Abstract
Objective
To analyse location and frequency, and change over time, of radiolucent lines (RLLs) around trabecular metal tibial components in total knee arthroplasty (TKA).
Methods
Osteoarthritic knees in patients who had undergone TKA were retrospectively evaluated via analysis of RLLs on anteroposterior and lateral X-rays obtained at 2 and 6 months, and 1, 2 and 3 years following TKA.
Results
In 125 osteoarthritic knees from 90 patients (mean age, 75.0 ± 6.2; 21 male/69 female), frequency of RLLs around trabecular metal tibial components was generally highest at 2 and 6 months, and 1 year following TKA, then gradually decreased over the 3-year follow-up. Frequency of RLLs around trabecular metal tibial components was greater at the tip of the two pegs, particularly the medial peg, and around the pegs, versus other zones. No postoperative revisions were performed for loosening.
Conclusions
Over 3 years following TKA, RLLs were most frequently observed up to 1 year, then gradually decreased. RLLs were significantly more frequent in the medial peg zone and zones close to the medial peg than in other zones.
Introduction
Total knee arthroplasty (TKA) is a reliable and reproducible procedure with an estimated rate of survival of more than 90% after 15 years.1–3 The main cause of mechanical failure is aseptic loosening, 4 and the risk of surgical revision caused by aseptic loosening is positively correlated with the presence of radiolucent lines (RLLs). 5 RLLs are radiolucent intervals between the implant and the adjacent bone caused by micromotion. This can lead to the formation of gaps, which may prevent osteointegration in uncemented TKA, inducing the formation of fibrous tissue.6,7
Trabecular metal is composed of highly porous tantalum, and has several theoretical advantages when used as a material for uncemented TKA, for example, bony ingrowth and sufficient biological fixation have been shown in case studies and in animal models of TKA.8–11 Excellent cellular adherence, growth, and differentiation of osteocytes to the trabecular metal surface have also been demonstrated.12,13 Moreover, trabecular metal tibial components in TKA have shown excellent clinical results after 5–10 years of follow-up.14–20 Regarding RLLs around trabecular metal tibial components in TKA, however, the frequency and site of occurrence, and change over time remain unknown. An understanding of the time course and site of appearance of RLLs in TKA with trabecular metal tibial components will be useful in decisions regarding the need for revision surgery versus conservative treatment. The purpose of the present study was to investigate the frequency and site of occurrence, and change over time, of RLLs around trabecular metal tibial components, by retrospectively analysing knee X-rays in patients following TKA. Pre- and postoperative knee function was also assessed.
Patients and methods
Study population
This retrospective observational study included patients who had undergone uncemented primary TKA using the NexGen® cruciate retaining-type femoral component and NexGen® Trabecular Metal Monoblock Tibia (Zimmer, Warsaw, IN, USA) for osteoarthritis (OA) at the Ichihara Hospital, Tsukuba, Japan between April 2012 and March 2014. Patients were sequentially enrolled and inclusion criteria comprised available records for ≥1 year of follow-up. Pre-surgery and follow-up data, including demographic and clinical data, X-rays, and knee function analyses were retrieved from medical records.
The ethics committee of Ichihara Hospital reviewed and approved the study (approval number: 1701). Since this was a retrospective observational study, an opt-out method was employed, in which consent to use patient data was assumed unless the patient denied consent for their data to be used in this research.
Surgical procedure and rehabilitation
The surgical procedure and rehabilitation were similar to that described previously. 21 Briefly, all surgical procedures were performed under general anaesthesia, induced using 2 mg/kg Propofol and 0.6 mg/kg Rocuronium (both by intravenous [i.v.] injection), and maintained using 1.0–1.5% inhaled Sevoflurane and 0.2 µg/kg/min Remifentanil (i.v.). Following a midline skin incision and medial parapatellar approach, TKA was performed under tourniquet control using an intramedullary alignment rod for the femoral cuts and an extramedullary guide system for the tibial cuts. The patella was not replaced if articular cartilage remained. The tourniquet was released after skin closure and application of a compressive dressing. Continuous passive movement was started on postoperative day 3, and standing and walking with full weightbearing were allowed from 1 week postoperatively.
Outcome assessment
Anteroposterior and lateral X-rays were evaluated at 2 and 6 months, and at 1, 2 and 3 years following TKA. RLLs were labelled as either ‘present’ or ‘absent’ in each zone, using a previously described protocol. 22 Knees were excluded from the evaluation when the X-rays were too difficult to evaluate because the photographed components were in an oblique position or when X-rays were not taken. Two blinded orthopaedic surgeons (H.M. and A.W.) independently re-evaluated the anonymous anteroposterior and lateral X-rays of all included patients, assessing the location and appearance of RLLs according to a method described previously. 23 The trabecular metal component was divided into nine zones from medial to lateral on anteroposterior X-rays, and into five zones from anterior to posterior on lateral X-rays (Figure 1). The intraclass correlation coefficient (ICC) of inter-rater reliability on anteroposterior X-rays was 0.8 (P < 0.001), and the ICC of inter-rater reliability on lateral X-rays was 0.7 (P < 0.001), indicating that the measurement accuracy was good.

Representative X-rays from patients with osteoarthritis, taken at 6 months following total knee arthroplasty. (a) Anteroposterior X-ray of the trabecular metal tibial component, which was divided into nine zones, from medial to lateral, as follows: medial portion of the baseplate (zone 1), medial portion of the medial peg (zone 2), tip of the medial peg (zone 3), lateral portion of the medial peg (zone 4), central portion of the base plate (zone 5), medial portion of the lateral peg (zone 6), tip of the lateral peg (zone 7), lateral portion of the lateral peg (zone 8), and lateral portion of the base plate (zone 9); 23 Radiolucent lines are visible in zones 2, 3, 4, 5, 6, 7, 8 and 9 in this X-ray. (b) Lateral X-ray of the trabecular metal tibial component, which was divided into five zones, from anterior to posterior, as follows: anterior portion of the base plate (zone 1), anterior portion of the pegs (zone 2), tip of the pegs (zone 3), posterior portion of the pegs (zone 4), and posterior portion of the base plate (zone 5); 23 A radiolucent line is visible in zone 3 in this X-ray.
The Japanese Orthopaedic Association OA knee rating (JOA) score 24 was assessed preoperatively and at the last postoperative follow-up for each patient. The JOA score rates pain during walking (0–30 points), pain during ascending and descending stairs (0–25 points), range of motion (0–35 points), and joint swelling (0–10 points) in patients with OA, giving a maximum total score of 100 points. Higher scores represent better clinical outcome.
Statistical analyses
Data are presented as mean ± SD or n (%) prevalence. Cochran's Q test and McNemar’s test were used to analyse RLL data between each zone at the same time-point, and Pearson's χ2-test was used to analyse RLL data between each time-point at the same zone. The JOA scores were analysed by paired sample t-test. A P value ≤ 0.05 was considered to indicate a statistically significant difference, and all analyses were performed using IBM SPSS software, version 24.0 (SPSS Inc., Chicago, IL, USA).
Results
A total of 105 patients underwent 144 uncemented primary TKA for OA, and of these, 90 patients (125 knees) had follow-up data for ≥ 1 year and were included in this study. Preoperative characteristics, including age, sex, height, weight, body mass index, preoperative femorotibial angle, implant installation angle, 23 and proportion of patients at each follow-up time-point are summarized in Table 1.
Preoperative characteristics, and proportion of follow-up data analysed, in patients who underwent total knee arthroplasty for osteoarthritis.

Data presented as mean ± SD or n (%) prevalence.
The RLL results are summarized in Tables 2 and 3. On anteroposterior X-rays (Table 2), RLLs were increased, or were at the highest frequency, at 6 months following surgery, in zones 3 (tip of medial peg), 4, 6 and 8 (around the pegs), then decreased over the 3-year period. In zone 2 (around the medial peg), RLLs were increased at 1 year following surgery, then decreased. RLLs in zone 5 gradually decreased from 1 year to 3 years. RLLs in zone 7 (tip of the lateral peg) gradually decreased from 2 months to 3 years. There were no statistically significant changes in zones 1 and 9. Between-zone comparisons showed that RLLs occurred significantly more frequently in zones 3 and 7 at 2 months, in zones 3, 4, 6, 7 and 8 at 6 months, in zones 2, 3 and 8 at 1 year, in zones 2, 3 and 4 at 2 years, and in zone 3 at 3 years postoperatively, than in other zones (Table 2).
Frequency of radiolucent lines on anteroposterior X-rays showing the trabecular metal tibial component (divided into nine zones) in patients who had undergone total knee arthroplasty for osteoarthritis.
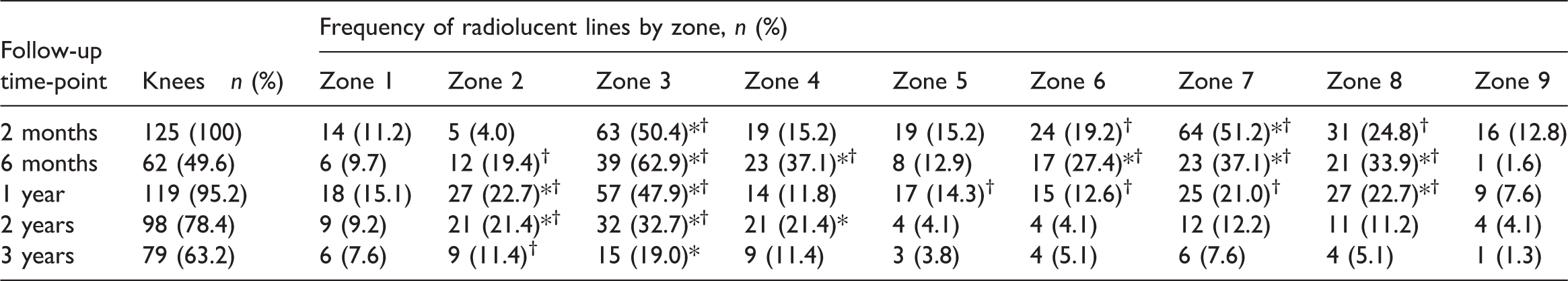
Data presented as n (%) prevalence.
Zone 1, medial portion of the baseplate; Zone 2, medial portion of the medial peg; Zone 3, tip of the medial peg; Zone 4, lateral portion of the medial peg; Zone 5, central portion of the base plate; Zone 6, medial portion of the lateral peg; Zone 7, tip of the lateral peg; Zone 8, lateral portion of the lateral peg; Zone 9, lateral portion of the base plate.
*Significantly higher than at least one of the other zones at the same time-point (P < 0.05; Cochran's Q test and McNemar’s test).
†Significantly higher than at least one of the other time-points in the same zone (P < 0.05; Pearson's χ2-test).
Frequency of radiolucent lines on lateral X-rays showing the trabecular metal tibial component (divided into five zones) in patients who had undergone total knee arthroplasty for osteoarthritis.
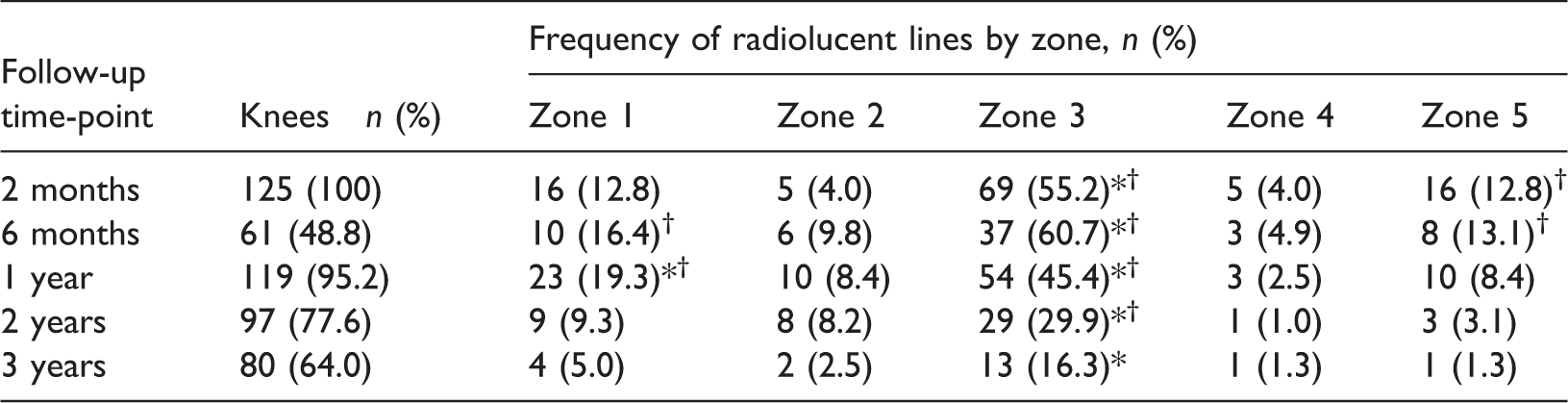
Data presented as n (%) prevalence.
Zone 1, anterior portion of the base plate; Zone 2, anterior portion of the pegs; Zone 3, tip of the pegs; Zone 4, posterior portion of the pegs; Zone 5, and posterior portion of the base plate.
*Significantly higher than at least one of the other zones at the same time-point (P < 0.05; Cochran's Q test and McNemar’s test).
†Significantly higher than at least one of the other time-points in the same zone (P < 0.05; Pearson's χ2-test).
On lateral X-rays (Table 3), analyses of the different follow-up time-points showed that RLLs in zones 3 (tip of the peg) and 5 (posterior portion of base plate) were increased at 6 months, then gradually decreased to 3 years postoperatively. RLLs in zone 1 (anterior portion of base plate) were increased at 1 year then gradually decreased. There were no statistically significant changes in frequency of RLLs in zones 2 and 4. Between-zone comparisons showed that RLLs occurred significantly more frequently in zone 3 than in other zones (Table 3).
No revisions were performed for loosening during the 3-year postoperative period.
Mean postoperative JOA score was significantly higher than mean preoperative score (82.0 ± 8.6 versus 53.2 ± 9.2, P < 0.001).
Discussion
In the present study, RLLs between the trabecular metal tibial component and bone were evaluated in 90 patients (125 TKAs) regarding location and frequency, and changes in frequency over time, from 2 months to 3 years following TKA. The location of RLLs relative to the tibial component, and the frequency of RLLs, significantly changed over time. RLLs were most frequently observed at 2 and 6 months, and 1 year postoperatively, and gradually decreased over the 3-year follow-up period. RLLs occurred significantly more frequently in the medial peg zone (zone 3) and the zones close to the medial peg (zones 2 and 4) than in the other zones.
In the present authors’ opinion, radiolucent lines may be associated with instability, including migration, inadequate load distribution, and particularly elasticity of the trabecular metal tibial tray. RLLs reportedly appear either immediately following surgery or within 2 years postoperatively in both cemented and cementless TKAs,6,7,25 however, RLLs are more frequently associated with cementless than cemented TKA.26,27 Progression of RLLs has been reported in a cementless twin-bearing low-contact-stress tibial tray, in which almost all RLLs appeared within 12 months postoperatively, and 4% of knees evaluated developed progressive RLLs. 7 The implants used in this previously published study were made from cobalt-chromium alloy, and the bone surface was coated with pure titanium beads. In contrast, the RLLs in the present study were non-progressive and decreased with time, possibly due to the unique properties of the trabecular metal material used. The 2-year and 5-year results of a radiostereometric analysis study have been reported, comparing uncemented trabecular metal cruciate-retaining monoblock tibial components with cemented NexGen cruciate-retaining tibial components in patients aged < 60 years.28,29 These studies showed that after an initial settling period over the first 3 months, both the trabecular metal implants and the cemented tibial implants had stabilized by 2 years, and the stability was maintained for up to 5 years postoperatively. Another study also showed that early migration does not continue and stabilization occurs relatively quickly. 30 Osteocyte growth on the trabecular metal components can be promoted within the pores of porous tantalum, as a biocompatible scaffold for bone ingrowth.8–13 The present authors have observed that as bone ingrowth on trabecular metal components progresses with time, the frequency of RLLs can decrease until 3 years postoperatively.
In the present study, RLLs in trabecular metal tibial TKA components were more frequent at the tip of the two pegs, particularly the medial peg, and around the pegs, than in the other zones. Trabecular metal components have been shown to undergo migration in the first 3 months following surgery, including rotation, subsidence, and/or lift-off.28,29 The medial compartment of the trabecular metal may be placed under greater stress than the lateral compartment, and this might be the reason for the present results showing a greater frequency of RLLs in the medial peg than in the lateral peg.
No revisions were performed for loosening during the follow-up period in the present study. Moreover, JOA scores were higher following TKA than before surgery. The frequency of RLLs gradually decreased over the 3-year follow-up period, thus reducing the possibility of loosening of the trabecular metal implant. Trabecular metal components can bond with bone, however, there are potential risk factors for implant failure, including osteoporosis, tall stature, and obesity.31,32 A postoperative follow-up period longer than 3 years would be needed to analyse risk factors for the development of RLLs and loosening of trabecular metal implants.
In clinical terms, the present results suggest that if RLLs increase beyond 1 year following TKA, it may be necessary to consider the possibility of loosening. In the present study, although RLLs were visible (and increased) during the first postoperative year, frequency decreased over time, no revision surgeries were performed for loosening, and mean JOA scores (obtained at the last follow-up meeting for each patient) indicated clinical improvements compared with preoperative scores. These results suggest that if RLLs are visible within the first year postoperatively, but do not increase further, observation or conservative treatment can be pursued. RLLs were observed in 19% of cases in the area around the medial peg tip at 3 years postoperatively, however, further supporting the need for a longer follow-up period to analyse the frequency of RLLs and potential loosening of implants.
The results of the present study may be limited by several factors. First, this was a single-centre study conducted with a small sample of patients, and this should be considered when applying the results in terms of the wider population. Secondly, as trabecular metal implants have been shown to stabilize for up to 2 years,28,29 X-rays were evaluated up to 3 years postoperatively; however, this follow-up period is still relatively short. Finally, since the study was retrospective, the follow-up rate was low and ideal tangential X-rays were not obtained in some cases, and some available radiographs were not suitable for evaluation. For evaluation of the exact integration between the components and bones, serial radiostereometric analysis with six tantalum-sphere markers in tibial bone, or computed tomography analysis without metal artefact may be required. Therefore, prospective, longer-term follow-up studies with a larger number of patients are required to clarify the development and progression of RLLs and loosening of the trabecular metal implant over time.
In conclusion, the present study showed that although the frequency of RLLs around trabecular metal tibial components following TKA increased up to 1 year postoperatively, their frequency gradually decreased by 3 years. The frequency of RLLs around trabecular metal tibial components in TKA was greater at the tip of the two pegs, particularly the medial peg, and around the pegs, than in the other zones. No revisions were performed for loosening during the follow-up period and mean JOA scores indicated clinical improvements following TKA.
Footnotes
Acknowledgments
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
