Abstract
Objective
To evaluate the efficacy of pre-injection of butorphanol on etomidate-induced myoclonus during anesthesia induction.
Methods
Randomized controlled trials (RCTs) of the ability of butorphanol to prevent etomidate-induced myoclonus were collected by searching PubMed, Cochrane Library, CNKI, and WanFang databases, from the day of database establishment until May 2017. The literature was screened independently by two evaluators, and the data were then extracted and independently evaluated. Finally, meta-analysis was performed by using RevMan 5.2 software.
Results
Eight RCTs were analyzed. The results of meta-analysis showed that: 1. compared with the control group, butorphanol was effective in preventing etomidate-induced myoclonus [RR = 0.15, 95% CI: 0.11, 0.21]; 2. butorphanol was effective in preventing mild, moderate, and severe etomidate-induced myoclonus [RR = 0.40, 95% CI: 0.25, 0.63; RR = 0.15, 95% CI: 0.08, 0.27; and RR = 0.04, 95% CI: 0.01, 0.09]; 3. butorphanol did not increase the incidence of dizziness and nausea associated with etomidate.
Conclusions
Butorphanol could reduce the incidence and degree of etomidate-induced myoclonus. Notably, it did not increase the incidence of dizziness and nausea associated with etomidate.
Introduction
As a non-barbiturate sedative drug, etomidate is recommended for anesthesia induction, particularly to control hemodynamic instability, because it has a less dramatic cardiovascular effect; however, etomidate causes intravenous pain and myoclonus. Currently, the use of etomidate fat emulsion has reduced the degree of injection pain. In the absence of pretreatment, the incidence rate of etomidate-induced myoclonus remains as high as 50% to 80%. 1 Research regarding the clinical prevention of myoclonus caused by etomidate has primarily comprised the use of opioid drugs, such as fentanyl, sufentanil, and remifentanil;2–4 notably, large doses of opioid drugs may reduce etomidate-induced myoclonus, but might induce adverse reactions, such as apnea and chest wall myotonia.
Butorphanol, a type of opioid, is a competitive inhibitor of both κ-opioid and μ-opioid receptors. Recently, there have been numerous studies regarding the use of butorphanol in the prevention of etomidate-induced myoclonus. This study comprised a meta-analysis of the validity and safety of butorphanol for the prevention of etomidate-induced myoclonus.
Subjects and methods
This study was approved by the ethics committee of Zhaoqing Medical College (Zhaoqing City, China). The requirement for informed consent was waived owing to the retrospective nature of the study.
Subjects in included studies
1) Patients with anesthesia induced by etomidate.
Inclusion and exclusion criteria
Inclusion criteria
1) Test group was treated with butorphanol, while the control group was administered placebo; 2) Study types were limited to randomized controlled trials; 3) Main outcome indicators were limited to the incidence of myoclonus. Secondary outcome indicators were limited to the incidence of different degrees of myoclonus, as well as incidences of dizziness and nausea.
Exclusion criteria
1) Studies that comprised clinical research with design defects or reported incomplete data; 2) Duplicate articles and documents where data were unavailable; 3) Studies with research design defects (e.g., random method error or statistical method error).
Retrieval strategy
The computer retrieval method was used to collect relevant RCT data regarding prevention of etomidate-induced myoclonus with preliminary butorphanol injections; databases searched were PubMed, Cochrane Library, CNKI, and WanFang, from database inception through May 2017. Search terms included: butorphanol, etomidate, and myoclonus; retrieval was performed by combinations of subject words and free words. Only randomized controlled trials were included. In addition, unpublished relevant literature was searched where possible.
Literature screening and data extraction
Two researchers independently searched the literature, extracted the data, and evaluated the risks involved in the included studies. Disagreements were resolved through discussion during cross-checking. The researchers contacted the original authors for verification in cases of incomplete or unclear data.
Quality evaluation of literature
The Jadad scale was used to evaluate the quality of the screened randomized controlled studies; these studies were evaluated with respect to randomization, blinding, withdrawal, and loss to follow-up, with a total score of 5 points. The PRISMA guidelines were applied in this meta-analysis.
Statistical method
Meta-analysis was performed with RevMan 5.2 software; the q test and I2 statistics were used to evaluate heterogeneity among all studies. If the heterogeneity among studies was small (I2 ≤ 50%), the fixed model was selected to merge effect values through the backward variance method. If the heterogeneity was large (I2 > 50%), the random model was chosen to merge effect values. Potential publication bias was evaluated through a funnel map.
Results
Retrieved results
Upon initial application of the search method, 123 references were retrieved. After reading the titles, abstracts, and full texts, eight studies were finally included.5–12 The selection process and results are shown in Figure 1.
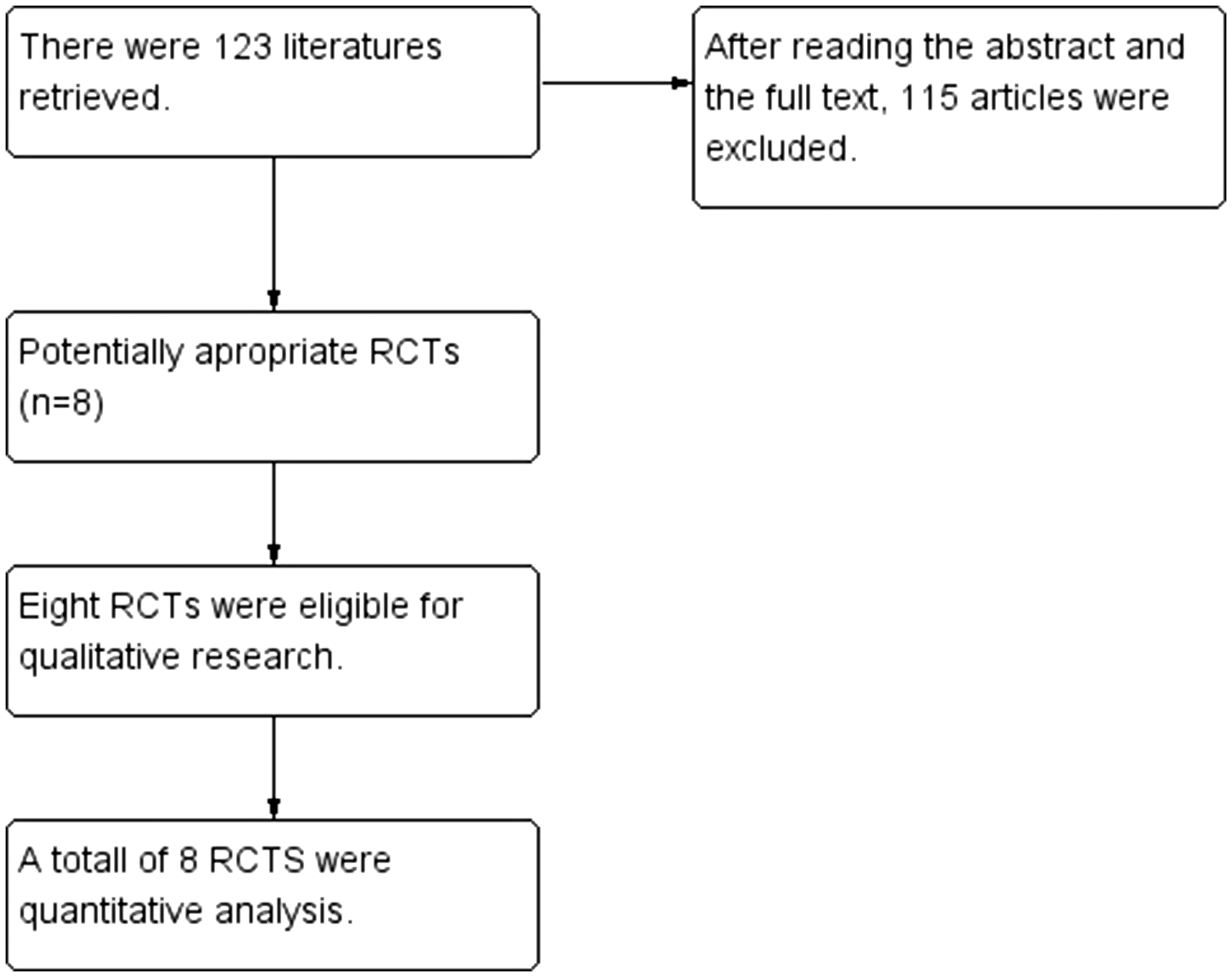
Flow diagram.
The basic condition and quality evaluation of literature
The basic information and quality scores of the clinical studies included in the meta-analysis are shown in Table 1.
Characteristics of studies included in the meta-analysis.

Meta-analysis results
Total myoclonus events
There were eight studies5–12 regarding the use of butorphanol to prevent etomidate-induced myoclonus in randomized controlled trials (heterogeneity I2 = 0%). In fixed effects model analysis, butorphanol was effective in preventing overall etomidate-induced myoclonus, compared with the control group (RR = 0.15, 95% CI: 0.11, 0.21; P<0.00001) (Figure 2).

Total myoclonus events.
Mild myoclonus events
There were seven studies5–10,12 regarding the use of butorphanol to prevent etomidate-induced mild myoclonus in randomized controlled trials (heterogeneity I2 = 0%). In fixed effects model analysis, butorphanol was effective in preventing mild etomidate-induced myoclonus, compared with the control group (RR = 0.40, 95% CI: 0.25, 0.63; P<0.0001) (Figure 3).

Mild myoclonus events.
Moderate myoclonus events
There were seven studies5–10,12 regarding the use of butorphanol to prevent etomidate-induced moderate myoclonus in randomized controlled trials (heterogeneity I2 = 0%). In fixed effects model analysis, butorphanol was effective in preventing moderate etomidate-induced myoclonus, compared with the control group (RR = 0.15, 95% CI: 0.08, 0.27; P<0.00001) (Figure 4).

Moderate myoclonus events.
Severe myoclonus events
There were seven studies5–10,12 regarding the use of butorphanol to prevent etomidate-induced severe myoclonus in randomized controlled trials (heterogeneity I2 = 0%). In fixed effects model analysis, butorphanol was effective in preventing severe etomidate-induced myoclonus, compared with the control group (RR = 0.04, 95% CI: 0.01, 0.09; P<0.00001) (Figure 5).

Severe myoclonus events.
Incidences of dizziness and nausea
There were three studies regarding the incidences of dizziness and nausea,5,7,12 which showed no significant heterogeneity (I2 = 0%). In fixed effects model analysis, butorphanol and control groups showed insignificant differences in the incidences of etomidate-associated dizziness and nausea (Figure 6).
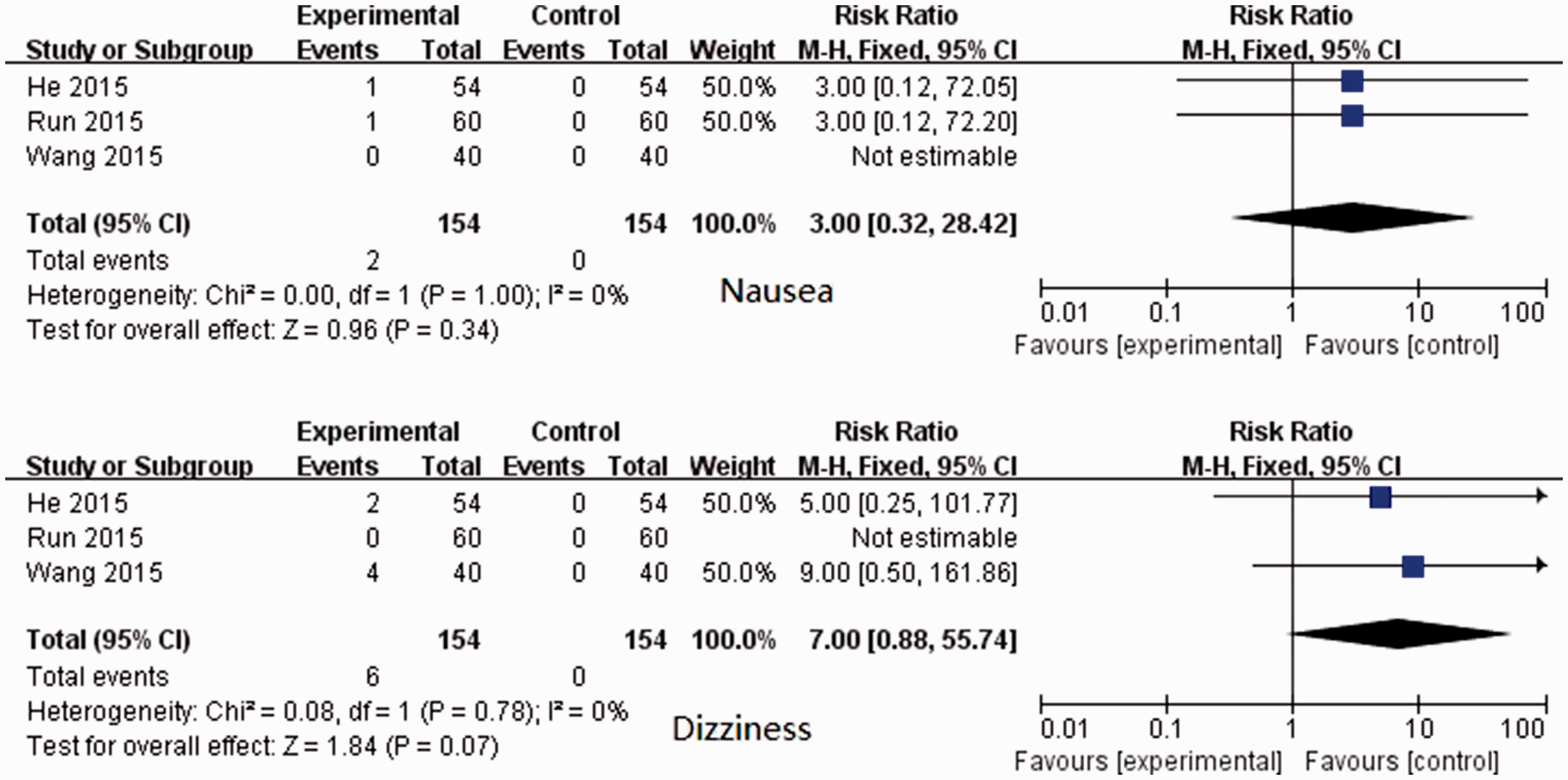
Incidence of dizziness and nausea.
Publication bias and sensitivity analysis
Publication bias was evaluated by using a funnel graph, which showed no publication bias among the eight included randomized controlled trials; the results showed no significant changes upon exclusion of any clinical study, indicating a high degree of reliability.
Discussion
This meta-analysis showed that butorphanol can be effective in the prevention of multiple degrees of etomidate-induced myoclonus, without dizziness or vomiting.
Etomidate primarily provides an anesthetic effect through its action on the GABA receptor; however, the neural mechanisms that cause myoclonus are unclear. Notably, some studies have suggested that myoclonus is similar to a convulsive attack. 13 Alternatively, it might suppress the spinal cord, or inhibit the cerebral cortex and subcutaneous structures. 1 Wang et al. 14 speculated that etomidate might compete with endogenous dopamine to bind with dopamine receptors in areas such as the melanin and striatum, thus constituting competitive inhibition; this might cause symptoms similar to the reduction of endogenous dopamine, which is characterized by myoclonus.
Butorphanol can bind to GABA receptors, which might inhibit reticular activation of the central nervous system. Although studies of the mechanism of etomidate-induced myoclonus are ongoing, 15 the neurological mechanism remains unclear, as noted above. Related studies have confirmed that etomidate-induced myoclonus may result from disinhibition of the cerebral cortex, similar to the phenomenon of “restless leg syndrome”; notably, epilepsy patients do not exhibit this phenomenon. Butorphanol binds to μ-opioid and κ-opioid receptors, at a ratio of 1:4:25, 16 as well as the primary excitatory κ receptors. Several studies have shown that κ receptors play an important role in anticonvulsion. 17 Studies of butorphanol used for anticonvulsion have shown that butorphanol interacts with multiple neurotransmitter systems, such as opioid receptors, ZBD-GABA (A) ion channel complexes, GABA (B) receptors, and NMDA channels; 18 this suggests that butorphanol might reduce the incidence of myoclonus by means of interactions with these receptors.
The limitations of this meta-analysis include: (1) Data of eligible studies were not comprehensive, and baselines differed among studies—the conclusions could be strengthened by the addition of further studies; (2) There might have been differences among subject populations in different regions, as well as in drug dosage and delivery time, assessment of severity, and accuracy of the index; (3) There were few eligible studies, resulting in a small sample size.
In conclusion, butorphanol may be effective in preventing etomidate-induced myoclonus.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Footnotes
Funding
This research was supported by the Zhaoqing Science and Technology Innovation Guidance Project (No. 201624030202) and Guangdong Medical Research Foundation (No. A2018498).
