Abstract
Objective
To investigate the clinical efficacy of neoadjuvant chemotherapy (NAC) with irinotecan (CPT-11) and nedaplatin (NED) followed by radical hysterectomy.
Methods
Patients with locally advanced cervical cancer (stage Ib2–IIb) were treated with NAC followed by surgery, primary surgery or primary radiotherapy. NAC was usually performed using transuterine arterial chemotherapy (TUAC) or intravenous CPT-11/NED. Survival rates were analysed in the three treatment groups; response rates and adverse events associated with NAC, TUAC and CPT-11/NED were compared, along with previously reported adverse events of chemoradiotherapy.
Results
A total of 165 patients with cervical cancer were recruited. Of these, 70 were treated with NAC followed by surgery (48 with CPT-11/NED, 18 with TUAC and four with other types of chemotherapy), 73 were treated with primary surgery and 22 with primary radiotherapy (including chemoradiotherapy). There were no significant differences in progression-free survival or overall survival rates between the three treatment groups. The response rates for the NAC regimen of CPT-11/NED and TUAC were high (75% and 78%, respectively). The frequency of severe thrombocytopenia was lower in patients receiving CPT-11/NED compared with TUAC, and the incidence of severe anaemia, vomiting and cystitis was lower in patients receiving CPT-11/NED compared with chemoradiotherapy.
Conclusions
The use of CPT-11/NED as a NAC regimen shows favourable activity, with lower toxicity compared with NAC using TUAC or chemoradiotherapy, for the treatment of locally advanced cervical cancer.
Keywords
Introduction
Treatments for locally advanced cervical cancer, defined as International Federation of Gynecology and Obstetrics (FIGO) stage Ib2–IIb, 1 include primary surgery, neoadjuvant chemotherapy (NAC)2–4 and concurrent chemoradiotherapy (CCRT).5,6 In many countries, CCRT is accepted as the standard therapy for such tumours.7,8 However, each of these therapies has both advantages and disadvantages.
In our institute, locally advanced cervical cancer is treated surgically, with NAC being given prior to surgery in many patients. NAC was previously administered in the form of transuterine arterial chemotherapy (TUAC), 9 but more recently it has been given using intravenous irinotecan hydrochloride (CPT-11) and nedaplatin. 10
DNA topoisomerases are enzymes that regulate and control DNA topology. Topoisomerase 1 catalyzes the transient cutting of a single DNA strand, the passage of another DNA strand through the break and then resealing of the DNA break. 11 Camptothecin (CPT), an antitumour alkaloid isolated from Camptotheca acuminata, interferes with DNA topoisomerase 1 function. 12 A derivative known as CPT-11 has been synthesized in Japan 13 and exhibits relatively high efficacy in patients with recurrent or refractory cervical cancer, with a response rate of 23.6%. 14
Nedaplatin (cis-diammine glycolato platinum, also known as 254-S) is a platinum analogue and second-generation platinum-co-ordination complex, developed in Japan. 15 It has higher water solubility than cisplatin and shows very limited binding to plasma proteins. This results in lower levels of renal, gastrointestinal or neurological toxicity for nedaplatin compared with cisplatin, 16 with no need for hydration during nedaplatin administration. The sensitivity of cervical cancer to nedaplatin has been reported to be high in vitro. 17 High efficacy has been described in patients with cervical cancer, with an overall response rate of 46.3% and a response rate of 53.1% in squamous cell carcinoma (SCC). 18
Based on these findings, the combination of CPT-11 and nedaplatin (CPT-11/NED) may be clinically useful for treating cervical cancer. The inhibition of topoisomerase 1 by CPT-11 is enhanced 10-fold in the presence of nedaplatin; 19 patients with cervical cancer display a high response rate to CPT-11/NED,20,21 with the highest reported response rate being 81%. 22 These data support the use of CPT-11/NED as a NAC regimen in stage Ib–IIb cervical cancer.
In the present study, survival of patients treated with NAC followed by surgery, primary surgery or primary radiotherapy (including CCRT) for stage Ib2–IIb cervical cancer was analysed. In addition, the effectiveness of NAC using CPT-11/NED or TUAC was compared, and the adverse events associated with these two NAC regimens were compared with the known adverse events reported for CCRT.
Patients and methods
Patients with stage Ib2–IIb uterine cervical cancer treated at Kyoto University Hospital, Kyoto, Japan, between January 1999 and December 2012 were recruited to the study. Patients were treated with primary surgery, NAC followed by surgery, or primary radiotherapy. Further adjuvant treatments were used in some patients after primary surgery or NAC followed by surgery.
Until 2006, most patients with stage Ib2–IIa SCC of the cervix underwent primary surgery, with only those with very bulky tumours receiving NAC in addition. This policy was changed in 2007, after which NAC was used in most patients with Ib2–IIb cervical SCC. The protocol for NAC was also changed during the study period. Between 1999 and 2007, NAC was mostly performed using TUAC. After this time, NAC was primarily given in the form of intravenous CPT-11/NED.
The study protocol was approved by the Ethics Committee of Kyoto University Hospital, and all patients provided written informed consent prior to study entry.
Preoperative NAC regimens
The TUAC regimen comprised transuterine administration of cisplatin 70 mg/m2, doxorubicin 40 mg/m2, mitomycin C 20 mg and 5-fluorouracil 500 mg. 9 The CPT-11/NED regimen comprised intravenous administration of CPT-11 (60 mg/m2) on days 1 and 8, and nedaplatin (80 mg/m2) on day 1 of a 21-day cycle. Radical hysterectomy was performed after between one and three courses of NAC.
Other NAC regimens used in a small number of patients included intravenous paclitaxel (175 mg/m2) plus carboplatin with a target area under the concentration versus time curve of 6 mg/ml per min, and intravenous nedaplatin (80 mg/m2) plus peplomycin (5 mg daily for 5 days) plus ifosfamide (1200 mg).
Evaluation
Tumour size, degree of parametrial invasion and extent of uterine corpus and/or bladder/rectal invasion were evaluated using computed tomography before treatment in all patients and again after NAC in the NAC group. Lymph node status 23 was evaluated by computed tomography before treatment in the NAC and radiotherapy groups, and pathologically after treatment in the NAC and primary surgery groups. Lymph node swelling was defined as a short axis diameter ≥ 10 mm. Progression-free survival (PFS) and overall survival (OS) rates were recorded in all three groups. Adverse effects were assessed in accordance with Common Terminology Criteria for Adverse Events version 4.0; 24 toxicities of G3 and G4 were defined as ‘severe’.
Statistical analyses
Data were presented as mean, mean ± SD, n or n(%). The required sample size was calculated based on analyses of the mean ± SD age of patients treated with NAC, primary surgery and radiotherapy, and the proportion of patients with stage IIb cancer.
Differences in PFS and OS between the groups were compared using the log-rank test. Patient and tumour characteristics and adverse events were compared using Fisher’s exact test, apart from age and tumour size, which were compared using Student’s t-test.
A P-value < 0.05 was considered to be statistically significant. Statistical analyses were performed using STATA™ software, version 13 (StataCorp LP, College Station, TX, USA) and JMP Pro version 11 (SAS Institute Inc., Cary, NC, USA).
Results
A total of 165 patients with stage Ib2–IIb uterine cervical cancer were recruited to the study. Of these, 70 patients were treated with NAC followed by surgery, 73 were treated with primary surgery and 22 were treated with radiotherapy, including 12 patients treated with CCRT. Of the 70 patients treated with NAC, 18 received TUAC, 48 received CPT-11/NED, two received paclitaxel and carboplatin, and two received nedaplatin, peplomycin and ifosfamide.
Of the 73 patients who underwent primary surgery, seven (10%) received no further treatment, 33 (45%) received chemotherapy and 33 (45%) received CCRT. Of the 70 patients who underwent NAC followed by surgery, three (4%) received no further treatment, 53 (76%) received chemotherapy and 14 (20%) received CCRT. In these patients, chemotherapy was selected as an adjuvant treatment if the tumour was sensitive to chemotherapy; if it was not, CCRT was selected. CCRT was also selected as the adjuvant treatment for patients who were older (>75 years old) and/or had serious complications (heart failure, respiratory failure, malnutrition, etc.).
Patient and tumour characteristics of patients with stage Ib2–IIb uterine cervical cancer treated with neoadjuvant chemotherapy followed by surgery (NAC), primary surgery or radiotherapy (n = 165).

Data presented as mean (range) or n (%) of patients.
P < 0.001, bP = 0.002 and cP ≤ 0.001 compared with the other two groups using Fisher’s exact test or Student’s t-test.
Clinical efficacy of neoadjuvant chemotherapy (NAC) in patients with stage Ib2–IIb uterine cervical cancer evaluated using computed tomography.
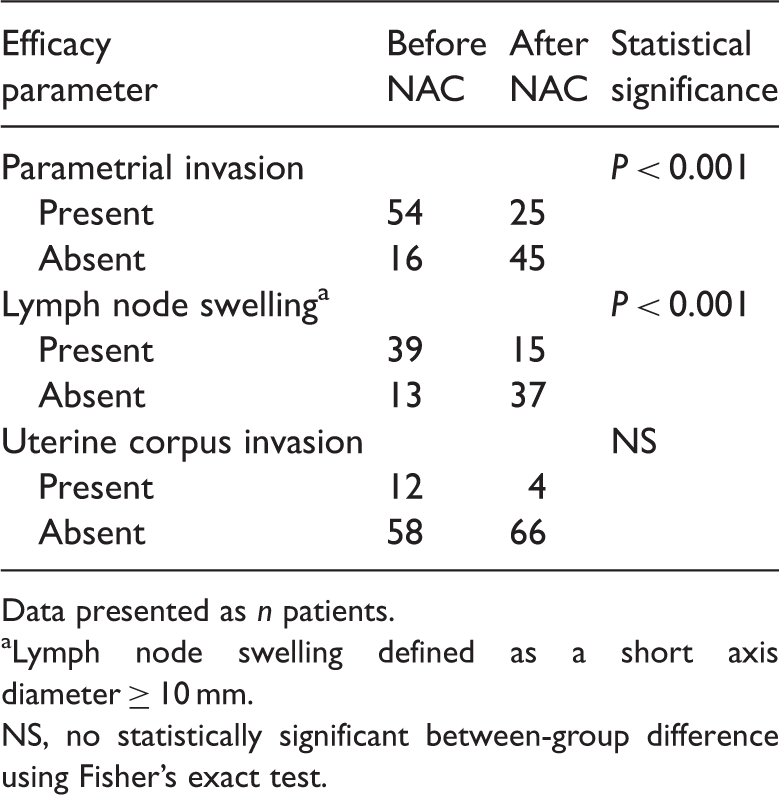
Data presented as n patients.
Lymph node swelling defined as a short axis diameter ≥ 10 mm.
NS, no statistically significant between-group difference using Fisher’s exact test.
A higher proportion of patients with stage IIb disease underwent NAC followed by surgery than underwent primary surgery. However, the rate of microscopic residual parametrial cancer cells in resected tissue in patients receiving NAC followed by surgery (31/70; 44%) was significantly lower than in those receiving primary surgery (52/73; 71%) (P = 0.0013). The rate of microscopic residual lymphovascular cancer cells in resected tissue in patients receiving NAC followed by surgery (37/70; 53%) was also significantly lower than in those receiving primary surgery (52/73; 71%) (P = 0.0261).
Comparison of PFS and OS rates between the three groups showed no significant differences (Figure 1). When OS rates among patients with stage Ib2 SCC cervical cancer (n = 32) in the three treatment groups were compared, patients treated with NAC followed by surgery had significantly higher OS rates than those treated with primary surgery (P = 0.034) (Figure 2).
(A) Progression-free survival (PFS) and (B) overall survival (OS) rates in patients with stage Ib2–IIb uterine cervical cancer treated with neoadjuvant chemotherapy followed by surgery (NAC), primary surgery or radiotherapy (n = 165). NS, no statistically significant between-group differences using log-rank test. Overall survival (OS) rates in patients with stage Ib2 squamous cell carcinoma of the cervix (n = 32) treated with neoadjuvant chemotherapy followed by surgery (NAC), primary surgery or radiotherapy. P-value calculated using log-rank test.

Use of neoadjuvant chemotherapy (NAC) with systemic irinotecan and nedaplatin (CPT-11/NED) compared with transuterine arterial chemotherapy (TUAC) in patients with stage Ib2–IIb uterine cervical cancer.

Data presented as mean, n patients or n (%) of patients.
Severe toxicities observed in patients with stage Ib2–IIb uterine cervical cancer receiving neoadjuvant chemotherapy with systemic irinotecan and nedaplatin (CPT-11/NED) or transuterine arterial chemotherapy (TUAC) and previously reported adverse events associated with chemoradiotherapy (CCRT). 24

Compared with CPT-11/NED group using Fisher’s exact test.
NS, no statistically significant difference.
Discussion
In our institute, locally advanced cervical cancer (stage Ib2–IIb) is treated using NAC prior to radical surgery, primary radical surgery or primary radiotherapy. The present study analysed the use of these treatments and their outcomes in order to assess the clinical efficacy of NAC using CPT-11/NED.
Older patients with advanced disease and/or serious complications were treated with primary radiotherapy or CCRT, because of the high risks of surgery in these circumstances. Younger patients with earlier stage disease or cervical adenocarcinoma were treated with primary radical surgery, as cervical adenocarcinoma may display resistance to chemotherapy and radiotherapy.26–28 Patients with lymph node metastasis and parametrial invasion on CT imaging as far as possible (i.e. other than the high-risk patients who could not be operated on) were given NAC prior to radical hysterectomy. In patients receiving NAC followed by surgery, further chemotherapy was given as an adjuvant treatment if the tumour was found to be chemotherapy sensitive.
In the present study, there were no significant differences in PFS or OS rates for stage Ib2–IIb cervical cancer between the three different treatment groups. However, more patients with advanced-stage disease were treated with NAC than with primary surgery. A comparison of OS rates between the NAC and primary surgery groups in patients with stage Ib2 SCC cervical cancer showed the prognosis was better in the former group than in the latter (P = 0.034), suggesting that NAC with CPT-11/NED or TUAC may result in a significantly improved prognosis compared with primary surgery. These results are consistent with a Cochrane review. 29 In addition, in the present study the use of NAC was associated with other advantages, including significant reductions in the frequency of parametrial invasion or lymph node swelling (Table 2). These changes improve the likelihood of achieving complete tumour resection after NAC in previously unresectable tumours. However, it is important to recognize the potential for remaining cancer cells within lymph nodes that have been reduced in size. The cancer stage must therefore be accurately diagnosed after NAC, although this may be difficult because the status of tumour tissue can sometimes be radically altered.
There are few published reports of the use of CPT-11/NED as a NAC regimen. Yamaguchi et al. 10 reported a response rate to CPT-11/NED of 75.8%, which is similar to the response rate in the present study (75%). These authors concluded that NAC with CPT-11/NED is an effective and well-tolerated treatment for patients with bulky stage Ib2–IIb SCC of the uterine cervix. 10 However, they did not evaluate the advantages and disadvantages of this therapy compared with other treatments.
In the present study, the administration of CPT-11/NED or TUAC as an NAC regimen prior to radical surgery had comparable or superior survival rates to primary surgery alone and radiotherapy. Analysis of the change in NAC protocols from TUAC to systemic chemotherapy (CPT-11/NED) demonstrated very high response rates for both regimens (78% and 75%, respectively); the difference in rates was not significant. In contrast, severe thrombocytopenia was more frequent in the TUAC group (72%) than in the CPT-11/NED group (2%). Furthermore, the technique required to administer TUAC is more complicated than that for systemic chemotherapy. Therefore, systemic chemotherapy using CPT-11/NED as a NAC regimen appears to be gentler on the body and requires less skill to administer than TUAC. However, CPT-11 has been reported to be associated with severe adverse events, including leukopenia and diarrhoea; 30 nedaplatin has been reported to cause leukopenia, although milder than that associated with cisplatin. 31 To reduce severe adverse events while maintaining the anticancer effects of CPT-11, the schedule for CPT-11 administration can be modified. 32 Addition of granulocyte-colony stimulating factor successfully prevented or controlled CPT-11- and nedaplatin-induced neutropenia, 20 and the use of the Kampo medicine Hangeshashin-to (TJ-14) ameliorated diarrhoea associated with CPT-11 treatment in patients with nonsmall-cell lung cancer. 33 In the present study, no fatal events occurred when NAC was performed using CPT-11/NED.
In the present study the adverse events of NAC using CPT-11/NED were compared with data reported for patients treated with CCRT. Severe anaemia, vomiting and cystitis were less frequently reported in patients treated with NAC with CPT-11/NED than in those treated with CCRT. Pignata et al 25 reported that diarrhoea was the only severe and dose-limiting nonhaematological toxicity associated with CCRT. In a recent report on long-term health-related quality-of-life in cervical cancer, survivors who received radiotherapy were significantly worse in terms of sexual dysfunction (P = 0.002), voiding and abdominal symptoms (P = 0.01) and lymphoedema (P = 0.01) compared with survivors treated by surgery alone. 34 Therefore, the administration of adjuvant chemotherapy, but not radiotherapy, after NAC plus radical hysterectomy is recommended. In the present study, all 70 patients who received NAC remain alive without any serious sequelae.
The initial treatment for patients with locally advanced cervical cancer has been the subject of debate in many countries. CCRT is the standard therapy in the USA,5–8 whereas NAC followed by radical hysterectomy is performed in some institutions in Europe and Asia.2–4 Therefore, there is a question as to whether NAC is, or is not, more efficacious than CCRT in patients with locally advanced cervical cancer. Currently, no studies show that the survival rates for patients treated with CCRT exceed those of patients treated with NAC. In a retrospective patient-data review conducted over 10 years in Korea, there were no statistically significant differences in the 5-year disease-free survival rates for stage Ib2 cervical cancer between the surgery, NAC and CCRT groups. 35 In contrast, another retrospective study showed that NAC followed by radical hysterectomy improved the long-term disease-free survival and OS compared with CCRT. 36 However, simple prognostic comparisons between NAC, CCRT and other therapies are of limited value because of differences in adjuvant treatments.
In conclusion, the use of CPT-11/NED as a NAC regimen in the present study showed favourable activity, with lower toxicity compared with NAC using TUAC or CCRT, for the treatment of locally advanced cervical cancer, particularly in patients with stage Ib2 disease.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grants from any funding agencies in the public, commercial, or not-for-profit sectors.
