Abstract
Liver transplantation is suitable for acute and chronic liver diseases that cannot be cured by other methods. Immunosuppressants such as azathioprine, methylprednisolone, cyclophosphamide, cyclosporine A, and tacrolimus have been applied to prevent rejection after liver transplantation. Among them, tacrolimus is generally effective in resisting rejection, and its main adverse reaction is nephrotoxicity. Tacrolimus-induced seizures are rarely reported. The present report describes trismus, restlessness, and generalized muscle twitching in a 44-year-old man and a 59-year-old man who received tacrolimus after liver transplantation. Tacrolimus-induced epilepsy was diagnosed by clinical symptoms and video-electroencephalography. After the patients developed epileptic symptoms, they received intramuscular injections of diazepam and phenobarbital. When the symptoms were relieved, the patients were treated with oral levetiracetam tablets. The tacrolimus was immediately stopped, and the epilepsy symptoms gradually disappeared after treatment with sedatives and levetiracetam. The patients continued taking the levetiracetam for approximately 2 weeks. No evidence of seizures occurred during the next 8 months. Although tacrolimus is reportedly effective against rejection after liver transplantation, tacrolimus-induced epilepsy should be carefully managed to prevent death. Additionally, epilepsy may rarely occur in patients with a normal blood concentration of tacrolimus. Further study on the mechanism of such neurological complications is needed.
Abbreviations
CT = computed tomography; MRI = magnetic resonance imaging; EEG = electroencephalography
Introduction
Liver transplantation involves implantation of a healthy liver into a patient with end-stage liver disease to restore good liver function. 1 Tacrolimus, also known as FK506, is a fermentation product of Streptomyces tsukubaensis. Tacrolimus is a powerful new immunosuppressant that is mainly used to inhibit the release of interleukin-2. In recent years, it has been viewed as a first-line drug for liver and kidney transplantation. In particular, it exhibits a good anti-rejection effect after liver transplantation. Tacrolimus is a macrolide antibiotic that has been shown to be safe and effective for patients who have undergone liver transplantation. 2 In clinical practice, common adverse events related to tacrolimus include kidney injury, gastrointestinal disorders, and heart and endocrine abnormalities. 3 The mechanism of tacrolimus-induced epilepsy remains unknown, and literature on this topic is scarce. The present report describes two patients with epilepsy triggered by tacrolimus who were treated with a combination of diazepam and levetiracetam. 4
Case reports
Case 1
A 44-year-old man presented with a 6-month history of gingival bleeding with no obvious cause. The bleeding became obvious after eating and brushing, and it could not be stopped easily. The bleeding improved after a platelet transfusion at a local hospital, and the hospital recommended continuing treatment at a higher-level hospital. Because the patient was on a high-protein diet after two hepatic comas, he went to Beijing People’s Liberation Army 302 Hospital for a computed tomography (CT) scan and was diagnosed with decompensated cirrhosis. He was then transferred to the Affiliated Hospital of Tsinghua University for liver transplantation. After completion of a preoperative examination, the patient underwent a liver transplantation. Tacrolimus (2 mg every 12 hours) was given as anti-rejection therapy for 3 days postoperatively. The patient’s blood concentration of tacrolimus was 3.94 ng/mL, which was maintained within the reference range for postoperative treatment. One week later, the patient suddenly developed convulsions accompanied by eye twitching, restlessness, and sudden weakening of the muscles on the left side of the body, including positive facial and Babinski reactions. He had no history of epilepsy. Electroencephalography (EEG) examination revealed the following three abnormalities (Figure 1): (1) synchronous or asynchronous bilateral frontal, temporal, and frontal midline irregular slow-wave bursts of 3 Hz (bilateral symmetry); (2) occasional localized single spike bursts in the right occiput; and (3) occasional single spike bursts in the right frontal posterior and frontal midline. An intramuscular injection of diazepam (0.5 mg) was immediately administered, indicating mild demyelination of the white matter on cranial magnetic resonance imaging (MRI) (Figure 2). The patient’s symptoms were relieved after beginning oral treatment with levomethylacetanilide tablets (0.5 mg). Two days later, no abnormalities were observed on brain MRI (Figure 3). Oral administration of tacrolimus at 1.5 mg every 12 hours was continued for about 2 weeks, and the plasma concentration of tacrolimus was 7.55 ng/mL on reexamination. The adverse events were believed to be related to the tacrolimus and were relieved after symptomatic treatment. Finally, his left muscle strength returned to normal and he had no seizures for several months.

Synchronous or asynchronous bilateral frontal, temporal, and frontal midline, irregular, slow-wave bursts of 3 Hz (bilateral symmetry).

Cranial magnetic resonance imaging with mild demyelination of white matter and a right frontal sinus submucosal cyst.
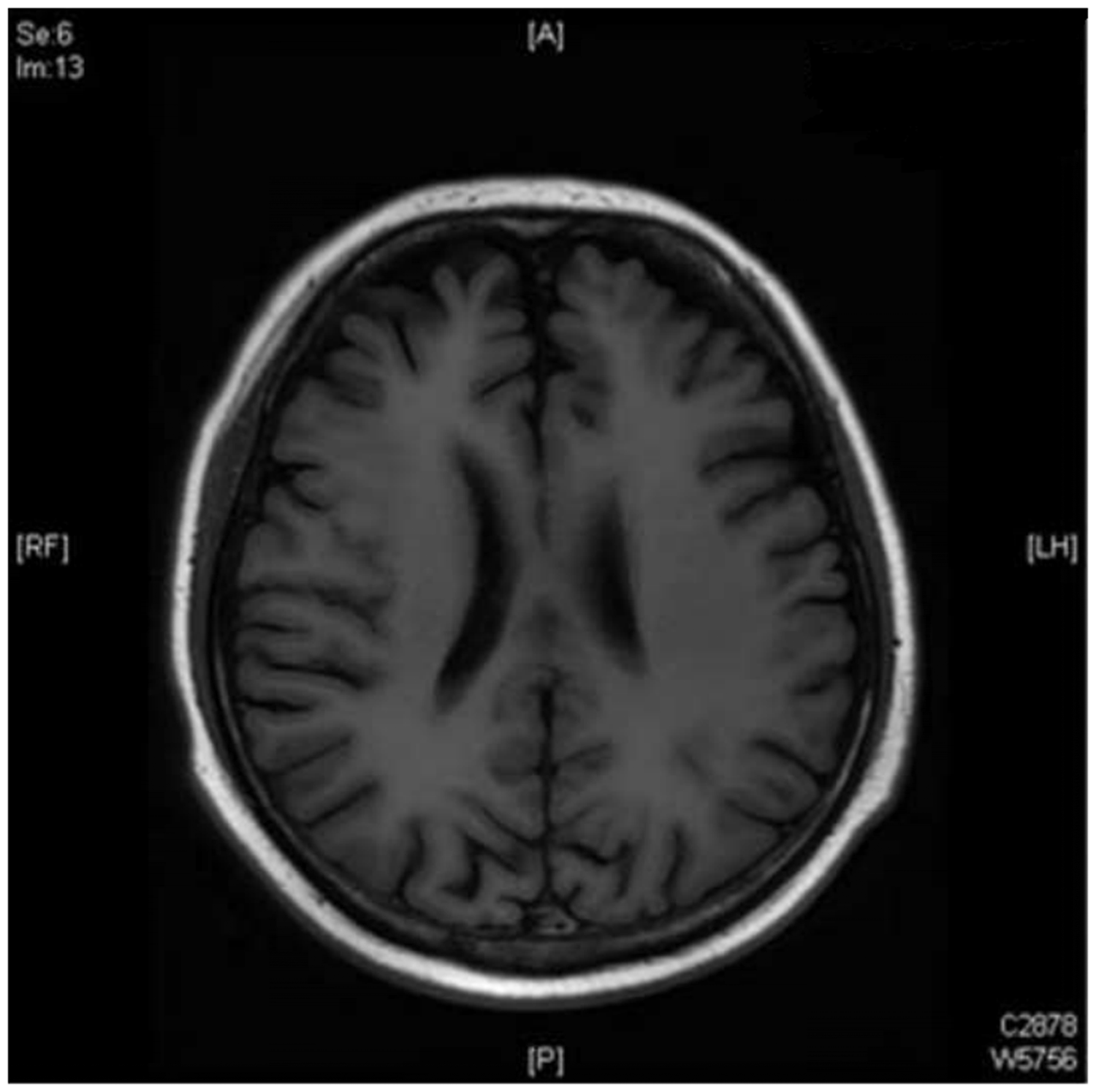
No obvious abnormalities were found on brain magnetic resonance imaging reexamination.
Case 2
A 59-year-old man was found to have liver cirrhosis with multiple nodules in the liver during a physical examination at the Fourth People’s Hospital of Lianyungang City. He had no other symptoms. CT examination of the liver showed a high possibility of small liver cancer in the right lobe of the liver, cirrhosis of the liver, and multiple cirrhotic nodules in the liver. For further treatment, he went to the Affiliated Hospital of Tsinghua University, where he underwent a liver transplantation and received oral anti-rejection treatment with tacrolimus (1.5 mg every 12 hours) on the first day after surgery. His blood concentration of tacrolimus was 1.9 ng/mL, which was within the reference range for postoperative treatment. On the fourth day after starting the tacrolimus, the patient suddenly shouted loudly at noon. He immediately closed his teeth, and his upper and lower limbs bent and convulsed. EEG examination revealed abnormalities (Figure 4) in the form of a bilateral explosive high-amplitude spinous wave rhythm that quickly converted to high-amplitude three-times/second synthesis of multi-spinous slow waves, with a total duration of 2 to 3 seconds. The patient’s symptoms were relieved after intravenous diazepam and intramuscular phenobarbital injections. Emergency brain CT showed posterior edematous change as indicated by disappearance of the sulcus (Figure 5), and his symptoms were relieved after the second intravenous injection of diazepam. Meanwhile, he began oral administration of levomethylacetanilide tablets. Arterial blood analysis revealed no other abnormalities. On day 2, CT re-examination exhibited no shadows of abnormal density in the brain parenchyma. Oral administration of tacrolimus (1.5 mg every 12 hours) was continued for about 2 weeks, and the plasma concentration was 8.81 ng/mL on re-examination. The patient had developed no recurrence of epilepsy after 8 months of follow-up.

Bilateral explosive high-amplitude spinous wave rhythm quickly converted to high-amplitude three-time/second synthesis of multi-spinous slow waves for a total duration of 2 to 3 seconds.

Brain computed tomography shows posterior edematous change as indicated by disappearance of the sulcus.
Discussion
Studies have indicated that tacrolimus binds to an immunoavidin-FK506 binding protein (FKBP) after entering T cells in vivo. The FKBP-FK506 complex inhibits calcineurin activity, blocks the dephosphorylation of activated T nuclear transcription factor, and then inhibits the gene transcription of interleukin-2, thereby inhibiting the subsequent activation of T cells. 5 Sakamoto et al. 6 studied the relationship between the tacrolimus concentration and cerebral neurotoxicity. The results illustrated that various doses of tacrolimus significantly affected the incidence of neurotoxicity in rats. The neurotoxicity was more severe in the high- than low-dose group. The researchers reported a 16.9% incidence of neurological complications after liver transplantation, with insomnia, headache, and tremor being the most common complications. Seizures were only seen in individual patients. They suggested that neurotoxicity may be related to the blood drug concentration. However, Saner et al. 7 reported that the incidence of neurological complications was as high as 43% and concluded that there was no definite relationship between the occurrence of neurological symptoms after liver transplantation and the primary disease or the concentration of immunosuppressive drugs. No studies have shown that tacrolimus neurotoxicity is related to the plasma concentration, dose, or other factors. The two patients described in the present report developed seizures after administration of tacrolimus, and this adverse effect should therefore be considered in individual patients. However, the tacrolimus dose was low and the plasma concentration was within the therapeutic range during the seizures. Although the dose of tacrolimus was reduced after about 2 weeks of drug withdrawal, the plasma concentration was higher than that during the seizures (no recurrence); this suggests that the seizures were not related to the plasma concentration of tacrolimus. Studies have confirmed that the distributions of tacrolimus-binding protein, calmodulin, and cyclophilic protein are consistent in most brain tissues. 8 Therefore, the neurotoxicity may be the outcome of further inhibition of calmodulin.
Pharmacologically, diazepam selectively acts on the limbic system of the brain, binds to the central bromodomain 2 receptor, and promotes γ-aminobutyric acid release or synaptic transmission. 9 Compared with diazepam, phenobarbital has basically the same pharmacological effect; however, barbiturates are more prone to inducing dependence. 10 According to the international guidelines for the diagnosis and treatment of epilepsy, the exact mechanism of the antiepileptic effect of levetiracetam tablets remains unclear, and such treatment is only given as intensified medication for epilepsy.
For epileptic seizures, MRI provides higher image resolution than CT; therefore, clearer brain imaging can be obtained. MRI more clearly reflects the abnormal areas of the brain that may lead to epilepsy. Brain MRI can also exclude brain structural abnormalities that may lead to epilepsy. CT scan results cannot be used to directly diagnose epilepsy; instead, CT mainly demonstrates lesions in the brain, such as scars or damaged areas, that may lead to epilepsy. Cranial CT is not a necessary examination for epilepsy after liver transplantation. CT may be considered when MRI is not available or in some special cases. Changes consistent with the convulsive type of hand-foot syndrome on cranial CT are rare and may be related to inadequate resolution of soft tissue on CT. No obvious abnormalities were found on head CT and MRI of the two patients described in this article, proving that the patients’ epilepsy had not been triggered by a primary lesion in the head and providing diagnostic significance for epilepsy induced by tacrolimus. The two patients developed no fever, fatigue, or liver dysfunction after liver transplantation; they rapidly responded to tacrolimus and maintained a normal blood concentration. However, the two patients’ neurotoxicity was almost identical. According to the epileptic seizure and epilepsy classification introduced by the International League Against Epilepsy in 2017, both patients had comprehensive spasms. 11 They took no prescription drugs other than tacrolimus. Additionally, they had no history of epilepsy or neurological disorders. Therefore, the seizures must have been triggered by tacrolimus. With respect to drug-induced epilepsy, several randomized clinical trials have shown that diazepam or phenobarbital treatment effectively induces a sedative and hypnotic effect. 12 Epilepsy is a neurological symptom regardless of the cause. Thus, after our patients’ symptoms were relieved, we administered oral levomethylacetanilide tables for 2 days to strengthen the effect of the medication and prevent another attack.
Finally, we reviewed the neurological complications of adult liver transplantations 1 year later in our hospital. Of 80 patients, 20 (25%) developed complications. Two patients (2.5%) developed early complications in the form of seizures. The most common neurological complications triggered by drugs after liver transplantation are encephalopathy (47.6%), followed by epilepsy (9.5%). The occurrence of neurological complications did not affect the clinical efficacy because most survivors nearly completely recovered. 13
Footnotes
Acknowledgements
The authors thank Professor Haining Fan (from the Affiliated Hospital of Qinghai University, Xining, China) for reviewing the manuscript and improving the language quality. The authors also thank the two patients and their families.
Author contributions
YL, LZ, and ZW were responsible for the data collection and assembly. HW, DH, SY, HW, and HF performed the data analysis and literature search. All authors contributed to the data analysis and the drafting and revising of the paper. All authors agree to be accountable for all aspects of the work.
Consent for publication
Both patients provided informed consent and agreed to publication of their case reports.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics approval
This study was approved by the Scientific Research Ethics Committee of the Affiliated Hospital of Qinghai University.
Funding
This research was supported by grants from Science and Technology Major Project of Qinghai Province (No. 2016-SF-A5).
