Abstract
Objective
In this study, we aimed to analyze cost trends for the outpatient treatment of lumbar intervertebral disc herniation (LDH).
Methods
We used cross-sectional data obtained from the Korea Health Panel Survey from 2011 to 2015. We compared outpatient medical expenses for conservative treatment of LDH using traditional Korean medicine (TKM) or Western medicine (WM).
Results
This analysis revealed that the total medical expenses for outpatient treatment of LDH using WM treatment methods increased by 30% from 2011 to 2015, and self-payment expenses increased by 50%. The total medical expenses for outpatient treatment of LDH using TKM methods increased by 8%, and self-payment expenses decreased by 33%. The National Health Insurance Service (NHIS) expenditure for WM increased by 7%, and non-covered costs increased by 83%. The NHIS expenditure for TKM increased by 41%, and non-covered costs decreased by 66%.
Conclusions
The total medical expenses for WM treatments are increasing in Korea, especially for non-covered treatments. The non-covered costs for TKM treatments are decreasing, suggesting a change in medical cost trends according to whether Korea’s actual medical expense insurance scheme is applied.
Keywords
Introduction
Back pain is a very common condition, with 61.3% of Koreans experiencing back pain at least once in their lifetime. 1 Back pain is the most common cause of absence from work, leaving work early, or visiting a hospital. The highest level of disability-adjusted life years (DALYs) in Korea during 2015 was for back pain, with 2671 DALYs per 100,000 people. 2 Back pain occurs worldwide, increasing the socioeconomic burden. Studies have shown that the prevalence of back pain has increased over the past few decades, 3 as have the costs of treating back pain. 4 The costs of treating back pain vary depending on the treatment method but are among the highest treatment costs, together with costs for treating heart disease, depression, and headache. 5
The first incidence of lower back pain typically occurs between the ages of 20 and 29 years, and approximately 40% of patients develop degenerative changes in the intervertebral discs. 6 Lumbar intervertebral disc herniation (LDH) causes back pain and radiating pain 7 and is one of the most common causes of back pain.8,9 LDH is more likely to occur between the ages of 30 and 40 years, when degenerative changes worsen as the water content of the discs decreases.10,11
In South Korea’s 2018 Health Insurance Statistical Yearbook, 1,967,561 individuals had intervertebral disc disorders (International Classification of Diseases Tenth Revision [ICD-10] code M51, other intervertebral disc disorders). Many patients in South Korea are burdened by medical expenses owing to intervertebral disc disorders, reaching approximately 616,475,181 USD. These statistics correspond to benefits of public health insurance; however, when considering non-covered costs and socioeconomic production loss owing to disease, the cost of treating intervertebral disc disorders is much higher than the above amount. Using health insurance data from 2011, Ahn et al. analyzed the treatment costs and general treatment processes of patients with LDH in Korea. 12 However, the health insurance data used in that study did not provide information on non-covered costs, and the data on traditional Korean medicine (TKM) were extremely limited.
In Korea, conservative treatment methods using Western medicine (WM) as well as non-surgical integrated treatment methods using TKM are actively being used in the treatment of LDH. 13 Since 1951, South Korea officially recognizes a dual license system for doctors with both WM and TKM licenses.14,15 WM and TKM treatments for LDH are performed using different treatment principles and methods. According to the 2018 Health Insurance Statistical Yearbook, LDH was the 19th most prevalent disease code, with a large number of people undergoing TKM treatment. 16
Korea’s health insurance system is a social security system that allows the public to pay insurance premiums and receive medical services through insurance benefits provided by the National Health Insurance Service (NHIS). The NHIS aims to prevent excessive burdens on households owing to high medical expenses caused by illness or injury. 17 In the present study, data from the Korea Health Panel Survey were used to analyze trends from 2011 to 2015 in costs for outpatient conservative treatment both in Korea and in other countries, including non-covered costs for LDH, and to identify factors that affect changes in the trends of medical expenses.
Methods
Data source and study population
The cross-sectional data used in this study were from the Korea Health Panel Survey. This is a joint survey conducted annually by the Korea Institute for Health and Social Affairs and the NHIS that began in 2008. The main goal of the Korea Health Panel Survey is to construct panel data that can be analyzed in-depth, covering information not only on medical use behavior and medical expenditures but also on factors affecting the use of medical facilities and medical expenditures. 18 The respondents of the Korea Health Panel Survey were chosen using a probability proportionate and stratified cluster sampling method to maintain national representativeness. We used data collected from 2011 to 2015, with the exception of 2014 when no survey was conducted. The survey data are available for public use, with all identifiable personal information eliminated for privacy and confidentiality purposes.
We analyzed cases where intervertebral disc herniation was the main diagnosis necessitating medical intervention; therefore, cases of injury were excluded. Each year, all patients who had been treated for LDH were evaluated; hence, the same patient may be represented in multiple years. We divided patients into those treated with WM and those treated with TKM. Among hospitalized patients, WM methods were mostly used for surgical treatment, and TKM was used for conservative non-surgical treatment. It may not be appropriate to directly compare costs of surgical and non-surgical treatments. Moreover, these are difficult to compare because there were relatively few inpatient data for TKM in the Korea Health Panel Survey. Therefore, inpatient cases were excluded from the study. The characteristics of excluded inpatients receiving WN and TKM treatment are presented in Supplementary Table 1. Age, sex, income level, insurance coverage, and education level were analyzed to determine the demographic characteristics of patients. Patients who performed moderate physical activity for more than 30 minutes a day for more than 5 days a week were classified as physically active and the remaining patients were considered not active.
Total medical expenses were the sum of the costs reimbursed by the Korean NHIS and self-payment costs. Self-payment costs were the sum of out-of-pocket payments and non-covered expenses. The amount of compensation from Korea’s actual medical expense insurance coverage (described in detail in the Discussion) was not recorded in the database. Patients diagnosed with ICD-10 code M51 were classified as M51 compensation if they had been covered by the actual medical expense insurance scheme in that year.
The reporting of this study conforms to the STROBE guidelines. 19
Statistical analysis
All analyses were performed using SAS version 9.4 (SAS Institute, Cary, NC, USA). All continuous variables are presented as mean ± standard deviation, and categorical variables are presented as frequency and percentage.
Ethics statement
Owing to the retrospective nature of this study, which used data with encrypted personal information, this research was granted an exemption waiver for ethics approval and patient informed consent by the Institutional Review Board of Jaseng Hospital of Korean Medicine in Seoul, Korea (JASENG 2019-04-005). This study was conducted in accordance with the principles laid down in the Helsinki Declaration. There was no patient or public involvement in the study design or research techniques.
Results
In 2011, the Korea Health Panel Survey used its own unique disease codes; there were 2306 cases of lumbar spine and intervertebral disc disorder. After 2012, ICD-7 codes were used, and 23,061 patients were diagnosed using the code M51 in extraction of the data on intervertebral disc disease.
The demographic characteristics of both the TKM and WM treatment groups are shown in Table 1. A large percentage of patients were in the age range 50 to 79 years. There were more women than men, and there were more married patients than unmarried patients. Most patients had a high school education or lower. Although there was no significant difference in income level, more patients in the TKM group were in higher income quartiles than those in the WM group, and more patients in the TKM group were covered by private health insurance. Detailed demographic information on all participants can be found in Supplementary Table 2.
Demographic characteristics of patients with lumbar disc herniation, 2011 to 2015.
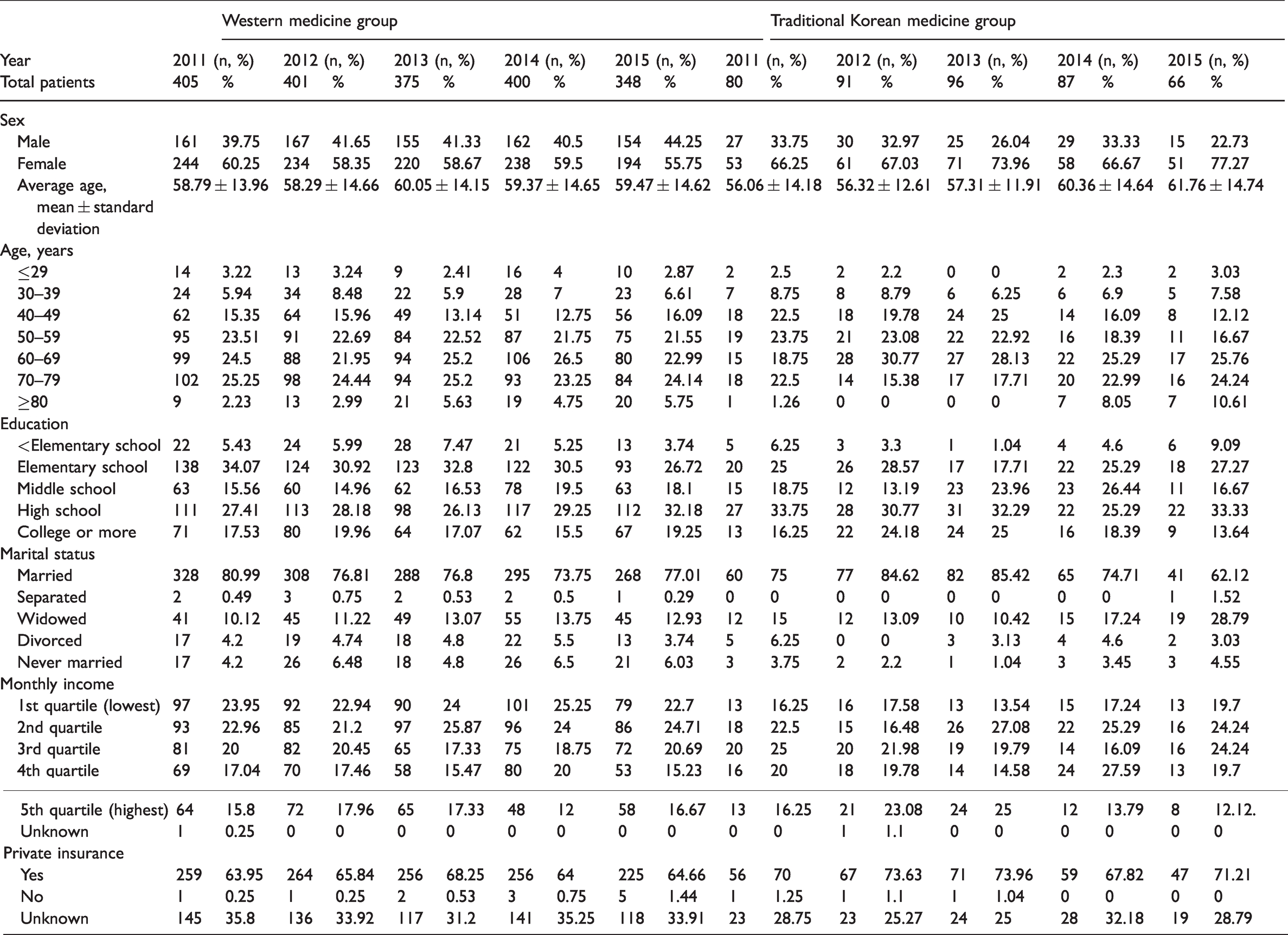
Table 2 shows patients’ characteristics in terms of health-related quality of life. Most patients in both groups had no history of smoking or drinking and were not physically active. A large percentage of patients self-reported their health as normal or poor. These results did not vary among survey years. Detailed quality of life data on all participants can be found in Supplementary Table 3.
Health-related quality of life in patients with lumbar disc herniation, 2011 to 2015.

NR, not reported; SD, standard deviation; EQ-5D, EuroQol five-dimension.
The results of cost analysis are shown in Table 3. The medical expenses per person in the WM treatment group increased from 297.61 USD in 2011 to 385.96 USD in 2015 (30% increase), and the self-payment costs increased from 147.93 USD in 2011 to 221.86 USD in 2015 (50% increase). The cost of medical treatment in the TKM group increased from 283.90 USD in 2011 to 307.72 USD in 2015 (8% increase), and the self-payment costs decreased from 172.73 USD in 2011 to 115.10 USD in 2015 (33% decrease). The medical expenses and self-payment costs in the WM group increased steadily each year from 2011 to 2015 (excluding 2014, when no survey was conducted). The medical expenses for TKM treatment increased from 2011 to 2013, before decreasing in 2014. The self-payment costs for TKM treatment were similar from 2011 to 2013 but decreased in 2014. The NHIS costs in the WM group increased from 139.99 USD in 2011 to 149.82 USD in 2015 (7% increase), and the non-covered costs increased from 97.46 USD in 2011 to 178.39 USD in 2015 (83% increase). Conversely, the NHIS costs in the TKM group increased from 145,975 won in 2011 to 205,239 won in 2015 (41% increase), and the non-covered costs decreased from 73.89 USD in 2011 to 25.46 USD in 2015 (66% decrease). In the WM treatment group, the NHIS costs increased until 2014 and then decreased in 2015; however, the non-covered costs rose sharply in 2015, accounting for an increase in total medical expenses. In the TKM treatment group, the NHIS costs were highest in 2013 and decreased in 2014. The non-covered costs decreased sharply in 2015, accounting for a decrease in total medical expenses. The costs of actual medical expense insurance for the WM treatment group increased from 201.97 USD in 2011 to 1186.69 USD in 2015 (488% increase). The costs of actual medical expense insurance for the TKM treatment group was 161.09 USD in 2011 and 0 USD in 2012; this showed a tendency to decrease until 2013 and then increased to 293.76 USD in 2015.
Comparison of treatment costs for patients with lumbar disc herniation, 2011 to 2015.

*Medical costs: sum of self-pay costs and NHIS costs paid to medical care institution.
§Non-covered costs: costs not guaranteed by the National Health Insurance, of which the patient must pay 100%.
NHIS, National Health Insurance Service.
The reasons for outpatient visits and treatment components of the WM and TKM treatment groups are summarized in Table 4. In both groups, most patients presented for treatment. In the WM treatment group, several patients received drug treatment and rehabilitation or physical therapy. More than 90% of patients did not undergo diagnostic testing, among which blood, urine, and stool testing as well as X-ray and MRI imaging were the most common types. In the TKM treatment group, acupuncture, moxibustion, and cupping treatments accounted for more than 90% of treatments.
Treatment components of Western medicine and traditional Korean medicine.

NA, not applicable. MRI, magnetic resonance imaging; CT, computed tomography.
Discussion
In this study, we compared and analyzed the trends in outpatient expenditure between patients with LDH who underwent WM treatment and those who used TKM treatment methods. There was no significant demographic difference between the two groups, and both groups had a large number of women aged 50 to 79 years. This is consistent with findings in an analysis of 165 studies from 54 countries between 1980 and 2009, which reported that low back pain occurs more frequently in women between the ages of 40 to 80 years. 20 Most patients in our study had no history of smoking, drinking, or physical activity.
In both treatment groups, drug therapy and physical therapy were the most common treatment types. These results are in line with those of a study by Ahn et al. 12 The medical panel data used in this study did not contain detailed treatment information; hence, the specific types of physical therapy received were unknown. According to the data presented in another Korean study, it can be assumed that the physical therapy included in our analysis involved a large number of non-covered manual therapies, given that the largest number of non-covered insurance claims, except for testing, were for non-covered manual therapies. 21
Acupuncture accounted for approximately 90% of treatment modalities in the TKM treatment group. Acupuncture controls pain through the regulation of connective tissue, nerve fibers, and endogenous nerve peptides.22–24 According to systematic reviews, acupuncture relieves pain in patients with chronic back pain, reduces the social and medical costs of back pain, and improves functioning alone or in combination with other therapies.25–28 In Korea, a number of herbal treatments using herbal medicines, pharmacopuncture, and Chuna therapy are performed to treat LDH, with positive results. 13 More patients in Korea use TKM treatment methods because even though the actual medical expenses for these methods are not covered by insurance, the non-covered costs have been gradually decreasing.
Korea’s actual medical expense insurance scheme was introduced in 2003 to supplement public health insurance. This type of insurance compensates patients for medical expenses, such as copayments and deductibles that are not covered by the NHIS. As of 2018, 34.21 million people were insured under this scheme in South Korea. 29 We found that the amount compensated by actual medical expense insurance in the WM treatment group increased by approximately 488% from 2011 to 2015 whereas the amount compensated by actual medical expense insurance in the TKM treatment group showed only a small increase. Because Korea’s actual medical expense insurance covers items that are not covered by public insurance, the number of non-covered treatments that can be covered by actual medical expense insurance is increasing rapidly. Actual medical expense insurance-related statistics show that as of 2013, the non-covered costs of total medical expenses for policyholders accounted for 36.3% of the total medical expenses of the entire population whereas the total non-covered costs of the entire population were 18%. 30 In other words, a policyholder of actual medical expense insurance is more likely to receive non-covered treatment because they can receive compensation from actual medical expense insurance. In comparison, non-covered treatments for TKM have been excluded from actual medical expense coverage since 2009. The total medical costs of TKM treatments have increased from 2011 to 2015. This is because the number of non-covered TKM treatments has decreased rapidly, and the number of treatments covered by health insurance has increased. Patients who had actual medical expense insurance prior to 2009 may have received compensation for more types of TKM treatments.
We found no remarkable difference in conservative outpatient treatments between the TKM treatment group and WM treatment group in this study. Although patient characteristics were not significantly different between the two groups, the cost trends changed differently. Compared with the WM group where the total and patient-borne medical expenses have been continuously increasing, the total medical costs in the TKM group have risen only slightly and patient-borne medical expenses have decreased. Furthermore, the non-covered costs for WM treatment have increased rapidly, and non-covered costs for TKM treatment methods have decreased rapidly. Actual medical expense insurance may have affected this trend. Because non-covered WM treatment is covered by actual medical expense insurance, the type of medical intervention used is changing in a way that reduces the patient’s burden and increases the total cost of using actual medical expense insurance. In practice, patients are free to choose non-covered treatments when the treatment is covered by actual medical expense insurance; however, receiving non-covered treatment without having actual medical expense insurance increases the personal burden of treatment costs. This trend is seen in other analyses in Korea wherein new subscribers to actual medical expense insurance have significantly increased total medical costs compared with non-subscribers. 31 Therefore, the changing trend of medical expenses in Korea may be influenced by the application of private insurance rather than the introduction of new treatment methods or changes in the medical environment. Moreover, the conclusion that actual medical expense insurance enrollments increase costs for non-covered WM treatment has been previously reported 31 ; however, that study did not account for the increasing number of TKM treatment modalities that are covered by health insurance.
This study has several limitations. First, Korea’s dual medical environment and health insurance system are different from those of other countries; hence, the results of this study cannot be generalized to countries other than Korea. It is necessary to interpret the results of this study in view of each country’s specific health care system. Second, the medical panel questionnaire was altered in the middle of our study period. Therefore, care must be taken in interpreting the results. Third, because the TKM treatment group was much smaller than the WM treatment group, there is a limitation in comparing the data. Fourth, owing to data limitations, we could not separate the expenses of patients who used both treatment methods simultaneously. Because it is unlikely that non-covered costs in the TKM treatment group were compensated unless these patients enrolled in actual medical expense insurance prior to 2009, it is possible that the affected patients all paid for WM treatments. It is difficult to confirm whether the actual medical expense insurance paid for each treatment type. Therefore, as the costs were included in both groups but the cost of TKM treatment was not likely to be compensated, it is probable that the amount of medical expense compensation for the TKM group was overvalued.
Despite these limitations, in this study, we successfully analyzed non-covered costs of LDH treatment using Korea Health Panel Survey data. The findings suggested that the difference in WM and TKM medical cost trends in Korea may have an impact on the use of WM treatment methods as well as the application of NHIS medical insurance and actual medical expense insurance.
Conclusion
In this study, we analyzed Korean Health Panel Survey data to provide information on trends in non-covered WM and TKM outpatient treatment costs from 2011 to 2015 among patients with LDH in Korea. The total medical expenses for WM treatments are increasing in Korea, especially for non-covered treatments. The non-covered costs for TKM treatments are decreasing. Non-covered WM treatment is compensated in all patients with private insurance whereas non-covered TKM treatment is not compensated in a significant number of patients with private insurance, resulting in a change in patients’ medical consumption patterns. This seems to account for the difference in trends between WM and TKM medical costs and suggests that this difference may be according to whether the actual medical expense insurance is applied. These data could be of interest to company stakeholders, as well as health policy makers.
Supplemental Material
sj-pdf-1-imr-10.1177_03000605211051583 - Supplemental material for Analysis of outpatient expenditure trends using Korean Health Panel Survey data of patients diagnosed with lumbar intervertebral disc herniation
Supplemental material, sj-pdf-1-imr-10.1177_03000605211051583 for Analysis of outpatient expenditure trends using Korean Health Panel Survey data of patients diagnosed with lumbar intervertebral disc herniation by Won-Jun Lee, Chang-Hyun Han, Changsop Yang, Sook-Hyun Lee, Doori Kim, Inhyuk Ha, Hyun Jin Song and Yoon Jae Lee in Journal of International Medical Research
Supplemental Material
sj-pdf-2-imr-10.1177_03000605211051583 - Supplemental material for Analysis of outpatient expenditure trends using Korean Health Panel Survey data of patients diagnosed with lumbar intervertebral disc herniation
Supplemental material, sj-pdf-2-imr-10.1177_03000605211051583 for Analysis of outpatient expenditure trends using Korean Health Panel Survey data of patients diagnosed with lumbar intervertebral disc herniation by Won-Jun Lee, Chang-Hyun Han, Changsop Yang, Sook-Hyun Lee, Doori Kim, Inhyuk Ha, Hyun Jin Song and Yoon Jae Lee in Journal of International Medical Research
Supplemental Material
sj-pdf-3-imr-10.1177_03000605211051583 - Supplemental material for Analysis of outpatient expenditure trends using Korean Health Panel Survey data of patients diagnosed with lumbar intervertebral disc herniation
Supplemental material, sj-pdf-3-imr-10.1177_03000605211051583 for Analysis of outpatient expenditure trends using Korean Health Panel Survey data of patients diagnosed with lumbar intervertebral disc herniation by Won-Jun Lee, Chang-Hyun Han, Changsop Yang, Sook-Hyun Lee, Doori Kim, Inhyuk Ha, Hyun Jin Song and Yoon Jae Lee in Journal of International Medical Research
Footnotes
Data statement
The data that support the findings of this study are available from the Korea Health Panel Study; however, restrictions apply to the availability of these data, which were used under license for the current study and are thus not publicly available.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This study was financially supported by grants from project KSN2021210 of the Korea Institute of Oriental Medicine, Republic of Korea.
Author contributions
Conceptualization, Inhyuk Ha and Yoon Jae Lee; Data curation, Won-Jun Lee and Yoon Jae Lee; Investigation, Doori Kim and Won-Jun Lee; Methodology, Sook-Hyun Lee and Hyun Jin Song; Project administration, Inhyuk Ha, Yoon Jae Lee, and Chang-Hyun Han; Supervision, Changsop Yang and Chang-Hyun Han; Writing – original draft, Won-Jun Lee; Writing – review and editing, Won-Jun Lee and Yoon Jae Lee.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
