Abstract
Objective
Metabolic syndrome (MS) is a common clinical condition associated with cardiovascular disease in patients undergoing peritoneal dialysis (PD); however, its prognostic implication among patients receiving PD remains controversial.
Methods
In a prospective study from January 2013 and June 2016, we enrolled 190 patients undergoing PD and followed them for 46.4 ± 30.7 months. We assessed the associations of clinical characteristics and measurements with diabetes mellitus (DM) status, MS, and prognostic outcomes among the included patients.
Results
We found that DM was associated with shortened duration of dialysis and poor survival. The prevalence of MS was 58.9% among all patients. We found significant differences in age, body weight, body mass index, triglycerides, high-density lipoprotein cholesterol, fasting plasma glucose, leukocytes, platelets, neutrophil percentage, and pre-albumin between patients with and without MS. We found a negative correlation trend between serum intact parathyroid hormone and MS among our patients. The arteriosclerosis index was significantly elevated in the MS group compared with the non-MS group. Serum calcium concentration and frequency of hospital admissions were significantly associated with mortality and technique failure.
Conclusions
MS was positively associated with cardiovascular disease. DM, and hypocalcemia. Frequent hospital admissions can predict poor prognosis in patients undergoing PD.
Introduction
Metabolic syndrome (MS) is a common clinical condition prevalent among patients undergoing peritoneal dialysis (PD) with end-stage renal disease (ESRD) owing to chronic exposure to glucose-based solutions. In the past few decades, the prevalence of MS has increased to over 50% among patients receiving PD with or without diabetes mellitus (DM). As expected, this prevalence varies by ethnicity, geographical region, and the different definitions used.1–4 MS refers to a constellation of several risk factors for cardiovascular disease (CVD), type II diabetes, systemic inflammation, and the development of chronic kidney disease (CKD). Among them, CVD is the leading cause of death in patients with ESRD under long-term PD treatment.5–7 Therefore, MS has been further linked to CVD mortality among all patients receiving maintenance PD.8–11 However, controversy remains regarding the clinical outcomes of MS, particularly with respect to survival in patients without DM.
Definitions of MS include abnormalities of hyperglycemia (DM, insulin resistance, impaired fasting glucose, impaired glucose tolerance, non-DM fasting hyperinsulinemia, or fasting plasma glucose (FPG)), obesity (increased body mass index (BMI), waist-to-hip ratio, or waist circumference), dyslipidemia (increased triglycerides (TG) or reduced high-density lipoprotein cholesterol (HDL-C)), hypertension, and microalbuminuria. 12 The concept of MS arose in the early 1950s, and the World Health Organization (WHO) first officially defined MS in 1988. 13 Based on the WHO proposal, the European Group for the Study of Insulin Resistance, 14 the National Cholesterol Education Program's Adult Treatment Panel III (NCEP-ATPIII) of the United States, 15 and the International Diabetes Federation 16 defined MS in different ways in 1999, 2001, and 2005, respectively, with a modified NCEP-ATPIII definition proposed in 2008. 17 The slight variations among these definitions are mainly focused around (central) obesity, DM, and insulin resistance, with some further details still being discussed.
Despite the variability in diagnosis and prognosis, preventing MS in patients undergoing PD is important in clinical practice. In this study, we aimed to investigate the associations among MS, clinical measurements, and their corresponding outcomes in patients receiving PD from a single center in northern China.
Materials and methods
Patients and sampling
This study was approved by the Ethics Committee of the Second Hospital of Tianjin Medical University. Written informed consent was provided by all patients before they participated in this study. We enrolled patients with ESRD (age >18 years) who had received a conventional glucose-based lactate-buffered PD solution (Dianeal, Baxter Healthcare, Guangzhou, China) from the start of PD therapy at our dialysis unit between January 2013 and June 2016 and who had maintained treatment for more than 3 months. All patients underwent daytime ambulatory PD with 1.5% dextrose dialysate. Outpatient records were reviewed to obtain participants’ demographic and clinically relevant information.
Definitions of MS
MS was defined based on the modified NCEP-ATPIII diagnostic criteria, 17 i.e., fulfillment of at least three of the following: BMI > 25 kg/m2 for Asians; TG ≥150 mg/ dL (1.7 mmol/L); HDL-C <40 mg/dL (1.03 mmol/L) in men, <50 mg/dL (1.29 mmol/L) in women; blood pressure ≥130/85 mmHg or receiving antihypertensive treatment; and FPG ≥100 mg/dL (5.6 mmol/L) or a diagnosis of DM and under treatment.
Clinical measurements
We collected general information including age, sex, body weight, height, primary renal diseases, the presence of DM, duration of dialysis, and history of hypertension. BMI was used to assess obesity. Body weight was measured to calculate BMI among patients undergoing PD, with either a dry abdomen or with PD dialysate in the abdomen minus the infused volume of PD dialysate, in liters. A trained nurse measured brachial blood pressure, with patients in a sitting position after resting for at least 5 minutes in a quiet room. Patients with hypertension took their usual antihypertensive medications on the morning of each clinic visit, and PD prescriptions for each patient were recorded. Patients fasted overnight for 10 hours, after which venous blood samples were collected in the morning for laboratory measurements, including hemoglobin, serum albumin, pre-albumin, FPG, calcium, phosphorus, TG, total cholesterol, HDL-C, low-density lipoprotein cholesterol (LDL-C), C-reactive protein, and intact parathyroid hormone (iPTH). All biochemical parameters were examined at the initiation of PD therapy and assessed regularly at 3-month intervals. iPTH was determined by immunoassay. Serum albumin level was used to reflect nutritional status. The arteriosclerosis index was calculated by dividing LDL-C by HDL-C.
Outcomes and endpoints
All patients were followed until December 2017. The outcomes of interest included the number of hospital admissions, duration of hospitalization, peritonitis, CVD (ischemic heart disease, cerebrovascular disease, congestive heart failure, or peripheral vascular disease), and mortality. Death, kidney transplantation, and transfer to hemodialysis were defined as technique failure. The time from the start of peritoneal dialysis to technique failure was considered the duration of technique survival.
Statistical analysis
Statistical analyses were performed using SPSS 19.0 software (IBM Corp, Armonk, NY, USA). The mean and standard deviation (mean ± SD) were computed for continuous data. Data were compared using chi-squared (χ2) analysis or one-way analysis of variance. Kaplan–Meier plots of survival curves and comparisons between groups with log-rank tests were used for descriptive analysis of survival data. Stepwise logistic regression was performed for all variables, to identify independent predictors. Hazard ratios (HRs) and 95% confidence intervals were estimated using a Cox regression model. All statistical analyses were conducted with a significance level of α = 0.05, and Bonferroni correction was applied for multiple tests.
Results
In this study, we enrolled 190 patients undergoing PD, including 28 patients with primary hypertension, 64 with DM, 84 with chronic glomerulonephritis, 5 with polycystic kidney disease, and 9 with other diseases. Patients’ clinical characteristics and biochemical measurements are summarized in Table 1. The median duration of PD was 46.4 ± 30.7 months. During this period, 75 (39.5%) patients experienced technique failure, including 51 (26.8%) who died, 15 (7.9%) who converted to hemodialysis, and 9 (4.7%) who received kidney transplantation. The causes of death were CVD (myocardial infarction, sudden cardiac arrest, and heart failure; 24 patients), digestive tract disorders (4 patients), stroke (2 patients), infection (14 patients), severe malnutrition (6 patients), and cancer (1 patient). The overall mortality in patients with and without DM was 48.4% and 15.9% (P < 0.01), respectively. In the DM group, mortality in patients with MS was 42.3% (22/52) whereas in the non-DM group, this was 16.7% (10/60, DM with MS vs. non-DM with MS: P < 0.01). During this period, all patients had an average of 0.55 ± 0.69 hospital admissions and 10.2 ± 15.1 days of hospitalization per year.
Clinical characteristics and biochemical measurements of patients.
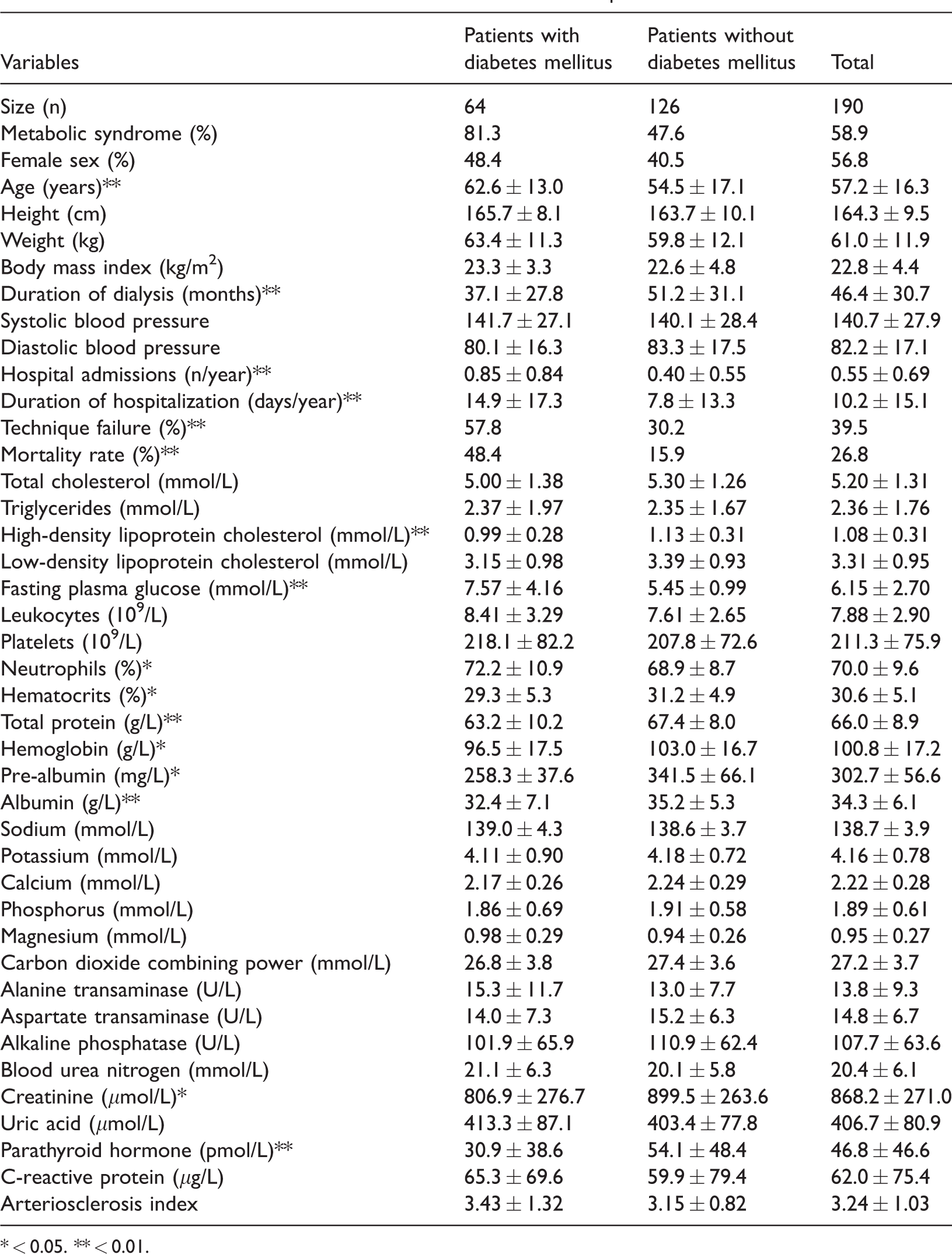
* < 0.05. ** < 0.01.
We compared all observations between patients with and without DM. Patients with DM were significantly older (P = 0.001), had more hospital admissions (P = 2.2 × 10−5), longer hospitalization (P = 0.002), more technique failures (P = 2.3 × 10−4), and a higher mortality rate (P = 1.7 × 10−6), FPG (P = 3.3 × 10−7), and neutrophil percentage (P = 0.029) than those without DM. In contrast, the duration of dialysis (P = 0.003), HDL-C (P =0.002), hematocrit percentage (P = 0.013), total protein (P = 0.003), hemoglobin (P = 0.013), pre-albumin (P = 0.015), albumin (P = 0.002), creatinine (P = 0.026), and iPTH (P = 0.005) were significantly lower in patients with DM.
The prevalence of MS, as defined using the modified NCEP-ATPIII criteria, was 58.9% (112/190) among all patients. We compared clinical findings between patients with and without MS (Table 2). Aside from some MS-related items, such as body weight, BMI, TG, HDL-C, and FPG, there were significant differences with respect to age (P = 0.012), percentage of DM (P = 8.4 ×10−6), leukocytes (P = 0.022), platelets (P = 0.043), neutrophil percentage (P =0.028), and pre-albumin (P = 0.024). The arteriosclerosis index was significantly increased in the MS group (3.52 ± 1.07) in comparison with the non-MS group (2.79 ± 0.80; P = 9.4 × 10−7).
Comparison analysis between patients with and without metabolic syndrome (MS).

* < 0.05. ** < 0.01.
Kaplan–Meier plots of overall and technique survival in a comparison of patients with and without MS (modified NCEP-ATPIII criteria) are shown in Figure 1. There was no significant difference in overall and technique survival between patients with and without MS. However, a slight decrease was observed between months 60 and 80 in overall survival. Cox regression analysis of risk factors revealed that high systolic pressure, HDL-C level, leukocyte content, platelet content, hematocrit, aspartate transaminase level, uric acid level, and hospital admissions were significantly associated with increased risks of mortality and technique failure; high diastolic pressure, total protein content, calcium concentration, creatinine level, and parathyroid hormone were significantly associated with adverse outcomes (Table 3). HDL-C levels (technique failure: HR = 4.152, P = 0.001), calcium concentration (technique failure: HR = 0.196, P = 0.001), and hospital admission (mortality: HR = 6.171, P = 9.3 × 10−11; technique failure: HR = 3.143, P = 9.1 × 10−11) were the three most important factors related to technique failure or mortality in patients receiving PD.
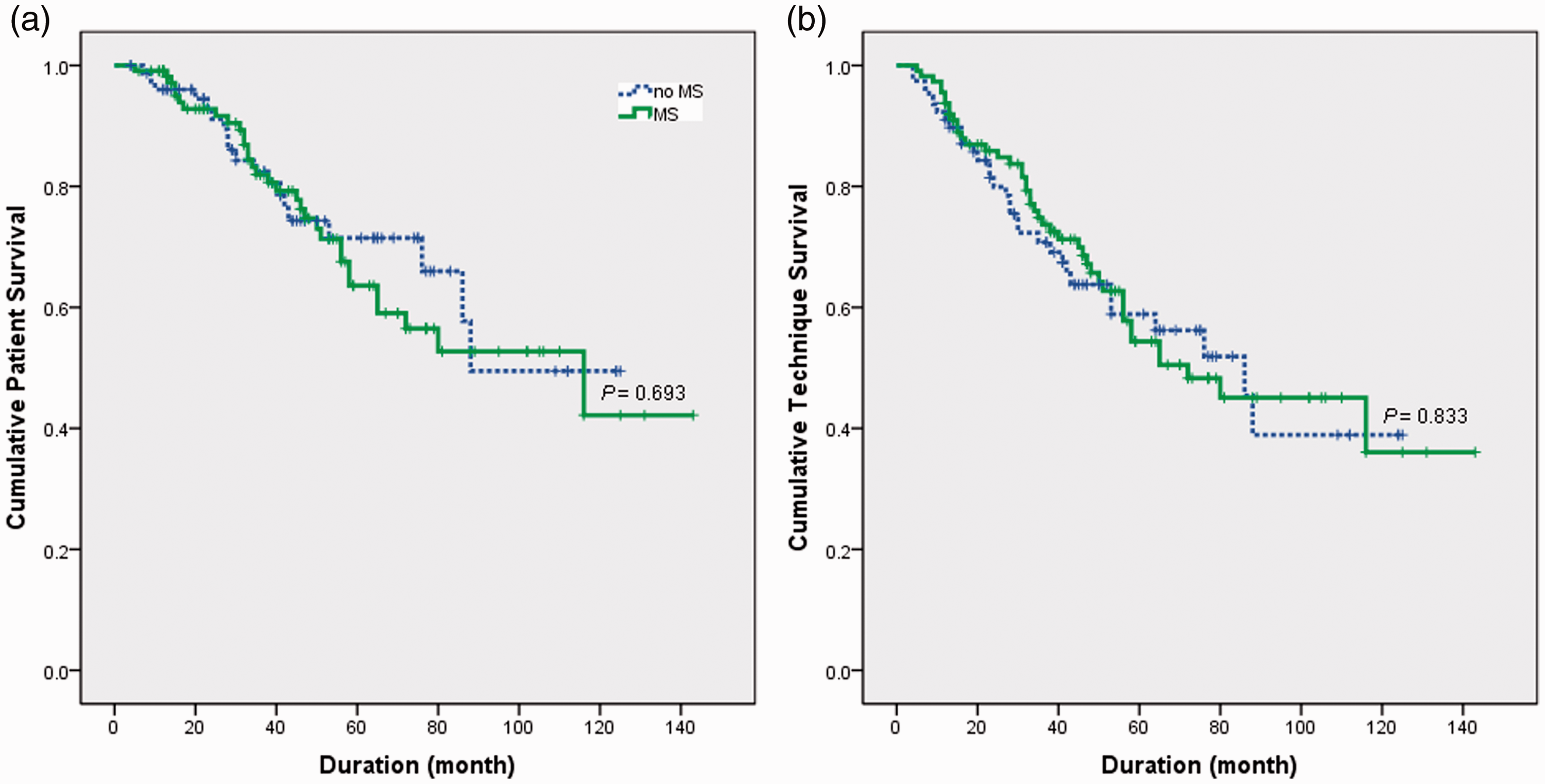
Kaplan–Meier survival plots. (a) Overall survival and (b) technique survival of patients with and without metabolic syndrome (MS). There was no significant difference in overall and technique survival between patients with and without MS.
Hazard ratios (HRs) and 95% confidence intervals (CIs) of significant risk factors (P < 0.05) for mortality and technique failure in patients undergoing peritoneal dialysis.

Discussion
In the present study, we diagnosed MS using the modified NCEP-ATPIII criteria. 17 Using BMI for the definition of obesity is more convenient in clinical practice than using waist circumference, especially in patients undergoing PD, owing to intraperitoneal infusion of dialysis solution. 18 The prevalence of MS in our patients receiving PD was 58.9%, which is generally in agreement with that of previous studies.3,19,20 DM was associated with shortened duration of dialysis and poor survival, and high prevalence of MS (81.3%) was observed in patients with DM (non-DM: 47.6%, Table 1). The core findings of our study are that leukocytes, platelets, and neutrophils were positively associated with MS prevalence whereas pre-albumin was inversely associated with MS prevalence (Table 2). Patients with MS who are receiving PD always have low-grade, chronic inflammation.21,22 Our findings may indicate a stronger inflammatory reaction in patients with MS than in those without MS. MS has been reported as an independent risk marker for CVD morbidity and mortality in patients without DM who are undergoing PD.1,23 Patients with MS had a higher risk of arteriosclerosis incidence than those without MS. Although we did not find higher mortality or technique failure in patients with MS undergoing PD, we did observe a higher arteriosclerosis index in this group.1,24 The arteriosclerosis index can reflect overall arterial elasticity in patients with MS. In our study, a significantly lower HDL-C level was observed in patients with MS. Low HDL-C has been shown to be important in increasing the risk for CVD. 25 Moreover, we observed that elevated HDL-C levels were associated with an increased presence of technique failure.
It has been reported that endogenous serum calcium is independently associated with insulin sensitivity. 26 Healthy people with low calcium levels have the lowest concentration of glucose and the least insulin resistance. 27 Positive relationships between serum calcium concentrations and MS have been described previously. 28 In this study, the serum calcium levels of patients with DM (2.17 ± 0.26 mmol/L) were at the lower limit of the recommendations (2.1–2.5 mmol/L) according to Kidney Disease: Improving Global Outcomes. 29 We found no significant variation in calcium concentrations between the MS and non-MS groups. However, we did observe that low calcium concentrations in our cohort were significantly associated with increased mortality and technique failure in patients undergoing PD. Both higher calcium concentrations and hypocalcemia are associated with increased mortality in patients with CKD or receiving dialysis.30–32 Low serum calcium indicates poor prognosis; therefore, we advocate intake of vitamin D to maintain serum calcium concentrations in patients undergoing PD. Further, greater attention is needed for patients with more hospital admissions. Patients receiving PD often present with inflammatory or cardiovascular diseases, as well as other risk factors that can increase their rates of hospital admission. In addition, these patients appear to have higher mortality.
Serum iPTH is positively correlated with the risk of MS.33–36 However, the opposite trend was reported by Dong et al. among Chinese patients undergoing PD 3 in a large, multi-center, cross-sectional study. Here, we found the same trend of negative correlation between serum iPTH and MS among our patients receiving PD (patients with MS: 42.0 ± 42.7 pmol/L; patients without MS: 53.9 ± 51.9 pmol/L), although the difference was not significant. Limited by our cohort size, the large variation affects the significance. Thus, this finding requires confirmation using a larger sample size in future studies.
Conclusion
In patients undergoing PD, overall survival and technique survival did not differ between patients with and without MS, as defined by the modified NCEP-ATPIII criteria. Calcium deficiency and frequent hospital admissions were related to poor prognosis.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by the National Natural Science Foundations of China (no. 81672113 and no. 81600591) and Tianjin Natural Science Foundation (no. 17JCQNJC12900) and Science and Technology grants from the Tianjin Health Bureau (no. 2013KZ080).
