Abstract
Objective
To investigate the clinical significance of cadherin 13 (CDH13) gene promoter methylation in the serum of patients with prostate cancer.
Methods
This prospective study examined the methylation status of CDH13 in serum samples obtained from patients with primary prostate cancer and age-matched control subjects, using methylation-specific polymerase chain reaction. Associations between methylation status of CDH13 and various clinicopathological features and patient survival were evaluated.
Results
A total of 98 patients with prostate cancer and 47 control subjects were enrolled in the study. CDH13 promoter methylation was detected in 44 out of 98 (44.9%) patients with prostate cancer; no methylation was found in control subjects. Methylation of CDH13 was significantly associated with an increased Gleason score, an advanced tumour stage, and a high prostate-specific antigen level. CDH13 methylation was associated with a worse survival outcome and a relative risk of death of 6.132 (95% confidence interval: 3.160, 12.187).
Conclusions
Promoter methylation of CDH13 occurred frequently in the serum of patients with prostate cancer, was associated with an increased risk of death, and may become a useful independent predictor of a poor prognosis.
Introduction
Prostate cancer is one of the most prevalent malignancies, a significant contributor to morbidity and a leading cause of cancer-related death in men in the United States of America, with an estimated 238 590 new cases and 29 720 deaths in 2013. 1 The level of prostate-specific antigen (PSA) in serum is commonly used for diagnosis, monitoring and prognosis, although the PSA assay is not particularly accurate. 2 The survival rate of patients with prostate cancer is decreased with tumour progression, despite advances in clinical surveillance and treatment strategies. 2 In addition to the use of conventional clinicopathological features, molecular biomarkers are needed, particularly those that are associated with the malignant behaviour of prostate cancer, in order to provide the most accurate diagnostic and prognostic information.
Like many other malignancies, prostate cancer is a complicated tumour that arises from progressive genetic and epigenetic alterations. 3 DNA methylation of selected gene promoters is recognized as the most common epigenetic change in prostate cancer.4,5 As observed in other human cancers, DNA methylation of tumour suppressor gene promoters might be detected through analyses of DNA from serum.4,5 This might result in the development of new methods for measuring tumour biomarkers, which could then be used to provide better screening, diagnosis, prognosis, and treatment strategies.
There has been a marked increase in the level of interest in DNA methylation of human cancers.6,7 DNA methylation can be detected not only in tumour samples but also in various body fluids such as blood, serum or plasma.4,5 It is well known that DNA fragments are frequently and abundantly found in the serum of cancer patients (including patients with prostate cancer), and the detection of circulating tumour-related methylated DNA may be used as a potential biomarker for the diagnosis, surveillance and prognosis of patients with prostate cancer.8–10
Cadherin 13 (CDH13), a member of the cadherin family, plays a crucial role in cell–cell adhesion. 11 Changes in CDH13 gene expression have been reported to be associated with tumour behaviour in some human tumours.11–13 Recent studies have highlighted the role of the CDH13 gene as a tumour suppressor in various human cancers such as lung cancer, bladder cancer, breast cancer and malignant melanoma.11–13 The human CDH13 gene is mapped to 16q23.3 on chromosome 16, which is often inactivated by promoter methylation. 11 Promoter methylation of the CDH13 gene in patients with prostate cancer has been reported,14,15 but the clinical significance of CDH13 promoter methylation detected in the serum of patients with prostate cancer remains unclear.
In the current study, methylation-specific polymerase chain reaction (MSP) was used to detect the methylation status of the CDH13 gene promoter in serum-derived DNA from patients with prostate cancer and age-matched control subjects. The clinical significance of the methylation status was determined by analysing the correlations with clinicopathological features and disease outcomes.
Patients and methods
Patients and specimens
This prospective study enrolled consecutive patients with primary prostate cancer who attended the Department of Urology, The Third Hospital of Hebei Medical University, Shijiazhuang, Hebei Province, China, between May 2005 and May 2007. Inclusion criteria were: first histopathological diagnosis of prostate cancer by prostate biopsy; no history of other malignant tumours. Histological grading of each tumour was determined according to the Gleason score; 16 disease stage was determined according to the clinical tumour–node–metastasis classification system of the American Joint Committee on Cancer (T1 to T4), 17 and the treatment strategy used for each patient was according to international guidelines. 18 Patients were followed up according to international guidelines. 18 The control group consisted of inpatients with benign prostatic hyperplasia (BPH), patients with bladder stones and healthy volunteers who were attending the same hospital. Controls were age-matched with prostate cancer patients and provided whole-blood samples for serum production. The inclusion criteria for the control subjects were: no history of malignant tumours; serum PSA concentration <4 ng/ml.
Whole peripheral blood samples (5 ml) were obtained, prior to any treatment, from both the patients and control subjects. These samples were then left at room temperature for 2 h to coagulate, centrifuged at 3000
The study was conducted in accordance with the Declaration of Helsinki and approved by the Ethics Committee of the Third Hospital of Hebei Medical University (registration no. HBMETH20050111E). Written informed consent was obtained from all study participants.
DNA extraction and MSP
DNA was extracted from 500 µl of serum (QIAmp DNA Blood Mini Kit; Qiagen, Valencia, CA, USA), then treated with bisulphite to convert any unmethylated (but not methylated) cytosine residues to uracil (EpiTect Bisulfite Kit; Qiagen) as previously reported. 19 The methylation status of the CDH13 gene was examined using MSP, as described previously.13,20 Briefly, the primers for the methylated reaction were as follows: CDH13 methylated sense, 5′-TCGC
GGGGTTCGTTTTTCGC-3′, and CDH13 methylated antisense, 5′-GACGTTTTCATTCATACACGCG-3′, which amplify a 243-base pair (bp) product (Shanghai Sangon Biological Engineering Technology & Services, Shanghai, China). The primer sequences of CDH13 for the unmethylated reaction were as follows: CDH13 unmethylated sense, 5′-TTGTGGGGTTGTTTTTTGT-3′, and CDH13 unmethylated antisense, 5′-AACTTTTCATTCATACACACA-3′, which amplify a 242-bp product (Shanghai Sangon Biological Engineering Technology & Services). The PCR reactions were carried out using ZymoTaq™ DNA polymerase and ZymoTaq™ PreMix (Zymo Research Corporation, Irvine, CA, USA) in a thermal cycler (BD Biosciences, Hercules, CA, USA). PCR amplification of the modified DNA samples consisted of preliminary denaturation at 95℃ for 5 min, followed by 33 cycles of denaturation at 95℃ for 30 s, annealing at 60℃ for 1 min, and elongation at 72℃ for 1 min for the unmethylated reaction; or 29 cycles of denaturation at 95℃ for 30 s, annealing at 70℃ for 1 min, and elongation at 72℃ for 1 min for the methylated reaction; followed by a final elongation step at 72℃ for 5 min.
Normal lymphocyte DNA methylated in vitro with CpG methyltransferase (SssI methylase; New England Biolabs, Beverly, MA, USA) was used as a methylation positive control, and normal lymphocyte DNA was used as an unmethylation positive control. Water blanks were included within each assay. The PCR products were separated in 2% agarose gel, stained with ethidium bromide, and visualized under ultraviolet illumination. Samples were scored as methylation positive when methylated alleles were present in the methylated DNA lane and methylation negative when bands were present only in the unmethylated DNA lane.13,20
Statistical analyses
All statistical analyses were performed using the SAS® statistical package, version 8.0 (SAS Institute, Cary, NC, USA). For statistical purposes, serum samples were divided into two tumour-grade categories (Gleason score ≤7 versus >7); patients were categorized by age groups (<65 versus ≥65 years) and according to the serum PSA levels (<10 versus ≥10 ng/ml). 21 Fisher’s exact test was used to evaluate the difference in the CDH13 gene methylation status between patients with prostate cancer and control subjects. χ2-test was used to assess the correlations between CDH13 methylation and clinicopathological features of disease. Kaplan–Meier survival analysis and log-rank test were used to assess the difference in 5-year overall survival between patients with prostate cancer with methylated and unmethylated CDH13. Multivariate Cox proportional hazard model analysis was used to estimate the independent prognostic effect of CDH13 methylation, controlling for the classic risk factors of age, tumour stage, Gleason score and PSA. A two-sided P-value <0.05 was considered to indicate statistical significance.
Results
This study analysed the methylation status of the CDH13 gene in serum samples collected from 98 patients with prostate cancer and 47 age-matched control subjects using MSP. In the patient group, 20 patients were stage T1, 23 patients were stage T2, 41 patients were stage T3, and 14 patients were stage T4 at diagnosis. In the control group, 27 patients had BPH, 11 had bladder stones and nine were healthy volunteers.
The MSP analysis found that CDH13 promoter methylation was detected in 44/98 (44.9%) patients with prostate cancer, while no methylation was found in the control subjects (P < 0.0001; Fisher’s exact test). Representative MSP results are shown in Figure 1. The detailed clinicopathological features of the patients with prostate cancer are shown in Table 1. Analysis of the association between the methylation status of CDH13 and the demographic, clinical and pathological features demonstrated that CDH13 methylation in serum was significantly associated with an increased Gleason score (P = 0.0395), an advanced tumour stage (P = 0.0001), and a high PSA level (P = 0.0071); there was no significant association between CDH13 methylation and age (Table 1).
Representative methylation-specific polymerase chain reaction results for cadherin 13 (CDH13) gene promoter methylation in serum from five patients with prostate cancer. M, methylated; U, unmethylated; bp, base pairs. Cases 56, 57 and 59 exhibited promoter methylation of the CDH13 gene. Relationship between cadherin 13 (CDH13) gene promoter methylation in serum and clinicopathological features of patients with prostate cancer (n = 98). Data presented as n (%). χ2-test was used to assess the correlations between CDH13 methylation and clinicopathological features. U, unmethylated CDH13 promoter; M, methylated CDH13 promoter; PSA, prostate-specific antigen; NS, not statistically significant (P ≥ 0.05).

Survival data were available from all patients with prostate cancer. Overall survival was defined as the time from date of diagnosis until date of death from any cause, or last contact if the patient was still alive (range: 9–60 months). When the methylation status of the CDH13 gene promoter was correlated with the overall survival of patients with prostate cancer, patients with unmethylated CDH13 had better outcomes than patients with methylated CDH13 (P = 0.0002; Figure 2). In addition, multivariate Cox proportional hazard model analysis was carried out to estimate the independent prognostic effect of CDH13 methylation, controlling for the classic risk factors of age, tumour stage, Gleason score and PSA. Multivariate analysis indicated that CDH13 methylation was independently associated with a worse outcome and had a relative risk of death of 6.132 (95% confidence interval 3.160, 12.187; P = 0.0073; Table 2).
Kaplan–Meier survival curves for patients with prostate cancer (n = 98) stratified according to their cadherin-13 (CDH13) gene promoter methylation status. P = 0.0002; log-rank test. Multivariate Cox proportional hazard analysis of independent predictors of 5-year overall survival in patients with prostate cancer (n = 98) controlling for classic risk factors. CI, confidence interval; CDH13, cadherin 13 gene; PSA, prostate-specific antigen; NS, not statistically significant (P ≥ 0.05).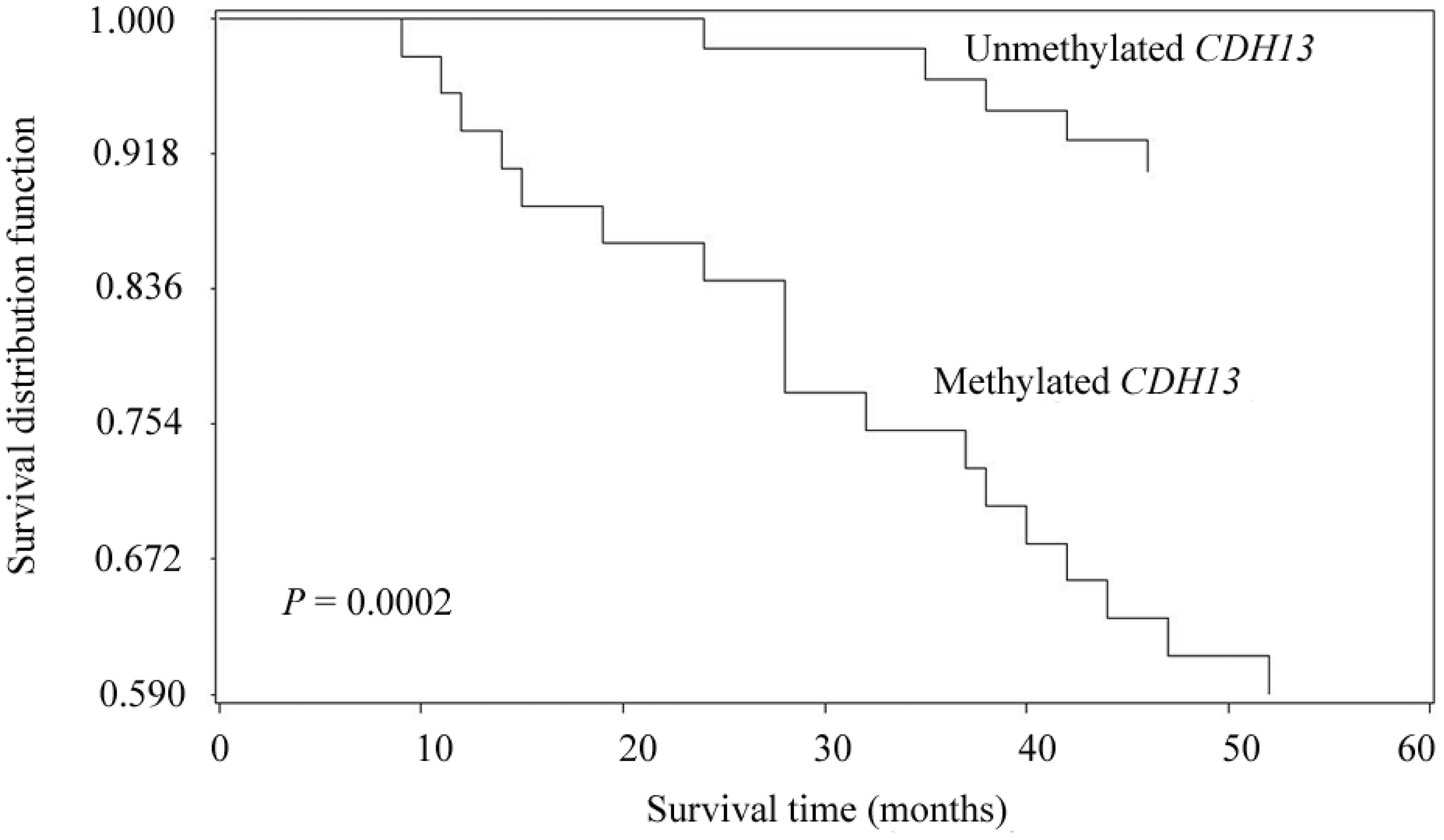

Discussion
Previous studies have described the importance of DNA methylation in human cancers, with aberrant DNA methylation in the promoter regions of tumour suppressor genes at cytosine-phosphate-guanine islands being recognized as one of the hallmarks of human cancers, and associated with the downregulation of gene expression. 22 Aberrant DNA methylation can be evaluated both in tissue samples and body fluids, especially in serum; serum contains abundant tumour-specific DNA fragments in cancer patients. 23 Testing DNA methylation in serum has the advantages of high sensitivity, noninvasiveness, low cost, and suitability for routine clinical application.10,19,21,24 Moreover, MSP is a simple, sensitive, specific and cost-effective method, and is the most commonly employed method for DNA methylation analysis.10,19,21,24 In the current study, MSP was used to detect the methylation status of the CDH13 gene promoter in the serum of patients with prostate cancer compared with control subjects in order to evaluate its clinical significance.
Studies have demonstrated that the CDH13 gene functions as a tumour suppressor in various human cancers; downregulation of CDH13 gene expression was associated with malignant behaviours of human cancers, and the introduction of CDH13 into human cancer cells can reduce their malignant potential. 11 Previous studies have demonstrated that aberrant DNA methylation is the main mechanism of the inactivation of CDH13 in human cancers. 11 Alumkal et al. 25 demonstrated that the methylation of CDH13 in tumour samples was independently associated with an increased risk of biochemical recurrence after radical prostatectomy; where biochemical recurrence was defined as the measurement of two successive values of serum PSA ≥0.2 ng/ml after initial treatment. Such findings suggest that CDH13 methylation may play a crucial role in prostate cancer, which provides the rationale for undertaking this present study, to evaluate the clinical significance of CDH13 methylation in the serum of patients with prostate cancer.
In the current study, the methylation of CDH13 in serum specimens from patients with prostate cancer and control subjects was analysed using MSP. The analysis demonstrated that CDH13 methylation occurred frequently in patients with prostate cancer, while no methylation was found in the control subjects. Moreover, CDH13 methylation was also observed in patients with stage T1/T2 disease. These current findings suggest that CDH13 methylation is tumour specific and an early event during the pathogenesis of prostate cancer. The results indicated that CDH13 methylation was associated with an increased Gleason score, an advanced tumour stage, and a high serum PSA level, suggesting that CDH13 methylation in serum is correlated with the clinical risk factors of death. In addition, the 5-year overall survival of patients with prostate cancer was examined according to the methylation status of CDH13 in serum. CDH13 methylation was associated with adverse 5-year overall survival. Moreover, multivariate Cox proportional hazard model analysis indicated that the methylation of CDH13 was independently associated with a statistically significant increased risk of death (hazard ratio 6.132; 95% confidence interval 3.160, 12.187; P = 0.0073). Thus, determination of CDH13 methylation in serum may convey relevant prognostic information and may become a useful predictor of disease outcomes in the future.
In conclusion, aberrant CDH13 promoter methylation in serum correlates with the clinical risk factors of death and was significantly associated with a worse disease outcome. Current findings suggest that aberrant CDH13 promoter methylation may be used as a novel biomarker and a potential therapeutic target for prostate cancer. However, this present study was limited by a small sample size, and future multicentre studies with larger sample sizes are needed, to confirm whether CDH13 promoter methylation in serum could be used as a novel predictor of overall survival in patients with prostate cancer.
Footnotes
Declaration of conflicting interest
The authors declare that there are no conflict of interests.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
