Abstract
Objective
To determine the correlation between anatomical features of the upper airway (evaluated via computed tomography imaging) and the ease of light wand-assisted endotracheal intubation in patients undergoing ear, nose and throat surgery under general anaesthesia.
Methods
Mallampati class, laryngoscopic grade, thyromental distance, neck circumference, body mass index, mouth opening and upper lip bite class were assessed. Epiglottis length and angle, tongue size and narrowest pharyngeal distance were determined using computed tomography imaging. Intubation success rate, time to successful intubation (intubating time) and postoperative throat symptoms were documented.
Results
Of 152 patients, 148 (97.4%) were successfully intubated on the first attempt (mean intubating time 11.5 ± 6.7 s). Intubating time was positively correlated with laryngoscopic grade and body mass index in both male and female patients, and Mallampati class and neck circumference in male patients. Epiglottis length was positively correlated with intubating time.
Conclusions
Ease of intubation was influenced by epiglottis length. Radiological evaluation may be useful for preoperative assessment of patients undergoing endotracheal intubation with light wand.
Introduction
Direct laryngoscopy is the standard method of tracheal intubation but it is either difficult or impossible to perform in 5.8% of apparently normal individuals, 1 particularly in unprepared patients or those requiring emergency intubation. 2 There is currently no method of airway assessment that can reliably predict difficult laryngoscopic intubation, however.3,4
Blind oral tracheal intubation using the transillumination technique with a light wand is simple, rapid and effective;5,6 it also results in fewer dental injuries than endotracheal intubation. 3 This approach does not require visualization of the vocal cords and is particularly useful in patients with difficult airways, whether the difficulty was anticipated or not.7–10 In patients with high Mallampati class, a light wand was found to have a higher rate of intubation success and shorter intubating time than direct laryngoscopic intubation. 8 The light wand is useful in cases of limited cervical motion, and may be an alternative to fibreoptic bronchoscopic intubation.9,10 Although light wand-guided intubation can be performed quickly and easily, the failure rate for a first intubation attempt is 28%; 4 it should thus be avoided in patients with known abnormalities of the upper airway. 11
It is unclear whether airway parameters that predict difficult laryngoscopic intubation can also be applied to light wand intubation. In the case of light wand intubation, obesity (body mass index [BMI] ≥ 30kg/m2) and Mallampati class III airway have been shown to predict prolonged intubating time in patients with no known airway abnormalities. 12 There was no apparent correlation between the laryngoscopic view and either orotracheal intubation 13 or nasotracheal intubation success rate, however. 14
Epiglottis length and tongue size (both measured radiologically) are used to predict difficulties in fibreoptic orotracheal intubation, 15 and may also be relevant to light wand intubation. 16 There are no studies that have investigated which airway anatomical features are associated with difficulties in light wand intubation in adults, however. The aim of the present study was to determine the correlation between anatomical features of the upper airway (evaluated via computed tomography [CT] imaging) and the ease of light wand intubation in patients undergoing ear, nose and throat (ENT) surgery under general anaesthesia.
Patients and methods
Study population
The study recruited adult patients (aged ≥20 years) with American Society of Anesthesiologists physical status I or II (https://www.asahq.org/resources/clinical-information/asa-physical-status-classification-system), who were scheduled to undergo ENT surgery with endotracheal intubation at the Department of Anaesthesiology and Pain Medicine, Uijeongbu St Mary's Hospital College of Medicine, The Catholic University of Korea, Seoul, Republic of Korea, between October 2012 and February 2014. Exclusion criteria were: known upper airway abnormalities (tumours, polyps, infections); history of neck surgery; morbid obesity (BMI ≥ 35 kg/m2); significant cardiorespiratory disease.
The ethics committee of Uijeongbu St Mary's Hospital College of Medicine, The Catholic University of Korea approved the study; and all patients provided written informed consent prior to enrolment.
Study parameters
The airway was evaluated at the preoperative visit, and the following parameters were recorded: modified Mallampati class with the patient's mouth wide open, head slightly extended and tongue maximally forward with phonation in the sitting position; 17 mouth opening (distance between first incisors, with mouth fully opened); thyromental distance (distance between thyroid notch and lower border of the mandibular mentum, with head fully extended); neck circumference at thyroid notch level; any neck motion limitation.
The upper lip bite test was performed and classified as: I (lower incisors can bite the upper lip above the vermilion line); II (lower incisors can bite the upper lip below the vermilion line); III (lower incisors cannot bite the upper lip). 18 Patient age, sex, height, weight and BMI were recorded.
Patients were stratified into groups according to the following criteria: BMI (<25kg/m2, ≥25kg/m2 to <30kg/m2, ≥30kg/m2); neck circumference (<40cm, ≥ 40cm); Mallampati class (I, II, III); laryngoscopic grade (1, 2, 3, 4); upper lip bite class (I, II, III). Overweight and obesity were classified according to the Centers for Disease Control and Prevention definition (http://www.cdc.gov/obesity/adult/defining.html).
All patients underwent routine preoperative CT scanning of the paranasal sinus or scout film of the temporal bone. CT scans were analysed by one investigator, blinded to possible intubation difficulties. Epiglottis length (tip of epiglottis to vallecula), tongue length (tip of tongue to vallecula), tongue height (from length line to highest portion of the tongue) and pharyngeal gap (narrowest pharyngeal dimension defined anteriorly by the posterior wall of the epiglottis and posteriorly by the posterior pharyngeal wall) were measured digitally on soft copies of scout views of temporal bone CT or sagittal views of paranasal sinus CT. Epiglottic angle was described as the angle between the perpendicular line subtended from the vallecula and the line subtended from the posterior wall of the epiglottis. Tongue size was calculated as its length × height (Figure 1).
Sagittal computed tomography image of the paranasal sinus indicating the measurements used in the study. 1, tongue length; 2, tongue height; 3, epiglottis length; 4, pharyngeal gap; 5, epiglottic angle (angle between a perpendicular line subtended from the vallecula and the line subtended from the posterior wall of the epiglottis)
Anaesthesia and intubation
None of the patients received premedication. Routine monitoring included electrocardiogram, noninvasive blood pressure and pulse oximetry. Patients were placed in the sniffing position with a 10-cm pillow under the head. Anaesthesia was induced with 2mg/kg propofol and 1.0–1.5 μg/kg fentanyl, after preoxygenation with 100% oxygen for 3 min. After loss of eyelash reflex, 0.6mg/kg rocuronium was administered intravenously. The lungs were manually ventilated by face mask with 3–4% sevoflurane in 100% oxygen, with fresh gas flow of 6l/min.
After muscle relaxation, laryngoscopy grade was determined in all patients via direct laryngoscopy using a Macintosh no. 3 blade. Laryngeal view was graded without external laryngeal pressure according to the Cormack classification as: grade I (complete visualization of the vocal cords); grade II (visualization of the inferior portion of the glottis); grade III (visualization of the epiglottis only); grade IV (inability to visualize the epiglottis). 19 Patients were ventilated by mask for 1 min after assessing laryngoscopic view in order to prevent hypoxaemia.
An experienced anaesthetist (J.K.) who was blinded to patients' radiological measurements performed all tracheal intubations using a well-lubricated endotracheal tube placed over a light wand (Surch-lite™; Aaron Medical, St Petersberg, FL, USA). The light source was placed at the level of the endotracheal tube tip, and the distal end of the wand and covering tube were bent to 90 ° at 7cm from the tip. 20 A size 7 endotracheal tube was used for women and a size 8 tube for men, regardless of body weight. Operating room lights were dimmed during intubation to assist visualization of transillumination. The jaw was lifted forwards with the left hand of the intubating anaesthetist, and the light wand and tube were passed down the midline of the tongue using the right hand. The cuff of the endotracheal tube was then inflated with air and intubation was confirmed by both auscultation of breath sounds and detection of carbon dioxide by the capnograph. All patients were mechanically ventilated with 2–3% sevoflurane in air/oxygen and received continuous remifentanil infusion.
The time to intubation (intubating time) and numbers of attempts and failures were recorded. Intubating time was defined as the interval from the device touching the patient's lip to complete unthreading of the light wand. A maximum of two attempts, each lasting ≤30s, was allowed; the 30-s time limit was adopted because intubation using light wand is successful within 30s in 95% of patients.7,8,12 Patients were ventilated with 100% oxygen by mask between intubation attempts. If tracheal intubation was unsuccessful after two attempts, intubation was achieved using conventional laryngoscopy.
Postoperative assessment
The presence and severity of sore throat, hoarseness and dysphagia were assessed at 18–24h postoperatively. Symptom grading was: sore throat (0, none; 1, less severe than with a cold; 2, like a cold; 3, more severe than with a cold); hoarseness (0, none; 1, noticed by patient; 2, obvious to observer; 3, aphonia); dysphagia (0, none; 1, painful with certain foods; 2, painful with all food and drink; 3, unable to swallow own secretions). 21 All complications were recorded.
Statistical analyses
The sample size calculation was based on the difference in intubating time (26.4 ± 12.1s) in a pilot study of 12 patients (unpublished data). We assumed that the difference in intubating time was clinically significant if >5.5s. Power analysis indicated that a sample size of 76 patients in each group should be adequate to detect a difference between the two groups, with a two-sided significance level of α = 0.05 and a power of 0.8.
Data were presented as mean±SD or n (%) of patients. Demographic data were analysed using an independent samples t-test, and radiological measurements in relation to intubating time were compared using univariate linear regression analysis. The correlation between Mallampati class and laryngoscopic grade was analysed by Spearman's rank correlation coefficient. Intubating times within groups were analysed using Kruskal–Wallis one-way analysis of variance on ranks, and intubating times for each variable were analysed using Pearson's and Spearman's rank correlation coefficients. The incidence and severity of sore throat were analysed using the Mann–Whitney U test and Fisher's exact test. All statistical analyses were performed using SPSS® version 13.0 (SPSS Inc., Chicago, IL, USA) for Windows®. P-values < 0.05 were considered statistically significant.
Results
Demographic and anatomical data of patients undergoing ear, nose and throat surgery under general anaesthesia included in a study to determine the correlation between anatomical features of the upper airway and the ease of light wand-assisted endotracheal intubation.

Data presented as mean±SD.
P < 0.05 versus female patients;
P < 0.01 versus female patients; independent samples t-test.
The 30-s time limit for intubating was exceeded in two patients, and oesophageal intubation occurred in two patients; all four of these patients were successfully intubated on the second attempt. Three of the four patients were overweight/obese (i.e., BMI ≥ 25kg/m2). First-attempt and overall tracheal intubation success rates were 148/152 (97.4%) and 152/152 (100%), respectively. Mean time to successful intubation on the first attempt and overall intubating time were 11.5 ± 6.7s and 12.4 ± 8.7s, respectively.
Data presented as n (%) of patients.
There was significant correlation between Mallampati class and laryngoscopic grade (P < 0.0001); Spearman's rank correlation coefficient.
Time taken to successful first-attempt light wand-assisted endotracheal intubation a in patients undergoing ear, nose and throat surgery under general anaesthesia (n = 152).

Data presented as mean±SD (range).
The interval from device touching the patient's lip to complete unthreading of the light wand.
P < 0.05 versus body mass index <25 kg/m2;
P < 0.05 versus neck circumference < 40 cm;
P < 0.05 versus Mallampati class I;
P < 0.05 versus laryngoscopic grade 1; Kruskal–Wallis one-way analysis of variance.
Univariate linear regression analysis of the association between anatomical features of the upper airway (evaluated via computed tomography imaging) and the time taken to successful first-attempt light wand-assisted endotracheal intubation a in patients undergoing ear, nose and throat surgery under general anaesthesia (n = 152).
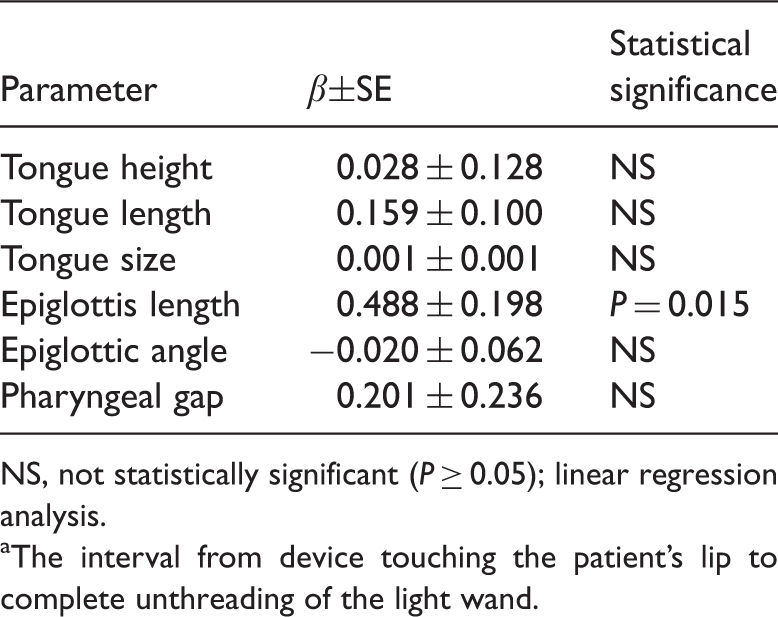
NS, not statistically significant (P ≥ 0.05); linear regression analysis.
The interval from device touching the patient's lip to complete unthreading of the light wand.
Correlation between anatomical parameters and time taken to successful first-attempt light wand-assisted endotracheal intubation a in patients undergoing ear, nose and throat surgery under general anaesthesia.

NS, not statistically significant (P ≥ 0.05).
Spearman's rank correlation coefficient for laryngoscopic grade and Mallampati class, Pearson's correlation coefficient for all other measurements.
The interval from device touching the patient's lip to complete unthreading of the light wand.
Throat discomfort parameters following light wand-assisted endotracheal intubation in patients undergoing ear, nose and throat surgery under general anaesthesia, stratified according to intubating time a

Data presented as n (%) of patients.
No statistically significant between-group differences (P ≥ 0.05); Mann–Whitney U test.
The interval from device touching the patient's lip to complete unthreading of the light wand.
Sore throat: 0, none; 1, less severe than with a cold; 2, like a cold; 3, more severe than with a cold.
Hoarseness: 0, none; 1, noticed by patient; 2, obvious to observer; 3, aphonia.
Dysphagia: 0, none; 1, painful with certain foods; 2, painful with all food and drink; 3, unable to swallow own secretions.
Discussion
Radiological assessment of airway anatomical characteristics determined that epiglottis length was correlated with intubating time in the present study. Both laryngoscopic grade and BMI were correlated with intubating time in male and female patients, and there were significant correlations between intubating time and Mallampati class and neck circumference in male patients. Epiglottic angle, tongue size, pharyngeal gap, mouth opening and upper lip bite class were not associated with intubating time in male or female patients.
Anaesthetic induction affects muscle tone, resulting in a degree of upper airway obstruction ranging from narrowing to complete obstruction, which may hinder manoeuvrability of a light wand. 22 Use of a jaw lift (as in the present study) elevates the epiglottis and enhances the passage of the intubation tube/light wand. 16 It is possible that a long epiglottis may prevent the free advancement of the tube into the trachea, even with the use of a jaw lift. A study of 76 patients undergoing light wand intubation with jaw lift found that the epiglottis was deviated in five patients (6.6%) and enfolded in one (1.3%), even when intubation was successful. 16
Although a long epiglottis significantly prolonged the time required for successful intubation in the present study, all of our patients were successfully intubated, in accordance with the findings of others.7,8,13 Moreover, there was no correlation between intubating time and any other radiologically assessed airway parameter (epiglottic angle, tongue size and pharyngeal gap) in the present study. We performed CT imaging with the patients awake and in the supine position, without jaw lifting. It is therefore possible that the position of the epiglottis and tongue in relation to the pharynx, as revealed by these scans, would differ from that occurring under general anaesthesia. However, even in cases where the epiglottis falls on the posterior pharyngeal wall, the tip of the light wand can be placed at the glottic opening when guided from the lateral posterior side through the piriform fossa. 5 Our findings are in accordance with others who showed that, in contrast to laryngoscopy, the ease of light wand-assisted intubation did not appear to be influenced by anatomical variations in the upper airway. 3 In a study of 265 patients who experienced difficult intubation, all patients were successfully intubated using a light wand. 7
The Cormack and Lehane classification of laryngoscopic view is frequently used to predict a difficult laryngoscopy. 19 Intubating time was longer in patients with high laryngoscopic grade in the present study, regardless of sex. Other studies have found no correlation between high laryngoscopic grade and orotracheal intubation 13 or nasotracheal intubation success rates. 14 These studies placed the patient's head and neck in a neutral or relatively extended position, in contrast to the present study where the head was placed in the sniff position with jaw lift. In a sniff position, the epiglottis is almost in contact with the posterior pharyngeal wall, making it difficult for the light wand to pass underneath the epiglottis. 11 The discrepancy between these studies and our study may, in part, be accounted for by the different head position during the intubation.
Mallampati class was significantly correlated with intubating time in the present study. This finding is in accordance with others, who reported that Mallampati class is a good indicator of ease of light wand intubation in patients without known airway abnormality. 12 In contrast, a further study reported no correlation between Mallampati class and ease of light wand intubation in patients without known or potential problems relating to intubation. 3 Mallampati class is a valuable estimate of tongue size relative to the capacity of the oropharynx, 23 and was modified to reliably predict difficult laryngoscopy with the patient sitting, head in extension, tongue out and with phonation. 17 Differences in the methods used to assess Mallampati class may explain the discrepancies between different study findings. Alternatively, these differences may be due to variation in the definition of intubating time. The present study defined the beginning of intubation as the moment when the device touched the patient's lip, whereas Hung et al 3 used the point when the device was inserted into the hypopharynx – this may have meant that the time-consuming part of intubation in patients with a large tongue was excluded, resulting in a similar intubation time in patients with or without hindrance from the tongue.
Being overweight or obese (i.e., BMI ≥ 25 kg/m2) significantly increased intubating time in the present study. In accordance with our findings, others have noted failure of light wand-assisted intubation in overweight or obese patients.3,7,24 Intubation using the Surch-lite™ requires visualization of a central bright transillumination glow through the anterior neck rather than visualization of the laryngeal structure. Magnetic resonance imaging of fat deposits around the upper airway in obese patients revealed that these fat deposits were anterior to the laryngopharyngeal airspace and in submental regions. 25 It is expected, therefore, that intubating time would be prolonged with increasing BMI, because the increased fat deposits in the neck mask the light, and thereby increase the time taken to visualize the transillumination. 26 Patients with severe obesity (BMI≥35kg/m2) were therefore excluded from the present study.
Neck circumference is significantly correlated with visceral abdominal and neck fat. 27 Light wand-guided intubation has been shown to be difficult in obese patients and in those with short, thick necks. 28 These problems may be overcome by using simple steps, such as extending the neck by placing a support under the shoulder, using a brighter light source, and switching off or dimming the operating room lights when necessary.6,7,11 Transillumination of the light wand at the neck can also be enhanced by adjustment of the bent length or angle of the light wand against the wall of the trachea. 20
Sore throat and hoarseness are common complaints after laryngoscopy and endotracheal intubation. 21 Since light wand-guided intubation is performed without visualization of the laryngeal structures, it would be expected to result in airway complications more frequently than laryngoscopic intubation. Sore throat has been shown to occur less frequently after light wand-guided intubation than laryngoscopic intubation (17.1% versus 25.3%), however, 3 thus suggesting that the former is less traumatic than the latter. The incidence of throat discomfort was higher in the present study than in other studies; 3 this is because we included mild degrees of discomfort, most of which would not have been regarded as true symptoms in routine practice. The incidence of more severe symptoms (grade 2/3) in our study was comparable with the findings of others. 29 We found no relationship between intubating time and the incidence and severity of throat discomfort symptoms.
The current study has several limitations. First, the epiglottis is concave and round but was measured as a straight line, meaning its true length may not have been represented. Secondly, a reduction in light intensity may affect the success rate of light wand intubation, but we did not adjust the intensity of the light bulb. Thirdly, we excluded patients with known upper airway abnormalities because these are absolute contraindications to the blind light wand technique. 6 As a result, our findings may not be applicable to patients with known abnormalities. Finally, all intubations were performed by a single anaesthetist, and our data may therefore be biased towards the expertise of that operator. Patients were unintentionally sampled so that the likelihood of a difficult airway was dispersed throughout the study period, however. In addition, the anaesthetist was very experienced in light wand intubation.
In conclusion, the ease of intubation using a light wand (Surch-lite™) is influenced by epiglottis length. In addition, high laryngoscopic grade and high BMI in male and female patients, and high Mallampati class and neck circumference in male patients, may complicate light wand-guided tracheal intubation. Radiological evaluation may be useful for preoperative assessment of patients undergoing endotracheal intubation with light wand.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.

