Abstract
Objective
To identify whether the medial or lateral approach is superior for patients with valgus knees undergoing primary total knee arthroplasty (TKA).
Methods
Studies evaluating the 2 approaches were sourced from the PUBMED, EMBASE, Web of Science, and OVID databases. The quality of included studies was assessed using a modified quality evaluation method, and differences between approaches were systematically reviewed.
Results
Seventeen observational studies were included. The studies were published between 1991 and 2016, and included 5 retrospective studies and 12 prospective studies. Sixteen evaluation methods for the study outcomes were identified. Twelve and eight complication types were identified by studies reporting the lateral and medial approaches for valgus knee, respectively. Several studies showed that pain scores and knee function were superior using a lateral approach.
Conclusion
The lateral approach (combined with a tibial tubercle osteotomy or proximal quadriceps snip) was more useful and safer than the medial approach in the treatment of severe uncorrectable valgus knee deformity in patients undergoing TKA. Most of the available evidence supports the use of a lateral approach provided that the surgeon is familiar with the pathological anatomy of the valgus knee.
Introduction
The prevalence of the valgus-aligned knee when the valgus deformity is greater than 10 degrees reaches 15%.1,2 Although not as common as the varus knee, the valgus knee introduces a greater challenge in maintaining soft tissue balance when performing total knee arthroplasty (TKA). Ranawat et al. 3 described 3 degrees of valgus deformity: Grade I accounts for 80% of all valgus deformities and has an axis of less than 10°; Grade II accounts for 15% of valgus deformities, where the axis ranges between 10° and 20°; Grade III is found in the remaining 5% of valgus deformities, with an axis of more than 20°. Krackow et al. 4 reported 3 types of valgus deformity: Type I is characterized by a valgus deformity secondary to bone loss, with soft tissue contracture in the lateral compartment while the medial soft tissues remain intact; Type II is characterized by a distinct attenuation of the medial ligament and capsular complex; Type III is characterized by serious valgus deformity with valgus malpositioning of the joint line after overcorrected proximal tibial osteotomy. The valgus knee is characterized by a contracted iliotibial band (ITB), posterolateral capsule, posterior cruciate ligament (PCL), and lateral collateral ligament (LCL), as well as osseous deficiency of the posterior lateral femoral condyle and medial collateral ligament (MCL) laxity. 5 Because of these complex anatomies, the treatment options for valgus knee are more limited compared with the varus knee and present greater challenges.
Different surgical techniques have been performed to balance the soft tissues in knees with valgus deformity during TKA, and a number of options exist for prosthesis selection. The treatments for valgus knee with moderate to severe ligament laxity include constrained or unconstrained implants, which remains an area of controversy.6,7 In terms of surgical techniques, the lateral approach has been advocated as an alternative to the medial approach for knees with valgus deformity undergoing TKA, since the lateral approach facilitates the release of tight lateral structures. 8 Keblish 9 and Buechel 10 were the first to recommend a lateral parapatellar approach for TKA in the valgus knee. The lateral approach was associated with better clinical performance and anatomical axis correction. 9 Stern et al. 11 have also reported disappointing results with the medial capsular approach for valgus knees. Because of the paucity of studies in the literature comparing the medial and lateral approaches, there is no consensus regarding which of the two approaches is superior for primary TKA in the valgus knee. This study systematically reviews the available evidence in the literature on this topic to make a recommendation on whether the medial or lateral approach should be preferentially used.
Materials and Methods
Search strategy
The methods used in this systematic review were derived from the Centre for Reviews and Dissemination guidance,12,13 according to the preferred reporting items for meta-analyses and systematic reviews. 14 The studies were sourced from the Web of Science, PUBMED, EMBASE, and OVID. The publication date range was set to February 2019 with no lower date limit. Keywords for performing the search included: “valgus knee,” “lateral approach,” “medial approach,” and “total knee arthroplasty”. Manual searches were performed for relevant references listed in the included studies. In addition, all databases from relevant conferences that provided gray literature were searched. The search strategy for PUBMED was: #1 – valgus knee, #2 – lateral approach, #3 – medial approach, #4 – total knee arthroplasty, #5 – #1 AND #2 AND #3 AND #4.
Inclusion and exclusion criteria
Inclusion criteria were: 1) Observational studies (including case-control and cohort studies); 2) studies containing a clearly defined group of valgus knee patients undergoing TKA using a lateral or medial approach; 3) studies comparing different approaches in TKA for treating valgus knees. Exclusion criteria were: 1) unicompartmental knee arthroplasty (UKA); 2) conversion from UKA to TKA; 3) high tibial or femoral osteotomy. Biomechanical studies, case reports, and reviews were also excluded.
Study selection
The literature search and study selection were performed by two reviewers. The title and abstract of the studies were independently analyzed by the two reviewers based on the inclusion and exclusion criteria. If a study could not be excluded based on the title and abstract, both reviewers reviewed the full text to reach a consensus on the inclusion or exclusion of the study.
Data extraction
The following data were extracted by two independent reviewers from all included studies: author(s), year of publication, sample size, study design, surgical approach, follow-up period, complications, major findings.
Quality assessment
The methodological quality of included studies was evaluated according to the Newcastle–Ottawa scale. The criteria used for methodological assessment 15 have previously been applied in systematic reviews of observational studies. 13 Reporting was conducted in accordance with PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) Guidelines.
Statistical analysis
The results were summarized, analyzed, and sorted using Microsoft Excel 2011 (Microsoft, Redmond, Washington, USA). The quality and risk of bias of this systematic review were evaluated using AMSTAR instrument (A MeaSurement Tool to Assess systematic Reviews) and ROBIS tool (Risk Of Bias In Systematic reviews).
Results
Identification of relevant studies
Nine potential citations were removed after checking for duplications. Thirty publications were identified after screening the titles and abstracts. Seventeen studies were selected for final analysis after reading the full text for each study (Figure 1). Two classification systems were identified that describe the degree of valgus knee (Figure 2).

Flow of studies through the systematic review.
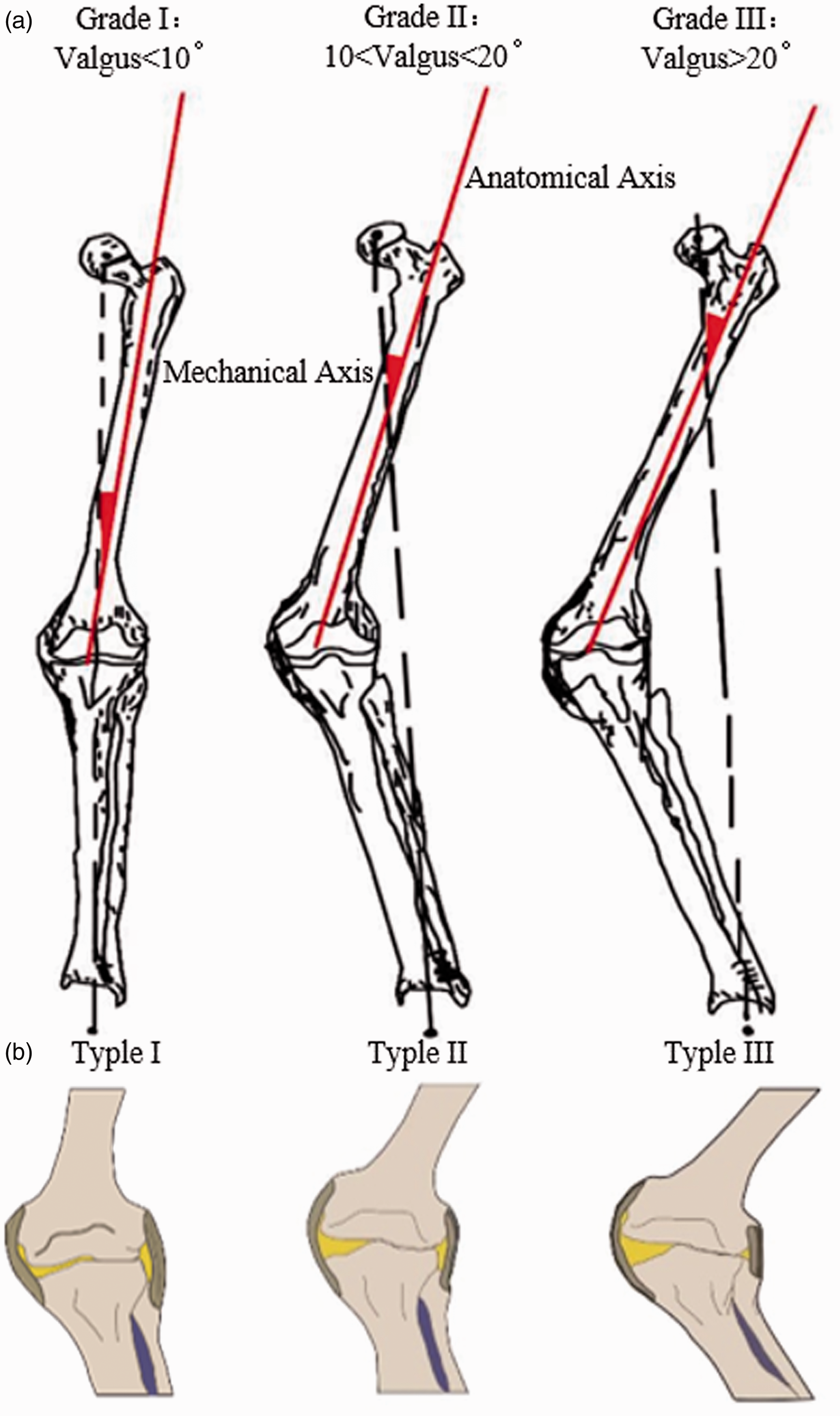
Schematic illustration of 2 common forms of valgus deformity. (a) Ranawat’s type, the mechanical and anatomical axis of the knee with valgus deformity grade I, II, and III. (b) Krackow’s type, the bone loss and soft tissue around the knee with valgus deformity type I, II, and III.
Study characteristics
The characteristics of the included studies are presented in Table 1 and 2. The 17 included studies were published between 1991 and 2016, and included 5 retrospective studies and 12 prospective studies. Sample size ranged from 8 to 164 patients. However, the mean duration of follow-up was not calculated, and the reported follow-up ranged from 3 to 180 months.
The characteristics of included articles that reported one surgical type.

TKA: total knee arthroplasty; TTO: tibial tubercle osteotomy; IKSS: International Knee Society Score; ROM: range of motion; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index; NJOHS: New Jersey Orthopaedic Hospital scoring scale; VAS: Visual Analog Scale; DVT: deep venous thrombosis.
The characteristics of included articles that reported different surgical types.

TKA: total knee arthroplasty; TTO: tibial tubercle osteotomy; IKSS: International Knee Society Score; ROM: range of motion; WOMAC: Western Ontario and McMaster Universities Osteoarthritis Index; VAS: Visual Analog Scale; DVT: deep venous thrombosis; MIS: minimally invasive surgery; CAS-TKA: computer-assisted total knee arthroplasty; PE: pulmonary embolism.
Methods evaluating pain and knee function
Sixteen evaluation methods were identified by the included studies to evaluate pain and knee function following TKA in the valgus knee, as shown in Table 1 and 2. These methods included: Visual Analog Scale (VAS) pain score, free walking distance, Knee Society Score (KSS), KSS functional score, Hospital for Special Surgery (HSS) score, International Knee Society Score (IKSS), IKSS functional score, maximum flexion, postoperative range of motion (ROM), Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), Kujala score, leg alignment, patellar height, New Jersey Orthopaedic Hospital Scoring (NJOHS), VF-12, and the University of California Los Angeles (UCLA) score.
Complications using the lateral or medial approach
Twelve potential types of complications were identified by the studies reporting on the lateral approach for valgus knee, including: proximal migration of the osteotomized tibial tubercle, deep venous thrombosis, hematoma, bruise, skin blister/necrosis, temporary nerve paralysis, infection, fracture, pulmonary embolism, wound dehiscence, tibial tubercle displacement, and irritation issue. Eight potential types of complications were reported for the medial approach, including: wound infection, progression of patellofemoral osteoarthritis, deep vein thrombosis, anterior notching of the femur, hematoma, bruise, skin blister/necrosis, and fracture. These complications are shown Table 1 and 2. The revision rate with the lateral approach (4%) was higher than with the medial approach (1.5%). 16 However, no difference was reported in most of the studies.17,18
Comparisons between the lateral and medial approaches
Mean preoperative valgus angle, mean postoperative valgus angle, complications, and outcome measures were used to compare the lateral and medical approaches for TKA in the valgus knee, as shown in Table 2. Both lateral and medial approaches resulted in significant changes in mean postoperative valgus angle compared with the mean preoperative values. Some studies showed no significant differences in outcome measures between the two approaches,17,19–22 while other studies showed superior VAS score, KSS score, postoperative ROM, and knee flexion in groups using a lateral approach.16,18
Discussion
Despite the difficulty of conducting a meta-analysis on the topic of this study due to the heterogeneity of the selected articles, the available evidence suggested that a lateral approach was a better choice for TKA in knees with valgus deformity compared with a medial approach, despite the requirement for a longer learning curve. Keblish 9 was the first one to address the pathological anatomy in valgus deformity, proposing that the medial approach was indirect, pushing the contracted posterolateral corner away from the operative field. “Extensive” lateral release was mandatory for obtaining adequate patellar tracking, vascularity was compromised, and a lateral soft-tissue gap was frequently uncovered. Such extensive soft tissue dissection might devitalize the patella and cause considerable hemorrhage and edema. This might provide an explanation for why the results of valgus knee replacement seemed to be more disappointing when a medial approach was used. 2 Therefore, a lateral approach might be favored in correcting the moderate to severe valgus knee for several reasons:1,17,18,23 1) It is necessary in valgus knees to perform a lateral release, particularly for patients who have already undergone medial arthrotomy, to maintain the patella’s blood supply; 2) the lateral approach can facilitate the release of the lateral contracted element for a better view; 3) the lateral approach combined with tibial tubercle osteotomy (TTO) can improve patellar tracking. Burki et al. 24 reported good results in 88% of patients who underwent a combination of lateral approach and TTO. However, soft tissue closure on the lateral side may be difficult; a Hoffa fat pad flap is usually necessary and may even be insufficient. 25 Koninckx et al. 26 found that TKA for a fixed valgus knee could be easily performed through a minimally invasive far medial subvastus approach, leading to a rapid functional recovery. The far medial subvastus approach was used for Type I or II valgus deformities, and allows leaving the MCL attached to not further destabilize the valgus knee during the medial approach. This allows faster quadriceps recovery in the early postoperative phase, with quick ambulation and rapid ability to straight leg raise and negotiate stairs, which can lead to a shorter length of stay and without malalignment or complications. 27
The lateral structures that may need to be released include the LCL, iliotibial band, posterolateral capsule, lateral head of the gastrocnemius muscle, and popliteus tendon. However, there is no consensus regarding which lateral structures should be released, and the most suitable valgus degree for different approaches. Gunst et al. 17 found that both medial and lateral approaches resulted in good outcomes in knees with mild valgus (mean 6°) following TKA. However, Sekiya et al. 18 found that patients with severe preoperative valgus deformity (mean 13.7°) were more suited for a lateral approach, and TKA using a lateral approach without TTO could provide improved postoperative ROM compared with a medial approach. For patients with a larger valgus deformity, the lateral approach could be more efficient in restoring alignment and improving patellar tracking.1,20 Hendel et al. 28 found that a modified lateral approach combined with medial quadriceps snip was easier and safer to perform than TTO, as described by Keblish and colleagues. 9 Zhou et al. 29 found that a lateral approach combined with Z-plasty of the capsule was an effective surgical technique. This was corroborated by Satish et al., 30 who found that a modified lateral approach with Z-plasty of the lateral retinaculum capsule complex and quadriceps snip without TTO provided good functional results. Chalidis et al. 31 found that a lateral approach combined with TTO was an effective technique for addressing non-correctable valgus deformity during TKA. Filho et al. 21 found that a lateral approach provided better patellar tilt following TKA in valgus osteoarthritic knees. Finally, Niki et al. 19 found that lateral minimally invasive TKA might offer a useful technical option that can be utilized for most patients with valgus deformity.
Favorito et al. 32 reported that the complications in patients with valgus deformities undergoing TKA can include recurrent valgus deformity (4%–38%), tibiofemoral instability (2%–70%), wound problems (4%–13%), postoperative motion deficits requiring manipulation (1%–20%), patellar tracking problems (2%–10%), patellar stress fracture or osteonecrosis (1%–12%), and peroneal nerve palsy (1%–4%). It is certain that TTO migration leading to a need for refixation was one of the reasons for revision with the lateral approach; the rate of TTO proximal migration was 4% with the lateral approach compared with 0% with the medial approach. 20 Surgeons unfamiliar with the lateral approach might consider it technically more difficult than the medial approach. On this note, Kornilove et al. 22 suggested that with the help of computer-assisted TKA, both medial and lateral approaches might be equally effective in achieving proper balance and good alignment in patients with valgus deformity. Huang 33 and Chou 34 discussed the use of computer-assisted technique in arthritic valgus knees, which provides radiographic benefit but no significant benefit in short-term clinical functional outcomes when performed by an experienced surgeon.
For common TKA not involving a valgus deformity, Hay et al. 35 and Nikolopoulos et al. 20 identified no differences in outcomes between the medial and lateral groups at 2 years after surgery. They concluded that the lateral approach with TTO was a safe technique with comparable outcomes to the medial approach for TKA. The lateral approach was considered especially suitable for patients with a history of valgus deformity or patellar instability if patella baja was present preoperatively or after closing-wedge high tibial osteotomy or for TKA revision.
Besides the surgical approach, there are many other factors that need to be considered when performing TKA, such as component selection, femoral anatomy, anterior-posterior axis for femoral component placement, and recognizing the soft-tissue asymmetry. Some prefer a posterior-stabilized (PS) insert in the valgus knee: first, the use of PS TKA for the valgus knee can make the surgery more productive because it is easier to balance the valgus deformity if the PCL is released; second, cruciate-retaining (CR) knees require joint line restoration, which is impossible in a valgus knee after a lateral release.5,26 The PS design is more stable than a CR design because the post-cam mechanism allows for greater lateralization of the tibial and femoral components. 8 Consequently, the surgeon must confidently achieve soft-tissue balancing, resulting in better load distribution and enhancing longevity and component stability. 32 Valgus knees operated on using a medial access route tend to require implants with greater constriction, 23 but authors from this article used different implants as well as different approaches, so direct comparison may not be possible.
There were some limitations in this study. First, different types of studies were included, including prospective and retrospective studies and randomized controlled trials, which could not be merged using the meta-analysis. Second, the number of studies reporting operations on valgus knees using a lateral approach was limited, suggesting that this was not a popular approach among surgeons. Third, the studies included in this review contained highly heterogeneous data reflecting different surgical techniques, outcome measures, and methods of reporting the results. A systematic review was the only means by which the results of these studies could be meaningfully analyzed.
Conclusion
The lateral approach (combined with a TTO or proximal quadriceps snip) was more useful and safer than the medial approach in the treatment of severe uncorrectable valgus knee deformity in patients undergoing TKA. The available evidence supports the use of a lateral approach provided that the surgeon is familiar with the pathological anatomy of the valgus knee.
List of abbreviations
total knee arthroplasty (TKA)
iliotibial band (ITB)
posterior cruciate ligament (PCL)
lateral collateral ligament (LCL)
unicompartmental knee arthroplasty (UKA)
Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA)
Visual Analog Scale (VAS)
Knee Society Score (KSS)
Hospital for Special Surgery (HSS)
International Knee Society Score (IKSS)
range of motion (ROM)
Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC)
New Jersey Orthopaedic Hospital Scoring (NJOHS)
University of California Los Angeles (UCLA)
tibial tubercle osteotomy (TTO)
posterior-stabilized (PS)
cruciate-retaining (CR)
Footnotes
Authors’ contributions
BW and DX designed the work and drafted the manuscript. YYZ and JJL participated in the collection of data. SJD and BZ performed the statistical analysis. All authors read and approved the final manuscript.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Ethics approval and consent to participate
Our database was password-protected, the study was approved by the Ethics Committee of our University, and all participants provided written informed consent.
Funding
This study was supported by National Natural Science Foundation of China (Grant No.81802204, 81973606), Second Hospital of Shanxi Medical University Doctor’s Funds (No. 2017-105), Natural Science Foundation of Shanxi Province (Grant No.201801D221117), and the Program for the Outstanding Innovative Teams of Higher Learning Institutions of Shanxi (2019L0410).
