Abstract
Objective
Percutaneous cardiac catheterization has been used as a diagnostic tool and as a therapeutic option in neonates with congenital heart disease (CHD). This study aimed to evaluate the procedural and short-term follow-up data of newborns who underwent cardiac catheterization procedures.
Methods
This retrospective study reviewed demographic, diagnostic and clinical data from the medical records of newborns who underwent percutaneous transcatheter interventions to treat CHD.
Results
Forty-six newborns were included in the study. The median gestational week and weight were 35.0 weeks and 2723 g, respectively. The median time to the procedure was 7.6 days. Aortic and pulmonary balloon valvuloplasty, ductal stenting, atrial balloon/blade septostomy and coronary fistula embolization procedures were used. The overall success rate was 73.9% (34 of 46 patients) with a complication rate of 28.3% (13 of 46 patients). Eleven patients (23.9%) underwent reinterventions after initial catheterization. Five patients (10.9%) died in the first 48 h after their procedures.
Conclusions
Interventional cardiological procedures applied during the neonatal period provide alternative life-saving methods to surgery, especially in developing countries where surgical outcomes are poor and newborn mortality rates are high.
Introduction
Severe forms of congenital heart disease (CHD) occur in 2.5–3.0 per 1000 live birth infants and is a major cause of neonatal mortality and morbidity even when diagnosed antenatally. 1 Around 25% of neonatal deaths due to congenital malformations have been attributed to severe forms of CHD.2,3 Although many forms of CHD do not require immediate postnatal intervention, some forms require early surgery or catheterization in the neonatal period. 4 In particular, in neonates with ductus-dependent CHD, the immediate initiation of a prostaglandin infusion saves lives until palliative or therapeutic interventions can be scheduled. 5 If early diagnosis and interventions are lacking, certain forms of CHD can cause severe morbidity and mortality, including death, multiorgan failure and brain damage. 6 Recent advances in interventional paediatric cardiology and neonatal intensive care techniques have improved survival. 7 Percutaneous cardiac catheterization is increasingly used both diagnostically and therapeutically in neonates; in some cases (e.g. critical pulmonary stenosis), it is the first-line therapy. 8 In neonates, less invasive interventions are preferred because open heart surgery cannot be performed at all centres and is associated with a high mortality risk, especially in developing countries. 9 Currently, percutaneous cardiac interventions afford higher success rates with lower morbidity compared with surgery in newborns in poor general condition. 10
This study retrospectively evaluated the demographic characteristics, diagnoses, procedures, complications and early outcomes of newborns who underwent interventional cardiological procedures between January 2014 and December 2016 in a neonatal intensive care unit (NICU) at a tertiary care centre in Turkey.
Patients and methods
Patient population
This retrospective study reviewed data on newborns who underwent percutaneous transcatheter interventions to treat CHD when hospitalized in the NICU of the Department of Paediatrics, Division of Neonatology, Faculty of Medicine, The University of Gaziantep, Gaziantep, Turkey between January 2014 and December 2016. Patients who underwent patent ductus arteriosus closure, percutaneous temporary pacemaker implantation or diagnostic catheterization were excluded.
The study was approved by the Gaziantep University Ethics Committee of Clinical Research, Gaziantep, Turkey (no. 2016/336). Written informed consent was obtained from the parents or guardians of all patients.
Data collection
Demographic data, diagnoses, clinical data, echocardiographic and angiographic results, transcatheter procedure types used, procedural success, complications, length of NICU stay, reasons for surgery and any need for a second catheterization were retrieved from the medical records. Standard echocardiography was performed on all patients both before and after their percutaneous transcatheter procedures.
A prostaglandin E1 infusion was used to maintain arterial duct patency in patients with ductus-dependent CHD; the dose was 0.05–0.1 µg/kg per min. If severe cyanosis redeveloped, the prostaglandin infusion was resumed. Catheterization was performed under deep sedation with midazolam or general anaesthesia for intubated patients. Arterial and venous vascular access was achieved using the Seldinger technique. Surgical or transcatheter reintervention was performed if the peripheral oxygen saturation fell below 75%. For patients requiring ductal stenting, heparin at a dose of 20–28 U/kg per h administered as an intravenous continuous infusion was initiated and maintained for 24 h after the procedure followed by oral aspirin at 3–5 mg/kg per day.
Statistical analyses
All statistical analyses were performed using the Statistical Package for Social Sciences, version 25.0 (IBM Corporation, Armonk, NY, USA). Quantitative variables are shown as median (range) and categorical variables are shown as n of patients (%).
Results
Forty-six neonates who underwent interventional cardiac catheterization in the NICU between January 2014 and December 2016 were enrolled in the study. Of these, 26 patients (56.5%) were male and 20 (43.5%) were female. The median gestational period was 35.0 weeks (range, 33–40 weeks). The median infant weight was 2723 g (range, 1800–4000 g) and the median time to the procedure was 7.6 days (range, 1–22 days). Five patients (10.9%) were born at Gaziantep University Medical Faculty Hospital and 41 (89.1%) were referred from other hospitals. Only eight patients (17.4%) were prenatally diagnosed with CHD. The prenatal and postnatal echocardiographic diagnoses were identical. Of the 46 patients, nine patients (19.6%) underwent aortic balloon valvuloplasty or angioplasty (ABV-ABA), nine (19.6%) had pulmonary balloon valvuloplasty (PBV), 24 (52.2%) had ductal stenting (DS), three (6.5%) had atrial balloon/blade septostomy and one (2.2%) had coronary fistula embolization with an overall success rate of 73.9% (34 of 46).
Of the ABV-ABA patients, three had critical aortic valve stenosis and six had coarctation of the aorta (Table 1). The median age of this group at the time of the procedure was 13.4 days (range, 5–22 days) and the median weight was 3.1 kg (range, 2.2–3.8 kg). All patients were first admitted to the emergency ward or the paediatric cardiology outpatient clinic; none had been prenatally diagnosed. Four of the nine patients experienced cardiovascular collapse and heart failure during admission and required both a prostaglandin E1 infusion and inotropic support. Technical success was achieved in seven of the nine patients. Partial success was achieved in one (peak residual gradient: 60 mmHg) but the other failed coarctatic segment dilatation and was referred for surgical repair. One patient developed a transient atrioventricular (AV) block during the procedure, but no mortality was noted. The median NICU stay was 6.8 days (range, 2–14 days).
Demographic characteristics and procedural details of neonatal patients who underwent aortic balloon valvuloplasty or angioplasty (n = 9).

GW, gestational week; PGE1, prostaglandin E1; NICU, neonatal intensive care unit; Cr AS, critical aortic stenosis; Co Ao, coarctation of the aorta.
A total of nine patients underwent PBV. Of these, eight had critical pulmonary valve stenosis/near-atretic pulmonary valve issues and one had tetralogy of Fallot (Table 2). The median postnatal age at the time of the procedure was 2.7 days (range, 1–5 days) and the median weight was 2.9 kg (range, 1.9–4.0 kg). Prostaglandin E1 infusions were commenced in five patients prior to the procedure because of deep cyanosis and metabolic acidosis. No patient required additional treatment after the first session or repeat catheterization. There was no need for continuation of the prostaglandin E1 infusion. Procedural complications developed in three patients, of which one was an asymptomatic right ventricular outflow tract perforation and the other two patients experienced minor arrhythmias. The median NICU stay was 17.8 days (range, 2–80 days).
Demographic characteristics and procedural details of neonatal patients who underwent pulmonary balloon valvuloplasty (n = 9).

GW, gestational week; PD, prenatal diagnosis; PGE1, prostaglandin E1; NICU, neonatal intensive care unit; CPS, critical pulmonary stenosis; TOF, tetralogy of Fallot.
A total of 24 neonates underwent ductal stenting (Table 3). Their median age was 5.4 days (range, 1–21 days) and their median weight was 2.9 kg (range, 1.8–4.0 kg) at the time of the procedure. Ductal stenting was successfully achieved in 14 patients (58.3%). Additional interventions or responses to emergencies were required for eight neonates during the same session; three required drainage of haemorrhagic pericardial effusions, one required a pacemaker, two required a balloon atrial septostomy, and three required the repair of the pulmonary valve perforation/valvuloplasty. Eleven patients underwent reinterventions because of the failure of the initial ductal stenting or the persistence/worsening of cyanosis during the NICU stay. Of these 11 patients, seven underwent surgical systemic-to-arterial shunting, two underwent PBV, one underwent balloon atrial septostomy and one received stent revision and thrombolysis. The median NICU stay was 14.6 days (range, 2–42 days).
Demographic characteristics, procedural details and a summary of the clinical course of neonatal patients who underwent ductal stenting (n = 24).
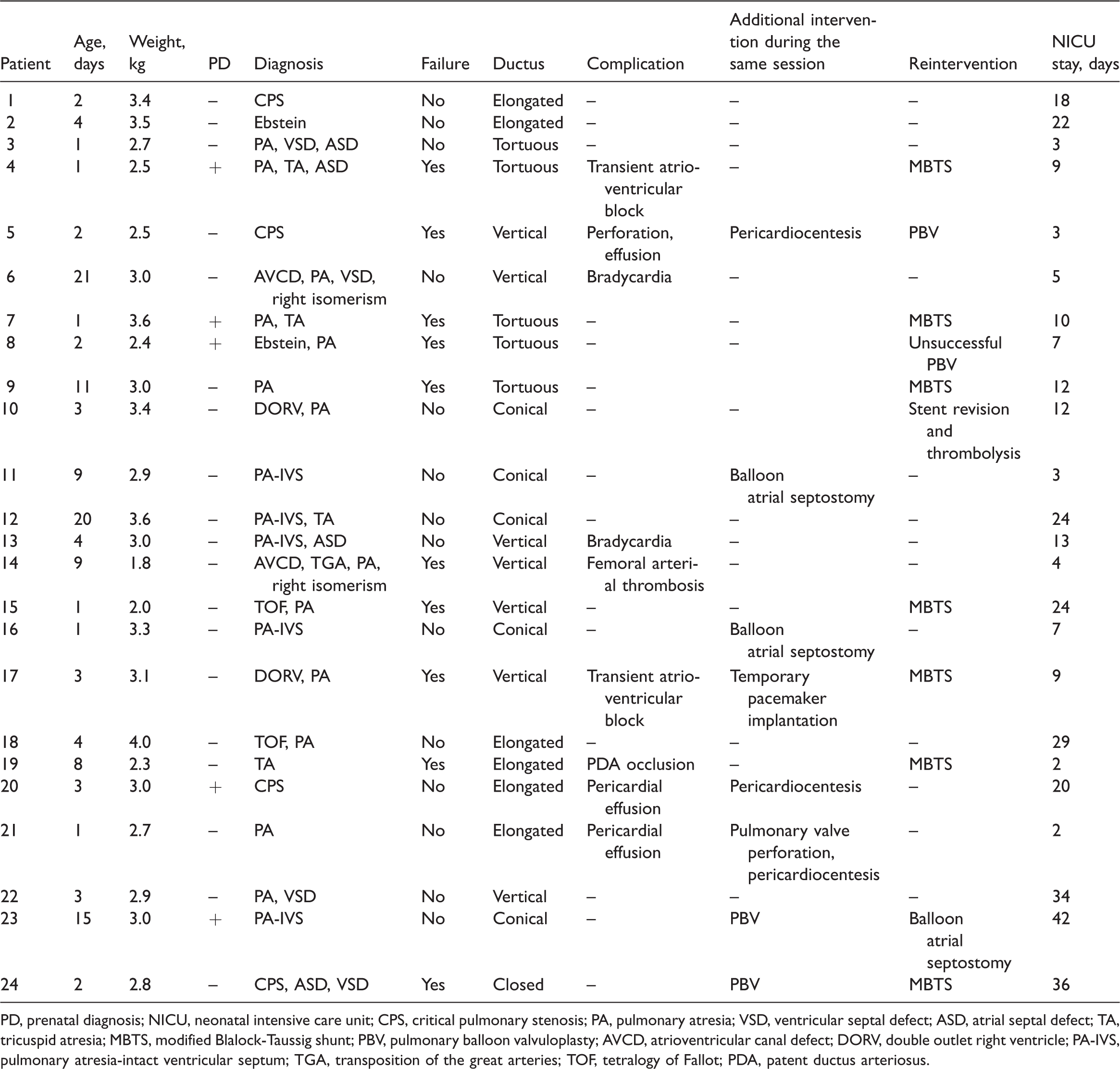
PD, prenatal diagnosis; NICU, neonatal intensive care unit; CPS, critical pulmonary stenosis; PA, pulmonary atresia; VSD, ventricular septal defect; ASD, atrial septal defect; TA, tricuspid atresia; MBTS, modified Blalock-Taussig shunt; PBV, pulmonary balloon valvuloplasty; AVCD, atrioventricular canal defect; DORV, double outlet right ventricle; PA-IVS, pulmonary atresia-intact ventricular septum; TGA, transposition of the great arteries; TOF, tetralogy of Fallot; PDA, patent ductus arteriosus.
Three patients underwent atrial balloon/blade septostomy. Two were diagnosed with transposition of the great arteries (TGA) and one with hypoplastic left heart syndrome. One TGA patient was septic and died 3 days after catheterization while waiting for surgical repair; the other TGA patient was referred to a cardiac centre for surgery. The patient with a hypoplastic left heart syndrome died on postnatal day 20 from multiorgan failure.
Only one patient was diagnosed with a congenital cameral fistula and heart failure; coil embolization was successful on postnatal day 14 (weight, 2.9 kg).
Thirteen of 46 patients (28.3%) developed complications during catheterization. Most of these were minor (i.e. not life-threatening). They are summarized in Tables 1–3. The most common complication was a transient AV block. Pericardiocentesis was performed during the same session if required. Only one patient required a temporary pacemaker.
Five of 46 patients (10.9%) died in the first 48 h after their procedures and ductal stenting was performed in all (Table 4). All of these patients either developed complications during catheterization or required emergency surgery; and their general condition was poorer than that of the survivors.
Demographic characteristics and procedural details of neonatal patients who died within the first 48 h after the procedures (n = 5).
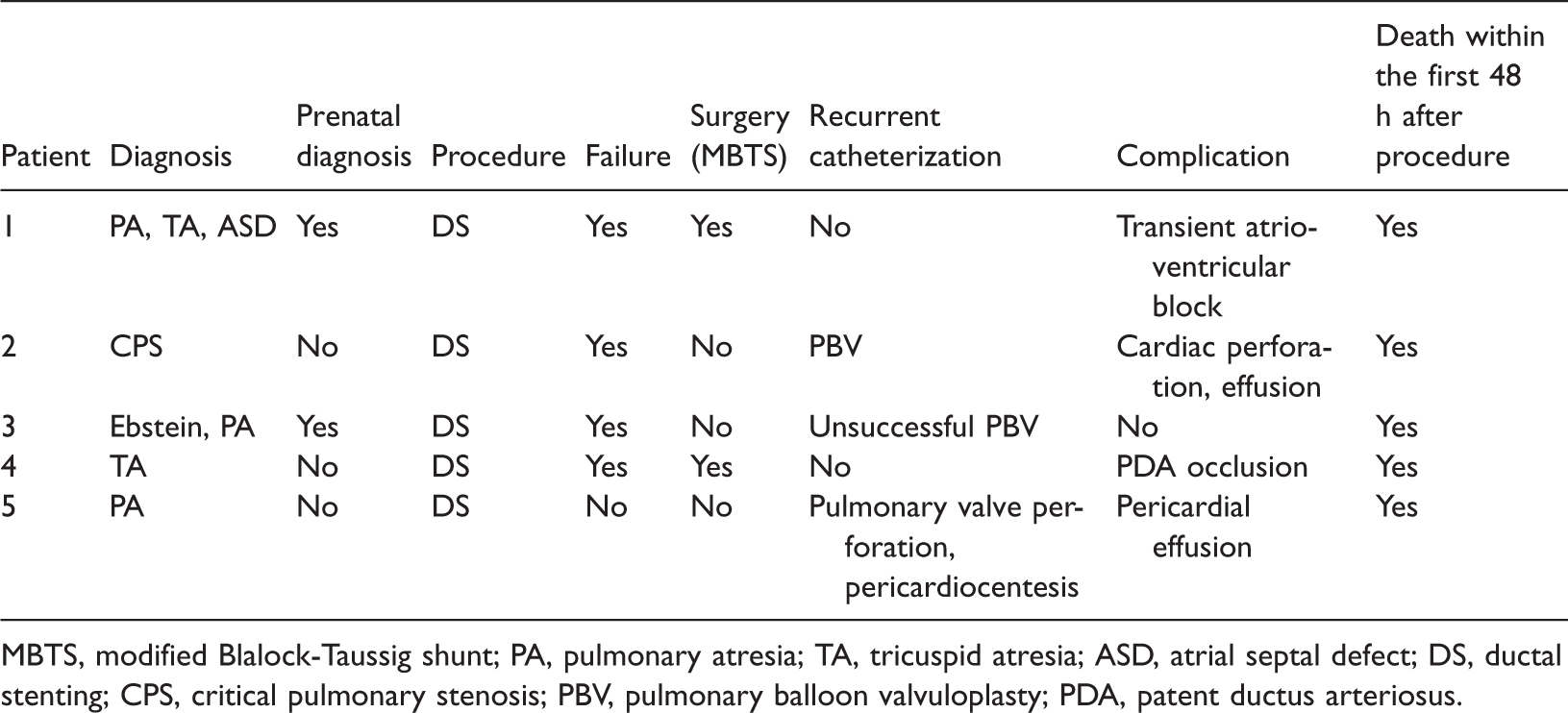
MBTS, modified Blalock-Taussig shunt; PA, pulmonary atresia; TA, tricuspid atresia; ASD, atrial septal defect; DS, ductal stenting; CPS, critical pulmonary stenosis; PBV, pulmonary balloon valvuloplasty; PDA, patent ductus arteriosus.
Discussion
Not all patients with CHD are suitable candidates for surgery, which is contraindicated in those of low birth weight, those with a complex cardiac anatomy, infants in poor general condition, and those with comorbid congenital anomalies. 11 Transcatheter treatment of CHD has become popular in recent years with improvements in surgical techniques and pre- and post-intervention intensive care. Newborn survival prior to total surgical repair has increased significantly. 12 Apart from being less invasive than surgery, transcatheter interventions afford the advantages of a short hospital stay, repeatability, palliative effects and no scarring. 13 Catheter-based therapies are good alternatives to surgery both in terms of initial palliation and cure. 14
This current retrospective study described the experience of neonates with CHD who underwent transcatheter cardiac interventions at a tertiary care centre. This retrospective study evaluated the procedures, success rates, complications, mortality rates and short-term follow-up data. Forty-six neonatal patients underwent either ABV/PBV, balloon angioplasty to treat coarctation of the aorta, stent placement in arterial ducti, balloon/blade atrial septostomy or an embolization of a cameral fistula between January 2014 and December 2016.
In patients with critical pulmonary stenosis, the pulmonary blood flow is mostly ductal-dependent. Thus, PBV with or without stent placement constitutes rescue therapy. In some cases, if interventional cardiologists cannot get past the valve, surgery is required. In this current study, the success rate was 100% in the nine affected patients, no additional intervention was required and the hypoxaemia did not persist. Complications developed in three of nine patients. A previous study reported a success rate of 98% in a PBV group; and ductal stenting was required in 20 of 56 patients (in the same or a subsequent session) because of persistent hypoxaemia. 15
The use of balloon angioplasty to treat native aortic coarctation and critical aortic stenosis remains controversial in neonates because restenosis after initial catheterization may trigger a need for surgical repair. 16 Also, balloon angioplasty is limited by patient size. Neonatal ABA is effective but associated with high risks of complications, death and suboptimal outcomes. 17 Since there is a lack of a neonatal cardiac surgery centre in our hospital, transcatheter balloon angioplasty was the preferred method for these patients. This also results in reduced hospitalization and procedure durations and reduced invasiveness. 18 In haemodynamically-sick newborns, balloon angioplasty allows for a faster recovery. 19 The success rate in the current study was 77.8% (seven of nine patients). To date, no patient has required coarctation dilatation or surgical repair. A meta-analysis of nine studies comparing the outcomes of surgery versus balloon angioplasty for coarctation showed that the short-term outcomes were comparable, but surgery was better in the mid- and long-term. 20
The most frequently applied procedure was ductal stenting (52.2%; 24 of 46 patients). A ductal stent facilitates biventricular circulation and this is the final outcome in those with ductus-dependent CHD. The success rate in the current study was 58.3% (14 of 24 patients) and the complication rate 37.5% (nine of 24 patients). Five patients died within 48 h of their procedures. Most developed complications during the procedures or required urgent shunt surgery after failure of the intervention. All were haemodynamically unstable because of primary disease and were at a high risk of mortality.
If technically possible, transcatheter stent placement is preferred to ductal stenting in our institution. Modified Blalock-Taussig shunt (MBTS) placement is the most commonly used palliative procedure for infants with ductal-dependent pulmonary flow. 21 Although MBTS shunting generally yields reliable and regulated pulmonary blood flow, the risks of mortality and morbidity are high, as are those of prolonged intubation, bleeding, the need for transfusions and inotropic agents, sepsis, phrenic or vagal paralysis, pulmonary branch distortion, shunt occlusion and pulmonary hypertension. 22 Recent innovations in percutaneous CHD treatment use different techniques or hybrid approaches, especially in neonates with ductal-dependent pulmonary flow. 23 A single-centre study from Turkey evaluated the early and mid-term outcomes of 13 patients who underwent ductal stenting and suggested that this was a useful nonsurgical alternative to corrective or palliative surgery. 24 Another study compared ductal stenting and a systemic pulmonary artery shunt procedure in 29 newborns (13 DS and 16 shunted patients) and reported similar success rates, but surgery was associated with a significantly higher complication rate, a longer hospital stay and a greater need for postoperative ventilation. 25
All transcatheter cardiac procedures, both diagnostic and interventional, are associated with risks. The overall complication rate in the current study was 28.3% (13 of 46 patients). Few studies have reported the procedural complications of unselected transcatheter interventions. One study reported only three complications in 20 infants weighing less than 2500 g. 26 Another study reported 135 cases with one or more complication among 964 infants (14%) catheterized at < 6 months of age. 27 It was emphasized that adverse events were more likely in younger patients. 28 The higher rate of complications in the current study was probably due to the fact that the study only included neonates. In addition, most of the patients in the current study did not have a prenatal diagnosis and they were admitted to the emergency department with circulatory collapse and shock. To improve the haemodynamic state of these patients, interventional cardiac procedures were performed under urgent conditions. These patient-related conditions explain why the complication rate in the current study was high. This current study also included benign self-limiting minor arrythmias as a complication, which would have contributed to the high complication rate. The most common complications of cardiac catheterization are minor arrhythmias, bleeding/haematomas of/on the entry site, arterial/venous thrombosis, cardiac perforation, exposure to ionizing radiation and death. 27 Arrhythmia was the most common complication in the current study. Arrhythmia associated with catheter manipulation can be well-tolerated, but medications or a pacemaker are sometimes required. The complication rate is lower than that of open-heart surgery in newborns with CHD. 29 A previous study reported that almost one-third of patients admitted for CHD surgery had one or more complications. 30 The authors evaluated 1597 patients who underwent open-heart surgery at <30 days of age and 604 (38%) developed complications. 30 Thus, although the complication rate was high in the current study, it was lower compared with that associated with open-heart surgery. 30 Another study considered that CHD patients of all ages can expect to undergo safe procedures with a minimal risk of serious complications. 31 Complication rates should gradually decrease with advances in procedural techniques, miniaturization of equipment, improvements in imaging technologies and increasing clinical experience. Transcatheter interventions should become increasingly applied to smaller newborns.
An analysis of outcomes of major cardiac operations in low weight neonates reported that the overall surgical mortality rate was 18% when neonates weighing <2500 g underwent early surgery to treat CHD, but many minor and major complications were encountered (53% of patients). 32 Low weight is an independent risk factor for both mortality and resource utilization after surgery; it is best to employ nonsurgical methods in such patients. 33
In conclusion, interventional cardiological procedures applied during the neonatal period are alternative life-saving methods used both for urgent correction of clinical conditions and initial palliative therapy prior to surgery. Given the wide variability of cardiac anatomy and defect size, catheter-based therapy must be individualized for each patient. In low-to-middle income countries, centres that can perform surgical correction are generally few in number and always full. Also, as preoperative weight gain is essential for corrective surgery, emergency palliative care interventions in dedicated NICUs are of great importance, particularly in developing countries.
Footnotes
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
