Abstract
Objective
This study was performed to evaluate the effects of propofol on the electroencephalogram (EEG) default mode network (DMN) in patients of advanced age.
Methods
Fifteen men aged >60 years (mean, 70 years) were selected. Propofol target-controlled infusion was performed under EEG bispectral index monitoring. The propofol target effect-site concentration, blood pressure, heart rate, and distributions and powers of the EEG spectrum were recorded in an awake state and under anesthesia. The EEG included seven bands: delta (0.5–3.5 Hz), theta (4.0–7.0 Hz), alpha-1 (7.5–9.5 Hz), alpha-2 (10–12 Hz), beta-1 (13–23 Hz), beta-2 (24–34 Hz), and gamma (35–45 Hz).
Results
From an awake state to anesthesia, the brain topographic map showed that the energies of delta, theta, alpha-1, alpha-2, and beta-1 were concentrated in the frontoparietal site, and the power increased significantly. The energy distribution of beta-2 was significantly decreased and the power significantly reduced. The energy distribution of gamma in the temporal lobe was also markedly decreased and the power significantly reduced.
Conclusions
This study revealed the changes in the spatial distribution and regional energy of the EEG DMD in men of advanced age from the awake state to the anesthetized state.
Introduction
Propofol is a short-acting intravenous anesthetic characterized by rapid and complete recovery and no accumulation after continuous infusion. After induction of anesthesia, the frequency of the electroencephalogram (EEG) is inhibited and the activity of neurons is significantly decreased as the drug concentration increases, and the typical erosive suppression waveform may occur. 1 However, quantification of the traditional EEG energy is mainly based on measurement of the frequency and amplitude of a single channel or one-by-one channel. The brain does not produce frequency changes corresponding to brain functions at a single point but instead produces regional brain function changes with the functional area as a unit. Therefore, we need to fully study and show changes in the EEG in a more comprehensive and intuitive way. The EEG default mode network (DMN) refers to the presence of a set of resting states in the brain when a subject closes his or her eyes in a quiet state, which is more active than a cognitive task. The DMN is employed to calculate the spectral powers of the region of interest, forming a three-dimensional brain color image. The DMN can reflect the default state of brain activity, and its integrity can be used to evaluate the consciousness level of patients with confusion of consciousness. 2
To date, the impact of anesthetics on EEG research has only been studied in adults; few reports involving patients of advanced age have been published. As the aged population grows, increasingly more older patients require surgical treatment. One study showed a negative correlation between propofol clearance and the central compartment volume and age in patients aged >60 years. 3 Older patients have a reduced tolerance and need for various narcotic drugs. In fact, changes in the anesthetic requirement are parallel to the rate of loss of cortical neurons, the rate of decrease in cortical neuron density, the absolute values of the decrease in the brain metabolic rate and cerebral blood flow, and the decrease in age-related neurotransmitter activity and related receptors. 4 These characteristics of older patients cause them to be more prone to postoperative cognitive dysfunction and postoperative mental disorder than younger patients.
Therefore, as a special group, individuals of advanced age have drawn increasingly more attention, and basic research of the effect of anesthetics on brain function in these patients is also increasing. This study was performed to explore the impact of propofol anesthesia on brain function in individuals of advanced age.
Materials and methods
Subjects and experimental conditions
Fifteen male volunteers (American Society of Anesthesiologists grade I or II) aged 60 to 78 years (mean, 70 years) participated in this study. Patients with cerebrovascular diseases (e.g., cerebral infarction, cerebral hemorrhage), Alzheimer’s disease, or a history of a psychological disorder and those who took psychiatric drugs were excluded. All patients provided written informed consent under the requirements of the Helsinki Declaration. This study was approved by the ethics committee of Capital Medical University [approval No. (2011) CMU (041)]. All subjects were identified as right-handed by the Edinburgh Handedness Questionnaire Survey. All subjects were required to complete various scales of psychological characteristics before the experiment to ensure that their mental state was within the normal range. These scales were the State Anxiety (SA) scale, Trait Anxiety (TA) scale, Fear Survey Schedule-II (FSS-II), General Self-Efficacy Scale (GSES), and Simplified Coping Style Scale (SCSS).
During this study, the subjects lay in bed and the room remained quiet with a room temperature of 22°C to 24°C. Electrocardiogram, noninvasive blood pressure, and peripheral oxygen saturation monitors were connected. Venous access was established in the right upper limb, and Ringer’s lactate solution was infused. The electrodes were arranged according to the 10/20 combined paradigm system, 5 with the double-lug electrode used as the reference electrode. A bispectral index (BIS) electrode was attached as required and connected with an A-200XP BIS monitor (Aspect Medical Systems, Norwood, MA, USA). Target-controlled infusion (TCI) of 500 mg of 1%W/V propofol (Batch ER 782; AstraZeneca, Milan, Italy) was started via a Diprifusor TCI system (AstraZeneca) with a Graseby 3500 syringe pump (Graseby, UK) at a rate of 4 µg/mL until anesthesia was achieved (BIS of 40). The EEG data were recorded throughout the whole course, and the BIS, blood pressure, heart rate, and target effect-site concentration per minute were recorded at the same time. During administration, the patient continuously inhaled pure oxygen through the mask with an oxygen flow rate of 5 L/minute, and the oxygen saturation was maintained at >95%.
EEG recording and pretreatment
The EEG treatment method was based on a previous study performed by our group. 6 The Al/AgCl electrode data on high-density 22-channel EEG and 2-channel electro-oculogram (EOG) data were collected continuously for 2 minutes in the awake and anesthetized states using the ANT EEG system (ANT Neuro, Enschede, the Netherlands). Figure 1 shows all electrode positions and names.

(a) Front view and (b) back view of the 10/20 22-channel EEG electrodes. Positions and names of the EEG recording electrodes are depicted: FP1, FP2, F7, F8, F3, F4, FZ, T3, T4, T5, T6, C3, C4, CZ, P3, P4, PZ, O1, O2, OZ, M1, M2, A1, and A2. EEG, electroencephalogram.
The EOG contaminated part of the scalp and was removed from the offline analysis. All EEG waves were recorded with an average reference value, but both sides were re-referenced offline (A1 + A2 on average). The EEG wave data were collected at 512 Hz, and the electrode impedance remained below 5 kΩ. The EEG data were filtered by a 0.16- to 100-Hz filter offline, and segmentation (2 s each), delineation, and false exclusion pretreatment were performed. The artifact suppression method includes the use of large amplitudes (over ±80 µV) to exclude cells, direct current bias, flicker, and slow eye movement consistent with EOG.
The extrapolated virtual value of the adjacent electrode was used to replace the “bad electrode.” After exclusion of EOG contamination and nonspecific illusion, the EEG wave data (cycle: 2 s) of each group were analyzed by fast Fourier transform (FFT) to obtain seven bands of EEG power (µv2). The seven bands were delta (0.5–3.5 Hz), theta (4–7 Hz), alpha-1 (7.5–9.5 Hz), alpha-2 (10–12 Hz), beta-1 (13–23 Hz), beta-2 (24–34 Hz), and gamma (35–45 Hz). The above bands were defined using conventional International Federation of Clinical Neurophysiology guidelines rather than according to individual spectral characteristics.
For both the awake and anesthetized state, a 2-minute-long EEG wave was analyzed in 2-s units, resulting in a total of 60 cells. For each awake and anesthetized state, the mean value of the effective cells was calculated for FFT analysis using ASA4.7.3.1 software (ANT Neuro). The total mean value of the FFT plot at different stages of the brain topographic map (256 tones) and the average amplitude of the surface EEG waves were calculated using the three-dimensional “quasi-realistic” cerebral cortical model of the spline interpolation function. For each of the seven EEG frequencies, the scalp power spectrum was inserted with an interpolation from a 22-channel EEG, separating the maximum power point/electrode and calculating its value. The ranges of the maximum and minimum values of the EEG spectral power frequency were established by automatic scaling.
The total power (the sum of the spectral energy of the electrodes) of each EEG frequency in the region of interest (ROI) was calculated by the relative measured value of the seven frequencies in each state (awake and anesthetized) We converted the ROI of each brain topographic map to a standard value to obtain a comparable quantification of the field power and to define the spatial range of the main spectral operation with the field power of the ROI. The ROI was spatially separated by a region where the spectral power displayed in the electrode exceeded the critical effective value (EV), which was equal to 70.7% of the maximum value (EV = 0.707, Vmax), which was defined as the ROI effective energy. The EV was taken as 70.7% of the maximum value, and all EEG values were arranged from small to large. For statistical comparisons between different states or conditions, the ROI containing the electrode array was selected as the template. We calculated the sum of the electrode values in the ROI of each subject and performed a statistical analysis with its mean value, in which the dependent variable of interest was the average field power of the electrode array above the EV rather than the power of a single electrode.
Statistical analysis
All data were analyzed with SPSS for Windows, Version 16.0 (SPSS Inc., Chicago, IL, USA). The paired t test was used to assess the EEG power, blood pressure, heart rate, and BIS. A P value of <0.05 was considered statistically significant.
Results
Psychological health
All enrolled subjects had normal results on the psychological scales: 35 for the SA scale (39.71 ± 8.89), 39.67 for the TA scale (41.11 ± 7.74), 69.53 for the FSS-II (<300), 3.04 for the GSES (2.69 ± 0.57), 2.1 (1.78±0.52) for the positive SCSS, and 1.49 (1.59 ± 0.66) for the negative SCSS.
Effects of propofol on EEG
From the awake state to anesthesia, the systolic blood pressure significantly decreased from 137.06 ± 17.35 to 101 ± 11.77 mmHg, and the diastolic blood pressure significantly decreased from 79.67 ± 11.61 to 71.67 ± 11.89 mmHg (P < 0.001). The heart rate significantly increased from 65.6 ± 10.93 to 71.67 ± 11.89 beats/minute (P < 0.001). The target effect-site concentration under anesthesia was 3.19 ± 0.56 µg/mL. Figure 2 shows that the BIS significantly decreased from 94.13 ± 4.36 to 33.13 ± 6.78 (P < 0.001). The time from the awake state to anesthesia was 7.33 ± 2.19 minutes.

BIS and interval from the awake to anesthetized state. The decrease in the mean BIS from the awake to anesthetized state in the patient group is depicted: the x-axis represents the change from the awake to anesthetized state for all patients, and the y-axis represents the mean BIS. BIS, bispectral index.
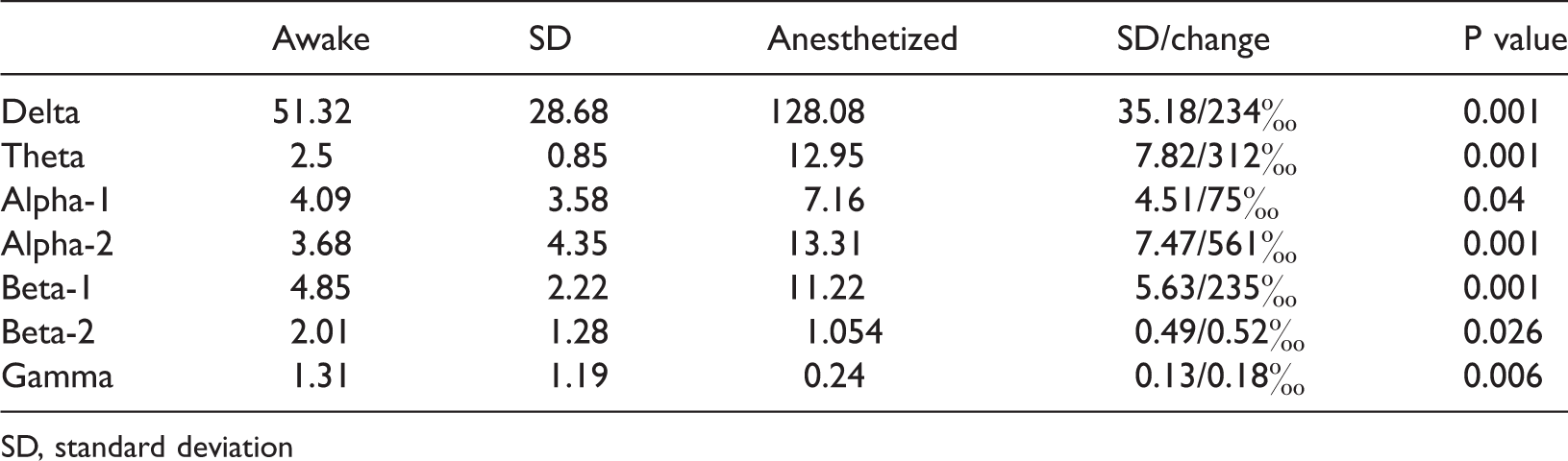
Figure 3 exhibits the field powers of the seven frequency bands distributed on brain topographic maps from the awake state to the anesthetized state. Table 1 shows that the seven band field powers significantly changed from the awake state to the anesthetized state (P < 0.05). From the awake state to anesthesia, the brain topographic maps showed that the energies of delta, theta, alpha-1, alpha-2, and beta-1 were concentrated in the frontoparietal site, and the power increased significantly (P < 0.05). Meanwhile, the energy distribution of beta-2 and the power significantly decreased (P < 0.05). The energy distribution of gamma in the temporal lobe also markedly decreased, and the power was significantly reduced (P < 0.01).

Field powers of the seven frequency bands distributed on brain topographic maps from the awake to anesthetized state. Topographic spectral mapping of the delta, theta, alpha-1, alpha-2, and beta-1 field powers are distributed in the frontoparietal areas. These field powers showed marked enhancement from the awake state to the anesthetized state. The beta-2 field power was mainly distributed in the frontoparietal area, and the gamma field power was distributed in the temporal area. In both areas, a marked reduction in the field power from the awake to anesthetized state was observed.
Seven band field powers from the awake state to the anesthetized state.
SD, standard deviation
Discussion
Several studies have shown that the prefrontal region of the brain, which is the main site of action for propofol, may exhibit an amplitude increase and energy aggregation of different EEG frequencies, mainly involving the delta waves, 7 beta waves, and alpha waves.8,9 However, our results are somewhat different. The three main reasons for the differences between the results of previous studies and those of our study are as follows. First, the EEG recording method was different. Previous studies used the traditional method of EEG recording, which detects increased amplitudes of individual EEG frequencies; this method only calculates the changes in such frequencies and does not fully reflect the EEG changes in all frequency bands or clearly show the distribution area of different frequency bands in the brain. The EEG DMN used in the present study can detect the EEG changes of all seven frequency bands; it is not limited to detection of only an increased amplitude of the band. Therefore, this method can more fully and accurately indicate the EEG distribution and changes in the brain. Second, some studies used propofol in combination with other sedatives, opioids, or muscle relaxants, which have an impact on the effect of propofol. 10 Finally, the anesthetic administration routes differed. The main intravenous administration methods for general anesthetics are single administration, constant-speed infusion, and TCI. Previous studies were based on a single administration, in which a stable plasma concentration and anesthetic cannot be maintained; additionally, the EEG might exhibit a series of different changes as the plasma concentration fluctuates. Compared with the traditional intravenous modes of administration, the use of TCI technology is more accurate and allows for easier maintenance of a stable depth of anesthesia. 11 In addition, a good correlation exists between the BIS and drugs acting on the cerebral cortex, such as propofol, midazolam, and sevoflurane; thus, the BIS can be used to assess the depth of anesthesia. 12 Therefore, through TCI and BIS monitoring, a stable anesthetic depth can be achieved using propofol with more accurate recording of EEG changes. Moreover, propofol metabolism can be affected by age, sex, weight, and ethnic factors, among which age is an important influencing factor. Previous studies mostly involved adults, 13 but our study focused on subjects of advanced age as a special population.
The brain of older individuals undergoes great changes in anatomical structure and physiological function, which may correspondingly affect the EEG. This is mainly because the anatomical structure and functional status of the brain in older people is considerably different from that in young people as follows. First, both the thickness of the cerebral cortex and the overall structure decline in older individuals. 14 Second, the gray matter atrophies and white matter lesions appear between healthy and pathologically degraded tissue. 15 Third, older individuals have increased ventricular space. 16 Finally, skull and scalp atrophy may affect EEG conduction. Moreover, the drug metabolic capacity in older individuals is substantially decreased because of decreased organ function. Both the minimum alveolar concentration and the tolerance to propofol are reduced in patients of advanced age, 17 and these changes may be associated with the marked decline in GABA receptor tension associated with aging. 18 Nevertheless, no comprehensive and reasonable physiological explanation of the relationship between EEG changes and age has been established. Synchronous reduction of cortical synaptic density and cortical cells may be the main factors affecting the EEG in individuals of advanced age. 19 The hypnotic effect of propofol and the spectrum pattern in EEG differ between old and young patients. During induction, patients aged >70 years may reach a deeper EEG level than younger patients and require a longer time to reach deeper EEG phases and be restored to lighter EEG phases. 20 Additionally, our comparison of men of advanced age and young men in the EEG DMN closed-eye state showed that the delta, theta, alpha-2, and beta-1 wave powers were lower and the alpha-1 and gamma powers were higher in the older men than in the young men. Accordingly, the low- and medium-frequency EEGs of older individuals are weakened as a whole compared with those of young people, resulting in different reactions to propofol.
The central mechanism of action of propofol in general intravenous anesthesia remains incompletely understood. Many scholars have studied the effect of propofol on the EEG using different methods and have drawn some meaningful conclusions. Propofol, like other general anesthetics, acts on a variety of cortical and subcortical structures involving a variety of neuronal cell types and molecular targets that can produce changes in the EEG. The DMN is the brain’s default mode and can reflect the connection between brain anatomy and function. The default mode of the neural network reflects the brain’s level of consciousness in a normal state, and its integrity can be used as a sign of disturbance of consciousness. Studies have shown that the alpha wave frequency is correlated to the awake and quiet state when the eyes are closed, and the beta wave frequency is closely associated with the blood oxygen level of the DMN; 21 the ultra-slow frequency EEG wave (<0.1 Hz) is also related to the DMN activity. 22 Gamma wave energy size and synchronization can help maintain a sense of wakefulness. Some studies have suggested that gamma wave activity is decreased after anesthesia, 23 while others have shown an increase in gamma wave energy after anesthesia. 24 This contradiction may be derived from differences in the anesthetics and the depth of anesthesia, which lead to the nonidentity of drug action and thus affect the accuracy and comparability of study. In the present study, TCI was used to maintain a fixed depth of anesthesia under BIS monitoring conditions, which could more accurately reflect the effect of propofol on the EEG.
In conclusion, we used EEG DMN to study EEG changes in 15 men of advanced age with propofol anesthesia. The method was based on the spatial distribution and quantitative analysis of powers. The results showed that low-frequency EEG (0.5–23 Hz) accumulated in the frontal and parietal lobes of the brain after propofol anesthesia while the power significantly increased, and the spatial distribution and energy of high-frequency EEG (24–45 Hz) significantly decreased. The DMN can be used to qualitatively and quantitatively analyze the EEG in different states in a comprehensive way, which is an effective method to further study the mechanism of action of general anesthetics. For a more comprehensive analysis of the mechanism of general anesthetics, more detailed observations of EEG changes may be made to choose different types of general anesthetics and different depths of anesthesia in the future.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
