Abstract
Schwannomas are tumours that arise from Schwann cells of the peripheral nerve sheath and rarely occur in the retroperitoneum. We report a 45-year-old woman who presented with a 2-year history of continuous progressive right-sided lower back and dull flank pain radiating into her posterolateral thigh. Abdominal magnetic resonance imaging showed a homogenous soft-tissue tumour with thick capsular lining, which lay in the right retroperitoneum. The tumour was removed at surgery. A histological examination confirmed the diagnosis of benign encapsulated cellular schwannoma. Complete tumour excision should be regarded as the treatment of choice for benign retroperitoneal schwannomas. Successful treatment of these tumours requires thorough preoperative planning and a multidisciplinary approach.
Keywords
Introduction
Schwannomas (neurilemmomas) are soft-tissue tumours that arise from Schwann cells of the peripheral nerve sheath and predominantly occur in women aged between their 2nd and 5th decades. These tumours are typically solitary and encapsulated, and are slow growing and noninvasive. Although schwannomas can occur anywhere in neural tissue where Schwann cells are present, they are usually found in the head, neck, and flexor surfaces of the extremities, and rarely found in the posterior mediastinum. 1 Schwannomas are not commonly larger than 5 to 6 cm in diameter. The histological nature of schwannomas is determined by the presence of high and low cellularity areas (Antoni A and B tissue, respectively). 2 The majority of schwannomas are benign, although malignant tumours can occur usually in the presence of Von Recklinghausen’s disease (in up to 60% of cases). 3
Schwannomas rarely occur in the retroperitoneum, and these comprise 1% to 10% of all primary retroperitoneal tumours. 4 Among schwannomas, only approximately 3% (0.7% are benign and 1.7% are malignant tumours) are reported to be located in the retroperitoneum.4,5 Retroperitoneal schwannomas (RSs) are rare and may grow to a large size, displacing and rarely invading adjacent structures. Therefore, RSs are most often clinically “silent.” RSs are incidentally found during imaging, until they enlarge to a size capable of compressing surrounding organs (mass effect) when presenting with vague, non-specific symptoms. Imaging modalities for RSs include abdominal ultrasound, computed tomography (CT), and magnetic resonance imaging (MRI). RSs present as well-defined, encapsulated masses, possibly with cystic degeneration and central necrosis. Percutaneous biopsy and a histopathological examination may be useful. However, these procedures are not always feasible and conclusive because of the risk of misinterpretation of cellular pleomorphism in degenerated areas, harvesting insufficient amount of tissue, and bleeding from vessels involved.2,6 Additionally, there is a radiological resemblance between schwannoma and some tumours in which preoperative tissue sampling is discouraged, such as gastrointestinal stromal tumours. 7 Considering that resection is the primary treatment option, obtaining preoperative histopathological diagnosis is not mandatory for an RS.
We report here a patient with a large, benign schwannoma in a rare location who presented with chronic back pain. We also discuss diagnosis and treatment strategies for this uncommon condition with a review of the literature.
Case report
A 45-year-old woman presented to our centre with a 2-year history of continuous progressive right-sided lower back and dull lateral abdominal pain radiating to her posterolateral thigh. The pain was independent of activities and poorly responded to nonsteroidal anti-inflammatory drugs and physiotherapy. A physical examination showed a painless palpable mass in the right paraumbilical and lower abdominal region without peripheral neurovascular deficits. Laboratory tests were normal, except for an unspecific, mildly elevated erythrocyte sedimentation rate. Abdominal ultrasound showed a large, encapsulated, oval soft-tissue mass, which was 21 × 16 cm in diameter in the right retroperitoneum. Subsequent abdominal MRI confirmed a homogenous soft-tissue tumour with a thick, smooth, capsular lining. This tumour lay in the right retroperitoneum paravertebrally and displaced the iliopsoas muscle distally and the right kidney craniolaterally, without any signs of ipsilateral hydronephrosis (Figure 1). Although the tumour was large, it was considered benign because it was not heterogenous, had no irregular margins, and there were no signs of adjacent organ involvement. Management options were discussed at a staff meeting. We decided not to perform a percutaneous biopsy because of the difficult position of the tumour. Symptom-relieving surgery was decided as the best choice of treatment.

Magnetic resonance images showing a large, homogenous, soft-tissue tumour with a thick, smooth capsule in the right paravertebral retroperitoneum. This tumour displaces the iliopsoas muscle distally and the right kidney craniolaterally, without any signs of ipsilateral hydronephrosis and adjacent organ involvement.
Following preparation, the patient underwent surgery. The encapsulated mass was removed in toto together with its capsular lining, but without definable and clear peripheral nerve encasement or invasion. Identification of the nerve of origin is common, despite complete tumour excision. The procedure was performed without complications and there was no need for blood product substitution. However, extensive bleeding may be encountered from the adjacent vessels.
A histological examination and immunohistochemical staining confirmed the diagnosis of benign encapsulated cellular schwannoma. The tumour had no infiltrative margin and there was a well-defined collagenous capsule and hyalinized vessels. The diagnosis was based on highly ordered, dense, cellular components, typical, well-organized spindle cells with a palisading arrangement (arranged in short bundles of interlacing fascicles), and with Verocay bodies formed by two parallel lines of nuclei with a nuclear space between them indicating an Antoni A pattern (Figure 2A). Reactive hyperplasia of adjacent lymph nodes was also found. Immunohistochemistry showed S100 protein-positive (Figure 2B) and vimentin-positive, and epithelial membrane antigen-negative and CD34-negative tumour cells. The lack of epithelial membrane antigen immunoreactivity indicated the absence of perineurial cell differentiation. Therefore, the results of the immunohistochemical examination suggested benign schwannoma. The issue of whether the lesion was benign or malignant was resolved with the finding of a low proliferative index (Ki-67 = 1.6%), which highly suggested its benign nature (Figure 2C).
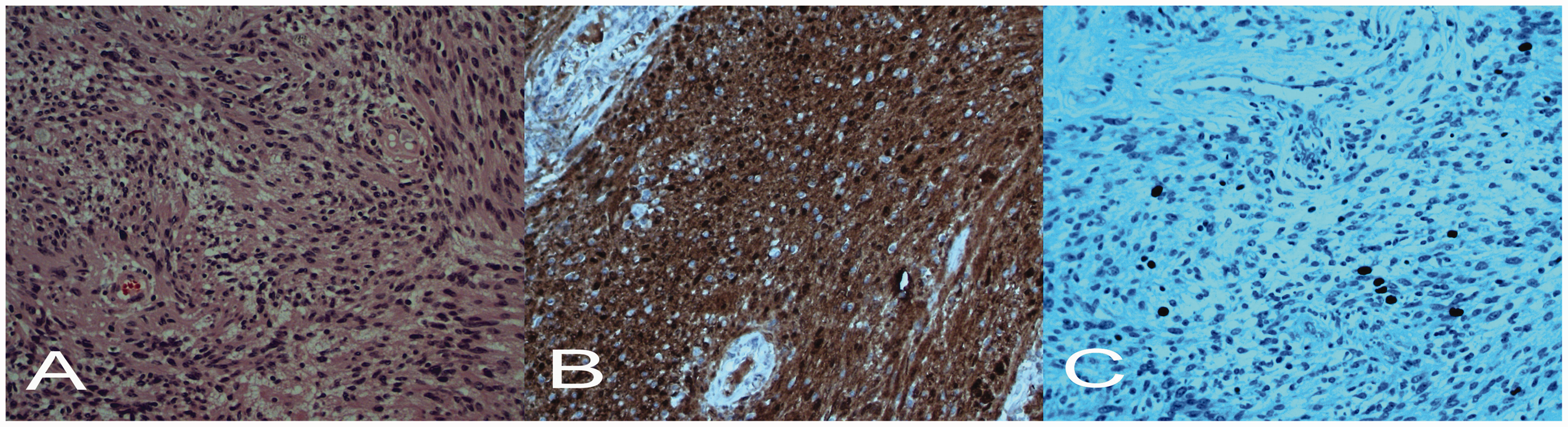
Histopathology of benign schwannoma. Spindle cells show a palisading arrangement with Verocay bodies formed by two parallel lines of nuclei and blood vessels. (A) Haematoxylin and eosin staining, ×10. (B) S100-positive cells, ×10. (C) The Ki-67 index was 1.6%, ×20.
The patient’s postoperative course was uneventful except for the transient mild posterolateral thigh pain, paraesthesia, and muscle weakness. She was administered pain relievers, vitamin B complex supplements, and exercise rehabilitation for 3 weeks. After medication and physiotherapy, there was no pain, her muscle power was completely restored, and paraesthesia greatly improved. Considering the benign nature of the tumour and an expected good prognosis, no adjuvant treatment was administered. The follow-up period was 13 months. Abdominal ultrasound was performed every 3 months and MRI was performed at the end of follow-up. During the follow-up, the patient was well, asymptomatic, did not require any therapy and imaging, and did not show disease recurrence, which would require additional surgery. The patient provided verbal informed consent for this report.
Discussion
Only a small number of schwannomas are found in the retroperitoneum and comprise up to 6% of all primary retroperitoneal tumours. When schwannomas are located in the retroperitoneum, they are usually located in the paravertebral or presacral space. 8 This uncommon site allows slow and asymptomatic expansion of these tumours. Additionally, when these tumours are enlarged they present with unspecific, vague, and bizarre symptoms, which cannot be considered diagnostic. The most common symptoms are pressure symptoms, such as poorly localized pain and discomfort, and non-specific digestive disturbances. Urinary or faecal incontinence and leg neuropathy are rare. 9 Therefore, chronic lower back and dull lateral abdominal pain radiating into the posterolateral thigh, occurring independently of activities and poorly responding to nonsteroidal anti-inflammatory drugs and physiotherapy as in our patient, could be explained by a retroperitoneal peripheral nerve sheath tumour. However, considering these unspecific and inconclusive symptoms and normal laboratory results also typical for RSs, the diagnosis is based on exclusion, and is often delayed. Nevertheless, reported clinical presentations of RSs are numerous and extremely variable, and include colitis, adrenal mass, psoas abscess, and acute urine retention.1,10,11,12 Although referred pain and neurological deficits in the lower extremities caused by RSs have also been described, this presentation is rare. 13 Additionally, a clinician rarely suspects RS because the occurrence of unspecific lower back pain in middle-aged patients is almost always regarded as an epidemic symptom affecting the majority of the population once or more during life. 14
Considering the presentation of our patient, investigation of patients with lower back pain and neurological disturbances around the saddle area and thigh must include a thorough abdominal examination. Abdominal ultrasound is a rapid, inexpensive, and effective tool for initial diagnostic orientation regarding abdominal/retroperitoneal lesions, such as RS. Currently, MRI is accepted as the imaging method of choice for diagnosis of most soft-tissue tumours because of its higher diagnostic predictability compared with ultrasound or CT. The features of neurogenic tumours, such as bundles (fascicular sign) and a hypointense centre with hyperintense periphery (target sign), are well presented on MRI scans. Additionally, schwannomas are characterized by low-signal intensity on T1-weighted imaging (similar to muscle) and high-signal intensity on T2-weighted imaging (similar to fat). Schwannomas may require acquisition of a fat suppression sequence for delineation from purely lipomatous lesions. However, although MRI may lead to a more accurate preliminary diagnosis, MRI may not reliably distinguish between benign and malignant lesions. Irregular contours, heterogeneity, large size (>5 cm) peripheral enhancement, degenerated areas, intratumoural lobulation, peritumoural oedema, non-cystic appearance of the tumour, and invasion of adjacent structures displayed on MRI scans have been reported as signs of malignancy. 15 These signs should alert surgeons to treat the schwannoma as potentially malignant, especially in patients with Von Recklinghausen’s disease.
Definitive diagnosis and determination of the nature of schwannoma are ultimately based on a histological examination. This examination should be supported by immunohistochemical staining using immunoperoxidase techniques for S100 protein and CD34, which are highly positive and negative, respectively, in benign lesions. A strong diffuse expression of S100 protein is a distinct immunohistochemical feature of schwannoma. 16 Additionally, although positive cytoplasmic reactivity for vimentin may identify all mesenchymal cells, it is more consistently expressed in Schwann cells. 17 Furthermore, unlike neurofibromas, most schwannomas do not demonstrate major CD34 immunoreactivity. 18 However, preoperative CT- or ultrasound-guided biopsy may not always yield diagnosis because of harvesting a small tissue sample, and may be associated with the risk of bleeding, infection, and tumour seeding. Therefore, a definitive diagnosis of schwannoma should be made on postoperative histopathology. 16
Considering the lack of sensitivity to radiation and chemotherapy, surgery is the primary treatment choice for these tumours.8,19 The malignancy of schwannoma cannot be totally excluded preoperatively. Therefore, a wide surgical resection of the tumour, even with excision of adjacent structures suspicious of involvement, is advocated by some authors as the treatment of choice. 20 Removal of an RS may be challenging regarding a potentially increased risk of uncontrollable haemorrhage due to tumour adherence to retroperitoneal vessels and its hypervascularity. The most frequent complication after radical surgery is postoperative neurological deficits, which occur in up to 80% of patients, regardless of the atraumatic technique used. 21 This was also the case in our patient who developed transient, mild, posterolateral thigh pain, paraesthesia, and muscle weakness, which responded well to administered therapy. The local recurrence of malignant schwannomas after marginal excision is expected in up to 72% of cases and in only 11.7% of patients after resection with a wide margin. 22 Therefore, in patients with postoperatively proven malignancy, a re-resection with an adequate surgical margin should be considered. Because malignant transformation of benign schwannomas almost never occurs, complete local tumour excision, or even just simple enucleation, may be regarded as the treatment of choice. 23 However, although the prognosis of benign RSs is good and local resection is generally sufficient, the incidence of tumour recurrence because of incomplete excision is 5% to 10%, and metastatic cases after surgery have been reported.12,24 Therefore, these patients require long-term follow-up. Additionally, special care must be taken in patients with underlying Von Recklinghausen’s disease in whom malignant transformation (neurofibrosarcoma), although rare, is usually observed. 25
Conclusion
RSs are rare. Complete local tumour excision should be regarded as the treatment of choice for these tumours. Prognosis of benign RSs is good. Long-term follow-up of these patients is required for postoperative neurological deficits and local recurrence of the tumour. Because of numerous diagnostic and therapeutic problems that may be encountered, successful treatment of RSs require thorough preoperative planning and a multidisciplinary approach.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
