Abstract
Objective
This study aimed to assess the safety and efficacy of left liver anatomical resection via the left vertical groove following intraoperative antegrade cholangioscopy (biliary exploration through the left hepatic duct orifice) in patients with left-sided hepatolithiasis (LSH) and previous biliary tract surgery.
Methods
Between January 2012 and January 2016, eligible patients with LSH (n = 28) who underwent left liver anatomical resection via the left vertical groove followed by intraoperative antegrade cholangioscopy, were referred to our hospital. Clinical results, such as the overall operative time, length of hospital stay, intraoperative complications, residual stones and postoperative bile leaks, were recorded and analyzed.
Results
No residual stones and bile leakage occurred in the patients. No patients experienced intraoperative complications or T-tube placement. The mean operative time was 135.1 ± 18.9 minutes. The mean postoperative duration of hospitalization was 7.8 ± 1.8 days.
Conclusions
Left liver anatomical resection via the left vertical groove combined with intraoperative antegrade cholangioscopy is a safe and useful method for patients with LSH and previous biliary tract surgery. This technique simplifies the operative procedure by avoiding dissection of the porta hepatis and subsequent choledochotomy.
Keywords
Introduction
Hepatectomy and subsequent bile duct exploration are usually performed in patients with left-sided hepatolithiasis (LSH). Some of these patients undergo several previous biliary surgeries to address gallstones before receiving left hepatectomy, which may make dissecting the common bile duct (CBD) difficult. However, following left hepatectomy, an approach for bile duct exploration from the left hepatic duct (LHD) orifice to the CBD is possible. This approach has been applied to laparoscopic surgery for managing left-sided hepatolithiasis. This approach has significantly reduced the occurrence of intraoperative complications and accelerated postoperative recovery compared with conventional choledochotomy.1,2
In the present study, we describe our early experience with left liver anatomical resection via the left vertical groove and intraoperative antegrade cholangioscopy in patients with LSH and previous biliary tract surgery.
Patients and methods
Patients
Between January 2012 and January 2016, 170 patients who were admitted to our institution for management of hepatolithiasis were retrospectively studied. We included 28 patients with LSH and previous biliary tract surgery and with concomitant right-sided hepatolithiasis or choledocholithiasis. These 28 patients were well informed and gave informed consent before surgery. The study was reviewed and approved by the Yancheng City No. 1 People’s Hospital Institutional Review Board. Patients were excluded when they had right-sided intrahepatic biliary stricture and hepatic atrophy requiring bilateral hepatectomy or hilar cholangiocarcinoma requiring resection of the extrahepatic bile duct and lymph nodes. Preoperative ultrasonography and magnetic resonance cholangiopancreatography were routinely performed to determine the presence of CBD stones. Patients with cholangitis and acute pancreatitis were treated before the operation. Comorbid conditions, presenting symptoms, previous operations, length of hospital stay, overall operative time, and intraoperative/postoperative morbidity were recorded and analyzed.
Left liver anatomical resection via the left vertical groove
After adhesions around the left liver were addressed, we sequentially transected the falciform ligament, left coronary ligament, left triangular ligament, and hepatogastric ligament. The left portal vein, left hepatic artery, and left hepatic bile duct were dissected near the left vertical groove (Figure 1).

Dissection of the left portal vein (c) and left hepatic artery (a) near the left vertical groove. (b) Left hepatic duct.
Left hemihepatectomy and left lateral segmentectomy were performed using a standard technique as previously described. 3 For left hemihepatectomy, the left hepatic artery, left portal vein, and left hepatic vein were individually ligated with a Hem-o-lok (Teleflex Medical, Research Triangle Park, NC, USA) and divided. We transected the hepatic parenchyma with the assistance of an ultrasonic dissector (Söring GmbH, Quickborn, Germany) along a proposed division line. For left lateral segmentectomy, the left hepatic artery, left portal vein, and left hepatic vein were temporarily disrupted. The left lateral segment of the liver was transected approximately 2 cm along the falciform ligament. During the transection, we clipped the major vessels and bile ducts with a metal titanium clip. The orifice of the LHD was then identified and labeled.
Intraoperative antegrade cholangioscopy
The LHD stump was dilated by sutures. A fiber cholangioscope (model CHFP20; Olympus, Tokyo, Japan) was inserted through the LHD stump into the CBD (Figure 2). We explored the right hepatic duct, CBD, and caudate lobe duct. After confirmation of stones by a choledochoscope, a Dormia retrieval basket (Wilson-Cook Medial Inc. Winston-Salem, NC, USA) was used to extract the stones. After all of the stones were cleared, the LHD orifice was securely clipped with a Hem-o-lok.

Biliary exploration by intraoperative antegrade cholangioscopy.
Postoperative care and follow up
The patients received routine care and resumed oral food intake 24 hours after surgery. In the absence of biliary leaks, the peritoneal drain was removed in 48 hours. All patients received postoperative liver function tests and ultrasonography every 3 months or more frequently if biliary symptoms were present.
Results
The 28 patients had a median age of 52 years (range: 36–78 years), and there were 11 men and 17 women. The baseline characteristics of the patients are shown in Table 1. Bile duct exploration and stone extraction were completed in all patients via the LHD orifice. The mean (standard deviation) operative time was 135.1 ± 18.9 minutes. The mean postoperative duration of hospitalization was 7.8 ± 1.8 days. No patients underwent T-tube placement. There were no intraoperative complications, postoperative bleeding, residual stones, and biliary leakage in any of the 28 patients (Table 2). There was no mortality of patients during the hospital stay and a follow-up period of 18 months.
Baseline characteristics of the patients.

Surgical outcomes of the patients.
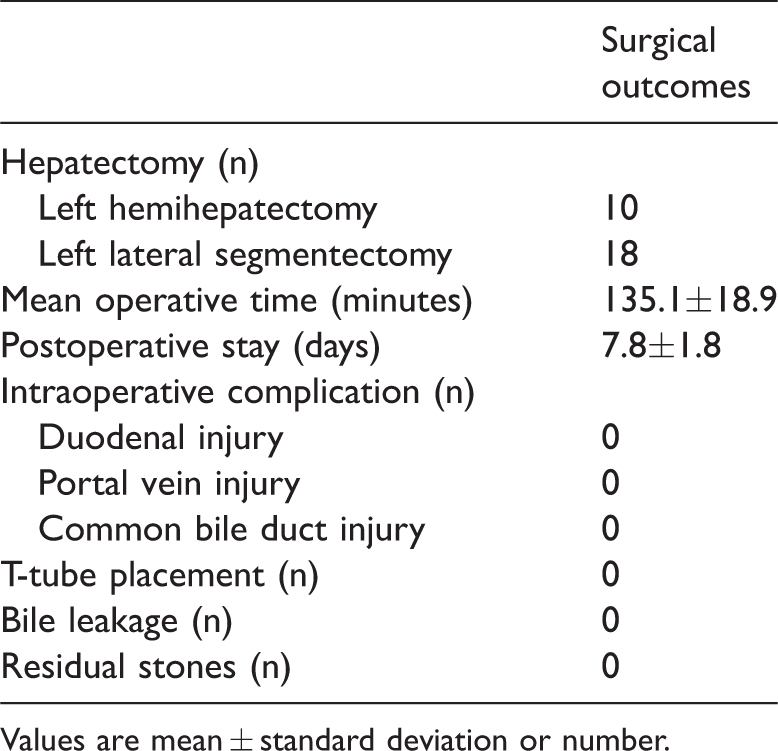
Values are mean ± standard deviation or number.
During the follow-up period, two (7.1%) patients suffered from recurrence of bile duct lithiasis. Postoperative ultrasonography confirmed that one patient developed cholangitis and one had small stones at the right hepatic duct.
Discussion
Left-sided hepatolithiasis constitutes the majority of cases of primary hepatolithiasis. 4 Left-sided hepatolithiasis usually requires left hepatectomy and additional bile duct exploration after long-term recurrent cholangitis. Notably, some of these patients have usually undergone several biliary operations before they accept hepatectomy. In China, some patients can only provide limited information regarding their previous operations. Prior unknown biliary surgery may result in technical difficulty in the first hepatic portal dissection and common bile duct dissection during conventional hepatectomy and choledochotomy.
Hwang et al. 5 explored the CBD through the LHD orifice and more than 90% of patients avoided choledochotomy and subsequent T-tube placement in their study. Furthermore, in laparoscopic-assisted or laparoscopic treatment of left-sided hepatolithiasis, LHD cholangioscopy significantly reduces the occurrence of intraoperative complications and accelerates postoperative recovery compared with conventional choledochotomy.1,2 This finding was confirmed in our study. In our study, patients underwent successful stone clearance, and no patients experienced intraoperative complications or T-tube replacement. All of our patients had previous biliary surgery. We believe that left liver anatomical resection via the left vertical groove followed by intraoperative antegrade cholangioscopy has some advantages for patients LSH and previous biliary tract surgery.
Patients with LSH usually require repeated bile duct exploration because of their high rate of recurrence. Although endoscopic retrograde cholangiopancreatography/endoscopic sphincterotomy is widely accepted as a safe and effective approach for recurrent stones, 6 it cannot achieve good CBD clearance in patients with previous biliary tract surgery. 7 If endoscopic sphincterotomy fails, conventional choledochotomy as a salvage procedure requires dissection of the CBD. Patients with a history of biliary surgery may experience several procedural complications during dissection of the CBD. 8 Adhesions form between the visceral surface of the liver and adjacent organs after biliary surgeries. During conventional hepatectomy and choledochotomy, these adhesions need to be addressed before dissecting the first porta hepatis and CBD, which may result in injures to the duodenum and the transverse colon. Furthermore, the tissues surrounding the CBD become tougher after each biliary surgery. This process may increase the likelihood of injuring the common bile duct or the portal vein. However, exploration of the common bile duct can be easily completed by left liver anatomical resection via the left vertical groove and intraoperative antegrade cholangioscopy. During this procedure, we need to address adhesions around the left liver, and then dissect the left portal vein and left hepatic artery near the left vertical groove.
Biliary leakage and anastomotic stricture constitute the predominant postoperative morbidities of choledochotomy. Although most biliary leaks spontaneously resolve within a few days, this complication prolongs the length of hospitalization. We recommend using a T-tube instead of primary closure in a subset of patients with intrahepatic gallstone presenting with an undilated CBD (diameter <8 mm) to avoid the risk of anastomotic stricture and subsequent complications. However, because of minimal interference with the CBD, biliary leakage, anastomotic stricture, and placement of a T-tube rarely occur in patients undergoing intraoperative antegrade cholangioscopy.
The LHD stump can be enlarged to 1 to 2 cm in diameter by forceful dilatation, which provides a suitable angle to detect the CBD and right hepatic duct. Because few blind spots are present, this technique can easily be manipulated. 4 CBD exploration via the LHD orifice follows the direction of bile flow, which is basically an antegrade choledochoscopy in contrast to endoscopic retrograde cholangiopancreatography. Furthermore, antegrade choledochoscopy has a lower chance of flushing out small gallstones into second- or third-order bile ducts compared with conventional choledochotomy. These small stones are the predominant sources of residual stones. In our study, all of the patients experienced successful stone clearance without T-tube placement.
Conclusions
Left liver anatomical resection via the left vertical groove combined with intraoperative antegrade cholangioscopy is a safe and feasible procedure for left-sided hepatolithiasis in patients with previous biliary surgery. This procedure simplifies left hepatectomy and biliary exploration by avoiding dissection of the first hepatic portal and following choledochotomy.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
The study was supported by the Jiangsu Provincial Young Talents Program of Medicine (Grant No. QNRC2016471) and Yancheng Medical Science Development Foundation (Grant No. YK2017006).
