Abstract
Objective
Adipose-derived stromal vascular fractions (SVFs) are heterogeneous complex populations of cells with therapeutic efficacy for tissue generation and vascular stabilization. SVFs have cardiomyogenic potential, and many researchers have examined the possibility of SVF transplantation for heart disease. In cell-based therapies, donor age affects the regenerative capability, cell yield, and differentiation potential of adult tissues; however, opposing or controversial results have been found in humans. We examined whether SVF transplantation into impaired heart tissue shows differential effects according to donor age.
Methods
We investigated differences in protein expression in human umbilical vein endothelial cells (HUVECs) co-cultured with adipose-derived adherent stromal cells (ADASs) from donors of different ages [>40-year-olds (40s group) and >60-year-olds (60s group)] under oxidative stress conditions.
Results
Although co-culturing HUVECs with ADASs ameliorated inflammation due to increased oxidative stress conditions, few differences were observed between the ADASs from the 40s and 60s groups. Moreover, the Database for Annotation, Visualization, and Integrated Discovery classification tool revealed differentially expressed genes in the Kyoto Encyclopedia of Genes and Genomes pathway associated with cytokine–cytokine receptor interaction in response to ADASs.
Conclusion
Protein expression profiles were unchanged in HUVECs induced by isolated ADASs from donors of different ages under oxidative stress conditions.
Keywords
Introduction
Adipose tissue is a rich source of cells with prospects for tissue engineering and regenerative medicine.1,2 Adipose-derived stromal vascular fractions (SVFs) contain adipose-derived stem cells (ASCs), endothelial (progenitor) cells, vascular smooth muscle cells, mesenchymal stem cells (MSCs), fibroblasts, macrophages, and pericytes, all of which exhibit mesodermal and ectodermal capacity.3,4 This heterogeneous complex population has shown efficacy in tissue generation and vascular stabilization3,4 as well as substantial potential for therapeutic applications in lipotransfer, management of diabetes-related complications, nerve regeneration, burn wound therapy, and other uses.1,2 In particular, SVFs also have cardiomyogenic potential, 5 and many research groups are studying the possibility of SVF transplantation as a therapy for heart disease.3,6–8 ASCs improve cardiac function and perfusion after acute and chronic myocardial infarction in the rodent and pig,3,6,7 and their transplantation has been suggested as a useful therapeutic option for angiogenesis in chronic ischemic heart disease. 8 Despite these attractive advantages of SVFs in clinical interventions, their use in many diseases has not been fully evaluated in clinical studies. 9
Donor age is known to affect the regenerative capability of adult tissues in cell-based therapies; donor age also affects the number of adipose-derived MSCs, cell yield of the SVF, and differentiation potential and angiogenic functional capacity of adipose tissue.10–12 However, controversial results have been shown in humans.13–16 Researchers have found that adipose-derived MSCs exhibit similar osteogenic paracrine activity in all age groups of donors. 13 No correlation has been shown between the cell yield of ASCs from liposuction aspirates and donor age, 14 and the age of the donor does not affect the proliferation and differentiation capacities of cultured ASCs. 15 In addition, one study showed that the effect of autologous SVF transplantation for rheumatoid arthritis was unrelated to donor age. 16
Therefore, to clarify the above discrepancies in previous research, we performed the present study to determine whether SVF transplantation into impaired heart tissue shows differential effects according to donor age. We investigated the differences in protein expression in human umbilical vein endothelial cells (HUVECs) co-cultured with adipose-derived adherent stromal cells (ADASs) from individuals of different ages under oxidative stress conditions due to an abundant number of endothelial cells in the heart. 17 This study was based on the concept that redox signaling influences many physiological processes in the heart and plays a critical role in pathological cardiac remodeling. 18
Materials and methods
Donors and adipose tissue harvesting
Human adipose tissue samples for isolation of SVFs were obtained from donors recruited at International St. Mary’s Hospital of Catholic Kwandong University. All patients provided verbal informed consent to participate. The study protocol was approved by the ethics review committee of the Institutional Review Board, College of Medicine, Catholic Kwandong University. Liposuction was performed from the abdominal wall by gentle manual techniques under general anesthesia and sterile conditions. In all cases, the fat was harvested from the abdominal wall by gentle manual techniques.
Isolation of SVFs and culture of ADASs
SVFs were isolated from human adipose tissue samples by an enzymatic digestion method using the SmartX kit (DongKoo Bio & Pharma Co., Seoul, South Korea) following the manufacturer’s instructions. Briefly, adipose tissue was centrifuged at 1,700 × g for 5 min to remove water, tumescent solution, and oil. Next, 50 ml of fat tissue was digested with 0.075% collagenase type I at 37°C for 30 min under gentle agitation. After the digested tissue was filtered through a 75-μm strainer to remove residual tissue, the cell suspension was centrifuged and washed three times with phosphate-buffered saline (PBS) (HyClone, Logan, UT, USA). Total and live cell counts were performed using the NucleoCounter® NC-200™ automated cell counter (ChemoMetec, Allerød, Denmark). The SVFs were cultured in 10% fetal bovine serum (HyClone)–supplemented Dulbecco’s Modified Eagle’s Media (HyClone) and 1% penicillin/streptomycin at a density of 5 × 104 cells/cm2 in a 100-mm dish in a humidified atmosphere with 5% CO2 at 37°C. After plating on culture dishes, non-adherent cells were discarded by changing the culture medium and ADASs passaged three times.
HUVEC culture
HUVECs (Lonza, Walkersville, MD, USA) were cultured in Clonetics Endothelial Growth Basal Medium 2 (Lonza) supplemented with Clonetics Endothelial Growth Medium 2 SingleQuots (Lonza) using dishes and plates coated with 0.1% gelatin (BD, Sparks, MD, USA) in a humidified atmosphere of 5% CO2 and 95% air at 37°C.
Cell viability assay
Cell viability was measured using Ez-Cytox (Daeillab Service, Seoul, Korea). HUVECs were seeded 24 h prior to H2O2 treatment at a density of 5 × 104 cells/cm2 onto a 96-well plate. After 24 h, H2O2 (0, 10, 20, 30, 40, or 50 μM) was applied to the HUVECs for 2, 4, or 6 h. After the addition of 10 μL of Ez-Cytox into each well, cell viability was evaluated by measuring the optical density at 450 nm.
Reactive oxygen species detection assay
Reactive oxygen species (ROS) production in H2O2-treated HUVECs was assessed according to the levels of bright green-colored 2′,7′-dichlorofluorescein (DCF) produced by the oxidation of DCF diacetate (DCF-DA) dye. The HUVECs were plated 24 h prior to H2O2 treatment at a density of 5 × 104 cells/cm2 in a 6-well plate and washed twice with PBS after 24 h. ROS generation was induced in HUVECs after 2, 4, or 6 h of treatment with 0 to 50 μM H2O2, followed by incubation with 50 μM DCF-DA (Sigma-Aldrich, St. Louis, MO, USA) for 30 min in the dark at 37°C. The green fluorescence was detected by flow cytometry using a BD Accuri™ C6 Cytometer (BD Biosciences, Piscataway, NJ, USA).
Co-culture of ADASs and HUVECs
HUVECs at passage 5 were plated 24 h prior to H2O2 treatment at a density of 5 × 104 cells/cm2 in a 6-well plate and then treated with or without 40 μM H2O2 for 4 h. After 4 h, the cells were co-cultured with individual ADASs at passage 3 using trans-well inserts with a 0.4-μm porous translucent polyethylene terephthalate membrane (Falcon; Corning Life Sciences, Pittston, PA, USA) at a cell density identical to that of the HUVECs. Following co-culture for 24 or 48 h after the incubation period, the cells in the lower well were then harvested for further analysis. The experimental groups were designed as follows: Group 1 (negative control), HUVECs (monoculture); Group 2 (H2O2), HUVECs (monoculture) + H2O2; Groups 3, 4, and 5 (40s group), HUVECs and ADASs (40s group #1, #2 or #3, co-culture) + H2O2; and Groups 6, 7, and 8 (60s group), HUVECs and ADASs (60s group #1, #2, or #3, co-culture) + H2O2.
Flow cytometry
For the flow cytometric analysis, cells were collected using Accutase Cell Detachment Solution (Thermo Fisher Scientific, Waltham, MA, USA). The cells (5 × 105 cells/50 μL) were incubated for 1 h with antibodies to CD31, CD34, CD45, CD90, CD105, CD106, or isotype control (Santa Cruz Biotechnology, Santa Cruz, CA, USA) on ice and then washed three times with PBS containing 2.5% fetal bovine serum and 0.1% sodium azide (Sigma-Aldrich; washing solution). The cells were further incubated for 1 h with fluorescein isothiocyanate-conjugated anti-mouse IgG or anti-rabbit IgG (Santa Cruz Biotechnology) on ice in the dark. The cells were then washed three times and analyzed via flow cytometry using a BD Accuri™ C6 Cytometer (BD Biosciences).
Immunoblot analysis
The immunoblot analysis was performed according to the normalized methods of our previous studies. 19 Primary polyclonal antibody (Santa Cruz Biotechnology) and secondary antibodies (horseradish peroxidase-conjugated anti-goat IgG, anti-mouse IgG or anti-rabbit IgG; Santa Cruz Biotechnology) were used for detection of proteins of interest. The results were visualized using an enhanced chemiluminescence (ECL, Western Blotting Detection kit, GE Healthcare, Sweden) system, and the band intensities were quantified using ImageJ software.
RNA isolation, reverse-transcription polymerase chain reaction (PCR), and quantitative real-time PCR (qPCR)
Total RNA was isolated from HUVECs using TRIzol Reagent Solution (Life Technologies, Frederick, MD, USA) according to the manufacturer’s instructions. Oligo dT-primed cDNA was synthesized from total RNA using the Maxime RT PreMix kit (iNtRON Biotechnology, Seongnam, Korea). The level of each gene transcript was quantitatively determined by qPCR using a StepOnePlus real-time PCR system (Applied Biosystems, Foster City, CA, USA) with the SYBR Green Dye system [SYBR Premix Ex Taq (Tli RNase H Plus) and ROX reference dye (Takara Bio Inc., Foster City, CA, USA)]. The transcript level of each gene was normalized to the GAPDH transcript levels. Primers were designed using Primer3 and BLAST, and the primer set sequences are listed in Table 1.
Donor characteristics

Network analysis
For the gene/protein network analyses, targets identified in this study were analyzed using GeneMANIA (http://www.genemania.org) and the Database for Annotation, Visualization, and Integrated Discovery (DAVID).20,21 DAVID provides a comprehensive set of functional annotation tools to interpret the biological relevance of such a large list of genes/proteins, whereas the GeneMANIA interface generates a list of genes with functional similarity based on the available genomics and proteomics information in the database. The GeneMANIA algorithm contains two integral parts: 1) a linear regression-based algorithm for calculating a single, composite functional association network from multiple networks derived from different proteomic or genomic data sources and 2) the prediction of gene function.
Statistical analysis
All data were compared via one-way analysis of variance using the Statistical Package for the Social Sciences (SPSS, version 14.0K; SPSS Inc., Chicago, IL, USA). Data are expressed as mean ± standard error of the mean. Group means were considered significantly different at p<0.05, as determined by the protected least significant difference test when analysis of variance indicated an overall significant treatment effect (p<0.05).
Results
Characterization of human ADASs by passage
Sequences of primers used for quantitative real-time polymerase chain reaction
F, sequence of sense strands; R, sequence of anti-sense strands; IL6, interleukin-6; IL8, interleukin-8; IFNG, interferon gamma; TNF, tumor necrosis factor; FGF1, fibroblast growth factor-1; FGF2, fibroblast growth factor-2; VEGFA, vascular endothelial growth factor A; VEGFB, vascular endothelial growth factor B; PDGFA, platelet-derived growth factor subunit A; PDGFB, platelet-derived growth factor subunit B; ANG, angiopoietin
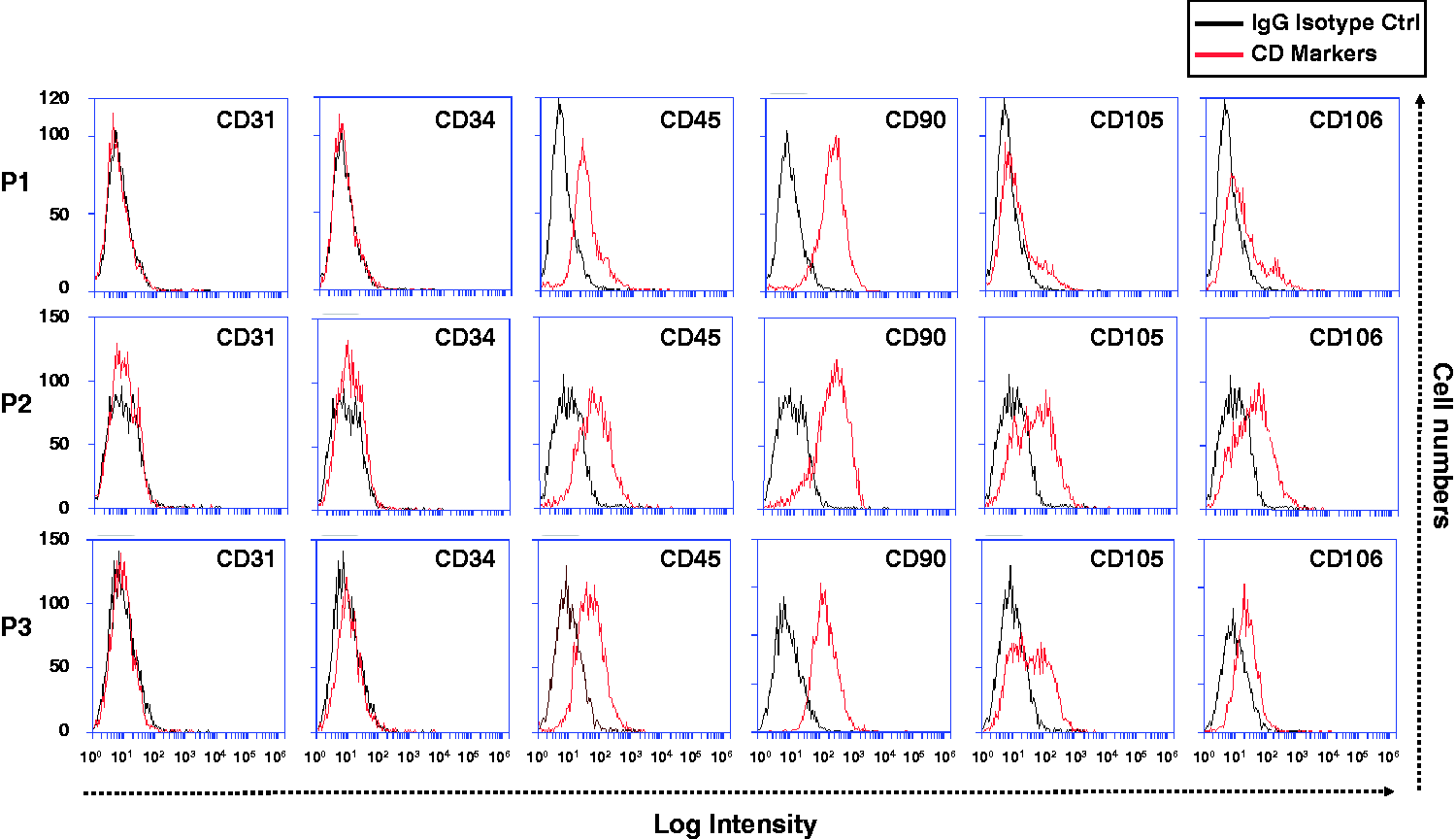
Surface marker expression on ADASs according to passage number as determined by flow cytometry. This figure shows the ADAS characterization results. The donor characteristics are summarized in Table 1. ADASs, adipose-derived adherent stromal cells; P, passage.
Determination of the concentration and treatment time of H2O2 in HUVECs
Analysis of the treatment duration and titration of H2O2 in HUVECs is necessary to evaluate the differential responses of HUVECs to isolated ADASs from donors of different ages under oxidative stress conditions. Accordingly, cell viability and ROS generation of HUVECs were measured using Ez-Cytox and DCF-DA with different concentrations of H2O2 (0–50 μM) and treatment times (0, 2, 4, or 6 h). Figure 2(a) shows the percentage of viable cells, and Figure 2(b) presents the number of ROS-generating HUVECs under oxidative stress conditions. HUVECs were most strongly affected by ROS generation when treated with 40 μM H2O2 for 4 h (Figure 2(b)), although the cell viability was 87% at this concentration and treatment time (Figure 2(a)). Therefore, HUVECs were treated with 40 μM of H2O2 for 4 h in further studies.
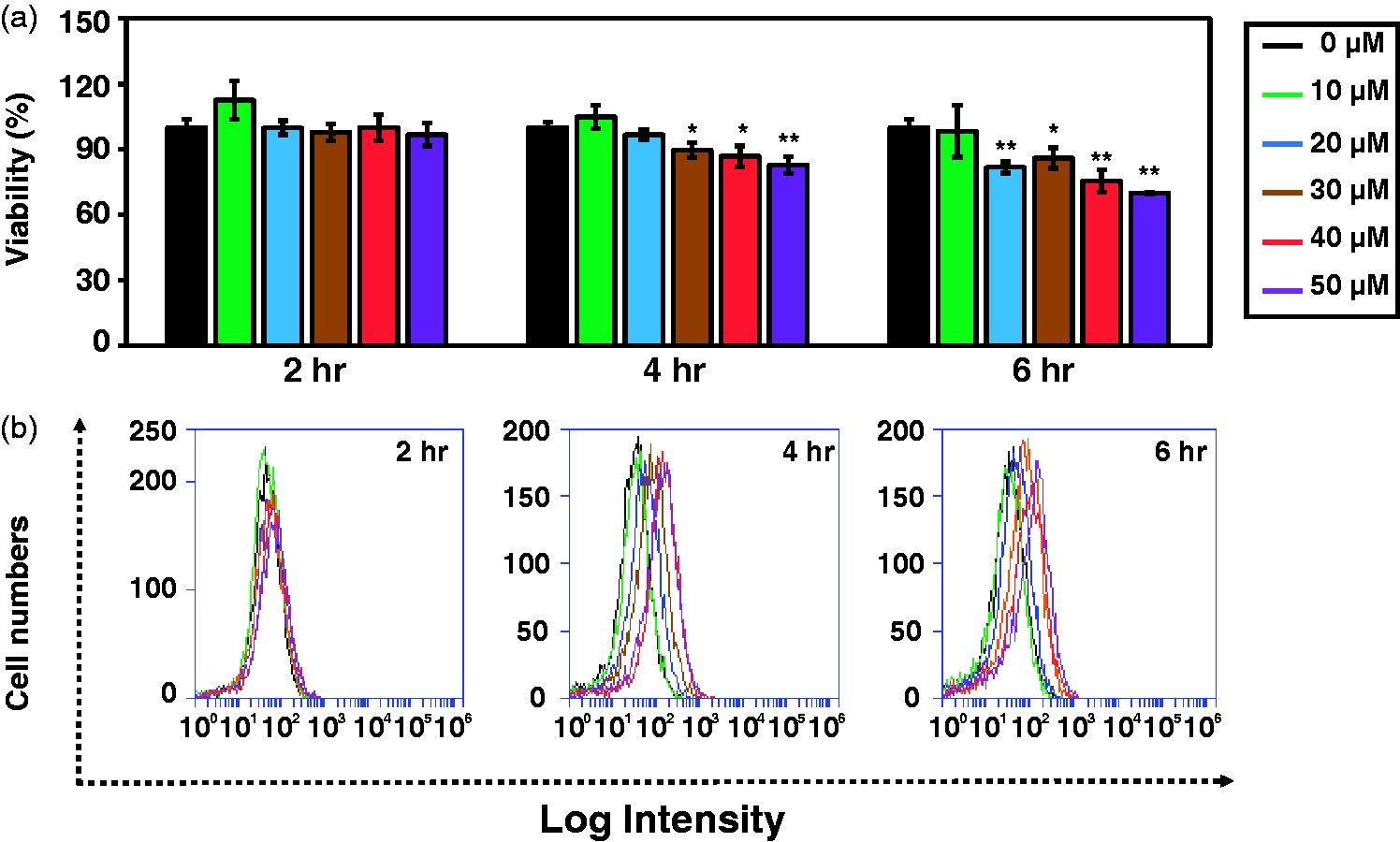
Cell viability and reactive oxygen species generation of human umbilical vein endothelial cells for various concentrations and times of H2O2 treatment. (a) Cell viability and (b) Reactive oxygen species generation were measured using Ez-Cytox and 2′,7′-dichlorofluorescein diacetate, respectively. Data are representative of three independent experiments. Significant differences between the untreated (0 μM) and H2O2-treated (10, 20, 30, 40, or 50 μM) groups were determined via analysis of variance. *p<0.05, **p<0.01.
Differential regulation of proteins related to anti-oxidant activity, apoptosis, inflammation, adhesion, and calcium regulation in HUVECs by ADASs
HUVECs pretreated with H2O2 were cultivated with ADASs isolated from human adipose tissue from both donor age groups (40s and 60s groups) for 48 h. The expression levels of proteins related to anti-oxidant activity, apoptosis, inflammation, adhesion, and calcium regulation in HUVECs were compared between the 40s and 60s groups using western blot analysis. The expression of anti-oxidant proteins [peroxiredoxin (PRX) and thioredoxin (TRX)] in HUVECs was down-regulated by H2O2 but showed an upward trend in HUVECs co-cultured with ADASs (40s and 60s groups) (Figure 3). In contrast, the expression of HUVEC protein associated with apoptosis (p53) was increased by H2O2 but decreased in HUVECs co-cultured with ADASs despite variations among individuals (Figure 3). Moreover, proteins that are important for inflammation (phosphorylated p38), adhesion (intercellular adhesion molecule-1), and calcium regulation (Ca2+/calmodulin-dependent protein kinase II and calreticulin) exhibited a tendency to increase in H2O2-treated HUVECs and were more highly expressed in HUVECs co-cultured with ADASs than in H2O2-treated HUVECs (Figure 3). However, p38 was largely unchanged in all groups (Figure 3). Interestingly, little differences were observed in protein expression related to anti-oxidant activity, apoptosis, inflammation, adhesion, and calcium regulation between the 40s and 60s donors (Figure 3).

Differential regulation of proteins related to anti-oxidant activity, apoptosis, inflammation, adhesion, and calcium regulation in human umbilical vein endothelial cells in response to adipose-derived adherent stromal cells and H2O2 treatment. (a) Differential regulation as determined via an immunoblot analysis. (b) Band intensity was measured as area density and analyzed by the ImageJ program. Relative intensity levels indicate protein levels normalized to β-actin levels. Data are representative of three independent experiments. Significant differences between the H2O2 treatment conditions in the negative control group and 40s and 60s groups were determined via analysis of variance. *p<0.05, **p<0.01.
Gene expression related to inflammation and angiogenesis in HUVECs co-cultured with ADASs
H2O2-treated HUVECs were co-cultured with ADASs for 24 h, and the gene expression levels of pro-inflammatory cytokines [interleukin-6 (IL6), IL8, interferon gamma (IFNG), and tumor necrosis factor (TNF)] and angiogenic factors [fibroblast growth factor-1 (FGF1), FGF2, vascular endothelial growth factor A (VEGFA), platelet-derived growth factor subunit A (PDGFA), PDGFB, and angiopoietin (ANG)] were determined by qPCR. Consequently, IL8, IFNG, and TNF, but not IL6, were remarkably increased in H2O2-treated HUVECs but significantly decreased in HUVECs co-cultured with ADASs (Figure 4(a)). In addition, the expression of all monitored angiogenesis-related genes (ANG, FGF1, FGF2, PDGFA, PDGFB, and VEGFA) was dramatically increased by ADASs (Figure 4(b)). Little differences were observed between the 40s and 60s donors (Figure 4).

Gene expression related to (a) inflammation and (b) angiogenesis in human umbilical vein endothelial cells co-cultured with adipose-derived adherent stromal cells was determined via quantitative real-time polymerase chain reaction. Data are representative of three independent experiments. The transcript level of each gene was normalized to the GAPDH transcript levels. Significant differences between the H2O2 treatment conditions in the negative control group and 40s and 60s groups were determined by analysis of variance. *p<0.05, **p<0.01.
Functional classification of differentially expressed proteins/genes by various bioinformatics resources
To determine the gene interactions for proteins/genes that were differentially altered in H2O2-treated HUVECs, 15 proteins/genes associated with anti-oxidation, apoptosis, inflammation, angiogenic factors, or calcium regulation were analyzed using GeneMANIA to determine the interactions of these proteins/genes [Figure 5(a)]. The 14 query genes (inside circle) and their interacting genes are presented in Figure 5(a). Function-based interactions with identified partners were predicted with genes associated with positive regulation of cell motility, cell migration, and the cellular components required for movement. Furthermore, identification of enriched functional gene groups using DAVID showed that the most strongly affected functional genes in ADASs were found in the Kyoto Encyclopedia of Genes and Genomes pathway [Table 3 and Figure 5(b)]. Six of these genes (CXCL8, IFNG, PDGFA, PDGFB, TNF, and VEGFA) were localized to cytokine–cytokine receptor interaction and may play important roles in the development of new therapeutic strategies for various diseases using SVF transplantation.
Functional classification by various bioinformatics tools. (a) Networks from the GeneMANIA analysis showing the results of 15 queries (located inside the circle) and the function-based relationships. (b) Enriching the top term hit using DAVID identified cytokine–cytokine receptor interaction from the Kyoto Encyclopedia of Genes and Genomes pathway. Differentially expressed targets are marked with a red star on the figure. Target functional gene groups as identified by Functional Annotation Clustering Benjamini, Benjamini–Hochberg critical value; FDR, false discovery rate; KEGG, Kyoto Encyclopedia of Genes and Genomes; MAPK, mitogen-activated protein kinase; HTLV-1, human T-lymphotropic virus 1; PI3K, phosphoinositide 3-kinase; Akt, protein kinase B; NF-kappa B, nuclear factor kappa B

Discussion
Adipose-derived SVFs contain pluripotent stem cells that can differentiate into osteogenic, adipogenic, myogenic, neurogenic, chondrogenic, and hematopoietic lineages.22,23 Specifically, these cells spontaneously show a cardiomyocyte phenotype, which suggests that this phenotype may be required for differentiation in response to specific conditions. 5 Additionally, many reports have been published regarding the possibility of transplantation of adipose-derived SVFs as a therapy for heart disease.3,6–8 Donor age is a critical factor in the regenerative capability of the cells in this cell-based therapy,10–12 but controversial results have been observed in humans.13–16 Our aim was to determine the effects of donor age on adipose-derived SVF transplantation into impaired heart tissue. Thus, we examined the effects of ADASs on HUVECs because endothelial cells are abundant in the heart, 17 and oxidative stress conditions were used as an environmental stimulus because of their critical role in many physiological processes in the heart. 18 Therefore, we explored the differential expression of proteins in endothelial cells co-cultured with adipose-derived ADASs from donors of different ages (40s and 60s groups) under oxidative stress conditions (H2O2). Interestingly, although co-culturing HUVECs with ADASs ameliorated inflammation caused by an increase in oxidative stress conditions, few differences were observed between the ADASs from the 40s and 60s groups.
SVF cells are composed of heterogeneous cell populations including blood-derived cells (CD45+), ASCs (CD31−, CD34+, CD45−, CD90+, CD105−, and CD106+), MSCs (CD31−, CD34−, CD45−, CD90+, CD105+, and CD106+), endothelial (progenitor) cells (CD31+, CD34+, CD45−, CD90+, CD105−, and CD106+), vascular smooth muscle cells (CD31−, CD34+, CD45−, CD90+, CD105−, and CD106-), pericytes (CD31−, CD34−, CD45−, CD90+, CD105−, and CD106+), and other cells.4,23,24 Differences exist in the phenotype and kinetics of differentiation between freshly isolated SVFs and cultured ADASs.24,25 However, by passage 3, the differences in surface marker expression of cultured ADASs were negligible (Figure 1). In addition, the ADASs used in our study expressed CD45, CD90, CD105, and CD106 but neither CD31 nor CD34 (Figure 1). After plastic adherent culture, CD45 in ADASs is usually almost absent. 26 Interestingly, the expanded ADASs used in the present study expressed CD45 by passage 3 (Figure 1). The most likely reasons for this are the method used for isolation of SVFs, 27 the short period of time for adherent culture, and the increased numbers of adherent leukocytes in patients with arthritis 28 (Table 1). These factors may make CD45 expression possible in cultured and expanded ADASs. In this study, we used cultured ADASs from passage 3 to ensure that sufficient numbers of ADASs were available for co-culturing with HUVECs.
Prior to the beginning of this study, we anticipated that anti-oxidant proteins would be down-regulated and that proteins related to apoptosis, inflammation, adhesion, and calcium regulation would be up-regulated in H2O2-treated HUVECs. We also predicted that these proteins would show opposite expression patterns when exposed to ADASs compared with H2O2 treatment. Consistent with our expectations, the expression levels of most proteins were altered in HUVECs treated with H2O2 (Figure 3 and Figure 4). However, contrary to our expectations, proteins other than anti-oxidant proteins and apoptosis-related proteins were up-regulated to a greater extent in cells exposed to ADASs than in the H2O2-treated HUVECs (Figure 3).
Oxidative stress is characterized by elevated intracellular ROS that damage lipids, proteins, and DNA, and numerous metabolic, structural, and functional effects due to oxidative stress have been observed in many experimental and clinical investigations. 29 The defense mechanisms against oxidative stress include (enzymatic) anti-oxidant defenses such as superoxide dismutases, glutathione peroxidases, catalases, PRX, and TRX. 26 Moreover, oxidative stress induces p53 activation and apoptotic induction. 29 Consistent with previous reports,26,29 anti-oxidant proteins (PRX and TRX) were down-regulated in HUVECs by H2O2 and enhanced by treatment of ADASs, although individual variations were observed. However, p53 was increased by H2O2 and decreased by ADASs (Figure 3). These results imply that proteins and/or extracellular vesicles secreted in response to ADASs may induce enzymatic anti-oxidant defenses and/or anti-apoptotic signals in endothelial cells.
We assumed that proteins showing reverse trends in expression in response to ADASs were affected by pro-inflammatory cytokines through paracrine and/or autocrine reactions 8 ; however, some genes were decreased by co-culturing HUVECs with ADASs (Figure 4(a)). Angiogenesis is a therapeutic target for the treatment of cardiovascular disease, 8 and some proteins show opposite expression patterns during angiogenesis. 30 We also observed that angiogenic factors were remarkably increased by co-culturing HUVECs with ADASs (Figure 4(a)). These results suggest that ADASs may induce angiogenesis and anti-inflammation in endothelial cells and contribute to restoration in patients with cardiac failure. Despite the controversial results regarding donor age with respect to SVF transplantation,11–17 we showed very little difference in the expression of proteins between donors in the 40s and 60s groups under oxidative stress conditions (Figure 3 and Figure 4). In the functional analysis by GeneMANIA, enriched functional-related gene groups were predicted with 14 genes associated with positive regulation of cell motility, cell migration, and cell component movement in functional features. Furthermore, the most strongly affected functional genes (CXCL8, IFNG, PDGFA, PDGFB, TNF, and VEGFA) were those associated with cytokine–cytokine receptor interaction based on the DAVID enrichment analysis and may play important roles in the development of new therapeutic strategies for various diseases.
This study has shown that the profiles of proteins expressed in HUVECs in response to isolated ADASs exhibit few differences according to donor age under oxidative stress conditions. We expect that these results will provide the basis for the clinical application of SVF transplantation into impaired heart tissue. However, further studies using more donors with diverse ages, various environmental conditions, and varied target proteins are required for a better understanding of the influences of age on human ADASs.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was supported by the Korea Ministry of Science, ICT and Future Planning (NRF-2015M3A9E6029519).
