Abstract
Objective
This study was performed to analyse factors influencing the effect-site concentration (Ce) of propofol at return of consciousness (ROC) with target-controlled infusion of propofol–remifentanil after laparoscopic surgery.
Methods
In total, 112 patients who underwent laparoscopic surgery under general anaesthesia were given propofol at the target concentration of 3.5 µg/ml. Remifentanil (Ce: 4.0 ng/ml) and 0.9 mg/kg of rocuronium were administered when the Observer’s Assessment of Alertness/Sedation score reached 1. Two minutes after injection of rocuronium, tracheal intubation was initiated. The bispectral index (BIS) was maintained between 45 and 55.
Results
Ce values of propofol at loss of consciousness (LOC) and ROC were significantly correlated. Age was significantly correlated with Ce of propofol at ROC. At LOC, propofol Ce values of patients aged 65–80, 45–64, and 20–44 years were 1.8 ± 0.8, 2.2 ± 0.7, and 2.3 ± 0.8 µg/ml, respectively, and the BIS was 70 ± 10, 68 ± 7, and 69 ± 10, respectively. At ROC, the propofol Ce values of the three groups were 1.2 ± 0.3, 1.4 ± 0.3, and 1.5 ± 0.3 µg/ml, respectively, and the BIS was 80 ± 5, 82 ± 6, and 83 ± 6, respectively.
Conclusions
The concentration of propofol at ROC was significantly affected by age, and ROC of propofol–remifentanil anaesthesia after laparoscopic surgery was well predicted by the concentration at LOC.
Keywords
Introduction
Anaesthesiologists have endeavoured to perform safe and rapid anaesthesia during induction and to realize precise and comfortable return of consciousness (ROC) after surgery. 1 The propofol dose for adequate ROC can be obtained by predicting its effect-site concentration (Ce), which can also reduce the workload of anaesthesiologists, save resources and time, and render recovery safer. 2 The propofol Ce values at ROC from anaesthesia have a wide range (0.8–2.7 µg/mL)3,4; therefore, it is rather difficult to predict the minimum concentration for effective sedation. Laparoscopic surgery, which is minimally invasive, has been widely used in clinical practice. The propofol Ce at ROC after laparoscopic surgery or during total intravenous anaesthesia remains unknown. Therefore, the present prospective clinical study was performed to analyse the factors influencing the propofol Ce at ROC with target-controlled infusion (TCI) of propofol–remifentanil after laparoscopic surgery.
Materials and methods
Selection of patients and study preparation
The present study included 112 patients with an American Society of Anesthesiologists physical status of 1 to 3 and age of 20 to 80 years who underwent laparoscopic colon surgery or nephrectomy under general anaesthesia. The study was approved by the ethics committee of our hospital, and written consent was obtained from all patients.
The exclusion criteria were a body mass index of ≤ 18 or ≥ 30 kg/m2, hearing loss or other neurological deficits, history of mental disorders and renal or hepatic disease, recent administration of opioids or sedatives, drug addiction, and intraoperative blood loss of > 800 ml.
Before surgery, the patients were fasted for 8 h and given no premedication. Routine monitoring was applied after they entered the operating room. The arterial blood pressure was continuously monitored by inserting a 20-gauge plastic cannula into the radial artery, and drugs and fluid were intravenously administered by inserting an 18-gauge catheter into an upper limb vein. After 10 min of stabilization, the baseline blood pressure and heart rate were detected. The forehead skin was then sterilized with 75% ethanol, and the bispectral index (BIS) was recorded with an A-2000 BIS Monitor (XP Version; Aspect Medical Systems, Natick, MA, USA). Prior to drug administration, 5 ml/kg of lactated Ringer’s solution was intravenously administered at an infusion rate of 7 ml/kg per min.
Propofol was given through TCI by a motor-driven syringe pump (Graseby 3500; Smiths Medical International, Watford, UK) with a TCI system (Diprifusor; AstraZeneca, Cambridge, UK) containing the modified Marsh’s pharmacokinetic model. This system can predict the Ce of propofol.5,6 The model for remifentanil was proposed by Minto et al.7,8
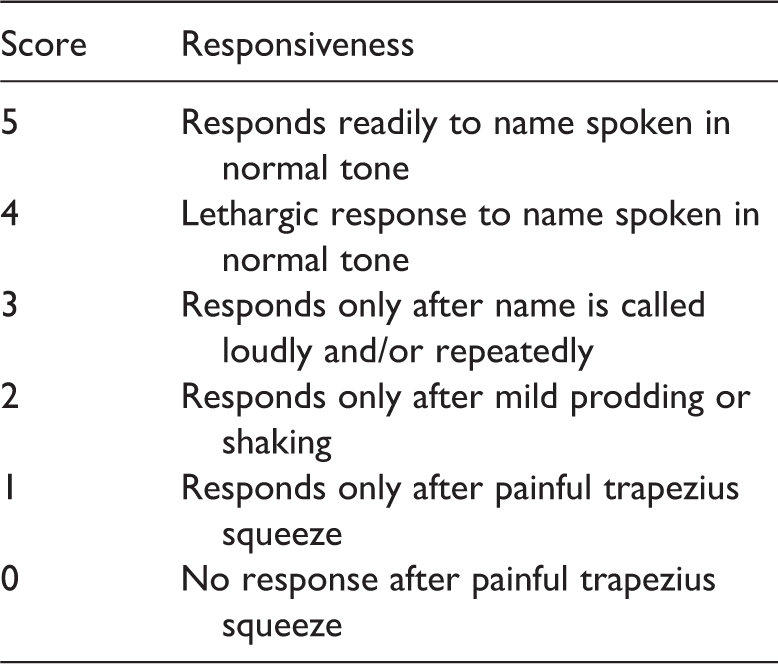
Responsiveness scores of the modified Observer’s Assessment of Alertness/Sedation scale.
Detection of variables
The Ce, mean arterial pressure, and heart rate were recorded at eight time points: at baseline before induction (T0), at achievement of an OAA/S score of 1 [loss of consciousness (LOC)], immediately before intubation (T2), immediately after intubation (T3), 3 min after intubation (T4), 2 min after establishment of pneumoperitoneum (T5), before termination of infusion (T6), and at ROC. The BIS was recorded 5 s after each time point. All variables were detected by the same anaesthesiologist to minimize bias.
Statistical analysis
All data were analysed using SPSS version 11.5 (SPSS Inc., Chicago, IL, USA). The normality of all continuous data was tested with the Kolmogorov–Smirnov method. The correlations between clinical variables and ROC were evaluated using linear correlation analysis. Comparisons among three groups were conducted with one-way analysis of variance. Multiple comparisons of inter-individual data were carried out by Friedman’s repeated-measures analysis of variance on ranks with Tukey’s all pairwise comparison method. A P value of < 0.05 was considered statistically significant.
Results
Propofol Ce, remifentanil Ce, BIS, MAP, and HR at eight time points.

T0: Baseline values before induction; LOC: OAA/S score of 1; T2: immediately before intubation; T3: immediately after intubation; T4: 3 min after intubation; T5: 2 min after pneumoperitoneum; T6: before termination of infusion; ROC: return of consciousness; MAP: mean arterial pressure; HR: heart rate.
Data and correlation coefficients between clinical variables and propofol Ce at ROC.

BMI: body mass index; LOC: loss of consciousness; ROC: return of consciousness; Ce: effect-site concentration; *P < 0.01. Pearson’s correlation analysis was used.
Relationship between propofol Ce at ROC and LOC
Linear regression analysis revealed a significant correlation between the propofol Ce at ROC and LOC. The regression equation was: Ceroc = 0.29Celoc + 0.82 (µg/ml) (r = 0.647, P < 0.01) (Figure 1).
Linear regression analysis for propofol Ce at ROC and propofol Ce at LOC. Statistically significant correlation: r = 0.647, P < 0.01; positive slope: P < 0.01.
Relationship between propofol Ce at ROC and age
Linear regression analysis suggested that the propofol Ce at ROC was significantly correlated with age. The regression equation was: Ceroc = −0.013age + 2.101 (µg/ml) (r =−0.622, P < 0.01) (Figure 2).
Linear regression analysis between Ce of propofol at ROC and patients’ age. Statistically significant correlation: r = –0.622, P < 0.01; non-positive slope: P < 0.01.
The propofol Ce at LOC was negatively correlated with age. The equation was: Ceroc = −0.029age + 3.431 (µg/ml) (r =−0.601, P < 0.01) (Figure 3).
Linear regression analysis between Ce of propofol at LOC and patients’ age. Statistically significant correlation (r = –0.601, P < 0.01).
Allocation of patients
Patient characteristics in the three groups.

LN: laparoscopic nephrectomy; LCS: laparoscopic colon surgery; *P < 0.010
Clinical responsiveness, BIS, propofol Ce, and variables
The BIS values of the three groups at LOC were similar. The propofol Ce of Group L was significantly lower than that of Groups Z and Q (P = 0.032 and 0.024, respectively), but the latter two groups had similar Ce values (P = 0.082). Group L took significantly less time to lose consciousness than did Groups Z and Q (P < 0.05).
Propofol Ce and BIS values at LOC/ROC.

T1: time taken to lose consciousness; Celoc: Ce of propofol at LOC; T2: time for recovery; Ceroc: Ce of propofol at ROC; Cestop: Ce of propofol upon stopping infusion; TD: total dose. *P < 0.05, **P < 0.01.
The BIS values at LOC and ROC were positively correlated, but the correlation coefficient was not high (correlation equation: BISROC = 0.146BISLOC + 70.896) (r =0.266, P < 0.05).
Discussion
In this study, we analysed the factors that affected the propofol Ce at ROC with TCI of propofol–remifentanil after laparoscopic surgery. Iwakiri et al. 10 reported that the propofol Ce at ROC was significantly correlated with the Ce at LOC, but they did not describe a related analysis or equation. In the present study, we found that the propofol Ce at ROC was negatively correlated with age and positively correlated with the Ce at LOC.
The propofol Ce values of Groups L, Z, and Q were 1.8 ± 0.8, 2.2 ± 0.7, and 2.3 ± 0.8 µg/ml, respectively. The oldest group had a significantly lower propofol Ce. Similarly Servin 11 reported that 1.69 ±0.50 µg/ml of propofol was required for their TCI group at LOC. Ouattara et al. 12 recommended decreasing the propofol concentration and dosage for elderly patients and using the same dose of remifentanil. Based on this recommendation, remifentanil at a Ce of 4 ng/ml was used during anaesthetic induction and maintenance in the present study. As indicated by the hemodynamic indices during induction, maintenance, and recovery, the analgesic effects indeed met the requirements of laparoscopic surgery.
In addition, the propofol Ce values at ROC in Groups L, Z, and Q were 1.2 ± 0.3, 1.4 ± 0.3, and 1.5 ± 0.3 µg/ml, respectively, and their recovery times were 819 ± 286, 712 ± 228, and 648 ± 232 s, respectively. In other words, older patients had a significantly lower propofol Ce at ROC, and their recovery time was markedly prolonged, with the longest being > 16 min. Similarly, Vuyk et al. 13 found that younger patients recovered more easily from anaesthesia than did older patients and that sudden awakening had the potential to cause body movement or even injury. Older patients often recover more slowly than do younger patients. Thus, older patients, especially sensitive ones, should be closely monitored during postoperative recovery to avoid low ventilation, respiratory depression, and other sleep-induced complications. Based on the results in the present study, if the recovery time and concentration can be predicted according to the concentration of propofol given to patients when they lose consciousness and stop using drugs, the depth of anaesthesia can be adjusted on an individual-patient basis, thereby allowing timely recovery and precise anaesthesia.
Nevertheless, the BIS values of older and young patients at LOC or ROC were not significantly different, indicating that older patients were more sensitive to propofol and that the BIS was more closely correlated with other clinical indices. The BIS did not reflect the susceptibility of patients to drugs, as reported previously. 14
This study had several limitations. The main limitation is that the concentration of propofol when the infusion was stopped was read from the infusion pump and in most cases was 2.0, 2.5, 3.0, or 3.5 µg/ml. Therefore, the data were non-normally distributed. This could be circumvented by drawing venous blood at different time points to detect the plasma concentration. Moreover, a wider variety of surgery types should be evaluated in future studies, which will show differences in surgical times, intraoperative blood loss, and body temperature.
ROC from propofol–remifentanil anaesthesia after laparoscopic surgery was well predicted by the propofol concentration at LOC. The patient’s age and propofol concentration were significantly correlated with the time point at which ROC occurred. Older patients had a lower propofol concentration during recovery than did young patients.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
