Abstract
Objective
In Japan, stroke care is provided through medical cooperation and standardized treatment. However, various factors affect mortality in the hyperacute phase. The present study investigated factors associated with death within 24 h after admission for acute stroke.
Methods
Among 2335 patients admitted within 24 h after stroke onset from 1 January 2007 to 31 December 2012, a total of 139 deaths occurred. Forty-eight deaths occurred within 24 h after admission. We retrospectively examined the clinical features of these 48 patients.
Results
The overall mortality rate was 6.0%. When the initial 72-h period was divided into ≤24 h (Period I), >24 to 48 h (Period II), and >48 to 72 h (Period III), deaths were significantly more frequent in Period I than in the other two periods. The frequency of intracerebral haemorrhage (ICH) was also significantly higher in Period I than in the other two periods. Factors significantly associated with death from ICH were systolic blood pressure, hematoma volume, and surgery.
Conclusion
The mortality rate was low among patients with stroke transported to the authors’ medical center within 24 h of onset. Blood pressure management and the timing of determining indications for surgery are important factors in acute haemorrhagic stroke care.
Introduction
Since the Guidelines for the Management of Stroke 2003 were published, effective treatment of acute stroke in stroke care units (SCUs)/stroke units (SUs)1,2 and standardized treatments have been developed and applied in Japan. In October 2005, intravenous recombinant tissue plasminogen activator (rt-PA) was approved for coverage by the medical insurance system and became the first-line treatment for hyperacute stroke.2,3 In 2006, immediate stroke life support was developed as off-the-job training aimed at standardizing the initial treatment of patients with stroke in hospitals. 4
If this system of primary care for patients with stroke is maintained, the stroke mortality rate will presumably decrease. In five previous reports, the mortality rates in stroke care hospitals or hospitals with SCUs/SUs were 20.9%, 12.1%, 10.47%, 10.1%, and 9.2%5–9, and were significantly lower than those in general hospitals (20.9% vs. 25.4%, 12.1% vs. 16.6%, 10.1% vs. 12.5%, and 9.2% vs. 10.3%).5,6,8,9 In the present study, the mortality rate at the authors’ medical centre was compared with the mortality rates from previous reports. No previous reports seem to have described factors associated with death within 24 h after admission when incomplete patient information is available or when the status of the patient may worsen. The stroke mortality rate 24 h after admission may decrease by aggressive treatment of factors related to stroke death within 24 h after admission. This study therefore investigated factors associated with poor outcomes in patients with acute stroke who died within 24 h after admission to our medical centre, which has an SCU, and examined future treatment needs.
Patients and methods
Among 3265 patients hospitalized for stroke (excluding transient ischemic attacks) from 1 January 2007 to 31 December 2012, at total of 2335 patients were admitted within 24 h after stroke onset. Of these, 139 died during the clinical course. Seventy-five deaths occurred within 72 h after admission, including 48 deaths within 24 h after admission. Among these 48 patients, we retrospectively examined the clinical features including stroke type, sex, mean age, level of consciousness on admission (Japan Coma Scale (JCS) score), 10 neurological severity (National Institutes of Health Stroke Scale (NIHSS) score or World Federation of Neurosurgical Societies (WFNS) classification), 11 systolic blood pressure (SBP), lesion site, and cause of death (due to primary disease or not). The appropriateness of treatment was also reviewed.
In the authors’ institution, patients with acute stroke are admitted to the SCU (formerly the SU), and acute care is provided by an SCU team comprising physicians, nurses, rehabilitation specialists, and medical social workers. Physicians in the SCU include specialists in neurosurgery, neurology, and cardiovascular medicine as well as neurosurgery residents.
Japan Coma Scale (JCS).

Note: R: Restlessness, I: Inconsistence, A: Apallic state or Akinetic mutism
For instance it is represented as 30 R or 30 restlessness, or 20 I or 20 incontinence.
WFNS grading scale for SAH.

WFNS = World Federation of Neurological surgeons; SAH = subarachnoid hemorrhage; GCS = Glasgow Coma Scale.
Statistical analysis
We used an unpaired t-test, χ2 test, or Fisher’s exact test for comparisons between two independent groups (number of deaths, mean age, sex ratio, consciousness, lesion site of intracerebral haemorrhage (ICH), SBP on admission, and hematoma volume). In the investigation of factors associated with death in patients with ICH within 24 h after admission (hematoma volume, blood pressure, and surgery), we performed multiple logistic regression analysis for dependent variables of survival and death. We considered two-sided P values of <0.05 to be significant. SPSS version 21.0 (IBM, Armonk, NY) was used for all statistical analyses.
Results
Breakdown of stroke inpatients within onset 24 h of onset (survival vs death).

p < 0.05, **p < 0.01
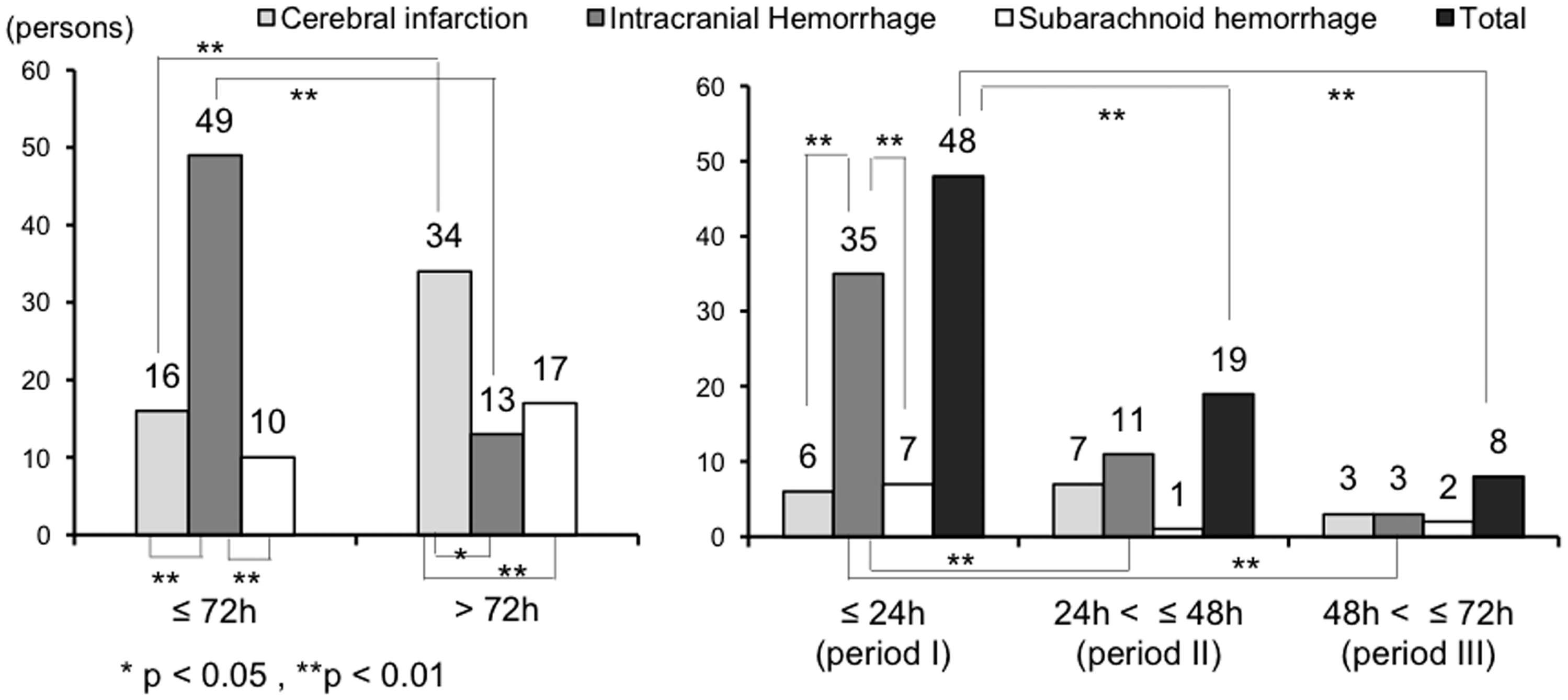
Number of stroke-related deaths.
Breakdown of sex ratio and mean age of deaths according to the stroke type.

p < 0.05, upper stage: number (male: female), lower stage: mean age
Deaths of cerebral infarction patients within 24 h after admission (n = 6).

Group: N; non-cardiogenic infarction, C; cardiogenic infarction
Past illness: HT; hypertension, CI; cerebral infarction, (p)af; (paroxysmal) atrial fibrillation, PC; prostate cancer, cKD; Chronic kidney disease, PMI; implantation
lesion: BA; basilar artery, VA; Vertebral artery, MCA; middle cerebral artery, ACA; anterior cerebral artery, PICA; posterior inferior cerebellar artery
Deaths of ICH within 24 h after admission (n = 35).

Group: A; anticoagulants therapy, B; Non-anticoagulants therapy
Anticoagulants: a; Warfarin, b; Aspirin, c; Clopidogrel, d; Ticlopidine
Past illness: HT; hypertension, HL; hyperlipidemia, CI; cerebral infarction, DM; diabetes mellitus, TIA; Transient ischemic attack, ICH; intracerebral hemorrhage, af; atrial fibrillation, PE; pulmonary embolism, CHF; congestive heart failure, AR; aortic regurgitation, IHD; ischemic heart disease, post CABG; post heart bypass operation, ASO(stent); arteriosclerosis obliterans, DVT; deep vein thrombosis, IC stenosis; internal carotid artery stenosis, SSS(PMI); sick sinus syndrome(pacemaker implantation), CD; coagulation disorder, cLD; chronic liver dysfunction, LC; liver carcinoma
Characteristics of survival and death of ICH patients admitted within 24 h after stroke onset.

Odds ratios for factors associated with deaths in ICH patients within 24 h post-admission.
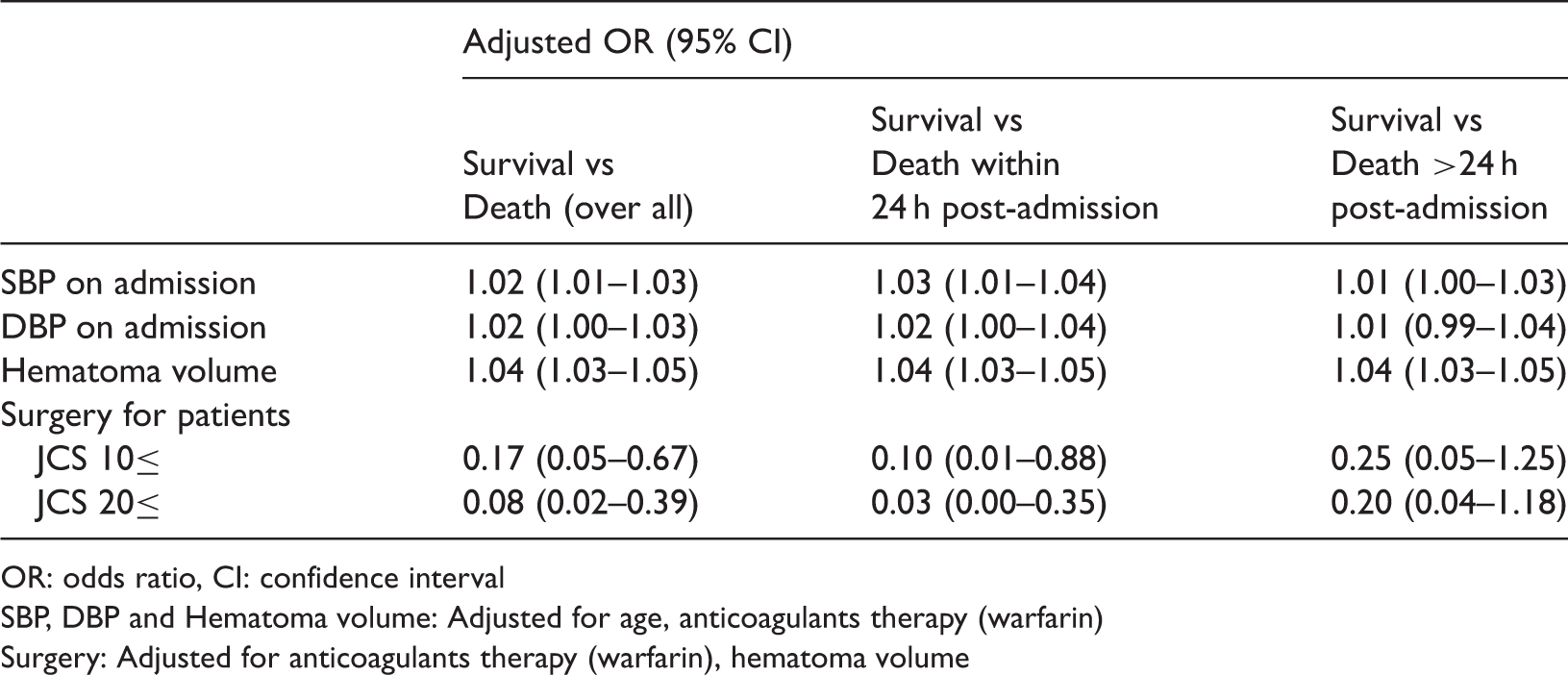
OR: odds ratio, CI: confidence interval
SBP, DBP and Hematoma volume: Adjusted for age, anticoagulants therapy (warfarin)
Surgery: Adjusted for anticoagulants therapy (warfarin), hematoma volume
Deaths of SAH patients within 24 h after admission(n = −7).

Post illness: HT; hypertension, HL; hyperlipidemia, TIA; transient ischemic attack, AP;angina pectoris, PTCA; percutaneous transluminal coronary angioplasty
location: MCA; middle cerebral artery, A com; anterior communicating artery
The cause of death during Period I in all except one patient with stroke was the primary disease. This one patient (Patient 6) died of systemic embolism associated with cardiogenic stroke (Table 5).
A review of the appropriateness of treatment based on the Guidelines for the Management of Stroke 2009 2 ) and the treatment manual for the authors’ medical centre indicated no problems with the treatment of CI or SAH. However, in two patients with ICH, an investigation of the indications for surgery was considered necessary. The level of consciousness in both patients was a JCS score of 3 to 10. One patient (Patient 11) was undergoing antithrombotic therapy and had a hematoma volume of ≥50 ml at the time of admission, and the other patient (Patient 30) had difficult-to-control hypertension (Table 6).
Discussion
Initial treatment of acute stroke in SUs has reduced deaths due to stroke complications, leading to decreased mortality rates and shorter hospital stays.5,6,9 The authors’ medical centre, which provides initial treatment to patients with acute stroke through an SCU, has a mortality rate of 6.0%; this is lower than previously reported rates of 20.9%, 12.1%, 10.47%, 10.1%, and 9.2%.5–9 This low rate was achieved using a team-oriented medical approach within the SCU established at the authors’ medical centre in September 1997, providing a systematic approach to acute stroke care. 12
The reported mortality rate among a large number of hospitals in Japan is 10.8%. 13 The reported mortality rate for the acute period (within 30 days) in the USA is 10.47%. 7 In New York state, the reported mortality rate ranges from 10.1% to 12.5%. 8 These mortality rates resemble those in Japan. In other reports, the stroke mortality rates among 22 countries classified into 5 groups by area or economics were 4% in high-income countries (Australia, Canada, Croatia, Denmark, Germany, Iran, and Poland), 13% in South America (Argentina, Brazil, Chile, Colombia, Ecuador, and Peru), 4% in Southeast Asia (China, Malaysia, and Philippines), 11% in India, and 22% in Africa (Mozambique, Nigeria, South Africa, Sudan, and Uganda). 14 In another study, the mortality-to-incidence ratio in different countries was <0.32 in Japan, China, Korea, Canada, and the USA; 0.32 to 0.35 in Mexico, Brazil, and Europe; and >0.36 in sub-Saharan Africa. 15 Although the characteristics of patient registration differed among these reports, the mortality rates were low in Asia (including Japan), the USA, and Europe and high in India and sub-Saharan Africa. These results may be related to the medical environment in each country (e.g., medical system characteristics such as the number of doctors or hospitals, insurance systems, and economic conditions).
The present study revealed that deaths within 24 h after admission for acute stroke were significantly higher among patients with ICH than among those with SAH or CI. Although many patients are already not considered to be surgical candidates based on their level of consciousness at the initial evaluation, hematoma volume, and lesion site, it may be appropriate to consider surgery in patients with mild to moderate impairment of consciousness (JCS score of 3–20), depending on the lesion site, to improve the vital prognosis and functional prognosis.16,17
Although retrospective in design, the present study identified 2 of 35 patients (5.7%) in whom the treatment strategy should have been reconsidered during SCU management and determination of the surgical indications. Both of these patients had ICH. The first (Patient 30) had untreated hypertension and liver dysfunction, an SBP of 230 mmHg on admission, and a hematoma size that was thought to have increased after confirmation of the diagnosis because of resistance to antihypertensive therapy. When controlling blood pressure in patients with ICH, a reduction in the SBP to <160 mmHg within 1.5 h after admission has been shown to significantly reduce hematoma expansion.18,19 Strict management of SBP within the range of 120 to 160 mmHg also reportedly prevents hematoma expansion and poor outcomes. 20 Rapid, strict BP control is thus necessary in patients with untreated hypertension and liver dysfunction. The other patient (Patient 11) was undergoing antithrombotic therapy, and although the level of consciousness was only mildly impaired on admission (JCS score of 3), the hematoma volume on admission was 50 ml. Thus, if the vital prognosis alone had been considered, surgery might have been indicated.
The indications for surgery at our medical centre include lesions in the putamen, cerebellum, or subcortical area with a JCS score of ≤20, regardless of hematoma volume. A meta-analysis of the effectiveness of surgery showed significantly better outcomes of surgery when performed within 8 h of onset or for patients with a hematoma volume of 20 to 50 ml, Glasgow Coma Scale score of 9 to 12, or age of 50 to 69 years. 17 However, one study reported no significant differences in outcomes between conservative treatment and early surgery. 21 Therefore, in the absence of a definitive consensus, treatment is left to the discretion of the institution. A recent meta-analysis showed that minimally invasive surgery for treatment of initial supratentorial hematoma offers a significantly lower mortality rate than do internal medicine treatments or craniotomy. 22 Aggressive treatment with minimally invasive surgery may therefore be effective.
Treatment of acute stroke includes intravenous alteplase, which is an rt-PA, within 4.5 h of stroke onset23–25 or, in patients in whom an rt-PA is contraindicated or proves ineffective, use of a thrombus-retrieval device within 8 h of stroke onset.26–29 Because of these limited indications, conventional treatments such as intravenous edaravone23,24 are used for the many patients for whom these treatments are not indicated. Although this represents a limitation of treatment, the current study found a low rate of death within 24 h after admission. Investigation of deaths occurring ≥24 h after admission was therefore considered important, specifically to clarify treatment needs for improving the vital prognosis.
Treatment strategies for SAH can be determined according to the WFNS classification with respect to prevention of aneurysm rerupture, 32 and the present study revealed no problems regarding treatment strategies for patients with SAH. Furthermore, the present findings suggest the importance of preventing SAH secondary to unruptured cerebral aneurysm. Detection of an unruptured cerebral aneurysm on brain screening examinations (e.g., the “Brain Dock,” a brain health checkup system in Japan) may represent an effective strategy.
This study investigated the clinical features of patients with acute stroke who died within 24 h after admission. A future study is planned to investigate patients who die within 72 h after admission and to identify associated factors.
Conclusion
The mortality rate among patients with stroke transported to the authors’ hospital within 24 h of onset was lower than in previous reports. Haemorrhagic stroke accounted for many of these deaths, with a significantly high rate of ICH. Blood pressure management and the time of determining indications for surgery are important factors in acute stroke care. Detection of unruptured cerebral aneurysms is considered an important prognostic factor in SAH.
Footnotes
Declaration of conflicting interest
The Authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
