Abstract
Objective
This study was performed to assess the feasibility of conservative treatment for stage II or III serous borderline ovarian tumors (BOTs).
Methods
Twenty-one patients were treated conservatively for advanced serous BOTs from 2006 to 2017. Two patients were lost to follow-up. The patients’ clinical status, surgical results, fertility results, and oncological outcomes were collected.
Results
The patients’ median age at surgery was 28 years (range, 22–37 years). The median follow-up interval was 74 months (range, 16–214 months). Among the 19 patients who were followed up, 8 had stage II tumors and 11 had stage III tumors. Sixteen patients had noninvasive peritoneal implants. Two patients developed tumor metastasis to the fallopian tubes and one developed metastasis to the pelvic lymph nodes and omentum. The total recurrence rate was 26.3%. Seventeen (89.5%) patients were nulliparous. Four of 10 patients who wished to preserve their fertility obtained natural pregnancy. No patients died of their disease.
Conclusions
This study supports the efficacy of conservative treatment for advanced BOTs with respect to its favorable fertility result. The overall prognosis is not changed by conservative treatment.
Keywords
Introduction
A borderline ovarian tumor (BOT), which is of low malignant potential, is defined as “an ovarian tumor exhibiting an atypical epithelial proliferation greater than that seen in the benign counterpart but without destructive stromal invasion” by the World Health Organization. 1 It constitutes about 10% to 20% of ovarian neoplasms. Unlike invasive carcinoma, its prognosis is very good: the 10-year survival rate is 99% for stage I, 98% for stage II, 96% for stage III, and 77% for stage IV.2–4 A serous BOT, especially with exophytic growth, is likely to implant into the surface of the peritoneum and develop into low-grade serous carcinoma. 5 A serous BOT is likely to affect younger women and be diagnosed before childbearing occurs. Because of its favorable prognosis, fertility-sparing surgery can be proposed to patients with stage I serous BOT who desire pregnancy.6–8 However, because of the low morbidity of and lack of experience with advanced-stage serous BOTs, few evaluations have focused on conservative surgery in these patients.
According to the National Comprehensive Cancer Network guideline, fertility-sparing surgery, which preserves the uterus and at least one ovary, can be applied to patients with BOT. If no invasive implants are present, this type of surgery can also be applied after incomplete staging procedures. 9 In contrast to its declaration that fertility-sparing surgery can only be used in patients with apparent early-stage invasive ovarian carcinoma, the guideline does not place restrictions on the stages of BOT. Unlike studies of early-stage BOT, few studies have specifically focused on the preservation of fertility for patients with advanced-stage BOT. The present study was performed to review a single institution’s experience with preserving fertility for patients with stage II or III BOT.
Materials and methods
Patient selection
We performed a retrospective chart review of patients diagnosed with stage II or III serous BOT from January 2006 to December 2017 in the Obstetrics and Gynecology Hospital, Fudan University. Every patient involved in this study provided verbal informed consent. The tumor staging system was based on the International Federation of Gynecology and Obstetrics 2013 criteria (FIGO 2013). 10 Only patients who had undergone fertility-sparing surgeries were included in the study. The benefits and risks of preserving fertility were carefully considered by both doctors and patients. The present study was approved by the Ethics Committee of the Obstetrics and Gynecology Hospital of Fudan University (approval number OBGYN 2017-07).
Clinical and follow-up data
The following data were obtained from the patients’ medical records: patient demographics, treatment, therapeutic results, time interval to recurrence, overall survival, and subsequent obstetric outcomes. The surgery was performed through laparotomy or laparoscopy. Four types of fertility-sparing surgery were performed 11 : unilateral salpingo-oophorectomy (USO), unilateral ovarian cystectomy (UOC), USO combined with contralateral ovarian wedge resection (USO + CWR), and bilateral ovarian cystectomy (BOC). Additional procedures were performed selectively: removal of macroscopic lesions, multiple peritoneal biopsies, omentectomy or omental biopsy, and peritoneal washing cytology. Adjuvant chemotherapy was administered to patients with lymph node metastasis, positive ascites cytology, coexisting microinvasion and a micropapillary pattern, or incomplete lesion resection. 12
After tumor excision, the patients were followed up with pelvic examinations every 3 months during the first year, every 6 months during the second year, and every 12 months thereafter. The follow-up indicators were the physical examination findings, tumor marker (cancer antigen 125) concentration, ultrasound examination findings, pelvic magnetic resonance imaging findings, and subsequent obstetric outcomes.
Statistical analysis
Baseline characteristics were compared between patients with stage II/III BOT with versus without relapse by Fisher’s exact test and the Wilcoxon rank-sum test. For all tests, a p-value of <0.05 was considered statistically significant. Stata 15.1 software (StataCorp, College Station, TX, USA) was used to perform all statistical analyses.
Results
Of 800 patients diagnosed with serous BOTs from January 2006 to December 2017 in our institution, 80 had stage II or III tumors. Of these 80 patients, 21 underwent fertility-sparing surgeries and were included in the study. Two patients were lost to follow-up; therefore, 19 patients were available for analysis. The median age at surgery was 28 years (range, 22–37 years). The median follow-up interval was 74 months (range, 16–214 months). Seventeen (89.5%) patients were nulliparous. Two patients were diagnosed with stage IIA BOT because the tumor had invaded the serosal surface of the fallopian tubes. Six patients were diagnosed with stage IIB BOT and 11 with stage III BOT. The patients’ clinical features are summarized in Table 1. In one patient, the BOT lesions were discovered upon accepting the second cycle of in vitro fertilization (IVF). The tumor relapsed 18 months after fertility-sparing surgery. No patients underwent postoperative infertility treatment.
General and oncological characteristics of the study population (n = 19).
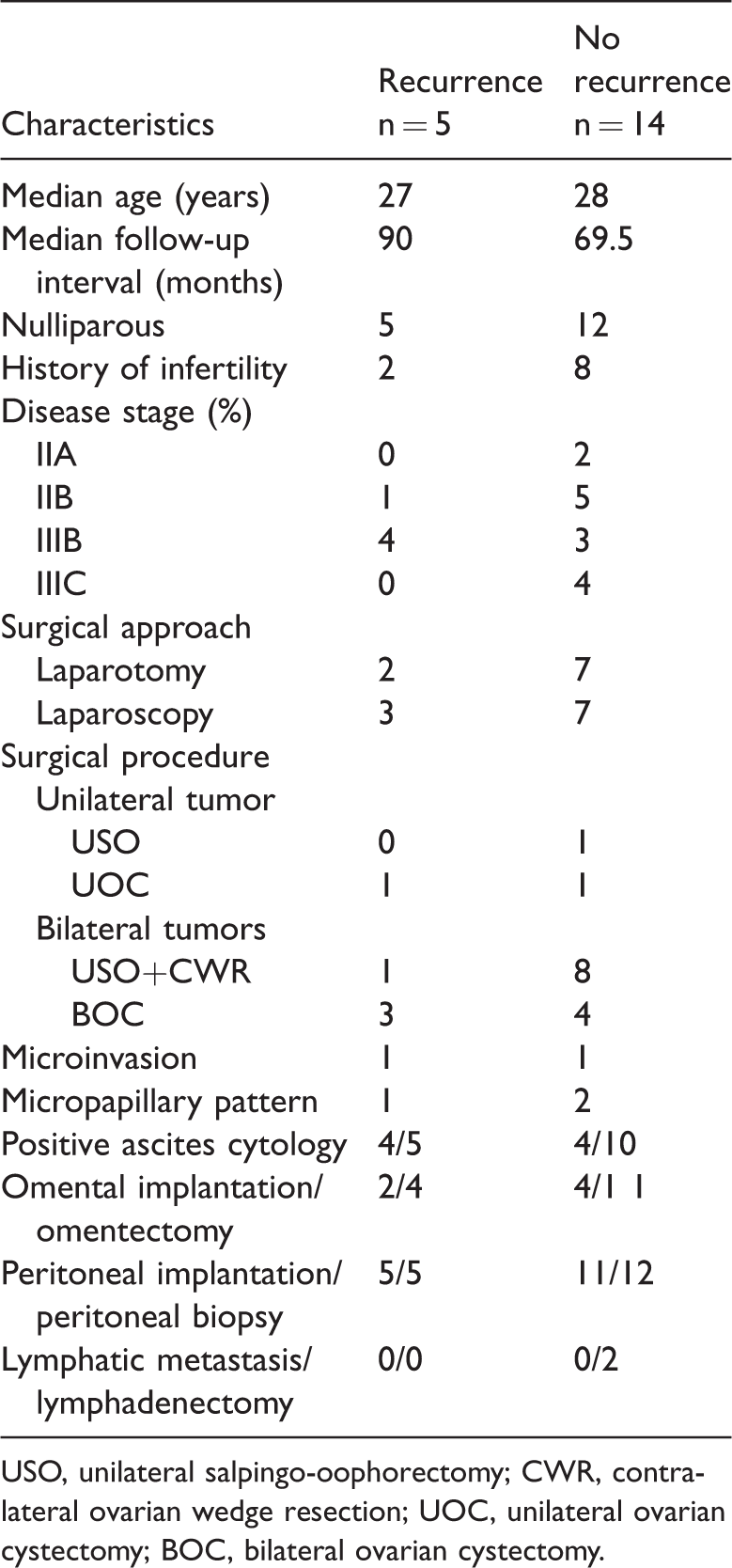
USO, unilateral salpingo-oophorectomy; CWR, contralateral ovarian wedge resection; UOC, unilateral ovarian cystectomy; BOC, bilateral ovarian cystectomy.
Of three patients with a unilateral BOT, one underwent salpingo-oophorectomy and two underwent unilateral cystectomy. Of 16 patients with bilateral BOTs, 9 underwent BOC and 7 underwent USO with contralateral cystectomy. Nine patients underwent laparoscopic surgery and 10 underwent abdominal surgery. Omental biopsy or excision was performed in 15 patients, 8 of whom had positive findings. Magnetic resonance imaging revealed suspicious enlarged lymph nodes in two patients; both patients underwent lymphadenectomy, and lymph node metastasis was confirmed in one.
Microscopic evaluation revealed microinvasion in 2 of the 19 patients. Noninvasive peritoneal implants were found in 17 patients, of whom 3 exhibited a micropapillary pattern. One patient with microinvasion and a micropapillary pattern developed tumor relapse 26 months after surgery. Ascites cytology was performed in 15 patients, of whom 8 had positive results.
Five of the 19 patients developed postoperative recurrence of their BOTs. The types of fertility-sparing surgery in these five patients were UOC in one patient, USO+CWR in one patient, and BOC in three patients. No patients had an invasive tumor. The overall recurrence rate was 26.3%, and the median interval to recurrence was 26 months (range, 18–53 months). No patients died of their disease. All patients had peritoneal noninvasive lesions, and the ascites cytology of four patients was positive. Two patients underwent radical surgery after relapse, and three patients underwent a second fertility-sparing surgery (one developed amenorrhea and two maintained a regular menstrual cycle). All patients with recurrence were disease-free at the last follow-up consultation. Their information is presented in Table 2.
Oncological characteristics of patients with relapse (n = 5).

USO, unilateral salpingo-oophorectomy; CWR, contralateral ovarian wedge resection; UOC, unilateral ovarian cystectomy; BOC, bilateral ovarian cystectomy; OMEN, omentectomy; PB, peritoneal biopsy; TC, carboplatin plus paclitaxel.
*Microinvasion, †noninvasive implantation with micropapillary pattern, §four times before surgery and four times after surgery.
The correlations between clinical characteristics and recurrence are shown in Table 1. We found no significant correlation between recurrence and patient age, tumor stage, or tumor type (unilateral or bilateral). Likewise, the surgery type and surgical approach showed no significant correlation with recurrence.
Ten patients expressed the desire to become pregnant after surgery, and four of them (40%) achieved spontaneous pregnancy and successfully delivered (Table 3). No ectopic pregnancies or abortions occurred. The median interval between surgery and pregnancy was 29 months (range, 18–35 months). Of the patients who became pregnant, only one who underwent UOC with peritoneal biopsy developed recurrence as a borderline cyst in the right ovary 53 months after the initial surgery. The primary pathology was a BOT with noninvasive implants and positive ascites cytology. The patient underwent three cycles of chemotherapy and conceived 18 months after the surgery by regular monitoring of ovulation. After undergoing salpingo-oophorectomy, she remained disease-free until the last follow-up. No patients developed tumor recurrence during the gestational period. All six patients who desired to become pregnant but failed had a history of infertility. The history of infertility significantly affected the postoperative pregnancy rate (p = 0.033).
Reproductive outcomes of patients desiring to preserve fertility (n = 10).
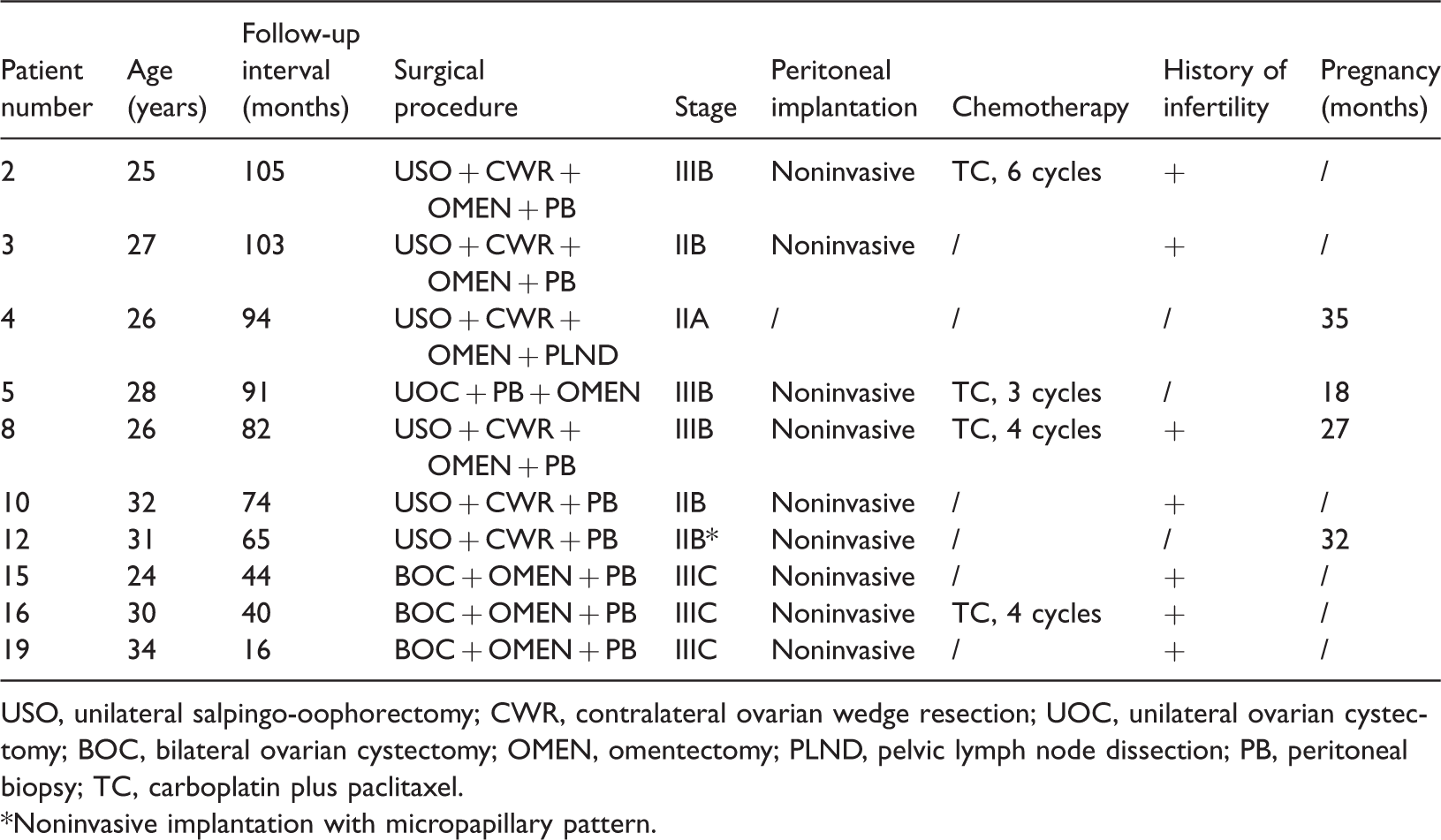
USO, unilateral salpingo-oophorectomy; CWR, contralateral ovarian wedge resection; UOC, unilateral ovarian cystectomy; BOC, bilateral ovarian cystectomy; OMEN, omentectomy; PLND, pelvic lymph node dissection; PB, peritoneal biopsy; TC, carboplatin plus paclitaxel.
*Noninvasive implantation with micropapillary pattern.
Discussion
In this study, we reviewed 19 patients with stage II or III serous BOTs who underwent fertility-sparing surgeries. Five patients (26.3%) developed recurrence during follow-up. This recurrence rate was not worse than that in previously published studies of patients with advanced-stage BOT who underwent conservative treatment and had clear fertility and oncological results (25.0%–56.4%); additionally, the pregnancy outcome was similar (33.3%–75.0%) (Table 4).13–17 The 2- and 5-year survival rates were 100%, and all patients were disease-free until the last follow-up. A recent meta-analysis of 74 patients from 4 studies concluded that compared with radical surgery, fertility-sparing surgery was associated with a significantly higher recurrence rate [odds ratio (OR), 3.87; 95% confidence interval (CI), 1.02–12.44; p = 0.02] but not a significantly higher survival rate (5-year survival rate: OR, 0.85; 95% CI, 0.03–23.82 and 7-year survival rate: OR, 0.80; 95% CI, 0.08–8.41). 18 BOT can relapse as BOT lesions (10%) or develop into invasive cancer (3%), and patients without invasive implants will achieve long-time survival.19,20 All five patients with recurrence in our study developed the recurrence as BOT lesions. Most recurrences present as BOT lesions with noninvasive implants, which can be removed by a second conservative surgery, leaving the total survival rate unchanged. Because of its favorable prognosis, fertility-sparing surgery can be applied to patients with advanced-stage BOT. However, because BOTs have low malignant potential, they require long-term follow-up. Because of the lack of research on conservative versus non-conservative surgery, the long-term risk requires further evaluation.
Literature review of oncological and reproductive outcomes in patients with advanced serous BOTs who underwent conservative treatment.

BOT, borderline ovarian tumor; IVF, in vitro fertilization.
In the present study, recurrence developed in one of two patients in the UOC group, in one of nine patients in the USO+CWR group, and in three of seven patients in the BOC group. Neither the surgical approach (laparotomy versus laparoscopy) nor the surgery type (USO, UOC, BOC, or USO+CWR) differed significantly between patients with and without recurrence. In a large-scale meta-analysis involving 433 patients with serous BOTs who were treated conservatively, the recurrence rate after cystectomy (unilateral and bilateral), USO, and USO+CWR was 43.2%, 32.1%, and 15.3%, respectively. 21 The study showed a significantly higher recurrence rate after cystectomy in patients with stage I to III serous BOTs (OR, 1.96; 95% CI, 1.178–3.266; p = 0.01), but complete data on the pregnancy rate were not available. This meta-analysis included three reports that showed complete data of the pregnancy results in patients with serious BOTs: 12 of 21 women who underwent USO achieved pregnancy, and 5 of 14 women who underwent cystectomy achieved pregnancy.14,15,21 Cystectomy was associated with a higher recurrence rate and lower pregnancy chance, but insufficient data were available for statistical analysis. This may have been because although cystectomy is a more conservative surgery that is performed to preserve more ovarian tissue, it is likely to increase the risk of recurrence; thus, it may not be a better choice. Further studies of patients with advanced-stage serous BOT are needed.
In the present study, the pregnancy rate among the patients who desired pregnancy was 40% (4/10), and the pregnancy outcome was similar to that of previous studies (33.3%–75.0%). The only relevant factor associated with the postoperative pregnancy outcome was whether the patient had a history of infertility (p = 0.033). The feasibility of preserving and promoting fertility for patients with BOT with a history of infertility remains controversial. A systematic literature review of 15 reports involving 62 patients with BOT who underwent 152 ovarian stimulation cycles and 135 oocyte retrievals showed a baby take-home rate of 28.3% per stimulation cycle with a recurrence rate of 19.4%.Forty-one (66%) of the reported patients had serous type BOT. Among them, nine (22.0%) patients developed relapse, five had stage I disease, and four had stage III disease. 22 Because of the lack of comparison with a control group, whether the prognosis was worsened by ovarian stimulation was unknown. Among the case reports13,15,17,23–28 of patients with advanced-stage serous BOT listed in Table 5, 18 patients delivered a live baby after ovarian induction or oocyte retrieval. Six patients developed relapse as BOT lesions, and one developed serous carcinoma and died. This patient, reported by Song et al., 17 was found to have invasive implants during surgery. Based on this limited number of cases, ovarian induction and IVF are safe for patients with advanced serous BOT without invasive implants. More research is needed to further confirm this conclusion.
Literature reports of patients with advanced-stage serous BOTs who underwent ovarian induction or oocyte retrieval as IVF procedures for infertility treatment.

*Patient died of the disease.
BOT, borderline ovarian tumor; IVF, in vitro fertilization.
Our study supports the performance of conservative treatment in patients with advanced BOTs because of its favorable fertility outcomes. Although the recurrence rate may be higher, the prognosis is good. We recommend ovarian cystectomy over adnexectomy for fertility-sparing surgery. Ovarian induction and IVF are safe to promote fertility but require further confirmation. We recognize that the limited number of cases made it difficult to draw definitive conclusions regarding fertility-sparing surgery for patients with stage II and III BOTs. Fertility-preserving management is worth attempting, but the safety and feasibility of fertility promotion require further exploration. Future prospective studies and laboratory research are needed to give answers to these questions.
Footnotes
Acknowledgements
The authors thank the doctors from the pathology departments of the Obstetrics and Gynecology Hospital of Fudan University for carefully reviewing the pathologic diagnosis of each patient involved in this research.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was supported by NSFC Grant 81101953 (to Chao Gu) and Natural Science of Shanghai 19ZR1406800 (to Bin Li).
