Abstract
Objective
Baicalin is a compound extracted from the dried root of
Materials and methods
We established a hypertensive pregnant rat model to study vascular endothelial injury during pregnancy-induced hypertension. Plasma epoprostenol (PGI-2), thromboxane A2 (Txa-2), β-human chorionic gonadotropin (β-HCG), and estrogen levels in rats were detected using ELISA. Vascular endothelial growth factor (VEGF), endothelial nitric oxide synthase (eNOS), and C-reactive protein (CRP) expression were detected using western blotting and quantitative PCR (q-PCR).
Results
Results showed that baicalin alleviated symptoms of pregnancy-induced hypertension. CRP, Txa-2, and β-HCG expression were significantly upregulated, while VEGF, eNOS, PGI-2, and estrogen expression was decreased in plasma and placental tissues of hypertensive rats. However, the levels of these injury indicators were significantly decreased after baicalin therapy, while the expression of protective indicators was significantly increased.
Conclusion
Baicalin reversed vascular endothelial cell injury in pregnant hypertensive rats by promoting VEGF, eNOS, PGI-2, and estrogen expression.
Introduction
Pregnancy-induced hypertension is a common disease in pregnant women. The main symptoms of this disease are a persistent increase in blood pressure, proteinuria, and edema after 20 weeks gestation. These symptoms will affect normal fetal development. 1 Pregnancy-induced hypertension is also harmful for the pregnant woman. When gestational-induced hypertension occurs, the permeability of the glomerular filtration barrier is increased and a large amount of albumin is filtered by the glomerulus, which in turn causes edema and severe complications such as metabolic disorders. 2 The liver is the main organ of metabolism. Higher levels of estrogen and progesterone in the serum of pregnant women markedly affect the metabolic process of the liver, which increases synthesis and secretion of enzymes and accelerates metabolism of harmful substances. In patients with pregnancy-induced hypertension, because of hepatic arteriolar vasoconstriction and hepatic ischemic injury, liver metabolism is suppressed, which affects the health of the pregnant woman. 2 Studies have shown that the hypertension will lead to the damage of the vascular endothelium. 3 Vascular endothelial injury accompanied by decreasing nitric oxide (NO) bioavailability could ultimately lead to the development and occurrence of multiple vascular diseases. 4 Elevated blood pressure levels can be treated with many different drugs, but complications such as vascular endothelial damage that is associated with hypertension is difficult to treat and resolve.5,6 Therefore, it is critical to develop a new medicine to treat various types of hypertension including pregnancy-induced hypertension and complications such as vascular endothelial injury.
The
In our research, we established pregnancy-induced hypertension animal models and these rats were treated with baicalin. Blood pressure and urinary protein content were then measured. Plasma and placental vascular endothelial growth factor (VEGF), endothelial nitric oxide synthase (eNOS), and C-reactive protein (CRP) levels in these rats were measured to clarify the efficacy of baicalin on the damage to the vascular endothelium, which is a complication of pregnancy-induced hypertension.
Materials and methods
The experiments in this study were approved by the ethics committee at Shanghai Sixth People’s Hospital.
Establishment of the hypertensive rat model
In this study, we established the hypertensive rat model by intraperitoneal injection of the nitric oxide synthase (NOS) inhibitor N(ω)-nitro-L-arginine methyl ester (L-NAME). Rats were treated using the L-NAME dose that was determined in a previous study. 20 These pregnant rats were intraperitoneally injected with L-NAME from day 11 to day 18 (50 mg/kg, once a day) to establish the hypertension model. The specific pathogen free (SPF) levels in Sprague–Dawley rats (13–14 weeks) were obtained from the Laboratory Animal Center, Shanghai Academy of Chinese Science (Shanghai, China). All rats were divided into six groups (control group, positive group-magnesium sulfate 100 mg/kg, model group, baicalin 50 mg/kg, baicalin 100 mg/kg, and baicalin 150 mg/kg). The pregnant rats in the control group were intraperitoneally injected with normal saline from day 11 to day 18. The model group was injected with the L-NAME once a day (50 mg/kg). The positive group was injected with magnesium sulfate (100 mg/kg), which is an effective drug to induce hypertension in pregnancy.21,22 The baicalin groups were injected with different doses of the baicalin. The blood pressure (systolic blood pressure) in the caudal artery of these pregnant rats was detected on days 8 and 18, respectively. A 24-hour urine sample was collected from these rats to detect changes in the urine protein content. All the pregnant rats were sacrificed after 3 weeks. The placental tissue was then collected and stained using hematoxylin and eosin (HE). HE staining was performed based on the standard procedure (fixation, dehydration, embedding, section, and staining).
Blood pressure and urine protein measurement
A rat sphygmomanometer was used to detect blood pressure in the caudal artery on days 8 and 18 to confirm establishment of the hypertension models. The rats’ tails were initially warmed, and then a fixator was used to limit the rats’ movement. Blood pressure (systolic blood pressure), using the same position on the rats’ tail, was detected using the rat sphygmomanometer (Yuyan Co., Shanghai, China). Urine output from these pregnant rats was collected on days 9 and 19. The urine protein content was examined using the bicinchoninic acid (BCA) (Beyotime, Jiangsu, China) method.
ELISA assay
Plasma epoprostenol (PGI-2; Cayman Chemical Co., Ann Arbor, MI, USA), thromboxane A2 (Txa-2; Cayman Chemical Co.), β-human chorionic gonadotropin (β-HCG; ab53087, Abcam, Cambridge, MA, USA), and estrogen levels were determined using ELISA assays, in accordance with the manufacturer’s protocol. Plasma was collected when the rats were sacrificed. A reagent tube (BD Biosciences, San Jose, CA, USA), which contained an anticoagulant, was used to collect and extract the plasma.
Western blotting
Placental VEGF (ab32152, Abcam), eNOS (ab76198, Abcam), and CRP (ab211631, Abcam) levels were detected using Western blotting. RIPA (Beyotime) was used to extract the proteins from the tissues. The sample concentration was then determined using the BCA method. Loading buffer (Beyotime) was added to the samples and they were incubated at 99°C for 10 minutes. These samples were separated using 10% sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE; Beyotime). Then these proteins were transferred to a polyvinylidene fluoride (PVDF) membrane (Millipore, Billerica, MA, USA), and the membrane was blocked with 5% skimmed milk powder and incubated with the primary antibody at 4°C overnight. The next day, the membrane was washed with the phosphate buffered saline Tween-20 (PBST) three times. The membrane was then incubated with the second antibody at the room temperature for 2 hours, and the membrane was washed with the PBST three times and exposed using a Tanon 4600 (Tanon Co., Shanghai, China).
RT-PCR
Total RNA was extracted from the rat placenta using Trizol (Thermo Fisher Scientific, Rockford, IL, USA) method. The mRNA was then reverse transcribed using a Reverse Transcriptase kit (Takara, Shiga, Japan). PCR was performed using the Applied Biosystems™ 7500 (Thermo Fisher Scientific). The target gene levels were calculated using the 2–ΔΔCT method. Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) was used as a reference gene. The primers used in this research are listed in Table 1.
Primer sequences.

VEGF, vascular endothelial growth factor; eNOS, endothelial nitric oxide synthase; CRP, C-reactive protein; GAPDH, glyceraldehyde 3-phosphate dehydrogenase.
Statistical analysis
Data analysis was performed using GraphPad Prism7 (GraphPad Software Inc., La Jolla, CA, USA). A Student’s
Results
Baicalin reduced the symptoms of pregnancy-induced hypertension
Hypertension during pregnancy is a normal gynecological disease. Previous research has established a rat model of hypertension in pregnancy by adding the L-NAME into the drinking water of pregnant rats to induce the higher blood pressure (systolic blood pressure ≥140 mmHg). 23 We constructed a rat model to study hypertension during pregnancy in this study. Blood pressure was measured to confirm the establishment of the hypertension models and the effect of the baicalin. As shown in Figure 1a and Figure 1b, the blood pressure in the model group was significantly higher compared with the control group (P < 0.05). After 24 hours, the urinary protein content was also increased compared with the control group (P < 0.05). However, after baicalin treatment, the blood pressure of these rats had significantly decreased (P < 0.05) and the urinary protein content was also significantly decreased after 24 hours (P < 0.05) compared with the model group. With an increase in the baicalin dose, the symptoms resolved. The blood pressure and urinary protein content in the positive control group rats, which received magnesium sulfate to induce high blood pressure, was similar compared with the baicalin treated groups.

Hypertensive symptoms in rats were alleviated after baicalin therapy. (a) Rat blood pressure was measured using a rat blood pressure meter. (b) The urine protein content was detected using commercial kits. *p<0.05, **p<0.01, ***p<0.001.
Baicalin alleviated placental injury
HE staining was performed to observe the pathological changes in the placenta. The main cells of placental villus in the control group were syncytiotrophoblasts, and there were fewer cytotrophoblasts in the placental villus compared with the control group (Figure 2). Compared with the control group, the number of placental villi decreased and the structure of the placental villi shrank, part of the villus showed fibrinoid necrosis, and the trophoblast cells showed compensatory proliferation in the model group. However, after baicalin treatment, the placental villous fibrosis and the syncytiotrophoblast nodules were reduced. The status of the HE staining in the positive group was similar to that of the control group. Therefore, baicalin treatment reduced the formation of nodules and lesions that were induced by hypertension during pregnancy in the placenta.

Treatment with baicalin reversed placental damage. Representative photographs of HE stained placenta. These images showed that baicalin therapy reversed the formation of nodules and lesions.
Baicalin reduced vascular endothelial cell damage during the progression of pregnancy-induced hypertension
To further explore the effect of the baicalin, we determined the PGI-2 and Txa-2 levels in the plasma (Figure 3a). The PGI-2 levels in the model group were decreased (P < 0.05), while Txa-2 levels were increased (P < 0.05) compared with the control group. After treatment with baicalin, Txa-2 levels remained decreased and PGI-2 levels remained increased. The Txa-2 levels decreased and PGI-2 levels increased with an increasing of dose of baicalin. Additionally, β-HCG and estrogen levels in the plasma were detected. The results (Figure 3a) showed that compared with the control group, β-HCG levels were increased (P < 0.05), but estrogen levels were decreased (P < 0.05) in the model group. In the baicalin-treated group, β-HCG expression was suppressed (P < 0.001) and the estrogen level was gradually increased (P < 0.01) compared with the model group. Similarly, the degree of the change in these proteins increased with an increasing dose of baicalin.
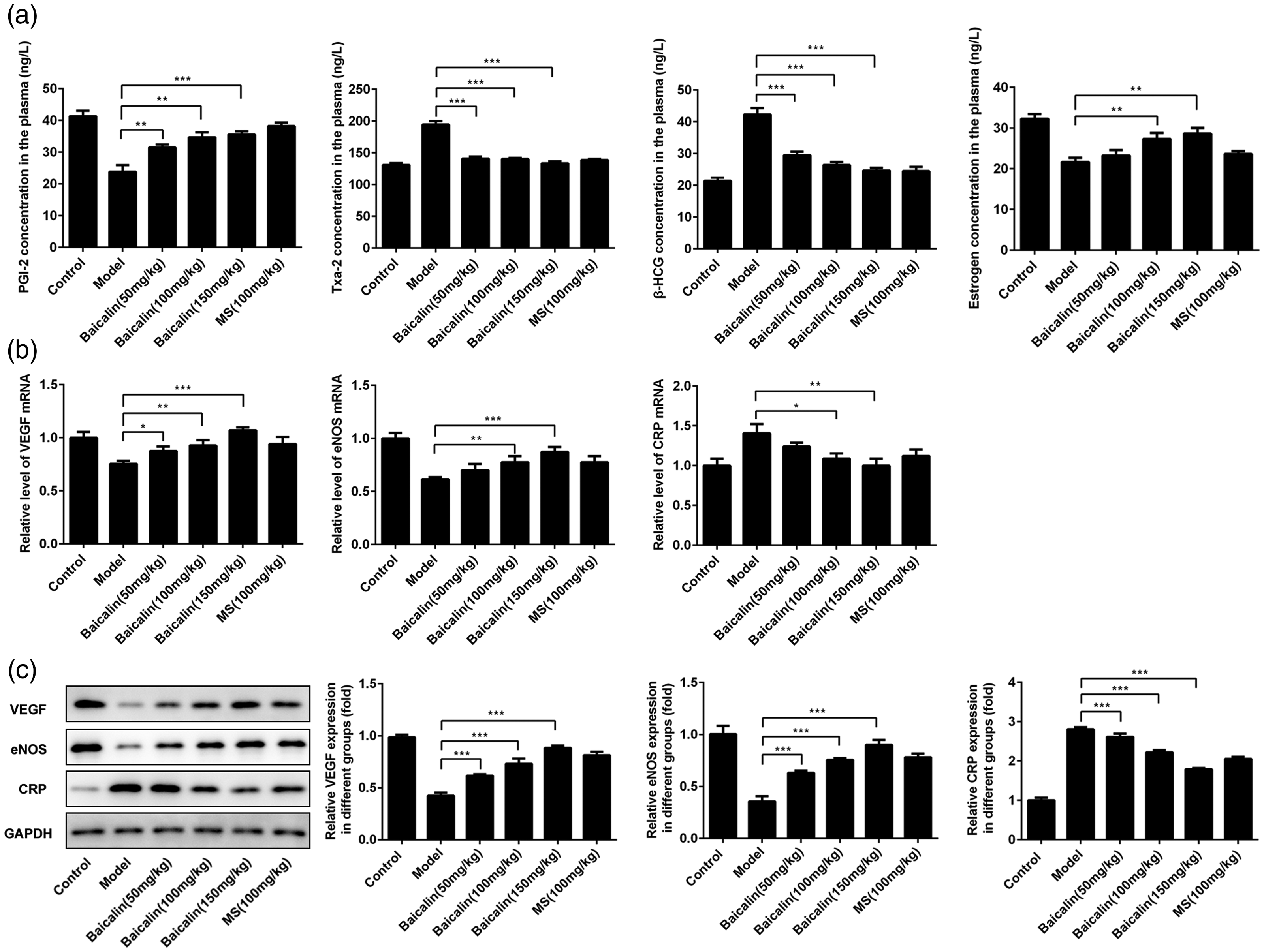
Treatment with baicalin reduced vascular endothelial cell damage. (a) PGI-2, Txa-2, β-HCG, and estrogen levels in plasma were determined using ELISA. (b) VEGF, eNOS, and CRP mRNA levels were detected using q-PCR. (c) VEGF, eNOS, and CRP protein levels were determined using western blotting. Quantitative protein expression data were also displayed in this figure.
VEGF plays a crucial role in the health of endothelial blood vessels, and eNOS is also critical for the health of the vascular endothelium. Therefore, VEGF and eNOS expression in placental tissues of these rats were detected using the qPCR and western blotting. The results show that the VEGF and eNOS expression was suppressed after the construction of the model compared with the control group (P < 0.05 for both). However, with the increase in the baicalin dose, eNOS and VEGF levels gradually increased (P < 0.01 for all) (Figure 3b and Figure 3c). In addition, the CRP is a widely studied marker of inflammation, and it has often been used to predict the risk of cardiovascular disease.24,25 In our research, we showed that the CRP levels in the placental tissues of these rats were increased in the model group compared with the control group (P < 0.05), and the CRP levels were decreased after treatment with baicalin compared with the model group (P < 0.05 for all) (Figure 3b and Figure 3c).
Discussion
Pregnancy-induced hypertension is a common disease during the gestational period. It includes preeclampsia, eclampsia, and gestational hypertension, and it is also an important cause of maternal death worldwide. 26 The development of pregnancy-induced hypertension is also accompanied by proteinuria, edema, and vascular endothelial injury. Vascular endothelial injury and dysfunction are primary complications in multiple types of hypertension including the pregnancy-induced hypertension. 3 Research has indicated that pregnancy-induced hypertension patients often have a decrease in circulating endothelial cells and circulating endothelial progenitor cells. 27
VEGF is a protein that causes angiogenesis and maintains vascular endothelial cell health. 28 Upregulation of VEGF could protect the HUVECs from apoptosis. 29 CRP is an indicator of inflammation and damage to the vascular endothelium. 30 Higher CRP levels increase the risk of hypertension and cerebrovascular disease. 31 In this study, we found that VEGF and eNOS expression in plasma and placental tissues from pregnancy-induced hypertension rats were lower, but CRP levels were higher compared with the control group. Therefore, our results indicated that pregnancy-induced hypertension is associated with vascular endothelial injury. Additionally, Txa-2 and PGI-2 play an important role in the blood. PGI-2 is a powerful anticoagulant that could inhibit the development of atherosclerosis.32,33 A study also showed that Txa-2 could prevent blood vessel formation. 34 We observed that PGI-2 expression decreased while Txa-2 levels increased in the model group compared with the control group. These experimental results further demonstrated that pregnancy-induced hypertension could lead to vascular endothelial injury and dysfunction.
The baicalin is a component that is extracted from
Overall, these results demonstrated the protective efficacy of baicalin against vascular endothelial and placental injury. The results suggest the value of baicalin for treating vascular endothelial injury during pregnancy-induced hypertension. Our research also provides a traditional Chinese medicine-based approach for the clinical treatment of pregnancy-induced hypertension.
Supplemental Material
sj-pdf-1-imr-10.1177_0300060520934288 - Supplemental material for Effect of baicalin on gestational hypertension-induced vascular endothelial cell damage
Supplemental material, sj-pdf-1-imr-10.1177_0300060520934288 for Effect of baicalin on gestational hypertension-induced vascular endothelial cell damage by Yang Liu, Miao Xiong, Fangfang Zhou, Nana Shi and Yunbin Jia in Journal of International Medical Research
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
