Abstract
Objective
A 29-year-old male from Guizhou, China, had been suffering from obsessive–compulsive disorder since graduation from junior high school at 14 years. He was afraid of putting glass substances in his mouth. His main symptoms were repetitive thoughts, inquiries and examinations for more than 6 hours a day. He dropped out of school and stayed at home. He had been taking 60 mg/day paroxetine for 7 consecutive years. Over the past 2 years, his obsessive–compulsive symptoms had increased and were present for 12 hours a day.
Methods
The patient was treated using a combination of drugs, transcutaneous electrical acupoint stimulation–exposure and response prevention therapy (TEAS–ERP) and parental involvement.
Results
After 28 days, his Yale–Brown Obsessive Compulsive Scale score dropped from 40 to 11 points. After 1 month, telephone follow-up showed that he was able to do housework and was ready to go to work. After 6 months, he was able to easily work, and his compulsive behaviour only occurred 1 to 2 times each day for about 0.5 minutes each time.
Conclusions
The combination of TEAS–ERP, sertraline and clomipramine had a rapid effect. There was no resumption of obsessive–compulsive symptoms during post-treatment follow-up.
Keywords
Introduction
Obsessive–compulsive disorder (OCD) is characterized by forced thinking, compulsive behaviour or both, 1 and is a painful, time-consuming and severely damaging disorder. Adolescence is the peak period of OCD occurrence, and OCD often causes difficulties in learning, dropping out of school, inability to work and difficulties with family life.2,3 OCD is the fourth most common psychiatric disorder and has a lifetime prevalence of 1% to 3%.2,4 Adolescents who are unable to effectively reduce their compulsive symptoms experience poorer quality of life; therefore, the identification of more effective interventions is a top public health priority. 5 This is a case report of a young patient with OCD. The study protocol was approved by medical ethics committee of Tongde Hospital of Zhejiang Province and registered at www.chictr.org (ChiCTR-TRC-09000484), a member of the World Health Organization International Clinical Trial Registry Platform. We previously performed a randomized controlled trial of transcutaneous electrical acupoint stimulation (TEAS) that showed good efficacy for OCD; in the present study, we improved this treatment to obtain a more rapid effect. 6
Case
Medical history
The patient experienced OCD from the time he graduated from junior high school at the age of 14 years. One day, he suddenly stated to his family that he felt like he had eaten glass. He was terrified and soon dropped out of school. He did not dare to go out and was afraid of glass substances. He performed vomiting actions daily to spit out glass he felt was in his mouth. He would repeatedly inquire whether an item was made of glass, and repeatedly asked his parents if he had eaten glass. Before bathing, he would constantly inquire whether there was glass in the bathroom. Before eating, he would keep checking whether there was glass in the rice, and before any activity he would count repetitively to a number he considered auspicious. The symptoms affected him for more than 6 hours per day. He lived in Guizhou Province, China. In 2009, he went to Kunming city, Yunnan Province, which is 300 km from Guizhou. A physician diagnosed him with OCD and prescribed paroxetine tablets. The dose of paroxetine was gradually increased from 20 mg per day to 60 mg per day. His condition improved, but soon his obsessive symptoms became more obvious; he insisted on taking 60 mg of paroxetine tablets daily, and he took them for 7 consecutive years. He finally stopped taking the medication 2 years prior to his visit to our hospital. Subsequently, his OCD symptoms further increased. His symptoms lasted for 12 hours per day, and prevented him from going out. He felt forced to think all the time. His father feared that untreated individuals with OCD would be removed from Guizhou Province, and travelled 1900 km to bring his son to our hospital’s OCD treatment centre.
Diagnosis
The patient had no tic symptoms, no history of psychoactive substance consumption, no major depression or anxiety and no obvious psychotic symptoms. His Yale–Brown Obsessive Compulsive Scale (Y-BOCS) score was 40 points; his Hamilton Depression Scale (HAMD) score was 12 points and his Hamilton Anxiety Scale (HAMA) score was 16 points. The patient was given a primary diagnosis of OCD, following the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR) guidelines. 7 The institutional review board (ethics committee of Tongde Hospital of Zhejiang Province) approved the study protocol. The patient participated voluntarily and provided written informed consent prior to the treatment.
Treatment
Treatment at our hospital is undertaken with the realization that patients often travel great distances, seek urgent treatment and have financial difficulties. After consultation with patients and parents, patients are treated using multiple therapies. The usual combination therapy for OCD comprises (a) drug treatment (100 mg/day sertraline, 50 mg/day clomipramine), (b) twice-weekly TEAS–exposure and response prevention therapy (TEAS–ERP) 8 and (c) parental participation.
Sertraline tablets (Pfizer Pharmaceutical Co., Ltd., Dalian, China) were given; the initial dose was 25 mg/day and increased to 100 mg/day on the seventh day. Clomipramine tablets (Hunan Dongting Pharmaceutical Co. Ltd., Hunan, China) were also given; the initial dose was 25 mg/day and increased to 50 mg/day on the third day.
TEAS–ERP comprises exposure and response prevention therapy (ERP) and transcutaneous electrical acupoint stimulation (TEAS). The TEAS and ERP treatment was given simultaneously for 50 minutes per session (Figure 1). The acupuncture points used were mainly Neiguan points (PC6). Neiguan (PC6) is located on the anterior forearm, between the tendons of palmaris longus and flexor carpi radialis. The point is at the midpoint of the wrist, one-sixth of the distance from the distal wrist crease and five-sixths of the distance from the elbow crease (Figure 1).

Treatment implementation method, the location of Neiguan points (PC6) and the stimulator.
The instruments used for the stimulation were a low frequency electric stimulator (Shenzhen Ryan Medical Treatment Appliance Co. Ltd., Shenzhen, Guangdong, China; model SNH-138, power supply DC9V [006P], product standard number: YZB/Yue 0138-2003, production license: Guangdong Food and Medicine Equipment Production Xu 20010106). A conductive adhesive patch was placed on the left and right PC6 acupoints. The patient’s most prominent compulsive symptom was a fear of accidentally eating glass. We used broken pieces of a glass water bottle as props for exposure therapy in ERP implementation. In the ERP treatment, we let the patient hold a broken piece of glass and assessed symptoms of wanting to eat the glass piece. As the treatment progressed, the obsessive–compulsive behavioural symptoms gradually decreased. This treatment also includes teaching patients how to treat and prevent obsessive–compulsive symptoms, such as exercising gradual control over repetitive counting behaviour and repeated questions, reducing bathing time, increasing exercise time, going out more often and being exposed to the outside world, and getting a haircut and shave.
Therapy also included parental involvement. The patient’s parents went out for a walk with him initially for 1 hour every day. They increased the duration by 1 hour every 3 days, finally walking for 3 hours every day. Walking could be strolling by the side of the road or visits to the park and supermarket. These sessions included urging the patient to reduce his bathing time, get a haircut and shave and gradually reduce his repetitive questioning behaviour.
Evaluation
The primary evaluation tool was the Y-BOCS total score and subscale scores.8–10 By the first weekend after initiating treatment, the Y-BOCS score was 28 points and the patient was still fearful of glass; he kept repeatedly checking the location of the glass item and looking at it for a prolonged time. By the second weekend, the Y-BOCS score was 22 points and the patient showed no fear of broken glass in the clinic. However, after returning to the hotel, he was fearful; he asked where the glass was and kept counting before any activity. At this stage, he was too fearful to shave or get a haircut. By the third weekend, the Y-BOCS score was 16 points and the patient got a shave and haircut; the duration and number of repetitive inspection and counting behaviours were reduced to 2 to 3 times a day, 1 to 2 minutes each time. By the end of the fourth week, the Y-BOCS score was 11 points and the symptoms had almost disappeared; the patient’s bath time was within 30 minutes (Figure 2). Laboratory tests at baseline and at the end of treatment showed no abnormalities in liver or kidney function, electrocardiogram results or electroencephalogram results. Safety was assessed using the Treatment Emergency Symptom Scale (TESS). 11 There were no adverse effects other than mild dry mouth. After 4 weeks of combination treatment, the patient went home with his parents and continued the same drug maintenance treatment. Monthly follow-up was carried out by 30-minute telephone calls. The telephone follow-up focused on the current status of the patient, stressing the importance of adhering to medical treatment and guiding further ERP training (e.g., advising the patient that when he thought of checking if there was glass in his mouth, he should actively transfer his attention to happier thoughts, such as finding a job or going out for exercise). His parents were simultaneously reminded to help him in the ERP training and build his confidence in overcoming the disease. The 6-month follow-up schedule is shown in Table 1.
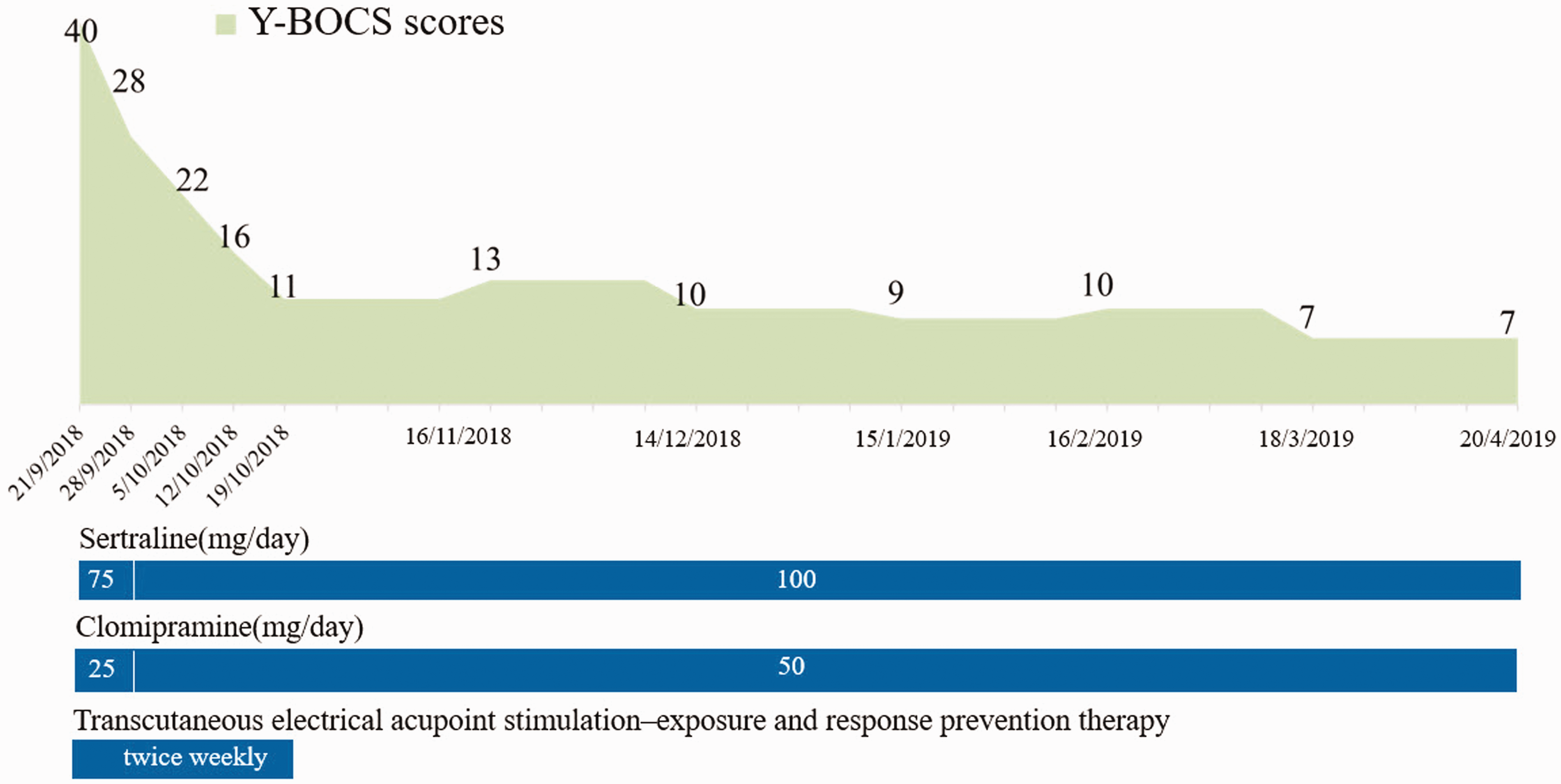
Patient treatment record.
The 6-month follow-up schedule.

Y-BOCS: Yale–Brown Obsessive Compulsive Scale.
Discussion
The rate of OCD remission in adults is low (20%), 7 and the likelihood of relieving symptoms using medication alone is low (11% of patients in one study). 12 Only approximately one-third of patients with OCD receive appropriate drug combination therapy, and less than 10% receive evidence-based psychotherapeutic interventions. 13 The present case was a patient with very severe OCD. His condition had persisted for 15 years because of a lack of effective treatment. The consequences included dropping out of school, not going out, not working and even having personal difficulties. Although a high dose of paroxetine (60 mg/day) was initially used for treatment, the patient’s symptoms were not alleviated and more effective treatment was necessary to restore his quality of life. Treatment with clomipramine in combination with sertraline is an alternative method of drug therapy. In the present case, a conventional dose of sertraline (100 mg/day) was administered and a low dose of clomipramine (50 mg/day) was added. The patient did not show significant side effects or synergistic effects. The results of exposure therapy in combination with drugs are superior to those of drugs alone. 14 ERP is a more effective behavioural therapy for OCD, but approximately 18.7% of patients who receive ERP withdraw from treatment owing to intolerance. 15 Therefore, we used TEAS in addition to ERP. TEAS allows the nerves to relax quickly and rapid relaxation increases both compliance and the efficacy of ERP. The participation of the patient’s parents in the entire treatment was also extremely important. After 4 weeks of combination treatment, the Y-BOCS score declined to 11. We believe the combination of TEAS–ERP, sertraline and clomipramine has a rapid onset of action. During the 6 months follow-up, there was no resumption of OCD symptoms after the TEAS–ERP treatment.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
