Abstract
Objective
This study was performed to develop a prediction model for requiring manipulation under anesthesia (MUA) for flexion contracture after total knee arthroplasty (TKA) in patients of advanced age.
Methods
We retrospectively reviewed 269 patients of advanced age undergoing primary TKA in one center with a minimum 1-year follow-up. Patients who underwent postoperative MUA had flexion contracture of >10° after 4 weeks of postoperative rehabilitation, and their demographic data and preoperative clinical conditions [knee diagnosis, diabetes mellitus, hypertension, lumbar spinal disorders, hip disorders, ankle disorders, knee deformity (varus/valgus), preoperative flexion contracture (PFC), range of motion (ROM), and Hospital for Special Surgery (HSS) knee score] were compared with those of patients without MUA. All preoperative factors were collected to develop the predictive model.
Results
Thirty patients underwent MUA. Patients who underwent MUA after surgery had significant differences in PFC, higher HSS knee scores before surgery (59.10 ± 7.22 vs. 55.70 ± 13.09), and lower preoperative ROM (81.57 ± 30.86 vs. 95.47 ± 24.36) than those who did not undergo MUA.
Conclusion
A prediction model for MUA in advanced-age patients with flexion contracture was developed and mainly consisted of preoperative risk factors including PFC, HSS scores, and ROM.
Keywords
Introduction
Total knee arthroplasty (TKA) has been proven to be an extremely successful procedure for relief of chronic pain associated with degenerative joint disease in patients of advanced age. 1 The postoperative knee range of motion (ROM) is a crucial factor for patient satisfaction after surgery. Decreased ROM can result in a poor quality of activities of daily living, such as kneeling, stair climbing, and rising from a seated position.2–4 Despite improvements in surgical techniques, implant positions and designs, and postoperative management, postoperative stiffness is still a relatively common complication and has negative effects on the physical and mental health of advanced-age patients. The etiology of stiffness after TKA is most commonly multifactorial, and some factors are still controversial. 5 Manipulation under anesthesia (MUA) within 12 weeks after surgery may play a key role in improving outcomes for patients with stiffness after TKA.6,7 In other words, MUA is an effective solution for poor postoperative ROM. In the present study, we focused on patients of advanced age with flexion contracture after TKA because this type of stiffness is associated with abnormal gait requiring excessive energy expenditure and quadriceps loading, 8 with an increased risk of pain, knee dysfunction, and patient dissatisfaction as shown by outcome scores. 9 Although some low-grade contractures after TKA may be eventually resolved, 10 contracture is likely to persist if lack of extension (>15°) still exists 3 months postoperatively. 3
Establishment of a preoperative prediction model would be useful for improvements in the high morbidity, high costs, and poor quality of life associated with postoperative knee stiffness in patients of advanced age. Previous studies have shown that patient-related factors such as sex, race, and obesity were statistically significant risk factors for knee stiffness requiring MUA after TKA.1,11,12 The present study was performed to develop a model for patients of advanced age undergoing TKA and to evaluate its effectiveness in predicting the need for MUA for flexion contracture postoperatively. Such a model would be an easy-to-use and economical tool for practitioners to prevent this type of stiffness.
Methods
This study was approved by Institutional Review Board of Xuanwu Hospital, Capital Medical University [approval code: (2018) 047], and written informed consent was obtained from all study participants. Using the clinical database at this institution, we retrospectively reviewed the data of advanced-age patients (≥60 years old) who underwent primary TKA from April 2012 to December 2016. We included only patients who underwent unilateral TKA and in whom the clinical outcomes were followed up for a minimum of 1 year. The patients had no other complications, such as malalignment, infection, or dislocation.
Clinical information was gathered and maintained in our database by an independent investigator. Information regarding demographics [sex, age, and American Society of Anesthesiologists (ASA) grades], preoperative clinical conditions [knee diagnosis, diabetes mellitus, hypertension, lumbar spinal disorders, hip disorders, ankle disorders, knee varus/valgus, and preoperative flexion contracture (PFC)], and postoperative flexion contracture evaluation were collected within 12 weeks after surgery.
Five knee diagnoses were assessed: severe osteoarthritis, traumatic knee arthritis, moderate to severe osteoarthritis, rheumatoid arthritis, and benign tumor of the knee. In addition, PFC was classified into four types: recurvatum of ≤9° to 5° of limited extension, 6° to 19°, ≥20°, and recurvatum of ≥10° according to the degree of extension loss. 9 The preoperative ROM of the knee and the Hospital for Special Surgery (HSS) knee score were also evaluated.
All surgeries were performed by the same group of surgeons using the same prosthesis (GENESIS II; Smith & Nephew, Memphis, TN, USA). The operations were performed under spinal anesthesia. All patients underwent a standard surgical procedure with the medial parapatellar approach. The tourniquet pressure was set at 280 mmHg. To achieve complete correction of flexion contracture, patients underwent the same 12-week rehabilitation protocol. They visited the rehabilitation department for training with crutches or walking aids and received daily physiotherapy while in the hospital, and ROM was increased as tolerated until discharge. At home, the patients continued the ROM and muscle-strengthening exercises according to the physical therapy plan.
The indication for postoperative MUA was flexion contracture of >10° after 4 weeks of postoperative rehabilitation.13–15 All patients in the study were divided into two groups: those who did and did not undergo MUA within 12 weeks after TKA.
All manipulations were performed under general anesthesia with the limb rotated into a neutral position. The surgeon pressed the knee joint with proper force for 10 to 20 minutes until full extension of the knee was achieved. After the MUA, the patients pressed the knee with a 4-kg sandbag by themselves (4 times per day, 15 minutes each time).
Using the outcome “MUA within 12 weeks postoperatively” as the positive level, the area under the curve showed whether the fitted logistic regression model effectively predicted this outcome.
Statistical analysis
Categorical data are presented as frequency (count) and percentage. The chi-squared test was used to compare the distribution of categorical variables in the two groups of advanced-age patients who did and did not undergo MUA after TKA. Numerical variables are presented as mean and standard deviation, and Student’s t test was used to compare the mean values of the numerical variables between the two groups of patients. We established a logistic regression model of the surgical outcome on the following covariates: sex, age at time of TKA, diabetes mellitus, diagnosis of knee (osteoarthritis or rheumatoid arthritis), hypertension, lumbar spinal disorders, hip disorders, ankle disorders, PFC, preoperative HSS score, and preoperative ROM.
Results
Of 518 patients who underwent unilateral TKA and were followed up for at least 1 year, we excluded 249 because they could not undergo the standardized postoperative rehabilitation protocol for various reasons: periprosthetic infection (n = 13); other complications after TKA (n = 25); death unrelated to the surgery (n = 5); significant medical or mental problems unrelated to the surgery, including cardiovascular or cerebrovascular accident, malignant tumor, Parkinson’s disease, and Alzheimer disease (n = 109); and lack of available clinical outcomes evaluated postoperatively (n = 97). Consequently, 269 patients (218 female, 51 male) were selected for the final analysis. Of these 269 patients, 30 (11.15%) underwent MUA within 12 weeks after surgery. Tables 1 and 2 show the categorical variables and numerical variables of all patients. Through comparisons of the variables between patients who did and did not undergo MUA postoperatively, we found that patients who underwent MUA within 12 weeks after surgery had a significant difference in PFC (P = 0.002), higher HSS knee scores before surgery (59.10 ± 7.22 vs. 55.70 ± 13.09, P = 0.034), and lower preoperative ROM (81.57 ± 30.86 vs. 95.47 ± 24.36, P = 0.023). After MUA, the degree of postoperative flexion contracture was improved from 17.80° ± 5.51° to 4.30° ± 2.63°.
Patients’ demographic information and potential risk factors for MUA.
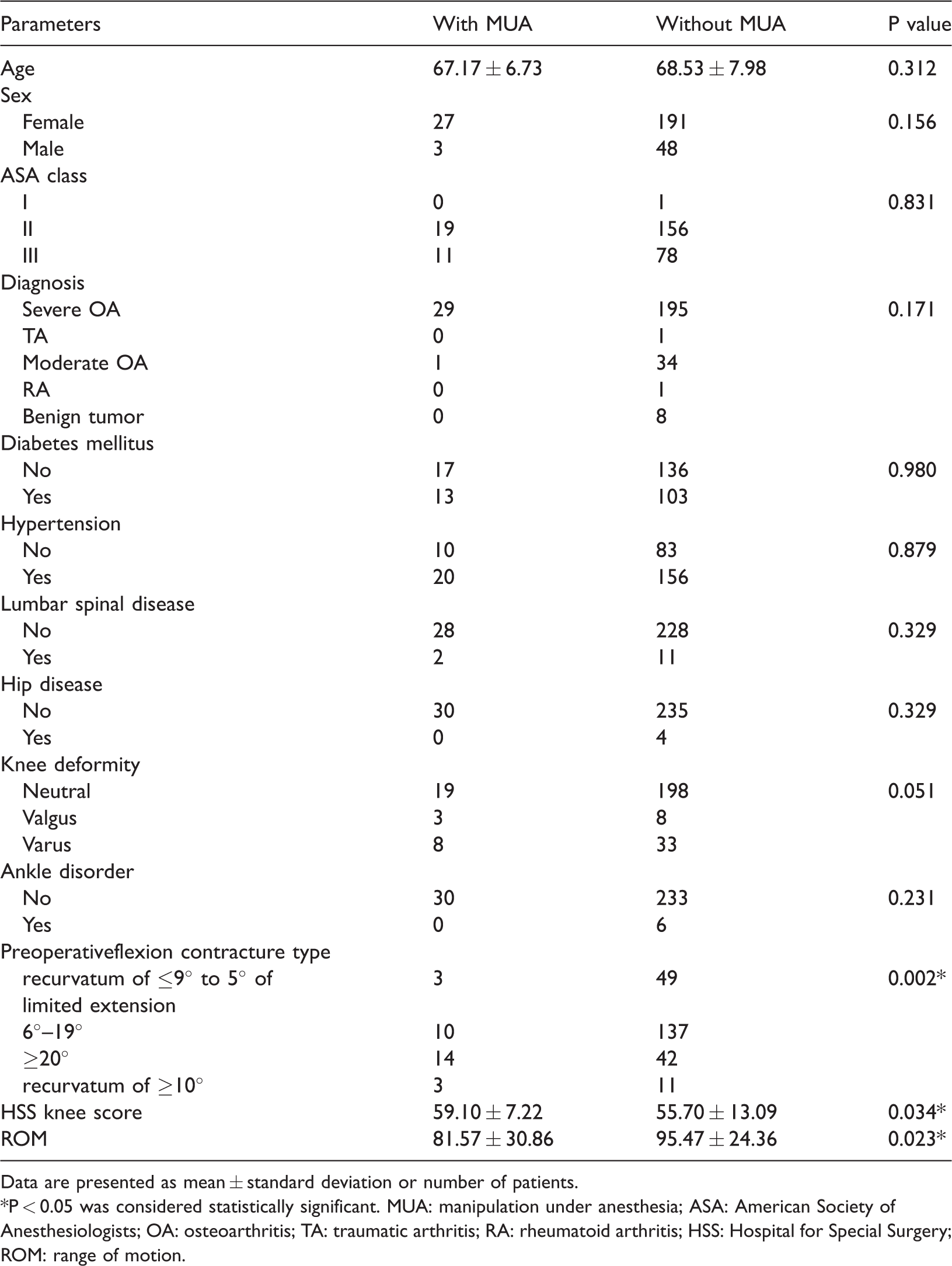
Data are presented as mean ± standard deviation or number of patients.*P < 0.05 was considered statistically significant. MUA: manipulation under anesthesia; ASA: American Society of Anesthesiologists; OA: osteoarthritis; TA: traumatic arthritis; RA: rheumatoid arthritis; HSS: Hospital for Special Surgery; ROM: range of motion.
Statistical results of numerical variables.

MUA: manipulation under anesthesia; HSS: Hospital for Special Surgery; ROM: range of motion; SD: standard deviation.
A fitted logistic regression model of the surgery outcome (MUA within 12 weeks after TKA in advanced-age patients) was developed using the following covariates: age, sex, ASA class, disease diagnosis, diabetes, hypertension, hip/lumbar/ankle disease, knee deformity, PFC, HSS knee score, and ROM before surgery. The results showed that PFC, the HSS knee score, and ROM played significant roles in predicting the requirement of MUA (Table 3).
Predictive results of logistic model.

MUA: manipulation under anesthesia.
PFC played a significant role in predicting the surgery outcomes (P = 0.0016). Patients with PFC of ≥20° had a higher risk of requiring MUA than patients with PFC of recurvatum of ≤9° to 5° of limited extension (odds ratio, 6.94; 95% confidence interval, 1.32–36.60; P = 0.0224). Patients with PFC of ≥20° had a higher risk of requiring MUA than patients with PFC of 6° to 19° (odds ratio, 6.78; 95% confidence interval, 2.39–19.26; P = 0.0003). The receiver operating characteristic curve for our prediction model is shown in Figure 1.

Receiver operating characteristic curve for the fitted logistic regression model in predicting the need for manipulation under anesthesia within 12 weeks after total knee arthroplasty in patients of advanced age. The accuracy, sensitivity, and specificity of the model are shown in the figure. The area under the curve is 0.8929.
The HSS knee score played a significant role in predicting the surgery outcomes (P = 0.0002). For each unit increment in the HSS score, the requirement for MUA increased by 0.087.
ROM played a significant role in predicting the surgery outcomes (P = 0.0259). For each unit increment in the ROM score, the requirement for MUA decreased by 0.021.
Discussion
TKA is a highly successful and cost-effective procedure. 16 As the demand for TKA continues to increase, especially in patients of advanced age,17–19 stiffness following TKA can lead to more cases of continuous pain, knee dysfunction, and patient dissatisfaction.4,11 Postoperative flexion contracture, a major type of stiffness, has negative effects on postoperative knee function and patient satisfaction.2,3 Previous studies have shown that stiffness after TKA is often multifactorial and includes patient, implant, and surgical factors, and that MUA performed within 12 weeks postoperatively can increase the ROM of the knee and improve the patient’s quality of life.5,20–22 Therefore, in the present study, we particularly focused on postoperative flexion contracture requiring MUA. It is crucial to establish a predictive model including confirmed patient-related preoperative high-risk factors, which may help physicians to treat high-risk patients earlier and decrease the incidence of this kind of stiffness after surgery.
The incidence of stiffness after TKA reportedly varies from 2% to 12% based on the definition used.23,24 Notably, the prevalence of postoperative stiffness requiring MUA in this study was 11.15%, higher than that in some previous studies because advanced-age patients were identified for the development of stiffness after TKA.10,19 The definition of advanced-age patients in this study was ≥60 years. Currently, independent orthopedists determine the acceptable level of postoperative stiffness and requirements for manipulation, resulting in various reported rates of MUA. In this study, the indication for postoperative manipulation was the presence of flexion contracture of >10° after 4 weeks of postoperative standard rehabilitation.
This study revealed risk factors for flexion contracture requiring MUA postoperatively among patients of advanced age undergoing TKA, and a prediction model was developed on the basis of these risk factors. Our findings suggest that the existence of PFC was a risk factor for postoperative stiffness treated by manipulation, which is partly in line with previous studies.9,10,24 Meanwhile, different from other studies, the type of PFC among the advanced-age patients in this study was differentiated according to the contracture angle, and a higher need of MUA after surgery was seen in severe PFC (>20°) than in PFC with recurvatum of ≤9° to 5° of limited extension or 6° to 19° of extension.
Our analysis suggests that the presence of poor ROM is a risk factor for postoperative stiffness requiring MUA in patients of advanced age, which is in agreement with previous studies.25,26 Poor preoperative ROM resulted in contracture of the posterior capsule, tendon, and ligament, even if they were released during the operation, which might cause flexion contracture deformity postoperatively. Meanwhile, severe pain might reduce patients’ satisfaction and functional exercise. 27
The mean HSS knee scores in both groups were <60, indicating worse knee function. The HSS score also played a key role in predicting stiffness requiring MUA after surgery, in which higher scores were associated with a greater need of MUA. The reason could be complex and multifactorial. The HSS score is composed of six factors: pain (30 points), function (22 points), ROM (22 points), muscle strength (10 points), flexion deformity (10 points), and instability (10 points). Because of severe postoperative pain, knee movements and the elasticity inherent in the tendons, ligaments, and muscle are reduced, ultimately leading to limited flexion and the development of flexion contracture. Inflammation in the soft tissues leads to variable amounts of arthrofibrosis in these structures. The high degree of preoperative flexion deformity of patients tends to have a long course and the inflammatory state is relatively low, so the HSS pain scores might be higher. Moreover, the HSS knee score system is heavily weighted toward pain and might not reflect the real situation. 23
PFC and ROM have also been reported as high-risk factors for stiffness after TKA in previous studies, and the present study is the first to report the HSS knee score as a new risk factor in the prediction model. Several limitations of this study should be noted. First, the proportion of female patients was 81.04% (218/269), which caused significant skewing of the data. This female sex predominance among patients undergoing TKA has been previously reported. 5 Further studies are needed to extrapolate and generalize our model across a larger population of patients (especially male patients). Second, the inaccuracy of a goniometer, as a measurement tool for ROM, might have influenced the data as reported in previous studies.3,9 Third, 249 patients who could not complete the 12-week rehabilitation protocol were excluded, which may have caused deviations in the statistical results. Finally, the relatively smaller sample size was another limitation of this study, and future studies with larger sample sizes should be encouraged.
Conclusion
The prevalence of advanced-age patients who required MUA for flexion contracture after TKA was approximately 11% in this study, and a prediction model based on risk factors (PFC, ROM, and HSS knee score) was highly effective in predicting postoperative stiffness treated by MUA.
Footnotes
Acknowledgment
We would like to thank Dr. Mingli Feng and Dr. Jiang Huang for their invaluable contributions during this collaboration.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was supported by the Beijing Municipal Administration of Hospitals’ Ascent Plan (Code DFL20150802), Acknowledgements-Beijing Municipal Commission of Health and Family Planning from National Clinical Research Center for Geriatric Disorders (Code No. PXM2017_026283_000002), Beijing Municipal Administration of Hospitals Clinical Medicine Development of Special Funding Support (Code: ZYLX201706), and Beijing Municipal Administration of Hospitals Clinical Medicine Development of Special Funding Support (Code: ZYLX201813).
