Abstract
Because of the lack of anatomical landmarks during reduction of multiple articular surfaces and fragments in comminuted patellar fractures, loss of bone fragments or aggravation of soft tissue and ligament injuries readily occurs. In the present case, we used multiple three-dimensional (3D)-printed guide plates to reduce and fix a comminuted patellar fracture. A 22-year-old man was hospitalized for 2 days because of left knee joint pain and limited movement caused by a traffic accident. Preoperative imaging revealed a comminuted fracture of the left patella (type 34-C3 according to the AO/OTA classification). Throughout a 2-year follow-up, the patient remained in generally good condition with no significant limitation of his left knee joint activity. Application of multiple 3D-printed guide plates is a safe and effective auxiliary technique for the treatment of comminuted patellar fractures. This novel technique can shorten the operation time, reduce the number of fluoroscopic procedures, and ensure fracture healing and recovery of knee joint function through reliable reduction of the articular surface.
Keywords
Introduction
In patients with comminuted patellar fractures, loss of bone fragments or aggravation of soft tissue and ligament injuries readily occurs because of the lack of anatomical landmarks during reduction of multiple articular surfaces and fragments. Therefore, an improved reduction technique is needed.1,2 A three-dimensional (3D)-printed guide plate can be used to accurately reduce the comminuted bone pieces and further guide the reduction of fracture pieces. This can in turn improve the reduction efficiency, shorten the operation time, and establish a foundation for later rehabilitation and fracture healing.3,4 In the present case, we used multiple 3D-printed guide plates to reduce and fix a comminuted patellar fracture, thus achieving accurate, rapid, and effective reduction and fixation.
Case presentation
A 22-year-old man was admitted to the hospital for 2 days because of left knee joint pain and limited movement caused by a traffic accident. Physical examination on admission showed that the left knee joint was swollen with local tenderness, but no open wounds were present. The floating patella test was positive, and the muscle strength of the left lower extremity was normal. Preoperative imaging revealed a comminuted fracture of the left patella (Figure 1), determined to be type 34-C3 according to the AO/OTA classification.
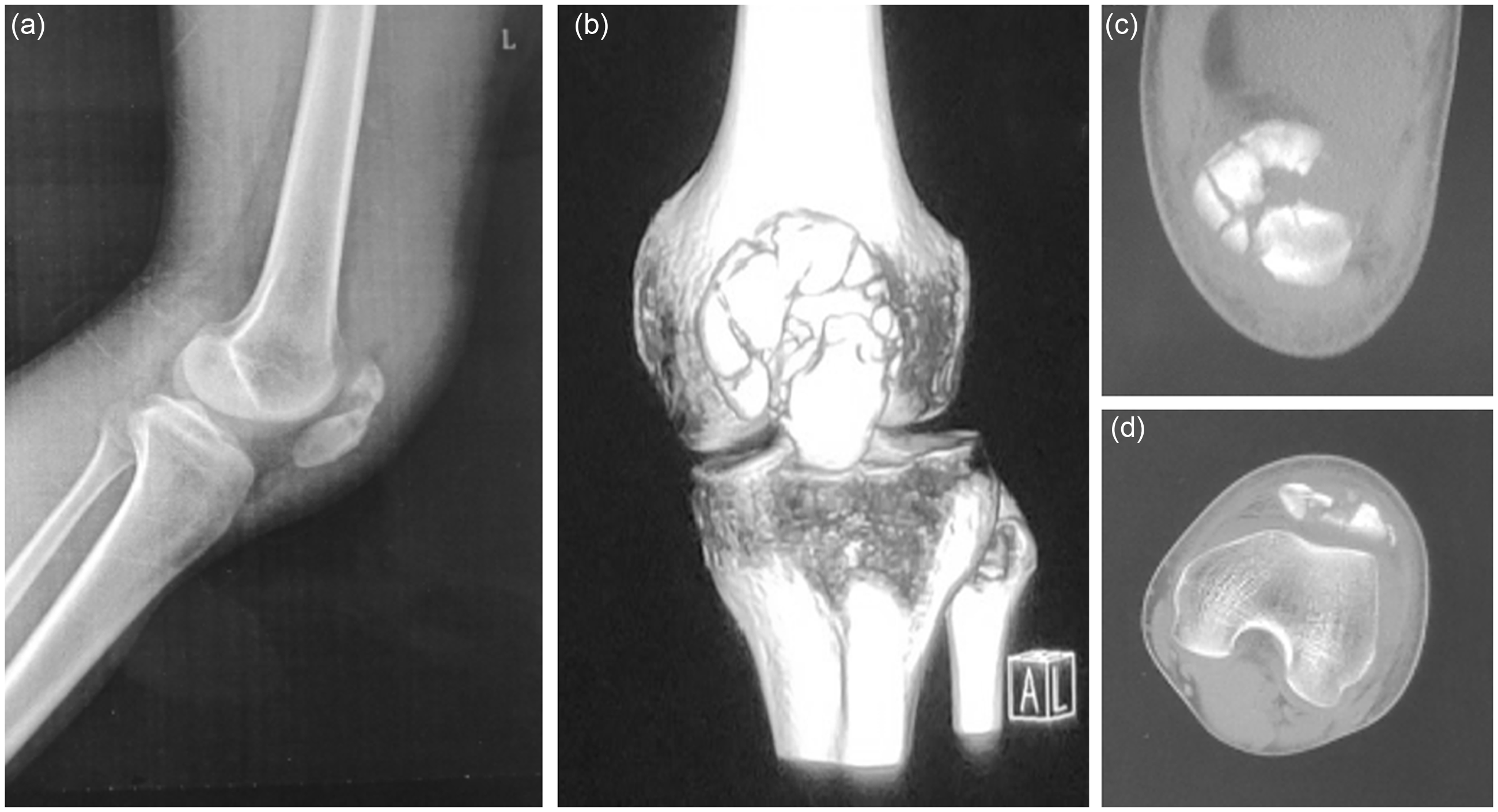
Preoperative imaging examination of the left patella. (a) Lateral radiograph of left patella fracture. (b) Anteroposterior radiograph left patella fracture. (c, d) Computed tomography image of left patella fracture.
Before the operation, both sides of the patella were scanned by computed tomography (CT) with a scanning thickness of 1 mm. The collected CT data were imported into Digital Imaging and Communications in Medicine format, and a 3D model was established by Mimics 19.0 software (Siemens, Berlin, Germany). Next, a mirror-image model of the healthy patella was used as a template to virtually reset the affected patella. This allowed us to further design and print the complete patella and the distal and proximal fractured patellar reduction guide plates with the cartilage surface as the mask. The patella model after virtual resetting and the data for the three corresponding reset guide plates were imported into the 3D printer in stereolithography format, and the model and guide plates were then printed out (Figure 2).

Morphology of patella presented in Mimics 19.0 software and morphology of reduction after attachment of guide plates. (a, b) Morphology of left patella fracture in Mimics 19.0 software. (c–e) Simulation and design of guide plate of left patella fracture in Mimics 19.0 software.
The patient underwent spinal anesthesia and was placed in the supine position, and an anterior median incision was made in the left knee joint. First, the local reduction guide plate of the proximal patella was placed behind the articular surface of the patella, and the large pieces adjacent to the cartilage surface were identified. The proximal patellar reduction guide plate was used for splicing, and a 1-mm fine Kirschner wire was used for temporary fixation in the coronal direction. All bone fragments with the cartilage surface at the proximal end of the patella were assembled together and temporarily fixed with a fine Kirschner wire, allowing the proximal patellar cartilage surface bone fragments to be restored to a whole. The other pieces of the proximal patella separated in the coronal position were then assembled together on the proximal patella, which had been anatomically reduced on the cartilage surface, and were also temporarily fixed with a fine Kirschner wire. Reduction and temporary fixation of the distal patellar comminuted fracture were completed using the same method. The patella was reinforced with a steel wire tension band, and all temporary fine Kirschner wires were removed for completion of precise reduction and fixation of the entire patella (Figure 3).

(a) Multiple guide plates and patella model printed by 3D printer. (b) Resetting and fixation of the bone blocks under the guidance of the guide plate. (c) Good restoration of the articular surface.
After the operation, the patient’s incision healed well. Reexamination of the left knee joint 1 week postoperatively showed that the patella was positioned well and that the internal fixation had not loosened. Six weeks after the operation, the patient was fully weight-bearing, and the fracture had healed completely at 3 months postoperatively (Figure 4). At the last follow-up (2 years after the operation), the patient’s visual analog scale score was 1, the range of motion of the left knee joint was 130°, and the Böstman score of the knee joint was 28.8 points.

General appearance and postoperative imaging examination of left patella. (a) Anteroposterior radiograph after fixation of left patella fracture. (b) Lateral radiograph after fixation of left patella fracture. (c) Two years postoperatively, the left knee joint activity was normal.
Discussion
The preferred treatment method for comminuted patellar fractures involving the articular surface is open reduction and internal fixation. The purpose of the operation is to restore the integrity of the articular surface and reconstruct the knee joint extension device. 5 However, the patella is often multi-articular and irregular, and comminuted patellar fractures often involve small bone blocks, apparent displacement, and lack of soft tissue adhesions. Thus, during the operation, a simple trial or direct vision is less effective for accurate reduction of the patella. Although the anterior bone block can often be perfectly reduced, the radiograph may still show that the articular surface has steps, openings, sagittal angles, or patellar deformation, which ultimately affects the postoperative functional outcomes. 6
Three-dimensional printing can assist virtual reduction of the affected patella through the mirror image of the healthy side. Virtual reduction of the patella can guide the identification of each broken bone block during the operation and confirm the mutual positional relationship between the broken bone blocks. Multiple guide plates can be used to effectively and accurately reset the crushed bone blocks. The local reduction guide plate can be used to guide effective reduction of the local bone blocks, plan the position of the Kirschner wire, and effectively avoid blocking the subsequent internal fixation device.7,8 In addition, the reduction guide plate with articular cartilage as the mask can be used to accurately reset and arrange the comminuted bone blocks on the surface of the guide plate, correct the angular and horizontal or sagittal displacement of the patella articular surface, and avoid poor joint reduction under X-ray fluoroscopy. Meanwhile, the proximal and distal local reduction guide plates can realize the reduction of local bone blocks and reduce the incidence of joint–bone block loss and internal fixation failure caused by repeated operations, thus enhancing the fixation strength.9,10
Precautions for the treatment of comminuted patellar fractures assisted by 3D-printed guide plates include the following. 1) When importing the CT data of the bilateral patellae into Mimics software, the scanning layer must be thinned as much as possible and the minimum scanning layer thickness must be controlled at 1 mm; this will be conducive to constructing the 3D data and avoiding the error of reduction. 2) The mirror image of the healthy patella is used as the template for virtual reduction of the affected patella, and a total patellar reduction guide plate with the cartilage surface as the mask can be designed and printed based on this image. 3) When designing local reduction guide plates, it is necessary to shear, move, rotate, and reset the comminuted fracture blocks in Mimics software. After virtual reduction, the proximal and distal reduction guide plates for the patella can be created according to the fracture line of the main bone blocks, and multiple small local reduction guide plates can be flexibly created to realize the local to overall reduction strategy. 4) The guide plate can be marked locally, and the relative normal residual bone can also be folded back to wrap the edge of the bone block and thus improve the accuracy of reduction. 5) When the whole guide plate is placed, the parapatellar retinaculum can be properly opened and sutured after reduction and fixation.
Conclusion
The application of multiple 3D-printed guide plates is a safe and effective auxiliary technique for the treatment of comminuted patellar fractures. This novel technique can shorten the operation time, reduce the number of fluoroscopic examinations, and ensure fracture healing and recovery of the knee joint function through reliable reduction of the articular surface.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics and consent statements
This study was conducted in accordance with the declaration of Helsinki and with approval from the Ethics Committee of Jiangxi Provincial People’s Hospital Affiliated to Nanchang University. Written informed consent was obtained from the patient.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
