Abstract
Squamous cell carcinoma (SCC) is a malignant epithelial tumor originating from the bronchial epithelium that shows keratosis and/or intercellular bridges. Papillary squamous cell carcinoma (PSCC) is an extremely rare subtype of SCC that manifests with a unique intrabronchial papillary growth pattern. Surgical resection is still the first recommendation for localized noninvasive SCC. However, some patients are not candidates for surgical resection. With the development of interventional pulmonology, bronchoscopic interventional therapy has played a key role in the treatment of central airway tumors. Here, we report a case of noninvasive PSCC in the airway treated with an electric snare, argon plasma coagulation (APC), and cryotherapy. After removing the tumor by electrotomy, cryotherapy, and APC, the tumor was injected with Endostar 15 mg (3 ml) and cisplatin 20 mg (diluted to 3 ml with 0.9% normal saline) in six separate sites, once every 21 days. The tumor was eliminated, and the treatment was stopped after four treatment cycles. During the 1-year follow-up, there was no recurrence of PSCC in the airway. In this case, submucosal injections of Endostar combined with cisplatin was a feasible and effective endoscopic method for treating a low-grade intratracheal malignant tumor.
Keywords
Introduction
Squamous cell carcinoma (SCC) is a malignant epithelial tumor originating from the bronchial epithelium that shows keratinization and/or intercellular bridges. Papillary squamous cell carcinoma (PSCC) is a rare variant subtype of SCC. 1 PSCC mostly manifests with a unique intrabronchial papillary growth pattern. 2 Although the preferred therapy is surgery for such benign tracheal tumors, our previous publication (Jiang et al) showed that bronchoscopic interventions (such as using Endostar and cisplatin) are important and effective alternatives for patients who are not candidates for surgical resection. 3
A variety of techniques, such as electrocautery, argon plasma coagulation (APC), laser, and cryotherapy through a flexible or rigid bronchoscope, have been used to treat tracheobronchial tumors. However, the combination of simple tumor excision and chemotherapy leads to a local recurrence rate of more than 40%. 4 As a result, an approach that can resect tracheal tumors with no recurrence is urgently needed.
Submucosal injection therapy by electronic bronchoscopy refers to the injection of various drugs into the lung parenchyma or tracheal mucosa through a special injection needle under bronchoscopy to treat diseases or make a definitive diagnosis. By injecting drugs into the submucosa, the tumor undergoes necrosis, the tracheal lumen becomes unobstructed, tumor growth is slowed, and recurrence is prevented.
Here, we report a case of noninvasive PSCC in the airway successfully treated with a combination of bronchoscopic intervention and submucosal injections of Endostar and cisplatin. The patient provided written informed consent for treatment and to have this case report and any accompanying images published. Institutional approval was obtained from the Institutional Ethical Review Board of Qingdao Haici Hospital (approval number: 2016HC06LQ036) to publish the case details.
Case presentation
A 78-year-old female patient was admitted to our hospital with a complaint of cough with sputum for more than 1 year, with worsening symptoms accompanied by chest congestion for more than 1 month. Breath sounds in both lungs were muffled, and loud wheezing sounds could be heard during both the inspiratory and expiratory phases. Renal function testing revealed the following: urea nitrogen: 9.2 mmol/L (reference range: 3.2–7.1 mmol/L), creatinine: 93 µmol/L (reference range: 35–80 µmol/L), and uric acid: 361 µmol/L (reference range: 140–340 µmol/L). Chest computed tomography (CT) revealed nodules in the right wall of the lower trachea, and the local lumen was narrowed. which could be clearly seen from the lung window (Figure 1a) and mediastinal window (Figure 1b), respectively. Enhanced CT showed a soft tissue mass in the right wall of the lower trachea. The maximum size was approximately 1.7 cm × 1.0 cm × 1.8 cm. Enhanced CT showed obvious areas of enhancement, and the local lumen was narrowed, as the lung window (Figure 1c) and mediastinal window (Figure 1d) showed. The patient underwent bronchoscopy, which showed a well-circumscribed posterior soft tissue mass occluding over 75% of the tracheal lumen, with the lower end invading the carina (Figure 2). The papillary stalk was composed of loose blood vessels and connective tissue interstitium. The surface of the papilla was covered with squamous epithelium, and the layer of spinous cells was significantly thickened. Atypical hollow cells were observed in a scattered, nested, or corded pattern. Atypical squamous cells were polygonal or oval in shape, with disorganization, diverse nuclear morphology, dark staining, visible mitosis, and invasive growth pattern. The pathology department determined that this pathological type is extremely rare, and the recommended diagnosis was PSCC (Figure 3a). Immunohistochemistry revealed Ki67 60% (+), cytokeratin (CK)5/6 (+), P40 (+), CK7 (−), cluster of differentiation (CD)56 (−), thyroid transcription factor 1 (ttf-1) (−), synaptophysin (Syn) (−), P53 (−), P63 (+), napsin A (−), villin (−), and CK20 (−) (Figure 3b). Microscopically, the tumor appeared as a typical squamous cell papilloma. The clear diagnosis was grade cT4N0M0 IIIa primary central exophytic PSCC. The patient refused surgical resection of the trachea and had a performance status (PS) score of 3, which did not meet the criteria for chemotherapy and radiotherapy. Considering that APC and cryotherapy may cause tumor recurrence, with full informed consent, she underwent the following: APC cauterization, freezing and thawing with carbon dioxide, and freezing and clamping the tumor tissues, including snare excisions (Figure 4a), argon plasma coagulation (Figure 4b), carbon dioxide freezing (Figure 4c), and tumor removal (Figure 4d). Additionally, 15 mg of Endostar was applied to the residual tumor roots, and 0.5 ml of cisplatin 20 mg was injected into six separate sections of the tumor (Figure 4e). At the third, sixth, and ninth weeks after the treatment, Endostar + cisplatin was injected into the submucosa again. Bronchoscopy findings 2 weeks after treatment are shown in Figure 5a. Tracheal zones II to III showed 30% lumen stenosis, and the tracheoscope (external diameter: 4.9 mm) could pass through (Figure 5b). After 6 weeks, pathological examination showed that there were many areas of necrotic tissue (Figure 5c). There were no significant abnormalities on chest CT 3 months after the operation, as shown in the lung window (Figure 6a) and mediastinal window (Figure 6b).

Chest computed tomography (CT) images. (a) Chest CT lung window: A nodular shadow is visible in the right wall of the lower trachea, with local luminal narrowing. (b) Chest CT mediastinal window: Small lymph nodes are visible. (c, d) Enhanced CT: A soft tissue shadow is present on the right wall of the lower trachea with a maximum size of 1.7 cm × 1.0 × cm × 1.8 cm, with obvious enhancement.

Bronchoscopy: The image shows a well-circumscribed posterior soft mass occluding over 75% of the tracheal lumen, with the lower end invading the carina. The tracheoscope (4.9 mm) could pass through the trachea.

Images of the squamous cell papilloma. (a) The tumor images show typical squamous cell papilloma. The papillary stalk consists of loose blood vessels and connective tissue stroma. The surface of the papilla is covered with multiple layers of squamous epithelium, and the spinous cell layer is obviously thickened. Atypical hollow cells are visible with a scattered, nested, or corded pattern. Heteromorphic squamous cells are polygonal or elliptical in shape and disorganized, with diverse nuclear morphology, deep staining, visible mitosis, and an infiltrative growth pattern. (b) Immunohistochemistry revealed Ki67 60% (+), cytokeratin (CK)5/6 (+), P40 (+), CK7 (−), cluster of differentiation (CD)56 (−), thyroid transcription factor-1 (ttf-1) (−), synaptophysin (Syn) (−), P53 (−), P63 (+), napsin A (−), villin (−), and CK20 (−).

Bronchoscopy. (a) Snare excisions; (b) Argon plasma coagulation; (c) Carbon dioxide cryotherapy; (d) Tumor removal; (e) Drug injection into the residual tumor root.
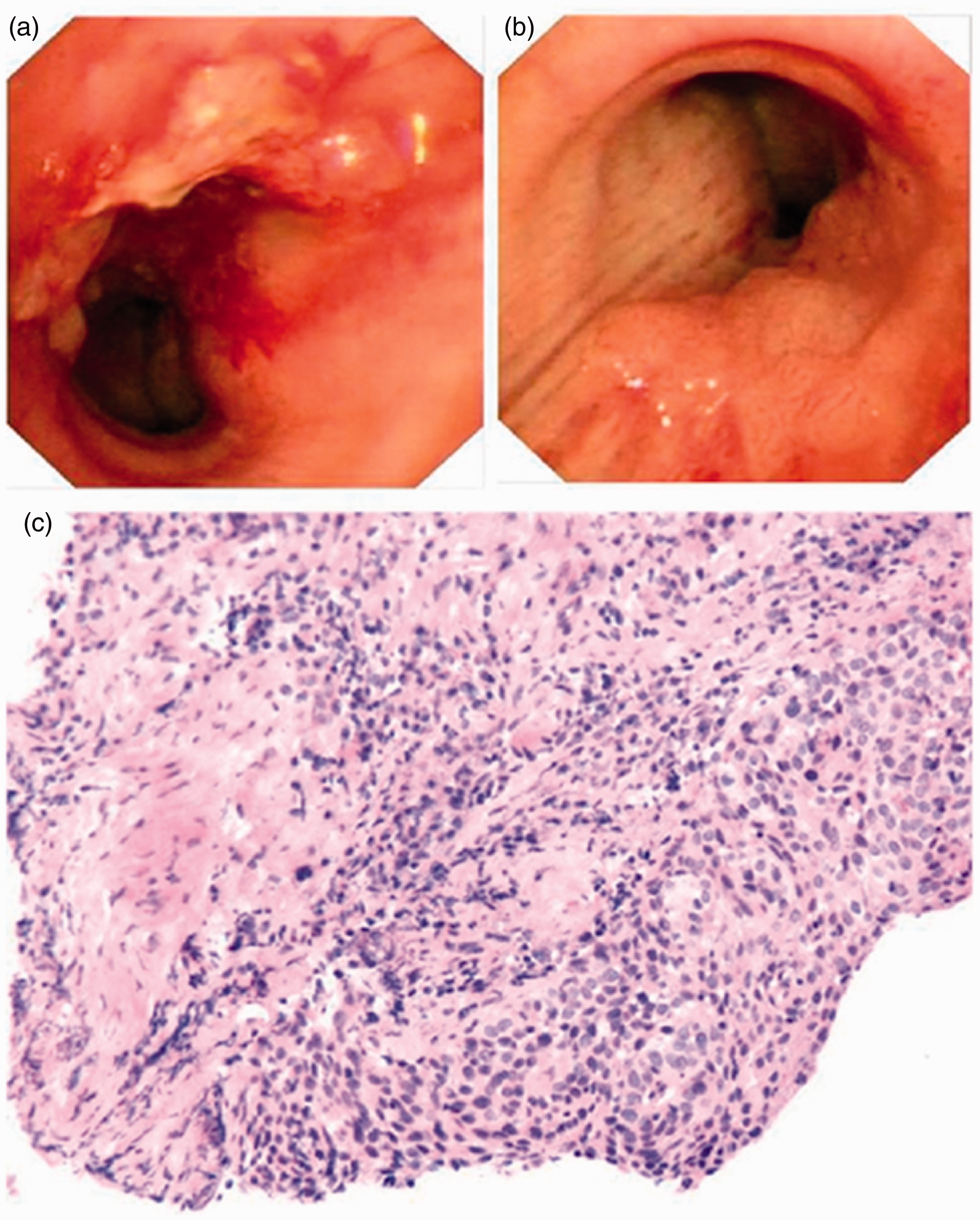
Bronchoscopy and cell death. (a) Bronchoscopy 2 weeks after treatment. (b) Bronchoscopy: Tracheal zones II to III show 30% luminal stenosis, and the tracheoscope (external diameter: 4.9 mm) passes through. (c) A large amount of necrosis and apoptosis are visible centrally. Pathological score: IIB.

Chest computed tomography (CT). (a) Lung window. (b) Mediastinal window. The right wall of the lower trachea is slightly thickened.
After a 2-year follow-up, no recurrence was found in the trachea, the patient was generally in good condition, and no obvious abnormalities were found in routine blood examination or liver and kidney function assessments. Note that at the beginning of the clinical observation, we also worried that this patient had abnormal renal function, which might increase the risks associated with chemotherapy with Endostar + cisplatin. Fortunately, to date, the patient’s renal function is good.
In addition, it has come to our attention that there is still tumor tissue in the inner wall of the trachea and that there is still some distance from a small protrusion located where the surgery was done. The treatment purpose of microscopic injections is to prolong the time to airway restenosis, improve tracheal ventilation, and improve the patient’s quality of life. The residual tumor in the inner wall needs to be inhibited by injection, argon, and freezing. The traditional methods for tumors outside the tracheal wall include but are not limited to chemotherapy, targeted therapy, radiotherapy, and immunotherapy. In addition, clinical injection combined with immunotherapy has been approved. We consider that injection therapy may increase the exposure of tumor antigens and enhance the efficacy of immunotherapy, to better treat extratracheal tumors.
The reporting of this study conforms to the CARE guidelines. 5 We have de-identified all patient details, such as confirming that all patient details are removed from the figures.
Discussion
PSCC is a rare type of SCC. Previously, the World Health Organization (WHO) guidelines classified PSCC as SCC, but PSCC is now classified as a unique malignant tumor, distinct from verrucous cancer and other exogenous SCCs. 6 Owing to the limited number of cases in the literature, the biological behavior of PSCC is currently unclear, although it is considered a low-grade malignancy. 7 Surgical resection is still the first recommendation for localized noninvasive SCC. Our patient was unable to undergo surgery because of the difficult lesion location, invasion into the carina, and the high degree of trauma associated with the operation. Therefore, we considered bronchoscopic interventional therapy, APC electrocautery, electric knife excision, and cryotherapy, combined with submucosal drug injection.
For patients with malignant intratracheal tumors, intratumoral injections of chemotherapeutic drugs combined with cryotherapy and hyperthermia can have synergistic effects. 8 This method of locally injecting drugs through a tracheoscope can significantly increase the drug concentration in the tumor, which rapidly shrinks the tumor body to quickly relieve airway obstruction and dyspnea, and effectively improve ventilation. High-concentration cisplatin injections in the tumor can efficiently kill tumor cells and effectively reduce the toxicity and side effects of systemic medications. Many doctors have performed this technique, clinically, and obtained positive results. 9 Regarding local injections of cisplatin combined with injections of Endostar, 3 we consider that Endostar has a significant anti-angiogenesis effect and can significantly reduce the expression of vascular endothelial growth factor (VEGF). Endostar has a marked effect on inhibiting tumor invasion and metastasis. Current studies have shown that Endostar can directly inhibit the proliferation, migration, and differentiation of endothelial cells and promote the growth of vascular endothelial cells. Endothelial cell apoptosis can promote angiogenesis and increase vascular permeability by inhibiting the growth of vascular endothelial cells. This approach has the advantages of a broad antitumor spectrum, low toxicity, and no drug resistance. The combination of endothelial cell apoptosis and cisplatin can have synergistic effects.10–12 The clinical response in our case supports our hypothesis. Our case shows that intratracheal submucosal injections are a good treatment that can fully inhibit the growth of low-grade malignant tracheal tumors and reduce the possibility of recurrence. In this case, Endostar combined with cisplatin submucosal injections increased the local drug concentration and the degree of tumor necrosis so that the clinical response was better than that with electrotomy and APC, only.
Notably, there are several limitations in our study. We reported only one case, and the efficacy of the combination of Endostar and cisplatin in treating benign or low-grade tracheal malignancies should be further evaluated. In addition, long-term follow-up should be performed to observe the long-term efficacy of submucosal drug injections. This is a rare disease at the limit between benign and malignant disease. In select cases surgery is not an option, and alternative treatments are under evaluation. Further studies are needed to evaluate this strategy; however, in the meantime, the medical community must benefit from this first experience.
Patients with PSCC who are not suitable for systemic or surgical treatments can be successfully treated with a combination of bronchoscopic interventional therapy and submucosal injection therapy.
Footnotes
Availability of data and materials
This is a case report, and it does not contain relevant materials and data.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
