigmoid sinus wall dehiscence, or a sigmoid sinus wall diverticulum.3,7 These are treatable anatomical anomalies that are relevant to the production of PT. Although clinical investigations have shown a high prevalence of transverse sinus (TS) stenosis as well as overlapping indicators linked to idiopathic intracranial hypertension (IIH) among people with venous PT, the exact origin of SSWAs is uncertain.7–9 TS stenosis has recently been considered the most sensitive hallmark of increased ICP, 10 although the cause–effect relationship between venous pathology and high ICP or vice versa remains contentious.11,12 However, the etiology of PT is more likely to be the presence of sigmoid plate dehiscence rather than TS stenosis or IIH. 8
Neurotologists tend to perform transmastoid sinus wall resurfacing surgery, which has been shown to be therapeutically beneficial in patients with PT.2,13,14 This operation consists of two separate curative procedures: (a) sinus wall resurfacing/reconstruction to reinforce the structural integrity of the sigmoid plate and thus insulate hydroacoustic and vibroacoustic noises and (b) extraluminal compression to reshape the protruding transverse–sigmoid sinus junction or diverticulum and thus eradicate flow anomalies.2,14,15 The latter procedure should be carried out with caution, however, because symptoms of elevated ICP appear only after total occlusion of the venous sinus lumen. 15
According to the Monro–Kellie doctrine, the combined volume of the brain, cerebrospinal fluid (CSF), and intracranial arterial/venous compartments is kept constant. 16 Iatrogenically increased ICP is caused by severe blockage of the transverse–sigmoid sinus on the ipsilateral side and poor collateral sinus flow on the contralateral side, leading to a restriction in the volume of outflow from the venous compartment.16,17 Operating on the venous sinus wall can be risky when surgeons disregard or are unaware of the pattern of the bilateral transverse–sigmoid sinuses, which are important conduits for the cerebral venous return of the posterior fossa. 15 Nonetheless, a standard approach for transtemporal sinus wall reconstruction surgery involves minimizing the diverticulum or significant transverse–sigmoid sinus junction, which necessarily reduces the volume of venous return.
This study was performed to quantitatively illustrate the relationship between the shape of the bilateral transverse–sigmoid sinuses and the dynamics of ICP alterations in patients with venous PT. Although extraluminal compression is believed to yield more effective therapeutic outcomes by reducing the kinetic energy of the regional flow and eliminating PT, 2 neurotologists can predict and prevent an increase in ICP after volumetric reduction in the venous compartment for patients with venous PT. This can be achieved by understanding the changes in ICP homeostasis and their correlation with the morphologies of the bilateral transverse–sigmoid sinuses.
Materials and Methods
Patient data
Through radiologic examinations, including temporal bone computed tomography and contrast-enhanced magnetic resonance (MR) angiography/venography, the patients in this study were assessed for venous PT while undergoing ipsilateral IJV compression, with a significant reduction or elimination of PT and the presence of SSWAs. Patients who exhibited PT that displayed no correlation with a venous origin, such as PT originating from an arterial origin, arteriovenous malformations, a temporal bone tumor, anemia, or hyperthyroidism, were excluded. Furthermore, patients who had incomplete data regarding their IJV compression test result or who underwent several lumbar punctures were also excluded from the study (Figure 1). Ultimately, 27 patients who had venous PT associated with SSWAs and were treated at our facility from July 2020 to July 2022 were retrospectively enrolled in the study. The reporting of this study conforms to the SRQR guidelines. 18
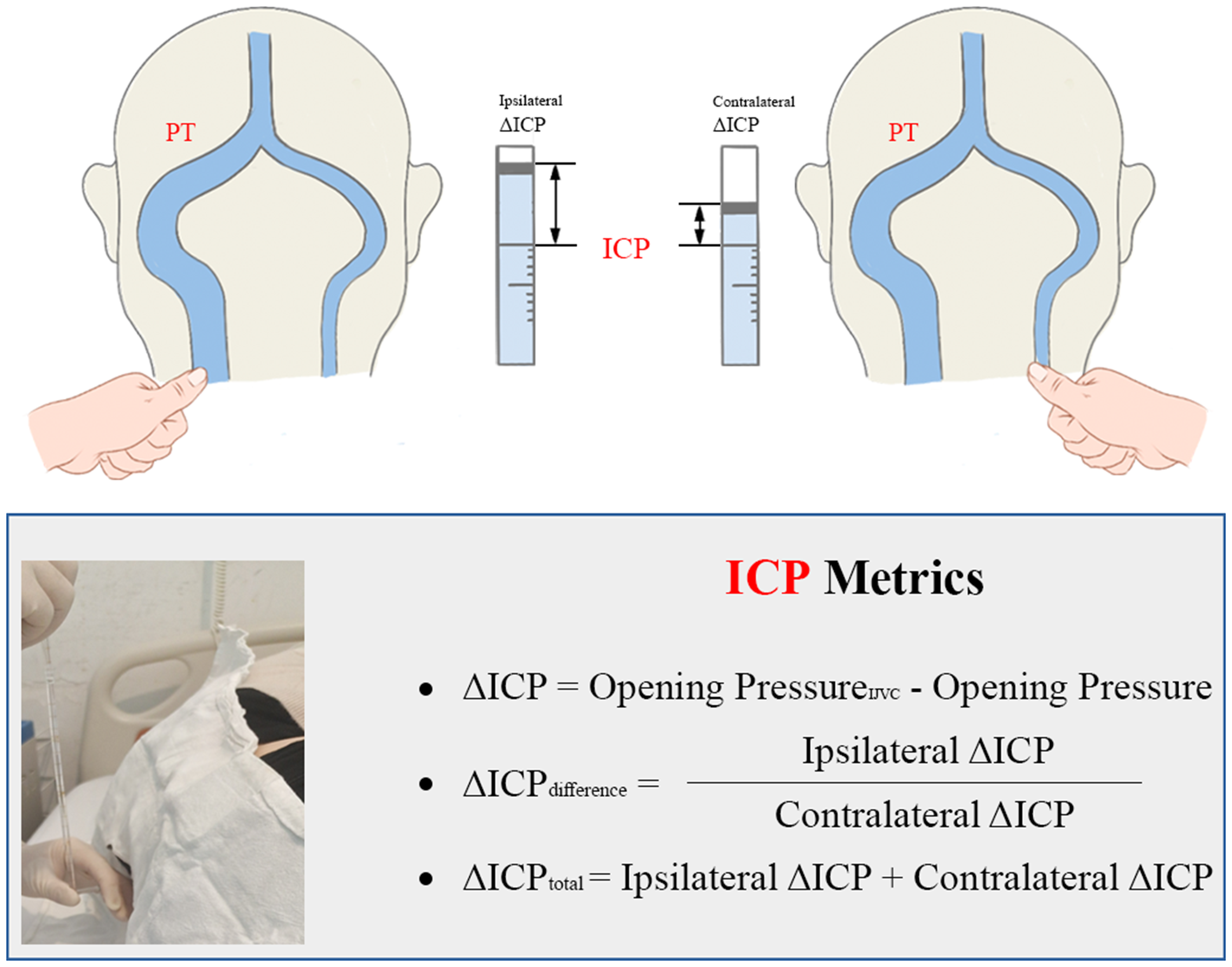
Schematic diagrams of the study design showing cerebrospinal fluid manometry, internal jugular vein compression test, and intracranial pressure metrics.
SSWAs are anatomical anomalies associated with venous PT and are identified based on radiologic examinations. In this study, sigmoid sinus dehiscence was defined as a defect in the bony plate overlying the sigmoid sinus vascular wall. A diverticulum was defined as protrusion of the sigmoid sinus wall into the mastoid air cells or cortex with a characteristic outpouching vascular silhouette. The laterality of the dominant transverse–sigmoid sinus was determined by a larger sinus diameter compared with the contralateral side. TS hypoplasia was diagnosed when the TS lumen was discontinuous and/or >40% smaller in diameter than on the contralateral side. 19
The present study involving human participants was reviewed and approved by the ethics committee of the Eye, Ear, Nose and Throat Hospital of Fudan University in Shanghai, China (No. 2022116). All patients provided written informed consent to participate in this study. All patient details have been deidentified.
Measurement of TS stenosis and bilateral transverse–sigmoid sinus morphologies
The bilateral sinus morphologic parameters measured in the 27 patients were the degree of TS stenosis, distance from the torcular herophili to the TS stenosis, and volume and length of the transverse–sigmoid sinus. TS stenosis was measured with Mimics software version 19.0 (Materialise, Leuven, Belgium) or the NUMARIS/4 workstation (SYNGO MR B17; Siemens AG, Munich, Germany) using patient-specific contrast-enhanced two-dimensional time-of-flight MR slices (MR parameters are described in the reports by Guo and Wang 15 and Guo et al. 16 ). After the TS measurements, volumetric and length measurements were recorded using 3-matic 11.0 (Materialise) based on three-dimensional computational models reconstructed using MR venograms. The sequences and parameters of MR imaging are listed in Table 1.
Sequences and parameters of magnetic resonance imaging.

The TS segment was defined as the venous sinus extending from the intersection of the torcular herophili and TS (proximal end) to 1 cm prior to the transverse–sigmoid junction (distal end) (Figure 2). TS stenosis was identified when the largest and smallest cross-sectional areas were located. The degree of TS stenosis was normalized using the following formula (Eq. 1):

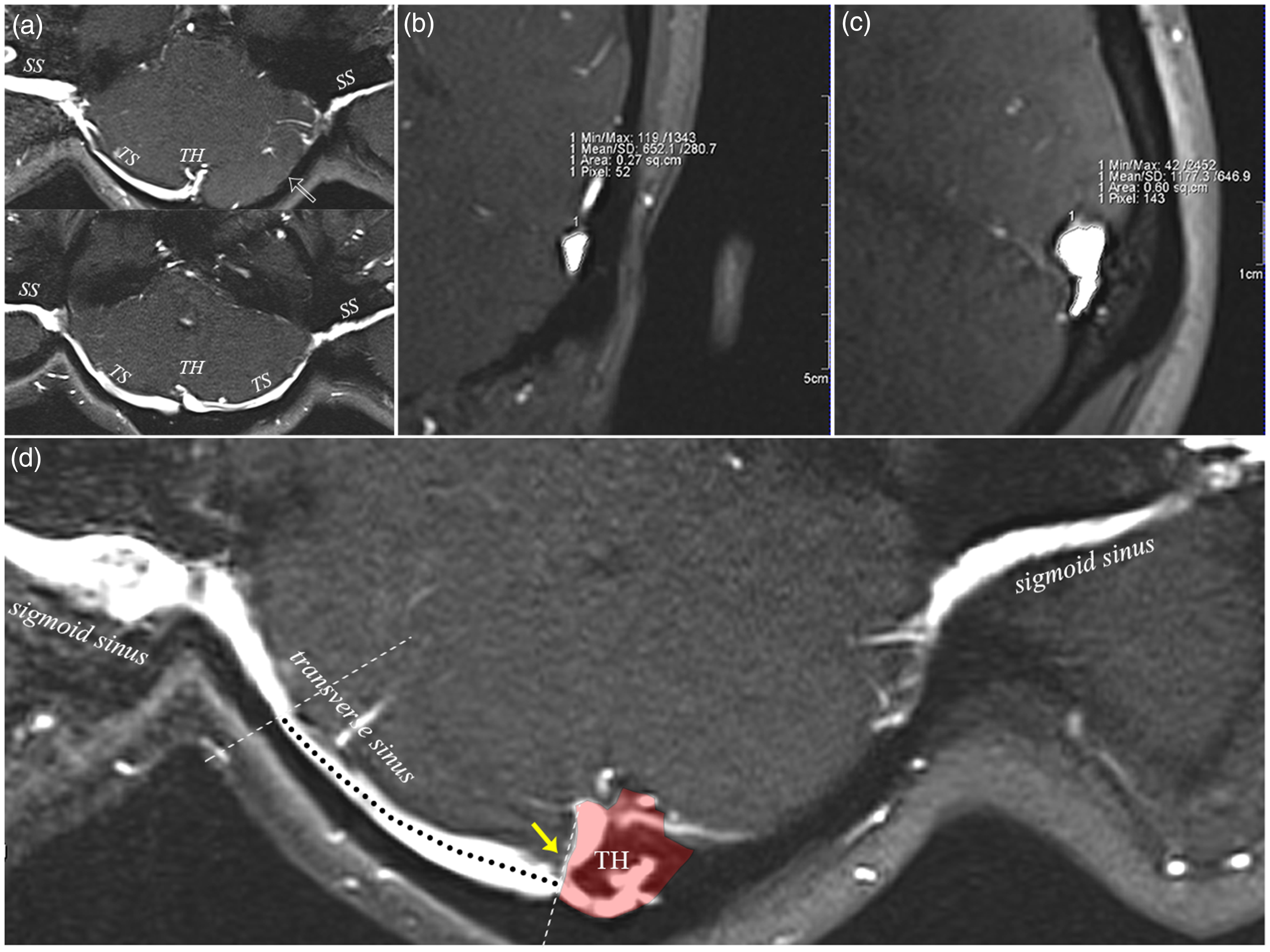
Morphological measurement of transverse–sigmoid sinus morphologies. (a) Curved reformats of bilateral transverse sinus. (Upper panel) Unilateral dominant transverse–sigmoid sinus. (Lower panel) Bilateral co-dominant transverse–sigmoid sinus. TH, torcular herophili; TS, transverse sinus; SS, sigmoid sinus. Arrow indicates transverse sinus hypoplasia. (b) Measurement of cross-sectional area of distal transverse sinus using coronal contrast-enhanced two-dimensional time-of-flight magnetic resonance slice. (c) Measurement of cross-sectional area of proximal transverse sinus using sagittal contrast-enhanced two-dimensional time-of-flight magnetic resonance slice and (d) Curved reformat of bilateral transverse–sigmoid sinus. The length from the proximal end to the transverse sinus stenosis was measured starting from the edge of the brain perpendicular to the sinus flow direction (yellow arrow) to the cut plane with the smallest cross-sectional area of the transverse sinus lumen. The torcular herophili was defined as the area within the bilateral edges of the brain (marked with translucent red fan-shaped area).
The index of TS stenosis (ITSS) was used to categorize the normalized degree of TS stenosis according to the criteria established by Da Silveira Carvalho et al.
20
(Eq. 2):

The segment of the transverse–sigmoid sinus was defined as the segment extending from the intersection of the torcular herophili and TS (proximal end) to the outlet of the sigmoid sinus (distal end) measured at the midportion of the mandibular ramus. The length from the proximal end of the TS to the stenosis was measured using curved reformatting from the edge of the torcular herophili (the inlet of the proximal TS) to the most stenotic TS cut plane, and the bilateral length and shortest length to the proximal end of the TS on either side were measured. Measurement from the proximal end of the TS to the stenosis on the side with TS hypoplasia/aplasia was not conducted.
The volume and length of the transverse–sigmoid sinus were measured on the anterior/top surface from the distal to proximal end of the three-dimensional vascular models tangential to the flow direction. In patients with a diverticulum, the length measurement bypassed the diverticulum and was maintained at the midline of the transverse–sigmoid junction. In patients with TS hypoplasia, the measurement ended at the proximal end of the sigmoid sinus or TS. Sinus branches and discontinued sinus segments were excluded from this study (Figure 3).

Demonstration of three-dimensional reconstruction of vascular models for length and volumetric measurements. (a) Maximum intensity projection (MIP) of a patient with bilateral co-dominant transverse–sigmoid sinus using axial magnetic resonance (MR) venography. (b) MIP of bilateral co-dominant transverse–sigmoid sinus of a patient using coronal MR venography and (c) MIP of ipsilateral dominant transverse–sigmoid sinus of a patient with a diverticulum using axial MR venography. Note that 1) the length measurement bypassed the diverticulum and was maintained at the antero-midline of the vascular model, and 2) the length measurement was initiated from the sigmoid sinus outlet to the proximal end of the sigmoid sinus. PT, pulsatile tinnitus.
CSF manometry and bilateral sinovenous patency test
The patients were requested to maintain the lateral decubitus position with their legs straightened throughout the entire CSF measurement process as described in our previous reports.21,22 After measuring the opening pressure, the IJV compression test was performed by digital compression on either side of the upper IJV lumen at the level of the mandibular angle to evaluate ipsilateral/contralateral sinus patency. The opening pressure and CSF pressure during the IJV compression test were recorded until the CSF level stabilized. The duration of the IJV compression on either side did not exceed 15 s. CSF specimens were collected for standard cytological and biochemical analyses after ICP measurements.
Morphological/ICP metrics and definitions
The change in ICP (
This equation highlights the magnitude of ICP change after complete obstruction of the ipsilateral/contralateral transverse–sigmoid sinus (
To determine the bilateral morphological influence on the parameters of interest, the bilateral sinus length (Eq. 4) and volume (Eq. 5) were converted into ratio differences:


Additionally, to avoid the absolute value of the intra-patient morphological difference that may skew the magnitude of 
Statistical analysis
Statistical analysis was performed using R (RStudio, Boston, MA, USA) and OriginPro version 9.1.0 (OriginLab Corporation, Northampton, MA, USA). Fisher’s exact test was used to analyze the descriptive statistics. The Shapiro–Wilk test was used to check the normality of continuous data. The two-sample t-test (normally distributed data) and nonparametric Mann–Whitney U test (non-normally distributed data) were used based on the results of data normality. Correlation analysis, including Pearson’s correlation coefficient (Pearson’s r value), was performed to examine the strength of the correlation among parameters of interest. The strength of the correlation was determined as very strong (0.5–1.0), moderate (0.3–0.5), or weak (<0.3) based on the Cohen criteria. 23 Univariate linear regression analysis was performed to examine the linearity of variables of interest.
Results
Clinical descriptive outcomes
Among the 27 patients (24 women, 3 men) with venous PT, the mean age was 33.1 ± 7.8 years. The mean ICP was 212.5 ± 47.3 mmH2O (range, 130–295 mmH2O), and six patients’ ICP was ≥250 mmH2O. The mean body mass index (BMI) was 23.7 ± 4.4 kg/m2, and the BMI was linearly correlated with the open pressure (
Dynamics of ICP variation
The mean ipsilateral and contralateral

Linear correlation between ICP metrics and volumetric difference of bilateral transverse–sigmoid sinus. (a) Linear correlation between ICP and total ICP variation and (b) Linear correlation between difference of bilateral ICP variation and difference of bilateral transverse–sigmoid sinus volume. ICP, intracranial pressure.
Linear correlation between ICP and variables of interest in the 27 patients.

ICP, intracranial pressure; BMI, body mass index; ITSS, index of transverse sinus stenosis; TS, transverse sinus; TS-SS, transverse–sigmoid sinus; SD, standard deviation.
Univariate linear regression was performed to check the correlation between ICP and variables of interest.
Linear correlation between ICP metrics and variables of interest in the 27 patients.

Results of the univariate linear correlation analysis are expressed as slope (B), p value, and r value.
Definitions of ICP metrics are presented in the Methods section.
ICP, intracranial pressure; ITSS, index of transverse sinus stenosis; Lendifference, bilateral length difference in transverse–sigmoid sinus; Voldifference, bilateral volumetric difference in transverse–sigmoid sinus; ΔICPtotal, sum of ipsilateral and contralateral ΔICP; ΔICPdifference, difference in bilateral ΔICP.
ICP metrics versus TS stenosis
The normalized degree of ipsilateral and contralateral TS stenosis was 68.0% ± 0.14% and 74.2% ± 7.2%, respectively, in 12 patients with contralateral TS hypoplasia. Patients with contralateral TS hypoplasia had a significantly higher open lumbar pressure than those without (two-sample t test, p = 0.036). However, there was no significant difference in ΔICP between patients with bilateral TS connected to the confluence of the sinuses and those with unilateral connection on either side (two-sample t test). The median ITSS score of the 27 patients was 9 (range, 8–12), and the ITSS score was significantly different between those with normal and elevated CSF pressure (Mann–Whitney U test, p = 0.019). The open lumbar pressure and
Bilateral sinus morphological and ICP metrics
Among the 27 patients, the median length and volume of the ipsilateral transverse–sigmoid sinus were 18.9 (range, 17.6–20.3) cm and 7.4 (range, 6.0–10.2) cm3, respectively, whereas those of the contralateral side were 16.4 (range, 11.9–19.2) cm and 2.5 (range, 1.5–4.1) cm3, respectively. The median length (
Discussion
This study is the first to establish a positive correlation between the difference in ICP (ΔICPdifference) and the ratio of the bilateral transverse–sigmoid sinus volume, length, and degree of transverse–sigmoid sinus stenosis (Voldifference, Lendifference, and ITSS) in patients with venous PT. The increased bilateral volume and sinus patency differences resulted in a corresponding increase in ICP, with a steeper rise in ICP if flow obstruction occurred on the significantly larger side of the transverse–sigmoid sinus with less contralateral drainage (larger Voldifference). Additionally, the magnitude of ICP variation showed a negative correlation with the opening pressure, and a significant difference in the ΔICPtotal was noted between the normal and elevated ICP groups. These results suggest that neurotologists must consider a more severe rise in ICP in patients with lower ICP if sinovenous flow patency is impeded. Our postulation is that venous compliance and intravenous pressure differ between patients with disparate ICP levels, which follows the principle of the Starling resistor-like mechanism. 24 The decreased ICP after removal of the CSF increases the venous compartment, and the volume of the venous compartment decreases when ICP rises as a secondary effect, leading to insufficient room for venous output. This suggests that increased central venous pressure (increased upstream pressure gradient) may play a critical role in limiting the magnitude of the ΔICPtotal, possibly serving as a protective mechanism. Another possibility is that patients with TSS and elevated ICP have already developed alternative and collateral outflow pathways, which limits the increase in ICP resulting from additional manual IJV compression.
A high degree of bilateral transverse–sigmoid stenosis may suggest an elevated ICP, which is a hallmark more sensitive than the presence of empty sellae and papilledema.10,19,25 However, most radiological findings of elevated ICP have high specificity but low sensitivity; flattening of the posterior sclera is, in isolation, the most specific finding. 26 Other MR imaging findings of elevated ICP include distention of the CSF sheath surrounding the optic nerve, nerve tortuosity, intraocular protrusion of the optic nerve head, and posterior flattening of the globe. 26 Our study showed that the coexistence of unilateral stenosis of the dominant TS sinus and contralateral TS hypoplasia is another radiological sign indicating elevated ICP, resulting in a large difference in volume between the bilateral sinuses (Voldifference). 10 In such cases, ICP may severely increase when the drainage of the dominant sinus, which is the only major conduit for intracranial venous drainage, is operatively impeded. 10 Additionally, we found that the difference in ICP and ΔICP was irrelevant to the ITSS and whether the lateral sinuses are connected to the torcular herophili. A higher degree of TS stenosis is suspected to impede the increase in ICP due to the enlarged trans-stenotic pressure gradient, which reduces the impact of downstream intravenous pressure on the ICP.27,28 Furthermore, the perivenous spaces may vary among patients, resulting in different maintenance of ICP.
Although a definitive gold standard for transverse–sigmoid stenting in patients with isolated PT and/or IIH is yet to be established, empirical evidence supports the effectiveness of TS stenting as a highly efficacious surgical intervention for simultaneous reduction of PT and improvement of sinus patency. 29 It is reasonable to consider TS stenting in patients who have venous PT and elevated ICP. Additionally, stenting may be optimal for patients with low ΔICPtotal or low ΔICP on the dominant side of sinus drainage and high Voldifference because these individuals may have reduced sinus functionality. While the occurrence of IIH-related symptoms is infrequent in patients with isolated venous PT, prioritizing the alleviation of these symptoms and enhancement of sinus patency can offer additional benefits alongside PT relief. 12 Regarding the reduction of PT, Guédon et al. 30 recently emphasized the significance of decreasing flow velocity, which may take precedence over the pressure gradient.
In this study, the absence of a correlation between unilateral ΔICP and morphological markers suggests that intra-patient variability plays a significant role in the variation of ICP. The changes in pressure following compression of the ipsilateral sinus wall can be unpredictable because of variations in the absolute length and volume of the bilateral sinus pathways across different patients. In such instances, the ratio of the bilateral sinus volume (Voldifference) can serve as a valuable reference marker for neuro-otologists who choose to employ the transtemporal compression technique, aiming to minimize operative risks while effectively addressing venous PT.
ICP has been suggested to vary in accordance with the hypothesis proposed by Davson et al., 31 which posits that ICP is influenced by factors such as total cerebral blood flow leaving the capillaries, venous resistance, and central venous pressure. 32 Whereas compression over the prominent transverse–sigmoid sinus junction or elimination of an outwardly protruding diverticulum may not necessarily reduce venous outflow volume and is advised to remain <70% according to computational studies, 33 complete obstruction of transverse–sigmoid sinus flow can lead to an iatrogenic increase in ICP, which can be reversed by retrieving the repairing materials. Some neurosurgeons have even considered sacrificing the unilateral sinus flow to ensure safety when the sinus pressure is <10 mmHg. 34 However, a recent systematic review of TS stenting suggested that the difference in the peak pressure gradient across TS stenosis ranges from 2 to 77 mmHg, and reducing the regional pressure gradient does not significantly lower the elevated opening pressure despite relieving symptoms. 35
Assessing and restoring bilateral sinus outflow patency requires various diagnostic approaches. Preoperative and postoperative comparison of the venous outflow volume using Doppler ultrasound at the upper IJV is crucial. Postoperative CT/MR venography provides insights into sinus wall compression and flow obstruction localization. Funduscopy and ocular ultrasonography aid in confirming and monitoring papilledema development. In rare cases where extraluminal compression leads to neurological symptoms such as headache, visual field defects, and abducens palsy, revision surgery becomes necessary to reverse the collapsed sinus wall by extracting operative fillers. 36 Figures 5 and 6 illustrate a case of augmented ICP resulting from extraluminal sinus compression and the associated radiologic details and papilledema development. Initially, persistent headache serves as an early indicator of increased ICP, typically appearing a few hours or days after surgery. Oral diuretics and/or intravenous mannitol injections are commonly prescribed for headache relief. However, if symptoms persist or mannitol injections only offer temporary relief, severe venous outflow obstruction may be present, necessitating revision surgery to restore venous return flow by retrieving the fillers.
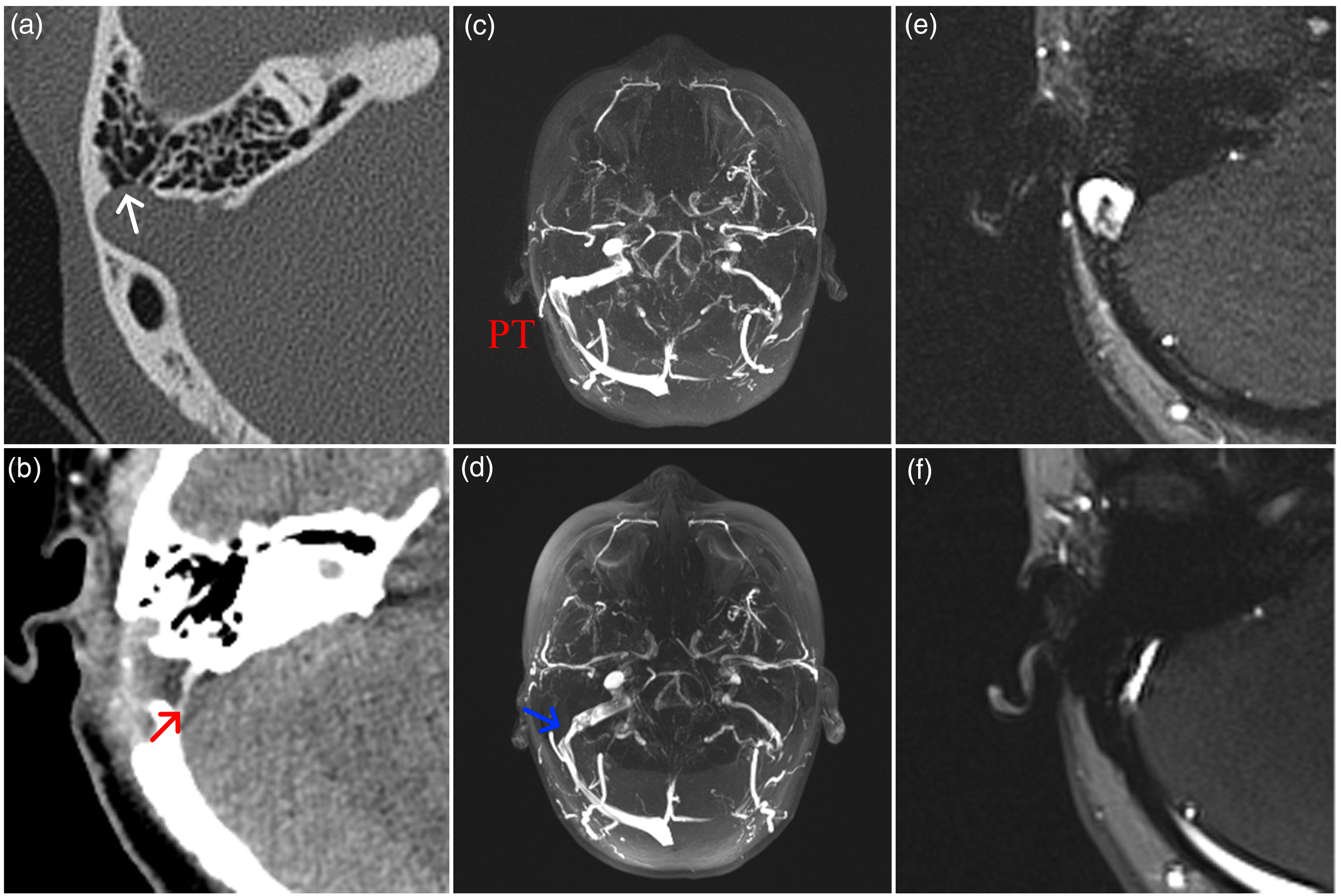
Radiologic details of a patient with right-sided pulsatile tinnitus (PT) who developed pulsating headache and bilateral papilledema after the PT was addressed by extraluminal compression surgery. (a) Preoperative computed tomography exhibiting the location of sigmoid sinus wall dehiscence (white arrow) and the laterally placed sigmoid sinus with prominent transverse–sigmoid sinus junction. (b) Postoperative contrast-enhanced computed tomography venogram showing the overly compressed right-sided transverse–sigmoid sinus junction. The red arrow indicates the narrowed blood flow at the compression site. (c) Preoperative maximum intensity projection of a case reconstructed using axial two-dimensional (2D) time-of-flight (TOF) magnetic resonance (MR) venography. (d) Postoperative maximum intensity projection of a case reconstructed using axial 2D TOF MR venography. (e) Preoperative 2D TOF MR venogram slice displaying the right-sided laterally placed sigmoid sinus with prominent transverse–sigmoid sinus junction and (f) Postoperative 2D TOF MR venogram slice displaying the overly compressed sigmoid sinus.
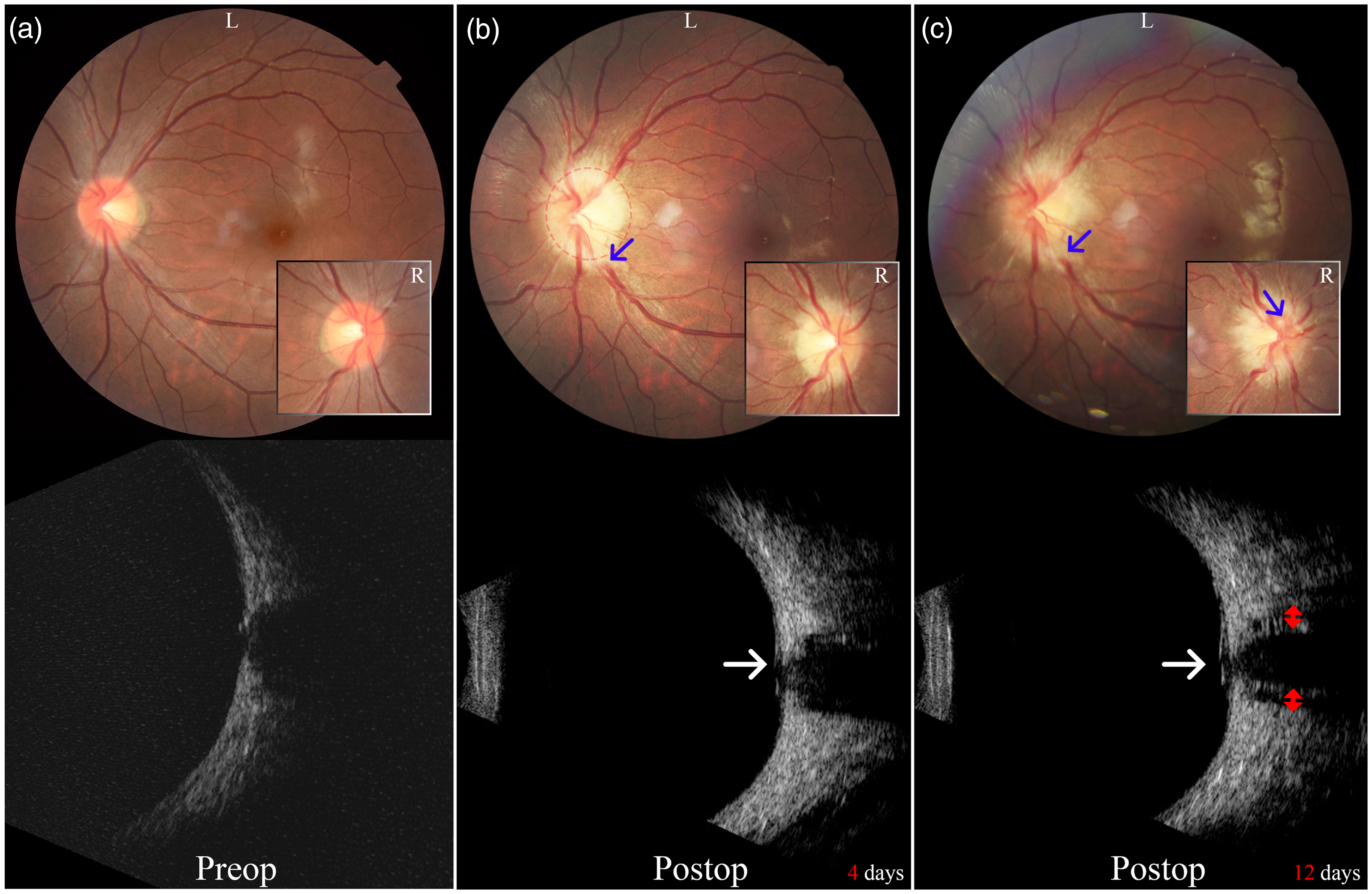
Operation-related morphological changes (preoperative, 4-day postoperative, and 12-day postoperative changes after extraluminal compression surgery) of bilateral optic discs captured using funduscopy and 20-MHz high-resolution transbulbar ultrasonography (left eye as the representative eye). (a) Preoperative absence of papilledema (both eyes: Frisén grade 0) shown by funduscopy and high-resolution transbulbar ultrasonography. (b) Postoperative funduscopy (blue arrow) and high-resolution transbulbar ultrasonography (white arrow) showing swollen optic discs 4 days after extraluminal compression (left eye: Frisén grade 3 papilledema; right eye: Frisén grade 2 papilledema). Loss of major vessels leaving the left optic disc and feathering of neurofibril layers (red dashed circle) were present and (d) Postoperative funduscopy (blue arrow) and high-resolution transbulbar ultrasonography (white arrow) showing swollen optic disc 12 days after extraluminal compression. Note the persistence of the obscuration of major vessels leaving the disc (both eyes: Frisén grade 3 papilledema). The bilateral subarachnoid space of the optic nerve 3 mm behind the lamina cribrosa was also increased (red double-headed arrows).
None of the patients in our study reported visual loss or changes in visual acuity, nor did they report chronic headache in addition to their stand-alone PT symptoms. Throughout a 12-year period of managing both inpatients and outpatients with stand-alone PT, we found that visual impairment and headache are rarely reported issues among Asian populations with isolated venous PT. Furthermore, our unpublished quantitative data suggest that papilledema is an infrequent finding among patients with isolated venous PT, with or without chronic headache. Moreover, the lower BMI of Eastern populations with isolated venous PT differs from reports focusing on IIH in Western countries, which may suggest a significant difference between the two populations.17,37,38 Both our current data and previous findings revealed a strong correlation between the BMI and ICP in patients with isolated venous PT. Additionally, ICP in 62% of Asian patients with isolated PT ranged from 200 to 250 mmH2O, which is lower than the ICP threshold proposed by the revised Dandy criteria.17,37 These results suggest that isolated PT might most appropriately be categorized as IIH without papilledema, a subcategory of IIH characterized by milder or intermittent intracranial hypertension. 24 The current study also showed that the loudness of PT decreased in 74.1% of patients after removal of CSF and resolved within 1 week. We surmise that dysregulation of CSF efflux and sinovenous hemodynamics may have existed but were not severe enough to induce worrisome ICP or ophthalmological/neurological symptoms among the current study population. Further studies comparing Eastern and Western populations will be critical for evaluating and treating patients with these conditions and may help to explain some of the differences in articles on this subject by authors from different regions.
This study has certain limitations that must be taken into account when interpreting the findings. First, ICP was determined exclusively in the lateral decubitus posture, which may raise questions regarding the generalizability of the results to other postures, such as sitting. However, according to Pascal’s law, which states that pressure changes within an incompressible fluid are uniformly transmitted throughout the fluid, substantial differences in ICP variations after compression of the IJV in different postures are unlikely to be observed. The primary factor influencing ICP variations is most likely the height of the TS when lying in a decubitus position. Second, the bilateral sinovenous patency test results were constrained by the small sample size of patients with venous PT associated with SSWAs. Despite this, our study was able to quantitatively demonstrate the consequences of sinus outflow obstruction and the dynamics of CSF pressure alteration as well as detect numerous statistical correlations. Third, we did not examine certain factors that could have contributed to a more comprehensive understanding of the mechanisms underlying the observed changes in ICP; such factors include sinus flow hemodynamics, venous branches, lymphatic vessels, capillaries, spinal compartments, and peri-venous/peri-arterial spaces. Moreover, intrinsic and extrinsic TS stenoses were not differentiated, although previous studies have demonstrated that the types of TS stenosis and arachnoid granulations in TS are not associated with ICP levels.35,36 Finally, the study focused primarily on the consequences of severe or complete obstruction, whereas reducing the diverticulum or extraluminal compression may facilitate venous return in milder cases of obstruction.
Conclusion
Individuals with isolated venous PT associated with SSWAs experience more intense increases in ICP when sinovenous flow obstruction occurs on the significantly larger side of the transverse–sigmoid sinus with less contralateral drainage. Although the extraluminal compression technique is safe and reversible, neurotologists must exercise caution when predicting ICP and avoid completely obstructing flow patency or overcompressing the sinus wall in patients with large Voldifference (high ipsilateral and low contralateral sinus patency) and low ICP to prevent a significant change in ICP. Furthermore, other important factors such as the patient’s BMI and the degree of bilateral stenosis should be considered before performing extraluminal compression surgery to safely resolve PT.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605231187949 - Supplemental material for Dynamics of cerebrospinal fluid pressure alterations and bilateral transverse–sigmoid sinus morphologies in Asian patients with venous pulsatile tinnitus
Supplemental material, sj-pdf-1-imr-10.1177_03000605231187949 for Dynamics of cerebrospinal fluid pressure alterations and bilateral transverse–sigmoid sinus morphologies in Asian patients with venous pulsatile tinnitus by Yue-Lin Hsieh, Bo Zuo, Yanhui Shi, Shenjiang Wang and Wuqing Wang in Journal of International Medical Research
Footnotes
Author contributions
Y-LH designed the study, analyzed all data, and drafted the manuscript. BZ and YS performed the cerebrospinal fluid manometry and collected the intracranial pressure data. SW performed the radiologic examinations. WW designed and supervised the study. All authors contributed to the article and approved the submitted version.
Declaration of Conflicting Interests
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Data availability statement
The original contributions presented in this study are included in the article/Supplementary Material. Further inquiries can be directed to the corresponding author.
Funding
This work was supported by the Natural Science Foundation of Shanghai (No. 20ZR1409600) to WW and by the Science and Technology Innovation Plan of Shanghai Science and Technology Commission (No. 22Y11902200) to WW.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
