Abstract
Objectives
To identify clinical features that predict Group A streptococcal (GAS) pharyngitis in a Japanese paediatric primary emergency medical centre.
Methods
The prevalence of GAS pharyngitis according to age and body temperature (BT) was calculated among 3098 paediatric patients with pharyngitis. The numbers of GAS-positive and -negative patients for each clinical parameter, and each point increase in the McIsaac score were compared and likelihood ratios (LRs) were calculated.
Results
The prevalence of GAS pharyngitis was extremely low in patients aged < 1 (1.2%) and 1 year (3.9%). The GAS-positive rate was significantly higher in patients with a BT < 38.0°C compared with ≥ 38.0°C (30.0% vs. 19.8%). A BT ≥ 38.0°C was not a predictive finding for GAS pharyngitis (positive LR: 0.82). Rash was the most useful individual predictor, and a McIsaac score of 4 or 5 increased the probability; however, the positive LRs were 1.74 and 1.30, respectively.
Conclusions
The prevalence of GAS pharyngitis is extremely low in patients aged < 1 and 1 year, and a BT ≥ 38.0°C is not a predictive symptom. Although a rash and McIsaac score of 4 or 5 are associated with an increased probability, they cannot be used to confirm GAS infection.
Introduction
Group A streptococcal (GAS) pharyngitis is a common infectious disease in the field of clinical paediatrics. An incidence of 9 to 12 cases per 100 person-years of GAS in children has been reported, 1 with GAS detected in 30% to 40% of cases of paediatric pharyngitis. 2 GAS causes several severe complications, such as acute rheumatic fever, post-streptococcal glomerulonephritis, and paediatric autoimmune neuropsychiatric disorders associated with Streptococcus. 3 Additionally, GAS is easily spread at nurseries and schools. Accurate and prompt diagnosis and treatment for patients with GAS pharyngitis is required not only for individuals, but also for control of public infection. Reducing unnecessary antibiotic use in patients with pharyngitis due to diagnosis of GAS infection is also important.
Because the signs and symptoms of viral and GAS pharyngitis overlap, various attempts to distinguish GAS have been made.4–7 The most widespread clinical prediction tool for GAS pharyngitis in children is the McIsaac score, which consists of the following five parameters: body temperature (BT) > 38°C; lack of a cough; tonsillar swelling or exudate; tender cervical lymph nodes; and age between 3 and 14 years. 8 For prediction of GAS pharyngitis, these clinical signs and symptoms, and the McIsaac score are controversial. Different results among studies can be explained by variations in study settings and participants. 7 Studies investigating predictive factors to distinguish GAS pharyngitis are required in various settings and participants. These studies are especially needed in paediatric emergency departments where many paediatric patients with pharyngitis present at the same time and undergo antigen detection tests using pharyngeal swabs. Moreover, there have been a limited number of studies that examined factors predictive of GAS pharyngitis in Japan. 9
To clarify the clinical features of GAS pharyngitis, the objectives of this study were as follows: to determine and analyse the prevalence of GAS pharyngitis according to age and BT; to identify clinical signs and symptoms that could distinguish patients with GAS infection from those with pharyngitis; and to validate the utility of the McIsaac score in a Japanese paediatric primary emergency medical centre.
Patients and methods
Study design and setting
A large retrospective cohort study involving 142,018 patients ≤ 15 years of age who visited the Kobe Children’s Primary Emergency Medical Center, Kobe, Japan, between December 1, 2010 and July 31, 2015 was conducted. This centre provides medical services for paediatric patients by more than 100 paediatricians during holidays and outside of working hours. Clinical data were obtained from medical charts and analysed based on approved study methods. This study was approved by the Ethics Committee of Kobe Children’s Primary Emergency Medical Center (No. 57-5 [approved November 7, 2014]). We opened this study project to the public using our homepage. Therefore, the need for formal informed consent of individual participants was waived. All of the procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee, and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Data collection
Clinical findings that were previously reported to be predictors of GAS infection4,6 were retrospectively collected. Symptoms, such as fever and cough, were based on medical interview sheets that were completed by patients or their family members. Physical findings, including rash, tonsillar swelling, tonsillar exudate, swollen cervical lymph nodes, and BT at visit, were collected from electronic medical charts.
Detection method for GAS
The rapid antigen detection test (Quicknavi™-Strep A, Denka Seiken Co., Ltd., Niigata, Japan), which is based on an immunochromatography method, was used for detecting GAS from pharyngeal swab samples. The medical package insert showed that the sensitivity and specificity of the Quicknavi™-Strep A compared with the culture method was 0.99 and 0.98, respectively. Patients were diagnosed as GAS-positive when a positive band was detected in this test.
Patients and methods
This study investigated three primary objectives, the first of which was determining the prevalence of GAS pharyngitis. Of the 142,018 paediatric patients who visited during the study period, 3098 (2.2%) patients with pharyngitis were tested for GAS because they showed symptoms of acute pharyngitis, including fever or a sore throat (cohort A, Figure 1). The diagnosis was conducted based on clinical findings, such as a sore throat or redness of the pharynx. The prevalence of GAS pharyngitis in patients with pharyngitis according to age and BT at the visit to the centre were calculated and compared.
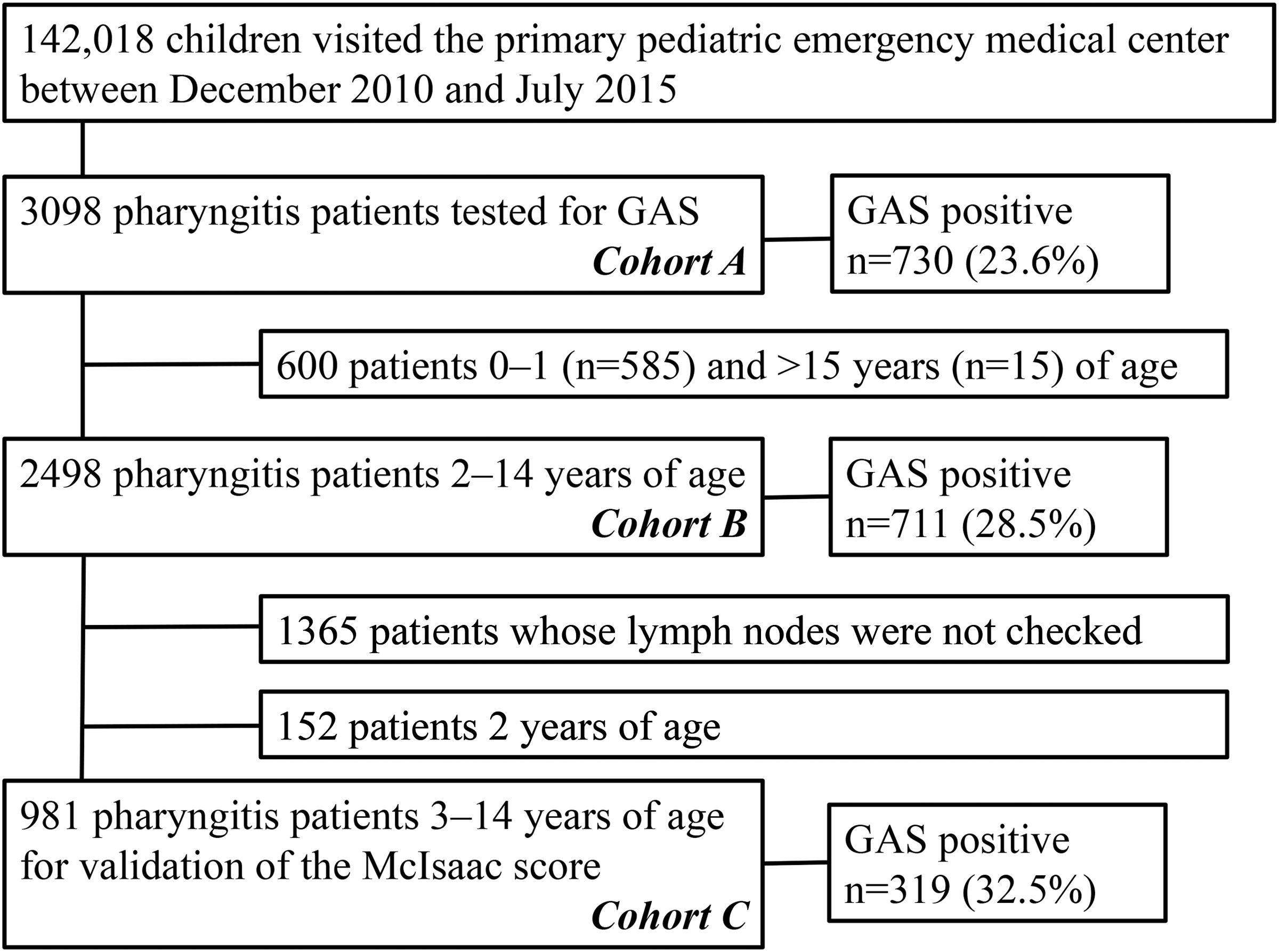
Flow chart of the patients.
Second, predictors of GAS pharyngitis were examined in a cohort that excluded 600 patients (0–1 [n = 585] and > 15 years of age [n = 15]) from cohort A (cohort B) because GAS positivity was extremely low in our results and previous reports 2 (Figure 1). The numbers of GAS-positive and -negative patients in cohort B for each clinical parameter were statistically compared and the positive and negative likelihood ratios (LRs) were calculated. Moreover, the numbers of GAS-positive and -negative patients for combined clinical parameters, which were selected based on the results of individual parameter analysis, were compared.
Third, patients with pharyngitis aged 3 to 14 years of age were selected for a validation study of the McIsaac score. This age range is an important predictive factor for GAS in the McIsaac score. 8 Patients whose lymph nodes were not checked were excluded because a tender cervical lymph node is one of the four parameters in the McIsaac score, except for the parameter of age. A total of 981 patients with pharyngitis aged 3 to 14 years were examined and scored for the four parameters included in the McIsaac score (BT > 38°C, lack of a cough, tonsillar swelling or exudate, and tender cervical lymph nodes) (cohort C, Figure 1). The number of GAS-positive and -negative patients in each score category (1, 2, 3, and 4 or 5) were statistically compared, and positive and negative LRs were calculated.
Statistical analyses
Statistical comparisons were performed using the chi-square test (JMP version 11.0 [SAS, Inc., Tokyo, Japan]). Positive and negative LRs and 95% confidence intervals (CIs) were calculated for prediction and validation of the study. A value of p < 0.05 was considered to be statistically significant.
Results
Prevalence of GAS pharyngitis
Of the 3098 patients who were tested for GAS (cohort A), 730 (23.6%) were GAS-positive (Figure 1). There was no sex difference in developing GAS pharyngitis. The age-specific rates of GAS positivity in cohort A are shown in Figure 2. These rates increased from 1.2% (2/171) at < 1 year old, to 3.9% (16/414) at 1 year old, and peaked at 6 years old (37.7% [106/281]). Thereafter, these rates decreased until 13 to 15 years of age (12.9% [12/93]). The GAS-positive rate in patients aged 2 to 15 years old (28.3% [712/2513]) was significantly higher than that in patients aged 0–1 years (3.1% [18/585]) (p<0.001).

Patients tested for Group A Streptococcus (GAS) and the GAS-positive rate according to age.
The prevalence of GAS according to BT is shown in Figure 3. The GAS-positive rate peaked at 33.3% (258/774) in patients with a BT of 37°C to 37.9°C. The GAS-positive rate in patients with a BT < 38.0°C was significantly higher than that in those with a BT at ≥ 38.0°C (30.0% vs. 19.8%, p < 0.001).

Patients tested for Group A Streptococcus (GAS) and the GAS-positive rate according to body temperature measured at the visit to the centre.
Predictors of GAS pharyngitis
Comparison of the numbers of GAS-positive and -negative patients for each clinical parameter in cohort B is shown in Table 1. Of the 2498 children in this cohort, 711 (28.5%) were GAS-positive (Figure 1, Table 1). All clinical parameters, except for fever, were significantly associated with GAS positivity. GAS-positive patients showed a significantly higher presentation rate of rash (p < 0.001), swollen cervical lymph nodes (p = 0.027), abnormal tonsillar findings (p < 0.001), visiting the centre between November and May (p < 0.001), and a lack of a cough (p < 0.001) compared with GAS-negative patients. Of these parameters, the positive LR for rash was highest (1.74 [95% CI 1.52–1.99]). In contrast, the positive LR of a BT ≥ 38.0°C was < 1.0 (0.82 [95% CI 0.76–0.89]). Comparison of the numbers of GAS-positive and -negative patients for combined clinical parameters is shown in Table 2. The positive LR in cases of rash, abnormal tonsillar findings, and visiting the centre between November and May was the highest (3.77 [95% CI 2.72–5.22]).
Comparison of the number of Group A Streptococcus-positive and -negative patients for each clinical parameter in cohort B.

Data are presented as n (%) unless otherwise indicated. *The numbers of GAS-positive and -negative patients with pharyngitis whose lymph nodes were checked by an attending paediatrician were 335 and 798, respectively. GAS, Group A Streptococcus; LR, likelihood ratio; CI, confidence interval.
Comparison of the number of Group A Streptococcus-positive and -negative patients for combined clinical parameters in cohort B.

Data are presented as n (%) unless otherwise indicated. GAS, Group A Streptococcus; LR, likelihood ratio; CI, confidence interval.
Validation of the McIsaac score
The overall GAS-positive rate in cohort C was 32.5% (319/981) (Figure 1, Table 3). The GAS-positive rate was 31.6% (12/36) in individuals with a McIsaac score of 1, 26.7% (58/218) with a score of 2, 30.8% (123/400) with a score of 3, and 38.5% (126/327) with a score of 4 or 5; these differences were significantly different among the scores (p = 0.024). A McIsaac score of 4 or 5 significantly predicted GAS positivity, but the positive LR was low (positive LR: 1.30 [95% CI 1.09–1.55]).
Comparison of the number of Group A Streptococcus-positive and -negative patients according to the McIsaac score in cohort C.

Data presented as n (%) unless otherwise indicated. GAS, Group A Streptococcus; LR, likelihood ratio; CI, confidence interval.
Discussion
This was the largest Japanese study to investigate clinical signs and symptoms for predicting GAS pharyngitis in a paediatric primary emergency medical centre. We found that the prevalence of GAS infection in children with pharyngitis differed according to age and was extremely low in patients aged approximately 1 month to 1 year old. We also found that the prevalence of GAS infection was lower in patients with pharyngitis with a BT ≥ 38°C than in those with a BT < 38°C. Moreover, a body temperature ≥ 38.0°C was not predictive for GAS pharyngitis. Third, rash was the most useful individual predictive parameter of GAS positivity, and although a McIsaac score of 4 or 5 significantly increased the probability of GAS pharyngitis, the positive LR of these factors was < 2.0.
This study clearly demonstrated that the prevalence of GAS infection in patients with acute pharyngitis differed according to age. Previous studies reported that the prevalence of GAS infection in patients with pharyngitis was higher in school-age children than in adults and preschool-age children.10–13 However, studies that investigated the prevalence of GAS infection in paediatric pharyngitis (<3 years of age) are limited. Gunnarsson et al. 14 reported a prevalence of GAS infection of 18% in 40 patients with pharyngitis aged 0 to 2 years. Conversely, Lin et al. 13 reported a prevalence of 0% in 70 patients with pharyngitis aged ≤ 2 years. However, the number of patients in these studies was small.13,14 Our study showed that the GAS-positive rate was only 1.2% at < 1 year old, 3.9% at 1 year old, and 13.0% at 2 years old, among more than 900 patients in this population. Our results clearly demonstrated that the prevalence of GAS infection was extremely low in patients aged 0–1 year old. This finding suggests that physicians should be aware of this low positive rate when treating patients with pharyngitis aged 0–1 year.
Another surprising finding in our study was the lower prevalence of GAS pharyngitis in patients who presented with a BT ≥ 38°C compared with those with a BT < 38°C. This finding is not consistent with previous studies involving adults or children > 3 years of age, with high-grade fever as a positive predictive finding.8,15 We speculate that a reason for the low positive rate of GAS in pharyngitis in patients with high-grade fever in our study may be that physicians tended to suspect GAS infection in cases of high-grade fever based on their knowledge of previous reports. Nevertheless, many patients who may have been exposed to environments that are favourable to transmission of GAS, such as exposure to siblings with GAS pharyngitis at home or classmates at school, were examined for GAS, despite the lack of high-grade fever. A body temperature ≥ 38.0°C was not a predictive finding for GAS pharyngitis in our study of paediatric patients aged 2 to 14 years. Our results suggest that high-grade fever alone is not a predictor of GAS infection.
Except for a BT ≥ 38.0°C, all of the clinical findings that were previously reported as predictors4,6 increased the probability of GAS positivity in the following order: rash, swollen cervical lymph nodes, abnormal tonsillar findings, visiting between November and May, and lack of a cough. The positive LR value for rash (1.74) was the highest among the symptoms. This finding is consistent with the results of a previous meta-analysis, which reported that scarlatiniform rash was the most useful symptom for identifying patients with GAS pharyngitis. 6 However, individual signs or symptoms are insufficient to identify GAS positivity because a positive LR > 5 (i.e., > 30% increase in probability) is generally required to include disease. 16 Several previous studies have proposed swollen cervical lymph nodes as an important sign and symptom for identifying patients with GAS pharyngitis.5–8,15,17 However, attending paediatricians in our centre examined the cervical lymph nodes in only 45% of the 2498 patients with pharyngitis in cohort B. Japanese paediatricians, even in a primary medical emergency centre where many patients visit at the same time, should examine the cervical lymph nodes of patients with pharyngitis by palpating with the hands.
We also found that a high McIsaac score (4 or 5) increased the probability of GAS positivity in pharyngitis patients aged 3 to 14 years. However, the positive LR value of a McIsaac score of 4 or 5 in our study (1.30) was significantly lower than that for a McIsaac score ≥ 4 that was previously found (6.43). 8 Our results are consistent with a meta-analysis, which concluded that the McIsaac score was not useful in diagnosing GAS pharyngitis (positive LR: 1.48 for a score of 4; 2.52 for a score of 5). 6 However, a combination of selected clinical parameters was more useful for predicting GAS pharyngitis than the McIsaac score in our study. The positive LR value of a combination of rash, abnormal tonsillar findings, and visiting between November and May was 3.77. However, the usefulness of this combination might be limited because the analysed cases comprised only 5.6% (140/2498) of the patients.
The present study has several limitations, the first of which was its retrospective design, which limited the analysis of clinical parameters. Second, our study was performed at a single institution, which may have introduced selection bias by the attending physicians. However, because more than 100 paediatricians worked at our primary emergency medical centre during the study period, any bias introduced by individual physicians would have been relatively small. Finally, a rapid antigen detection test, which can be practically useful in primary care settings, is not as efficacious as a throat bacterial culture. The sensitivity and specificity of a rapid antigen detection test for GAS were estimated to be 0.86 and 0.96, respectively, in a meta-analysis that involved a paediatric population. 18
Conclusions
The present study shows a low prevalence of GAS infection in patients with pharyngitis aged < 1 to 1 year. The prevalence of GAS infection is also lower in patients with pharyngitis with a BT ≥ 38°C compared with that in those with a BT < 38°C. Although a rash and a high McIsaac score are important signs in predicting GAS infection in many patients with pharyngitis, they cannot be used alone to diagnose GAS pharyngitis.
Footnotes
Acknowledgements
The authors thank Ms. Y. Hanabata for secretarial assistance.
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
A grant for Scientific Research (C) of JSPS KAKENHI (Grant Number: JP26461632, I.M.) supported the English language editing of this manuscript.
