Abstract
Objective
The GlideScope® videolaryngoscope provides a good view of the glottis. However, directing and inserting an endotracheal tube is sometimes difficult during intubation with the GlideScope®. In this study, we compared two GlideScope® stylet angulations (90° vs. 70°) in terms of the time to intubation.
Methods
In total, 162 patients scheduled for elective surgery under general anaesthesia were randomly assigned to one of two groups. In the 90 group (n = 79), a 90° stylet was used. In the 70 group (n = 78), a 70° stylet was used. The time to intubation was recorded. The number of intubation attempts was assessed.
Results
The time to intubation was significantly shorter in the 70 than 90 group [26.0 (23.0–32.0) vs. 37.0 (30.0–43.0) s, respectively]. The first-time intubation success rate was significantly higher and the number of failed intubations was significantly lower in the 70 than 90 group (100% vs. 87% and 0% vs. 6%, respectively).
Conclusions
This investigation suggests that a 70° angle stylet is superior to a 90° angle stylet for GlideScope® intubation.
Keywords
Introduction
The GlideScope® videolaryngoscope (GL) (Verathon Medical Inc., Bothell, WA, USA) is a special intubation device that provides an optimal view of the glottis.1,2 Although the video images obtained by the GL allow the operator to visualise the entire glottic structure, insertion of the endotracheal tube (ETT) can be difficult. GL intubation necessitates placement of the stylet in the ETT because of the 60° distal curvature of the GL blade. 3 Various types of stylets, including 60°, 90°, and J-shaped varieties, have been investigated with respect to facilitation of GL intubation.3,4 An inappropriate stylet angle or shape may lead to failed intubation attempts, which causes airway trauma and oedema. The optimal stylet design for GL intubation has yet to be identified.
Previous studies using the GL demonstrated that stylets with a 90° angle decreased the time to intubation (TTI) compared to those with a 60° angle.3,5 In GL intubation with a 90° angle stylet, however, 7% of patients were not intubated at the first intubation attempt. 3 The TTI with the GL is slower than that with direct laryngoscopy because of manipulation of the stylet and ETT. 2 The optimal shape and angle of the stylet required for successful GL intubation with a shorter TTI is unknown.
In this study, we compared the efficacy of 70° and 90° stylets for GL intubation in terms of the TTI, success rate, and incidence of postoperative airway complications.
Methods
Study population
This trial, which used a single-centre parallel-group randomised design, was performed at Keimyung University Dongsan Medical Center in Daegu, South Korea from October 2015 to January 2016. This investigation was registered at ClinicalTrials.gov (registration no.: NCT02547064) before enrolment of any patients. After receiving approval from the Institutional Review Board of Keimyung University (document no. 2015-09-003), written informed consent was obtained from all patients. Patients aged 18 to 80 years with an American Society of Anesthesiologists physical status of I to III and who were scheduled for elective surgery under general anaesthesia were enrolled. The exclusion criteria were as follows: a history of difficult airway, recent sore throat, friable teeth, head and neck surgery, requirement for rapid-sequence induction, or a contraindication for GL as determined by the attending anaesthesiologist. Anaesthesiologists (H.C.K., J.L., and J.D.S.) who had experience with more than 100 GL intubations using 70° and 90° angle stylets performed the intubations in this trial.
Study procedures and anaesthesia
The ETTs with stylets were prepared by a nurse who was blinded to the trial protocol (Figure 1). The ETT with the 70° angle stylet was prepared as follows: the ETT was bent by 60° at a point 10 cm from its distal end and by an additional 10° at a point 6 cm from its distal end to facilitate directing the distal tip of the ETT toward the vocal cords. The proximal portion of the ETT was formed in the shape of the GL blade until reaching the point of the handle to facilitate insertion of the ETT into the oral and pharyngeal cavity. The additional 10° at the 6-cm point helped to direct the tip of the ETT anterior to the vocal cords. The ETT with the 90° angle stylet was bent at a point 8 cm from its distal end. 3 The 70° and 90° angle stylets were prepared using a standardised template to ensure uniformity throughout the investigation.

(a) The two endotracheal tubes (ETTs) with stylets are shown: 70° (top) and 90° (bottom). The ETT with the 70° angle stylet was prepared as follows: the ETT was bent by 60° at a point 10 cm from its distal end and by an additional 10° at a point 6 cm from its distal end to facilitate directing the ETT distal tip toward the vocal cords. The proximal portion of the ETT was formed in the shape of the GlideScope® blade until the point of the handle was reached. The ETT with the 90° angle stylet was bent at a point 8 cm from its distal end. (b) The ETT with the 70° angle stylet and an illustration of the GlideScope® blade.
Patients were assigned to one of two groups. Randomisation was performed using Random Allocation Software, ver. 1.0.0 (Isfahan University of Medical Sciences, Isfahan, Iran). Group assignments were concealed in opaque envelopes and opened immediately before each patient entered the operating theatre. In the 70 group, the 70° angle stylet was used; in the 90 group, the 90° stylet was used. According to our institution’s protocol, an ETT with an internal diameter of 7.5 mm was chosen for male patients, and an ETT with an internal diameter of 7.0 mm was selected for female patients. The ETT with stylet was created by the investigator of the present study, who was not involved in subsequent patient care or outcome evaluations, according to a template.
The patients were transferred to the operating room with no premedication. Each patient’s Mallampati score and thyromental distance were assessed before the surgery by the attending anaesthetist. Basic monitoring including electrocardiography, oxygen saturation, and noninvasive blood pressure was performed. Preoxygen-ation was performed and anaesthesia was induced with propofol (2 mg/kg) and sufentanil (0.5 μg/kg). Rocuronium (0.8 mg/kg) was infused to facilitate intubation. After 100 s of mask ventilation with 100% oxygen, GL intubation was performed (ETT with 90° or 70° stylet). GL intubations were performed using the GL Four-Step Technique. 6 First, the GL was introduced while looking directly into the patient’s mouth. Second, the best glottic view was obtained while looking at the screen. Third, the ETT was introduced up to the tip of the GL blade while looking into the mouth. Finally, the ETT was redirected and intubation was completed while looking at the monitor. External laryngeal manipulation using bimanual laryngoscopy 7 was performed to improve the glottic view or adjust the position of the ETT tip relative to the vocal cords. The glottic view was graded using the Cormack–Lehane classification system 8 and the percentage of glottic opening (POGO) score. 9 After insertion of the ETT, the presence of laryngeal injury such as petechiae, laceration, and bleeding was checked using the GL and direct visualisation by the investigator, who was blinded to the group assignments. The difficulty of intubation was assessed by the operator on a 100-mm visual analogue scale (VAS) (0 = easiest, 100 = most difficult). 3 Haemodynamic variables, such as the blood pressure and heart rate, were recorded before and 2 min after intubation. Anaesthesia was maintained with desflurane 6% to 9% in oxygen and air. After extubation, blood staining on the ETT was evaluated by the investigator, who was blinded to the group assignment. Sore throat was assessed at 1 and 24 hours postoperatively using a 100-mm VAS by the investigator, who was blinded to the group assignment.
Outcome measurements
The primary endpoint was the TTI, which was recorded by a blinded anaesthetist. The TTI was defined as the time from the GL passing the lips until the end-tidal carbon dioxide reached at least 30 mmHg. 3 The blinded anaesthetist watched the patient until the evaluation started, after which they turned to watch the monitor and did not observe the ETT. Intubations that took ≥150 s were considered failures; in such cases, the intubation modality was changed. Failed intubations were included in the analysis (recorded as a TTI of 150 s). The secondary endpoints were the first-time success rate, intubation difficulty, number of failures, external laryngeal manipulation, haemodynamic variables (mean blood pressure and heart rate) before and 2 min after intubation, Cormack–Lehane grade, POGO score, incidence of larynx injury and blood on the ETT, and numeric pain score (NPS) (0 = no pain, 100 = worst pain imaginable) of postoperative sore throat at 1 and 24 h postoperatively.
Statistical analysis
The sample size calculation was based on a previous report by Jones et al., 3 in which the TTI in GL intubation with the 90° stylet was 47 ± 21 s. We assumed that a 10-s decrease in the TTI would be clinically relevant and calculated that a sample size of 69 patients would be needed in each group (type I error of 0.05, power of 0.8). Considering a 10% dropout rate and 95% compliance rate, 81 patients in each group were necessary. Statistical analysis was performed using IBM SPSS® Statistics software, ver. 22.0 (IBM Corp., Armonk, NY, USA). The TTI and intubation difficulty score were compared using the Mann–Whitney U test after the Kolmogorov–Smirnov test. Continuous variables including age, body mass index, operation time, haemodynamic variables, thyromental distance, POGO score, and NPS of postoperative sore throat were compared using Student’s t-test after a normality test. The first-time success rate, external manipulation, laryngeal injury, and blood staining on the ETT were assessed using the chi-squared test or, if there were ≤5 values per cell, Fisher’s exact test. The alpha value was adjusted with Bonferroni’s correction to compare postoperative sore throat between the two groups at each time point. The p values were compared with these adjusted alpha values. Otherwise, a P value of <0.05 was taken to indicate a significant difference. Data are presented as mean ± standard deviation or number (percentage).
Results
In total, 162 patients were enrolled in this study (Figure 2). Four patients were excluded, and 1 patient in the 90 group did not receive the allocated intervention (1 had no record of the TTI on the data sheet), leaving 157 patients in the final analysis. There were no differences in patient demographics between the two groups (Table 1, Figure 3). The TTI in the 70 group was shorter than that in the 90 group [26.0 (23.0–32.0) vs. 37.0 (30.0–43.0) s, respectively; difference, 19.9 s; 95% confidence interval [CI] of difference, 7.3–25.1 s; P < 0.001] (Table 2). A Kaplan–Meier plot showing the percentage of patients successfully intubated confirmed that the 70 group required a shorter TTI during the intubation (P < 0.001) (Figure 4). The first-time success rate was higher in the 70 than 90 group (100% vs. 87%, respectively; difference, 13%; 95% CI, 4%–23%; P = 0.001). In the 90 group, four and one patient was intubated after the second and third GL intubation attempts, respectively. The number of failed intubations was lower in the 70 than 90 group (0% vs. 6%, respectively; difference, 8%; 95% CI, −1%–15%; P = 0.028). Among five failed intubations, the thyromental distance was 55 mm in one patient. One patient showed a Mallampati grade of 3 and POGO score of 30%. The Mallampati grade was 4 in one patient. The POGO score was 0% in one patient. Among the five failed intubations in the 90 group, intubations were performed successfully using 70° stylets. External manipulation was used less often in the 70 than 90 group (4% vs. 18%, respectively; difference, 14%; 95% CI, 3%–25%; P = 0.005).
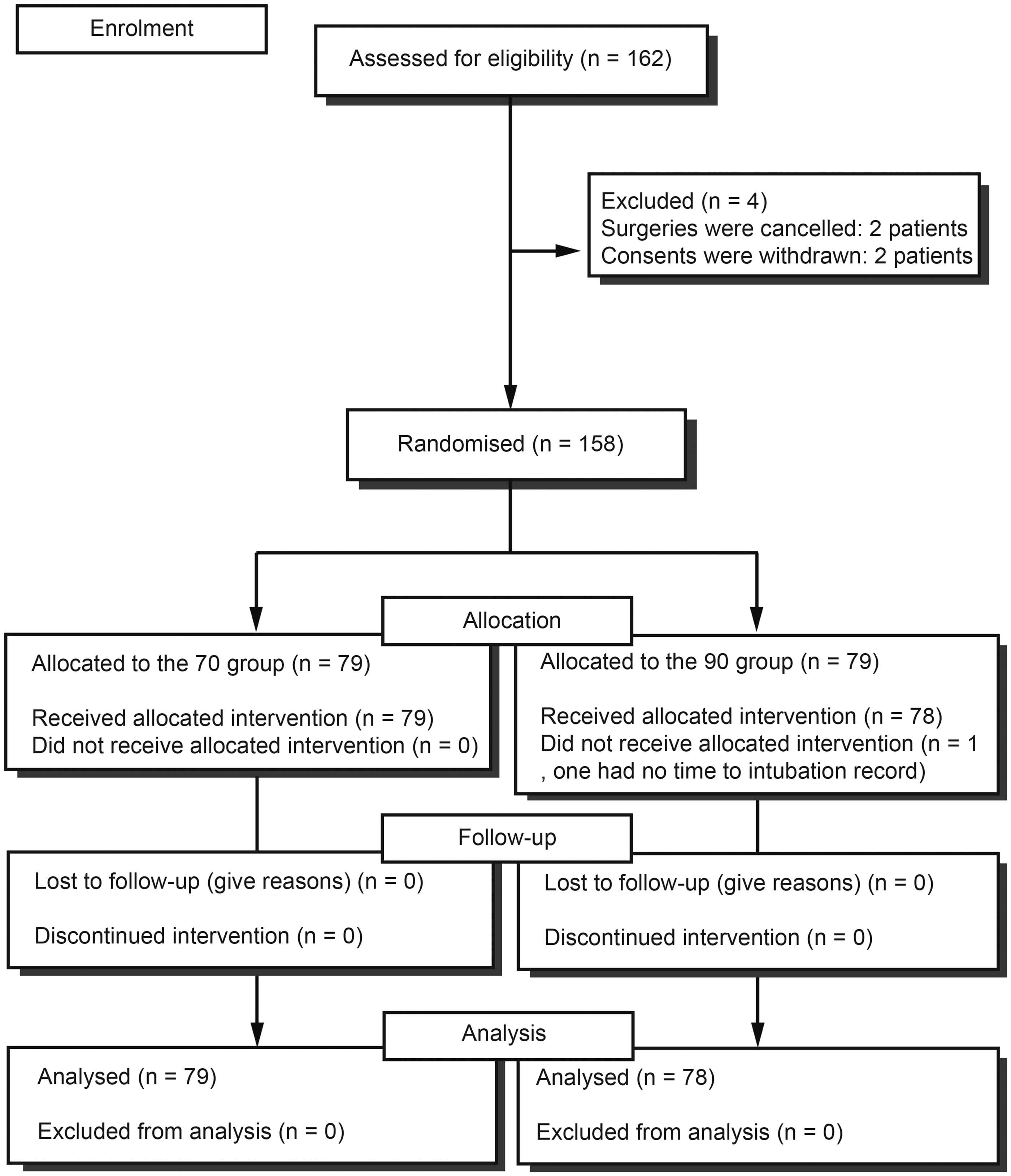
CONSORT diagram showing the flow of patients through the phases of the trial.
Baseline patient characteristics
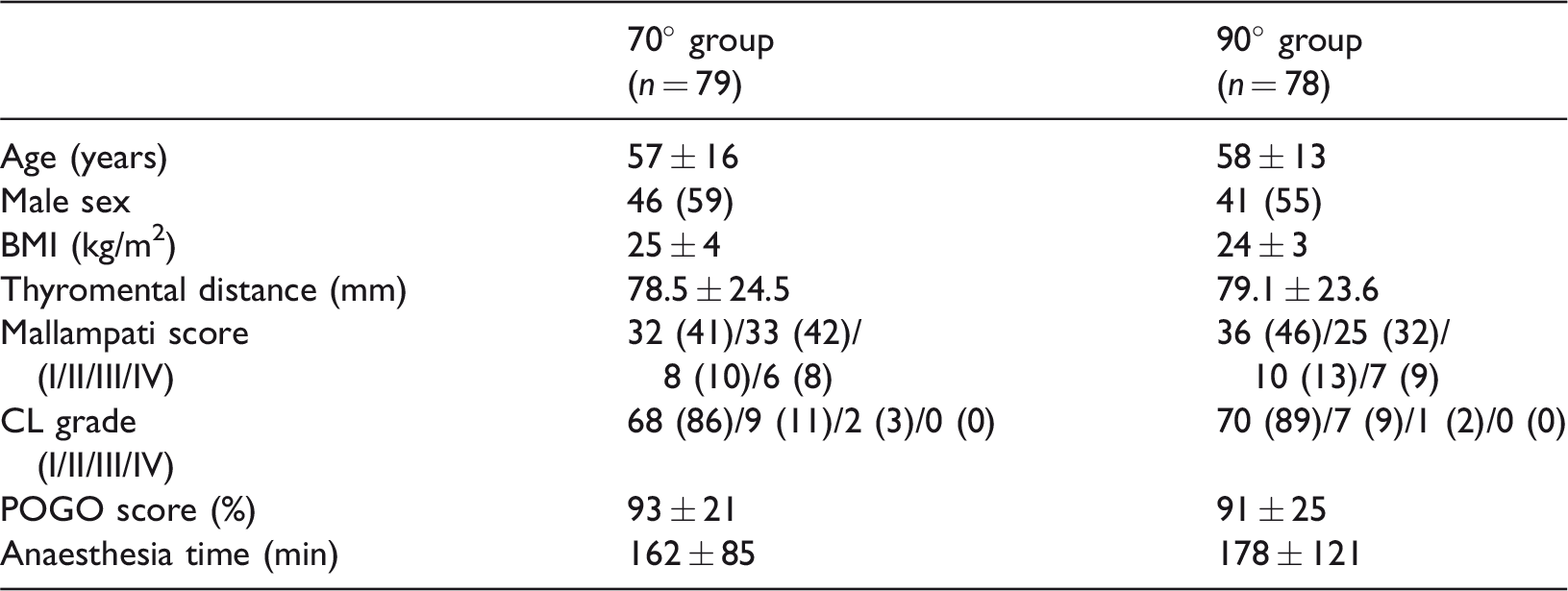

Data are presented as mean ± standard deviation or n (%).
BMI, body mass index; CL, Cormack–Lehane; POGO, percentage of glottis opening.
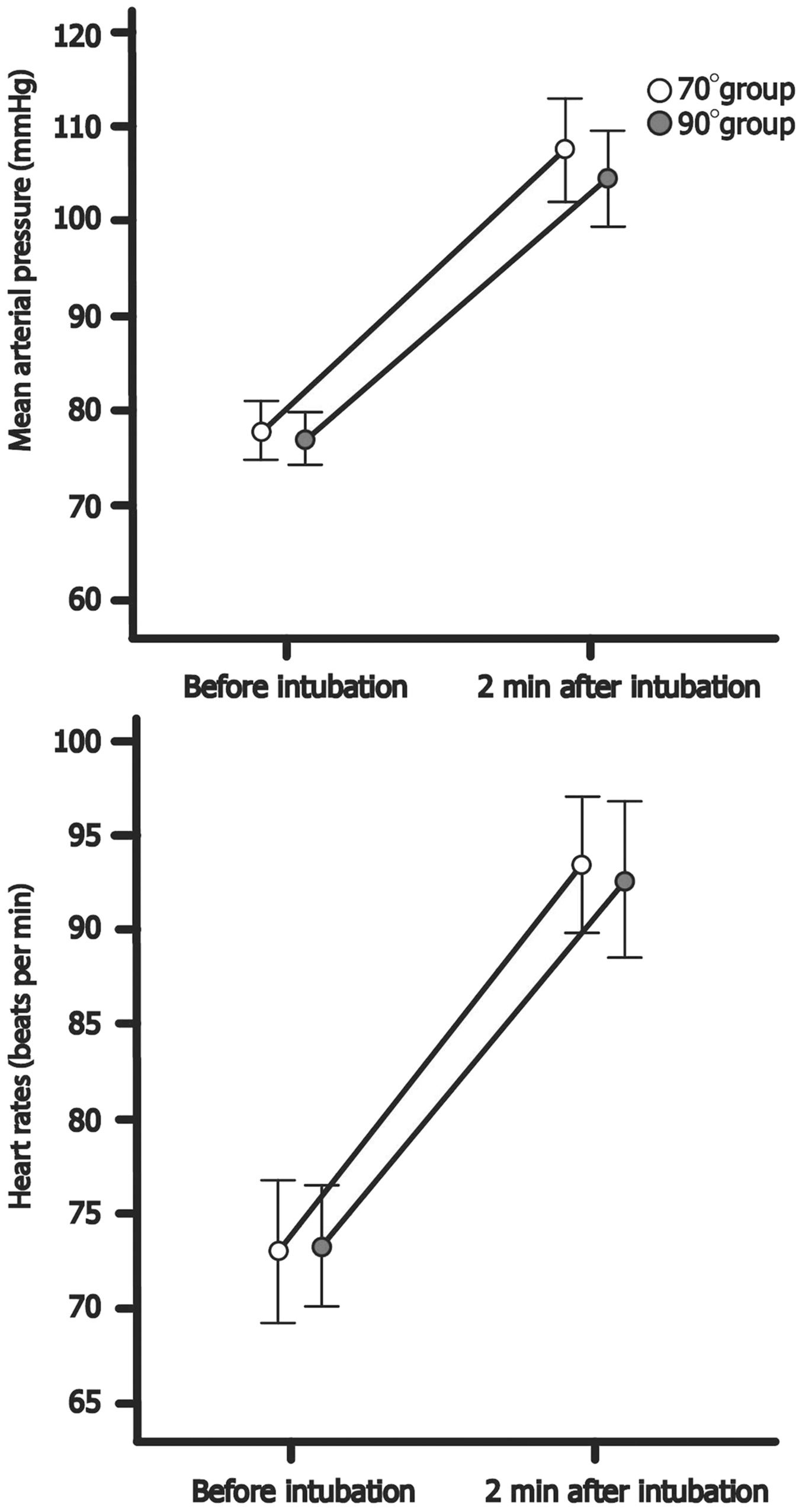
Haemodynamic variables before and 2 min after GlideScope® intubation.

Kaplan–Meier plot of time to intubation for patients using the 70° or 90° stylet. The log-rank test showed a significant difference between the groups (P < 0.001).
Intubation data of patients intubated by the GlideScope® using a 70° or 90° angle stylet

Data are presented as median (interquartile range), mean ± standard deviation, or n (%). The time to intubation and the intubation difficulty score were compared using the Mann–Whitney U test after the Kolmogorov–Smirnov Z test.
The incidence of larynx injury was lower in the 70 than 90 group (0% vs. 6%, respectively; difference, 6%; 95% CI, −1%–15%; P = 0.028) (Table 3). All larynx injuries involved mild petechiae. The incidence of blood-stained ETTs was comparable between the two groups. The NPS of sore throat at 1 and 24 h postoperatively was not significantly different between the two groups.
Complications related to ETT intubation by GlideScope® using the 70° vs. 90° angle stylet

Data are presented as n (%) or mean ± standard deviation.
ETT, endotracheal tube; NPS, numeric pain score
Discussion
This investigation showed that the 70° stylet decreased the TTI and increased the first-time success rate during GL intubation. The 70° stylet also had other advantages over the 90° stylet, including lower intubation difficulty and fewer external manipulations and postoperative airway complications.
The GL is widely used for airway management in routine clinical or emergency situations.10–12 Although the GL provides a good glottic view, the TTI required for GL intubation is longer than that required for direct laryngoscopy because of the difficulty in manipulating the stylet and ETT. 2 A relatively long TTI may increase the risk of hypoxaemia. In our study, the use of 90° stylets required a TTI of 47.2 ± 35.8 s, which is in agreement with a previous study reporting a TTI of 47.1 ± 21.2 s. 3 Furthermore, GL intubation with 70° stylets decreased the TTI by 26% compared with that achieved with 90° stylets. The Kaplan–Meier plot showing the proportion of patients successfully intubated over time confirmed that the TTI in the 70 group was superior to that in the 90 group at all time points. The proximal part of the 70° stylet followed the shape of the GL blade, and the distal part was angled at 70°. Thus, the proximal part of the 70° stylet may facilitate introduction of the ETT into the area viewed on the GL monitor and minimise obstruction of the glottic view compared with the 90° stylet. In the above-mentioned previous investigation, 3 however, the TTI when using the 60° stylet was longer than that when using the 90° stylet in GL intubation. Additionally, GL intubation with the 60° stylet was associated with more failure cases GL intubation that with the 90° stylet. 3 The authors suggested an inability to pass the ETT through the vocal cords. The 70° stylet in the present study is similar to the 60° stylet used in the previous study. 3 The 70° stylet in this investigation, however, had an additional 10° angulation to enhance anterior movement of the ETT toward the vocal cords, which may decrease the TTI and increase the first-time success rate. Our findings suggest that the 90° stylet can be replaced by the 70° stylet to decrease the TTI in GL intubation.
Insertion of the ETT on the first attempt is important to provide adequate oxygenation and ventilation. Multiple attempts of laryngoscopy can cause tissue injury, oedema, bleeding, difficulty of mask ventilation, hypoxaemia, oesophageal intubation, regurgitation, and cardiac arrest.13,14 Previous reports have demonstrated a first-attempt GL intubation failure rate of 8% to 10%.3,15 Despite the good glottic view, the inability to pass the ETT through the vocal cords may result in a failed GL intubation. 3 In the present study, the first-time success rate with the 90° stylet during GL intubation was 87%, which is consistent with a previous study reporting an 81% to 90% first-time success rate.3,15,16 GL intubation with the 70° stylet showed a significantly higher first-time success rate than that performed with the 90° stylet. These results suggest that used of a 70° stylet during GL intubation can be an ideal choice to increase the first-time intubation success rate compared with the 90° stylet.
GL intubation with a 90° stylet took more than 150 s in five patients. This result is in line with a previous report showing a 7% failure rate. 15 In cases of GL intubation failure with a 90° stylet, successful GL intubation was subsequently achieved using a 70° stylet. Changing the intubation modality during airway management may increase both the intubation and anaesthetic time. A delay between mask ventilation and intubation may induce hypoxaemia in patients with a low functional residual capacity, inadequate preoxygenation, or high oxygen consumption. 17 Considering that the GL may be used for difficult airway management or rescue intubation after failure, a 70° stylet may be recommended to decrease the risk of hypoxaemia.
The POGO score in this study was 91% or 93%, which is consistent with that in previous reports. 18 In our study, the intubation difficulty scores were lower when using the 70° stylet, which suggests that the ETT passes the vocal cords more easily with a 70° than 90° stylet.
Two palatopharyngeal arch injuries caused by styletted ETTs were reported in a previous study on GL intubation. 19 In these cases, the operator’s visual attention may have been diverted from the mouth to the GL monitor, leading to pharyngeal damage. In the present trial, we observed no serious injuries to laryngeal or pharyngeal structures. The insertion technique 6 recommended by the manufacturer was strictly followed to prevent damage caused by the styletted ETT; this may explain the lack of pharyngeal damage observed in our study.
Although stylets can facilitate manoeuvring of an ETT, their rigidity may cause airway injury during intubation. 20 More minor laryngeal injuries were detected and more external manipulations were applied in the 90 group of the present study. Directing the styletted ETT anteriorly and the larynx posteriorly by external pressure may result in larynx petechiae when using an ETT with a 90° stylet.
Our investigation has several limitations. First, the operators who performed the GL intubations were not completely blinded. This may have introduced bias to variables such as the TTI and success rate. However, the operator was blinded until the moment of intubation, and the individual who assessed the outcomes was also blinded. Second, it can be difficult to reproduce intubation using the 70° stylet, and the operation may be more time-consuming. In the clinical setting, an ETT with a 70° curvature may be impractical without using an ETT template. Thus, preformed reusable stylets or a template for the 70° curvature may be required. Third, patients with potentially difficult airways were excluded because of ethical issues. Thus, the result of this investigation cannot be applied to patients with difficult airways. Further studies on GL intubation in difficult cases are required. Fourth, our study was performed using the second-generation GL. Therefore, the results of this study may not be applied to those achieved with other generations of the GL or other types of videolaryngoscopes. Fifth, the operators who performed the intubations in this investigation had vast experience in GL intubations, and the patients were expected to have a normal airway. The results may differ in other settings such as the performance of GL intubations by novices for patients with difficult airways. Future investigations of GL intubations by novices or GL intubations in patients with difficult airways are needed. Finally, only two stylet configurations were tested in this study. ETT stylets have many possible angles and angulation points. We did not compare the 70° stylet with the 60° stylet used in the above-mentioned previous investigation 3 because of a lack of resources. Further investigation is needed to determine the optimal shape of the stylet for GL intubation.
Conclusion
This investigation demonstrated that GL intubation with a 70° stylet results in a shorter TTI, number of intubation failures, intubation difficulty, and laryngeal injuries and an increase in the first-time intubation success rate. These results suggest that the 70° stylet is superior to the 90° stylet for GL intubation. We therefore recommend use of the 70° stylet for GL intubation.
Footnotes
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research was supported by a Keimyung University Research Grant (No. 20160026).
