Abstract
Objectives
This study was performed to describe the health status of Chinese oldest-old individuals aged ≥80 years from 1998 to 2014 and explore differences in their health status based on demographic characteristics and socioeconomic status.
Methods
Data were obtained from the seven waves of the Chinese Longitudinal Healthy Longevity Survey. The Mini Mental State Examination, Katz Index of Independence in Activities of Daily Living, and chair stand test were used to examine cognitive and physical function. Logistic regression was used to evaluate the changes in health outcomes.
Results
Regression results showed increasing cognitive impairment trends and decreasing disability trends, indicating that the oldest-old individuals had worse body function in more recent years. Older people and women had a weaker health status. Rural elders had better physical performance but worse cognitive function. Participants with an education had better overall functioning. Individuals with severe disability had the shortest survival time among the study population.
Conclusions
From 1998 to 2014, the health status of oldest-old individuals was relatively stable in China. These findings indicate the need for specific and continuing attention to the oldest-old population to improve their health condition.
Keywords
Introduction
China became an aging society in 1999; in other words, the proportion of people aged >60 years reached 10%. 1 As the economy developed and health environment improved, the mortality rate declined. The life expectancy at birth rapidly increased from 40.8 years in 1950 to 74.8 years in 2010. 1 One-fifth to one-third of the Chinese population is expected to be elderly by the end of 2050. 2 The speed of societal aging in China is especially rapid, and the scale of aging is particularly large. 3
Oldest-old individuals aged ≥80 years present more severe challenges for social and medical care systems than do younger elders aged <80 years 4 because the oldest-old undergo body function decline and often need much more daily assistance and health care. 5 Researchers have found that more than one-third of a person’s lifetime health care expenditures will be spent after 85 years of age. 6 Long-term care needs and costs are especially high for the oldest-old and are predicted to increase rapidly. 7 The number of oldest-old in China has risen quickly in recent years. The population of 1.50 million people aged ≥80 years in 1950 increased nearly 10 times to 14.28 million in 2005 and 15 times to 22.35 million in 2015. 1 The possibility of surviving into the eighth decade of life also increased, mainly because of a reduction in early-life mortality after the founding of China and a decrease in mortality among elderly people. The oldest-old population has exhibited more rapid growth than any other age group. 8 Developed countries have experienced similarly rapid growth in their oldest-old populations, 9 and many studies have assessed the health status of these populations.10,11 Research has indicated that longevity is associated with many serious social and health problems, especially in the oldest-old population.12,13 However, little academic attention has been paid to this huge segment of the older population in China, where most literature has focused on elderly individuals aged <80 years. Research about this rapidly growing segment of the elderly population could be useful for policy makers.
Recent studies in developed countries have explored changes in elders’ health status.14,15 Some research has revealed a reduction in the proportion of elders with disabilities or cognitive impairment16,17; however, some results have been inconsistent. 18 The health trends in elders and disparities among socioeconomic groups remain unclear, especially in developing countries such as China. China has undergone rapid economic, political, social, and demographic transitions. 19 Hence, the changes in elders’ health status may not be equivalent between Western countries and China.
Using data from all seven waves of the Chinese Longitudinal Healthy Longevity Survey (CLHLS), we aimed to describe the health status of the Chinese oldest-old population from 1998 to 2014 and explore the differences in their health status based on demographic characteristics and socioeconomic status (SES).
Methods
Data sources
In this study, we used data from the CLHLS. The CLHLS was performed to meet the increasing needs of scientific research on the oldest-old population in China and to explore what factors (social, economic, biological, and environmental) influence healthy aging.
Zeng and Vaupel 4 introduced the survey design and sampling processes in detail. The survey covered 1.1 billion people, representing 85% of the total Chinese population. The CLHLS was conducted in 1998, 2000, 2002, 2005, 2008–2009 (late 2008 and early 2009), 2011–2012 (late 2011 and early 2012), and 2014 in 22 provinces of China. In 1998, one-half of each county and city of the 22 provinces was selected, and all centenarians from these regions who voluntarily participated in the CLHLS were interviewed. For each centenarian, one octogenarian and one nonagenarian was selected and matched with respect to residence and sex. In the follow-up surveys, some replacements for deceased elders were added. The CLHLS adopted a targeted random-sample design to ensure representativeness by ensuring almost identical numbers of interviews between different age groups and sexes. All participants in the study provided informed consent and were followed prospectively. Sampling weights were made according to age, sex, and residence to adjust for sample selection. The CLHLS data quality, including reliability coefficients, factor analysis, and sample attrition, was acceptable according to Gu. 20 The survey nonresponse rate of the CLHLS was about 4% in each wave. 21
The questionnaires of the CLHLS collected data on basic information, life evaluation and personality, cognitive function, lifestyle, activities of daily living (ADL), and personal background 4 of the participants in each wave. A proxy responder was allowed to participate in the interview if the elders were unable to answer because of illness. Some questions, such as those regarding cognitive function, were not allowed to be answered by proxies. Finally, the elders underwent some basic physical examinations and tests (e.g., heart rate and blood pressure measurement) after the interviews.
The Research Ethics Committees of Duke University and Peking University granted approval for the Protection of Human Subjects for the CLHLS. The survey participants provided written informed consent before the survey.
Study sample
We used data from all seven waves of the CLHLS in this study. In every wave, the numbers of participants who died, were lost to follow-up, or were newly added are shown in Figure 1. This study was limited to the oldest-old population aged 80 to 105 years at the time of the interview because self-reported age after 105 years is not reliable. 22 Thus, participants aged <80 years or >105 years were excluded.

Sample size in every survey.
Variables and measurement
Outcome variables
Cognitive function
We used the Chinese version of the Mini Mental State Examination (MMSE), which was modified for adaptation to Chinese culture based on the international standard MMSE questionnaire 23 and tested by pilot survey interviews 4 to show the cognitive function of the oldest-old. Items in the Chinese version of the MMSE are orientation, reaction, calculation, recall, and language, similar to the international standard MMSE. With the exception of the question asking participants to name types of food in 1 minute, which has a possible score of 7, each question has a score of 1 if the answer is correct and a score of 0 if incorrect. The maximum total score of the MMSE is 30, with lower scores indicating poorer cognitive ability. We classified scores of 24 to 30 as normal, scores of 18 to 23 as slightly impaired, scores of 10 to 17 as moderately impaired, and scores of 0 to 9 as severely impaired, according to Folstein et al. 23 In the analysis, we calculated the answer “not able to answer” as 0.5 points because every question has a 50% possibility of being correct. According to previous studies,16,24 most participants who were unable to answer questions had some degree of cognitive impairment. Thus, we performed a sensitivity analysis in which we calculated the answer “not able to answer” as a score of 0 to avoid overestimating the cognitive function of the oldest-old.
ADL
For every participant in every wave of the CLHLS, data were collected on ADL as assessed by the Katz Index of Independence in ADL. 25 This index comprises six items: dressing, bathing, indoor transferring, toileting, eating, and continence. Each item has three levels of answers: “without assistance,” “with one part of assistance” (i.e., the respondents could finish this item with some assistance), and “with more than one part of assistance” (i.e., the respondents require a large amount of assistance to finish the item or cannot finish even with assistance). We calculated the ADL score as the number of items the participant could perform without assistance. The maximum total ADL score is 6, with lower scores indicating poorer physical ability. We classified a score of 6 as normal, a score of 4 to 5 as slightly disabled, and a score of 0 to 3 as severely disabled. 4 All six questions without missing answers were used in the analysis.
Physical performance
We chose the chair stand test to reflect the physical performance of elders. The CLHLS tested whether participants could stand up from sitting in a chair. The three possible answers were “can, without use of arms,” “can, with use of arms,” and “cannot.” In the analysis, we regarded the first two answers as participants being able to stand up from the chair.
Exposure variables
Demographic characteristics
Residence was categorized as urban or rural, which reflected the participants’ economic level and lifestyle. 26 The other demographic characteristics were age and sex.
SES
Education was used to indicate the SES of the participants because during the participants’ childhood, only wealthy people could afford to send their children to school. 27 Information about education was collected by asking how many years the participants had attended school. We regarded participants who attended school for >1 year as literate and the remaining participants as illiterate. Co-residence was classified into three groups: “with household member(s),” “alone,” and “in an institution.” Marital status was categorized as “married,” “divorced/separated,” “widowed,” and “never married.”
Proxy
Only participants who answered all questions of the CLHLS interviews by themselves could be classified as “no” for this variable; otherwise, they were classified as “yes.”
Year trend
We used this variable to reflect changes in outcomes by year using logistic regression. This variable was assigned the value of 0 in 1998 and increased by 1 each subsequent calendar year to 16 in 2014.
Prior test exposure
This variable was used to adjust for potential effects of repeat cognitive function testing. We measured this variable as a dichotomous variable that represented whether participants had participated in previous waves of the CLHLS as mentioned in other studies.24,28
Statistical methods
In the statistical analysis, we first calculated the sample sizes in each wave. Descriptive analyses were used to show the information of the participants. T-tests and χ2 tests were used to evaluate differences in sample characteristics throughout the seven-wave survey period.
Next, to assess trends in the MMSE, ADL, and chair stand test results throughout the study period, we counted the unadjusted average scores for the overall results in every wave. We also tested the prevalence of being cognitively impaired, disabled, and unable to stand up from a chair in the demographic characteristics. Prevalence was compared separately by χ2 tests.
Finally, to address bias of differences in the demographic composition of different surveys and to control the study design features, we used logistic regression to evaluate the changes in health outcomes, adjusting for demographic characteristics and SES in order. Thus, we created two models for each health outcome. The annual percent change in the probability of being cognitively impaired, disabled, and unable to stand up from a chair was estimated as (1 − odds ratio) × 100 or (odds ratio − 1) × 100.
Furthermore, we chose the original participants who entered the CLHLS in 1998 to gain insight about the prognosis of the oldest-old participants’ physical function and survival from 1998 to 2014. We used Kaplan–Meier plots to show the survival time of three ADL groups. We then counted the average ADL score of those ADL groups in every survey period. The sample size of each ADL group progressively decreased from 1998 to 2014, and we eliminated the sample from the analysis if its size was <10.
We recorded MMSE data as missing if participants missed all answers of the MMSE, and we excluded them from the data analysis; if participants answered most questions of the MMSE, we counted each missing answer as a score of 0.5. For the chair stand test and ADL, we only excluded the missing data from the analysis because there were few such cases. We listed missing data of confounders and excluded them from other percentage calculations in the descriptive analyses. We also performed some sensitivity analyses to address bias, such as excluding all missing information from the analysis and calculating the missing answers as a score of 0 in the MMSE domain.
Results
Participants and basic information
After excluding participants aged <80 years and >105 years, the final study samples involved in the analyses of the seven waves were 8805, 10,972, 10,953, 10,400, 11,923, 6233, and 4493, respectively. In total, 63,779 assessments for living oldest-old individuals were performed; nearly 50% of these participants finished part or all of the assessment with a proxy in each wave. In the seven surveys, participants had a mean age of about 92 years, and >50% were female. The proportion of oldest-old participants who lived alone increased over time. The characteristics of each sample were significantly different among the seven waves (p < 0.001) (Table 1).
Sample sizes and participants’ characteristics in the seven waves.

Data are presented as mean ± standard deviation or n (%).
*Missing data are excluded from other percentage calculations.
Health outcomes
From 1998 to 2014, there were no clear trends in the unadjusted mean scores or grouped results among all three health outcomes. In the sensitivity analyses for the MMSE, the mean score was lower in every survey, but there was no obvious trend as the years progressed (Table 2).
MMSE, ADL, and chair stand test results for every survey.

Data are presented as mean ± standard deviation or n (%).
MMSE, Mini Mental State Examination; ADL, activities of daily living.
*Missing data are excluded from other percentage calculations.
The prevalence of having impaired cognitive function and being disabled in ADL showed fluctuation during the seven surveys, while changes in the chair stand test results were smoother. ADL and MMSE showed similar changes except in the year 2008 (Figure 2).
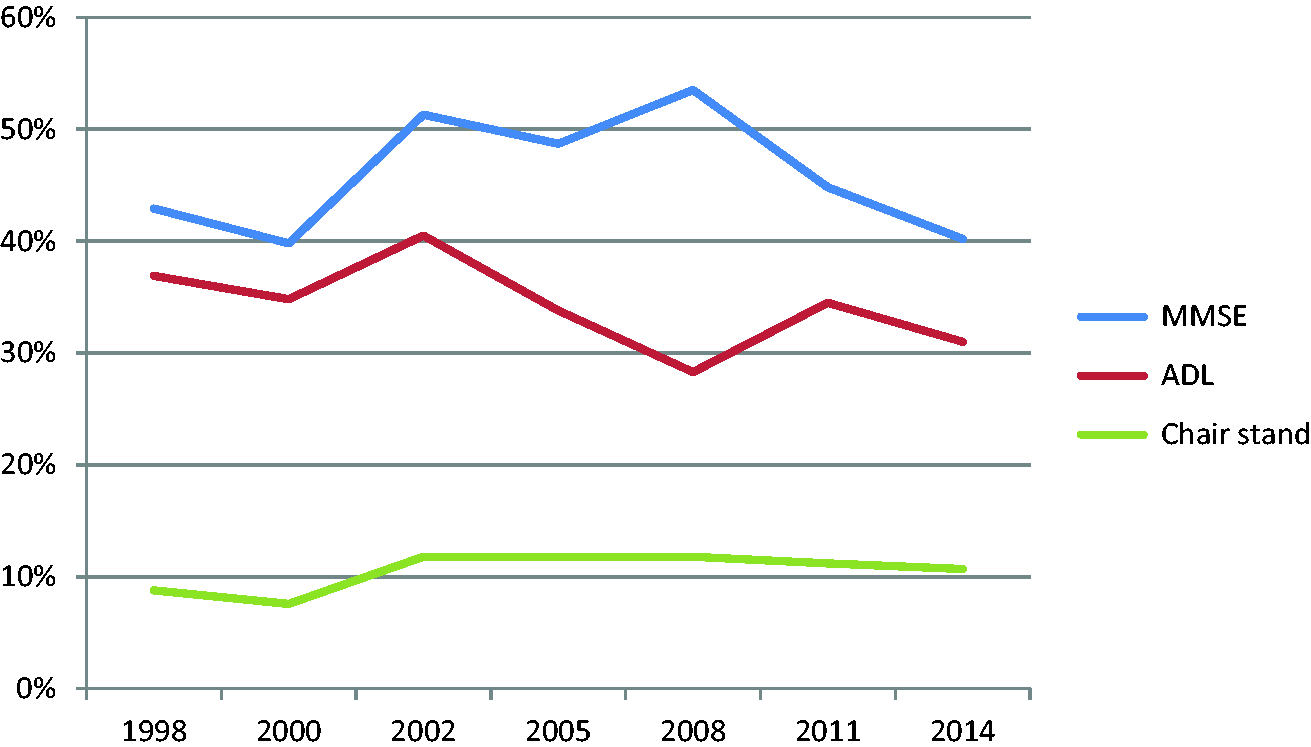
Proportion of participants who showed impairment on the MMSE, disabilities in ADL, and were unable to stand up from a chair for every survey. MMSE, Mini Mental State Examination; ADL, activities of daily living.
In every survey, older people had a higher proportion of being cognitively impaired, disabled in ADL, and being unable to stand up from a chair (p < 0.001 for all). Women were more likely than men to show disability in cognitive function and physical function (p < 0.001). The prevalence of rural participants with cognitive impairment was higher than that of urban participants in every survey (p < 0.001). In contrast, rural elders had a lower proportion of disability in ADL than urban elders (p < 0.001). The chair stand test showed no consistent comparison results (i.e., in seven waves there were no consistent results for the chair stand test, such as ADL and MMSE, when making comparisons between residences) (Table 3).
Proportion of impairment on MMSE, disability in ADL, and inability to stand from a chair by age group, sex, and residence for every survey.

MMSE, Mini Mental State Examination; ADL, activities of daily living.
Data are presented as percentage of participants.
Both models of MMSE function showed a slight increase of about 1.2% to 1.5% per year in the prevalence of cognitive impairment across time after adjustment for demographic characteristics and SES (p < 0.01). Adjustment for prior test exposure slightly increased the probability of cognitive impairment (p < 0.01). Nonagenarians and centenarians were more likely to be cognitively impaired than octogenarians in Models 1 and 2 (p < 0.01). Female and rural residents were more likely to be cognitively impaired (p < 0.01). Participants with an education were less likely to have impaired cognitive function (p < 0.01). Participants who lived alone were less likely to be cognitively impaired, and those who lived in an institution showed a higher probability of losing cognitive function (p < 0.01 for both). Compared with the married group, the other three groups were more likely to be cognitively impaired (p < 0.05). We obtained similar results in the MMSE sensitivity analyses (Table 4).
Adjusted odds ratios of logistic regression for impairment on MMSE.

OR, odds ratio; CI, confidence interval; ref, reference.
**p < 0.01, *p < 0.05
In the ADL domain, the proportion of participants with disabilities in ADL decreased slightly as time passed in both models (p < 0.01). Consistent with the MMSE results, older people and women were more likely to be disabled (p < 0.01). In contrast to cognitive function, urban participants had a higher probability of being disabled in ADL than rural participants (p < 0.01). Participants with an education were less likely to be disabled, although the difference was not statistically significant. Elders who lived alone were less likely to be disabled in ADL (p < 0.01). Widowed participants were more likely to be disabled than those who were married (p < 0.01) (Table 5).
Adjusted odds ratios of logistic regression for disability in ADL.

ADL, activities of daily living; OR, odds ratio; CI, confidence interval; ref, reference.
**p < 0.01
In the chair stand test results, a slight increase in the prevalence of failing to stand up from a chair was shown across time in both models (p < 0.01). Similarly, older people and women were less likely to successfully perform this body function test (p < 0.01). Participants who lived in rural areas or alone had a higher probability of being able to stand up from a chair (p < 0.01). Those who lived in an institution were less likely to stand up from a chair (p < 0.01). Compared with the married group, the other three groups were more likely to fail the chair stand test (divorced/separated, p < 0.05; widowed, p < 0.01; never married, not statistically significant) (Table 6).
Adjusted odds ratios of logistic regression for chair stand test.

OR, odds ratio; CI, confidence interval; ref, reference.
**p < 0.01, *p < 0.05
We chose the original participants of the first-wave survey to perform an additional analysis regarding the prognosis of oldest-old participants’ physical function and survival. We found that the normal group had the longest survival time and that the severely disabled group had the shortest survival time. On average, participants in the normal group had a nearly 3-year longer survival time than those with severe disability (Figure 3).

Kaplan–Meier survival curves by ADL groups. ADL, activities of daily living; Cum, cumulative.
For the oldest-old in the normal and slightly disabled groups, physical function declined from 1998 to 2014. The ADL score of the elderly participants in the normal group decreased to a lesser degree than that of participants with slight disability. Participants with severe disability showed a rising trend from 1998 to 2005. Thus, the oldest-old with severe disability died more quickly than other participants (Figure 4).

Average ADL scores in every survey by ADL groups. ADL, activities of daily living.
Discussion
The present study showed the health status of Chinese oldest-old from 1998 to 2014. Unadjusted scores showed no obvious trends for the three outcome measurements. After adjustment for demographic characteristics and SES, the ADL improved slightly, while physical performance and cognitive function slightly decreased as the years passed. Older people and women were more likely to be disabled and cognitively impaired. Rural participants had better physical function but worse cognitive function than urban participants. Participants with an education had a better health condition than those without an education. Participants with severe disability had the shortest survival time.
Although many studies of changes in health status trends have shown improved results over time,28–30 we found no obvious trends from unadjusted scores (Figure 2). This is consistent with the findings of the National Health Interview Survey from 1982 through 1993. 18 This may be because of the survey design and changes in the composition of the samples. For example, the increased MMSE impairment in 2008 may have been partly due to a higher proportion of participants responding “not able to answer” and higher proportions of female and rural participants (female and rural participants were more likely to be cognitively impaired). This may have led to underestimation of the results. The sensitivity analyses showed similar results. For this reason, we conducted logistic regression models to control for these biases.
After adjustment for the confounding features of the survey design and sample differences, only slight improvement in ADL and a slight decline in cognitive function and physical performance were observed. There are several possible reasons for these findings. First, health care for elderly individuals in China is generally inadequate, although the government established the Urban Employee Basic Medical Insurance Scheme in 1998, the New Rural Cooperative Medical Scheme in 2002, and the Urban Resident Basic Medical Insurance Scheme in 2007 to strengthen health care for elders. However, these policies aimed to meet the basic medical needs for all age groups, not just for elders. 31 The medical services for elderly are mainly offered by primary medical institutions, and the low-level medical capacity and staff of these institutions cannot meet all of the needs of elders. Therefore, the elderly care systems that have been adapted to Chinese aging society still need to be consummated. 32 For example, developed countries have mature and thorough care systems for elders to promote the health outcomes of this population, such as Medicare in the United States. Improvement in this population’s health status may need some time. 24 Second, the rapid developments of society, technology, and instruments have facilitated people’s lives. Therefore, many people have reduced their amount of daily exercise to maintain their body function. However, ADL measurements represent the more severe end of physical limitations. An improvement in ADL may be a good start to the improvement in the health status of the elderly population.
More female than male elderly individuals participated in every survey, and they performed worse than male participants in all three outcomes. In the physical domain, this is consistent with the findings from a previous study from the United States 33 and other research in China.4,34 The reasons for the differences are complex. They may be related to the differences in daily activities preferred by men and women. Other research has shown that differences in muscle mass between the two sexes may cause this health gap. 11 Due to the preference for sons in China, females may experience a more difficult early life than males, with less chance to attend school and less care. 35 This may lead to poorer cognitive function.
Participants living in rural areas had better physical function than those in urban areas. This may have been because rural participants performed more physical activities and lived in places with less air pollution. These conditions are advantages for elders’ physical health. Additionally, this result is consistent with the finding by Zeng and Vaupel 4 that oldest-old individuals who live in rural areas are significantly more active in daily living. Moreover, because of their poorer medical conditions, the survival of elders with disabilities has been shown to be lower in rural than urban areas. 36
Participants with an education were in better health. Many studies have shown similar results.24,37 Elders with a lower education level may reach old age with less cognitive reserves, 38 suggesting that elders with a higher education level may finish tasks more efficiently or be better at using some compensatory mechanisms that delay cognitive impairment. Higher education might reflect better SES in early life, more access to health care, and better nutrition to help brain development. 39 Meanwhile, education provides knowledge to help people live in healthy ways, such as maintaining a balanced diet and exercising in daily life. This result is consistent with the findings reported by Zimmer et al. 40 They used 15-year panel data to examine the disability trends of older persons in Beijing, China and found that educated individuals had a lower probability of being disabled.
Oldest-old who live alone had a better health status, while those who lived in institutions had a worse health status. Children of elders generally let elders live alone when they can take care of themselves. Living alone may force the oldest-old to perform daily activities on their own, and these exercises may improve their health status. 4 Elders with a worse health status may be more likely to be sent to institutions by their children.
In this study, previous survey exposure did not show a repeat effect as in other studies.24,28 This may have been because the interviewers did not tell the participants whether their answers to the MMSE were correct in every survey of the CLHLS. The repeat effect may have been slight because there was a 2- to 3-year gap between every two surveys.
This study has several limitations. First, selection bias may exist. The participants newly added to the samples did not completely replace the participants who were lost to follow-up or died between waves. However, this study focused on the oldest-old population at the national level instead of a particular sample. Second, societal changes may require a relatively longer time to exert their influences on the population’s health status. Continuous surveys and studies are needed. Third, period and cohort effects cannot be separated from each other. Further studies may help to resolve this aspect.
Measurement of the health status of elders is vital for determining policy priorities and making health system changes. Elder-friendly policies in developed countries are worthy to establish. More attention should be paid to the oldest-old population because they consume the most medical and health resources and social support within a society. If they have a better health status, the whole society will greatly benefit. Importance should also be placed on education. This would not only be valuable for economic development but also strategically important in reaching humans’ goal of healthy aging. 4 If such efforts are made at an early age, the oldest-old could benefit from them. 41 An elder-friendly environment should be established to help the increasing numbers of older people live in healthy ways. 42
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study (including the CLHLS data analyzed) was funded by projects 71490732, 71233001, and 71110107025 supported by the National Natural Science Foundation of China, UNFPA, the NIH (R01AG023627), and the WUN Research Development Fund Grants 2015.
