Abstract
Objective
This study was performed to observe the occurrence of corrected QT (QTc) interval prolongation during anesthetic induction for laryngeal mask airway insertion and the effects of cisatracurium administration on the QTc interval.
Methods
Eighty-eight patients were assigned to two groups: the cisatracurium administration group (n = 45) and non-cisatracurium administration group (n = 43). The QTc interval was continuously recorded by a 12-lead Holter electrocardiogram beginning in the hospital ward and continuing until after anesthetic induction.
Results
In the cisatracurium administration group, the QTc interval significantly increased from 417.9 ± 27.9 to 451.6 ± 32.5 ms after arrival in the operating room and significantly decreased to 432.4 ± 32.5 ms after a 15-minute rest; it significantly increased to 459.7 ± 23.8 ms again after propofol and fentanyl injection. However, the QTc interval decreased after cisatracurium injection. In the non-cisatracurium administration group, the QTc interval initially showed changes similar to those in the cisatracurium group until fentanyl and propofol were injected.
Conclusions
The QTc interval was significantly prolonged on arrival in the operating room and after propofol and fentanyl injection. The QTc interval did not significantly change by laryngeal mask airway insertion regardless of the administration of cisatracurium.
Keywords
Introduction
The QT interval is defined as the time from the onset of the QRS complex to the end of the T wave and reflects the duration of ventricular depolarization and repolarization. 1 Because the QT interval varies inversely with the heart rate, the corrected QT (QTc) interval is most commonly calculated by the Bazett formula. 2 QTc prolongation on an electrocardiogram (ECG) is considered to be associated with an increased risk of life-threatening arrhythmias, such as torsade de pointes. 3 Some drugs, including volatile anesthetics, antiarrhythmics, and antihistaminic agents, can prolong the QTc interval.4,5 During anesthetic induction, laryngoscopy and tracheal intubation may trigger catecholamine release and prolong the QTc interval.6,7 The laryngeal mask airway (LMA), a supraglottic airway device that is widely used for brief surgery, can attenuate the dramatic hemodynamic responses caused by performing tracheal intubation. 8
The increased risk of QTc prolongation during anesthetic induction results from potential drug–drug interactions among sedatives, analgesics, and muscle relaxants as well as the action of sympathoadrenal responses that are induced during airway establishment. During anesthetic induction, a paralytic agent is usually used before tracheal intubation but is not necessary for LMA insertion. The effect of muscle relaxants on the QTc interval during anesthetic induction remains incompletely evaluated. This study was designed to observe the QTc interval changes during anesthetic induction with or without cisatracurium administration in the setting of LMA insertion.
Methods
Design and study population
This study was approved by the Institutional Review Board of The First Hospital of Jilin University, and written informed consent was obtained from each patient. Recruitment occurred from January to June 2017 among patients scheduled for elective hysteroscopic surgery at The First Hospital of Jilin University. Patients were excluded if they had a body mass index of >30 kg/m2, a history of cardiac arrhythmias or abnormal ECGs, current treatment with drugs known to prolong the QTc interval, coronary heart disease or heart failure, a pacemaker, or severe pulmonary hypertension. All enrolled patients were female by the nature of their surgical procedure. The patients were randomized in a 1:1 ratio into the cisatracurium or non-cisatracurium group based on a computer-generated sequence of numbers.
Anesthetic management and measurements
The patients’ demographics, medical history, diagnosis, and comorbidities were recorded following the study protocol. The preoperative QTc interval was recorded in the ward at baseline using a 12-lead ECG machine. The patients were not premedicated. A 12-lead Holter ECG system (Mortara Instrument, Milwaukee, WI, USA) was connected in the ward before the patients were sent to the operating room, and each patient’s ECG was continuously recorded from this point until completion of anesthetic induction. In the operating room, patients were monitored using noninvasive blood pressure, an ECG, pulse oximetry, and an electroencephalogram (Narcotrend; MT Monitor Technik Gmbh, Bad Bramstedt, Germany). Anesthetic induction began after the patient had rested for 15 minutes after arrival in the operating room. In the cisatracurium group, 2 mg/kg of propofol and 3 µg/kg of fentanyl were injected intravenously during a 30-s period. One minute later, 0.15 mg/kg of cisatracurium was administrated intravenously, and 3 minutes later, a size 3 LMA Supreme (Teleflex, Athlone, County Westmeath, Ireland) was inserted. The same process was performed in the non-cisatracurium group except that the paralytic agent was not administered. In both groups, the patients were mask-ventilated by a volume-control model until LMA Supreme insertion; the tidal volume was 8 mL/kg, and the respiratory rate was 12 breaths per minute. After LMA Supreme insertion, mechanical ventilation was started with same volume control parameters until recovery of spontaneous breathing.
Patients who required additional medications during induction such as atropine (for a heart rate of <50 bpm), dopamine (for a heart rate of <50 bpm and mean blood pressure of <70 mmHg), and noradrenaline (for a mean arterial pressure [MAP] of <70 mmHg) were also excluded because these medications may potentially affect QTc interval prolongation.
All data recorded by the 12-lead Holter ECG were analyzed using HScribe software (Mortara Instrument), which derived an automatic beat-to-beat QT measurement for each minute. In the cisatracurium group, the QTc interval was recorded in the ward (T0), immediately upon arrival in the operating room (T1), after a 15-minute rest (T2), 1 minute after propofol and fentanyl injection (T3), 1 minute after cisatracurium administration (T4), 2 minutes after cisatracurium administration (T5), and 1 minute after LMA insertion (T6). In the non-cisatracurium group, the QTc interval was also recorded in the ward (t0), immediately upon arrival in the operating room (t1), after a 15-minute rest (t2), 1 minute after propofol and fentanyl injection (t3), 2 minutes after propofol and fentanyl injection (t4), 3 minutes after propofol and fentanyl injection (t5), and 1 minute after LMA insertion (t6) (Figure 1).

Flow diagram of cohort assignment and analysis. The flow diagram shows the process of enrollment, assignment to cohorts, validation, and analysis of the study population. QTc, corrected QT; LMA, laryngeal mask airway.
Statistical analysis
Demographic data were compared using an independent t-test or the χ 2 test. We compared each time point of the QTc interval between the two groups using an independent t-test. Nonparametric tests and adjustments for multiple pairwise post hoc comparisons (Games–Howell) were performed to test for differences in the QTc interval within and between groups.
QTc prolongation was defined as absent (QTc ≤ 450 ms), moderate (450 < QTc ≤480 ms), marked (480 < QTc ≤ 500 ms), or substantial (QTc > 500 ms). 9 Within each cohort, these QTc interval categories were compared using the Friedman test. In addition, post hoc pairwise comparisons and QTc intervals were established through the Wilcoxon text and post hoc comparisons.
Values are presented as mean ± standard deviation or number (%) of patients. SPSS software (version 20.0 for Mac; IBM Corp., Armonk, NY, USA) was used for all statistical analyses. A p value of <0.05 was considered to indicate statistical significance.
Results
In total, 150 evaluable patients who underwent general anesthesia for elective hysteroscopic surgery were recruited for this prospective cohort study, and 62 were excluded for various reasons (Figure 1). Therefore, 88 patients were enrolled (cisatracurium administration group, n = 45; non-cisatracurium administration group, n = 43). All patients were aged 20 to 65 years and had an American Society of Anesthesiologists (ASA) physical status class of I or II. There were no significant differences in age, body mass index, ASA class, or comorbidities between the two groups. Additionally, there were no significant differences in liver function, renal function, etiology, or serum electrolyte levels, including calcium, potassium, and magnesium, between the two groups (Table 1).
Patient characteristics.

An independent t-test or the χ 2 test was used for comparisons between groups. Values are presented as mean ± standard deviation or n (%) of patients. BMI, body mass index; ASA, American Society of Anesthesiologists; AST, aspartate transaminase; ALT alanine transaminase; BUN, blood urea nitrogen.
Hemodynamic data are shown in Figure 2. Both the cisatracurium group and non-cisatracurium group exhibited similar changes in their MAP and heart rate. Propofol and fentanyl administration significantly decreased the MAP (T0 vs. T3: 91.6 ± 4.4 vs. 76.6 ± 3.7 mmHg, p < 0.01; t0 vs. t3: 89.6 ± 3.8 vs. 79.4 ± 3.8 mmHg, p < 0.01) and heart rate (T0 vs. T3: 70.1 ± 3.6 vs. 65.4 ± 2.9 bpm, p < 0.05 [Figure 2(a)]; t0 vs. t3: 72.6 ± 3.1 vs. 63.4 ± 2.4 mmHg, p < 0.05 [Figure 2(b)]). Thirty-seven patients were administrated atropine, dopamine, and/or noradrenaline, and they were excluded from the data analysis. These data demonstrate that the patients’ hemodynamic parameters were significantly depressed by these dosages of propofol and fentanyl.

Hemodynamic data. The changes in (a) MAP and (b) heart rate are shown. *p < 0.05 vs. T0; **p < 0.01 vs. T0; #p < 0.05 vs. t0; ##p < 0.01 vs. t0. In
In the cisatracurium group, the QTc interval changes during anesthetic induction are shown in Figure 3(a). Upon arrival in the operating room, the QTc interval (T1) was significantly higher than baseline (T0 vs. T1: 417.9 ± 27.9 vs. 451.6 ± 32.5 ms, p < 0.001). The QTc interval then decreased after a 15-minute rest (T2) to 432.4 ± 31.4 ms (p < 0.05 compared with T1), while remaining significantly longer than the baseline T0 measurement (p < 0.01) (Figure 3(b)). The QTc interval then increased after fentanyl and propofol injection (T3) to 459.7 ± 23.8 ms (p < 0.001 compared with T2), and then decreased after cisatracurium injection (T4) to 440 ± 34.5 ms (p = 0.024 compared with T3) (Figure 3(c)).
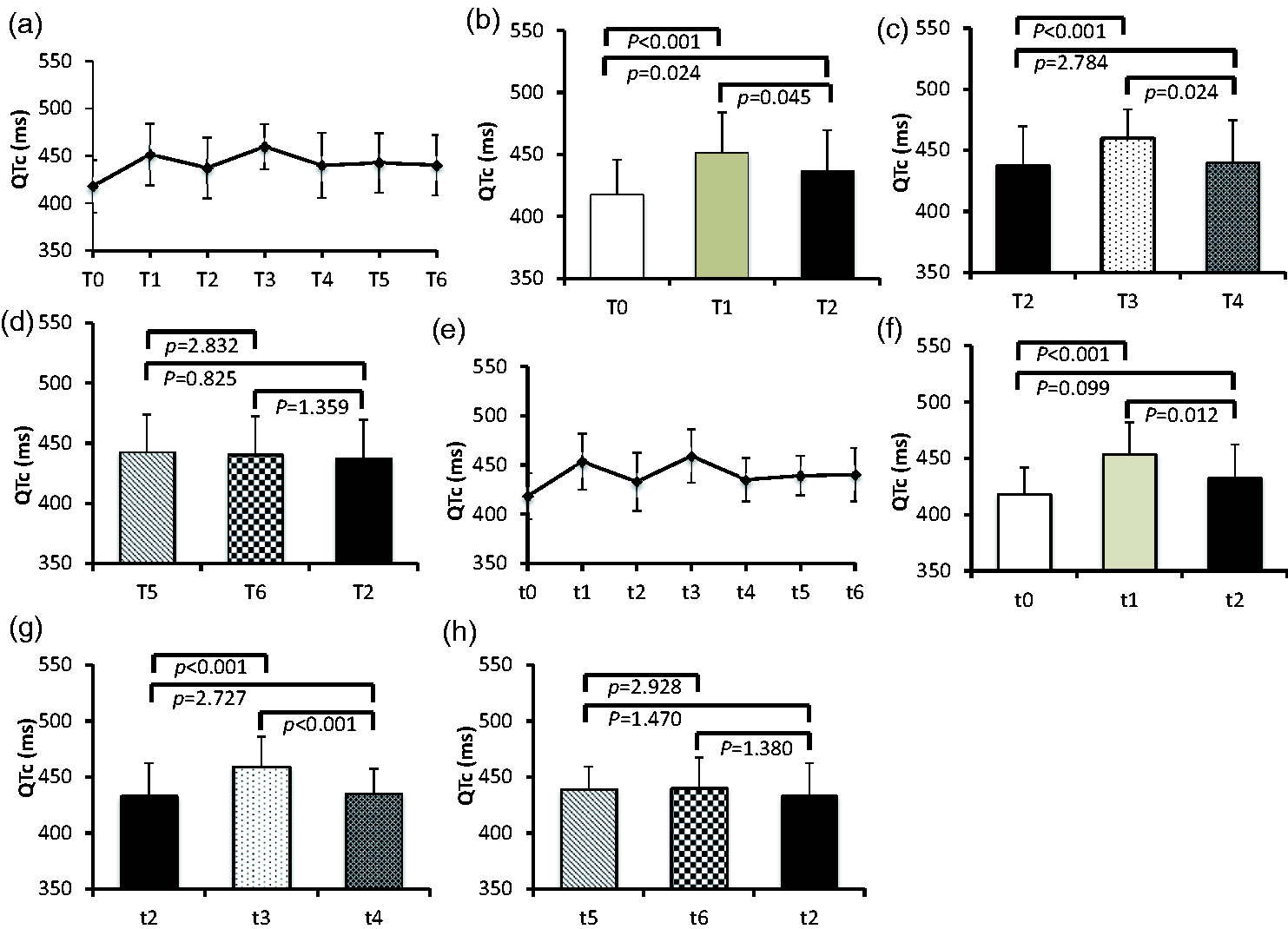
QTc interval changes in the cisatracurium administration group and non-cisatracurium group.
In the non-cisatracurium administration group, the QTc interval changes were similar to those in the cisatracurium group until after fentanyl and propofol injection (Figure 3(e–g)). The QTc interval in the cisatracurium group after cisatracurium injection was not significantly different from that in the non-cisatracurium group after anesthetic induction at 2 minutes (T4 vs. t4: 440 ± 34.5 vs. 435.3 ± 22.1 ms, p > 0.05), indicating that cisatracurium injection did not prolong the QTc interval during anesthetic induction. The QTc interval was not significantly changed by LMA insertion in either the cisatracurium group (T5 vs. T6: 442 ± 31.3 vs. 440.4 ± 31.9 ms, p > 0.05) (Figure 3(d)) or the non-cisatracurium administration group (t5 vs. t6: 439.2 ± 20.1 vs. 440.3 ± 27.3 ms, p > 0.05) (Figure 3(h)). After LMA insertion, the QTc interval in both groups similarly recovered to the level observed before fentanyl and propofol administration (Figure 3(d) and (h)).
In the cisatracurium group, the prevalence of marked or substantial QTc prolongation increased from 2% to 15% upon arrival in the operating room and from 13% to 33% after fentanyl and propofol injection (p < 0.001). After cisatracurium injection, the prevalence of marked or substantial QTc prolongation decreased from 33% to 4% (p < 0.001) and was not significantly affected by LMA insertion (6% to 9%). In the non-cisatracurium administration group, the prevalence of marked or substantial QTc prolongation showed changes similar to those in the cisatracurium group.
A comparison between the two groups showed no significant difference in the QTc interval before LMA insertion (442 ± 31.3 vs. 439.2 ± 20.1 ms), which indicates that addition of cisatracurium did not prolong the QTc interval during propofol and fentanyl induction. Furthermore, the QTc interval was also not significantly different between the two groups after LMA insertion (440.3 ± 27.3 vs. 440.4 ± 31.9 ms), which indicates that LMA insertion did not affect the QTc interval regardless of whether cisatracurium was administered (Figure 4(a)). Correspondingly, in both groups, comparison of the QTc prolongation categories revealed no difference before or after LMA insertion (Friedman test: p > 0.001 (Figure 4(b)).

QTc interval changes and prolongation after LMA insertion in the two groups.
Discussion
Many published studies have addressed QTc interval changes during anesthetic induction and airway management. In this prospective observational study, the QTc interval was significantly prolonged in patients after arrival in the operating room. This QTc interval prolongation was attenuated after a 15-minute rest but still remained longer than the baseline level, which was recorded in the ward. The QTc interval was prolonged again after fentanyl and propofol injection and decreased after 1 minute. However, cisatracurium administration did not affect the QTc interval changes during fentanyl and propofol anesthetic induction, and the QTc interval was not prolonged by LMA insertion with or without cisatracurium injection.
Prolongation of the QTc interval in association with transition from the ward to the operating room may be caused by anxiety. Indeed, the QTc interval duration is known to be influenced by interactions between sympathetic and parasympathetic activity as well as by hormone levels, hemodynamics, electrolytes, temperature, and structural cardiovascular disease.10–14 Catecholamines could be released by excited sympathetic nerves when patients enter the operating room. Anxiety should be considered as an important risk factor for QTc prolongation during anesthetic induction.
In both of our cohorts, the QTc interval was significantly prolonged after fentanyl and propofol injection. Anesthetic drugs cause QTc interval prolongation via cardiac ion channel blockade or via sympathetic stimulation. Propofol is not considered to prolong the QTc interval and is recommended as a safe drug for patients with QTc interval prolongation. It has been used as an active comparator when evaluating the QTc-prolonging effects of other general anesthetics.15,16 Fentanyl is a classical opioid agonist that has been widely used to attenuate sympathoadrenal responses. In addition, fentanyl has shown protective effects against anesthesia-induced QT changes and exhibits no QTc prolongation-related issues.17,18 Because both propofol and fentanyl have minimal effects on anesthetic-induced QTc prolongation, the cause of the transient QTc interval prolongation after propofol and fentanyl injection in this study was elusive. We speculate that one possible mechanism of this QTc interval prolongation may be a drug–drug interaction caused by successive administration of propofol and fentanyl, which triggered the significant QTc interval prolongation observed in this study. Alternatively, general anesthesia itself may induce changes in the QTc interval due to sympathetic and parasympathetic nerve depression, regardless of the sedative and analgesic used. During anesthetic induction, muscle relaxation/paralysis is not always necessary. Few studies to date have assessed the QTc interval prolongation induced by cisatracurium during anesthetic induction. In the present study, QTc interval prolongation was not observed after cisatracurium injection. From another viewpoint, the drug–drug interaction between propofol and fentanyl could be synergistic in decreasing the QTc interval, which may be the reason why we did not observe QTc interval prolongation after cisatracurium administration or LMA Supreme insertion.
Hemodynamic responses arising from tracheal intubation are primarily caused by supraglottic area stimulation and tissue irritation during direct laryngoscopy. Insertion of supraglottic airway devices confers less stimulation of the soft tissues of the pharynx and trachea. Byon et al. 19 showed that both laryngoscopic intubation and supraglottic airway device insertion could prolong the QTc interval, but the i-gel supraglottic airway device (Intersurgical, Wokingham, Berkshire, England) produced less QTc interval prolongation than laryngoscopic intubation. In the present study, prolongation of the QTc interval did not occur after LMA insertion regardless of cisatracurium administration. The propofol/fentanyl induction method used in this study is superior to that in the above-mentioned study by Byon et al. 19 This novel method with an optimized dosing regimen could potentially depress the LMA Supreme insertion-induced sympathoadrenal response more adequately than other methods. 17 This might explain why we did not observe QTc interval prolongation in our study cohorts. However, the dosage of fentanyl we provided may cause more hemodynamic fluctuation. Indeed, 37 patients were excluded from the data analysis because of the need for atropine, dopamine, and/or noradrenaline administration.
We only enrolled female patients in this study. Paulussen et al. 20 found that drug-induced long QT syndrome was twice as prevalent in female patients than in male patients. Li et al. 21 also demonstrated that female sex should be considered an independent risk factor for drug-induced long QT syndrome and torsade de pointes. Therefore, sex-specific studies are clinically meaningful with respect to providing scientific evidence of the effects of anesthetic drugs in patients of different sexes.
Like most clinical studies, the present study has several limitations. Some patients were excluded due to atropine, dopamine, and noradrenaline administration, which tended to preferentially exclude older patients. Younger patients may have a lower risk of QTc interval prolongation. Although the QTc interval was not significantly prolonged by cisatracurium administration and LMA insertion in the present study, the QTc interval measured at each time point during anesthetic induction was always longer than that recorded in the ward. We presume that catecholamines were released when the patient entered the operating room, but we did not measure the patients’ catecholamine concentrations. In future studies, we plan to measure catecholamines during anesthetic induction.
Conclusion
The present results indicate that the QTc interval is significantly prolonged when female patients arrive in the operating room prior to any medication and is also prolonged by propofol and fentanyl administration. In addition, this study revealed that cisatracurium administration and LMA insertion do not affect QTc prolongation. Although no dedicated study has been conducted to examine the safety of cisatracurium administration and LMA insertion in patients with long QTc syndrome, the results of this study reflect relatively significant efficacy and safety profiles of cisatracurium administration and LMA insertion in patients with long QTc syndrome and imply the need for profound guidance in the management of patients with long QTc syndrome.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This work was supported by the Jilin Province Science and Technology Department (#20150414012GH).
