Abstract
Objectives
To investigate the ability of synovial fluid from patients with rheumatoid arthritis (RA) or osteoarthritis (OA) to modulate cell-surface phenotype, function and viability of monocytes.
Methods
Monocytes from healthy donors were incubated with synovial fluid from patients with RA or OA. These were then cultured with autologous healthy CD4+ T-cells. Immunoglobulin-like transcript 4 (ILT4) and CD86 were evaluated on stimulated monocytes and CD4+ T-cells via fluorescence activated cell sorting.
Results
Monocytes incubated with synovial fluid from patients with RA (SF-RA; n = 12) had significantly lower ILT4 and higher CD86 levels than those incubated with synovial fluid from patients with OA (SF-OA; n = 12) or medium alone. In patients with RA, there was a significant negative correlation between ILT4 and disease activity score (DAS; r = −0.699), and a positive correlation between CD86 and DAS (r = 0.626). T-cells costimulated with monocytes cultured with SF-RA produced significantly more interferon-γ and tumour necrosis factor-α than those costimulated with monocytes cultured with SF-OA or controls.
Conclusions
Soluble mediators in SF-RA could contribute to modulating inflammation and local effectiveness of the immune response.
Keywords
Introduction
Monocytes and macrophages represent the major immune cells in synovial tissues and are responsible for the chronic inflammation and joint destruction evident in rheumatoid arthritis (RA). Hallmarks of local pathology are infiltration of neutrophils, lymphocytes and macrophages, as well as the expansion of resident fibroblasts in the synovium. The majority of immune cells within synovial tissues are macrophages; these are recruited profusely in RA and contribute to joint destruction.1,2 Several proteins involved in inflammatory pathways and the immune response have been identified in the synovial fluid of patients with RA (SF-RA). 3
The aim of the present study was to investigate the ability of SF-RA to modulate cell-surface phenotype, function and viability of monocytes in RA. We evaluated the presence of immunoglobulin-like transcript 4 (ILT4; a receptor crucial to monocyte tolerogenic function) and CD86 (a regulator of T-cell activation).
Patients and methods
Study population
The study recruited patients aged ≥18 years with active knee RA, and age- and sex-matched patients with knee osteoarthritis (OA), attending the Rheumatology Unit of the University of Rome “Tor Vergata”, Rome, Italy, between February 2013 and February 2014. Exclusion criteria for patients with RA were local intra-articular corticosteroid injection within 5 weeks before synovial fluid: aspiration and treatment with biological agents. Clinical data were collected retrospectively from patient charts and included disease duration, C-reactive protein (CRP), rheumatoid factor (RF) and anticyclic citrullinated peptide antibody (ACPA) levels, disease activity score (DAS) 44, 4 and treatment.
The study was carried out in accordance with the Declaration of Helsinki and International Conference on Harmonisation Good Clinical Practice Guidelines. The ethics committee of the University of Rome “Tor Vergata” approved the study, and all patients provided written informed consent prior to enrolment.
Synovial fluid collection
Synovial fluid was collected via joint aspiration in association with therapeutic arthrocentesis. Approximately 2–4 ml of synovial fluid was collected in sodium heparin-coated Vacutainer™ tubes (Becton, Dickinson and Co., East Rutherford, NJ, USA); samples contaminated with blood were discarded. Immediately after collection, samples were centrifuged at 1000
Monocyte culture
Whole venous blood samples from the antecubital vein were collected from healthy volunteers using standard methods; peripheral blood mononuclear cells (PBMCs) were isolated using Histopaque®1077 (Sigma, St. Louis, MO, USA) according to the manufacturer’s instructions. PBMCs were washed twice in phosphate buffered saline (PBS, pH 7.4) and centrifuged at 130
Elutriated monocytes were plated at 5 × 105 cells/well in 200 μl in 96-well V-bottom plates (Corning Incorporated, Corning, NY, USA), in RPMI-1640 medium supplemented with 20% FCS, 2 mM L-glutamine, 50 IU/ml penicillin, 50 µg/ml streptomycin (complete medium) and cultured at 37°C in a humidified atmosphere of 5% carbon dioxide in air for 72 h, in the presence or absence of 20 μl synovial fluid (from each study subject) and/or 10 µg/ml adalimumab (Humira®, AbbVie, Chicago, IL, USA).
FACS
Monocytes were washed once with washing buffer (3% (v/v) FCS and 0.1% (w/v) sodium azide in PBS (pH 7.4), then incubated with R-phycoerythrin-cyanine (PC5)-conjugated anti-CD14 (Immunotech, Marseille, France), phycoerythrin-conjugated anti-ILT4 (Immunotech), or fluorescein isothiocyanate (FITC)-conjugated anti-CD86 (BD Biosciences, San Jose, CA, USA) (each 1 : 10 dilution), for 30 min at 4°C in the dark. The negative range and staining specificity for each cell-surface marker was established using a corresponding isotype-matched control antibody, conjugated with the same fluorescent dye. Flow cytometry was performed using a FACScan™ flow cytometer and analysed with CellQuest™ software (both from Beckton Dickinson, Franklin Lakes, NJ, USA). For each analysis, 104 events were gated on CD14 expression and a light-scatter gate, designed to either include only viable cells (surface markers determination) or exclude cellular debris (determination of intracellular cytokine production).
The ability of synovial fluid to modulate the costimulatory effect of monocytes was evaluated as follows. PBMC from a single donor were used to generate (i) purified monocytes via elutriation, and (ii) purified CD4+ T cells using a T cell-negative isolation kit (Dynal®; ThermoFisher Scientific). Monocytes were used just after elutriation and CD4+ T cells were frozen just after purification. Monocytes were incubated for 72 h in the presence or absence of synovial fluid from each participant, harvested, washed, plated at 2 × 105/ml in a flat-bottom 96-well plate coated with anti-CD3 antibody (10 µg/ml; Beckton Dickinson), then mixed 1 : 1 with thawed autologous CD4+ T cells in the presence of 1 µg/ml brefeldin A (Sigma) and incubated for 18 h at 37°C in the dark. At the end of the incubation period, cells were washed with washing buffer (formulated as a neutral pH,7.4)] and incubated with 1 : 10 PC5-conjugated anti-CD3 (Immunotech) for 30 min at 4°C in the dark. Cells were permeabilized in BD Cytofix/Cytoperm™ (Pharmingen, San Jose, CA, USA), stained with 1 : 10 FITC-conjugated anti-interferon (IFN)-γ (R&D Systems, San Diego, CA, USA) for 30 min at room temperature. The negative range and staining specificity for each cell-surface marker and cytokine was established using a corresponding isotype-matched control antibody, conjugated with the same fluorescent dye.
Cell viability and apoptosis
Elutriated monocytes were cultured in the presence or absence of synovial fluid or serum from each patient with RA. At the end of the incubation period, cells were washed twice in PBS (pH 7.4), detached by gentle scraping, and collected by low-speed centrifugation (100
Statistical analyses
Data were presented as mean ± SD, median (interquartile range) or n (%). Normality of distribution was assessed using Kolmogorov–Smirnov goodness-of-fit test. Between-variable comparisons were made using Student’s t-test or Mann–Whitney U-test. Correlations were evaluated via Pearson’s parametric test for univariate analysis. P-values < 0.05 were considered statistically significant. All statistical analyses were performed using SPSS® version 10.0 (SPSS Inc., Chicago, IL, USA) for Windows®.
Results
Demographic and clinical characteristics of patients with rheumatoid arthritis (RA) or osteoarthritis (OA) included in a study investigating the effects of their synovial fluid samples on the surface phenotype of normal monocytes.

Data presented as mean ± SD, n (%), or median (interquartile range).
Student’s t-test or Mann–Whitney U-test.
NS, not statistically significant (P ≥ 0.05); DAS, disease activity score; NA, not applicable; CRP, C-reactive protein; RF, rheumatoid factor; ACPA, anticitrullinated protein antibody; NSAIDs, nonsteroidal anti-inflammatory drugs; DMARDs, disease-modifying antirheumatic drugs.
Cell-surface levels of ILT4 were significantly lower in monocytes cultured with SF-RA than in control cells cultured in medium alone (P = 0.0023; Figure 1a). In contrast, cell-surface levels of CD86 were increased in monocytes cultured with SF-RA compared with control cells (P = 0.0001; Figure 1b). There was a significant negative correlation between DAS and ILT4 levels (r = −0.699; P = 0.11; Figure 1c), and a significant positive correlation between DAS and CD86 levels (r = 0.626, P = 0.03; Figure 1d). There were no correlations between ILT4 or CD86 and CRP, RF or ACPA levels, duration of disease and medications (data not shown).
Cell-surface levels of (a) immunoglobulin-like transcript 4 (ILT4) and (b) CD86 in normal monocytes incubated with synovial fluid (SF) samples from patients with osteoarthritis (OA) or rheumatoid arthritis (RA). Pearson correlation analysis of disease activity score (DAS44)
4
with cell-surface levels of (c) ILT4 and (d) CD86 in patients with RA. (e) Effect of SF on production of interferon-γ (IFN-γ) by normal CD4+ T-cells costimulated with SF-primed monocytes. (f) Effect of SF on monocyte viability. Data are mean ± SD of three separate experiments, carried out with cells from three different subjects and conducted in triplicate wells.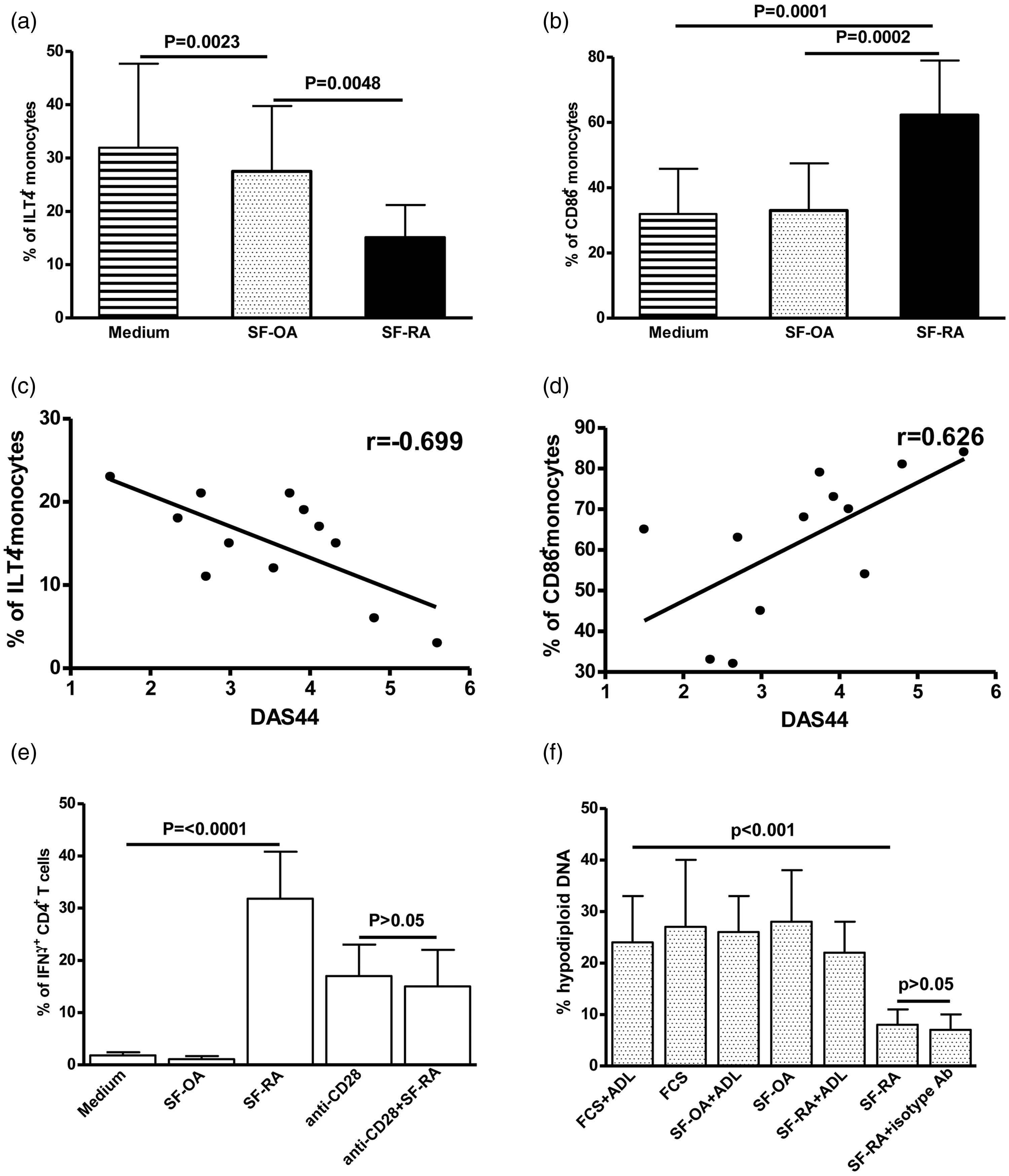
Costimulation of CD4+ T cells with monocytes incubated with SF-RA resulted in significantly higher IFN-γ and TNF-α production than observed in CD4+ T cells costimulated with monocytes incubated with SF-OA, or control monocytes (P < 0.001 for both comparisons; Figure 1e). SF-RA had no effect on IFN-γ production by normal lymphocytes stimulated with anti-CD3 monoclonal antibody (mAb) and anti-CD28 mAb (Figure 1e). As shown in Figure 1f, SF-RA significantly reduced the percentage of hypodiploid DNA compared with SF-OA or FCS. The addition of adalimumab significantly increased the amount of hypodiploid DNA formation compared with monocytes incubated with SF-RA.
Discussion
We have demonstrated that monocytes incubated with SF-RA acquire a nontolerogenic/activated surface phenotype, characterized by reduced levels of ILT4 and increased levels of CD86. 8 These changes in monocyte surface phenotype induced by SF-RA were associated with an increased ability to costimulate autologous CD4+ T cells, and increased proinflammatory cytokine production. Finally, we provided evidence that SF-RA reduces the rate of spontaneous apoptosis of monocytes that is reversed by the addition of adalimumab. ILT4 has been shown to exert a negative influence on the stimulatory capacity of antigen presenting cells, 9 exerting either a direct influence on innate effectors or an indirect effect on the adaptive response and possibly playing a pathogenic role in RA. 10 Indeed, changes in the relative balance of activating and inhibitory ILTs in the synovium could lead to inappropriate activity of innate immune agents that may then drive T-cell activation. 11 Our findings suggest that soluble mediators in SF-RA could be contributing factors in modulating the local effectiveness of the immune response and inflammation.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
Editorial assistance was provided by Gayle Robins on behalf of HPS–Health Publishing and Services Srl and funded by Pfizer Italia.
