Abstract
Objective
To evaluate the effectiveness of early (<3 months) cranioplasty (CP) and late CP (>3 months) on post-operative complications in patients receiving decompressive craniotomy (DC) for traumatic brain injury (TBI).
Methods
The Cochrane Library, PubMed and EMBASE databases were systematically searched for studies published prior to May 21, 2017. A meta-analysis examined post-operative overall complication rates, infection rates, subdural fluid collection and operating times according to early and late CP.
Results
Of the initial 1675 references, five studies, all cohort, involving a total of 413 patients, were selected for the review. There was no difference between early and late CP in post-operative overall complication rate (RR=0.68, 95%CI [0.36, 1.29]) and the post-operative infection rate (RR=0.50, 95%CI [0.20, 1.24]) in patients receiving DC for TBI. However, there was a significant difference in post-operative subdural effusion (RR=0.24, 95%CI [0.07, 0.78]) and mean operative time (mean difference = −33.02 min, 95%CI [−48.19, −17.84]) both in favour of early CP.
Conclusions
No differences were found between early and late CP in post-operative overall complications and procedural related infections in patients receiving DC for TBI, but early CP reduced the complication of subdural effusion and the mean operating time. These findings need to be confirmed by large, randomised controlled trials.
Introduction
Decompressive craniotomy (DC), a surgical procedure that involves removal of part of the skull, is regarded as a potential life-saving procedure in patients suffering from intracranial hypertension refractory to medical therapy.1–7 The commonest indications are traumatic brain injury (TBI), ischemic or haemorrhagic stroke, infection and other causes such as cancer. The neurosurgery leads to the subsequent clinical need for secondary cranial reconstruction.5–7
Cranioplasty (CP), which is considered a routine, straight-forward procedure, is required for protection of the brain exposed through the skull and for cosmetic purposes and reports suggest it also improves neurological recovery.6–13 However, the procedure is associated with a relatively high complication rate, ranging from 12% to 50%.14–18 Although the timing of CP appears to play an important role in avoiding procedure-associated complications, optimal timing remains controversial.12,14,16,18–20 While a recent literature review described the complications associated with DC, it did not consider the timing of the CP procedure. 21 Another systematic review that involved patients receiving DC for different reasons (i.e., TBI, ischemic/haemorrhagic stroke and other causes) concluded that, compared with late CP (i.e., 3–6 months after DC), early CP (i.e., 1–3 months after DC) was not associated with more complications or an increased risk of hydrocephalus 12 Nevertheless, in patients receiving DC for TBI which is the most common reason for the procedure, the effects of early CP compared with late CP on post-operative complications remains unclear.5,6,12,14,16,20 Therefore, the aim of this present study was to perform a systematic review and meta-analysis of publications in which authors reported data on post-operative complications following early or late CP following DC for TBI.
Methods
For a published report to be included in the meta-analysis, it had to fulfil the following criteria: (1) randomized, controlled trial or cohort study in English-language that compared early and late CP; (2) patients were receiving DC for TBI; (3) early CP was defined as <3 months after DC and late CP was defined as >3 months after DC. Case reports of <10 patients, case series, editorials, letters, animal studies, protocols, technical reports, guidelines, comments and cadaver articles were excluded.
The Cochrane Library, PubMed and EMBASE databases were searched for studies published prior to May 21, 2017. Key words/terms included, ‘cranial defect’, ‘calvarial defect’, ‘skull defect’, ‘cranioplast’, ‘skull repair’, ‘bone flap replacement’, ‘cranial replacement’, ‘cohort studies’, ‘randomized controlled trials’, ‘control and trials’ and ‘randomised’. Retrieval was adjusted according to each of the databases and the retrieval strategies were determined via multiple pre-retrieval tests using the combination of Mesh terms and free words. In addition, the reference lists of all included studies were checked for any potential additional publications.
Two reviewers (F.Z. and H.X.) independently screened the papers from their abstracts and selected relevant studies. Any discrepancy was resolved through discussion. The reviewers then assessed full text to determine if the study should be included. The following information was extracted from the papers: (1) publication date and authors; (2) number of patients receiving early CP (<3 months after DC) and late CP (>3 months after DC); (3) operating time, overall complications, subdural fluid collection, infection rate. Because of the large variability among studies in the definition of a ‘complication’, we defined a situation that required further intervention post-operatively as a ‘complication’.
The Newcastle Ottawa Scale (NOS) was used to assess the quality of the included studies. 22 This system offers a score out of a possible total of 9 stars and rates the studies according to three broad perspectives: selection of the study groups; comparability of the groups; outcome. Four stars are available from the selection category, 2 stars are available from the comparability section and a possible 3 stars can be achieved in the outcome category. Studies were graded as high quality (6+), moderate (4–5) or weak (0–3). 22 This was a meta-analysis of previously published papers and so institutional review board approval was not required.
Statistical analyses
The meta-analysis was performed by two investigators (F.Z. and H.X.) using Review Manager (RevMan) [Computer program] Version 5.3. Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration, 2014.
For dichotomous data, the Mantel–Haenszel method was used to calculate 95% confidence intervals (CI) and the risk ratio (RR) as the pooled mean effect size estimate. For continuous data, 95% CI and the standardized mean difference (SMD) were calculated. A P-value <0.05 was considered to indicate statistical significance.
Before the data analysis, heterogeneity was assessed according to Cochran’s χ2 (Q) test and I2 statistic. 23 No heterogeneity was defined as P>0.1, I2=0%, low heterogeneity was P>0.1, I2<50% and high heterogeneity was P<0.1, I2>50%.
A random-effects model was used to pool results from the studies and sensitivity analyses were applied in cases of high heterogeneity. Publication bias was not performed because the pooled estimate included fewer than 10 studies. 24
Results
The literature search yielded an initial pool of 1675 references (Figure 1). Of these, 249 references were duplicate and a further 1407 references were eliminated after screening titles and abstracts. Fourteen other references were excluded after perusal of the full text or contact with the author. A final total of five studies were eligible for the review and meta-analysis.5,6,13,16,20 All the studies were cohort studies and their characteristics are shown in Table 1.

Flow diagram of study selection.
Characteristics of the five studies included in the review and meta-analysis of early or late cranioplasty (C)P) following decompressive craniotomy (DC) for traumatic brain injury (TBI).

Values are shown as mean ± standard deviation or mean (range).
*Studies were graded as high quality (6+), moderate (4–5) or weak (0–3). 22
a: patients with dura suture, b: patients without dura suture.
Abbreviations: CP: cranioplasty; MMC: methylmethacrylate; NA: not available; DC: decompressive craniotomy; NOS: Newcastle Ottawa scale.
In total, 413 patients were involved in the five studies.5,6,13,16,20 Details of the number of overall complications are shown in Table 2. No significant differences between early and late CP groups in overall post-operative complications was detected (RR = 0.68, 95% CI [0.36, 1.29]) (Figure 2a). Due to high heterogeneity (I2=55%), a sensitivity analysis was applied to the data. After excluding one study 16 (I2=0), there was little effect on the result ([RR = 0.95, 95% CI [0.67, 1.36]) confirming it was robust and reliable (Figure 2b).
Outcomes of early and late cranioplasty (CP) from the five studies included in the review and meta-analysis.

Abbreviations: CP: cranioplasty; SD, standard deviation; NA: not available.

(a) Overall complications of early cranioplasty (CP) vs late CP in patients receiving decompressive craniotomy (DC) for traumatic brain injury (TBI). (b) Sensitivity analysis of overall complications of early CP vs late CP in patients receiving DC for TBI.
Four studies5,6,13,16 involving a total of 315 patients, evaluated post-operative infections; two studies recorded no infections. No significant difference between early and late CP was detected [RR = 0.50, 95%CI (0.20, 1.24)] (Figure 3).
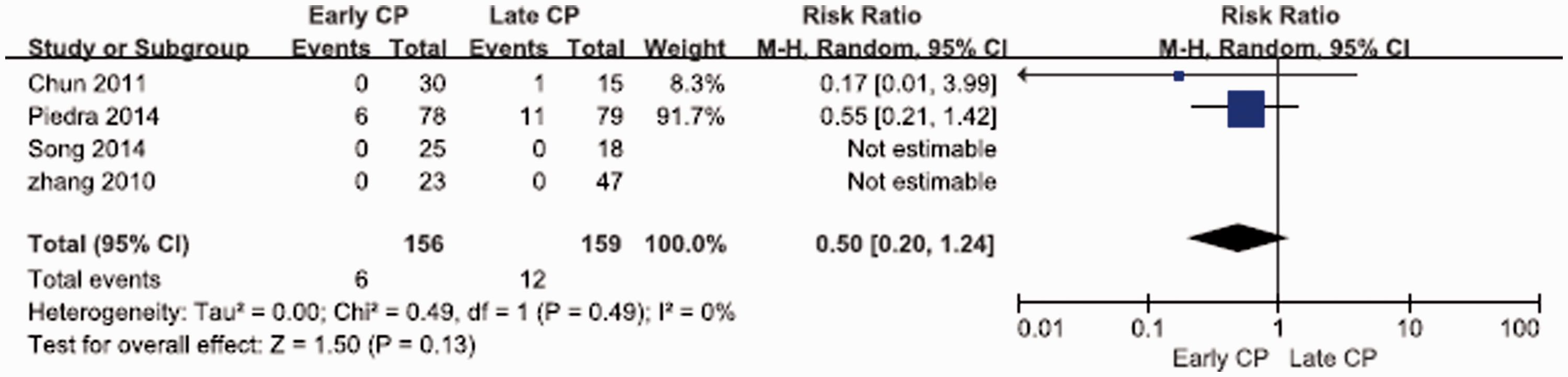
Post-operative infections of early cranioplasty (CP) vs late CP in patients receiving decompressive craniotomy (DC) for traumatic brain injury (TBI).
Two studies6,16 involving a total of 88 patients evaluated post-operative subdural fluid collection and a significant difference between early and late CP groups was found in favour of early CP [RR = 0.24, 95%CI (0.07, 0.78), P < 0.05] (Figure 4).

Postoperative subdural fluid collection of early CP vs late CP in patients receiving decompressive craniotomy (DC) for traumatic brain injury (TBI).
Two studies5,16 involving a total of 202 patients evaluated mean operating time and a significant difference between early and late CP was found in favour of early CP [mean difference = −33.02, 95%CI (−48.19, −17.84), P < 0.05] (Figure 5).

Mean operative time of early CP vs late CP in patients receiving decompressive craniotomy (DC) for traumatic brain injury (TBI).
Discussion
Cranioplasty is a well-established neurosurgical procedure,25,26 and is commonly used following DC surgery. Although the indications and efficacy of DC remain controversial, a large number of DC procedures are now performed worldwide and so many patients undergo subsequent CP.1,27–31
Initially, CP was considered to have a protective and cosmetic role only but recent studies have shown that it also improves neurological function.2,6,18,32 In addition, CP may restore some abnormalities caused by the DC, such as changes in CSF circulation, dynamics of local cerebral blood flow, cerebral metabolic rate of oxygen and glucose changes.6,18,33–35 Moreover, studies suggest that CP contributes to the prevention or recovery of ‘Syndrome of the trephined’ and ‘Craniectomy-associated Progressive Extra-Axial Collections with Treated Hydrocephalus’.10,36,37 These syndromes are recognised complications of DC. However, CP itself is associated with several potential complications, such as infection of central nerve system, subdural fluid collection and hydrocephalus, all of which would lead to prolonged hospital stay and an unfavourable outcome. 38 Therefore, an important concern of the neurological and neurosurgical community is how to minimize or prevent complications linked to CP.5,6,12,14,20
The timing of the CP procedure appears to be important not only in avoiding procedural associated complications but also in the neurological outcome of the patients.5–7,14,20 Nevertheless, the optimal timing of CP following DC remains ill defined. Although, several studies15,20,39–41 have reported that early CP produced a significantly higher complication rate compared with late CP, other studies have shown that early CP produced more favourable results than late CP.2,6,15,18,33 Benefits of late CP include the reduced possibility of surgical wound contamination due to delayed surgery, especially in cases of heavily contaminated open skull fractures, burst skull fractures, or penetrating head injuries. However, one study found that post-operative surgical related infections following CP were more determined by the anatomic location rather than the timing of the procedure. 17
Results from this current meta-analysis, showed that in patients receiving DC for TBI there was no difference between early (<3 months) and late (>3 months) CP in the overall complication rate and post-operative infection rate. These findings are consistent with results from other studies.5,6,13,16 However, there was a significant difference between early and late CP in the incidence of post-operative subdural effusion in favour of early CP. Early repair of the cranial defect could perhaps contribute to the recovery of the normal cerebrospinal fluid circulation.42,43
Another major complication of CP is the possible formation of multiple adhesions between the dura, galea and temporal muscle. 16 The adhesions may lead to subsequent intra-operative complications, such as excessive blood loss, prolonged operating time or inadvertent surgical injury to the dura and cortex. 16 In this current meta-analysis, there was a significant difference between early and late CP in mean operating time in favour of early CP. It has been suggested that early CP allows an easy dissection of tissue planes as there is less scar tissue.16,44 In addition, compared with late CP, early CP has other advantages, such as improvement in neurocognition and neurological functions and reduction of overall costs of care because it decreases the need lengthy hospital stay.14,18,44,45 For example, as soon as there is resolution of brain swelling as observed on Computed tomography (CT) scan and there is no evidence of infection, an early CP can be considered. 44
The study had some limitations. Firstly, no randomized controlled trials were identified in the literature review and the studies included in the meta-analysis were retrospective. Therefore, the results may be subject to observer recall bias. Secondly, patients with continuous intracranial hypertension due to severe TBI cannot undergo early CP which may have influenced the overall results. Thirdly, the duration of follow-up differed between the five studies which may have impacted on the observed complication rates. Finally, two of the outcomes of the present study are based on only two published articles. Therefore, future research is warranted to confirm our results.
In conclusion, although data were only available from five cohort studies, results of the meta-analysis showed that there were no differences between early and late CP in post-operative overall complications and procedural related infections in patients receiving DC for TBI. However, significant differences in favour of early CP were found in rates of subdural effusion and mean operating time.
Footnotes
Acknowledgments
No sources of support that require acknowledgement.
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
This work was supported by Affiliated Hospital of Guangdong Medical University and the National Natural Science Foundation of China (81660211).
